 International Journal of Clinical Medicine, 2015, 6, 845-851 Published Online November 2015 in SciRes. http://www.scirp.org/journal/ijcm http://dx.doi.org/10.4236/ijcm.2015.611111 How to cite this paper: Umesh, V. and Kavita, M. (2015) Original Research: Treating Sleep Disorders Has Positive Outcomes in Psychiatric Illnesses. International Journal of Clinical Medicine, 6, 845-851. http://dx.doi.org/10.4236/ijcm.2015.611111 Original Research: Treating Sleep Disorders Has Positive Outcomes in Psychiatric Illnesses Vyas Umesh1,2,3,4,5, Mundey Kavita6 1Park Center Inc., Fort Wayne, USA 2Indiana University School of Medicine, Fort Wayne, USA 3Fort Wayne Medical Education Program-Family Medicine Residency, Fort Wayne, USA 4University of Saint Francis, Fort Wayne, USA 5Ivy Tech Community College of Indiana, Fort Wayne, USA 6Veteran’s Administration Medical Center (VAMC), Milwaukee, USA Received 11 July 2015; accepted 16 November 2015; published 19 Nove mber 2015 Copyright © 2015 by authors and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). http://creativecommons.org/licenses/by/4.0/ Abstract Introduction: Sleep and psychiatric disorders are common, and often co-morbid. Sleep disorders may predispose to development or exacerbation of psychiatric disorders. Authors hypothesized that treatment of sleep disorders improve outcomes in psychiatric illnesses. Methods: Charts of patients diagnosed with sleep disorders from October 2007 to December 2007 were reviewed. Outcomes in patients with co-morbid psychiatric disorders were recorded at 6, 12 and 24 months after initiation of sleep disorder treatment. These patients received a baseline psychiatric status score of 0. Change in status at each subsequent time point was scored as: −2 (marked worsening), −1 (mild worsening), 0 (no change), +1 (mild improvement) or +2 (marked improvement). We indi- vidually compared change in average score at each time point to baseline using the signed rank test. We compared provider documented compliance to sleep therapies between patients with and without psychiatric disorders using Fisher’s exact test. Results: Of 127 charts reviewed, 10 were excluded as patients died within follow-up period. No death was reported as suicide. Of 117 pa- tients, 97.64% were men, 2.36% were women. Age range: 21 - 40: 7.69%, 41 - 60: 42.74%, 61 - 80: 47.87%, >81: 1.70%. 58 patients (45.67%) had coexistent psychiatric diagnoses. There was no difference in provider documented compliance rate to sleep therapies between patients with and without psychiatric disorders at 6, 12 and 24 months, (Fisher’s p value 0.1031, 0.2290 and 0.2248 respectively). Psychiatric status progressively improved compared to baseline (Change in average score by +0.45, +0.56, and +0.79 at 6, 12, and 24 months, respectively, p < 0.0001). Conclusion: Psychiatric disorders did not affect compliance to sleep related treatment. Treatment of co-m or- bid sleep disorders is associated with improvement in psychiatric disorders. Authors recommend need for prospective study with more subjects.  V. Umesh, M. Kavita Keywords Psychiatric Illnesses/Dis o rder s, Sleep Illnesses/Dis o rd ers 1. Introduction Sleep is an es sentia l ph ysiolo gical need, a nd it is an acti ve state t hat i s critical for our ph ysical, mental a nd e mo- tional well-being. Sleep is also important for op timal cognitive functio ning and sleep disruption results in func- tional impair ment. Sleep and psychiatric disorde rs are common disorders in clinical pop ulations; existing data supp orts high rate of co-morbidity between them, and the disturbance in quality and quantity of sleep due to sleep disorders