Journal of Biomaterials and Nanobiotechnology
Vol.3 No.1(2012), Article ID:16701,11 pages DOI:10.4236/jbnb.2012.31007
Multidrug Delivery Systems with Single Formulation
——Current Status and Future Perspective
![]()
Division of Biomolecular Chemistry, Institute for Materials Chemistry and Engineering, Kyushu University, Fukuoka, Japan.
Email: *kidoaki@ms.ifoc.kyushu-u.ac.jp
Received October 22nd, 2011; revised November 29th, 2011; accepted December 12th, 2011
Keywords: Multidrug Delivery System; Single Formulation; Combination Therapy; Biochemical Modulation
ABSTRACT
Development of new way and system for multidrug delivery has recently attracted much attention and became one of major issue in drug delivery research. Although this research field is still immature compared to the single drug delivery system, intensive efforts have recently been devoted by researchers in order to realize more efficient, functional, and safe combination therapy using multiple drugs or agents. In this review article, we outline several targets in terms of application for biochemical modulation together with various concrete attempts of simultaneous and sequential delivery of multiple drugs or agents with single formulation. Finally, we will also summarize the possible contribution of biomaterial sciences and nanobiotechnology for improvement of future multidrug delivery system.
1. Introduction
Almost all diseases, especially intractable diseases such as cancer and human immunodeficiency virus infection, cannot cure by treatment with only one type of drug because of pathological complexity. The combinatorial use of multiple drugs having different pharmaceutical action mechanism often redound to better outcome compared with monochemotherapy, because the combination of adequately selected drugs might bring the synergistic or additive effects at lower dose. Furthermore, the low dose combination therapy may concurrently lead to suppression of severe adverse effect. Therefore, the combination therapy by multiple drug treatment has been commonly used in clinical chemotherapy.
Biochemical modulation (BCM) is defined as one of a methodology of combination therapy that aimed to enhance pharmacological effect and/or suppress serious side effect by taking advantage of modulator drug(s) to modifying pharmacokinetics of effector (main) drug [1,2]. In the BCM-based chemotherapy, the drugs are administered sequentially or simultaneously according to action mechanism of individual drugs. Since Bertino et al. reported in 1977 [3], the theory of BCM has attracted much attention especially in clinical medication and now constructed a part of basis of current cancer chemotherapy. To date, several regimens have been developed and applied to clinical cancer chemotherapy by improving drug combination, administration dose, order, timing, and so on (Table 1). Refinement of BCM regimens has surely yielded better outcome of chemotherapy. Since most of regimens, however, need temporally controlled bolus injection, infusion, and continuous infusion, the patients are forced to restrain to the bedside for a long time. Therefore, the development of multi drug delivery systems (M DDSs) with single formulation that matched for BCM regimens has been expected.
The development of nanotechnology and subsequent fusion with biotechnology, i.e., the emergence of nanobiotechnology, has made significant impact on life science, especially medical and pharmaceutical sciences. In addition to development of nanobiotechnology, the rapid advances in materials science also contributes to improvement of quality of medicine. Although the excellent drugs often have some inconvenient natures and/or characters, such as low solubility, unfavorable biodistribution, and serious side effect, in return for its therapeutic potential, several drug delivery systems (DDSs) based on approaches in nanobiotechnology, such as liposomes [8], polymeric micelles [9,10], polymer particulate [11], and so on, have been developed so far. Some DDS formulations have already been reached to the market [12-15], and consequently the established DDSs, especially for cancer chemotherapy, have successfully improved not only therapeutic outcome of conventional drugs but also the patient’s quality of life.
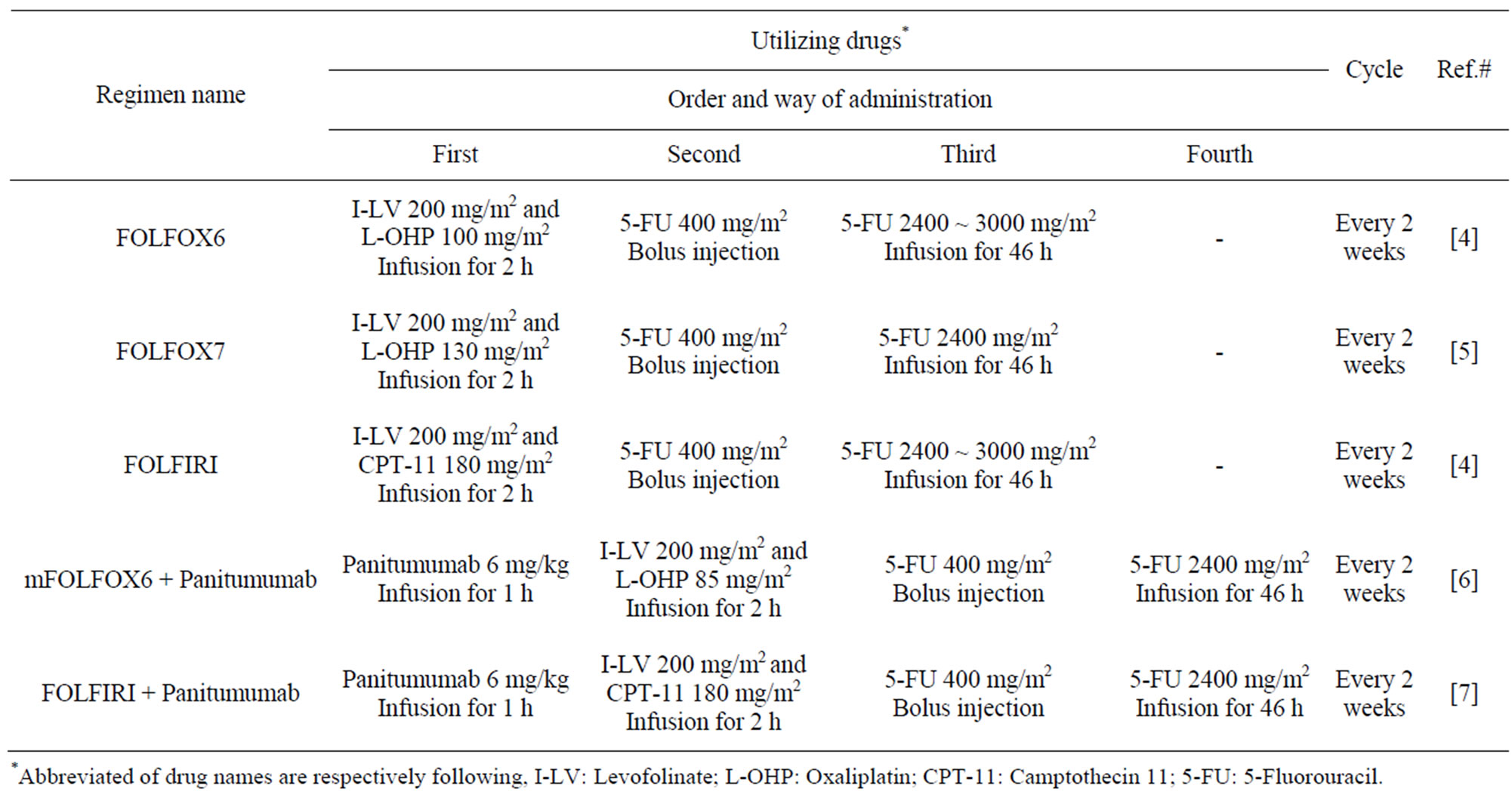
Table 1. Representative BCM based regimens for clinical cancer chemotherapy.
