Surgical Science
Vol.06 No.12(2015), Article ID:62452,10 pages
10.4236/ss.2015.612080
Incisional Negative Pressure Wound Therapy in the Prevention of Surgical Site Infection after Vascular Surgery with Inguinal Incisions: Rationale and Design of a Randomized Controlled Trial (INVIPS-Trial)
Julien Hasselmann1*, Tobias Kühme1, Jonas Björk2, Stefan Acosta1
1Vascular Center, Skåne University Hospital, Malmö, Sweden
2Division of Occupational and Environmental Medicine, Lund University, Lund, Sweden

Copyright © 2015 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 15 November 2015; accepted 27 December 2015; published 30 December 2015
ABSTRACT
Background/Aims: Inguinal incisions are a common route of access in vascular surgery. Due to anatomical challenges and a diverse bacterial flora in this area, surgical site infections (SSI) re- present a common, debilitating and sometimes life-threatening complication. The INVIPS-Trial evaluates the role of Negative Pressure Wound Therapy (NPWT) on closed inguinal incisions in elective vascular surgery to prevent SSI and other wound complications. Methods: This randomized controlled trial (RCT) registered at ClinicalTrials.gov (Identifier: NCT01913132) compares the effects of a NPWT dressing (PICO, Smith & Nephew, UK) and the center’s standard wound dressing (Vitri Pad, ViTri Medical, Sweden) on postoperative wound complications, especially SSI. The study includes two distinct vascular procedures with different SSI risk profiles: endovascular aortic repair (EVAR) and open surgical approaches involving the common femoral artery (OPEN). Results: Four hundred ninety-five groin incisions in both treatment arms are anticipated to be included in the EVAR group and 147 inguinal incisions in both treatment arms in the OPEN group. Since a large percentage of inguinal vascular procedures in both groups but especially in the EVAR group are performed bilaterally, many patients can serve as their own control by randomly receiving NPWT on one and the standard dressing on the contralateral inguinal incision. Conclusions: This ongoing RCT attempts to elucidate the potential benefit of NPWT on closed inguinal incisions after different vascular procedures. Outcome and conclusions of this trial could have implications on postoperative wound care of patients in both vascular surgery and other surgical specialties.
Keywords:
Incisional Negative Pressure Wound Therapy, Vascular Surgery, Inguinal Incisions, Surgical Site Infection, Randomized Controlled Trial, Research Design

1. Introduction
Vascular surgery today relies heavily on inguinal access for both endovascular and open surgical procedures. Unfortunately, the inguinal region contains a high concentration of virulent bacteria [1] , is fairly moist, a high risk area for postoperative lymphorrhea [2] and traverses the hip joint, thereby exposing it to friction and stretching forces. These factors increase the risk for surgical site infections (SSI) and infection rates of more than 20% [3] have been reported. SSI in vascular surgery are associated with significant risks for potentially fatal bleeding complications, limb loss, long inpatient length of stay and represent a significant financial burden. [4]
Negative pressure wound therapy (NPWT) has been established as an alternative treatment for chronic and infected wounds. Its application on closed, clean incisions, also called ‘incisional NPWT’ (INPWT), on the other hand is a more recent development. In the latest Cochrane review [5] evaluating INPWT on skin grafts, orthopedic, general surgery and trauma patients in nine trials with 785 participants, it was concluded that evidence for the effects of INPWT for reducing SSI and wound dehiscence remains unclear. The authors further advocate suitably powered, high-quality trials to evaluate INPWT.
Although the exact mechanism of action of INPWT and how it might be beneficial in the wound healing process has not yet been established, some works attempting to elucidate different factors are emerging. It has been demonstrated that INPWT decreases hematoma and seroma formation not only by removal of wound fluid across the suture line but also by locally enhancing the endogenous draining capacity of the lymphatic system [6] . This has shown to reduce drainage time in orthopedic patients. [7] The mechanism behind the amplification of lymphatic function is unknown but alternatives to the theory of merely locally increased tissue pressures are under discussion.
