Journal of Cancer Therapy
Vol.4 No.5(2013), Article ID:33777,5 pages DOI:10.4236/jct.2013.45109
An Analysis of the Potential Benefits of Metformin on Disease Recurrence in Oral and Oropharyngeal Squamous Cell Carcinoma*
![]()
1Department of Head and Neck Surgery, University of California, Los Angeles, USA; 2Surgical and Perioperative Careline, VA Greater Los Angeles Healthcare System, Los Angeles, USA; 3Department of Pathology and Laboratory Medicine, University of California, Los Angeles, USA; 4Department of Medicine Statistics Core, University of California, Los Angeles, USA.
Email: #chrthompson@mednet.ucla.edu
Copyright © 2013 Christopher F. Thompson et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received April 12th, 2013; revised May 15th, 2013; accepted May 23rd, 2013
Keywords: Metformin; Head and Neck Cancer; Oral Squamous Cell Carcinoma; Oropharyngeal Squamous Cell Carcinoma
ABSTRACT
Objective: Diabetes mellitus type 2 has been associated with increased cancer risk and cancer related mortality. Metformin, one of the most widely used anti-diabetic medications, has been found to have important anticancer properties in addition to hypoglycemic effects. The effects of metformin on clinical outcomes in oral cavity (OC) and oropharyngeal (OP) squamous cell carcinoma (SCC) have not been thoroughly analyzed. The purpose of this study was to evaluate the effects of metformin use on cancer recurrence in diabetic patients with oral cavity and oropharyngeal squamous cell carcinoma. Design: Retrospective review. Setting: Academic tertiary medical center. Patients: Seventy-seven patients with diabetes mellitus type 2 and oral cavity or oropharyngeal squamous cell carcinoma were treated and followed at our tertiary academic institution and the Veterans Affairs Greater Los Angeles Healthcare System from 1998 to 2012. Main Outcome Measure: Cox proportional hazards models and Kaplan-Meier curves were constructed to determine if metformin has an effect on disease recurrence after primary cancer treatment. Results: Metformin does not appear to have a significant effect on disease recurrence in patients with OC/OP SCC and diabetes mellitus type 2 (p = 0.53). Even when including only patients with stage I or II disease, metformin still did not decrease recurrence (p = 0.60). Conclusion: Herein, our data suggest that metformin use does not significantly impact time until recurrence for diabetic patients with OC/OP SCC.
1. Introduction
Head and neck cancer comprises 7% of all new cancer cases per year in the United States, with nearly 30% of these tumors arising from the oral cavity (OC) and oropharynx (OP) [1]. Squamous cell carcinoma (SCC) is the histological subtype in nearly 90% of these OC and OP SCC cases [2]. Despite advances in surgical treatment, radiation therapy and the development of new adjuvant chemotherapeutic regimens, the 5-year survival for OC/OP SCC remains unchanged at 50% [2]. Improvements in locoregional control have not influenced survival, largely due to a shift in the pattern of failure to the development of disease at distant sites and the development of second primary lesions, the risk of which approaches 30% over a patient’s lifetime [3,4]. This dismal prognosis, despite treatment advancements, has fueled interest in the identification of factors and adjuvant therapies that will improve treatment outcomes.
Metformin, one of the most widely prescribed oral hypoglycemic medications, has recently gained significant attention in the literature for its potential anticancer effects [5]. Clinical studies have already suggested that among diabetic patients, metformin users have decreased risk of colon cancer [6] and improved outcomes in hepatocellular carcinoma [7] and pancreatic cancer [8]. Recent in vitro and in vivo studies by Vitale-Cross et al. [9] with a mouse OC tumor model are promising in elucidating the cellular pathways describing how metformin exerts its beneficial effects in head and neck SCC. However, clinical studies analyzing the effects of metformin use on treatment outcomes in diabetic patients with OC/OP SCC are lacking. The purpose of our study was to determine whether metformin use has any effect on disease recurrence in diabetic patients with OC/OP SCC.
2. Methods
Our study was approved by the Institutional Review Board of the University of California at Los Angeles and the West Los Angeles Veterans Affairs Medical Center (WLA VAMC). We retrospectively reviewed the clinical data and treatment outcomes of all diabetic patients with pathologically confirmed oral cavity or OC/OP SCC treated and followed at UCLA from January, 1998 to August, 2012, and all patients from January 2001 to October 2012 at the WLA VAMC. Patients with OC/OP SCC from UCLA were obtained from the Department of Pathology’s database. Patients from the WLA VAMC were obtained from the head and neck cancer tumor board, a multi-disciplinary conference at which all patients with head and neck cancer are discussed. Inclusion criteria for our study included a disease free interval of at least 3 months after completion of primary treatment, since that is the date we routinely order post-treatment PET scans for tumor surveillance.
