Open Journal of Obstetrics and Gynecology
Vol.4 No.2(2014), Article ID:43021,5 pages DOI:10.4236/ojog.2014.42017
Clinical and investigative correlates of etiologic risk factors on treatment outcome of intrauterine adhesion in women with infertility: A descriptive study
![]()
1Department of Obstetrics & Gynaecology, Ahmadu Bello University Teaching Hospital, Zaria, Nigeria
2Medical Imaging Ghana Limited, Accra, Ghana
3Department of Obstetrics and Gynaecology, Benue State University, Makurdi, Nigeria
Email: biyi.adesiyun@yahoo.com
Copyright © 2014 Adebiyi Gbadebo Adesiyun et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. In accordance of the Creative Commons Attribution License all Copyrights © 2014 are reserved for SCIRP and the owner of the intellectual property Adebiyi Gbadebo Adesiyun et al. All Copyright © 2014 are guarded by law and by SCIRP as a guardian.
Received 12 November 2013; revised 10 December 2013; accepted 18 December 2013
ABSTRACT
Background: Intrauterine adhesion is a clinical entity that may present with subfertility. However, outcome of management depends on severity of intrauterine adhesion and type of treatment intervention employed. Objective: To evaluate clinical and investigative correlation of etiologic risk factors of intrauterine adhesion on fertility and pregnancy outcome following treatment. Patients and Methods: A 5 years prospective observational study. Treatment employed includes transvaginal blind intrauterine adhesiolysis, insertion of inert intrauterine device or inflated Foley’s catheter balloon and oestrogen therapy. Inclusion criteria are intrauterine adhesion as the only identifiable cause of infertility and post treatment follows up for at least a year. Results: Over a period of 5 years, 63 patients with mean age of 31.6 years and age range of 21 to 42 years were managed. Etiologic risk factors were dilatation and curettage 33 (52.4%), vacuum aspiration 13 (20.6%), myomectomy 11 (17.5%) and caesarean section in 6 (9.5%) patients. Of the 63 patients, 28 conceived giving a pregnancy rate of 44.4%. Nine out of the 28 patients that conceived had miscarriage, giving a miscarriage rate of 32.1%. The highest pregnancy rate and lowest miscarriage rate were recorded in the subgroup that had vacuum aspiration as their etiologic risk factor. Late pregnancy complications encountered are preterm contractions 5 (26.3%), placenta praevia 4 (21.1%), morbidly adherent placenta 5 (26.3%) and preterm delivery in 2 (10.5%) patients. Route of delivery was per vaginum in 13 (68.4%) patients and by caesarean section in 6 (31.6%) patients. Live birth rate was 89.5% (17/19 deliveries). There was no maternal mortality recorded. Conclusion: Compared to other risk factors, uterine vacuum aspiration was associated with higher fertility rate and better pregnancy outcome.
KEYWORDS
Intrauterine Adhesion; Infertility; Risk Factor; Pregnancy Outcome
1. INTRODUCTION
Intrauterine adhesion (IUA) is a known clinical entity that could present with female infertility. It results when adhesion partially or completely obliterates the endometrial cavity, the internal cervical os or the cervical canal individually or as a whole [1]. These are sequelae to uterine trauma which is almost always related to pregnancy [1]. Infections like tuberculosis and pelvic inflammatory disease should however be considered if there was no antecedent history of trauma. Trauma in the form of overzealous curettage of a pregnant or recently pregnant uterus is a common aetiologic factor of IUA in the developing world [2]. The immeasurable advantages of vacuum aspiration (VA) over traditional dilatation and curettage (D & C) are documented. Dilatation and curettage are less safe [3] and more painful [4] for women than the VA.
In the treatment of IUA, the aims are to restore the size and shape of the uterine cavity, to return normal endometrial/menstrual functions, and to make pregnancy possible. Treatment outcome is however related to the extent of intrauterine adhesions, which has been classified based on hysterographic findings [5,6] and hysteroscopic findings [7,8].