pre- disposes to the development or exacerbation of psychological distress and psychiatric illnesses. Likewise, the presence of psychiatric illnesses may complicate the diagnosis and treatment of sleep disorders. Sleep disturbances are so commonly seen in psychiatric disorders that they are listed as diagnostic criteria under DSM (American Psychiatric Association) [1]. Sleep and psychiatric disorders, by themselves are disabling, the treatment of the co-morbidity may reduce needless disability. The data not only underscore the high fre- quency of psychopathology and psychological distress in sleep disorders and vice versa, but also suggest that combined treatment of both should become the standard of care for effective therapy [2]. 2. Literature Review 40% of those diagnosed with insomnia, in a population-based study, also have a psychiatric disorder, and with hypersomnia the prevalence of psychiatric disorder is 46.5% [3]. Mood and anxiety disorders are associated with high rates of insomnia [4]. Prevalence for insomnia complaints was 12.7% in general population. The preva- lence of sleep disorders mostly insomnia due to mental disorder was 5.6%; primary psychiatric disorder diag- nosed were applied to 8.4% [4]. Another study, which followed 1007 young adults at a health maintenance organization for 3.5 years, found that a history of insomnia at baseline not only predicated new onset depression, but also other psychiatric dis- orders (any anxiety disorder, alcohol abuse, drug abuse, and nicotine dependence), [5], the adjusted odds of de- veloping a psychiatric disorders were highest for depression (OR = 3.95; 95% CI, 2.2 - 7.0), was based on 16 percent of the sample who developed depression with history of insomnia at baseline, as compared with 4.6 percent who developed depression without a history of insomnia. The study’s general findings are supported by another large study of 10,000 adults. That stud y found insomnia to have increased the risk of major depression by a similar magnitud e (5 -fold) and to have increased the risk of panic disorder even more strikingly, by 20-fold (OR = 20.3; 95% CI, 4.4 - 93.8) [6]. Insomnia is also a predictor of acute suicide among patients with mood dis- orders [7]. More than 2000 UK residents at baseline and 12-month follow up, measures of insomnia, depression and an- xiety demonstrated that baseline insomnia was a significant risk factor for incidence of depression and anxiety at follow up (adjusted risk ratio of 2.71 and 2.28 respectively) [8]. Zurich longitudinal epidemiologic study revealed that a new onset of depression developed in 17% to 50% of patients with persistent, pure insomnia of ≥2 weeks duration at a later interview, wit h p r e dictive odds ra tio of 1.6 to 1.9 [9]. Wisconsin Sleep Cohort, found substantially higher rates of psychiatric symptoms and disorders among those with daily Restless Leg S yndrome (RLS). Odds ratio to depression (Zung score > 50 or Anti-Depressant medi- cation use) in those the daily RLS was 2.17 and 1.80 in those with “frequent” RLS (one or six times per week). For anxiety disorders, odds ratio were 3.41 and 2.42 for the two RLS groups respectively [10]. Psychiatric co-morbidity in Obstructive Sleep Apnea (OSA) patients was examined in a large prospective chart review of >100,000 Veterans Affairs Hospital OSA patients. A significantly high prevalence of psychiatric disorders was found in this group, as compared with a non-OSA population. High co-morbidity was found for major depression 21.8%, anxiety disorder 16.7%, PTSD 11.9%, psychosis 5.1%, and Bipolar disorder 3.3% [11]. Depressive symptoms i mprove with treatment of OS