Patients with diabetes mellitus type 2 (DM II) were divided into two groups based on metformin use. Patients were considered to be metformin users if they were taking the medication at the time of cancer diagnosis or while in remission after treatment. Patients who were not taking metformin at any point during or after their cancer treatment were classified as non-users, and cancer treatment was not different based on metformin use. Patient clinical characteristics analyzed included sex, age, smoking and alcohol use, tumor subsite, TNM stage, and primary treatment modality. The tailored t-test was used to determine if there were differences in the demographics between metformin users and non-users. The main outcome measure was cancer recurrence during the study period. The Kaplan-Meier estimates of the disease recurrence probabilities are visualized in graphical displays (Figures 1 and 2).
3. Results
We identified 77 patients with DM II and OC/OP SCC that were followed at UCLA or the WLA VAMC during our study period. Total follow-up after completion of primary treatment until death or last clinical contact was
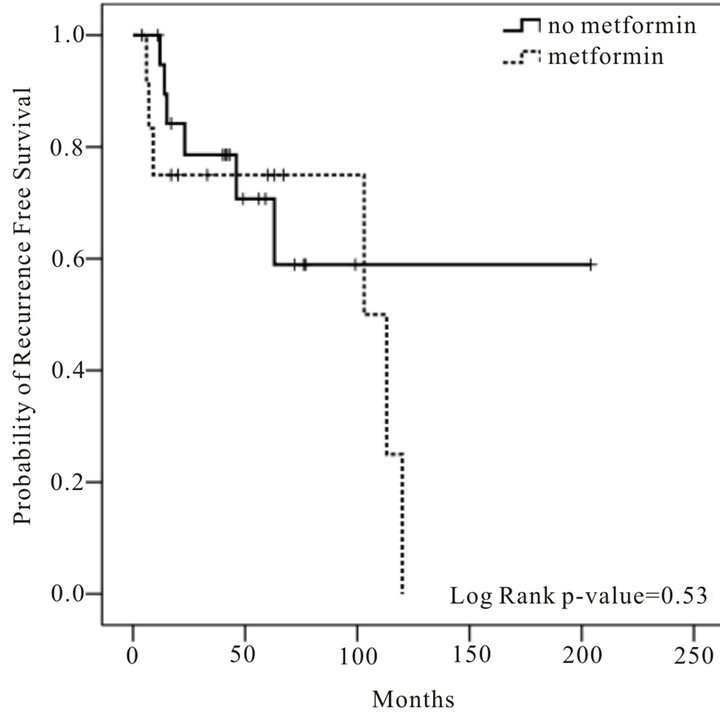
Figure 1. Kaplan-Meier curves for the recurrence-free survival of diabetic patients with oral cavity and oropharyngeal squamous cell carcinoma.
4 to 204 months (median = 44 mos.). There were no significant clinical differences between patients taking metformin (n = 33) and those who were not (n = 45) in terms of sex, age, tumor subsite, TNM stage at diagnosis, and smoking or alcohol use. The follow-up for patients on metformin was 6 to 143 mos. (median = 36 mos.), and the follow-up for patients not taking metformin was 4 to 204 mos. (median = 49 mos.).
In the analysis of all 77 patients, metformin does not appear to have a significant effect on disease recurrence (HR 1.26, 95% CI 0.62 - 2.56, p = 0.53) (Figure 1). Of the 45 patients not taking metformin, 17 patients had experienced recurrent disease, while 14 of the 32 patients using metformin had recurrences. When analyzing only patients with TNM stages I and II (early stage) OC/OP SCC, metformin still does not appear to have a significant effect on disease recurrence (HR 1.37, 95% CI 0.42 - 4.44, p = 0.60) (Figure 2). Of the 21 patients not taking metformin, 6 developed recurrences. Six of the 12 patients with early stage OC/OP SCC taking metformin developed recurrences.
