Paper Menu >>
Journal Menu >>
 Journal of Behavioral and Brain Science, 2011, 1, 167-171 doi:10.4236/jbbs.2011.13022 Published Online August 2011 (http://www.SciRP.org/journal/jbbs) Copyright © 2011 SciRes. JBBS Effect of Aripiprazole on Methamphetamine-Induced Disruption of Latent Inhibition in Rats Hisae Matsuo1, Hiroshi Abe1*, Tetsuya Ikeda2, Kosuke Ebihara1, Ryuichiro Takeda1, Toshikazu Nishimori2, Yasushi Ishida1 1Department of Psychiatry, Faculty of Medicine, University of Miyazaki, Miyazaki, Japan 2Division of Neuro biology, Faculty of Medicine, University of Miyazaki, Miyazaki, Japan E-mail: *abehiro@med.miyazaki-u.ac.jp Received June 23, 20 1 1; revised July 19, 2011; accepted August 2, 2011 Abstract Objectives: To elucidate the pharmacological profile of aripiprazole, we examined its ameliorating effect on the methamphetamine-induced disruption of latent inhibition (LI) in rats. Method: The effect was measured using a conditioned emotional response procedure. The conditioned stimulus was a tone (2.8 kHz, 90 dB), and the unconditioned stimulus was a mild foot shock delivered through a floor grid. The conditioning pro- cedure was repeated five times. Results: Methamphetamine-induced (1.0 mg/kg, i.p.) disruption of LI was ameliorated by the administration of haloperidol (0.2 mg/kg, i.p.) and by a moderate dose of aripiprazole (0.3 mg/kg, i.p.) but not by a lower or higher dose (0.1 or 3.0 mg/kg, i.p.) of aripiprazole. However, immunohis- tochemical examination showed increased levels of c-Fos expression in the shell of the nucleus accumbens after the administration of haloperidol (0.2 mg/kg, i.p.) but not of aripiprazole (0.3 mg/kg, i.p.). Conclusions: It is suggested that aripiprazole has an ameliorating effect on methamphetamine-induced disruption of latent inhibition within only a marginal therapeutic window. Keywords: Aripiprazole, Haloperidol, Latent Inhibition, c-Fos, Immunohistochemistry, Schizophrenia 1. Introduction The present study aimed to characterize the psychophar- macological profile of aripiprazole, 7-(4-[4-(2,3-dichloro- phenyl)-1-piperazinyl]butyloxy)-3,4-dihydrocar-bos- tycil, by examining its ameliorating effect on metham- phetamine-induced disruption of latent inhibition (LI) in rats, an animal model of the cognitive impairments seen in schizophrenia [1]. LI is typically measured in classical fear conditioning. That is, if a conditioned stimulus is presented several times without an unconditioned stimu- lus before conditioning, the animal learns to ignore, or not to pay attention to, the stimulus, and, consequently, the strength of the subsequent conditioning is inhibited [2]. This phenomenon is thought to relate to “attentional filtering mechanism”, which enables us to distinguish significant stimuli from irrelevant stimuli, and is known to be disrupted in patients with schizophrenia [1]. LI is also disrupted by the injection of the dopamine releasers, amphetamine and methamphetamine, in humans and ro- dents, and such