Wilkes et al. conducted bench-top and computer modelling experiments to evaluate a INPWT device (PrevenaTM, KCI, San Antonio, TX) and showed less biomechanical stress around skin and subcutaneous suture lines. [8] This may facilitate tissue apposition, creating a better microbial barrier and potentially even decrease scar formation. Although NPWT applied to open wounds is known to create positive tissue pressures [9] and associated microvascular perfusion changes, a recent study comparing biological effects of the canister-free PICOTM- system (Smith and Nephew, UK) to traditional systems found little effects on perfusion in incisional wounds. [10]
The relatively high frequency of SSI in the groin in combination with a well-established follow-up program at this center, represented good conditions to study interventions aimed at decreasing the inguinal SSI rate. Since a pharmacological approach with a change of the center’s antibiotic prophylaxis failed to improve SSI rates [11] , a randomized controlled trial (RCT) to assess the role of INPWT on inguinal vascular surgical incisions was initiated in 2013. The fact that a large proportion of inguinal procedures at this center are conducted bilaterally, allowed for a unique study design whereby patients could receive the INPWT dressing in one and the standard dressing in other groin, thereby serving as their own controls (Figure 1).
2. Material and Methods
2.1. Overall Design
Single center randomized controlled clinical trial.
2.2. Study Objectives
The study was initiated to determine whether a prophylactic negative pressure wound therapy pad (PICOTM) applied after vascular surgical procedures with inguinal incisions could reduce the surgical site infection rate as well as the frequency of other wound complications such as delayed healing, lymphorrhea, seroma and
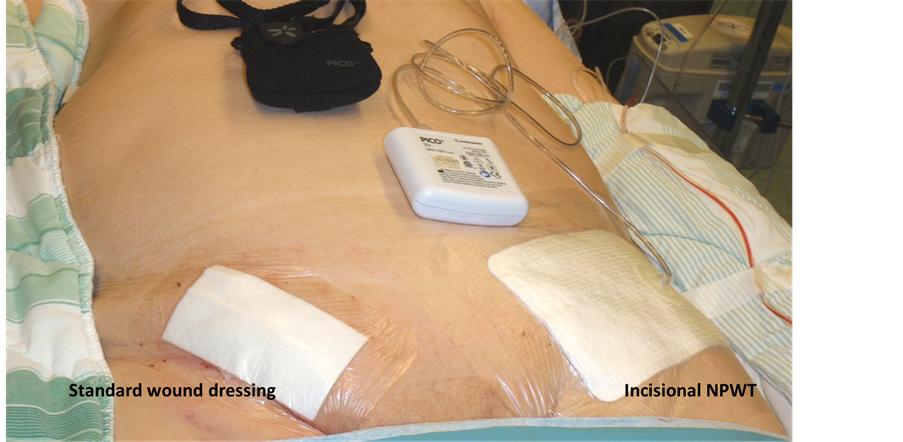
Figure 1. Standard dressing applied in the right and PICO dressing in the left groin after endovascular aortic repair in a patient with abdominal aortic aneurysm.
hematoma when compared to the standard wound dressing (Vitri Pad, ViTri Medical, Sweden).
2.3. Endpoints
The primary endpoint is the development of SSI and other wound complications within the first 90 days postoperatively. Secondary endpoints are occurrence of SSI and other wound complications up to one year postoperatively as well as mortality in the different treatment groups.
2.4. Setting
The Vascular Center, Malmö-Lund, Skåne University Hospital, is a tertiary referral center for the southernmost part of Sweden with a primary catchment population of 800,000 inhabitants. The center possesses a well-estab- lished postoperative follow-up program for all patients undergoing vascular surgery.
2.5. Eligibility Criteria
All adult patients without ongoing infection undergoing elective vascular procedures with inguinal incisions are eligible to participate.
2.6. Enrollment and Randomization
Patients scheduled for vascular surgical procedures with inguinal incisions are provided with written information before undergoing the admission procedure which takes place one to two weeks prior to scheduled surgery. During the admission process, the background and aim of the study are discussed with eligible patients, informed consent obtained and the randomization conducted by outpatient clinic nurses. In this study we apply simple randomization using an opaque randomization envelope containing equal numbers of “PICO” and “standard” notes. In bilateral groin incisions, the draw from the envelope dictates the wound dressing selection in the right inguinal incision and the contralateral incision is automatically assigned the alternate dressing. Randomization outcome and consent form are documented in the patient’s records.