4. Discussion
Over 30,000 new cases of oral and oropharyngeal cancers are expected to be diagnosed each year in the United States, with nearly 8000 patients dying annually from the disease [2]. Considering that the 5-year survival remains unchanged at around 50%, it is critical to identify factors that will improve outcomes for these patients. Despite the promising anticancer effects of metformin in
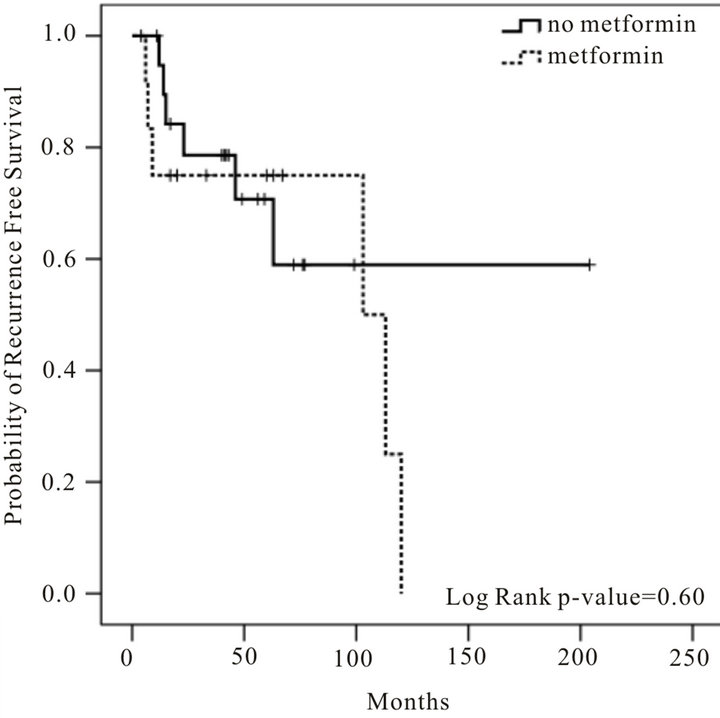
Figure 2. Kaplan-Meier curves for the recurrence-free survival of diabetic patients with stages I and II oral cavity and oropharyngeal squamous cell carcinoma.
other malignancies [10,11], our early results suggest that metformin likely does not have a significant role in adjuvant treatment for head and neck cancer patients with DM II (Figures 1 and 2).
Our interest in the potential benefit of metformin in OC/OP SCC developed from previous clinical trials that have already shown metformin’s benefit with breast cancer, hepatocellular carcinoma, colon cancer, and pancreatic cancer [7,8,12-14]. For example, in a retrospective review of breast cancer patients with diabetes receiving neoadjuvant chemotherapy, metformin users demonstrated a significantly better pathology clinical response than non-metformin patients [12]. With regards to hepatocellular carcinoma, diabetic patients on metformin have decreased incidence and improved outcomes [7,13]. Likewise, patients with diabetes taking metformin have decreased colon cancer [14] and improved outcomes in pancreatic cancer [8].
Metformin’s effects may be in part related to the medication’s effects of lowering circulating insulin levels, as insulin is a growth-promoting hormone with mitogenic effects [15]. However, early laboratory results suggest that metformin’s primary anticancer mechanism is separate from, and in addition to, its hypoglycemic effects.
The molecular pathway of how metformin may inhibit cell proliferation and prevent carcinogenesis appears to be from the medication’s direct activation of the AMP activated protein kinase (AMPK) pathway. The activation of AMPK prevents the activation of mammalian target of rapamycin (mTOR), which is a protein responsible for upregulating many energy consuming cellular processess. mTOR has a critical role in cell growth by controlling mRNA translation and ribosome genesis. Therefore, by directly inhibiting AMPK, mTOR is not activated and there is a subsequent downstream inhibition of cell proliferation and subsequently carcinogenesis [15,16].
The in vitro studies by Vitale-Cross, et al. [9] with head and neck SCC (HN SCC) cultured cells have supported this molecular mechanism of metformin’s downregulation of mTOR. In their experiments, metformin treated HN SCC cells had increased AMPK activity, decreased mTOR activity and decreased cell proliferation. Interestingly, when they controlled for and prevented metformin’s activation of AMPK, the metformin treated cells still demonstrated a decreased mTOR activity and tumor cell proliferation, which suggests metformin may also have an anticancer effect on mTOR independent of AMPK activation.
