Open Access Library Journal
Vol.02 No.07(2015), Article ID:68503,4 pages
10.4236/oalib.1101467
Congenital Lesions of Tip of Nose: Report of Two Cases with Review
Snigdha Goyal1*, Sunder Goyal2, Isha Saini2, Amit Jain3
1Department of Pathology, Dr. RML Postgraduate Institute of Medical Sciences, New Delhi, India
2Department of Surgery, Kalpana Chawla Government Medical College, Karnal, India
3Department of Surgery, Mewat Medical College, Mewat, India
Email: *drgoyal4@gmail.com
Copyright © 2015 by authors and OALib.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/


Received 1 July 2015; accepted 17 July 2015; published 22 July 2015

ABSTRACT
Tip of nose is most prominent part of the face. It has an aesthetic importance as well as influence on the psyche of children. Midline congenital lesions like dermoid cyst and haemangioma confined to the tip of nose are rare. Being midline structure of body congenital condition like dermoid cyst occurs due to the sequestration of the skin along the lines of embryonic closure. Haemangioma is another common congenital lesion of face in childhood. But haemangioma confined only to tip of nose is uncommon. We present these two uncommon congenital lesions of tip of nose.
Keywords:
Congenital, Tip of Nose, Dermoid, Haemangioma
Subject Areas: Pediatrics, Surgery & Surgical Specialties

1. Introduction
Midline congenital lesions of the tip of nose are uncommon congenital abnormalities. Their incidence is estimated at 1 per 20,000 to 40,000 births. Cause of swelling at the tip of nose may be inflammatory, post-traumatic, neoplastic or vascular. Gliomas, encephaloceles and nasal dermoid sinus cysts or dermoid cysts are the main congenital midline lesions of the nose. The term nasal dermoid sinus cysts (NDSC) was first used in 1982 for the congenital lesions which developed from ectoderm and mesoderm. Nasal dermoids are usually infrequent, although familial cases have been reported [1] .
Vascular lesions like haemangiomas of face are common but confined to nasal tip are rare. Incidence of hemangiomas in total population is about 4% - 10% [2] . In facial hemangiomas, in 15.8% of cases nose is involved where as the nasal tip is affected in about 5.1% of cases [1] . Female to male ratio is 3:1. We present one case of nasal tip dermoid and another case of nasal haemangioma due to clinical rarity.
2. Case Report
2.1. 1st Case
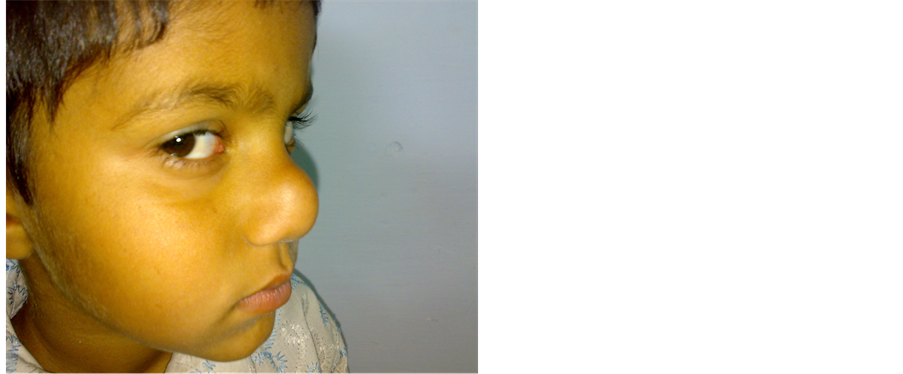
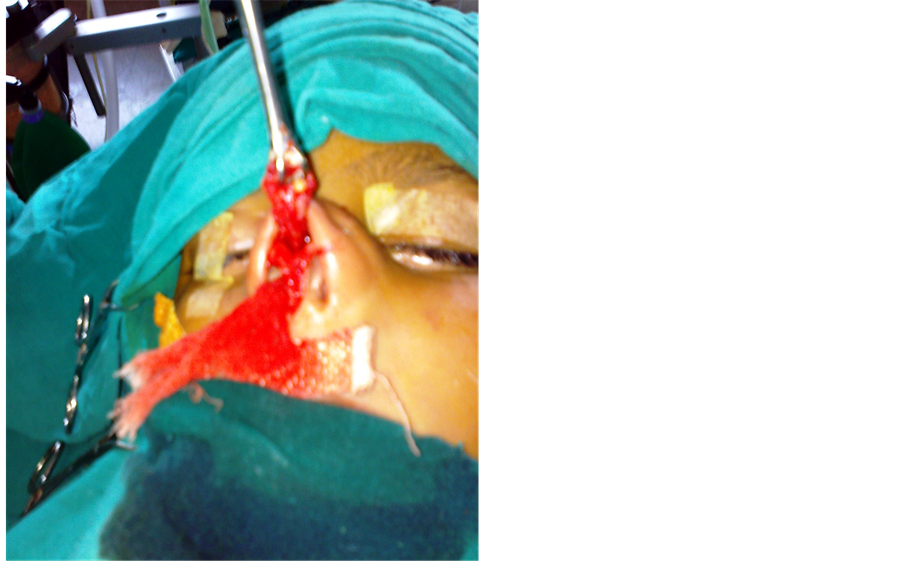