disruption is ameliorated by typical and atypical antipsychotic drugs (APDs) [3-6]. Th erefor e, the psychopharmacological profiles of novel APDs can be characterized by examining their ameliorating effect on amphetamine- or methamphetamine-induced disruption of LI. Aripiprazole, is a novel atypical APD that has been re- ported to have high affinity for dopamine D2, and it acts as a partial dopamine D2 receptor agonist [7]. These pharmaco- logical profiles play a central role in the therapeutic effects of aripiprazo le on schizophrenia. Although aripiprazole h as been reported to enhance some cognitive functions in schi- zophrenia [8] and so me animal model of schizophrenia [9], its effect on disrupted LI has not been examined. It has been suggested that the remedial effects of APDs on disrupted LI are related to some neural substrates, in which the nucleus accumbens would play a key role [1]. However, no in-dep th mor pholog ical study has been con- ducted, and, therefore, we examined the c-Fos expr ession in brain areas related to LI. 2. Materials and Methods Seventy-five adult male Sprague-Dawley rats (Charles  H. MATSUO ET AL. Copyright © 2011 SciRes. JBBS 168 River Laboratories, Japan), weighing 260 - 290 g, were used. They were housed in a temperature-controlled col- ony room (23˚C ± 1˚C) on a 12:12 h light:dark cycle. Water availability was restricted, as described below, while food was available ad libitum. The experimental procedures were approved by the ethical committee of animal experimentation at the University of Miyazaki. LI was assessed using an off-baseline conditioned emo- tional response procedure in rats licking for water. The test chamber was 24.0 cm long, 29.0 cm wide, and 25.0 cm high (Ohara Ika Sangyo, Tokyo, Japan) with a re- tractable water bottle and a speaker. The entire chamber was placed in a soundproof box. Licks were detected with a drinkometer (Ohara Ika), and the data were cap- tured using a prog ram written in LabVIEW (National In- struments Co., Tokyo, Japan). After being handled for 5 min, a rat was placed in the experimental chamber for 5 min on four consecutive days. For the next five consecutive days, rats were water re- stricted overnight, then placed in the chamber and al- lowed to take water freely for 15 min by licking the tip of the water bottle. Rats were given free access to water for 1 h after training at which time water was again re- moved. The LI indexing procedure was conducted on days 10 - 13 and consisted of four sessions, with a 24 h break between them. 1) In the preexposure session, the rats in the preexposed group (PE) received 20 tone pres- entations (2.8 kHz, 90 dB, 10 s) with an interstimulus interval of 50 s without the water bottle. The rats in the non-preexposed group (NPE) were placed in the chamber for the same period of time without being exposed to the tone. 2) In the conditioning session, without the water bottle, the conditioned stimulus (tone, 2.8 kHz, 90 dB, 10 s) was immediately followed by an unconditioned stimu- lus (0.5 mA, 1.0 s, foot shock via floor grid). The first pairing was given 5 min after the start of the session, and the pairings were given 5 times with an interpairng inter- val of 5 min. 3) In the retraining session, the rats took wa- ter freely for 15 min by licking the tip of the water bottle as in the initial training. 