Health
Vol.5 No.12(2013), Article ID:40889,7 pages DOI:10.4236/health.2013.512270
Low serum vitamin D among community-dwelling healthy women in Sri Lanka*
![]()
1Department of Anatomy, Faculty of Medicine, University of Ruhuna, Ruhuna, Sri Lanka; #Corresponding Author: manjula.hettiarachchi@gmail.com
2Nuclear Medicine Unit, Faculty of Medicine, University of Ruhuna, Ruhuna, Sri Lanka
3Center for Metabolic Bone Diseases, Department of Medicine, Faculty of Medicine, University of Ruhuna, Ruhuna, Sri Lanka
Copyright © 2013 Mahinda Rodrigo et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 30 September 2013; revised 29 October 2013; accepted 15 November 2013
Keywords: Phalangeal BMD; Phalangeal BMC; Vitamin D; Parathyroid Hormone; Anthropometry
ABSTRACT
Background: Although hypovitaminosis D is prevalent among healthy adults in Asia and other regions, available data among Sri Lankans are not consistent with this finding. We studied vitamin D level among healthy community-dwelling women and examined its effects on parathyroid hormone (PTH) level and bone mineral status. Methods: Females of 20 - 40 years (n = 434) who were employed in southern Sri Lanka were recruited to the study. Bone mineral density and content (pBMD and pBMC) of the middle phalanx of the middle finger of the non-dominant hand were measured in all subjects and 5.0 ml of venous blood was collected from each subject after an overnight fast for biochemical assessment of serum vitamin D, parathyroid hormone and total alkaline phosphatase. Results: Mean (SD) pBMD of the women studied was 0.493 (0.060) g/cm2 and pBMC was 1.49 (0.28) g. Severe vitamin D deficiency (<12.5 nmol/L) was seen in 21.4% of subjects, whereas 19.1% subjects had moderate (12.5 - 25.0 nmol/L) and 15.7% had mild (25.1 - 35.0 nmol/L) vitamin D deficiency. Serum vitamin D showed significant positive correlations with pBMD (r = 0.13, p = 0.008) and pBMC (r = 0.12, p = 0.01). In regression analysis, vitamin D showed a positive association with pBMD (regression coefficient 0.0003, SEM 0.0001, p = 0.007). Conclusions: Vitamin D insufficiency/deficiency is prevalent among healthy young and middle-aged women in this study group selected from southern Sri Lanka. The accompanying rise of PTH indicates the biological significance of low vitamin D level. The negative effects observed on bone mineral status suggest the clinical importance of this finding.
1. INTRODUCTION
Vitamin D has profound effects on the growth and skeletal development of children and it is a major determinant of adult bone health. Vitamin D deficiency leads to rickets or osteomalacia, and even a mild deficiency induces secondary hyperparathyroidism and increased bone resorption [1]. Vitamin D helps maintain the normal serum calcium level within a very narrow range [2]. Vitamin D deficiency lowers intestinal calcium absorption from 30% to 15% [3]. This leads to an increased serum parathyroid hormone level, which is an important determinant of cortical bone remodeling in the elderly [1]. Decreased serum phosphates due to increased renal excretion caused by secondary hyperparathyroidism and increased alkaline phosphatase are the other metabolic effects of Vitamin D deficiency [3].
Earlier studies which attempted to determine serum 25(OH)vit-D reference values among healthy subjects may have been influenced by diverse lifestyle and environmental characteristics, and therefore, may not be applied clinically and worldwide [4,5]. Defining vitamin D thresholds according to health consequences rather than population means is the preferred method but debate on “normal” or “optimal” 25(OH)vit-D level still continues. Several criteria have been used to define sufficient 25(OH) vit-D levels, including the level associated with optimal suppression of circulating parath hormone (PTH), greatest calcium absorption, highest bone mineral density (BMD), lowest rates of bone loss, falls, or fractures [6].
Previous studies have demonstrated low serum vitamin 25(OH)D levels in populations across neighboring countries of Sri Lanka. In North India, 91% of healthy school girls [7] and 84% of pregnant women [8] were found to have hypovitaminosis D with the cut-off value for serum 25(OH)D level below 50 nmol/L. Similar data have been reported from Pakistan [9] and Bangladesh [10]. Vitamin D status of the population in South-East Asian countries has received relatively less attention. However, the problem seems to be less severe in Thailand [11]. High prevalence of hypovitaminosis D in South Asia can be explained by skin pigmentation and traditional clothing. Air pollution and limited outdoor activity further compound this problem in the urban population.
Knowledge on vitamin D status among Sri Lankan is limited [12]. There were no studies done on Sri Lankan men’s vitamin D levels. Hence, clinicians vary in their practice regarding the dose of vitamin D prescribed in the treatment of osteoporosis. Sri Lanka has no major seasonal variation in weather and sunlight is available during most of the daytime throughout the year. This is taken as an assurance of adequate vitamin D levels among Sri Lankan but the accuracy of this statement has not been adequately examined. Although the vitamin D metabolism among elders is the major health concern, studies among community-dwelling healthy adults are considered priority in order to understand the state of vitamin D metabolism in the entire age range. This would allow us to determine whether vitamin D deficiency is restricted to certain age groups or it is more widely spread. Hence, in an ongoing study examining the association between vitamin D and bone health in different age groups, we initially selected a group of healthy pre-menopausal women.