This study sought to find if any, the impact of etiologic risk procedures on fertility and pregnancy outcome following treatment of IUA in a resource constrained setting.
2. METHODS
Between July 2003 and July 2008, 63 infertile patients were managed for varying severity of intrauterine adhesions at either Ahmadu Bello University Teaching Hospital, 345 Aeromedical Hospital or Alba Hospital, all in Kaduna city, Northern Nigeria.
This was a prospective observational study. The patients presented with infertility and history suggestive of IUA. Diagnosis of IUA was based on hysterographic findings of intrauterine filling defects and irregularity of the outlined uterine cavity using water soluble medium. Inclusion criteria was IUA as the only identifiable cause of infertility, absence of conception following the etiologic risk procedure and post treatment follow up for at least a year.
In this study, blind adhesiolysis, insertion of inert lippes loop intrauterine device (IUD) or inflated Foley’s catheter balloon and oestrogen therapy was the treatment modality offered. The surgery was a day case procedure performed with short acting intravenous anesthetic agent like ketamine hydrochloride and sodium thiopentone. Ergometrine was given before the commencement of the procedure, so as to decrease the likelihood of uterine perforation. Cervical dilatation was performed in patients with cervical stenosis, followed by assessment of uterine cavity length using a uterine sound. Intrauterine adhesiolysis was accomplished with uterine curette; this was followed by re-assessment of uterine cavity and insertion of IUD or Foley’s catheter with the balloon inflated. Prophylactic antibiotic was given post-operatively. Sequential oestrogen and progesterone was given for three cycles post-surgery. The first cycle of treatment commenced on the first day post-surgery. Inflated Foley’s catheter balloon was removed between ten and fourteen days post-surgery and inert IUD removed following three normal menstrual cycles/flow. The patients were subsequently followed up for a minimum of one year. In this study, treatment success was measured by pregnancy.
The patients were divided into four groups:
Group A: IUA following vacuum aspiration of the uterine cavity.
Group B: IUA following dilatation and uterine curettage.
Group C: IUA following caesarean section.
Group D: IUA following myomectomy In this study, hysterographic semi-quantitative evaluation and assessment of the defects as proposed by Toaff [5] was used. The gradings from grade 1 to grade 4 are as follows:
Grade 1: A single, filling defect, frequently well inside the uterine cavity, occupying up to about one-tenth of the uterine area.
Grade 2: A single, medium-sized filling defect occupying up to one-fifth of the uterine area, or several smaller defects adding up to the same degree of involvement, located inside the uterine cavity, whose outline may show minor indentations but no gross deformation.
Grade 3: A single, large, or several smaller filling defects involving up to about one-third of the uterine cavity, which is deformed or asymmetrical because of marginal adhesions.
Grade 4: Large-sized filling defects occupying most of a several deformed uterine cavity For this study, grade 1 IUA was referred to as mild IUA, grade 2 as moderate IUA and grade 3 and 4 as severe IUA.
3. RESULTS
Over a 5 years period (July 2003 to June 2008), 63 infertile women were managed with IUA as the only identifiable cause of infertility. Mean age of patients was 31.6 years with age range of 21 to 42 years. The most common etiologic risk procedure was D&C in 33 (52.45%) patients, followed by VA 13(20.6%), myomectomy 11 (17.5%) and C/S in 6(9.5%) patients (Table 1).
In subgroup A, that had VA as the etiologic risk procedure, of the 13 patients, incomplete abortion was the commonest indication in 5 (38.5%) patients. Other indications were missed abortion 3 (23.1%), induced abortion 2 (15.4%), post vaginal delivery 2 (15.4%) and post caesarean section 1 (7.7%) retained product of conception. In subgroup B with D&C as the etiologic risk procedure, of the 33 patients, incomplete abortion in 13 (39.4%) patients ranked the highest indication, followed by induced abortion 8 (24.2%), post vaginal delivery RPOC 6 (18.2%), missed abortion 5 (15.2%) and post caesarean section RPOC in 1 (3.0%) patient. Amongst the 6 patients with C/S as the etiologic risk procedure (subgroup C), prolong obstructed labour was the most common indication occurring in 4 (66.7%) patients while uterine fibroid with infertility and menorrhagia as complications 5 (45.5%) was the commonest indication for myomectomy in subgroup D (Table 2).