Although more functional and smart DDSs have been reported with recent remarkable advance of nanobiotechnology, the development of the MDDSs that are suitable for controlling of pharmacokinetics of multiple drugs have been still insufficient compared to DDSs for single drug delivery. Therefore, development of new modes and systems, which can effectively and functionally regulate release profiles of multiple drugs from a single formulation, is now important issue with significant interest in current and future DDS research. In past decade, many researchers have made huge effort to develop MDDS, and consequently various MDDSs, which can adopt for combination therapy, have been established. These attempts have been well summarized in some previous review articles that are described based on the types of formulation [16-18]. Meanwhile, we will especially focus on the MD DSs related to biochemical modulation (BCM), and review the recent attempts from this point of view in this article. The concrete examples of MDDS that can simultaneously deliver multiple agents will be respectively introduced according to individual applications (Section 2). Several approaches for development of sequential multiple agent delivery from single formulation are shown in Section 3. Finally, some future perspectives and conclusions will given in Section 4.
2. Applications of MDDS for BCM-Based Chemotherapies
2.1. Serious Side-Effect Reduction
Anticancer drugs often have intolerable side effects, such as cardiotoxicity, myelosuppression, and gastrointestinal dysfunction. Although anticancer drugs bring enough therapeutic efficiency, there are many cases in which administration of anticancer drug is forced to withdraw due to serious adverse effect. For instance, doxorubicin (DOX) that is one of the most effective and widely used anticancer drugs has crucial cardiotoxicity. Current major strategies to prevent heart injury caused by this drug are encapsulation of DOX into carrier molecules, such as poly (ethylene glycol) (PEG) modified liposome and polymeric micelles, or covalent conjugation to biocompatible polymer. These approaches have succeeded in suppression of side effect and enhancement of therapeutic outcome, however, it seems that more active approach against drug-induced cardiomyopathy is needed for more safe and efficient cancer chemotherapy.
Santucci et al. have developed simultaneous anticancer drug epirubicin (EPI) and nitric oxide (NO) carrying system (EPI-PEG-NO), in which NO (NO releasable moiety, butandiol mononitrate) and EPI were covalently conjugated to each terminal of PEG [19]. In their system, NO act as not only protecting reagent against anthracyclineinduced cardiomyopathy but also sensitizer of anticancer drug treatment. In order to increase anticancer efficacy and enhance cardiocyte-protecting ability of EPI-PEGNO system, the improved system used branched PEG as polymer backbone instead of linear one has been developed. The newly constructed PEG conjugates have one EPI and four or eight NO releasable moieties (EPI-bPEG- (NO)4, EPI-bPEG-(NO)8) [20]. The ternary conjugate showed higher anticancer activity for carcinoma cells (Caco-2), whereas it decreased cytotoxicity against endothelial cells and cardiomyocytes, with respect to free EPI treatment.
2.2. Modulation of Cancer Surviving Mechanism
A better understanding of cancer pathophysiology is very important on planning of chemotherapy. Mutated molecules and upor down-regulated molecules in cancer cells compared with normal cells must be good target of medication. Recently, several researches focused on these molecules as target of therapy have been actively progressed.
It is well known that the tumor suppressor gene, p53, is mutated in a wide variety of human cancer cells. The translational product of p53 gene plays an important role as a transcription factor. There are many target genes related to cell cycle arrest, senescence, and apoptosis, under the regulation of p53. Since the p53 protects cells from several damages by regulating programmed cell death mechanism in the downstream of p53 pathway, the mutation of p53 promotes the surviving of cancer cells. Therefore, it is expected that the recovery of p53 function lead to better outcome of cancer therapy. Wu et al. have reported that chemosensitivity of cancer against several anticancer drugs, such as DOX, cisplatin, paclitaxel (PTX), and mytomycin C, have been enhanced by adenoviral transfection of wild-type p53 gene [21]. Wiradharma et al. have developed the MDDS focused on this p53 mediated chemosensitizing mechanism [22]. In their co-delivery system of DOX and p53-encoding plasmid DNA (pDNA), the three blocks oligopeptide, Ac-(AF)6-H5-K15-NH2 (FA32), which can simultaneously assemble and form surface cationic core-shell structure at above the critical micelle concentration, was used as carrier molecule. DOX was encapsulated into hydrophobic core and p53-encoding pDNA was complexed with cationic surface of FA32 via electrostatic interaction. The synergistic effect on suppression of Hep-G2 cell proliferation was observed by co-delivery of DOX and p53- encoding pDNA using FA32, whereas no synergism was observed by individual treatment of free DOX and FA32/p53-encoding pDNA complex.
Survivin is an unique apoptosis suppressor molecule, which suppress the programmed cell death by inhibit caspase family in several cell types [23,24]. Since survivin molecules are expressed in almost of all major cancer cells whereas are not expressed in other differentiated cells [25], it is one of another good target molecule on tumor chemotherapy. To date, many attempts have been made to offset survivin function in cancer cells by dominant-negative mutant, antisense oligonucleotide (ASO), RNA interference, and so on. Recently, two successful examples of MDDS, in which abolishment of survivin function and anticancer drug treatment are combined, have been reported. Xiao et al. have constructed the liposomal co-delivery system of anticancer drug DOX and dominant negative survivin mutant (Msurvivin T34A)-encoding pDNA [26]. This survivin mutant has antiproliferative potential and caspase-dependent apoptosis induction ability for tumor cells. In this system, DOX was loaded into internal aqueous phase of truncated bFGF peptide-modified cationic liposome taking advantage of pH gradient remote loading method, and then Msurvivin T34A-encoding pDNA was complexed with DOX-loaded cationic liposome via electrostatic interaction. This MDDS has achieved dose reduction of DOX to 3-fold lower level compared to free DOX treatment in vitro. Furthermore, significant tumor growth suppression effect was observed in the Lewis lung carcinoma-bearing C57BL/6 mice by co-delivery of DOX and Msurvivin T34A-encoding pDNA compared to liposomal DOX or lipoplex alone. Another example of MDDS related to the combination of anticancer drug treatment and survivin counteraction has been reported from Xu et al [27]. In this system, the survivin-targeted RNAi encoding pDNA (iSur-pDNA)/protamine complexes and DCTX were encapsulated by folate-modified lipid-based envelope via the lipid film hydration technique. This newly constructed formulation showed lower cytotoxicity compared to commercially available liposomal transfection reagent and enhanced internalizing ability due to folatemodification. As the result of in vitro cytotoxicity evaluation against for hepatocellular carcinoma cell line BEL 7402, the MDDS showed much higher cytotoxicity than the single treatment by DCTX or iSur-pDNA monoloaded folate-modified lipid-based envelope. In addition, the cytotoxicity provided by co-delivery of DCTX and iSur-pDNA using the MDDS was also higher than the combination of free DCTX and iSur-pDNA mono-loaded folate-modified lipid-based envelope. These results suggest that the simultaneous delivery (i.e., the MDDS) is more effective on the combination of cancer chemotherapy and survivin targeted therapy.
