Surgical Science
Vol.5 No.5(2014), Article ID:46324,3 pages DOI:10.4236/ss.2014.55040
Malakoplakia of the Testis
Siddharth P. Dubhashi1*, Harsh Kumar2, Vivek Kulkarni1, Adil M. Suleman1
1Department of General Surgery, Padmashree Dr. D. Y. Patil Medical College, Hospital and Research Centre, Pune, India
2Department of Pathology, Padmashree Dr. D. Y. Patil Medical College, Hospital and Research Centre, Pune, India
Email: *spdubhashi@gmail.com
Copyright © 2014 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/


Received 4 April 2014; revised 3 May 2014; accepted 10 May 2014
ABSTRACT
Malakoplakia is an uncommon chronic inflammatory disease usually affecting the urogenital tract and often associated with the infection due to E. coli. It is characterised by the presence of Von Hansemann cells and intracytoplasmic inclusion bodies called Michaelis-Gutmann Bodies. Testes are affected in 12% cases. The lesion mainly occurs in middle aged men, appearing clinically as epididymo-orchitis or testicular enlargement with fibrous consistency and some soft areas. Orchidectomy is the only way to differentiate the lesion from other malignant or infected processes. This is a case report of a young patient with testicular malakoplakia.
Keywords:Michaelis-Gutmann Bodies, Plaques, Testicular Malakoplakia, Von-Hansemann Cells