Table 2 shows that VA (subgroup A) mostly (76.7%) resulted in grade 1 hysterographic adhesions while D&C (subgroup B) was mostly associated (54.5%) with grade 2 IUA. Caesarean section (subgroup C) 83.3% and myomectomy (subgroup D) 72.5% were mainly associated with grade 3 and 4 IUA. Pregnancy rate was highest in subgroup A (VA), with a rate of 76.9% and lowest
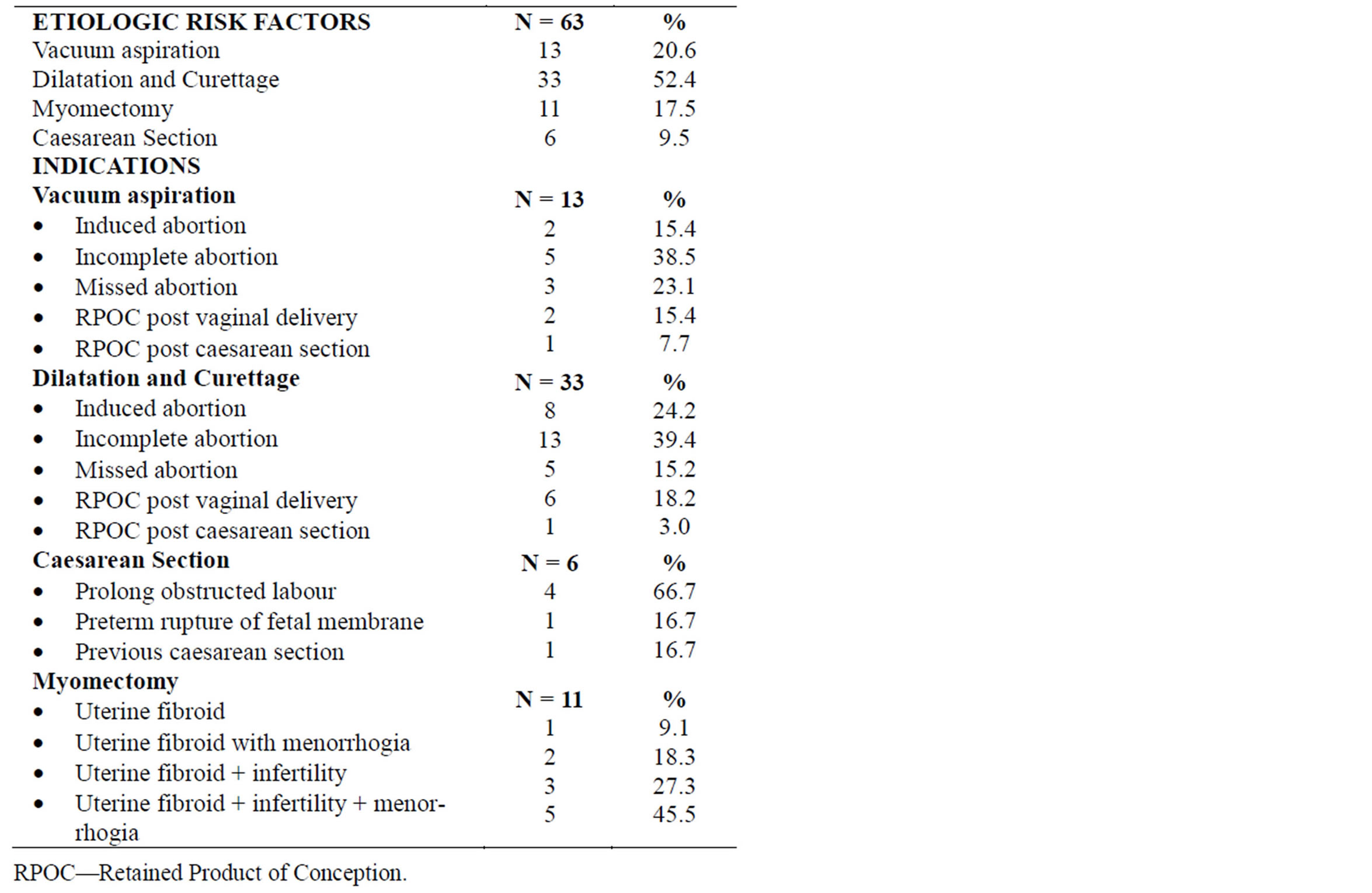
Table 1. Etiologic risk factors.