A, and untreated OSA may contribute to treatment resis- 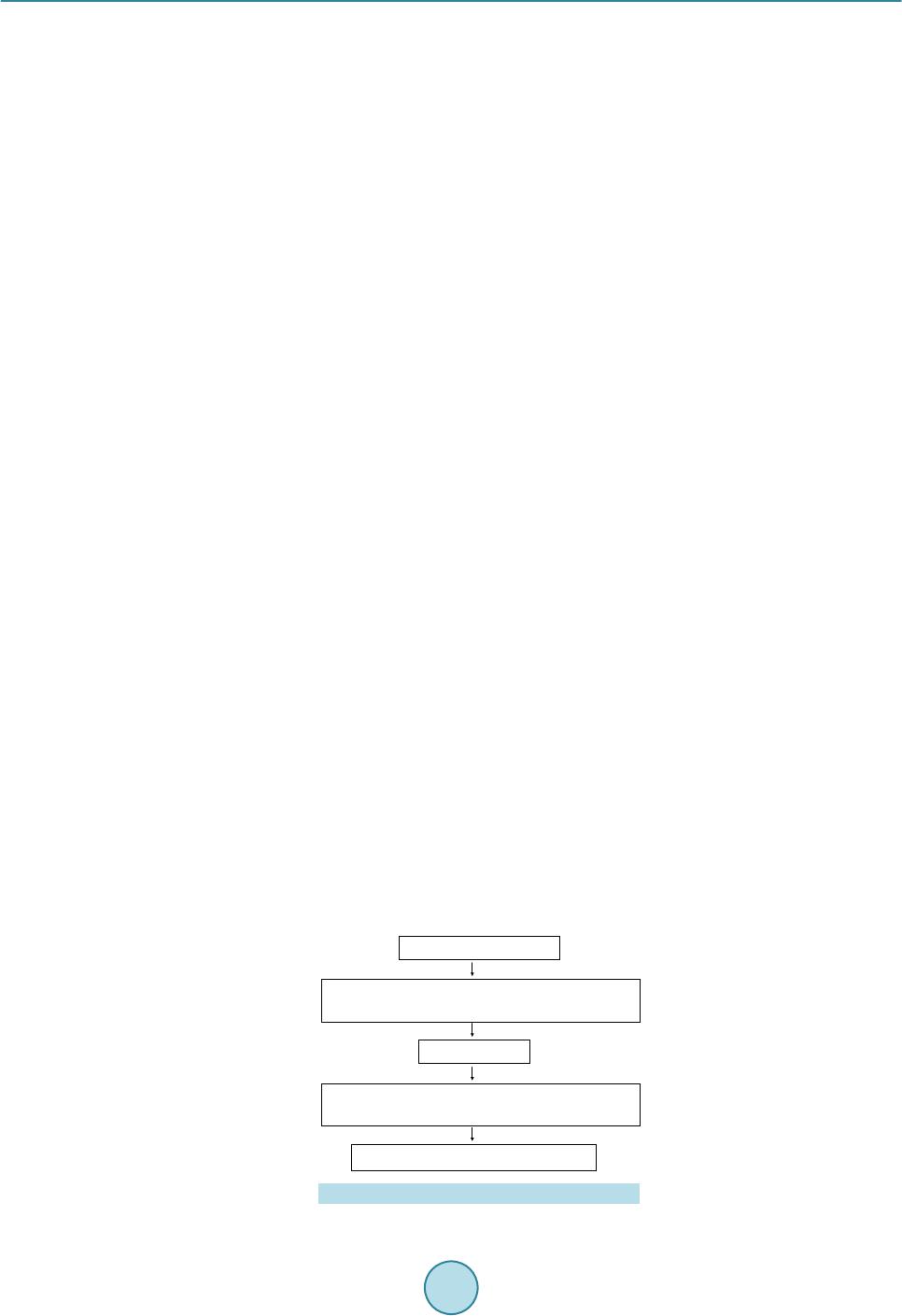 V. Umesh, M. Kavita tance in some cases of mood disorders [12]. OSA is a common sleep disorder, is well recognized as a cause of morbidity including psychiatric disorders. OSA needs to be excluded in cases of chronic or resistant depression and treatment of OSA will make it easier to treat depressive disorder [13]. Treatment of depression in OSA might improve acceptance of therapy, reduce sleepiness, fatigue and improve quality of life [14]. Reduction of depression scores (seven-item BDI) in OSA patients treated with continuous positive airway pressure (CPAP) [15]. Studies demonstrated high rates of depressive symptoms in OSA, as well as improvement of these symp- toms with treatment of OSA [16]-[18]. Combined therapies for both depression and insomnia are superior to anti-depressant medications alone in pa- tients with major depression [19] [20]. Study combining anti-depression medications with specific insomnia treatment (cognitive-behavioral therapy for insomnia) demonstrated that the combined treat ment was superior to anti -depressant alone both in terms of depression out-come (61.5% vs. 33.3% remission respectively) and in- so mni a out-come (50% vs. 7.7% respectively) [21]. Guidelines on the management of insomnia from American Academy of Sleep Medicine (AASM) recom- mend that treatment of insomnia in patients with co-morbid psychiatric disorders follow the general guidelines of psychological and behavioral therapies, possibly coupled with a benzodiazepine receptor agonist, but they al- so note the potential usefulness of sedating anti-depressant or atypical anti-psychotic medications in certain populations [22]. Evidence suggests that individuals seeking medical attention for sleep complaints are more likely to have drug or alcohol abuse problems than the general population. Withdrawal from nicotine, alcohol and drug abuse is also associated with insomnia, and this may result in an increased risk of relapse if the sleep problems are remain unresolved [23]. The Post-Traumatic Stress Disorder (PTSD), 37% had significant nightmare problems [24], and severity of sleep disturbance correlated with PTSD severity [25]. 3. Research Design Retrospective, observational, chart review study. 4. Method Electronic medical record reviewed for diagnosis of sleep disorders at VAMC Milwaukee, WI, USA from Oc- tober 2007 to December 2007, Figure 1. Patients with confirmed diagnosis and treatment for sleep disorders were included. Outcomes in patients with co-morbid psychiatric disorders were recorded at 6, 12 and 24 months after initiation of sleep disorder treatment. Measurements of change in psychiatric disorder defined as follows: Baseline score = 0. Marked improvement = +2. Partial improvement = +1. No change = 0. Partial worsening = −1. Mar ked wor s ening = −2. Figure 1 . Details of chart reviewed. 57 charts excluded due to lack of treatment 57 charts excluded due to lack of treatment or follow up or follow up 117 char ts included in study 117 char ts included in study 184 charts reviewed 184 charts reviewed 10 charts excluded as patients died within 10 charts excluded as patients died within follow follow- -up period. ( up period. ( No death reported as suicide). No death reported as suicide). 