4) In the test session, which was conducted in the behavioral experiment (experiment 1) but not in the immunohistochemical experiment (experiment 2), the rats took water freely from the tip of the water bot- tle in the test chamber. When the number of licks reached 300, the conditioned stimulus (2.8 kHz, 90 dB, tone) was continuously presented until the rats completed 1000 licks. The time taken to complete licks 150 - 250 (period A) and 302 - 402 (period B) was measured. The suppression ratio was defined as B/ (A + B). 2.1. Drugs Aripiprazole was supplied by Otsuka Pharmaceutical Co., Ltd., Tokyo, Japan as a bulk powder. Aripiprazole (50 mg) was dissolved in 99.5% N,N- dimethylformamide (Nacalai Tesque, Inc., Kyoto, Japan, 2.0 ml) and 0.1 M citrate buffer (8.0 ml) to make a stock solution with a pH between 4.5 and 5.0. Dilutions were made with saline to make 0.1, 0.3, and 3.0 mg/ml aripip- razole. Haloperidol (Dainippon Sumitomo Pharmaceuti- cal Co., Ltd., Tokyo, Japan, 5 mg/ml) was diluted with saline to make 0.2 mg/ml haloperidol, and bulk powder of methamphetamine (Dainippon Sumitomo) was diluted with saline to make 1.0 mg/ml methamphetamine. 2.2. Experiment 1 In experiment 1, the effect of 0.2 mg/kg haloperidol and 0.1, 0.3, and 3.0 mg/kg aripiprazole on methampheta- mine-induced (1.0 mg/kg) disruption of LI was examined. Sixty rats were randomly assigned to twelve experimen- tal groups. To obtain a standard suppression ratio, we pr e- pared five PE rats and five NPE rats without any drug treatment (naïve group). The remaining fifty rats were assigned to ten methamphetamine-treated groups in a 2 × 5 factorial arrangement with the main factors being pre- exposure (PE, NPE) and drug (saline (SAL), 0.2 mg/kg haloperidol (Hal 0.2), and 0.1, 0.3, 3.0 mg/kg aripipra- zole (Ari 0.1, Ari 0.3, Ari 3.0, respectively)). They were injected with aripiprazole (0.1, 0.3, 3.0 mg/kg, i.p.), haloperidol (0.2 mg/kg, i.p.), or saline (1.0 ml/kg, i.p.) 60 min before the conditioning, and 45 min after these in- jections, methamphetamine was injected (1.0 mg/kg, i.p.). 2.3. Experiment 2 In experiment 2, the expression patterns of c-Fos in the prefrontal cortex (PFC), nucleus accumbens core area (AcbC), nucleus accumbens shell area (AcbSh), and ba- solateral area of the amygdala (BLA) were examined. These patterns could be related to the ameliorating ef- fects of 0.2 mg/kg haloperidol and 0.3 mg/kg aripipra- zole on the methamphetamine-induced disruption of LI in experiment 1. Fifteen PE rats we re randomly assigned to three groups for 1.0 ml/kg saline i.p. injection (SAL), 0.2 mg/kg haloperidol i.p. injection (Hal 0.2), or 0.3 mg/kg aripiprazole i.p. injection (Ari 3.0) 60 min before conditioning. They were also injected with metham- phetamine (1.0 mg/kg, i.p.) 15 min before conditioning. The rats were then deeply anesthetized with sodium pentobarbital 90 min after the end of the conditioning session and perfused transcardially with saline followed by 4% paraformaldehyde in 0.1 M phosphate buffer (PB; pH 7.4). Their brains were removed immediately, post- fixed at 4˚C for 1 h in the above fixative, immersed in  H. MATSUO ET AL. Copyright © 2011 SciRes. JBBS 169 0.1 M PB with 10% sucrose at 4˚C for 1 h, and then cryoprotected at 4˚C overnight in the same buffer with 30% sucrose. The samples were subsequently cut on a freezing microtome into 50 µm coronal sections. An im- munohistochemical examination of c-Fos expression was performed in accordance with the manufacturer’s in- structions on the use of a streptavidin-biotin system (His- tofine SAB-PO(R) kit, Nichirei, Tokyo, Japan). Briefly, biotinylated secondary antibodies were coupled with streptavidin-biotinylated horseradish peroxidase, and the reaction was visualized using diaminobenzidine as a chromogen enhanced by cobalt chloride. Between each incubation step, the free-floating sections were thor- oughly rinsed with phosphate-buffered saline. The anti- bodies for c- Fos (1:5000) were rabb it polyclonal antisera (sc-52; Santa Cruz Biotechnology, CA, USA). Sections through the PFC, AcbC, AcbSh (approximately 1.70 mm rostral to the bregma), and BLA (approximately 2.80 mm caudal to the bregma) were selected (Figure 1) [10]. c-Fos immunoreactivity was analyzed using light mi- croscopy. Four sections were taken through each struc- ture of each animal. They were taken at the same level along the animal’s antero-posterior axis to avoid variance of the level of the structure among the animals. The ex- pression of c-Fos w as quantified by counting th e number of cells immunopositive for c-Fos in 0.25 × 0.25 mm squares using a 20 × microscope objective. c-Fos im- munopositive cells were counted bilaterally and averaged per structur e/animal. 3. Results In experiment 1, the naïve PE group showed a signifi- cantly lower suppression ratio than the naïve NPE group (t-test, p < 0.01) (Figure 2). Two-way ANOVA with main factors of preexposure (PE, NPE) and drug (SAL, Hal 0.2, Ari 0.1, Ari 0.3, Ari 3.0) carried out on the sup- pression ratios yielded the significant main effects of preexposure [F(1,40) = 10.92, p < 0.005], drug [F(4,40) = 5.28, p < 0.005], and their interaction [F(4,40) = 3.38, p < 0.05]. Figure 2 shows the mean suppression ratios of the PE and NPE groups for the five drug treatments. The simple main effect was significant for PE [F(4,40) = 7.77, p < 0.001] but not for NPE. For PE, a post hoc Bon- ferroni test revealed th at the su ppression ratio s of Hal 0.2 and Ari 0.3 were significantly lower than that of SAL (p < 0.01 for both). On the other hand, the simple main effects were sig- nificant