2.3. Tumor Starving Therapy
The tumor growth and angiogenesis are closely related to each other. The primary tumors and metastatic tumors upregulate angiogenesis by secreting of several angiogenesis related factors, such as vascular endothelial growth factor (VEGF), matrix metalloproteases (MMPs), and so on, and acquire nutrition needed for own growth from the induced neovessels. If suppression of the tumor-induced angiogenesis and/or disruption of neovessels that provide nutrition to tumor can be achieved, tumor growth inhibition therapy will be realized. The angiogenesis-targeted cancer therapy is especially called as “Tumor starving therapy”, because nutrition supply to tumor is blocked by suppression of angiogenesis or disruption of neovasculature.
Combrestatin A4 (CA4) is dephosphorylated form of combrestatin A4 phophate, which is natural product isolated from the South African tree Combretum caffrum. CA4 acts as tubulin inhibitor in endothelial cells, and consequently induce neovascularture disruption. Owing to its ability, CA4 gets much attention as antivasculature (vascular disrupting) agents. Even though the single CA4 treatment shows some promising results in clinical trial, it is expected that the combination of CA4 and another drug(s) will redound superior therapeutic outcome [28].
Some groups have developed the MDDS aimed for co-delivery of CA4 and anticancer drug [29-31]. Wang et al. have developed the MDDS, which can co-deliver CA4 and PTX [30]. In their system, nanocapsule that consists of mPEG2000-PLA2000 block copolymer was used as carrier molecule. PTX was covalently conjugated to the terminal of PLA side via ester bond, and then CA4 was encapsulated into hydrophobic core during nanocapsules formation. In the in vivo Matrigel plug assay, the dual loaded nanocapsule showed significant antiangiogenesis effect compared to treatment with single drug loaded nanocapsule. Moreover, in the Lewis lung carcinoma tumorbearing mice, the most significant tumor growth suppression effect was observed by dual drug loaded nanocapsule treatment. The improved co-delivery system of CA4 and DOX has been reported from Yang et al. [31]. The cyclic pentapeptide, cyclic arginine-glycine-aspartic acidtyrosine-lysine (cRGDyK), which is well known as recognition motif for integrins, was conjugated to the PEGside terminal of PEG-b-PLA block copolymer. Since expression of integrins, especially αvβ3 and αvβ5, are upregulating in sprouting neovasculature as well as various cancer cells, the targeting ability to angiogenic endothelial cells and tumor have provided to this system by introducing RGD motif (cRGDyK). The cRGDyK-modified nanomicelle system, in which DOX and CA4 were loaded by chemical conjugation and simultaneous encapsulation, respectively, showed significantly enhanced uptake of the drugs by cancer and endothelial cells via receptor-mediated endocytosis. Furthermore, in the in vivo experiment, this cRGDyk-modified and dual-loaded system achieved superior tumor growth inhibition, antineovasculature, and apoptosis induction compared to each single-drug loaded nanomicelles.
TNP-470 is a synthetic analogue of fumagillin with potent antiangiogenic ability [32]. Although TNP-470 has strong potency as anticancer drug, the use of TNP-470 is limited due to its dose limiting neurotoxicity. Since serious adverse effect of TNP-470 is ascribed to its unfavorable biodistribution characteristic and low solubility, the improvement of bioavailability has been achieved by conjugation to highly biocompatible N-(2-hydroxypropyl)methacrylamide (HPMA) copolymer [33]. In order to acquire further therapeutic outcome, Segal et al. have constructed the MDDS based on the HPMA-TNP-470 conjugate [34]. In this work, both alendronate (ALN) and TNP-470 were covalently conjugated to HPMA copolymer via short peptide linker (Gly-Gly-Pro-Nle), which can be cleaved by cathepsin K specifically overexpressed in bone tissue. The drug ALN has not only bone targeting ability but also antitumor activity and antiangiogenic potential. Thus this co-delivery system utilizing HPMA copolymer-ALN-TNP-470 conjugate exerted passive/activetargeting ability and synergistic antineovasculature and anticancer activity in vivo. The HPMA copolymer-ALNTNP-470 conjugate remarkably suppressed MG-63-ras human osteosarcoma growth in xenograft mice by 96%, whereas the only 45% growth inhibition was observed by combination treatment of free drugs. Simultaneously, immunohistochemistry revealed 74% reduction of neovascularization in mice treated with HPMA copolymerALNTNP-470 conjugate, meanwhile the dual treatment with free drugs showed only 39% reduction.
VEGF is one of glycoproteins, which is related to vasculogenesis and angiogenesis. VEGF binds to vascular endothelial cells via specific VEGF receptor on cell surface, and induces cell mitosis, migration, and differentiation. Since many cancer cells are upregulating the production and secretion of VEGF for own survival and growth, suppression of the VEGF expression in tumor cells and overriding of the secreted VEGF will be good strategies for cancer therapy. In several clinical trials, addition of VEGF specific monoclonal antibody (Avastin), which can void VEGF function, to pre-existing combination chemotherapy has lead to better outcome.
As far as the MDDS for VEGF targeted combination therapy is concerned, the combination between conventional anticancer drug treatment and knock down of VEGF production by RNAi has been attempted [35,36]. For instance, Huang et al. have developed the MDDS of DOX and VEGF targeted siRNA by using cationic polymer micelle that consists of stearic acid-grafted polyethyleneimine (PEI-SA) [36]. Since the carrier molecule PEISA can spontaneously form micelle structure having hydrophobic core and cationic hydrophilic shell, hydrophobic PTX was encapsulated into core region and then and anionic siRNA was complexed with cationic PEI-SA polymer micelle via electrostatic interaction. In the in vitro experiment, dual-loaded PEI-SA micelles treatment showed significant reduction of VEGF production in Hep G-2 (human hepatocellular carcinoma) cells. At day 30 of postintratumoral administration, remarkable tumor growth suppression (13.0% of control) by simultaneous delivery of DOX and VEGF targeted siRNA using PEI-SA micelles was observed, whereas siRNA or DOX single loaded PEISA micelles treatment displayed slightly lower effect (33.7% and 56.7% of control, respectively).
2.4. Multidrug Resistance Reversal of Cancer
Multidrug resistance (MDR) of malignant neoplasm is the survival ability of cancer cells under the treatment with structurally and functionally diverse anticancer drugs. Since MDR is a major obstacle in clinical cancer chemotherapy, establishment of treatment strategies to overcome the cancer MDR is now becoming the great issue to be resolved for success of tumor therapy. The underlying mechanism of cancer MDR has been intensively researched and revealed to date. MDR phenotype in various type of cancer is frequently associated with upregulation of the permeability-glycoprotein (P-gp). P-gp, encoded by the human multidrug resistance gene, MDR1, is a member of ATP-binding cassette (ABC) transporter superfamily, which can act as active efflux pump at plasma membrane. Cancer cells possessing MDR ability are exerting chemoresistance by reducing intracellular drug concentration utilizing the overexpressed P-gp. Therefore, P-gp has attracted much attention as a promising target for overcoming cancer chemoresistance, and many researches about cancer chemotherapy that combined with P-gp targeted MDR reversal and conventional anticancer drug treatment have been intensively progressed. As far as P-gp-targeted MDR reversal is concerned, two strategies, i.e., inhibition of P-gp function by chemosensitizers, and MDR1 gene silencing utilizing ASO or RNAi, have been employed.
