World Journal of Cardiovascular Surgery
Vol.3 No.2(2013), Article ID:33378,5 pages DOI:10.4236/wjcs.2013.32010
Interest of Ventricular Assist Device in Peripartum Cardiomyopathy, a Case Report and Review Article*
1Cardiology Department, Beirut Cardiac Institute, Beirut, Lebanon
2Intensive Care Unit Department, Beirut Cardiac Institute, Beirut, Lebanon
3Cardiovascular Surgery Department, Beirut Cardiac Institute, Beirut, Lebanon
4Head of Cardiovascular Surgery Department, Beirut Cardiac Institute, Beirut, Lebanon
Email: #mdrighabh@hotmail.com
Copyright © 2013 Righab Hamdan et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received February 26, 2013; revised March 26, 2013; accepted April 3, 2013
Keywords: Postpartum Cardiomyopathy; Left Ventricle Assist Device
ABSTRACT
We report a case of severe post partum cadiomyopathy in severe cardiogenic shock, treated successfully and urgently with the implantation of Left Ventricular Assist device. The patient recovered a normal left ventricle function shortly after implantation. This case illustrates the crucial place of left ventricular assist device in severe post partum cardiomyopathy as a bridge to recovery as well as a bridge to transplantation.
1. Introduction
Peripartum cardiomyopathy is a rare disease affecting women in the last month of their pregnancy or up to five months after delivery; it affects one in every 3000 to 4000 live births in the US each year [1]. It was first described by Demakis in year 1971 [2]. Clear etiology remains debated. Peripartum cardiomyopathy is characterized by a high mortality risk and limited therapeutic medical options, though there is a possibility for full recovery within one year, raising thus the need for a temporary short or long term support of the left ventricle.
2. Case Report
We report the case of a 26 years old female patient addressed to our center for cardiogenic shock. She had no cardiovascular risk factors or previous medical history. She started complaining of severe shortness of breath a month after giving birth to a healthy girl. Her symptoms worsened within few days, leading to severe lung edema and hypotension. Upon her admission she was obnibulated, with a systolic blood pressure about 60 mmHgclinical findings were consistent with left and right heart failure, including pulmonary crackles, turgescent jugular veins, and lower limbs swelling. Chest X ray showed a large cardiothoracic index and pulmonary edema. She was in normal sinus rhythm. Blood tests showed hyponatremia (127 mmol/l), hyperkalemia (7.2 mmol/l), renal failure (BUN: 51 mmol/l, creatinine: 2.43 mg/dl). Cardiac ultrasound revealed a dilated cardiomyopathy with severe impairment of the left and right ventricle function (LVEF < 20%) (Figure 1). We also note severe mitral and tricuspid regurgitation. She remained hemodynamically unstable despite optimal medical support including inotrope drugs and diuretics, and intra aortic balloon contra pulsation, which motivated left ventricular assist device implantation (LVAD) (Heat Mate II, Thoratec). After LVAD implantation she remained in intensive care unit 3 weeks, with progressive weaning of inotropic drugs. Echocardiographic findings at 6 months follow up revealed improvement of LV function and size with quasinormalization of the global kinetics, whereas right ventricle remained dilated with systolic function impairment (Figure 2). The patient at 2 years follow-up states good life quality, and no exertional dyspnea for daily activities.