We hypothesized that young women in Sri Lanka may be vitamin D deficient and this would have a negative effect on their bone health. We used AccuDXA which measures bone mineral content (BMC) and density in the middle phalanx of the middle finger, using Dual-energy X-ray absorptiometry technique, to measure bone mineral status. AccuDXA was particularly selected for this study due to the restricted availability of central-type densitometers in Sri Lanka and the easiness of using AccuDXA in the community settings. A previous study in Sri Lanka has shown a high correlation between phalangeal BMD measured by AccuDXA and BMDs in central sites such as spine and femoral neck [13]. Furthermore, phalangeal BMD predicts fractures to the same extent as BMDs in spine or proximal femur [14,15]. In a population-based study showing the inverse relationship between measured serum 25(OH)D levels and PTH levels, vitamin D levels were significantly higher in rural compared to urban subjects [16]. As the negative influence of elevated PTH is seen first in the peripheral cortical-rich skeletal sites, we believed that AccuDXA which measures BMD in the cortically-rich middle phalanx could be a valid tool to measure the effect of elevated PTH.
2. MATERIALS AND METHODS
The study was conducted in South of Sri Lanka after obtaining approval from the Ethical Review Committee of the Faculty of Medicine, Galle. Females of 20 - 40 years who were employed in the institutions located in the Galle district were the study population. Subjects were selected using multistage cluster sampling technique. These institutions were first stratified according to the number of female staff members and then seven such places were randomly selected such as a hospital (1), teacher training schools (2), technical colleges (2) and schools (2). All the females of this age group attached to the selected institutions were considered eligible for the study.
Selected institutions were informed one to two weeks before the intended visit and permission was obtained from the relevant authorities. Eligible women were informed about the study by the investigators and informed written consent was obtained. They (n = 582) were interviewed and a brief clinical examination was performed. Women who had taken medications such as systemic corticosteroids (n = 16), thyroxin (n = 8), hormone replacement therapy or contraceptive pills (n = 44), multi-vitamin preparations including vitamin D (n = 38), thiazide diuretics (n = 12), pharmacological doses of calcium (n = 20) and women who had chronic liver or renal disease (05) and endocrine disorders (05) were excluded from the study. Similarly women with long standing inflammatory or infective diseases were also excluded. However, women with non-communicable diseases such as diabetes, hypertension or hyperlipidaemia were not excluded unless they belonged to above mentioned exclusion criteria.
All individuals who were eligible after the first interaction (n = 434) were subjected to a comprehensive physical examination, including measurements of body weight and height. Height was measured using a portable stadiometer (IUCHI, Yamato Scientific, Japan) and weight was measured using a portable beam balance (Bauman, Germany) with non-detachable weights. We measured BMD (pBMD) and BMC (pBMC) of the middle phalanx of the middle finger of the non-dominant hand in all subjects. AccuDXA (Shick technology, New York, USA), portable densitometer with dual-energy X-ray absorptiometry technique (DXA) was used to measure BMD. AccuDXA has less than one minute scan time and measurement precision of less than 1.0%. All scans were done by one technician who had a prior training on accuDXA and the accuracy and precision of the machine were tested on each scanning day using the inbuilt software. Machine was kept in a cool environment during scanning to ensure the accuracy of measurements.
Five milliliters (5 ml) of venous blood was collected from each subject after overnight fast for the biochemical assessment of serum vitamin D, parathyroid hormone and total alkaline phosphatase. Specimens were immediately transported to the RIA laboratory of the Faculty of Medicine, Galle in a box containing ice packs and serum separation was done without delay and stored in a freezer at −80˚C. Liquid phase radioimmunoassay methodology was used for quantitative determination of 25(OH) vit-D levels in serum using the IDS Gamma-B 25-hydroxy-vitamin D kits obtained from Immunodiagnostic Systems (IDS) limited UK with a precision of the intra-assay of 6.1% and inter-assay 7.3%. The Immunotech radioimmunoassay kit was used for the determination of parathyroid hormone levels. In PTH estimations, the coefficients of variation of the intra-assays was 7.45%, whereas interassay was 8.5%. Serum total alkaline phosphatase (ALP) was measured using Kinetic photometric test where the lower limit of detection was 2 IU/L. Intra-assay precision of ALP estimation was below 0.50% and inter-assay coefficient variation was 2.0%.
Statistical Analysis
Data were analyzed using open source statistical software [17]. All results including pBMD and pBMC measurements are presented as mean (standard deviation) unless stated otherwise. Serum 25-vitD, PTH and ALP showed a skewed distribution and values were log transformed before analysis. Correlation and regression methods were used to examine the associations between pBMD/pBMC and other measurements recorded as continuous numerical variables. Analysis of variance (ANOVA) test was used to detect differences between groups. Twotailed p less than 0.05 was selected as the level of statistical significance.
3. RESULTS
The baseline measurements of phalangeal BMD/BMC and the anthropometry are given in Table 1. Out of 434 women in the study sample, 202 (46.5%) were married. None of the subjects admitted having smoked or taken alcohol at any stage in their lives. Anthropometric measurements (weight, height and BMI) were positively and significantly (p < 0.001) correlated, with both pBMD and pBMC.