Chemosentitizers, such as verapamil (VRP), Elacridar, Tariquidar, and so on, mainly act as antagonist for P-gp and suppress drug efflux, and consequently recover chemosensitivity of MDR cancer cells. Since required dose (2 µM - 6 µM) of VRP for P-gp inhibition is, however, significantly higher than the clinical dose for arrhythmia treatment and may induce cardiotoxicity, adoption of DDS, especially MDDS, to this system will be appropriate way to reduce unfavorable side effect and to enhance therapeutic outcome. Indeed, various liposomal or nanoparticulate MDDSs that can co-deliver both chemosensitizer and anticancer drug have been reported. Wang et al. developed the liposomal MDDS, in which both VRP and DOX were simultaneously loaded into internal aqueous phase of Stealth liposomes (PEGylated liposomes) by pHgradient remote loading method. [37]. This system had demonstrated high MDR reversal ability against the multidrug resistant rat prostate cancer cell line (Mat-LyLuB2 cells). Based on the preceding work, Wu et al. established improved liposomal MDDS possessing cancer-targeting ability [38]. In their system, transferrin (Tf), a ligand for transferrin receptor frequently overexpressed in tumor and leukemia cells, was conjugated to surface of Stealth liposome. Tf-modified dual-loaded Stealth liposome (Tf-L-DOX/VRP) showed Tf-mediated targeting ability and high efficiency of MDR reversal to DOX-resistant K562 leukemia cells. The MDR reversal efficiency of Tf-L-DOX/VRP was 5.61 times superior to free DOX treatment, whereas non-targeted Stealth liposome treatment was almost equivalent to free DOX.
In the case of nanoparticulate MDDSs aimed for MDR reversal, various types of carriers, such as ionic polysaccharide microsphere [39], polyalkylcyanoacrylate nanoparticle [40], nanoparticles consist of highly biocompatible polymers [41-43], and polymer-lipid hybrid nanoparticle [44,45], are utilized for dual-loading of chemosensitizer and anticancer drug. The successful example has been reported from Patil et al. [43]. In their system, PTX and tariquidar, the third generation P-gp inhibitor, were encapsulated into biotin-modified PLGA nanoparticle during preparation by oil-in-water emulsion solvent evaporation method. Dual loaded nanoparticles showed significantly higher cytotoxicity in vitro compared to PTX single-loaded nanoparticles. Enhanced cytotoxicity caused by dual loaded nanoparticles treatment had been in good agreement with increased PTX-accumulation in drug-resistant cancer cells. The remarkable tumor growth inhibition was observed in drug-resistant tumor-bearing mice that treated with biotinylated nanoparticles encapsulating both PTX and tariquidar. Noteworthy, this therapeutic effect had been achieved at lower PTX dose that would be ineffective in the absence of tariquidar.
MDR1 gene silencing by ASO or siRNA are also attempted to suppress overexpression of P-gp and increase chemosensitivity of drug-resistant cancer [46,47]. For example, three agents (DOX, MDR1 and Bcl-2 targeted ASO) loaded Stealth liposome was prepared and applied to MDR reversal [46]. The distinctive feature of this system is that simultaneously aiming for suppression of DOX efflux by P-gp and enhancement of DOX-induced apoptosis. Three agents loaded liposomal MDDS achieved almost five-order reduction of IC50 value against for multidrug-resistant A2870/AD human ovarian carcinoma cells compared to free DOX treatment. The PEGylated liposome encapsulating DOX and ASOs showed significant tumor growth inhibition that correlated to enhanced apoptosis observed in tumor tissue of multidrug-resistant A2870 xenograft mouse model.
3. Sequential Multi-Agent Delivery by Bulk System
In the preceding section, concrete examples of various BCM-based MDDS that can simultaneously deliver multiple agents are introduced. On the other hand, there are many cases, in which not only the drug combination but also administration order and/or time lag will be important. Development of sequential delivery system that can achieve differential release control of individual agent from single formulation is another major task of DDS research. From this point of view, many researchers have made much effort to establish novel sequential multidrug delivery system. In particulate systems, the core/shell structure has been employed for the sequential multidrug delivery [30,48,49]. Meanwhile, the type of developed system with bulk matrices could be roughly classified into two categories, i.e., multilayered and composite system.
3.1. Multilayered System
The structural feature of this system is the multilayered structure that composed of hydrogels, polymer-form, polymer-film, and so on. In the multilayered systems, the release sequence of individual agents can control by lamination of agent-loaded layer in adequate and required order. Exceptionally the monolayer system of alginate hydrogel, in which release order of VEGF and PDGF is controlled by difference of diffusibility from gel matrix, has been reported from Hao et al. [50].
Some multilayered systems have been reported to date [51-53]. For example, the two-layered heterogeneously loaded and crosslinked gelatin gel system was prepared for sequential delivery of two bone growth factors, BMP- 2 and IGF-I, by Raiche and Puleo [51]. In their system, the burst release of growth factors was suppressed by crosslink ratio of individual layer. Pluripotent C3H10T1/2 cells exhibited significantly higher levels of osteoblastic phenotype, such as alkaline phosphatase activity and mineralized matrix formation, at early phase through cultivation on the two-layered gel matrix, which was releaseable BMP-2 and IGF-I in appropriate order (i.e., BMP-2 followed sequentially by IGF-I or BMP-2 plus IGF-I). More practical use directed system has been developed by Strobel et al. [53]. In their system, titanium Kirschner wire (K-wire) commonly used for fracture treatment was multiply coated with poly(D,L-lactide) (PDLLA) by dipping method. To form multiple coating on the surface, K-wire was sequentially immersed into three solutions of PDLLA that individually included gentamicin (antibiotics), IGF-I, or BMP-2. Prevention of infections on wound region was also aimed in addition to the stimulation of bone healing in this system. The multilayer coated K-wire displayed distinctitve release profile: 1) a burst release of gentamicin; 2) a burst and sustained release of IGF-I; and 3) a slow sustained release of BMP-2.
3.2. Composite System
Composite systems are commonly constructed by doping particulate DDS into bulk materials, such as hydrogel, polymer-form, and so on. The agents should be delivered are separately incorporated into particulate DDS and bulk material, respectively. Or the agents are loaded respectively into different particulate DDSs, and the bulk material is used only as a support of doped particulate. In this system, release profiles of individual agents are controlled by diffusibility from bulk material and/or releasing property of the utilized particulate DDS.