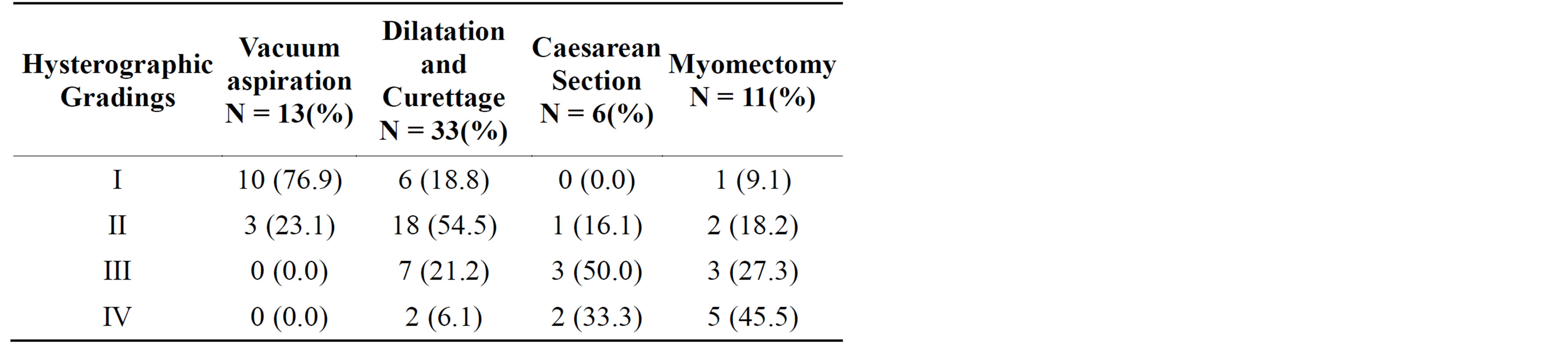
Table 2. Etiologic risk factors and hysterographic grading of intrauterine adhesions.
in subgroup D (myomectomy) 27.3%. Miscarriage rate was highest (100%) in subgroup C (C/S) and D (myomectomy). In tables 3 and 4, pregnancy rate was the highest and there was no miscarriage in patients with mild (grade 1) IUA.
Complications encountered during pregnancy and delivery were preterm contraction 5(26.3%), placenta praevia 4 (21.1%), morbidly adherent placenta 5 (26.3%) and preterm delivery in 2 (10.5%) patients. Live birth rate was 89.5 percent (Table 5).
4. DISCUSSION
Intrauterine adhesion is characterized by variable obliteration of the uterine cavity and may present with menstrual abnormalities, infertility, and habitual abortion. In Nigeria, infertility was reported to be associated with IUA in one fifth of patients seeking treatment for subfer-

Table 3. etiologic risk factors versus pregnancy and miscarriage rates.

Table 4. hysterographic grading of intrauterine adhesion versus pregnancy and miscarriage rates.