2.7. Ethical Considerations
The study has been approved by the regional ethical review board (Dnr 2013/322) and has been registered at ClinicalTrials.gov (Identifier: NCT01913132).
2.8. The Wound Dressings
There is no difference between the surgical procedures and perioperative care between the treatment and control groups. At the end of the procedure, wounds are sutured intracutanously in case of horizontal incisions whereas vertical incisions are closed according to surgeon’s preference. Steri-StripsTM (3M, St Paul, Minnesota) are often applied in case of intracutanous sutures. PICOTM is a negative pressure system employing −80 mm∙Hg continuous suction generated through a canister-free portable pump. The PICOTM dressing eliminates fluid predominantly by evaporative loss. It is directly applied onto the closed incisions and, according to the manufacturer’s recommendation, left in place for seven days, after which it stops working and can be removed by the patients themselves or nurses at the center’s outpatient clinic.
Vitri Pad is the institution’s standard wound dressing consisting of a sterile water-proof bandage with absorbent pad. Consistent with the recommendation of the Centers for Disease Control and Prevention (CDC) [12] it is left in place for at least 48 hours postoperatively.
2.9. Data Collection and Management
All data is collected using SPSS for Mac, version 22.0 (SPSS Inc., Chicago, Illinois, USA). The data is collected per groin incision as opposed to per patient and stems from the patient’s electronic records, the regional microbiological laboratory, the central transfusion registry as well as content from conducted phone interviews after three and twelve months postoperatively. Visits at the outpatient clinic are scheduled in line with the clinic’s and the Swedish vascular registry’s guidelines at one and twelve months postoperatively (Figure 2). The following variables are registered (Table 1).
2.10. Preoperative Data
Data collected preoperatively are identification number, age at operation, date of procedure, indication for procedure, gender, height (in cm), weight (in kg), body mass index (BMI, in kg/m2), ischemic heart disease (yes/no), atrial fibrillation (yes/no), arterial hypertension (yes/no), diabetes mellitus (yes/no), type of diabetes mellitus (regulated with diet only, oral anti-diabetic drugs, insulin-dependent), current smoker (yes/no), ex-smoker (yes/no) [according to the Centers for Disease Control and Prevention smoking status description: ex-smoker ≥ 100 cigarettes during lifetime [13] , history of cerebrovascular insult (yes/no), previous inguinal surgery on the side where the groin incision is performed (yes/no), previous extracardiac vascular surgery (yes/no), critical ischemia (yes/no), foot wound (yes/no), anticoagulation with warfarin (yes/no), rivaroxaban (yes/no) or dabigatran (yes/no), American Society of Anesthesiologists (ASA) score, use of systemic corticosteroids (yes/no), use of acetylsalicyclic acid (yes/no), type of procedure, groin (right/left), randomization (PICO/standard dressing).
2.11. Perioperative Data
Preoperative antibiotic treatment excluding antibiotic prophylaxis (yes/no), preoperative antibiotic prophylaxis
Figure 2. Study time flow.
Table 1. Data collection schedule.
ASA score = American Society of Anesthesiologists score, SSI = Surgical site infection, CT = Computed Tomography.
received (yes/no), preoperative anemia (yes/no), preoperative blood glucose concentration (mmol/L), preoperative albumin concentration (g/L), preoperative estimated glomerular filtration rate (ml/min), form of anesthesia (general/regional/local), groin incision performed (yes/no), bilateral incision (yes/no), vertical incision (yes/no), transverse incision (yes/no), use of wound products such as Floseal® (yes/no), Hemopatch® (yes/no), Tachosil® (yes/no) (all Baxter Healthcare Corporation, Deerfield, IL, USA), Collatamp® (EUSA Pharma, Oxford, UK) (yes/no), stent graft used (yes/no), synthetic graft used (yes/no), bovine pericardial patch used (yes/no), any patch used (yes/no), any foreign material applied in wound (yes/no), vein graft/patch (yes/no), arterial graft (yes/no), closure technique in case of EVAR (cutdown/fascia suture), duration of procedure (min), bypass (yes/no), wound dressing received (PICO/standard), postoperative antibiotic therapy (yes/no), number of transfused units of packed red blood cells, plasma and thrombocyte concentrates, postoperative treatment at intensive care unit (yes/no), inpatient length of stay (days).