Hasirci and co-workers have attempted to develop sequential multi-agents delivery system for bone tissue engineering utilizing composite system. They first reported the poly(4-vinyl pyridine) (P4VP)/alginate microsphere doped PLGA-form scaffold for sequential delivery of BMP-2 and BMP-7 [54]. In this system, the release profiles of two growth factors can be controlled by P4VP/- alginic acid concentration at microsphere preparation. They also reported another BMP-2/BMP-7 sequential delivery system [55]. Two different polymers, PLGA and poly(3-hydroxybutyrate-co-3-hydroxyvalerate) (PHBV), were used for preparation of fastand slow-releasing nanocapsules, respectively, and these nanoparticles having different release rate were loaded to the chitosan-based wet-spun fiber scaffold. In each system, the sequential delivery of BMP-2 and BMP-7 from single formulation synergistically enhanced osteogenic differentiation against rat bone marrow derived stem cells. On the other hand, the injectable sequential multi-agents delivery system, which consists of PLG microsphere loaded alginate hydrogel, has been developed by Sun et al. [56]. In their system, two angiogenesis related growth factors, VEGF and PDGF, were respectively incorporated into alginate hydrogel and PLG microsphere for efficient neovasculalization on ischemic lesion site. The local concentrations of VEGF and PDGF on injected site reached peak level at week 2 and 4, respectively, and sustained PDGF release lasted to week 6. Sequential VEGF/PDGF delivery significantly promoted angiogenesis and induced reperfusion compared to single VEGF delivery or control.
3.3. Approaches for More Rigorous Temporal Release Control
The importance of sequential administration with pre-determined order and/or timing has been demonstrated in several systems, such as BCM-based cancer chemotherapy [3,57,58], bone regeneration [59], angiogenesis [60], and so on. According to these reports, it is expected that the precise control of release characteristics, especially administration order and timing, can be led more improved therapeutic outcome. However, all systems that developed to date have simultaneous releasing period. To realize more functional and effective combination therapy, more rigorous temporally controlled sequential release system has to be developed. It seems that this is one of major issue should be attempted. To address this issue, some approaches have been reported.
For instance, sequential delivery systems, which are capable of controlled release behaviors in response to external environmental changes such as pH and temperature, have been established. Xia et al. have developed the pH-controlled selective gentamicin/naproxen release system utilizing mesoporous bioactive glass (MBG)/poly(γ- benzyl-L-glutamate)-poly(ethylene glycol) graft copolymer (PBGL-g-PEG) nanomicelle composite materials [61]. The water-soluble gentamicin and lipophilic naproxen were respectively encapsulated into interior of MBG via hydrogen bond and core of PBGL-g-PEG nanomicelle via hydrophobic interaction. At low pH condition, the interaction between gentamicin and MBG surface was weakened with increasing of H+, and consequently gentamicin was quickly released, whereas the L-glutamate side chain was protonated and naproxen was stably encapsulated in PBGL-g-PEG nanomicelle core. Meanwhile, the opposite phenomenon was caused at high pH condition. The pH-controlled release of this system was realized due to opposite pH-dependency of release behavior of each material. The further functionalized dual-drug delivery system that can be response to both pH and temperature has been reported from Wei et al. [62]. In their system, pH-responsive chitosan/poly(vinyl alchol) hydrogel and pH/temperature dual responsive poly(L-glutamic acid)-b-poly(propylene oxide) -b-poly(L-glutamic acid) (GPG) micelle were employed and combined to encapsulate aspirin and DOX, respectively. With increasing pH value, the release rate of aspirin from chitosan/PVA hydrogel was accelerated, whereas DOX release from GPG micelle was facilitated with pH value lowering and/or temperature elevation.
Although the above-mentioned approaches are very interesting and useful from the standpoint of the rigorous release timing control, the temporal regulation is still insufficient. To address this issue, we have developed the multilayered nanofiber mesh system for time-programmed dual-drug delivery utilizing the sequential electrospinning method [63]. Electrospinning is a key technology that can easily fabricate nano-/micro-fiber mesh from various polymers. Since electrospun products have some distinctive properties such as high surface-area-to-volume ratio, flexible designability of morphology, and extracellular matrix-like structure, they have attracted much attention in the research fields of DDS and tissue engineering. The multilayered drug-loaded fiber mat that consists of biodegradable PLCL was designed with the following construction from top to bottom: 1) the first drug-loaded mesh; 2) plain mesh act as barrier; 3) the second drug-loaded mesh; and 4) the basement plain mesh. In our system, to prevent simultaneous release of the second drug during the first drug release, the basement and barrier mesh were prepared as having enough thickness and the second drug loaded mesh was sealed between the basement and barrier mesh. The release suppression period of the second drug could be prolonged in the barrier mesh thickness dependent manner. Based on four-layered structure, introduction of the complete suppression period of the seconddrug release at the end of the first-drug release was achieved by setting of barrier mesh with appropriate thickness, and subsequently the second-drug release was initiated and lasted. Moreover, since the release rate of individual drugs from electrospun fiber was accelerated with decreasing of fiber diameter, the release profile of whole system could be altered by controlling of fiber diameter. This is the first example of time-programmed dual-drug sustained release utilizing multilayered electrospun fiber mat formulation. Namely, we have successfully developed the sequential MDDS that would be able to realize more functional and effective combination therapy.
4. Future Perspective
As we introduced and mentioned in preceding sections, huge efforts have been devoted by researchers to establish the MDDSs with single formulation in the past decade. With recent remarkable evolution of nanobiotechnology and material sciences, not only exploitation of novel system but also improvement of pre-existing system have been actively attempted, and consequently various promising results have been demonstrated. However, it seems that there are still some rooms for further improvement. Especially, the development of more efficient active targeting system, more functionalized system, and more rigorously time controlled multi-drug/agent release system would be important issue in current and future DDS research.
The development of novel ligand would be essentially important for development of more efficient active targeting system. The contribution of nanobiotechnology would be indispensable for exploring of novel targeting molecules by high-throughput screening. Since DNA aptamers, which has antibody-compatible specific binding ability for several kinds of antigen, has been found out day by day [64], DNA aptamers would be one of promising molecule for more efficient active targeting. Furthermore, in recent years, development of multi-functional DDSs possessing not only drug delivery but also bioimaging ability has attracted much attention in the research field of DDS. Supplementation of bioimaging capability is very useful attempt in terms of visualization of the therapeutic effect. Indeed, development of bioimaging compatible MDDSs have been started [65-67]. The addition of extra function such as bioimaging has also been expected.
Meanwhile, site-specific drug release can be more easily achieved by bulk system in exchange for restriction of administration site. Furthermore, the individual release profiles of loaded drugs can also be easily controlled in the bulk system compared to particulate systems. As we mentioned in preceding section 3, rigorous release control of individual drugs has not sufficiently been achieved yet. However, we successfully demonstrated that the rigorously temporal controlled MDDS could be developed by appropriate material design and fine processing utilizing electrospinning. Therefore, both exploitation of novel functional materials and technical advance of material processing would be essentially needed for fine release control. Concretely, smart material that can change own characteristics responded to various environmental stimuli such as temperature, pH, and so on, and nanoscale precise processing technology such as layering, alignment, and configuration will be extensively required. In addition, although pre-constructed bulk formulation is potentially possessing restriction on selection of administration site, this issue will be circumvented by development of more flexible system such as injectable hydrogel that can perform in situ sol-gel phase transition or chemical polymerization.