3. Discussion
Peripartum cardiomopathy:
Peripartum cardiomyopathy was first defined by De-
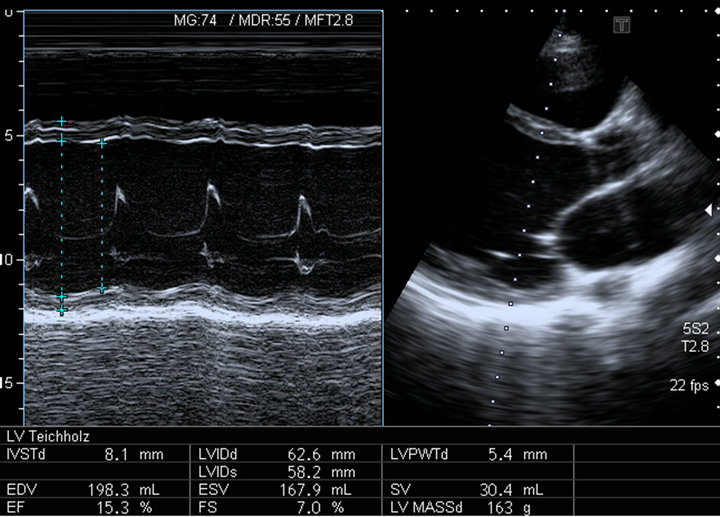
Figure 1. The first cardiac ultrasound on admission showed a dilated left ventricle with severe systolic function impairment, Time motion sequence (left) shows an end diastolic diameter of 62 mm.
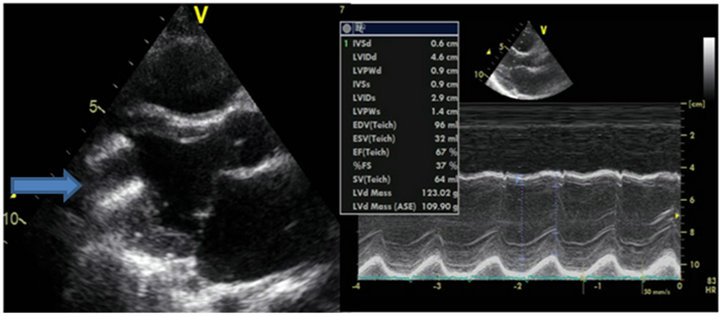
Figure 2. Cardiac ultrasound at 6 months follow up after LVAD implantation: on the left the bidimensional ultrasound shows the LVAD inflow canula with the left ventricle apex, time motion sequence on the right shows normal left ventricle dimensions and contractility, with an end diastolic diameter of 46 mm, and an ejection fraction of 67%.
makis in year 1971 [2] by the following criteria: 1—Development of heart failure in the last month of pregnancy or within the first 5 postpartum months, 2—Absence of a determine etiology, and 3—Absence of a demonstrable heart disease before the last month of pregnancy. Recently, echocardiographic criteria have also been added [3], which propose an ejection fraction of less than 45%, left ventricular end diastolic dimension greater than 2.7 cm/m2 and fractional shortening of <30%.
Risk factors include multiparity, black race, older maternal age, pre-eclampsia, gestational hypertension, maternal cocaine abuse, long term tocolytic therapy and familial etiology. Selenium deficiency leading to PPCM is controversial [4].
The clear mechanism remains not fully understood. Possible etiologies include myocarditis, auto-immune mechanisms, and pregnancy associated hormonal changes against a susceptible genetic background. Recently oxidative stress-cathepsin D-16 k Da prolactin hypothesis has been raised.
The prognosis remains poor despite advances in heart failure therapy with mortality rates ranging from 4 to 80%, this is due in part to the delayed diagnosis [3,5]. There is a possibility of partial or complete recovery of left ventricular function, during the first year. The ejection fraction normalizes in about 50% of surviving patients. In a single centre prospective study of 100 South African patients, 15% died and only 23% recovered normal left ventricular function after 6 months [6]. The recovery phase is not limited to the first 6 - 12 months as continuing improvement can be observed in the second and third years after diagnosis [6].
Predictors for recovery are mainly an initial left ventricular end-diastolic dimension < 56 mm and an ejection fraction > 45% at two months raising thus the need for efficient temporary shortand long-term artificial support for the acute and critically ill patients Medical treatment options include classical heart failure treatment in addition to Bromocriptine, a promising disease specific treatment. Patients refractory to medical therapy and intra-aortic balloon pump (IABP) counterpulsation or in whom weaning from these therapies is impossible, are candidates for a left ventricular assist device (LVAD) as a bridge to recovery or transplant [1]. Extra corporeal membrane oxygenation (ECMO) can be used as a short term temporary support for emergency rescue in patients with refractory cardiogenic shock. Only few reports exist about the place of LVAD and ECMO in severe refractory cardiomyopathy [1].