127 charts 127 charts  V. Umesh, M. Kavita Various parameters used to assess outcomes of psychiatric disorders to assess improvement or worsening Ta- ble 1. Change in average score for psychiatric disorders was compared individually at each time point to baseline using the signed rank test. Compliance was compared to sleep disorder treatment between patients with and without psychiatric disorders using Fisher’s exact test. Difference in score changes at each time point to baseline was compared for a specific psychiatric disorder using Wilcoxon test. Compliance to management defined as: • Attendance o f follow up visits in sleep c linic/pri mary care clinic/respiratory therapist clinic. • Documentation of patient reported compliance to positive airway pressure therapy and other treatments of- fered. • Clinic visit ca ncella tion ≤2 consecutive appointments. 5. Discussion, Results and Conclusions Current data demonstrate important bidirectional relationship between sleep and psychiatric disorde rs, and men- tal disorders co-morbid with sleep disorders contribute to disease burden and adversely affect the outcome of patients with these conditions, therefore effective comprehensive evaluation and management of patients with sleep disorders require careful psychological assessment and evaluation for specific psychiatric disorders and vice versa. It also requires necessary independent pharmacological and psychological treatment of sleep disorder and psychiatric disorder. Our study subject’s demographic and age distribution (Age range: 21 - 40: 7.7%, 41 - 60: 42.7%, 61 - 80: 47.9%, >81: 1.7%) was very typical of Veteran’s Administration Medical Center (VAMC), Figure 2. Our st ud y supports treatment of co-morbid sleep disorders was associated with significan t improvement in ps ychiatric d is- orders, Wilcoxon Signed rank test used, Figure 3 and Table 2. Psychiatric disorders did not affect compliance with sleep disorders treatment Table 3, Fisher’s exact test used. Compliance among patients with psychiatric Table 1. Parameters to as sess ou tco mes of psychiatric disorders. DSM Diagnosis Psychiatric Medications MHC Follow up/In-Pt Man agemen t Documented Improvement/Worsening Substance Abuse Marked Improvement (+2) Removal of Dx Completely stopped Discharged from MHC Significant Improvement Stopped completely Partial Improvement (+1) Mild/NOS cat egory of Dx Lower doses required Less fr equent visit Mild/moderate improvement Reduced ab use No Change (0) Partial Worsening (−1) New Mild cat egory Dx add ed More number/doses required More frequent visits Mild/moderate worsening More su bstan ce abuse Marked Worsening (−2) Changed or added sever e cat egory of Dx Maximum doses and/or augmentation required In-Pt management required Significant worsening Rela pse an d/or new substance abuse Table 2. Changes in psychiatric disease statu s after treatment. Comp aris on Mean (Time 1) Mean ( Time 2) p value Baseline vs. 6 Months 0 0.45 0.0004 Base l i ne vs. 12 Mont hs 0 0.56 0.0002 Base l i ne vs. 24 Mont hs 0 0.79 <0.0001 6 Mon ths vs. 12 Mo nt hs 0.45 0.56 0.1094 6 Mon ths vs. 24 Mo nt hs 0.45 0.79 0.0005 12 Months vs. 24 Months 0.56 0.79 0.0039  V. Umesh, M. Kavita Table 3. Comparison of compliance among patients with and without psychiatric diagnosis. Tim e Fisher’s p V a lue 6 Months 0.1031 12 Months 0.2290 24 Months 0.2248 Figure 2 . Demographics and age distribution. Figure 3 . Change in psychiatric illness status during two years follow-up period. diseases was 77%, and compliance in patients without psychiatric disea ses was 87%. Wilcoxon test was used to find if there were significant differences in score change at each time point based on the presence of a specific psychiatric disorder. Authors found this was not statistically significant. This may be due to small number (N) for a specific psychiatric disorder; since most subjects had various co-exist ing psychiatric disorders Table 4 . All statistical analysis was performed in SAS (Cary, NC). 