When all the anthropometric measures were included in a regression model and weak associations were excluded in a step-wise fashion, height remained the strongest predictor of pBMD (regression coefficient 0.004; SE 0.0004; p < 0.001). In this model, height alone explained 12% of variation in pBMD. A one centimeter difference in height was associated with 0.004 g/cm2 difference in pBMD. Similarly, a change of one kilogram was associated with 0.002 g/cm2 change in pBMD. A unit increase in BMI was associated with an increase in pBMD of 0.003 g/cm2.
The median (interquartile range-IQR) serum vitamin Dand PTH concentrations were 30.86 (15.61 - 52.37) nmol/L and 52.00 (30.80 - 70.00) pg/mL respectively. Serum alkaline phosphatase level was 61.76 (IQR 44.98 - 78.00) IU/L (Table 2). Severe vitamin D deficiency (below 12.5 nmol/L) defined according to the Lips classification (Lips, 2001) was seen in 21.4% of subjects. Further, 19.1% subjects had moderate (12.5 - 25.0 nmol/L) and 15.7% had mild (25.1 - 35.0 nmol/L) vitamin D deficiency. Elevated serum PTH concentrations (>65.0 pgm/L) was observed in 142 (33.5%) women whereas elevated serum ALP (>95.0 IU/L) was observed in 51 (11.7%) subjects. Serum vitamin D showed significant positive correlations with BMD (r = 0.13, p = 0.008) and BMC (r = 0.12, p = 0.01) and a significant negative correlation with PTH (r = −0.62, p < 0.001). Serum PTH showed a significant negative correlations with both BMD (r = −0.16, p = 0.001 and BMC (r = −0.15, p = 0.002). Although ALP showed negative correlations with BMD (−0.02, p = 0.74) and BMC (−0.03, p = 0.52), they were not statistically significant. In regression analysis involving pMBD as the dependent variable and vitamin D as the independent variable, vitamin D showed a positive association with pBMD (regression coefficient 0.0003, SEM 0.0001, p = 0.007). Inclusion of height, weight or BMI in the model did not change the results materially.
Regression model was fitted with PTH as the dependent variable and vitamin D as the independent variable to assess the relationship of these two variables (Figure 1). Using the regression equation (intercept = 73.08 and
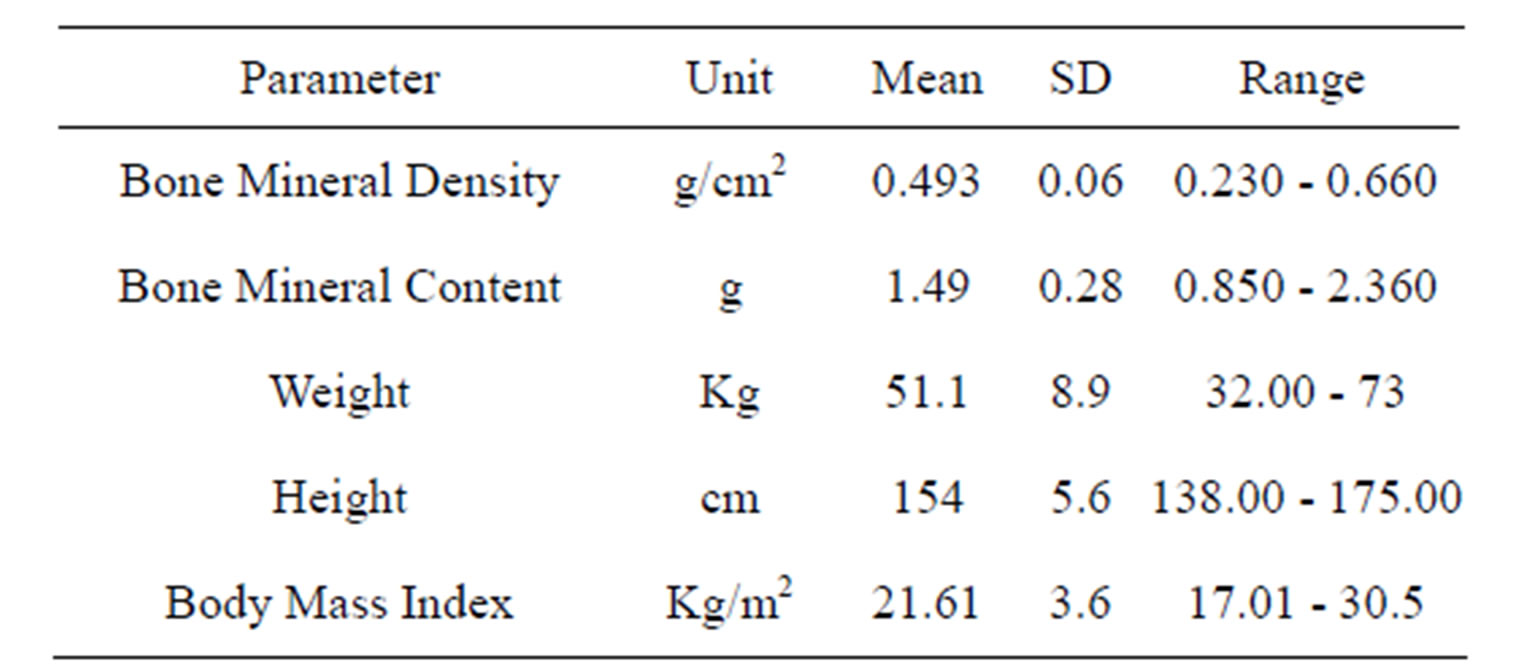
Table 1. Baseline characteristics of the study population1.