Let us now have a quick review over the ventricular assist devices.
Ventricular assist device (VAD):
The therapeutic option for severe, symptomatic end stage heart failure despite optimal medical treatment and eventually cardiac resynchronization therapy is heart transplantation, though this option is reserved to eligible young candidates, and requires a long waiting time. The development of VAD aimed to, first keep the patient alive till heart transplantation or as bridge to transplantation, and second as a destination therapy for end stage heart failure patients not eligible to heart transplantation. In the early 1960s, DeBakey developed the first VAD [7]. In Europe nowadays, more VAD systems are implanted than hearts transplant. Despite enormous progress in the field of VAD in the past 50 years, there remain many obstacles yet to be overcome. The old generation VAD consisted on pulsatile flow pumps. New generation Continuous-flow pumps were introduced in the past 13 years, And has revolutionized the management of heart failure, with significantly lower complications than with earlier pulsatile systems and excellent durability [7]. This technological improvement allowed not only saving lives but also improving life quality.
In patients on an LVAD, right ventricular function is crucial. Right ventricular dysfunction (RVD) post implantation has been reported in 5% to 39% of patients [8,9].
The presence of RV failure is defined by the occurrence of two of the following criteria in the first 48 hours after surgery, in the absence of signs of cardiac tamponade [8]:
• Mean arterial pressure < 55 mm Hg;
• Central venous pressure > 16 mm Hg;
• Mixed venous saturation < 55%;
• Cardiac index < 2 liters/min/m2;
• Inotropic support > 20 units;
• Need for an RVAD after LVAD insertion was regarded as a single criterion identifying RV failure.
There is no clear agreement on the best markers of risk for RV failure after LVAD implantation, the mostly studied predictors are tricuspid incompetence and geometry/function of the RV (a ratio between short and long axis > 0.6) [8]
Therapeutic option for patient at high risk to develop RV failure is RV support either temporary, or permanent via Bi VAD or total artificial heart implantation. For many reasons, isolated LVAD support is preferred to biventricular support or total artificial heart placement in patients with end-stage cardiac failure. A study showed no differences in short-term outcome between patients who underwent LVAD implantation with concomitant Tricuspid Valve Repair and those with BVAD implantation [9].
Long term complications of LVAD include:
1) Aortic valve: Unloading the left ventricle, leads to a decrease in the number and extent of aortic valve openings and consequently at long term to a degeneration of the aortic valve with fusion and regurgitation [10]. After 18 months on device support, up to 50% of patients present with moderate or severe aortic regurgitation [11].
2) Coagulation system and bleeding: Anti coagulation is necessary in LVAD implanted patients to overcome potential thrombosis and thromboembolic events, this may in turn cause bleeding complications.
The incidence of serious bleeding of any cause, requiring red blood cell transfusion or necessitating Surgery, with different types of VAD ranges between 0.16 and 2.45 events per patient per year. The incidence of thromboembolic events is 0.05 - 0.28 events per patient per year [12]. Bleeding is mainly related to overdosing in anticoagulant agents, it can also be due to Heparin induced Thromboytopenia or to a deficit in Von Willebrand factor.
Heparin-induced thrombocytopenia (HIT) type II may develop and is caused by platelet activation by heaprin/antiplatelet factor 4 antibodies. The incidence of clinical HIT II approaches 10. When HIT occurs the patient is at higher risk to develop bleeding and/or thrombosis. Alternatively, successful use of bivalirudin has been described. Continuous-flow VADs can also lead to the development of acquired von Willebrand factor (vWF) deficit [13]. Acquired vWF syndrome contributes in part to bleeding episodes observed during support. The mechanism remains not fully understood, it can be related to the interaction between the pump and blood components, due to changes in the shear stress. It has been shown that pump removal increases the levels of vWF.
Additionally, arterio-venous malformations in the gastrointestinal tract—pre-existing or newly developed due to loss of physiological pulsatility during support with continuous flow pumps—may cause gastrointestinal bleeding [14].