Six years male child presented with painless, gradually increasing swelling at the tip of nose since birth. On examination, there was a single, non tender, smooth, well defined cystic swelling present at the tip of nose. Overlying skin was not adherent (Figure 1). A clinical diagnosis of nasal dermoid cyst was made. Open rhinoplasty approach was used. Nasal dorsum skin was lifted up. Cyst was dissected and total excision of cyst was done (Figure 2) and send for histopathology. Histopathology slide revealed dermoid cyst (Figure 3). Postoperative period was uneventful.
Figure 1. Showing dermoid cyst of nasal tip.
Figure 2. Showing trans-septal removal of cyst.
Figure 3. Histopathology slide showing dermoid cyst.
2.2. 2nd Case
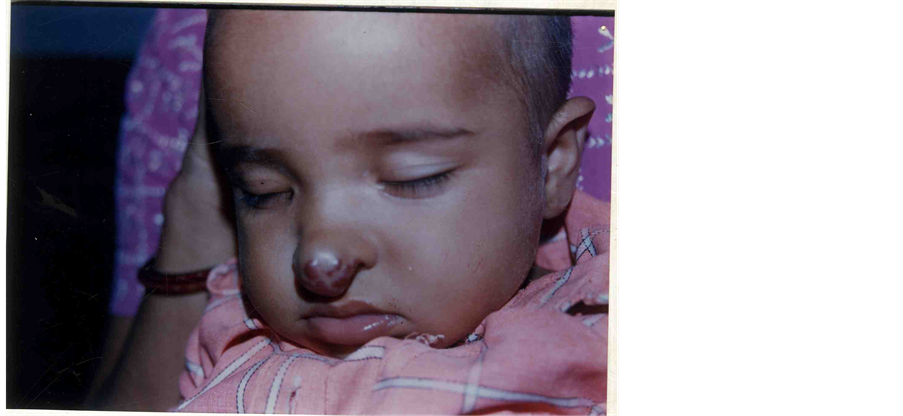
4 years old child presented with a reddish purple colored gradually progressing swelling over the tip of nose since birth. Swelling increased in size at a faster rate since 1 year. On examination, there was a reddish purple color, single, nontender compressible swelling at tip of nose (Figure 4). Clinical diagnosis of haemangioma at tip of nose was made. Patient was managed with intralesional Injection bleomycin and syrup propanolol. A short course of prednisolone was also given. Patient responded well. Size and color of swelling reduced with treatment.
3. Discussion
The tip of the nose is most conspicuous portion of the face. It is an important functional and aesthetic organ which has got a psychological influence in life. As nasal tip is highly noticeable area of face, onlooker stares at tip of nose for the maximum time [4] . Nasal dermoid cysts in a nasal tip location are rare, but they may produce social and psychologic problems in children [5] . Congenital lesions of the midline should always be approached with caution because failure to identify and early management of these dermoid cysts may cause a progressive skeletal distortion and/or recurrent infection with a potential for meningitis or cerebral abscess.
The first report about Nasal dermoid sinus cyst (NDSC) was published in 1890. There are various theories like sequestration, trilaminary and prenasal, about NDSCs .The most accepted theory for pathogenesis of nasal dermoid sinus cyst (NDSC) is that of presnasal theory by Prattand the cranial theory by Bradley [6] . There is a common embriologic pathway of gliomas, encephaloceles and naso-frontal dermoid sinus tract. During the extension of dura between the unconnected bones in the skullbase to nasal region the dura is related with dermis in the nasal tip. If the bone tissue could not separate the dura from dermis during the ossification, anomalies occur [1] .