1There were 434 subjects enrolled for the study.
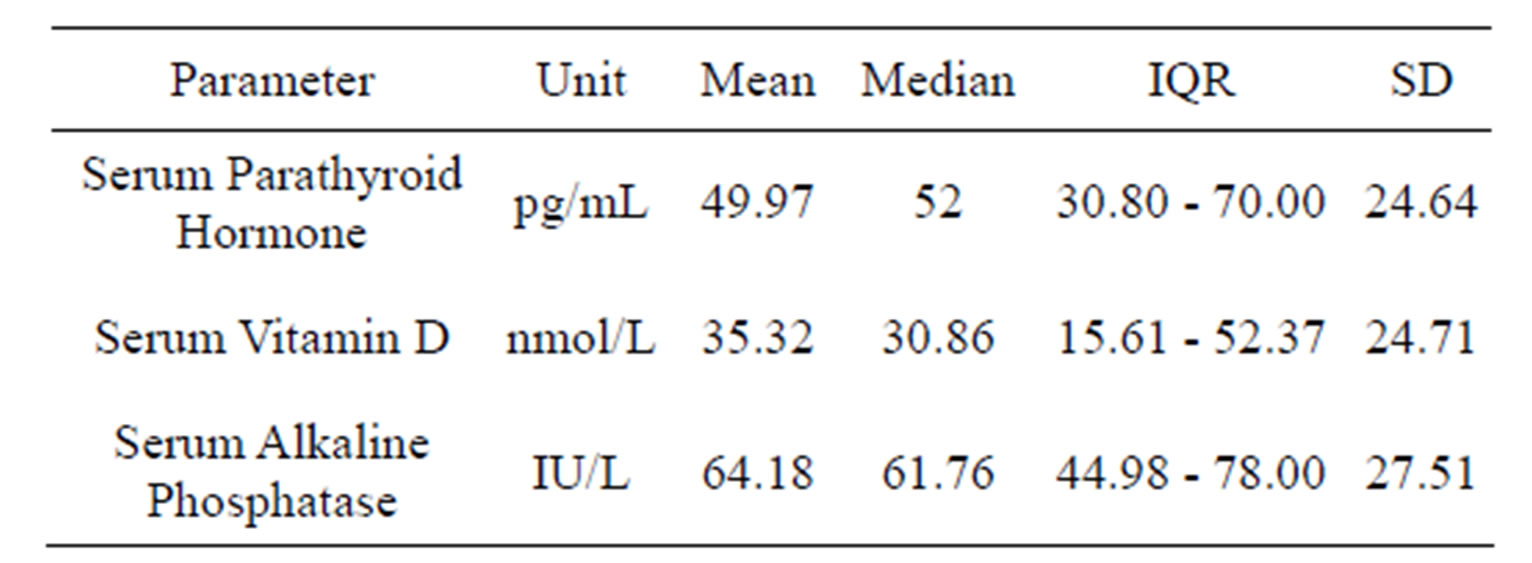
Table 2. Distribution of serum vitamin D, PTH and ALP1.
1There were 434 samples for analysis.
gradient = −0.62), rising of PTH above 65.0 pg/mL was seen at the vitamin D level of 13.02 nmol/L. Ninety six subjects (22.1%) of our study sample had vitamin D levels < 13.02 nmol/L. Among them, 76% of subjects (n = 73) had elevated PTH (>65 pg/mL). Other 24 % (n = 23) had mean PTH concentration of 51.64 pg/mL (median of 58.00 pgm/L).
Further, BMC/BMD, anthropometric indices and other serum measurements were analyzed in the tertiles of vitamin Dconcentration (Table 3). In contrast to women in the lower tertile of vitamin D, women in the upper tertile were shorter, had higher BMD and lower PTH level. BMC, weight and BMI showed no difference in the tertiles of vitamin D. Women with lower vitamin Dhad higher PTH level and women with higher vitamin D had lower PTH level. Furthermore, PTH showed a trend across the tertiles of vitamin D. Serum ALP, the widely used surrogate marker of vitamin D deficiency in clinical evaluation of patients, showed poor correlation with vitamin D and PTH levels indicating that it is not reflective of serum vitamin D level.