Severe hemolysis is another complication following VAD implantation, it may be related to the pump design, malpositioning of the apical cannula, kinking of outflow grafts, or pump thrombosis [15].
3) Malposition of the inflow cannula: With time some movement of the inflow cannula in the LV may occur, mostly towards the lateral Wall leading to partial occlusion of the cannula and subsequently to hemolysis, low pump flow, arrhythmia and inadequate LV unloading, resulting in right ventricular failure [10].
4) Driveline and device infection: Exit site infection develops in most patients within 1 year on support [16]. Most of the cultured organisms are Staphylococcus aureus (27.5% - 35.0%), Corynebacterium (15%) and Pseudomonas aeruginosa (10% - 13.7%). The impact of body weight on the incidence of infection, and in particular on the infection of the driveline, is controversial.
5) Cable damage: Cable damage occurs in 5% - 9% and results from chronic kinking or twisting of the cable [10]. Weight gain may enhance cable damage by slow pulling on or kinking of the cable by the growing abdomen.
6) Psychosocial complications: Some patients develop depression and may commit suicide [17], particularly by disconnecting the pump or cutting the cable.
There are only a few reports on the use of assist devices in the setting of post partum cardiomyopathy. In cases where LVAD acts as bridge to recovery, it will help maintaining the patient alive, allowing the myocardium to recover. Recovery of the left ventricle function in this case is due mainly to recovery of the underlying disease, nevertheless there is now compelling evidence, that near complete unloading of the left ventricle with the use of a left ventricular assist device is associated with structural reverse remodeling that can be accompanied by functional improvement [18-23]. Sufficient recovery of left ventricular function, allowing LVAD explantation, however, is rare and is mainly feasible in patients suffering from acute myocarditis or post partum cardiomyopathy (PPM) [18]. Explantation in this case can be considered if the following criteria are met while the left ventricular assist device is off for 15 minutes: 1—Echocardiographic criteria [18,23]: a left ventricular end diastolic diameter of less than 60 mm, a left ventricular end-systolic diameter of less than 50 mm, a left ventricular ejection fraction (LVEF) of more than 45%, No or maximum grade II mitral and/or aortic valve regurgitation, No RV dilation (RVOT diameter < 35 mm, short-/long-axis ratio < 0.6), and No or maximum grade II tricuspid or pulmonary valve regurgitation. 2—Catheterization criteria: left ventricular end-diastolic pressure (or pulmonary-capillary wedge pressure) of less than 12 mm Hg and Cardiac index > 2.6 L/min/m2.
Long-term results after explantation are favorable (oneand five-year survival rate of 86 and 78%, respectively).
Our patient is an illustrative case of refractory post partum cardiomyopathy requiring LVAD implantation. She did not benefit yet from heart transplantation due to lack of organ donors in our country. The improvement of the left ventricle function in this case raises the question for LVAD explantation, nevertheless the right ventricle remains hypokinetic. Future follow up will tell us whether this case will end out as a bridge to transplantation, destination therapy, or to LVAD explantation.
4. Conclusion
In conclusion, peripartum cardiomyopathy is a potentially life threatening obstetric emergency that can be rapidly and highly fatal if not correctly diagnosed and early and aggressively treated. We reported the case of a severe dilated post partum cardiomyopathy refractory to medical treatment and intra aortic balloon counter pulsation; it was successfully treated by the implantation of a LVAD. Temporary ventricular support, instead of immediate heart transplantation, is becoming the cornerstone of treatment in severe post partum cardiomyopathy, both with short term (ECMO) therapy as a bridge to LVAD, or with long term (LVAD) therapy as a bridge to recovery or to transplantation.