2.12. Follow-Up Data
Readmission within 30 days postoperatively (yes/no), surgical site infection (SSI) within 30 days (yes/no), wound culture obtained within first 3 months postoperatively (yes/no), pseudoaneurysm formation on computed tomography follow-up 30 days (yes/no), reoperation 30 days (yes/no), sought medical attention because of groin problem within 90 days (yes/no), reoperation 90 days (yes/no), SSI 90 days (yes/no), reoperation 1 year (yes/no), SSI 1 year (yes/no), wound cultures within 1 year (yes/no), 1 year mortality (yes/no), mortality due to groin infection (yes/no), type of bacterial isolate, SSI grading according to Szilagyi classification, C-reactive protein concentration at infection diagnosis (mg/L), presenting symptoms, surgical revision (yes/no), negative pressure wound therapy after surgical revision (yes/no), sepsis (yes/no), bleeding (yes/no), wound dehiscence (yes/no), seroma (yes/no), hematoma (yes/no), lymphorrhea (yes/no), amputation within 1 year (yes/no).
The diagnosis SSI is made according to the 1999 diagnostic criteria defined by the Centers for Disease Control and Prevention, USA. [12] In addition, diagnosed infections involving grafts are graded based on the Szilagyi classification [14] which is a tool often used to describe SSI in vascular surgery with prosthetic implants. The data analysis and subsequent establishment of the diagnosis SSI or other wound complications is done under blinded conditions. The investigator does not know whether a particular groin incision was treated with NPWT or the standard wound dressing.
The primary analysis principle applied will be intention-to-treat. The only condition for initial inclusion is application of the correct wound dressing at the end of the procedure. Exclusion criteria are death or re-operation before reaching the primary or secondary endpoints. As a safety aspect, we will conduct a mortality analysis in the treatment groups.
2.13. Statistical Issues
We defined two main groups of vascular surgical procedures with groin incisions that carry different infection risk profiles. Infection rates and other statistics stem from a review of data collected during four consecutive months in 2013 after changing the center’s antibiotic prophylaxis from cloxacillin administered intravenously at three time points to trimethoprim/sulfamethoxazole administered orally once in the morning of the operation. [11] In preparation for the INVIPS-Trial (Incisional NPWT on vascular surgical inguinal incisions in the prevention of SSI), we conducted a reanalysis of the 2013 material and focused on elective procedure outcomes only.
In about 80% of cases, endovascular aortic repair (EVAR) requires a bilateral inguinal approach whereby the transverse incisions are conducted at the end of the procedure and merely serve to repair the femoral artery defect created by the introduction of endovascular material. This type of procedure carries an infection risk of about 4.4% at this center. Mortality in this group was 4.4% at three and 6.7% at twelve months.
Open inguinal procedures (OPEN) such as thrombendarterectomies (TEA) and arterial bypass operations with vertical incisions involving the femoral artery in the groin have a much higher infection rate of about 30%. Bilateral inguinal approaches were performed in 24% in this procedure category. Three and twelve-month mortality was 0%.
The different characteristics of these endovascular and open procedures have to be taken into account when conducting sample size determination and statistical analysis planning.
2.14. Sample Size Calculation
We used G*Power 3.1 [15] software for power calculations. We first conducted power calculations, 80% power at 5% significance level, assuming all cases were either unilateral (Fisher’s exact test, sample size n1) or bilateral (McNemar’s test, sample size n2). Central to the power analysis of bilateral cases is the proportion of discordant pairs, meaning the proportion of outcomes that differ between the two sides, e.g. the proportion of cases where an infection is observed on one but not the other side. Assuming for instance a SSI rate reduction from 30% to 10% in bilateral open inguinal procedures, the proportion of cases in which the infection outcome is different in the right and left groin wounds respectively has to be at least as large as the difference between the current SSI rate with the standard dressing and the predicted SSI rate with the PICOTM system (30% − 10% = 20%). The proportion of discordant pairs needs to be larger than the difference in SSI rate to account for the possibility that some patients may suffer from an infection on the PICO dressing side and not the standard dressing side. After having determined the required sample sizes for the uni-and bilateral scenarios individually, the final sample size required was calculated as a weighted average based on the expected proportion (p) of unilateral and bilateral operations (Table 2).