Nasal dermoid cysts consist of both ectodermal and mesodermal elements, including hair follicles, sweat glands and sebaceous glands. They are probably embryologically related to nasal gliomas and nasal encephaloceles and all the three can occur as a result of an anterior skull base defect [7] . Nasal dermoid cyst can present as midline mass, sinus tracts, or as a combination of the two. They are usually diagnosed within the first 3 years of life and account for 1% - 3% of all dermoid cysts. They account for 4% - 12% of head and neck dermoid cysts.
Commonly, nasal dermoid sinus cyst (NDSC) presents as a firm, non-compressible, non-pulsatile lumps or a “furuncle like” lesion on the midline of the nose. They are usually present at birth and may appear anywhere along the nasal midline from the glabella to the nasal tip [8] .
Most of the time there is keratinous material discharge on squeezing the lesion. In about 50% cases, they may present with intermittent discharge of sebaceous material. The main cause of worry in a case of nasal dermoid sinus cyst is the possible communication between the dermoid cyst to the skull base or the anterior cranial fossa through abnormal foramen caecum [9] . In about 20% - 45% of cases nasal dermoid cysts have an intracranial connection [7] . A blind probing should not be attempted in a case of NDSC due to possibility of intracranial communicating tract from the dermoid sinus cyst, which can lead to meningitis. These cysts do not get bigger on crying or with Valsalva maneuver. These lesions are common over the lower third of the nasal bridge.
Figure 4. Showing haemangioma at nasal tip.
The differential diagnosis for midline nasal swelling includes nasal gliomas, nasal encephalocele, congenital heamangiomas, and epidermoid cyst [10] [11] . Nasal encephalocele presents a soft compressible bluish swelling which changes in size on crying or straining (Valsalva maneuver) and shows transillumination due to its cerebrospinal fluid content [6] .
Imaging modalities like computed tomography (CT) and magnetic resonance imaging (MRI) are useful in diagnosis of dermoid cyst along with nasal encephaloceles and nasal gliomas. CT imaging can detect bony defects of the skull base. In general, MRI is more sensitive and specific; it is superior to CT for visualizing soft tissues and for detection of intracranial extension. Nasal dermoid cysts appear very hyperintense on T1-weighted MRI images [12] .
Local Inflammation or abscess formation can occur in untreated cases. If there is an intracranial connection, they may result in cerebrospinal fluid (CSF) leakage, meningitis, cavernous sinus thrombosis, or periorbital cellulitis. Nasal bones or cartilages can be deformed with gradual expansion of nasal dermoid cyst.
Atresia of pinna, cleft lip and palate, hydrocephalus, and hypertelorism can be associated developmental anomalies with NDSC [13] .
Surgery is treatment of choice and should be carried out at earliest to avoid complications. Intracranial extension of cyst should be excluded before removal of cyst. The nasal portion of the dermoid can be removed using any one of various incisions, including midline vertical, transverse, lateral rhinotomy, or midbrow [14] . The external rhinoplasty approach allows good surgical exposure in combination with a superior cosmetic result [15] . Recently, nasal dermoid cyst has been removed with endoscopic approach [16] .
Recurrence rates for nasal dermoid cysts are very high when excised incompletely. Prognosis is good when removed completely. Facial scarring and saddle nose deformity are common postoperative complications.
Hemangiomas are observed in 4% - 10% of the population and represent the most common hamartoma of infancy [2] . They occur in up to 10% - 12% of Caucasian children and up to 22% of premature infants. Females are affected three times in comparison to males. The head and neck are the most common sites (59%). In facial hemangiomas, 15.8% show involvement of the nose, and the nasal tip is affected in 5.1% [3] . Hemangiomas can be intra-or extranasally and can result in nasal obstruction. Rate of involution of nasal hemangiomas is lower in comparison to hemangiomas found in other locations.
As the lesion is absent at birth and it start as an erythematous macule or telangiectasia during the first days or weeks of life, a proper history and examination is important for the diagnosis of hemangiomas. These facial infantile hemangiomas can be focal type or diffuse type. Focal type is tumour-like in appearance and are more common than diffuse type which are plaque-like in appearance. The growth phase, which can either be gradual or rapid, is usually six months long and is followed by a longer involution phase of 6 - 12 months [17] .