6. Limitations • Retrospective, chart review with small number of subjects. • Single author reviewed all charts, therefore personal bias cannot be ruled out. • Limitation of Li ker t Sc a le-Central tendency bias. • Most sleep disorder patients had diagnosis of sleep-related breathing disorder (OSA). • No objective compliance data were available for every subject to ascertain compliance. • VA elderly male patient population; cannot be a pplied to general slee p clinic patient p opulation. There is a strong need for prospective studies with more subjects, to establish not only importance of man- agement of sleep disorders in psychiatric disorders, but also need for comprehensive evaluation. • •117 patients 117 patients • •97.6% were men, 2.4% 97.6% were men, 2.4% were women were women • •54 patients (46.2%) had 54 patients (46.2%) had coexistent psychiatric coexistent psychiatric diagnoses. diagnoses. 0 10 20 30 40 50 60 21-40 41-60 61-80>81 Change in psychiatric status during 2 Change in psychiatric status during 2 year follow year follow- -up period up period 0 0.2 0.4 0.6 0.8 1 Baseline 6 months12 months24 months  V. Umesh, M. Kavita Table 4. Wilcoxon test for significant difference in score change (baseline vs. 6, 12, 24 months) based on presence of psy- chiatric disorder. Psychiatric Disorder Mean Score Change (disorder not present) Mean Score Change (disorder present) p value Psychotic 6 month s 12 mont hs 24 mont hs 0.46 0.57 0.81 0 0 0 0.4814 0.4061 0.2875 Mood 6 month s 12 mont hs 24 mont hs 0.60 0.90 1.10 0.42 0.49 0.72 0.6171 0.3515 0.3701 Anxiety 6 month s 12 mont hs 24 mont hs 0.43 0.53 0.73 0.63 0.75 1.13 0.7311 0.7237 0.3703 Sub-related 6 month s 12 months 24 months 0.61 0.71 0.97 0.12 0.24 0.41 0.1009 0.1159 0.0701 PTSD 6 month s 12 months 24 months 0.32 0.35 0.61 0.67 0.90 1.10 0.1457 0.0396 0.0983 Conflict of Interest The authors declare that they have no conflict of interest. Hypothesis Authors hypothesized that treatment of sleep disorders improve outcomes in psychiatric illnesses. Objectives Evaluate effect of treatment of sleep disorders on outcomes of psychiatric disorders. References [1] (2013) Diagnostic and Statistical Manual of Mental Disorders. 5th Edition, DSM-5. [2] Michael, S.J. (2009) Upda te on Sleep and Psychiatric Disorders. Chest, 135 , 1370-1379. http://dx.doi.org/10.1378/chest.08-1834 [3] Ford, D.E. and Kamerow, D.B. (1989) Epidemiologic Study of Sleep Disturban ces and P sychiatric Disorders. An Op- portunity for Prevention? Journal of the American Medical Association, 262, 1479 -14 84 . http://dx.doi.org/10.1001/jama.1989.03430110069030 [4] Ohayon, M.M. (1997) Prevalence of DSM IV Diagnostic Criteria of Insomnia; Distinguishing Insomnia Related to Mental Disorders from Sleep D isorders. Journal of Psychiat ric Research , 31, 333 -34 6 . http://dx.doi.org/10.1016/S0022-3956(97)00002-2 [5] Breslau, N., Roth , T., Rosenth al, L., et al. (1996) Sleep Disturbance and P sychiatric Diso rders: A Longitudinal Epide- miological Study of Young Adults. Biological Psychiatry, 39, 411-418. http://dx.doi.org/10.1016/0006-3223(95)00188-3 [6] Weissman, M.M., Greenwald, S., Nino-Murci a , G., et al. (1997) The Morbidity of Insomnia Uncomplicated by Psy- chiatric Disorders. General Hospital Psych iatry, 19, 245 -250. http://dx.doi.org/10.1016/S0163-8343(97)00056-X [7] Fawcett, J., Scheftner, W.A., Fogg, L., et al. (1990) T i me -Related Predictors of Suicide in Major Affective Di sorder. American Journal of Psyc hiatry, 147, 1189-1194. http://dx.doi.org/10.1176/ajp.147.9.1189 [8] Morphy, H., Dunn , K.M., Lewis, M., et al. (2007) Epidemiology of Insomnia: A Longitudinal Study in a UK Pop ul a- tion. Sleep, 30, 274 -28 0.  