for Hal 0.2 [F(1,40) = 8.99, p < 0.01] and Ari 0.3 [F(1,40) = 14.57, p < 0.001] but not for SAL, Ari 0.1, and Ari 3.0. In experiment 2, the number of c-Fo s-immunopositiv e cells counted in the PFC, AcbC, AcbSh, and BLA sec- tions for the animals in the SAL, Hal 0.2, and Ari 0.3 groups, which were all preexposed to the conditioned stimulus (tone), were used for statistical analysis. Two-way ANOVA with main factors of region (PFC, AcbC, AcbSh, BLA) and drug (SAL, Hal 0.2, Ari 0.3) yielded significant main effects of region [F(3,48) = 12.09, p < 0.001] and region x drug interaction [F(6,48) = 4.01, p < 0.005], but not of drug [F(2,48) = 2.55, p < 0.1]. Significant simple main effects were detected for AcbSh (p < 0.001) but not for A cbC (p > 0.1), PFC (p > 0.1), or BLA (p > 0.1). A post hoc Bonferroni test carried out for an AcbSh section revealed that the number of cells in the Hal 0.2 was significantly greater than that in the Ari 0.3 and SAL (p < 0.001 for both) (Table 1). 4. Discussion These results showed that the di sr upt i o n of LI induced by methamphetamine was significantly ameliorated by ad- ministration of haloperidol (0.2 mg/kg) and by a moder- ate dose of aripiprazole (0.3 mg/kg) but not by a relatively low or high dose of aripiprazole (0.1 or 3.0 mg/kg). It has been reported that amphetamine-induced disrup- tion of LI is ameliorated by APDs, olanzapine [3], chlor- promazine [4], haloperidol [5], and clozapine [6]. Even though the receptor binding profiles (D2 and D3 partial agonistic, 5HT1A agonistic, and 5HT2A antagonistic [7, 11]) of aripiprazole differ from those of other APDs, its effect on disrupted LI induced by injection of a dopa- mine-releasing agent was sugg ested to be equivalent. Since lower and higher doses of aripiprazole did not have an ameliorating effect on disrupted LI, simple dose dependency was not confirmed. It is reported that aripip- razole has a functional D2 partial agonist effect at low Table 1. Number of c-Fos-immunopositive cells/0.0625 mm2 in SAL, Hal 0.2, and Ari 0.3 groups. The brain sample was obtained 90 min after conditioning. Animals had preexpo- sure to the conditioned stimulus (tone) one day before con- ditioning. Saline, haloperidol 0.2 mg/kg, or aripiprazole 0.3 mg/kg was injected 60 min before conditioning, and all groups had an injection of methamphetamine 1.0 mg/kg 15 min before conditioning. Group Area SAL Hal 0.2 Ari 0.3 PFC 15.1 ± 1.7 8.9 ± 1.4 12.2 ± 2.8 AcbC 20.7 ± 4.2 24.1 ± 2.8 17.5 ± 2.0 AcbSh 17.2 ± 3.1 33.3 ± 5.9* 16.8 ± 2.0 BLA 13.9 ± 1.4 9.8 ± 1.0 11.9 ± 0.8 Value represents mean number ± SEM. PFC: prefrontal cortex, AcbC: nu- cleus accumbens core area, AcbSh: nucleus accumbens shell area, BLA: basolateral area of amygdala. *Number of c-Fos-positive cells was signifi- cantly higher for Hal 0.2 tha n A ri 0.3 and SAL in Ac bSh ( p < 0.001 for both). 