In addition to their in vitro studies, Vitale-Cross, et al. [9] have also studied the effects of metformin in an oral specific carcinogenesis mouse model. In their study, mice were first treated with 4-Nitroquinoline-1-oxide (4NQO; Sigma-Aldrich), which is a synthetic carcinogen that causes the development of oral cavity tumors. With time, many of these tumors progress to carcinoma. In the animals treated with metformin, there was a significant reduction in the number of overall tumor lesions, as well as a significant decrease in the progression of these tumors to carcinoma.
Further laboratory studies from MD Anderson also suggest that metformin may offer some potential benefit for patients with HN SCC [17]. Specifically, these studies demonstrated that HN SCC cells with “disruptive” p53 mutations, defined as mutations that affect the p53 protein’s binding to DNA, demonstrated increased radiosensitivity when treated with metformin [17]. To further support their in vitro findings, this laboratory next analyzed the effects of metformin use on oral tongue SCC in an orthotopic mouse model. They discovered that tumor growth was significantly decreased when metformin was given in addition to radiation therapy compared to only radiation or metformin use alone. Furthermore, they also retrospectively analyzed the treatment effects of metformin use during post-operative radiation on the outcomes of a small cohort of patients with HN SCC. Their study population included 10 patients with HN SCC taking metformin during post-operative radiation therapy, and the outcomes were compared to patients with similar disease and clinical characteristics who were not taking metformin during post-operative radiation. They found that the patients using metformin had significantly decreased locoregional recurrence compared to controls.
Despite these promising studies with HN SCC, our larger clinical study does not support metformin’s potential benefit. We specifically analyzed the effects of metformin use in diabetic patients with OC/OP SCC and did not find any significant impact for metformin in disease recurrence for early (I and II) or late (III and IV) stage patients (Figures 1 and 2). The finding that metformin did not have a significant effect in late stage tumors is not entirely surprising (HR 0.84, 95% CI 0.34 - 2.10, p = 0.71), considering that increased stage and regional or distant metastases have already been shown to be significantly poor prognostic factors [18,19]. The anticancer effect of metformin likely cannot overcome the advanced disease state.
5. Conclusion
This is the largest clinical study to date evaluating the effects of metformin on recurrence rates in diabetic patients with head and neck cancer. The dismal and unchanging prognosis of OC/OP SCC despite treatment advancements has fueled interest into the identification of factors and additional therapies that can improve treatment outcomes. Although metformin has been shown to have a beneficial effect in patients with various malignancies, the results from our study do not suggest that metformin decreases recurrence for diabetic patients with OC/OP SCC. Further study with a larger cohort may be useful to confirm our findings.
6. Acknowledgements
Kim Nguyen, MD and Brandon J. Kim, BS of the UCLA Department of Head and Neck Surgery contributed to the collection and presentation of the data. Support for statistical analyses was provided by the UCLA CTSI, NIH grant number UL1TR000124.
REFERENCES
- H. T. Hoffman, L. H. Karnell, G. F. Funk, et al., “The National Cancer Data Base Report on Cancer of the Head and Neck,” Archives of Otolaryngology—Head and Neck Surgery, Vol. 124, No. 9, 1998, pp. 951-962.
- S. Silverman, “Demographics and Occurrences of Oral and Pharyngeal Cancers. The Outcomes, the Trends, the Challenge,” The Journal of the American Dental Association, Vol. 132, Supplement 7S-11S, 2001, pp. 7s-11s.