REFERENCES
- S. Gevaert, Y. Van Belleghem, S. Bouchez, Herck, F. De Somer, Y. De Block, F. Tromp, E. Vandecasteele, F. Martens and M. De Pauw, “Acute and Critically Ill Peripartum Cardiomyopathy and ‘Bridge to’ Therapeutic Options: A Single Center Experience with Intra-Aortic Balloon Pump, Extra Corporeal Membrane Oxygenation and Continuous-Flow Left Ventricular Assist Devices,” Critical Care, Vol. 15, No. 2, 2011, p. R93. doi:10.1186/cc10098
- J. G. Demakis and S. H. Rahimtoola, “Peripartum Cardiomyopathy,” Circulation, Vol. 44, No. 5, 1971, pp. 964-968. doi:10.1161/01.CIR.44.5.964
- A. M. Amos, W. A. Jaber and S. D. Russell, “Improved Outcomes in Peripartum Cardiomyopathy with Contemporary,” American Heart Journal, Vol. 152, No. 3, 2006, pp. 509-513. doi:10.1016/j.ahj.2006.02.008
- J. D. Fett, A. A. Ansari, J. B. Sundstrom and G. F. Combs, “Peripartum Cardiomyopathy: A Selenium Disconnection and an Autoimmune Connection,” International Journal of Cardiology, Vol. 86, No. 2-3, 2002, pp. 311-316. doi:10.1016/S0167-5273(02)00359-5
- J. Abboud, Y. Murad, C. Chen-Scarabelli, L. Saravolatz and T. M. Scarabelli, “Peripartum Cardiomyopathy: A Comprehensive Review,” International Journal of Cardiology, Vol. 118, No. 3, 2007, pp. 295-303. doi:10.1016/j.ijcard.2006.08.005
- M. Diao, I. B. Diop and A. Kane, “Electrocardiographic Recording of Long Duration (Holter) of 24 Hours during Idiopathic Cardiomyopathy of the Peripartum,” Archives des Maladies du Coeur et des Vaisseaux, Vol. 97, No. 1, 2004, pp. 25-30.
- E. V. Potapov, T. Krabatsch, H. O. Ventura and R. Hetzer, “Advances in Mechanical Circulatory Support: Year in Review,” Journal of Heart and Lung Transplantation, Vol. 30, No. 5, 2011, pp. 487-493. doi:10.1016/j.healun.2011.01.703
- E. V. Potapov, A. Stepanenko, M. Dandel, M. Kukucka, H. B. Lehmkuhl, Y. Weng, F. Hennig, T. Krabatsch and R. Hetzer, “Tricuspid Incompetence and Geometry of the Right Ventricle as Predictors of Right Ventricular Function after Implantation of a Left Ventricular Assist Device,” Journal of Heart and Lung Transplantation, Vol. 27, No. 12, 2008, pp. 1275-1281. doi:10.1016/j.healun.2008.08.012
- E. V. Potapov, M. Schweiger, A. Stepanenko, M. Dandel, M. Kukucka, J. Vierecke, R. Hetzer and T. Krabatsch, “Tricuspid Valve Repair in Patients Supported with Left Ventricular Assist Devices,” ASAIO Journal, Vol. 57, No. 5, 2011, pp. 363-367. doi:10.1097/01.MAT.0000398944.12757.eb
- E. V. Potapov, A. Stepanenko, T. Krabatsch and R. Hetzer, “Managing Long-Term Complications of Left Ventricular Assist Device Therapy: Review,” Current Opinion in Cardiology, Vol. 26, No. 3, 2011, pp. 237-244. doi:10.1097/HCO.0b013e328345af80
- J. Cowger, F. D. Pagani, J. W. Haft, et al., “The Development of Aortic Insufficiency in Left Ventricular Assist Device-Supported Patients,” Circulation: Heart Failure, Vol. 3, 2010, pp. 668-674. doi:10.1161/CIRCHEARTFAILURE.109.917765
- M. S. Slaughter, F. D. Pagani, J. G. Rogers, et al., “Clinical Management of Continuous-Flow Left Ventricular Assist Devices in Advanced Heart Failure,” Journal of Heart and Lung Transplantation, Vol. 9, No. 4S, 2010, pp. S1-S39. doi:10.1016/j.healun.2010.01.011