In general, hemangiomas demonstrate an early 3 - 9 month proliferative phase followed by quiescence and then involution, generally by 5 - 7 years of age. As many as 50% - 98% of hemangiomas regress spontaneously, often making close observation the most appropriate treatment. Different therapies such as topical, systemic or intra-lesional applications of steroid, alpha 2a and 2b interferon injections, cytotoxic medications like bleomycin, angiogenesis inhibitors, embolization, with carbon dioxide or Nd: YAG lasers and conventional surgery have all been described [18] [19] . Imiquimod as 5% cream has also recently been described for the treatment of severe complicated hemangiomas. However, side effects and the small study size make further studies necessary in order to assess this therapeutic option [20] .
Recently, Leaute-Labreze and colleagues have achieved impressive results by treating severe fetal hemangiomas of the face with systemic application of the beta-blocker propranolol [21] . After treatment with propranolol administered orally at 2 to 3 mg/kg per day, the authors observed a consistent, rapid, therapeutic effect, leading to a considerable shortening of the natural course of infantile hemangiomas with good clinical tolerance and a low rate of side effects(as in our case). Initially described in a case report, this has recently been confirmed in larger studies (>100 patients) [22] . Nasal reconstruction may be necessary when nasal cartilages or bones have been destroyed or distorted.
4. Conclusion
Facial scarring and saddle nose deformity are common postoperative complications. So, scar less surgery of these lesion is essential as tip of nose is most noticeable and central part of the face. It has an aesthetic importance as well as influence on the psyche of children.
Cite this paper
Snigdha Goyal,Sunder Goyal,Isha Saini,Amit Jain, (2015) Congenital Lesions of Tip of Nose: Report of Two Cases with Review. Open Access Library Journal,02,1-4. doi: 10.4236/oalib.1101467
References
- 1. Tatar, E.C., Selçuk, O.T., Saylam, G., Özdek, A. and Korkmaz, H. (2009) The Management of Rare Nasal Mass— Nasal Dermoid Sinus Cysts: Open Rhinoplasty. Rare Tumors, 1, e40.
- 2. Bailey, B.J. (2001) Head & Neck Surgery—Otolaryngology. 3. Lippincott Williams & Wilkins, Philadelphia, 1117-1124.
- 3. Waner, M., North, P.E., Scherer, K.A., Frieden, I.J., Waner, A. and Mihm Jr., M.C. (2003) The Nonrandom Distribution of Facial Hemangiomas. Archives of Dermatology, 139, 869-875.
http://dx.doi.org/10.1001/archderm.139.7.869 - 4. Sand, M., Sand, D., Thrandorf, C., Paech, V., Altmeyer, P. and Bechara, F.G. (2010) Cutaneous Lesions of the Nose. Head Face Medicine, 6, 7.
http://dx.doi.org/10.1186/1746-160X-6-7 - 5. Tatlidede, S., Egemen, O., Ozkaya, O. and Erol, O. (2011) Witch Nose: An Embarassing Metaphor for Nasal Tip Dermoid Cysts. Journal of Craniofacial Surgery, 22, 1948-1951.
http://dx.doi.org/10.1097/SCS.0b013e31822ea787 - 6. Madke, B., Nayak, C., Giri, A. and Jain, M. (2013) Nasal Dermoid Sinus Cyst in a Young Female. Indian Dermatology Online Journal, 4, 380-381.
http://dx.doi.org/10.4103/2229-5178.120669 - 7. Bilkay, U., Gundogan, H., Ozek, C., et al. (2001) Nasal Dermoid Sinus Cysts and the Role of Open Rhinoplasty. Annals of Plastic Surgery, 47, 8.
http://dx.doi.org/10.1097/00000637-200107000-00002 - 8. Paller, A.S., Pensler, J.M. and Tomita, T. (1991) Nasal Midline Masses in Infants and Children. Dermoids, Encephaloceles, and Gliomas. Archives of Dermatology, 127, 362-366.
http://dx.doi.org/10.1001/archderm.1991.01680030082011 - 9. Wang, I.J., Lin, S.L., Tsou, K.I., Hsu, M.C., Chiu, W.T., Tsai, S.H., et al. (2010) Congenital Midline Nasal Mass: Cases Series and Review of the Literature. Turkish Journal of Pediatrics, 52, 520-524.