- G. L. Day and W. J. Blot, “Second Primary Tumors in Patients with Oral Cancer,” Cancer, Vol. 70, 1992, pp. 14-19. doi:10.1002/1097-0142(19920701)70:1<14::AID-CNCR2820700103>3.0.CO;2-S
- L. G. Morris, A. G. Sikora, R. B. Hayes, S. G. Patel and I. Ganly, “Anatomic Sites at Elevated Risk of Second Primary Cancer after an Index Head and Neck Cancer,” Cancer Causes & Control, Vol. 22, No. 5, 2011, pp. 671- 679. doi:10.1007/s10552-011-9739-2
- R. Rattan, R. Ali Fehmi and A. Munkarah, “Metformin: An Emerging New Therapeutic Option for Targeting Cancer Stem Cells and Metastasis,” Journal of Oncology, Vol. 2012, 2012, Article ID: 928127. doi:10.1155/2012/928127
- K. Hosono, H. Endo, M. Sugiyama, et al., “Metformin Suppresses Colorectal Aberrant Crypt Foci in a ShortTerm Clinical Trial,” Cancer Prevention Research (Philadelphia), Vol. 3, No. 9, 2010, pp. 1077-1083. doi:10.1158/1940-6207.CAPR-10-0186
- T. M. Chen, C. C. Lin, P. T. Huang and C. F. Wen, “Metformin Associated with Lower Mortality in Diabetic Patients with Early Stage Hepatocellular Carcinoma after Radiofrequency Ablation,” Journal of Gastroenterology and Hepatology, Vol. 26, No. 5, 2011, pp. 858-865. doi:10.1111/j.1440-1746.2011.06664.x
- N. Sadeghi, J. L. Abbruzzese, S. C. Yeung, M. Hassan and D. Li, “Metformin Use Is Associated with Better Survival of Diabetic Patients with Pancreatic Cancer,” Clinical Cancer Research, Vol. 18, No. 10, 2012, pp. 2905-2912. doi:10.1158/1078-0432.CCR-11-2994
- L. Vitale-Cross, A. A. Molinolo, D. Martin, et al., “Metformin Prevents the Development of Oral Squamous Cell Carcinomas from Carcinogen-Induced Premalignant Lesions,” Cancer Prevention Research (Philadelphia), Vol. 5, No. 4, 2012, pp. 562-573. doi:10.1158/1940-6207.CAPR-11-0502
- E. Giovannucci, D. M. Harlan, M. C. Archer, et al., “Diabetes and Cancer: A Consensus Report,” Diabetes Care, Vol. 33, No. 7, 2010, pp. 1674-1685. doi:10.2337/dc10-0666
- R. J. Dowling, P. J. Goodwin and V. Stambolic, “Understanding the Benefit of Metformin Use in Cancer Treatment,” BMC Medicine, Vol. 9, No. 33, 2011, pp. 1-6. doi:10.1186/1741-7015-9-33
- S. Jiralerspong, S. L. Palla, S. H. Giordano, et al., “Metformin and Pathologic Complete Response to Neoadjuvant Chemotherapy in Diabetic Patients with Breast Cancer,” Journal of Clinical Oncology, Vol. 27, No. 20, 2009, pp. 3297-3302. doi:10.1200/JCO.2009.19.6410
- H. P. Chen, J. J. Shieh, C. C. Chang, et al., “Metformin Decreases Hepatocellular Carcinoma Risk in a DoseDependent Manner: Population-Based and in Vitro Studies,” Gut, Vol. 62, No. 4, 2013, pp. 606-615.
- C. H. Tseng, “Diabetes, Metformin Use, and Colon Cancer. A Population-Based Cohort Study in Taiwan,” European Journal of Endocrinology, Vol. 167, No. 3, 2012, pp. 409-416. doi:10.1530/EJE-12-0369
- I. Ben Sahra, Y. Le Marchand-Brustel, J. F. Tanti and F. Bost, “Metformin in Cancer Therapy: A New Perspective for an Old Diabetic Drug,” Vol. 9, No. 5, 2010, pp. 1092- 1099.
- M. F. McCarty, “MTORC1 Activity as a Determinant of Cancer Risk-Rationalizing the Cancer-Preventive Effects of Adiponectin, Metformin, Rapamycin, and Low-Protein Vegan Diets,” Medical Hypotheses, Vol. 77, No. 4, 2011, pp. 642-648. doi:10.1016/j.mehy.2011.07.004
- H. D. Skinner, V. C. Sandulache and T. J. Ow, et al., “TP53 Disruptive Mutations Lead to Head and Neck Cancer Treatment Failure through Inhibition of Radiation-Induced Senescence,” Clinical Cancer Research, Vol. 18, No. 1, 2012, pp. 290-300. doi:10.1158/1078-0432.CCR-11-2260
- S. Sklenicka, S. Gardiner, E. J. Dierks, B. E. Potter and R. B. Bell, “Survival Analysis and Risk Factors for Recurrence in Oral Squamous Cell Carcinoma: Does Surgical Salvage Affect Outcome?” Journal of Oral and Maxillofacial Surgery, Vol. 68, No. 6, 2010, pp. 1270-1275. doi:10.1016/j.joms.2009.11.016
- D. H. Lee, M. J. Kim, J. L. Roh, et al., “Distant Metastases and Survival Prediction in Head and Neck Squamous Cell Carcinoma,” Otolaryngology—Head and Neck Surgery, Vol. 147, No. 5, 2012, pp. 870-875. doi:10.1016/j.joms.2009.11.016
NOTES
*No financial funding or support. Conflict of interest: none.
#Corresponding author.

