Open Journal of Rheumatology and Autoimmune Diseases
Vol.3 No.1(2013), Article ID:28171,3 pages DOI:10.4236/ojra.2013.31009
Dystrophic Calcinosis in the Hands of a Patient with Rheumatoid Arthritis and Secundary Sjögren’s Syndrome
![]()
Internal Medicine, Rheumatology, Department of Internal Medicine, Rheumatology Unit, Universidad Nacional de Colombia, Bogotá, Colombia.
Email: *dajaramilloar@unal.edu.co, *kenkorva@yahoo.com.ar, ge_quintana@yahoo.com, federicorondonh@hotmail.com, iglesias.antonio1@gmail.com
Received January 16th, 2013; revised February 16th, 2013; accepted February 24th, 2013
Keywords: Dystrophic Calcinosis; Rheumatoid Arthritis; Sjögren Syndrome
ABSTRACT
Salts of calcium phosphate and inorganic phosphate are normally found in serum and extracellular fluids, balancing through poorly understood factors that prevent abnormal tissue deposition of these minerals. However, in those tissues that are injured, especially due to chronic inflammatory processes, a predisposition to the deposition of these minerals is developed, triggering what has been called Dystrophic Calcinosis (DC), common in different Connective Tissue Diseases (CTD), especially dermatomyositis and scleroderma, but there is no a frecuent association with diseases like Rheumatoid Arthritis (RA) and Sjögren Syndrome (SS). We report a case of a female patient of 63 years old with RA and Secundary SS who presents with DC in the hands and no evidence of other connective tissue.
1. Case Presentation
The patient, who lives in Bogotá—Colombia, diagnosed with early RA at 56’s with 6 months history polyarthritis at the time of consultation and without other significant medical history. During her first visit in June of 2005 she was included in the protocol of early arthritis at the Universidad Nacional de Colombia, where tests was performed: ESR 32 mm/h, CRP 1.0 mg/dL, RF 60.1 U/mL (0 - 30 U/mL, by Nephelometry), ACPA 6.4 (negative), ANA by IIF 1/160 Speckled Pattern, genotype HLADR1 *0301 - *0407, TNF Alpha Polymorphism: −308 G/A.
Initial Sharp Van de Heidje 41/448. RA diagnosis was made and immediately she started to take methotrexate 15 mg/week, folic acid 12 mg/week, prednisolone 7.5 mg/day, with excellent response from clinical and laboratory standpoint. In May of 2009, in a control MCP synovitis was found in 2 - 3 in both hands, x-ray was made, finding periarticular calcification at the PIP, MCP (bilateral) and feet without clinical evidence of Raynaud’s phenomenon, acroosteolisis, muscle weakness, skin compromise (mRSS = 0, no rash), dysphagia or another CTD sign or symptom. She begins at the same time with sicca, with out fever, parotid enlargement, lymphadenopathy or vasculitis. New anti-antibody requested (June 2009) found ANA 1/1280 Nucleolar pattern, SSA/ RO 188.9, SM 5.1, RNP 8.7, RA test IgG 85.2, RA test IgA 120, RA test IgM 625 , ACPA 6.8, Alkaline phosphatasa, PTH, 25 (OH) vit D, Serum Calcium, phosphorrus inorganic, 24 h urine calcium, 24 h urine phosphorrus were all normal; Minor salivar gland biopsy with Chisholm-Mason Class IV, serum protein electrophoresis with polyclonal gamma pathy and video capillaroscopy with a nonspecific pattern of scleroderma, DM o MCTD. Diagnosis of DC associated with RA and secondary SS was made and further clinical and laboratory monitoring was performed. The patient its in clinical remission of RA and without sicca simptoms, the pain secondary to her DC has improved with RA treatment and addition of colchicine (MTX 15 mg/week; prednisone 5 mg QD, folic acid 12 mg/week, colchicine 0.5 mg QD), Figure 1.
2. Discussion
Calcinosis cutis is characterized by the deposition of insoluble calcium salts in the skin and subcutaneous tissue and is the result of local tissue damage, with levels of calcium, phosphorus, vitamin D and normal parathormone. It is classified into 5 groups: dystrophic, tumor, metastatic, idiopathic and iatrogenic [1,2,3].