In conclusion, although development of MDDS with single formulation having simultaneous or precisely-controlled sequential delivery capability is still immature and challenging field in DDS research, it is expected that establishment of more improved and functional MDDS would expand the potential of combination therapy based on BCM. For realization of more efficient, functional, and safe BCM-based multiple medications with the MDDS, the contributions of biomaterials science and nanobiotechnology to every steps of MDDS construction are essentially required. Moreover, since investigation and selection of effective drug combinations is an important factor for BCM-based chemotherapy, strategic alliance among experts of different fields such as medical doctors, paramedics, biologists, and engineers, would be also needed. We have expected early realization of combination therapy by MDDS with single formulation in clinical medication by synergistic cooperation of researchers.
REFERENCES
- D. S. Martin, R. L. Stolfi, R. C. Sawyer and C. W. Young, “Application of biochemical modulation with a therapeutically inactive modulating agent in clinical trials of cancer chemotherapy,” Cancer Treatment Report, Vol. 69, No. 4, 1985, pp. 421-423.
- B. Leyland-Jones and P. J. O’Dwyer, “Biochemical modulation: application of labolatory models to the clinic,” Cancer Treatment Report, Vol. 70, No. 1, 1986, pp. 219- 229.
- J. R. Bertino, W. L. Sawicki, C. A. Lindquist and V. S. Gupta, “Schedule-Dependent Antitumor Effects of Methotrexate and 5-Fluorouracil,” Cancer Research, Vol. 37, No. 1, 1977, pp. 327-328.
- C. Tournigand, et al., “FOLFIRI Followed by FOLFOX6 or the reverse sequence in advanced colorectal cancer: a randomized GERCOR study,” Journal of Clinical Oncology, Vol. 22, No. 2, 2004, pp. 229-237. doi:10.1200/JCO.2004.05.113
- F. Maindrault-Goebe, et al., “High-dose intensity oxaliplatin added to the simplified bimonthly leucovorin and 5-fluorouracil regimen as second-line therapy for metastatic colorectal cancer (FOLFOX 7),” European Journal of Cancer, Vol. 37, No. 8, 2001, pp. 1000-1005. doi:10.1016/S0959-8049(01)00068-5
- J. C. Bendell, et al., “Randomized phase II study of perifosine in Combination with capecitabine (P-CAP) versus capecitabine plus placebo (CAP) in patients with secondor third-line metastatic colon cancer (mCRC): Updated results,” Gastrointestinal Cancers Symposium, Orland, 22-24 January 2010.
- M. Peeters, et al., “Randomized phase III study of panitumumab (pmab) with FOLFIRI versus FOLFIRI Alone as second-line treatment (tx) in patients (pts) with metastatic colorectal cancer (mCRC): Patient-Reported Outcomes (PRO),” Gastrointestinal Cancers Symposium, Orland, 22-24 January 2010.
- V. Torchilin, “Recent advances with liposomes as pharmaceutical carriers,” Nature reviews Drug discovery, Vol. 4, No. 2, 2005, pp. 145-160. doi:10.1038/nrd1632
- Y. Kakizawa and K. Kataoka, “Block copolymer micelles for delivery of gene and related compounds,” Advanced Drug Delivery Reviews, Vol. 54, No. 2, 2002, pp. 203-222. doi:10.1016/S0169-409X(02)00017-0
- M. Yokoyama, “Polymeric micelles as a new drug carrier system and their required considerations for clinical trials,” Expert opinion on drug delivery, Vol. 7, No. 2, 2010, pp. 145-158. doi:10.1517/17425240903436479
- C. Amin, N. Mackman and N. S. Key, “Microparticles and Cancer,” Pathophysiology of haemostasis and thrombosis, Vol. 36, No. 3-4, 2008, pp. 177-183. doi:10.1159/000175155
- H. Maeda, T. Sawa and T. Konno, “Mechanism of tumortargeted delivery of macromolecular drugs, including the EPR effect in solid tumor and clinical overview of the prototype polymeric Drug SMANCS,” Journal of Controlled Release, Vol. 74, No. 1-3, 2001, pp. 47-61. doi:10.1016/S0168-3659(01)00309-1
- N. D. James, et al., “Liposomal doxorubicin (Doxil): an effective new treatment for Kaposi’s sarcoma in AIDS,” Clinical oncology, Vol. 6, No. 5, 1994, pp. 294-296. doi: 10.1016/S0936-6555(05)80269-9
- S. de Marie, R. Janknegt, and I. A. Bakker-Woudenberg, “Clinical use of liposomal and lipid-complexed amphotericin B,” The Journal of antimicrobial chemotherapy, Vol. 33, No. 5, 1994, pp. 907-916. |doi:10.1093/jac/33.5.907
- M. Harries, P. Ellis and P. Harper, “Nanoparticle albuminbound paclitaxel for metastatic breast cancer,” Journal of clinical oncology, Vol. 23, No. 31, 2005, pp. 7768- 7771. doi:10.1200/JCO.2005.08.002
- F. Greco and M. J. Vicent, “Combination therapy: opportunities and challenges for polymer-drug conjugates as anticancer nanomedicines,” Advanced Drug Delivery Reviews, Vol. 61, No. 13, 2009, pp. 1203-1213. doi:10.1016/j.addr.2009.05.006
- C.-M. J. Hu, S. Aryal and L. Zhang, “Nanoparticle-Assisted combination therapies for effective cancer treatment,” Therapeutic Delivery, Vol. 1, No. 2, 2010, pp. 323- 334. doi:10.4155/tde.10.13
- H. Zhang, G. Wang, and H. Yang, “Drug delivery systems for differential release in combination therapy,” Expert opinion on drug delivery, Vol. 8, No. 2, 2011, pp. 171-190. doi:10.1517/17425247.2011.547470
- L. Santucci, et al., “Nitric Oxide Modulates Proapoptotic and Antiapoptotic Properties of Chemotherapy Agents: The Case of NO-Pegylated Epirubicin,” The FASEB Journal, Vol. 20, No. 6, 2006, pp. 765-767. doi:10.1096/fj.05-4452fje
- G. Pasut, et al., “Polymer-drug conjugates for combination anticancer therapy: investigating the mechanism of action,” Journal of Medicinal Chemistry, Vol. 52, No. 20, 2009, pp. 6499-6502. doi:10.1021/jm900804m
- Q. Wu, R. Kreienberg and I. B. Runnebaum, “Growth suppression of human ovarian carcinoma OV-MZ-2a and OV-MZ-32 cells mediated by gene transfer of wildtype p53 enhanced by chemotherapy in vitro,” Journal of Cancer Research and Clinical Oncology, Vol. 126, No. 3, 2000, pp. 139-144. doi:10.1007/s004320050023
- N. Wiradharma, Y. W. Tong and Y. Y. Yang, “Self-assembled oligopeptide nanostructures for co-delivery of drug and gene with synergistic therapeutic effect,” Biomaterials, Vol. 30, No. 17, 2009, pp. 3100-3109. doi: 10.1016/j.biomaterials.2009.03.006
- S. Shin, et al., “An Anti-Apoptotic Protein Human Survivin Is a Direct Inhibitor of Caspase-3 and -7,” Biochemistry, Vol. 40, No. 4, 2001, pp. 1117-1123. doi:10.1021/bi001603q
- A. Chandele, V. Prasad, J. C. Jagtap, R. Shukla and P. R. Shastry, “Upregulation of survivin in G2/M cells and inhibition of caspase 9 activity enhances resistance in staurosporine-induced apoptosis,” Neoplasia, Vol. 6, No. 1, 2004, pp. 29-40.