EVAR
Previous data indicated an inguinal SSI rate of 4.4% when using the standard dressing. For bilateral cases, we estimated the proportion of discordant pairs to be 5%. Assuming all cases are either unilateral or bilateral, and a reduction in SSI rate from 4.4% to 1.0%, yields n1 = 750, and n2 = 340, respectively. Among all EVAR-cases, 20% are assumed to be unilateral (i.e. p1 = 0.2):
n = p1 × n1 + (1 − p1) × n2. n = 0.2 × 750 + 0.8 × 340 = 422
Taking into account the previously identified 12-month mortality of 6.7%, yields a mortality-corrected sample size of n = 452 (422/(1 − 0.067)).
In an attempt to adjust for other types of “loss to follow-up” such as missing data and re-operations on the respective side, we added an additional 10% (45 cases) resulting in a total sample size of 497.
OPEN
Previous data indicated an inguinal SSI rate of 30% when using the standard dressing. Assuming all cases are either unilateral or bilateral, and a reduction in SSI rate from 30% to 10% with a proportion of discordant pairs of 25% in bilateral cases yields n1 = 138 and n2 = 120, respectively. Among all Open-cases, 76% are assumed to be unilateral (i.e. p1 = 0.76):
n = p1 × n1 + (1 − p1) × n2. n = 0.76 × 138 + 0.24 × 122 = 134
The 12-month mortality in this group was 0%. To adjust for other types of “loss to follow-up”, we added an additional 10% (13 cases) resulting in a total sample size of 147.
Table 2. Characteristics of the two main types of procedures studied.
1Based on earlier data collection, 2n = required number of groin incisions, EVAR = Endovascular aortic repair, SSI = Surgical site infection.
2.15. Statistical Analysis
We will conduct a descriptive analysis of background data such as comorbidities, procedure-related risk factors and different operation techniques. Important differences will be accounted for in a sensitivity analysis.
The study involves both uni-and bilateral inguinal incisions. Unilateral incisions are treated with either standard or NPWT dressing according to the randomization result and analyzed with Fisher’s exact test for independent samples. In case of bilateral incisions, one is randomly designated to either standard or NPWT treatment group, the other by default to the alternate treatment group. It is important to recognize that the outcomes in the treatment groups in this scenario will most likely not be independent of one another and will therefore be analyzed with McNemar’s test for paired data. The advantage of the bilateral design is that all patient-related risk factors, such as comorbidities and hygiene factors, are exactly the same in both treatment groups and patients serve as their own control. The bilateral design thus decreases the required group size at a fixed level of statistical power, as can be seen from the assessments of n1 and n2 above. The obtained p-values from the uni- and bilateral analyses will subsequently be combined to an overall p-value using Fisher’s method of combining p-values [16] . By using McNemar’s test for analysis of bilateral incisions, we avoid the problem of “clustering” due to statistically dependent observations which, if not accounted for, would lead to too small standard errors and p-values [17] .
3. Discussion
Vascular surgery with inguinal incisions carries a significant risk for surgical site infections. This is true for endovascular but even more so for open procedures.
INPWT could be an important tool in the postoperative care of these anatomically and microbiologically challenging wounds. Although various mechanisms of action of this technique have been described, a central effect of INPWT in this anatomical location could simply be to provide a protective cover to the healing wound. The constant suction that is being applied by the INPWT-system provides a highly-adaptive surface that prevents kinking and a subsequent breach of the sterile barrier resulting in bacterial contamination during movements of the hip joint.
In this study, only elective procedures were included. That is partially because we observed much higher SSI rates among elective cases but also due to the fact that only elective patients are able to follow hygiene and other routines thereby limiting the amount of uncontrollable variables. In addition, there are some obvious ethical concerns linked to the inclusion of acute patients that could be avoided.