V. Umesh, M. Kavita [9] B uys se , D.J., Angst, J., Ga mma, A., et al . (2008) Prevalence, Course and Co-Morbidity of Insomnia and Depression in Young Adults. Sleep, 31 , 4 73 -48 0. [10] Winkelman, J.W., Finn, L. and Young, T. (2006) Prevalence and Correlates of RLS Symptoms in Wisconsin Sleep Cohort. Sleep Medicine, 7, 545-55 2 . http://dx.doi.org/10.1016/j.sleep.2006.01.004 [11] Sharafkhaneh, A., Giray, N., Richardson, P., et al. (2005) Association of Psychiatric Disorders and Sleep Apnea in Large Cohort. Sleep, 28, 1405-1411. [12] Baran, A.S. and Richert, A.C. (2003) Obstructive Sleep Apnea and Depressi on. CN S Spectrums, 8, 128-134. [13] Kaplan, R. (1992) Obstructive Sleep Apnea and Depression-Diagnostic and Treatment Implications. Australian and New Zealand Journal of Psychiatry, 26, 586-591. http://dx.doi.org/10.3109/00048679209072093 [14] Harris, M., Glozier, N., Ratnavadivel, R., et al. (2009 ) Obstructive Sleep Apnea and Depression. Sleep Medicine Re- views, 13, 437-444. http://dx.doi.org/10.1016/j.smrv.2009.04.001 [15] Schwartz, D.J. an d Karatinos, G. (2007) For Individuals with OSA, Institution of CPAP Therapy Is Associated with an Amelioration of Symptoms of Depression Which Is Sustained Long Term. Journal of Clinical Sleep Medicine, 3, 631 - 635. [16] M o s ko , S., Zetin, M., Gl en , S., et a l. (1989 ) Self-Reported Depressive Symptomatology, Mood Ratings and Treatment Outco me in Sleep Disorders Patients. Journal of Clinical Psychology, 45, 51-60. http://dx.doi.org/10.1002/1097-4679(198901)45:1<51::AID-JCLP2270450107>3.0.CO;2-H [17] Ohayon, M.M. (2003) The Effects of Breat hi ng-Related Sleep Disorders on Mood Disturbances in the General Popula- tion. Journal of Clinical Psychiatry, 64, 1195-1200. http://dx.doi.org/10.4088/JCP.v64n1009 [18] Millanan, R.P., Fo gel , B.S., McNamara, M.E., et al. (1989) Depressio n as a M anifestati on o f Obstructive S leep Apnea; Reversal with Nasal Continuous Positive Airway Press ure. Journal of Clinical Psychiatry, 50, 348 -351. [19] F ava, M., McCall, W.V., Krystal, A., et al. (2006) Eszopiclone Co-Administered with Fluoxetine in Patients with In- somnia Coexisting with Major Depressive Disorder. Biological Psychiatry, 59, 1052-1060. http://dx.doi.org/10.1016/j.biopsych.2006.01.016 [20] Krystal, A., Fava, M., Rubens, R., et al. (2007) Evaluation of Eszopiclone Discontinuation after Co-Therapy with F lu- oxeti ne for Insomnia with Coexisting Depression. Journal of Clinical Sleep Medicine, 3, 48-55. [21] Manber, R., Edinger, J.D., Gre ss, J.L., et al. (2008) Cognitive Behavioral Therap y for Inso mnia Enhan ces Depression Outcome in Patients with Co-Morbid Major Depressive Disorder and Insomnia. Sleep, 31, 489-495. [22] Schutte-Rodin, S., Broch, L., Buysse, D., et al. (2008) Clinical Guideline for the Evaluation and Management of Chronic Insomnia in Adults. Journal of Clinical Sleep Medicine, 4, 487-50 4. [23] Roth, T. (2009) Does Effective M anagement of Sleep Disorders Reduce Substance Dependence? Drugs, 69, 65-75. Does Effe ctive M anag e ment of S l eep Di sor ders Redu ce Dep ressive Symptoms and the Risk of Depression? Drugs, 69, 43-64. [24] Calhoun, P.S., Wiley, M., Dennis, M.F., et al. (2007) Objective Evidence of Sleep Disturbance in Women with Post- traumatic Stress Disor der. Journal of Traumatic St ress , 20, 1009 -1018. http://dx.doi.org/10.1002/jts.20255 [25] Waldrop, A.E., Back, S.E., Sensenig, A., et al . (2008) Sleep Disturbance Associated with Posttraumatic Stress Disord- er and Alcohol Dependence. Addictive Behaviors, 33, 328-335. http://dx.doi.org/10.1016/j.addbeh.2007.09.019
|