In Dystrophic Calcinosis, tissue damage predisposes to precipitation of calcium salts at the extra skeletal. Is clearly unknown what factors predispose this local precipitation but could be considered that the calcium/phosphorus ratio is increasing extracellular fluid associated
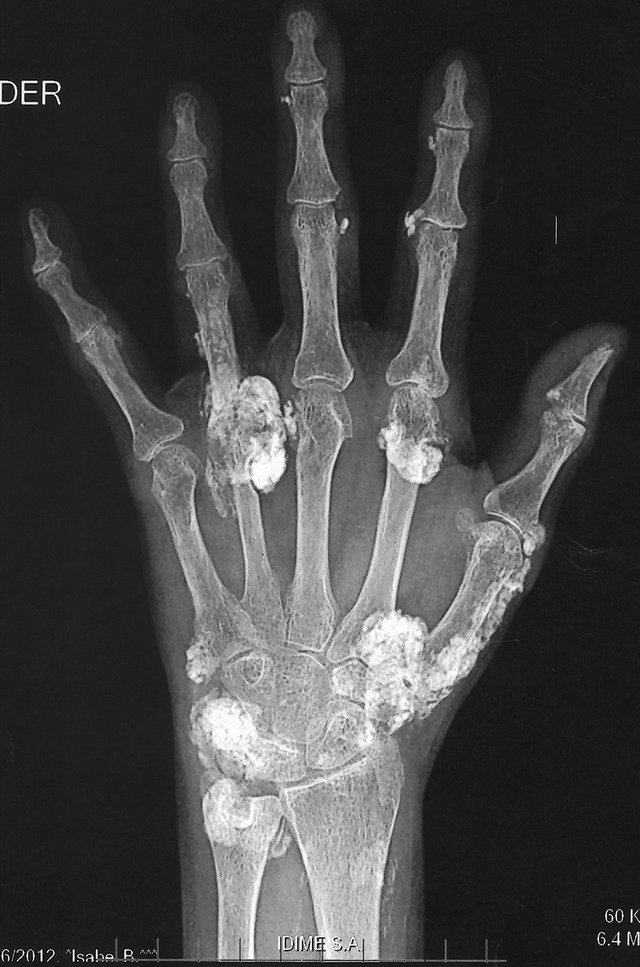
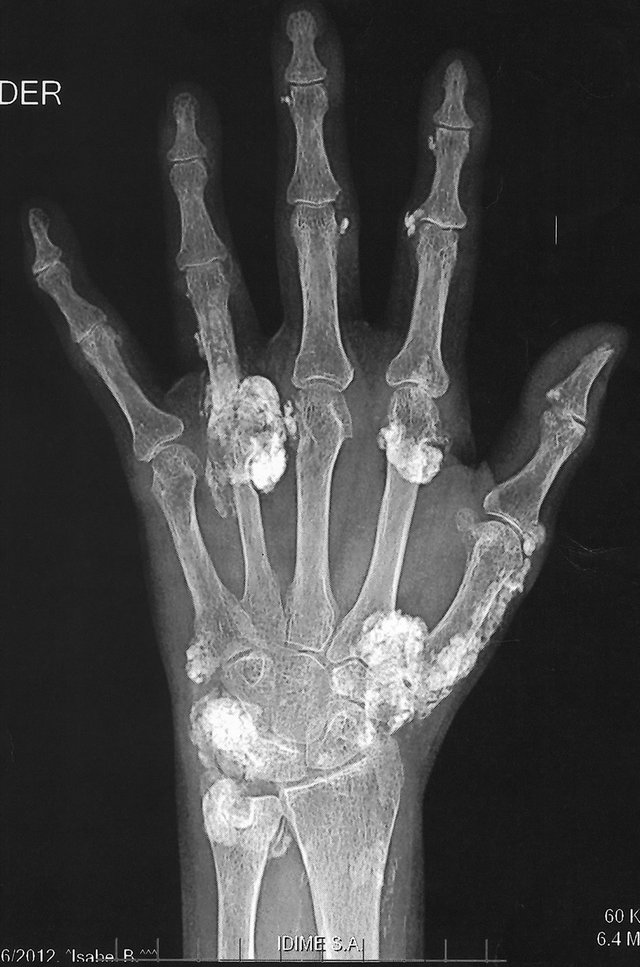
Figure 1. Dystrophic Calcinosis (DC) of the hands associated with RA and SS.
with local inflammatory factors that facilitate the development this illness.