A potential limitation of this study could be that the randomization takes place before the operation, not at its end. One might argue that this could create bias since the surgeon in charge, theoretically, could be aware of the respective randomization outcome before conducting the operation. In addition, only inguinal sites that in fact are subject to surgical incisions would be randomized if randomized at the end of procedure. In the current setup, a few randomized treatment outcome results needs to be excluded postoperatively if percutaneous vascular closure devices are used instead of incision followed by fascial closure or open vascular repair or if no incision is performed on one side.
In our view, the most compelling argument against intraoperative randomization was that the large number of rotating on-duty operating room personnel would make it very difficult to achieve the necessary sense of awareness for the study and to thereby limit the amount of missed randomizations. In addition, the logistics in the operating room are not such that randomization envelopes could easily be accessible.
When conducting the three-month survey of vascular procedures with groin incisions at this center in 2013, it was noteworthy that open procedures carried a 0% one-year mortality. Because this was most likely just by chance, one could argue that the estimated sample size for the OPEN arm of the INVIPS-Trial should be corrected upwards to account for a likely higher mortality. We did however feel that a correction not based on our own data would somehow be arbitrary.
In a retrospective comparative cohort analysis, highly prone to the Hawthorne effect [18] , INPWT seemed to provide good results after femoral vascular procedures. [19] The aim of this randomized controlled trial is to provide more conclusive evidence as to the effects of INPWT after vascular surgery with groin incisions. To avoid bias, the authors have decided to publish the rational and methods of this study, especially the sample size calculation, prior to enrollment completion and analysis. The results of the trial could not only be important for postoperative wound management in vascular patients, but could be relevant to other specialties conducting operations with inguinal incisions.
Fund
The research group has received an unrestricted unconditional research grant 15,550 USD and donation of 100 PICO dressing kits from Smith and Nephew in 2013. We have also received 12,900 USD from the Swedish SUS Stiftelser och Fonder: Grant-number 95407.
The trial is registered at ClinicalTrials.gov (Identifier: NCT01913132).
Cite this paper
Julien Hasselmann,Tobias Kühme,Jonas Björk,Stefan Acosta, (2015) Incisional Negative Pressure Wound Therapy in the Prevention of Surgical Site Infection after Vascular Surgery with Inguinal Incisions: Rationale and Design of a Randomized Controlled Trial (INVIPS-Trial). Surgical Science,06,562-571. doi: 10.4236/ss.2015.612080
References
- 1. Grice, E.A. and Segre, J.A. (2011) The Skin Microbiome. Nature Reviews Microbiology, 9, 244-253.
http://dx.doi.org/10.1038/nrmicro2537 - 2. Giovannacci, L., Renggli, J.C., Eugster, T., Stierli, P., Hess, P. and Gurke, L. (2001) Reduction of Groin Lymphatic Complications by Application of Fibrin Glue: Preliminary Results of a Randomized Study. Annals of Vascular Surgery, 15, 182-185.
http://dx.doi.org/10.1007/s100160010049 - 3. Turtiainen, J., Saimanen, E., Partio, T., et al. (2010) Surgical Wound Infections after Vascular Surgery: Prospective Multicenter Observational Study. Scandinavian Journal of Surgery, 99, 167-172.
- 4. Engin, C., Posacioglu, H., Ayik, F. and Apaydin, A.Z. (2005) Management of Vascular Infection in the Groin. Texas Heart Institute Journal, 32, 529-534.
- 5. Webster, J., Scuffham, P., Stankiewicz, M. and Chaboyer, W.P. (2014) Negative Pressure Wound Therapy for Skin Grafts and Surgical Wounds Healing by Primary Intention. Cochrane Database of Systematic Reviews, 10, Article ID: CD009261.
http://dx.doi.org/10.1002/14651858.cd009261.pub3 - 6. Kilpadi, D.V. and Cunningham, M.R. (2011) Evaluation of Closed Incision Management with Negative Pressure Wound Therapy (CIM): hematoma/seroma and involvement of the lymphatic system. Wound Repair and Regeneration, 19, 588-596.