4. DISCUSSION
This study which examined vitamin D, PTH and alkaline phosphatase among women of 20 - 40 years in Southern Sri Lanka showed a high prevalence of vitamin D insufficiency among subjects. In addition, serum ALP level showed a poor correlation with vitamin D indicating its limited ability to demonstrate underlying hypovitaminosis D. While hypovitaminosis D was prevalent among the study subjects, a corresponding rise in serum PTH among them indicated that the low levels of vitamin D observed is not a mere biochemical finding but has
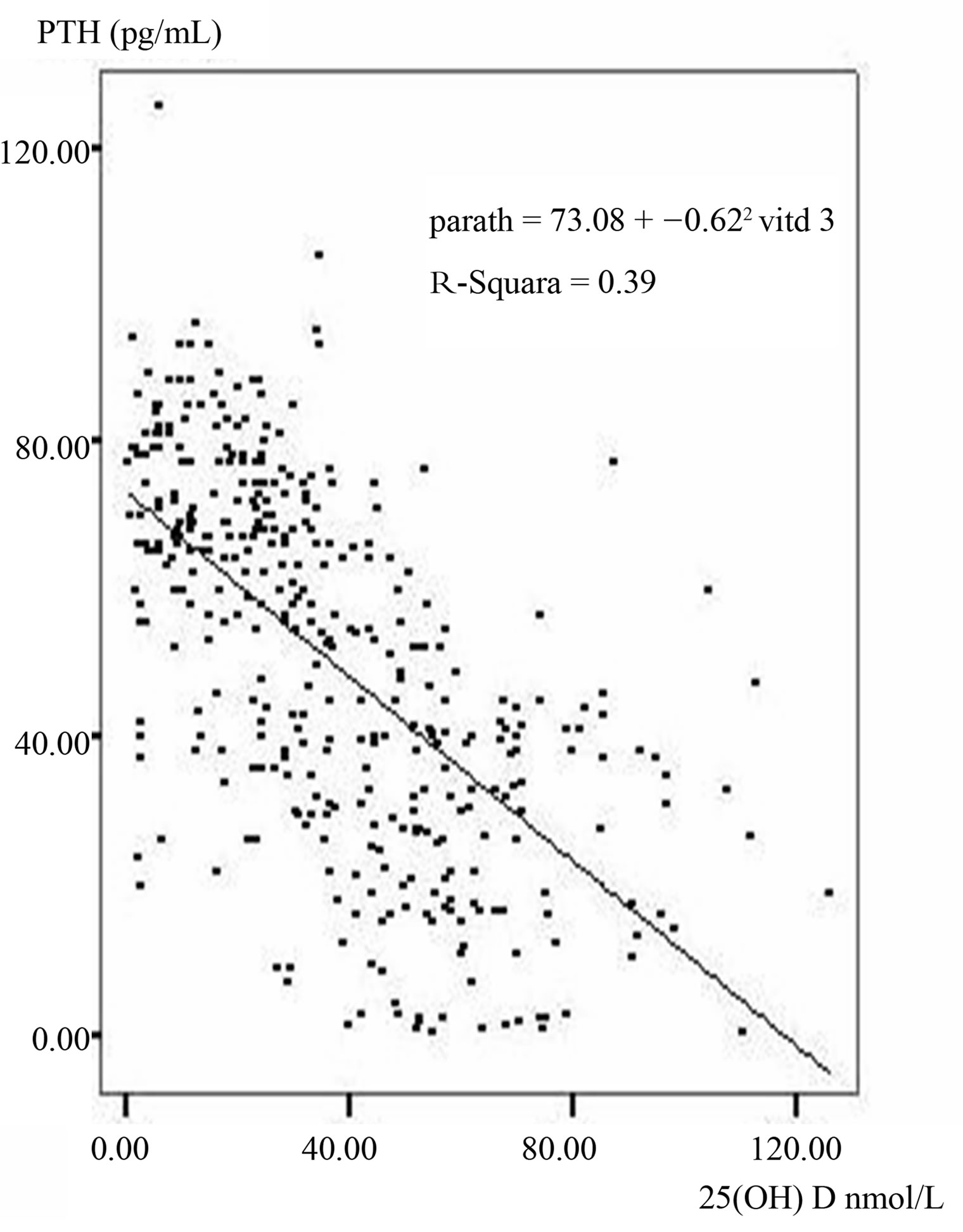
Figure 1. Linear regression between PTH and vitamin D levels of the study sample.
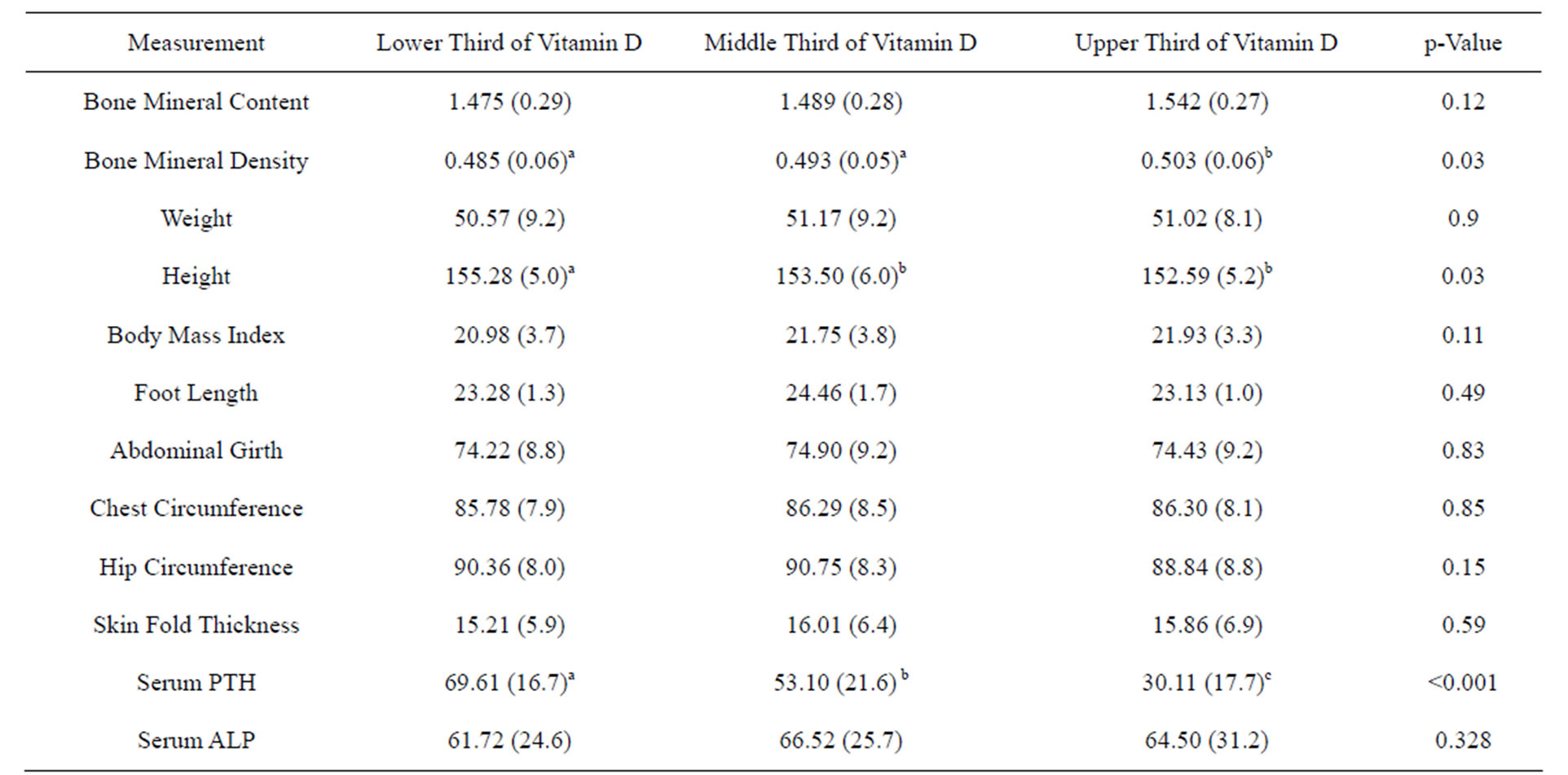
Table 3. Anthropometry, BMD and other serum measurements (PTH, ALP) in the tertiles of vitamin D concentrations1.
1There were 145 subjects in each thirds of serum vitamin D. a,b,cvalues with different superscript in a row are significantly different (ANOVA; p < 0.05).
definite metabolic consequences. This was further strengthened by finding lower pBMD/pBMC among vitamin D deficient subjects.
Data on vitamin D status among Sri Lanka are limited. Mayer et al., [12] estimated 25-vitD levels of Sri Lankan ethnic Tamils from the central part of the country and compared it with a similar ethnic group in Norway. In their analysis among 30 - 60-year-old community-dwelling Sri Lankan women, the mean 25-vitD level was 47.4 ± 15.8 nmol/L. This level was 1.4 times higher than what we have seen in the southern coastal border of the country. Further, they observed only 6.3% of subjects to have 25-vitD levels <25.0 nmol/L. We observed 40.5% of subjects in our sample to be below this cut-off value. There can be several reasons for this disparity. Firstly, ethnic Tamils may synthesize more vitamin D with sunlight exposure. Secondly, the period of sun exposure of subjects in the two studies could be different. Most of our study subjects were employed in office-based jobs and had less sun exposure, often limited to 5 - 15 min/day in the early morning hours. This information, however, is not readily available in the other study. Thirdly, the differences in eating habits between the two ethnic groups may provide an explanation for the observed differences.