1. Introduction
Malakoplakia is an uncommon chronic inflammatory disease usually affecting the urogenital tract and often associated with the infection due to E. coli [1] . The condition was originally described by Michaelis and Gutmann in1902 [2] . The term malakoplakia was coined by Von Hansemann (from the Greek malakos, soft and plakos, plaque) in 1903 [3] . The urinary bladder is the most commonly affected site, though involvement of the extravesical sites such as kidneys, testis, prostate and colon is also reported [4] . Malakoplakia is characterised by the presence of large cells with abundant eosinophilic cytoplasm called Von Hansemann cells and within the cytoplasm are present calcified inclusion bodies called as Michaelis-Gutmann (MG) bodies which exhibit a concentric laminated (targetoid or owl’s eye) appearance with a basic dye like haematoxyline [4] [5] . This is a case report of a young patient with testicular malakoplakia.
2. Case Report
A 24-year-old patient presented to the surgical emergency room with pain in left hemiscrotum since 3 weeks. There were no urinary complaints. On examination, there was swelling of the left hemiscrotum with an erythematous overlying skin. Palpation revealed a firm, tender swelling with local rise in temperature. There was no evidence of inguinal lymphadenopathy. A clinical diagnosis of pyocele was made. Urine examination showed few pus cells. Ultrasound showed an enlarged left testicle with hypoechoicechotexture with highly increased vascularity on colour doppler study. A 9 mm size hypo to isoechoic wedge shaped lesion was noted at its anterior aspect with no obvious vascularity within it, suggestive of a haematoma. A diagnosis of left orchitis with small intratesticular haematoma was made and the patient was administered anti-inflammatory treatment with analgesia. The condition did not improve clinically after 5 days of treatment. The urine culture report revealed infection with E. coli. A decision for scrotal exploration was taken. Intraoperatively, the tunica albugenia was thickened and showed haemorrhagic areas. There was evidence of thick, purulent fluid within the left testis with yellowish plaques (Figure 1). Left orchidectomy was performed and histopathological examination of specimen revealed atrophy of the tubules along with interstitial infiltration by large number of histiocytes with abundant granular eosinophilic cytoplasm. The histiocytes showed intracytoplasmicMichaelis-Gutmann bodies (Figure 2). PAS stain confirmed the same. A final diagnosis of malakoplakia of testis was made. The culture report of
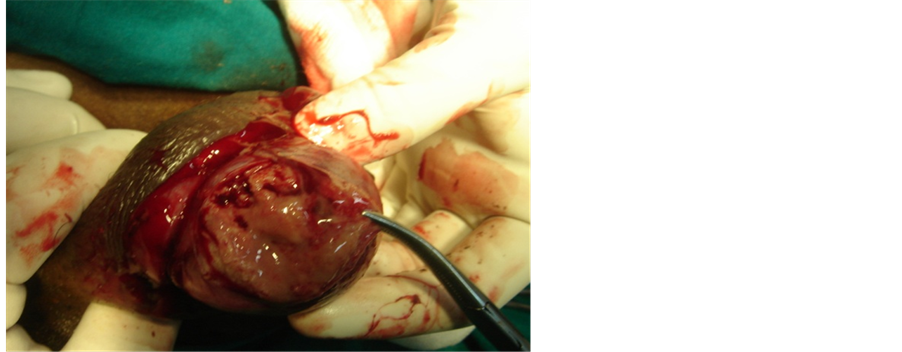
Figure 1. Necrotic material with yellow plaques in testicle.
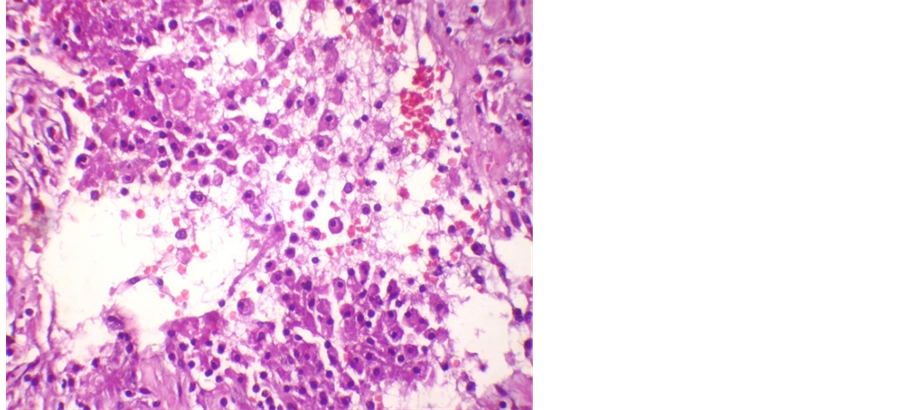
Figure 2. Photomicrography of testis (×1000 H & E). Higher magnification showing macrophages with Michaelis-Gutmann bodies.
the purulent fluid revealed Klebsiellapneumoniae sensitive to Quinolones. Ciprofloxacin was administered for 3 months. The patient has been asymptomatic with a follow up of one year till date.
3. Discussion
The first case of testicular malakoplakia was published in 1958 by Haukohl and Chinchinian [6] . The lesion occurs mainly in middle-aged men, appearing clinically as epididymo-orchitis affected in 12% cases. Several theories have been put forth, with three factors playing a major role: altered phagocytic function of macrophages, gram-negative infection and an abnormal immune response [7] . It may be an expression of microtubular/microfilamentaldysfunction [5] . Ineffective phagocytosis occurs due to defect in the lysosome response of macrophages to bacterial infections, usually by E. coli, as seen in our case. There seems to be an imbalance between cyclic adenosine monophosphate (AMPc) and cyclic guanosine monophosphate (GMPc), which causes inadequate lysosomic degranulation in the monocytes [7] .
The association of coliform urinary infection with testicular malakoplakia can be explained by the fact that testicular infection may be acquired by retrograde spread from the urinary tract and is intratubular initially. The Sertoli cells and macrophages interact with bacteria, forming intracellular phagosomes which may fuse to form giant cytosegrosomes which undergo calcification resulting in MG bodies [4] .
Grossly the lesions are yellowish soft plaques as seen in our case or nodules. Microscopically Von Hansemann cells and intensely PAS-positive structuresMG bodies are pathognomonic of malacoplakia [4] . In a study by McClure, out of the six cases in whom testicular tissue was taken and cultured for microorganisms, E. coli was cultured in four cases, Klebsiella pneumonia and Proteus species in other cases [4] . An increased frequency of malakoplakia in immunocompromised patients is well established and seen in upto 40% cases [8] . Other conditions which can coexist include cancer, diabetes, alcoholic liver disease and tuberculosis [7] . No such coexistent illness was observed in our case.
Orchidectomy is the only way to differentiate the lesion from other malignant or infectious processes like granulomatous orchitis. Although an infectious aetiology is evident, no antimicrobial therapy has been successful in the long term. Fluoroquinolones, especially ciprofloxacin, are the first choice drugs due to 80% to 90% effectiveness [7] . Patients with malakoplakia should be followed up periodically.
4. Conclusion
Malakoplakia of the testis is an uncommon chronic inflammatory condition which should be considered in the differential diagnosis of testicular swellings especially in association with gramnegative infections.
References
- Stanton, M.J. and Maxted, W. (1981) Malakoplakia: A Study of the Literature and Current Concepts of Pathogenesis, Diagnosis and Treatment. Journal of Urology, 125, 139.
- Michaelis, L. and Gutmann, C. (1902) UbreEinschlusse in Blasentumore. Klin Med, 47, 208.
- VonHansemann, D. (1903) Ubermalakoplakia der Harnblase. Virchows Archiv Pathol Anat, 173, 302-308.
- McClure, J. (1980) Malakoplakia of the Testis and Its Relationship to Granulomatous Orchitis. Journal of Clinical Pathology, 33, 670-678. http://dx.doi.org/10.1136/jcp.33.7.670
- McClure, J. (1981) Malakoplakia of the Gastrointestinal Tract. Postgraduate Medical Journal, 57, 95-103. http://dx.doi.org/10.1136/pgmj.57.664.95
- Haukohl, R.S. and Chinchinian, H. (1958) Malakoplakia of Testicle-Report of a Case. American Journal of Clinical Pathology, 29, 473-478.
- Alvarez, Bandres, S., Guarch, Troyas, R.M., Cebrian, Lostal, J.L., Ripa, Saldias, L., de Pablo, Cardenas, A., Jimenez, Parra, J.D. (2009) Malakoplakia of Testis: A New Case Report and a Literature Review. Urologic Surgical Pathology, 33, 1028-1031.
NOTES

*Corresponding author.