- S. Crow, D. Chen, C. Milano 3rd, et al., “Acquired von Willebrand Syndrome in Continuous-Flow Ventricular Assist Device Recipients,” The Annals of Thoracic Surgery, Vol. 90, No. 4, 2010, pp. 1263-1269. doi:10.1016/j.athoracsur.2010.04.099
- G. V. Letsou, N. Shah, I. D. Gregoric, et al., “Gastrointestinal Bleeding from Arteriovenous Malformations in Patients Supported by the Jarvik 2000 Axial-Flow Left Ventricular Assist Device,” Journal of Heart and Lung Transplantation, Vol. 24, No. 1, 2005, pp. 105-109. doi:10.1016/j.healun.2003.10.018
- C. Heilmann, U. Geisen, C. Benk, et al., “Haemolysis in Patients with Ventricular Assist Devices: Major Differences between Systems,” European Journal Cardio-Thoracic Surgery, Vol. 36, No. 3, 2009, pp. 580-584. doi:10.1016/j.ejcts.2009.04.015
- A. Zierer, S. J. Melby, R. K. Voeller, et al., “Late-Onset Driveline Infections: The Achilles’ Heel of Prolonged Left Ventricular Assist Device Support,” The Annals of Thoracic Surgery, Vol. 84, No. 2, 2007, pp. 515-520. doi:10.1016/j.athoracsur.2007.03.085
- K. Tigges-Limmer, M. Schonbrodt, D. Roefe, et al., “Suicide after Ventricular Assist Device Implantation,” Journal of Heart and Lung Transplantation, Vol. 29, No. 6, 2010, pp. 692-694. doi:10.1016/j.healun.2009.12.005 L. Oosterom, N. de Jonge, J. Kirkels and C. Klöpping, “Lahpor. Left Ventricular Assist Device as a Bridge to Recovery in a Young Woman Admitted with Peripartum Cardiomyopathy,” Netherlands Heart Journal, Vol. 16, No. 12, 2008, pp. 426-428.
- D. Mancini, A. Beniaminovitz, H. Levin, K. Catanese, M. Flannery, M. DiTullio, et al., “Low Incidence of Myocardial Recovery after Left Ventricular Assist Device Implantation in Patients with Chronic Heart Failure,” Circulation, Vol. 98, 1998, pp. 2383-2389. doi:10.1161/01.CIR.98.22.2383
- E. Birks, P. Tansley, J. Hardy, R. George, C. Bowles, M. Burke, et al., “Left Ventricular Assist Device and Drug Therapy for the Reversal of Heart Failure,” The New England Journal of Medicine, Vol. 355, No. 18, 2006, pp. 1873-1884. doi:10.1056/NEJMoa053063
- S. Maybaum, D. Mancini, S. Xydas, R. Starling, K. Aaronson, F. Pagani, et al., “Cardiac Improvement during Mechanical Circulatory Support/A Prospective Multi Center Study of the LVAD Working Group,” Circulation, Vol. 115, No. 19, 2007, pp. 2497-2505. doi:10.1161/CIRCULATIONAHA.106.633180
- M. Simon, R. Kormos, S. Murali, P. Mair, M. Heffernan, J. Gorcsan, et al., “Myocardial Recovery Using Ventricular Assist Devices/Prevalence, Clinical Characteristics, and Outcomes,” Circulation, Vol. 112, No. S1, 2005, pp. I-32-I-36.
- M. Dandel, Y. Weng, H. Siniawski, A. Stepanenko, T. Krabatsch, E. Potapov, H. Lehmkuhl, C. Knosalla and R. Hetzer, “Heart Failure Reversal by Ventricular Unloading in Patients with Chronic Cardiomyopathy: Criteria for Weaning from Ventricular Assist Devices,” European Heart Journal, Vol. 32, No. 9, 2011, pp. 1148-1160. doi:10.1093/eurheartj/ehq353
NOTES
*We state that the patient has given her consent for the Case reports to be published. We state non competing interests.
#Corresponding author.