Despite the abundant sunlight, previous studies have reported a high prevalence of vitamin D deficiency in South Asian countries [10,18-20]. In fact, a comparison of the present findings on serum vitamin D data with other studies may not be entirely appropriate as the studies have been conducted in different seasons, with different study subjects and using different assays. However, the present study indicates the occurrence of high prevalence of hypovitamin D in a country with abundant sunlight. The possible reasons could be the restricted availability of ultra violet light in the correct range to facilitate skin vitamin D synthesis, or the shaded sunshine due to overcastting of sky, or shadows created by buildings and trees and type of dresses which cover most of the body surface.
The renal production of 1,25-dihydroxy vitamin D is tightly regulated by plasma parathyroid hormone and serum calcium and phosphorus levels [21]. Although there is no consensus on optimal levels of 25-vitD as measured in serum, vitamin D deficiency is defined by most experts as a 25-vitD level of <50 nmol/L [22]. The 25-vitD levels are inversely associated with parathyroid hormone levels until the former reach 30.0 - 40.0 pg/L, at which point parathyroid hormone levels begin to level off [23]. Some studies have used increased PTH as a surrogate of vitamin D deficiency. Need et al., [24] showed a gradual increase in PTH levels in subjects with 25-vitD <40.0 nmol/L. Other studies using PTH change as the surrogate marker of vitamin D deficiency have selected different levels: 30.0 nmol/L [25] and 37.5 nmol/L [26]. In our study, the mean PTH concentration in women with normal vitamin D (>35.0 nmol/L) was 32.7 pg/mL. However, mild vitamin D deficient women had a mean PTH level of 57.2 pg/mL (p < 0.05). Our analysis revealed that the rise in PTH begins at vitamin D level of 13.02 nmol/L. Hence this level would demarcate vitamin D deficiency among our subjects. Twenty two percent (n = 96) of subjects had their vitamin D levels < 13.02 nmol/L. In this subgroup of vitamin D insufficient women, 76.0% of subjects (n = 73) had elevated PTH (>65 pg/mL). Although the role of PTH in the pathogenesis of osteoporosis may not be fully elucidated as yet, PTH level is considered to be a useful marker of vitamin D adequacy.