http://dx.doi.org/10.1111/j.1524-475X.2011.00714.x - 7. Stannard, J.P., Robinson, J.T., Anderson, E.R., McGwin Jr., G., Volgas, D.A. and Alonso, J.E. (2006) Negative Pressure Wound Therapy to Treat Hematomas and Surgical Incisions Following High-Energy Trauma. The Journal of trauma, 60, 1301-1306.
http://dx.doi.org/10.1097/01.ta.0000195996.73186.2e - 8. Wilkes, R.P., Kilpad, D.V., Zhao, Y., Kazala, R. and McNulty, A. (2012) Closed Incision Management with Negative Pressure Wound Therapy (CIM): Biomechanics. Surgical Innovation, 19, 67-75.
http://dx.doi.org/10.1177/1553350611414920 - 9. Eisenhardt, S.U., Schmidt, Y., Thiele, J.R., et al. (2012) Negative Pressure Wound Therapy Reduces the Ischaemia/ Reperfusion-Associated Inflammatory Response in Free Muscle Flaps. Journal of Plastic Reconstructive and Aesthetic Surgery, 65, 640-649.
http://dx.doi.org/10.1016/j.bjps.2011.11.037 - 10. Malmsjo, M., Huddleston, E. and Martin, R. (2014) Biological Effects of a Disposable, Canisterless Negative Pressure Wound Therapy System. Eplasty, 14, e15.
- 11. Hasselmann, J., Kuhme, T. and Acosta, S. (2015) Antibiotic Prophylaxis with Trimethoprim/Sulfamethoxazole Instead of Cloxacillin Fails to Improve Inguinal Surgical Site Infection Rate after Vascular Surgery. Vascular and Endovascular Surgery, 49, 129-134.
http://dx.doi.org/10.1177/1538574415600531 - 12. Mangram, A.J., Horan, T.C., Pearson, M.L., Silver, L.C. and Jarvis, W.R. (1999) Guideline for Prevention of Surgical Site Infection, 1999. Centers for Disease Control and Prevention (CDC) Hospital Infection Control Practices Advisory Committee. American Journal of Infection Control, 27, 97-132; Quiz 3-4; Discussion 96.
http://dx.doi.org/10.1016/S0196-6553(99)70088-X - 13. Schoenborn, C.A. and Adams, P.E. (2010) Health Behaviors of Adults: United States, 2005-2007. Vital and Health Statistics, Series 10, 1-132.
- 14. Szilagyi, D.E., Smith, R.F., Elliott, J.P. and Vrandecic, M.P. (1972) Infection in Arterial Reconstruction with Synthetic Grafts. Annals of Surgery, 176, 321-333.
http://dx.doi.org/10.1097/00000658-197209000-00008 - 15. Faul, F., Erdfelder, E., Buchner, A. and Lang, A.G. (2009) Statistical Power Analyses Using G*Power 3.1: Tests for Correlation and Regression Analyses. Behavior Research Methods, 41, 1149-1160.
http://dx.doi.org/10.3758/BRM.41.4.1149 - 16. Fisher, R.A. (1925) Statistical Methods for Research Workers. Oliver & Boyd, Edinburgh.
- 17. Roberts, C. and Roberts, S.A. (2005) Design and Analysis of Clinical Trials with Clustering Effects Due to Treatment. Clinical Trials, 2, 152-162.
http://dx.doi.org/10.1191/1740774505cn076oa - 18. McCambridge, J., Witton, J. and Elbourne, D.R. (2014) Systematic Review of the Hawthorne Effect: New Concepts Are Needed to Study Research Participation Effects. Journal of Clinical Epidemiology, 67, 267-277.
http://dx.doi.org/10.1016/j.jclinepi.2013.08.015 - 19. Matatov, T., Reddy, K.N., Doucet, L.D., Zhao, C.X. and Zhang, W.W. (2013) Experience with a New Negative Pressure Incision Management System in Prevention of Groin Wound Infection in Vascular Surgery Patients. Journal of Vascular Surgery, 57, 791-795.
http://dx.doi.org/10.1016/j.jvs.2012.09.037
NOTES
*Corresponding author.