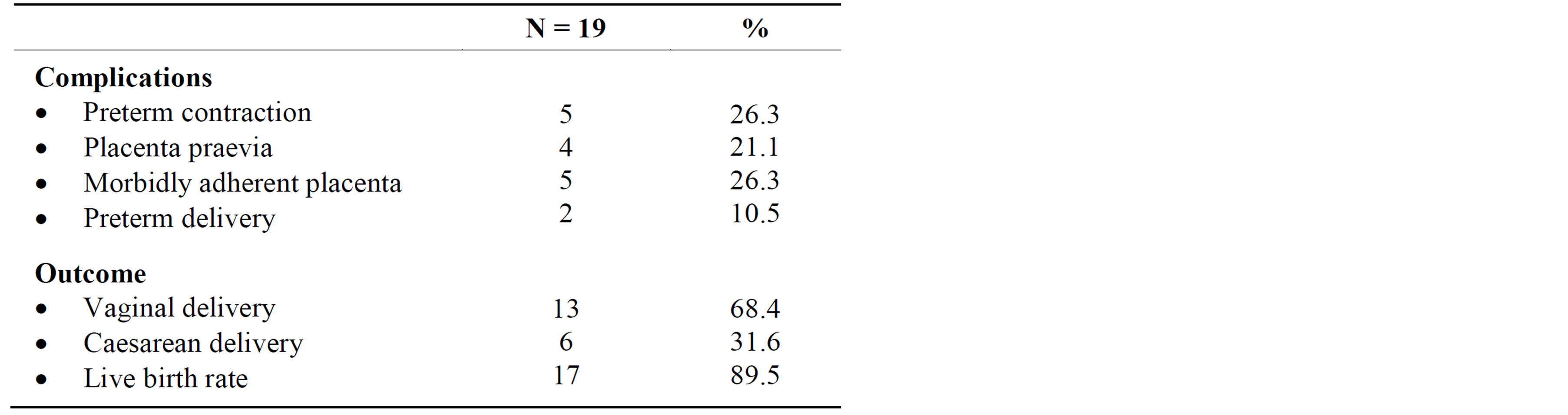
Table 5. pregnancy complications and delivery outcome.
tility [9,10]. The pathogenesis of IUA is still not fully understood, but trauma which can complicate all the etiologic risk procedures found in this study is a common denominator. Vacuum aspiration is documented to be safer than D&C, the rates of major complications associated with D&C are two to three times higher than those of VA [4]. The role of infection in the pathogenesis of IUA is inconclusive, however clinical infection rate of 26% was reported in cases of IUA [11]. Especially in resource constrained setting, infection is a possible complication of all the etiologic risk procedures found in this study.
In this series, diagnosis of IUA was based on clinical presentation and hysterographic findings. However, authors [12] have reported poor correlation between radiographic findings with those at hysteroscopy in some cases. False positive findings may be associated with hysterosalpingographic diagnosis of IUA, as seen in cases of submucous leiomyoma, endometrial polyps, uterine septae, physiologic contractions and air bubbles. Although hysteroscopic evaluations are more reliable, especially in diagnosing cervical lesions, it is however an expensive and invasive procedure that may require general anesthesia. These attributes make it unpopular in a resource poor setting like ours. The same applies to magnetic resonance imaging, which can also be employed in the diagnosis of IUA [13].
There are several treatment modalities that can be employed in the management of AS. Lysis of intrauterine adhesion can be achieved by cervical dilatation, curettage, hysteroscopic scissors, electro or laser energy. Traditional dilatation and curettage are a blind procedure with attendant risk of perforation and creation of false routes. Hysteroscopic adhesiolysis is the safest and least traumatic, and it is currently considered as the standard management for AS [14,15]. Hysteroscopy is however expensive, requiring general anaesthesia and it is not universally available. Pressure lavage under ultrasound guidance (PLUG), is a safe and ideal office procedure for treating mild cases of AS, which may reduce the need for hysteroscopic treatment [16]. A new hysterosocpic technique, myometrial scoring was introduced for the treatment of dense intrauterine adhesion and markedly contracted uterine cavity [17]. It involves longitudinal cuts in the endometrium. Ikeda [18] described a useful technique in the lysis of mild intrauterine adhesion, using continuous ongoing instillation of iodine contrast medium through an insemination catheter; however the radiation dose may be unacceptably high in patients with more extensive disease. Other treatment modalities that may be performed for severe disease are laparotomic hysterotomy with transfundal adhesiolysis and fallopian tube transplant. A patient in subgroup C in this series had hysterotomy and intrauterine adhesiolysis which was not successful due to total obliteration of the uterine cavity with dense scar tissue.