Subclinical vitamin D deficiency is considered to be a risk factor for osteoporosis and fractures [27]. In the present study, we observed a trend of progressive increase in pBMD with increasing tertiles of 25-vitD concentrations. In addition, 25-vitD showed a significant and positive (P < 0.001) influence on the pBMD/pBMC. In a previous study, serum vitamin D level was directly related to BMD in white, black, and Mexican-American men and women, with a maximum density achieved when the vitamin D level reached 100.0 nmol/L or more [28]. When the level was 75.0 nmol/L or less, there was a significant decrease in intestinal calcium absorption [29] that associated with increased PTH response [23]. The Women’s Health Initiative study [30] also showed that serum level of vitamin D had little effect on the risk of fracture when levels were 65.0 nmol/L or less. However, women who were most consistent in taking calcium and vitamin D3 had a 29% reduction in hip fracture. Optimal prevention of both non-vertebral and hip fracture occurred only in trials providing 700 to 800 IU of vitamin D3 per day in patients whose baseline concentration of vitamin D was <42.0 nmol/L and whose mean concentration of vitamin D then rose to approximately 100.0 nmol/L [28].
The limitations of our investigation would be the use of phalangeal BMD. AccuDXA is portable, hence easy to use in community surveys. The availability of central DXA technology in Sri Lanka is greatly limited. In previous studies, phalangeal BMD has shown a good correlation with BMDs in central sites such as hip and spine [31]. Still BMDs in different sites behave differently limiting applicability of our finding to other skeletal sites. Secondly, our sample was limited to females who were working indoors. Other employment categories such as field workers and unemployed women may have different nutritional and sunlight exposure patterns resulting different vitamin D levels. Thirdly, the country’s geographical and ethnic variations are not represented in the study sample. This could compromise the external validity of the results. However, the supervised sample collection, timely transportation and storage of serum samples as well as employment of radioimmunoassay techniques for the analysis of serum PTH and vitamin D assessment may result in higher accuracy in the estimated parameters.
Our results indicate a high frequency of 25-vitD insufficiency/deficiency and its association with PTH hormone status. Data also indicate the positive association between BMD and anthropometric measures of nutrition such as height, weight and BMI. This study needs to be repeated using subjects of different categories to clarify the issue. This is especially needed as two available studies show contrasting results.
5. ACKNOWLEDGEMENTS
We would like to acknowledge the assistant given by the technical staff of the Nuclear Medicine Unit in analyzing the serum samples and the technical staff of the CBMD for performing BMD measurements.
REFERENCES
- Parfitt, A.M., Gallagher, J.C., Heaney, R.P., et al. (1982) Vitamin D and bone health in the elderly. The American Journal of Clinical Nutrition, 36, 1014-1031.
- Deluca, H.F. (1988) The vitamin D story: A collaborative effort of basic science and clinical medicine. Proceedings of American Society Experimental Biology, 2, 224-236.
- Devine, A., Wilson, S.G., Dick, I.M. and Prince, R.L. (2002) Effects of vitamin D metabolites on intestinal calcium absorption and bone turnover in elderly women American Journal of Clinical Nutrition, 75, 283-288.
- Holick, M. (2002) Vitamin D: The underappreciated Dlightful hormone that is important for skeletal and cellular health. Current Opinion in Endocrinology, Diabetes and Obesity, 9, 87-98. http://dx.doi.org/10.1097/00060793-200202000-00011
- Lips, P. (2001) Vitamin D deficiency and secondary hyperparathyroidism in the elderly: Consequences for bone loss and fractures and therapeutic implications. Endocrine Reviews, 22, 477-501. http://dx.doi.org/10.1210/er.22.4.477
- Dawson-Hughes, B., Heaney, R.P., Holick, M.F., et al. (2005) Estimates of optimal vitamin D status. Osteoporosis International, 16, 713-716. http://dx.doi.org/10.1007/s00198-005-1867-7
- Puri, S., Marwaha, R.K., Agarwal, N., et al. (2008) Vitamin D status of apparently healthy schoolgirls from two different socioeconomic strata in Delhi: Relation to nutrition and lifestyle. British Journal of Nutrition, 99, 876- 882. http://dx.doi.org/10.1017/S0007114507831758
- Sachan, A., Gupta, R., Das, V., et al. (2005) High prevalence of vitamin D deficiency among pregnant women and their newborns in northern India. The American Journal of Clinical Nutrition, 81, 1060-1064.
- Rashid, A., Mohammed, T., Stephens, W.P., et al. (1983) Vitamin D state of Asians living in Pakistan. British Medical Journal, 286, 182-184. http://dx.doi.org/10.1136/bmj.286.6360.182
- Islam, M.Z., Shamim, A.A., Kemi, V., et al. (2008) Vitamin D deficiency and low bone status in adult female garment factory workers in Bangladesh. British Journal of Nutrition, 99, 1322-1329. http://dx.doi.org/10.1017/S0007114508894445
- Chailurkit, L.-O., Rajatanavin, R., Teerarungsikul, K., et al. (1996) Serum vitamin D, parathyroid hormone and biochemical markers of bone turnover in normal Thai subjects. Journal of the Medical Association of Thailand, 79, 499-504.