- J. C. Reed, “The Survivin Saga Goes in Vivo,” The Journal of Clinical Investigation, Vol. 108, No. 7, 2001, pp. 965-969. doi:10.1172/JCI14123
- W. Xiao, X. Chen, L. Yang, Y. Mao, Y. Wei and L. Chen, “Co-delivery of doxorubicin and plasmid by a novel FGFR-mediated cationic liposome,” International Journal of Pharmaceutics, Vol. 393, No. 1-2, 2010, pp. 119- 126. doi:10.1016/j.ijpharm.2010.04.018
- Z. Xu, Z. Zhang, Y. Chen, L. Chen, L. Lin and Y. Li, “The characteristics and performance of a multifunctional nanoassembly system for the co-delivery of docetaxel and iSur-pDNA in a mouse hepatocellular carcinoma model,” Biomaterials, Vol. 31, No. 5, 2010, pp. 916-922. doi:10.1016/j.biomaterials.2009.09.103
- G. M. Tozer, C. Kanthou and B. C. Baguley, “Disrupting Tumour Blood Vessels,” Nature Reviews Cancer, Vol. 5, No. 6, 2005, pp. 423-435. doi:10.1038/nrc1628
- Y.-F. Zhang, J.-C. Wang, D.-Y. Bian, X. Zhang and Q. Zhang, “Targeted delivery of RGD-modified liposomes encapsulating both combretastatin A-4 and doxorubicin for tumor therapy: in vitro and in vivo studies,” European journal of pharmaceutics and biopharmaceutics, Vol. 74, No. 3, 2010, pp. 467-473. doi:10.1016/j.ejpb.2010.01.002
- Z. Wang and P. C. Ho, “A nanocapsular combinatorial sequential drug delivery system for antiangiogenesis and anticancer activities,” Biomaterials, Vol. 31, No. 27, 2010, pp. 7115-7123. doi:10.1016/j.biomaterials.2010.05.075
- T. Yang, et al., “Targeted delivery of a combination therapy consisting of combretastatin A4 and low-dose doxorubicin against tumor neovasculature,” Nanomedicine: Nanotechnology, Biology, and Medicine, 2011, in press. doi:10.1016/j.nano.2011.05.003
- D. Ingber, et al., “Synthetic analogues of fumagillin that inhibit angiogenesis and suppress tumour growth,” Nature, Vol. 348, No. 6301, 1990, pp. 555-557. doi:10.1038/348555a0
- R. Satchi-Fainaro, et al., “Targeting Angiogenesis with a Conjugate of HPMA Copolymer and TNP-470,” Nature Medicine, Vol. 10, No. 3, 2004, pp. 255-261. doi:10.1038/nm1002
- E. Segal, et al., “Targeting angiogenesis-dependent calcified neoplasms using combined polymer therapeutics,” PloS One, Vol. 4, No. 4, 2009, p. e5233. doi:10.1371/journal.pone.0005233
- C. Zhu, et al., “Co-delivery of siRNA and paclitaxel into cancer cells by biodegradable cationic micelles based on PDMAEMA-PCL-PDMAEMA triblock copolymers,” Biomaterials, Vol. 31, No. 8, 2010, pp. 2408-2416. doi:10.1016/j.biomaterials.2009.11.077
- H.-Y. Huang, W.-T. Kuo, M.-J. Chou and Y.-Y. Huang, “Co-delivery of anti-vascular endothelial growth factor siRNA and doxorubicin by multifunctional polymeric micelle for tumor growth suppression,” Journal of biomedical materials research Part A, Vol. 97, No. 3, 2011, pp. 330-338. doi:10.1002/jbm.a.33055
- J. Wang, et al., “In vitro cytotoxicity of Stealth liposomes co-encapsulating doxorubicin and verapamil on doxorubicin-resistant tumor cells,” Biological & Pharmaceutical Bulletin, Vol. 28, No. 5, 2005, pp. 822-828. doi:10.1248/bpb.28.822
- J. Wu, et al., “Reversal of multidrug resistance by transferrin-conjugated liposomes co-encapsulating doxorubicin and verapamil,” Journal of pharmacy & pharmaceutical sciences, Vol. 10, No. 3, 2007, pp. 350-357.
- Z. Liu, X. Y. Wu and R. Bendayan, “In vitro investigation of ionic polysaccharide microspheres for simultaneous delivery of chemosensitizer and antineoplastic agent to multidrug-resistant cells,” Journal of Pharmaceutical Sciences, Vol. 88, No. 4, 1999, pp. 412-418. doi:10.1021/js9803353
- C. E. Soma, C. Dubernet, D. Bentolila, S. Benita and P. Couvreur, “Reversion of multidrug resistance by co-encapsulation of doxorubicin and cyclosporin A in polyalkylcyanoacrylate nanoparticles,” Biomaterials, Vol. 21, No. 1, 2000, pp. 1-7. doi:10.1016/S0142-9612(99)00125-8
- X. Song, et al., “PLGA nanoparticles simultaneously loaded with vincristine sulfate and verapamil hydrochloride: systematic study of particle size and drug entrapment efficiency,” International Journal of Pharmaceutics, Vol. 350, No. 1-2, 2008, pp. 320-329. doi:10.1016/j.ijpharm.2007.08.034
- X. R. Song, et al., “Reversion of multidrug resistance by co-encapsulation of vincristine and verapamil in PLGA nanoparticles,” European journal of pharmaceutical sciences, Vol. 37, No. 3-4, 2009, pp. 300-305. doi:10.1016/j.ejps.2009.02.018
- Y. Patil, T. Sadhukha, L. Ma and J. Panyam, “Nanoparticle-mediated simultaneous and targeted delivery of paclitaxel and tariquidar overcomes tumor drug resistance,” Journal of Controlled Release, Vol. 136, No. 1, 2009, pp. 21-29. doi:10.1016/j.jconrel.2009.01.021
- H. L. Wong, R. Bendayan, A. M. Rauth and X. Y. Wu, “Development of solid lipid nanoparticles containing ionically complexed chemotherapeutic drugs and chemosensitizers,” Journal of Pharmaceutical Sciences, Vol. 93, No. 8, 2004, pp. 1993-2008. doi:10.1002/jps.20100
- H. L. Wong, R. Bendayan, A. M. Rauth and X. Y. Wu, “Simultaneous delivery of doxorubicin and GG918 (Elacridar) by new polymer-lipid hybrid nanoparticles (PLN) for enhanced treatment of multidrug-resistant breast cancer,” Journal of Controlled Release, Vol. 116, No. 3, 2006, pp. 275-284. doi:10.1016/j.jconrel.2006.09.007