Uterine splinting to keep walls apart and prevent recurrence of adhesion can be accomplished using inert IUD and balloon catheter as employed in this study. Also drains and polythene tubing may be used. In this study, endometrial regeneration was achieved with oestrogen preparation. Sildenafil may be used in patients who fail to form adequate endometrium despite hormonal treatment [19]. Sildenafil potentiates the vasodilator effect of nitric oxide, leading to increase uterine perfusion and endometrial regeneration. Other forms of treatment that may be employed in cases of failed/poor endometrial regeneration are use of donor endometrium, fetal membranes, deciduas and placenta. Amnion graft is a promising technique for encouraging endometrial regeneration [20]. Auto-crossed linked hyaluronic acid gel has been tried in the prevention of IUA, but it has been found not to reduce the incidence and severity of intrauterine adhesion after hysteroscopic surgery [21].
Success of treatment is directly related to the extent and severity of adhesion. In this study, patients in subgroup A and to a lower extent subgroup B were found to have mild adhesion at hysterographic assessment, while those in subgroup C and D had mainly severe IUA. This translates to high pregnancy rate and low miscarriage rate recorded in subgroup A and B. Overall pregnancy rate of 44.4% recorded in this study falls below reported range of 70% - 80% from other authors [22]. However, pregnancy rate of 86.7% recorded in patients with mild IUA (Grade 1) is similar to rate which is higher than 80% reported among patients treated for mild to moderate IUA [23]. An impressive live birth rate recorded in this study is similar to 87.2% reported with hysteroscopic lysis [24]. Low pregnancy complications recorded in this study may not be unrelated to mild IUA that most patients delivered had, although March [24] in his series did not record cases of placenta accreta and manual removal of placenta in his series following treatment with hysteroscopic lysis.
Remarkable in this series are the findings that VA was mostly associated with mild IUA and better treatment outcome. Introduction and training on diagnostic and therapeutic hysteroscopy in resource constrained setting will improve treatment outcome especially in those with severe IUA. Training and retraining of health workers on the use of VA would decrease the use of D&C in cases where VA is appropriate and would consequently minimize complications like IUA from both D&C and VA procedure.
REFERENCES
- Toaff, R. and Ballas, S. (1978) Traumatica hypomenorrhoea—Amenorrhoea (Asherman’s syndrome). Fertility and Sterility, 30, 379-387.
- Ogedendge, O.K., Giwa-Osagie, O.F., Adedeji, O.F. and Oyeyinka, O. (1991) Intrauterine adhesions in Lagos Nigeria. Journal of Obstetrics & Gynaecology, 11, 134-136. http://dx.doi.org/10.3109/01443619109013538
- Cates, W., Grimes, D.A. and Schultz, K.F. (2000) Abortion surveillance at CDC: Creating public health light out of political heat. American Journal of Preventive Medicine, 19, 12-17. http://dx.doi.org/10.1016/S0749-3797(00)00168-9
- Grimes, D., Schultz, K.F., Cates, W. and Tyler, C.W. (1977) The joint program for the study of abortion CDC —A preliminary report. In: Hern, W. and Andrikopolous, B., Eds., Abortion in the seventies, National Abortion Federation, New York, 41-46.
- Toaff, R. (1962) Amenorrhoea hypomerrhoea traumatic (Sindrome di Asherman). Atti de la Societa Italiana di Ginecol, 49, 258.
- Toaff, R. and Krochik, N. (1963) Le traitement des synechies uterines post traumatiques (syndrome d’ Asherman. Comptes Rendus de la Societe Francaise de Gynecologie, 5, 323.
- March, C.M., Israel, R. and March, A.D. (1978) Hysteroscopic management of intrauterine adhesions. American Journal of Obstetrics & Gynecology, 130, 653-657.