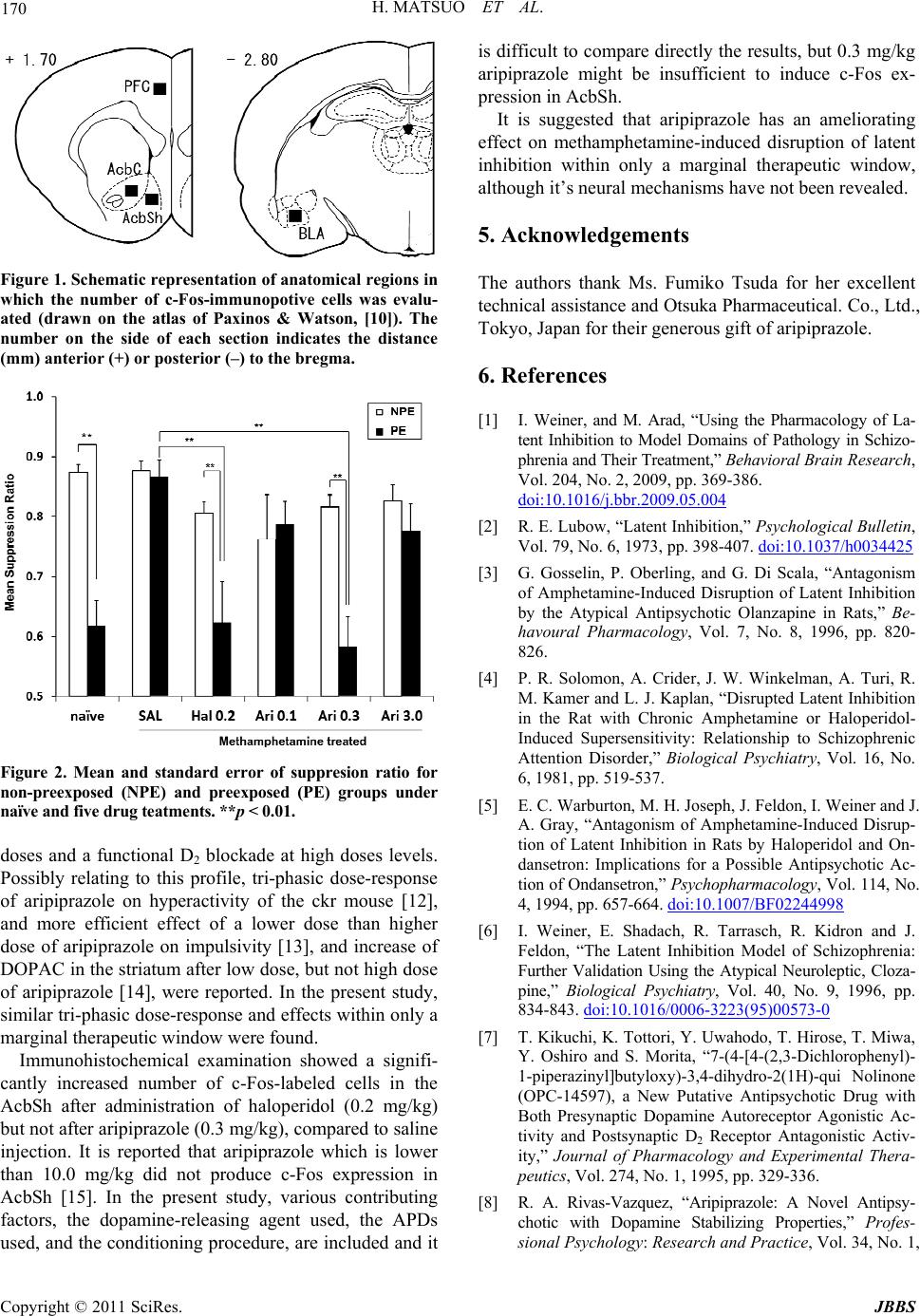 H. MATSUO ET AL. Copyright © 2011 SciRes. JBBS 170 Figure 1. Schematic representation of anatomical regions in which the number of c-Fos-immunopotive cells was evalu- ated (drawn on the atlas of Paxinos & Watson, [10]). The number on the side of each section indicates the distance (mm) anterior (+) or posterior (–) to the bregma. Figure 2. Mean and standard error of suppresion ratio for non-preexposed (NPE) and preexposed (PE) groups under naïve and five drug teatments. **p < 0.01. doses and a functional D2 blockade at high doses levels. Possibly relating to this profile, tri-phasic dose-response of aripiprazole on hyperactivity of the ckr mouse [12], and more efficient effect of a lower dose than higher dose of aripiprazole on impulsivity [13], and increase of DOPAC in the striatum after low dose, but not high dose of aripiprazole [14], were reported. In the present study, similar tri-phasic dose-response and effects within only a marginal therapeutic window were found. Immunohistochemical examination showed a signifi- cantly increased number of c-Fos-labeled cells in the AcbSh after administration of haloperidol (0.2 mg/kg) but not after aripiprazole (0 .3 mg/kg) , compared to saline injection. It is reported that aripiprazole which is lower than 10.0 mg/kg did not produce c-Fos expression in AcbSh [15]. In the present study, various contributing factors, the dopamine-releasing agent used, the APDs used, and the conditioning procedure, are included and it is difficult to compare directly the results, but 0 .3 mg/kg aripiprazole might be insufficient to induce c-Fos ex- pression in AcbSh. It is suggested that aripiprazole has an ameliorating effect on methamphetamine-induced disruption of latent inhibition within only a marginal therapeutic window, although it’s neural mechanisms have not been revealed. 5. Acknowledgements The authors thank Ms. Fumiko Tsuda for her excellent technical assistance and Otsuka Pharmaceutical. Co., Ltd., Tokyo, Japan for their generous gift of aripiprazole. 6. References [1] I. Weiner, and M. Arad, “Using the Pharmacology of La- tent Inhibition to Model Domains of Pathology in Schizo- phrenia and Their Treatment,” Behavioral Brain Research, Vol. 204, No. 2, 2009, pp. 369-386. Hdoi:10.1016/j.bbr.2009.05.004 [2] R. E. Lubow, “Latent Inhibition,” Psychological Bulletin, Vol. 79, No. 6, 1973, pp. 398-407. Hdoi:10.1037/h0034425 [3] G. Gosselin, P. Oberling, and G. Di Scala, “Antagonism of Amphetamine-Induced Disruption of Latent Inhibition by the Atypical Antipsychotic Olanzapine in Rats,” Be- havoural Pharmacology, Vol. 7, No. 8, 1996, pp. 820- 826. [4] P. R. Solomon, A. Crider, J. W. Winkelman, A. Turi, R. M. Kamer and L. J. Kaplan, “Disrupted Latent Inhibition in the Rat with Chronic Amphetamine or Haloperidol- Induced Supersensitivity: Relationship to Schizophrenic Attention Disorder,” Biological Psychiatry, Vol. 16, No. 6, 1981, pp. 519-537. [5] E. C. Warburton, M. H. Joseph, J. Feldon, I. Weiner and J. A. Gray, “Antagonism of Amphetamine-Induced Disrup- tion of Latent Inhibition in Rats by Haloperidol and