- 10. Cambiaghi, S., Micheli, S., Talamonti, G. and Maffeis, L. (2007) Nasal Dermoid Sinus Cyst. Pediatric Dermatology, 24, 646-650.
http://dx.doi.org/10.1111/j.1525-1470.2007.00555.x - 11. Farvolden, D., Sweeney, S.M. and Wiss, K. (2005) Lumps and Bumps in Neonates and Infants. Dermatologic Therapy, 18, 104-116.
http://dx.doi.org/10.1111/j.1529-8019.2005.05016.x - 12. Bratton, C., Suskind, D.L., Thomas, T. and Kluka, E.A. (2001) Autosomal Dominant Familial Frontonasal Dermoid Cysts: A Mother and Her Identical Twin Daughters. International Journal of Pediatric Otorhinolaryngology, 57, 249-253.
http://dx.doi.org/10.1016/S0165-5876(00)00437-7 - 13. Wardinsky, T.D., Pagon, R.A., Kropp, R.J., Hayden, P.W. and Clarren, S.K. (1991) Nasal Dermoid Sinus Cysts: Association with Intracranial Extension and Multiple Malformations. The Cleft Palate-Craniofacial Journal, 28, 87-95.
http://dx.doi.org/10.1597/1545-1569(1991)028<0087:NDSCAW>2.3.CO;2 - 14. Lees, M.M., Connelly, F., Kangesu, L., Sommerlad, B. and Barnicoat, A. (2006) Midline Cleft Lip and Nasal Dermoids over Five Generations: A Distinct Entity or Autosomal Dominant Pai Syndrome? Clinical Dysmorphology, 15, 155-159.
http://dx.doi.org/10.1097/01.mcd.0000204987.61990.f0 - 15. Mankarious, L. and Smith, R.J. (1998) External Rhinoplasty Approach for Extirpation and Immediate Reconstruction of Congenital Midline Nasal Dermoids. Annals of Otology, Rhinology & Laryngology, 107, 786-789.
http://dx.doi.org/10.1177/000348949810700909 - 16. Weiss, D.D., Robson, C.D. and Mulliken, J.B. (1998) Transnasal Endoscopic Excision of Midline Nasal Dermoid from the Anterior Cranial Base. Plastic & Reconstructive Surgery, 102, 2119-2123.
http://dx.doi.org/10.1097/00006534-199811000-00048 - 17. Waner, M., Kastenbaum, J. and Scherer, K. (2008) Hemangiomas of the Nose. Archives of Facial Plastic Surgery, 10, 329-334.
http://dx.doi.org/10.1001/archfaci.10.5.329 - 18. Musumeci, M.L., Schlecht, K., Perrotta, R., Schwartz, R.A. and Micali, G. (2008) Management of Cutaneous Hemangiomas in Pediatric Patients. Cutis, 81, 315-322.
- 19. Stier, M.F., Glick, S.A. and Hirsch, R. (2008) Laser Treatment of Pediatric Vascular Lesions: Port Wine Stains and Hemangiomas. Journal of the American Academy of Dermatology, 58, 261-285.
http://dx.doi.org/10.1016/j.jaad.2007.10.492 - 20. Barry, R.B., Hughes, B.R. and Cook, L.J. (2008) Involution of Infantile Haemangiomas after Imiquimod 5% Cream. Clinical and Experimental Dermatology, 33, 446-449.
http://dx.doi.org/10.1111/j.1365-2230.2007.02676.x - 21. Léauté-Labrèze, C., Dumas de la Roque, E., Hubiche, T., Boralevi, F., Thambo, J.B. and Taïeb, A. (2008) Propranolol for Severe Hemangiomas of Infancy. New England Journal of Medicine, 358, 2649-2651.
http://dx.doi.org/10.1056/NEJMc0708819 - 22. Löffler, H., Kosel, C., Cremer, H. and Kachel, W. (2009) Propanolol Therapy to Treat Problematic Hemangiomas. A New Standard Therapy Makes Its Debut. Der Hautarzt, 60, 1013-1016.
http://dx.doi.org/10.1007/s00105-009-1856-4
NOTES
*Corresponding author.