- Wamsteker, K. and DeBlok, S. (1993) Diagnostic hysteroscopy: Technique and documentation. In: Sutton, C. and Diamond, M., Eds., Endoscopic surgery for gynaecologists, Saunder, London, 263-276.
- Giwa-Osagie, O.F. and Emuveyan, E.E. (1968) Evaluation of secondary amenorrhea. Nigerian Medical Practitioner, 7, 79-83.
- Otubu, J.A.M. and Olanrewaju, R.S. (1989) Hysteroscopy in infertile Nigerian Women. African Journal of Medicine & Medical Sciences, 18, 117-120.
- Palter, F. (2003) Poly spyrou. Asherman’s syndrome: Etiologic factors, patterns of pregnancy loss and treatment results. Results from an international registry. Fertility and Sterility, 80, 26-37. http://dx.doi.org/10.1016/S0015-0282(03)01900-9
- March, C.M. and Israel, R. (1976) Intrauterine adhesions secondary to elective abortion. Hysterscopic diagnosis and management. Obstetrics & Gynecology, 48, 422-424.
- Letterie, G.S. and Haggerty, M.F. (1994) Magnetic resonance imaging of intrauterine synechiae. Gynecologic and Obstetric Investigation, 37, 66-68. http://dx.doi.org/10.1159/000292525
- March, C.M. (1995) Intrauterine adhesions. Obstetrics & Gynecology Clinics of North America, 22, 491-505.
- Schenker, J.G. (1996) Etiology of and therapeutic approach to synechic uteri. European Journal of Obstetrics & Gynecology and Reproductive Biology, 65, 109-113. http://dx.doi.org/10.1016/0028-2243(95)02315-J
- Coccia, M.E., Becattini, C., Bracco, G.L., Pampaloni, F., Bargelli, G. and Scarselli, G. (2001) Presuure lavage under ultrasound guidance: A new approach for outpatient treatment of intra-uterine adhesions. Fertility and Sterility, 75, 601-606. http://dx.doi.org/10.1016/S0015-0282(00)01770-2
- Protopapas, A., Shushan, A. and Magos, A. (1998) Myometrical scoring: A new technique for the management of severe Asherman’s syndrome. Fertility and Sterility, 69, 860-864. http://dx.doi.org/10.1016/S0015-0282(98)00036-3
- Ikeda, I., Morita, A., Inamura, A. and Mori, I. (1981) The separation procedure for intrauterine adhesions (synechia uteri) under roentgenographic view. Fertility and Sterility, 36, 333-338.
- Zinger, M., Thomas, M.A. and Liu, J.H. (2001) Vaginal sildenafil (Viagra) improves endometrium in Asherman’s syndrome. Fertility and Sterility, 76, 255. http://dx.doi.org/10.1016/S0015-0282(01)02765-0
- Mohammed, I.A. and Karim, H.A. (2006) Amnion graft following hysteroscopic lysis of intrauterine adhesion. Journal of Obstetrics and Gynaecology Research, 32, 559-566. http://dx.doi.org/10.1111/j.1447-0756.2006.00454.x
- Ducarme, G., Davition, C., Zarrouk, S., Uzan, M. and Poncelet, C. (2006) Interest of autocross linked hyaluronic acid gel in the prevention of intrauterine adhesions after hysteroscopic surgery. A case controlled stydy. Journal de Gynécologie Obstétrique et Biologie de la Reproduction, 35, 691-695. http://dx.doi.org/10.1016/S0368-2315(06)76465-1
- Speroff, L. and Fritz, M.A. (2005) Amenorrhoea. In: Clinical gynaecologic endocrinology and infertility, 7th Edition, Lippincott Williams and Wilkins, Philadelphia, 401-463.
- Ismajovich, B., Lidos, A., Confino, E., et al. (1985) Treatment of minimal and moderate intrauterine adhesions (Asherman’s syndrome). Journal of Reproductive Medicine, 30, 769-772.
- March, C.M. and Israel, R. (1981) Gestational outcome following hysteroscopic lysis of adhesions. Fertility and Sterility, 36, 455-459.