- R. I. Pakunlu, Y. Wang, M. Saad, J. J. Khandare, V. Starovoytov and T. Minko, “In vitro and in vivo intracellular liposomal delivery of antisense oligonucleotides and anticancer drug,” Journal of Controlled Release, Vol. 114, No. 2, 2006, pp. 153-162. doi: 0.1016/j.jconrel.2006.06.010
- X.-B. Xiong and A. Lavasanifar, “Traceable multifunctional micellar nanocarriers for cancer-targeted co-delivery of MDR-1 siRNA and doxorubicin,” ACS Nano, Vol. 5, No. 6, 2011, pp. 5202-5213. doi:10.1021/nn2013707
- S. Sengupta, et al., “Temporal targeting of tumour cells and neovasculature with a nanoscale delivery system,” Nature, Vol. 436, No. 7050, 2005, pp. 568-572. doi:10.1038/nature03794
- H. Nie, Z. Dong, D. Y. Arifin, Y. Hu and C.-H. Wang, “Core/shell microspheres via coaxial electrohydrodynamic atomization for sequential and parallel release of drugs,” Journal of Biomedical Materials Research Part A, Vol. 95, No. 3, 2010, pp. 709-716. doi:10.1002/jbm.a.32867
- X. Hao, et al., “Angiogenic effects of sequential release of VEGF-A165 and PDGF-BB with alginate hydrogels after myocardial infarction,” Cardiovascular Research, Vol. 75, No. 1, 2007, pp. 178-185. doi:10.1016/j.cardiores.2007.03.028
- A. T. Raiche and D. A. Puleo, “In vitro effects of combined and sequential delivery of two bone growth factors,” Biomaterials, Vol. 25, No. 4, 2004, pp. 677-685. doi:10.1016/S0142-9612(03)00564-7
- R. R. Chen, E. A. Silva, W. W. Yuen and D. J. Mooney, “Spatio-temporal VEGF and PDGF delivery patterns blood vessel formation and maturation,” Pharmaceutical Research, Vol. 24, No. 2, 2007, pp. 258-264. doi:10.1007/s11095-006-9173-4
- C. Strobel, N. Bormann, A. Kadow-Romacker, G. Schmidmaier and B. Wildemann, “Sequential release kinetics of two (gentamicin and BMP-2) or three (gentamicin, IGF-I and BMP-2) substances from a one-component polymeric coating on implants,” Journal of Controlled Release, Vol. 156, No. 1, 2011, pp. 37-45. doi:10.1016/j.jconrel.2011.07.006
- F. B. Basmanav, G. T. Kose and V. Hasirci, “Sequential growth factor delivery from complexed microspheres for bone tissue engineering,” Biomaterials, Vol. 29, No. 31, 2008, pp. 4195-4204. doi:10.1016/j.biomaterials.2008.07.017
- P. Yilgor, K. Tuzlakoglu, R. L. Reis, N. Hasirci and V. Hasirci, “Incorporation of a sequential BMP-2/BMP-7 delivery system into chitosan-based scaffolds for bone tissue engineering,” Biomaterials, Vol. 30, No. 21, 2009, pp. 3551-3559. doi:10.1016/j.biomaterials.2009.03.024
- Q. Sun, et al., “Sustained release of multiple growth factors from injectable polymeric system as a novel therapeutic approach towards angiogenesis,” Pharmaceutical Research, Vol. 27, No. 2, 2010, pp. 264-271. doi:10.1007/s11095-009-0014-0
- J. A. MacDiarmid, et al., “Sequential treatment of drugresistant tumors with targeted minicells containing siRNA or a cytotoxic drug,” Nature Biotechnology, Vol. 27, No. 7, 2009, pp. 643-651. doi:10.1038/nbt.1547
- J. Jiangm, et al., “Sequential treatment of drug-resistant tumors with RGD-modified liposomes containing siRNA or doxorubicin,” European journal of pharmaceutics and biopharmaceutics, Vol. 76, No. 2, 2010, pp. 170-178. doi:10.1016/j.ejpb.2010.06.011
- P. Yilgor, N. Hasirci and V. Hasirci, “Sequential BMP-2/ BMP-7 delivery from polyester nanocapsules,” Journal of Biomedical Materials Research Part A, Vol. 93, No. 2, 2010, pp. 528-536. doi:10.1002/jbm.a.32520
- J. E. Tengood, K. M. Kovach, P. E. Vescovi, A. J. Russell and S. R. Little, “Sequential delivery of vascular endothelial growth factor and sphingosine 1-phosphate for angiogenesis,” Biomaterials, Vol. 31, No. 30, 2010, pp. 7805-7812. doi:10.1016/j.biomaterials.2010.07.010
- W. Xia, J. Chang, J. Lin and J. Zhu, “The pH-controlled dual-drug release from mesoporous bioactive glass/ polypeptide graft copolymer nanomicelle composites,” European journal of pharmaceutics and biopharmaceutics, Vol. 69, No. 2, 2008, pp. 546-552. doi:10.1016/j.ejpb.2007.11.018
- L. Wei, C. Cai, J. Lin and T. Chen, “Dual-drug delivery system based on hydrogel/micelle composites,” Biomaterials, Vol. 30, No. 13, 2009, pp. 2606-2613. doi:10.1016/j.biomaterials.2009.01.006
- T. Okuda, K. Tominaga and S. Kidoaki, “Time-programmed dual release formulation by multilayered drug-loaded nanofiber meshes,” Journal of Controlled Release, Vol. 143, No. 2, 2010, pp. 258-264. doi:10.1016/j.jconrel.2009.12.029
- A. S. Barbas, J. Mi, B. M. Clary and R. R. White, “Aptamer applications for targeted cancer therapy,” Future Oncology, Vol. 6, No. 7, 2010, pp. 1117-1126. doi:10.2217/fon.10.67
- X.-B. Xiong and A. Lavasanifar, “Traceable multifunctional micellar nanocarriers for cancer-targeted co-delivery of MDR-1 siRNA and doxorubicin,” ACS Nano, Vol. 5, No. 6, 2011, pp. 5202-5213. doi:10.1021/nn2013707
- A. Singh, F. Dilnawaz, S. Mewar, U. Sharma, N. R. Jagannathan and S. K. Sahoo, “Composite polymeric magnetic nanoparticles for co-delivery of hydrophobic and hydrophilic anticancer drugs and MRI imaging for cancer therapy,” ACS Applied Materials & Interfaces, Vol. 3, No. 3, 2011, pp. 842-856. doi:10.1021/am101196v
- C.-C. Huang, W. Huang and C.-S. Yeh, “Shell-by-shell synthesis of multi-shelled mesoporous silica nanospheres for optical imaging and drug delivery,” Biomaterials, Vol. 32, No. 2, 2011, pp. 556-564. doi: 0.1016/j.biomaterials.2010.08.114
NOTES
*Corresponding author.