On- dansetron: Implications for a Possible Antipsychotic Ac- tion of Ondansetron,” Psychopharmacology, Vol. 114, No. 4, 1994, pp. 657-664. Hdoi:10.1007/BF02244998 [6] I. Weiner, E. Shadach, R. Tarrasch, R. Kidron and J. Feldon, “The Latent Inhibition Model of Schizophrenia: Further Validation Using the Atypical Neuroleptic, Cloza- pine,” Biological Psychiatry, Vol. 40, No. 9, 1996, pp. 834-843. Hdoi:10.1016/0006-3223(95)00573-0 [7] T. Kikuchi, K. Tottori, Y. Uwahodo, T. Hirose, T. Miwa, Y. Oshiro and S. Morita, “7-(4-[4-(2,3-Dichlorophenyl)- 1-piperazinyl]butyloxy)-3,4-dihydro-2(1H)-qui Nolinone (OPC-14597), a New Putative Antipsychotic Drug with Both Presynaptic Dopamine Autoreceptor Agonistic Ac- tivity and Postsynaptic D2 Receptor Antagonistic Activ- ity,” Journal of Pharmacology and Experimental Thera- peutics, Vol. 274, No. 1, 1995, pp. 329-336. [8] R. A. Rivas-Vazquez, “Aripiprazole: A Novel Antipsy- chotic with Dopamine Stabilizing Properties,” Profes- sional Psychology: Research and Practice, Vol. 34, No. 1,  H. MATSUO ET AL. Copyright © 2011 SciRes. JBBS 171 2003, pp. 108-111. Hdoi:10.1037/0735-7028.34.1.108 [9] S. Nakai, T. Hirose, T. Mori, A. Stark, H. Araki and T. Kikuchi, “The Effect of Aripiprazole on Prepulse Inhibi- tion of the Startle Response in Normal and Hyperdopa- minergic States in Rats,” International Journal of Neuro- science, Vol. 118, No. 1, 2008, pp. 39-57. [10] G. Paxinos and C. Watson, “The Rat Brain in Stereotaxic Coordinates,” Academic Press, San Diego, 1998. [11] B. Green, “Focus on Aripiprazole,” Current Medical Re- search and Opinion, Vol. 20, No. 2, 2004, pp. 207-213. Hdoi:10.1185/030079903125002919 [12] G. S. Dawe, R. Nagarajah, R. Albert, D. E. Casey, K. W. Gross and A. K. Ratty, “Antipsychotic Drugs Dose- Dependently Suppress the Spontaneous Hyperactivity of the Chakragati Mouse,” Neuroscience, Vol. 171, No. 1, 2010, pp. 162-172. Hdoi:10.1016/j.neuroscience.2010.08.061 [13] M. Carli, E. Calcagno, P. Mainolfi, E. Mainini and R. W. Invernizzi, “Effects of Aripiprazole, Olanzapine, and Haloperidol in a Model of Cognitive Deficit of Schizo- phrenia in Rats: Relationship with Glutamate Release in the Medial Prefrontal Cortex,” Psychopharmacology, Vol. 214, No. 3, 2010, pp. 639-652. Hdoi:10.1007/s00213-010-2065-7 [14] S. Nakai, T. Hirose, Y. Uwahodo, T. Imaoka, H. Okazaki, T. Miwa, M. Nakai, S. Yamada, B. Dunn, K. D. Burris, P. B. Molinoff, K. Tottori, C. A. Altar and T. Kikuchi, “Di- minished Catalepsy and Dopamine Metabolism Distin- guish Aripiprazole from Haloperidol or Risperidone,” European Journal of Pharmacology, Vol. 472, No. 1-2, 2003, pp. 89-97. Hdoi:10.1016/S0014-2999(03)01857-0 [15] S. Natesan, G. E. Reckless, J. N. Nobrega, P. J. Fletcher and S. Kapur, “Dissociation between in Vivo Occupancy and Functional Antagonism of Dopamine D2 Receptors: Comparing Aripiprazole to Other Antipsychotics in Ani- mal Models,” Neuropsychopharmacology, Vol. 31, No. 9, 2006, pp. 1854-1863. Hdoi:10.1038/sj.npp.1300983 |