- Meyer, H.E., Holvik, K., Lofthus, C.M. and Tennakoon, S.U.B. (2008) Vitamin D status in Sri Lankans living in Sri Lanka and Norway. British Journal of Nutrition, 99, 941-944. http://dx.doi.org/10.1017/S0007114507844138
- Lekamwasam, S., Wijayaratne, L., Rodrigo, M. and Hewage, U. (2007) Prevalence of osteoporosis among postmenopausal women in Sri Lanka: A cross-sectional community study. APLAR Journal of Rheumatology, 10, 234- 238. http://dx.doi.org/10.1111/j.1479-8077.2007.00301.x
- Reginster, J.Y., Dethor, M., Pirenne, H., Dewe, W. and Albert, A. (2003) Reproducibility and diagnostic sensitivity of ultrasonometry of the phalanges to assess osteoporosis. International Journal of Gynecology & Obstetrics, 63, 21-28.
- Sydney, L.B. and Lori, A.L. (2002) Bone densitometry for technologists. Humana Press Inc., Totowa.
- Harinarayan, C.V., Ramalakshmi, T., Prasad, U.V. and Sudhakar, D. (2008) Vitamin D status in andhrapradesh: A population based study. Indian Journal of Medical Research, 127, 211-218.
- Ripley, B.D. (2001) Using databases with R. R News, 1, 18-20.
- Goswami, R., Gupta, N., Goswami, D., Marwaha, R.K., Tandon, N. and Kochupillai, N. (2000) Prevalence and significance of low 25-hydroxyvitamin D concentrations in healthy subjects in Delhi. The American Journal of Clinical Nutrition, 72, 472-475.
- Tandon, N., Marwaha, R.K., Kalra, S., et al. (2003) Bone mineral parameters in healthy young Indian adults with optimal vitamin D availability. Internal Medical Journal of India, 16, 298-302.
- Arya, V., Bhambri, R., Godbole, M.M. and Mithal, A. (2004) Vitamin D status and its relationship with bone mineral density in healthy Asian Indians. Osteoporosis International, 15, 56-61. http://dx.doi.org/10.1007/s00198-003-1491-3
- DeLuca, H.F. (2004) Overview of general physiologic features and functions of vitamin D. The American Journal of Clinical Nutrition, 80(S), 1689S-1696S.
- Holick, M.F. (2006) High prevalence of vitamin D inadequacy and implications for health. Mayo Clinic Proceedings, 81, 353-373. http://dx.doi.org/10.4065/81.3.353
- Chapuy, M.C., Preziosi, P., Maamer, M., et al. (1997) Prevalence of vitamin D insufficiency in an adult normal population. Osteoporosis International, 7, 439-443. http://dx.doi.org/10.1007/s001980050030
- Need, A.G., Horowitz, M., Morris, H.A. and Nordin, B.C. (2000) Vitamin D status: Effects on parathyroid hormone and 1,25-dihydroxyvitamin D in postmenopausal women. The American Journal of Clinical Nutrition, 71, 1577- 1581.
- Leboff, M.S., Kohlmeier, L., Hurwitz, S., et al. (1999) Occult vitamin D deficiency in postmenopausal US women with acute hip fracture. Journal of the American Medical Association, 281, 1505-1511. http://dx.doi.org/10.1001/jama.281.16.1505
- Harris, S.S., Soteriades, E., Coolidge, J.A., et al. (2000) Vitamin D insufficiency and hyperparathyroidism in a low income, multiracial, elderly population. The Journal of Clinical Endocrinology & Metabolism, 85, 4125-4130. http://dx.doi.org/10.1210/jc.85.11.4125
- Lips, P., Duong, T., Oleksik, A., Black, D., et al. (2001) A global study of vitamin D status and parathyroid function in postmenopausal women with osteoporosis: Baseline data from the multiple outcomes of reloxifene evaluation clinical trial. The Journal of Clinical Endocrinology & Metabolism, 86, 1212-1221. http://dx.doi.org/10.1210/jc.86.3.1212
- Bischoff-Ferrari, H.A., Giovannucci, E., Willett, W.C., et al. (2006) Estimation of optimal serum concentrations of 25-hydroxyvitamin D for multiple health outcomes. The American Journal of Clinical Nutrition, 84, 18-28.
- Heaney, R.P., Dowell, M.S., Hale, C.A. and Bendich, A. (2003) Calcium absorption varies within the reference range for serum 25-hydroxyvitamin D. The Journal of the American College of Nutrition, 22, 142-146. http://dx.doi.org/10.1080/07315724.2003.10719287
- Jackson, R.D., LaCroix, A.Z., Gass, M., et al. (2006) Calcium plus vitamin D supplementation and the risk of fractures. The New England Journal of Medicine, 354, 669- 683. http://dx.doi.org/10.1056/NEJMoa055218
- Picard, D., Brown, J., Rosenthall, L., et al. (2004) Ability of peripheral DXA measurement to diagnose osteoporosis as assessed by central DXA measurement. Journal of Clinical Densitometry, 7, 111-118. http://dx.doi.org/10.1385/JCD:7:1:111
NOTES
*Conflict of interest and funding disclosure: The study was self funded. There is no conflict of interest among the authors.