From the pathophysiological point of view the DC occurs in tissues which have somehow had a change that promotes calcification although there is, in theory, a normal level of calcium and phosphorus. Factors that promote calcification have been described and are often found in patients with rheumatic diseases such as hypervascularity with secondary hypoxia, tissue structural damage, and tissue changes associated with age. However, it is important to consider the role of local inflamematory activity specifically mediated by macrophages and cytokines related to this (IL1-β, IL6, TNF-α), which found elevated locally at the site of calcinosis and less frequently in systemic levels (IL1-β) [4]. It has also been shown that at mitochondria level, an unusual increase of calcium salts and phosphate is observed, forming crystal deposits, tissue necrosis, foreign body reactions and fibrosis, generating an acidic microenvironment that interferes with endogenous inhibitors of calcification [3-5].
Other factors that become important for being therapeutic targets are the high levels of Calcium-Binding Amino Acid (CBAA) and the Gamma Carboxy Glutamic Acid (GCGA), modified from the pharmacological point of view by warfarin, with clinical improvement after decreasing its concentration at the site of calcinosis [6].
Dystrophic Calcinosis (DC) is the most common form of calcinosis cutis. This almost always in association with inflammatory diseases such as connective tissue diseases like dermatomyositis, juvenile dermatomyositis, Systemic Sclerosis, Systemic Lupus Erythematosus, mixed connective tissue disease and a lesser extent, with unknown explanation, in polymyositis [4,5]. As for the relationship between DC and RA, their concomitance is extremely rare, to date, there are only two reported cases of DC, both in buttocks [6,7], but no information on these cases involving hands and feet. Also, the association with SS is exotic, with one case reported in the literature [8].
With regard to treatment, there is no drug that has shown strong effectiveness in the management of patients with DC, but some drugs have shown mild pharmacological effects that may help somewhat to control the disease like warfarin, colchicine, probenecid, bisphosphonates, diltiazem, aluminum hydroxide, minocycline, intralesional corticosteroids, surgery and CO2 laser [2,4].
3. Conclusion
In conclusion, we present the first case of DC of the hands and feets in a patient with RA (the third case associated with this disease) simulating articular activity and the second case associated with SS. There are no evidence of another CTD that explains this manifestation. The objective of presenting this case is to inform the association described as an unusually rare even more mimicking RA activity and that despite the medical knowledge, we have not been able to figure out the pathogenesis or the treatment of DC.
REFERENCES
- N. Reiter, L. El-Shabrawi, et al., “Calcinosis Cutis: Part I. Diagnostic Pathway,” Journal of the American Academy of Dermatology, Vol. 65, No. 1, 2011, pp. 1-12. doi:10.1016/j.jaad.2010.08.038
- N. Reiter, L. El-Shabrawi, B. Leinweber, A. Berghold and E. Aberer, “Calcinosis Cutis, Part II: Treatment Options,” Journal of the American Academy of Dermatology, Vol. 65, No. 1, 2011, pp. 15-24. doi:10.1016/j.jaad.2010.08.039
- J. S. Walsh and J. A. Fairley, “Calcifying Disorders of the Skin,” Journal of the American Academy of Dermatology, Vol. 33, No. 5, 1995, pp. 693-710. doi:10.1016/0190-9622(95)91803-5
- N. Boulman, G. Slobodin, M. Rozenbaum and I. Rosner, “Calcinosis in Rheumatic Diseases,” Seminars in Arthritis and Rheumatism, Vol. 34, No. 6, 2005, pp. 805-812. doi:10.1016/j.semarthrit.2005.01.016
- S. Y. Kim, H. Y. Choi, K. B. Myung and Y. W. Choi, “The Expression of Molecular Mediators in the Idiopathic Cutaneous Calcification and Ossification,” Journal of Cutaneous Pathology, Vol. 35, No. 9, 2008, pp. 826-831. doi:10.1111/j.1600-0560.2007.00904.x
- K. Harigane, Y. Mochida, K. Ishii, S. Ono, N. Mitsugi and T. Saito, “Dystrophic Calcinosis in a Patient with Rheumatoid Arthritis,” Modern Rheumatology, Vol. 21, No. 1, 2011, pp. 85-88. doi:10.1007/s10165-010-0344-0
- S. Balin, D. Wetter, L. Andersen and M. Davis, “Calcinosis Cutis Occurring in Association with Autoimmune Connective Tissue Disease the Mayo Clinic Experience with 78 Patients, 1996-2009,” Archives of Dermatology, Vol. 148, No. 4, 2011, pp. 455-462.
- M. Llamas-Velasco, C. Eguren, D. Santiago, C. GasrcíaGarcía, J. Fraga and A. García-Diez, “Calcinosis Cutis and Sjögren’s Syndorme,” Lupus, Vol. 19, No. 6, 2010, pp. 762-764.
NOTES
*Corresponding author.

