International Journal of Clinical Medicine
Vol.3 No.4(2012), Article ID:20892,8 pages DOI:10.4236/ijcm.2012.34054
Psychotropic Drug Prescribing Trends in Bahrain: Implications for Sexual Functions
![]()
1Department of Pharmacology & Therapeutics, Arabian Gulf University, Manama, Bahrain; 2Department of Psychiatry, Arabian Gulf University, Manama, Bahrain; 3Psychiatric Hospital, Ministry of Health, Manama, Bahrain.
Email: *khlidj@agu.edu.bh
Received March 16th, 2012; revised April 28th, 2012; accepted May 4th, 2012
Keywords: Psychotropic-Associated Sexual Dysfunction; Prescription Audit; Antidepressants; Antipsychotics; Psychiatrists
ABSTRACT
Treatment-emergent sexual dysfunction is a frequent adverse effect of many psychotropic drugs. We have analyzed the prescribing trends and the likelihood of psychotropic-associated sexual dysfunction in outpatients with depression or other psychotic disorders treated by psychiatrists. A retrospective prescription audit was conducted at the Psychiatric Hospital, the only psychiatric facility in Bahrain that offers both inpatient and outpatient services. Psychotropic associated sexual dysfunction was graded as negligible (0), moderate (2+), moderately severe (3+) and uncertain (U) for antidepressants, and for antipsychotics as no effect (0), very low (1+), moderate (2+), moderately severe (3+) and uncertain (U) effect. As antidepressant monotherapy, a significant trend towards prescribing selective serotonin reuptake inhibitors (SSRIs; 3+) and selective norepinephrine reuptake inhibitors (SNRIs; 3+) in females, and tricyclic antidepressants (TCAs; 2+) in males was apparent. Atypical antidepressant mirtazapine (0) monotherapy was rarely prescribed. Mirtazapine with SSRIs or SNRI was the most often prescribed combinations followed by TCAs with other antidepressants. Risperidone (0 to 3+), an atypical antipsychotic, was the most popular antipsychotic prescribed to augment antidepressants; there was no gender-based difference. Clozapine (0) and olanzapine (1+) were rarely prescribed to augment antidepressant therapy. In Bahrain, the psychotropic prescribing trends suggest that there is a need to optimize drug therapy to achieve the therapeutic goal with minimal adverse impact on sexual function.
1. Introduction
Sexual dysfunction is a common symptom of depression and its prevalence approaches 70% in untreated depression [1]. Treatment—emergent sexual dysfunction is a frequent adverse effect of many antidepressants such as tricyclics (TCAs), selective serotonin reuptake inhibitors (SSRIs), selective norepinephrine reuptake inhibitors (SNRIs) and monoamine oxidase inhibitors (MAOIs) [1,2]. Sexual dysfunction is also common in patients with schizophrenia [3,4]. Antipsychotic drugs in general and typical antipsychotics in particular indicated for treating a range of psychiatric disorders are well known to produce sexual dysfunction [5-7]; elevation of plasma prolactin levels resulting from D2 receptor blockade has been implicated [6-9]. In both men and women, prolactinrelated disruption of the hypothalamic-pituitary-gonadal axis can lead to decreased libido and impaired sexual function [10]. Elevated prolactin levels can impair the sexual function by decreasing testosterone in male [6] or estradiol in female [7]. Erectile dysfunction and associated sexual dysfunctions (delayed ejaculation, anorgasmia, and decreased libido) secondary to antidepressant therapy may occur in up to 90% of men [11]. Although men experience a greater incidence of antidepressantassociated sexual dysfunction, women experience severe sexual dysfunction [12,13]. Whereas the incidence of antipsychotic-associated sexual dysfunction has been reported to be greater in men than in women, the severity of and tolerance to sexual dysfunction were worse in men than in women regardless of antipsychotics studied [13].
Treatment-emergent sexual dysfunction is a frequent adverse effect of many psychotropic drugs that may affect the patient’s quality of life and may compromise treatment compliance. It is therefore important to prescribe psychotropic drugs with least adverse impact on sexual function. In this outpatient prescription-based study, we have analyzed the prescribing trends and the likelihood of psychotropic-associated sexual dysfunctions in patients with depression or other psychiatric disorders.
2. Materials and Methods
2.1. Setting
The Kingdom of Bahrain, population 1,100,000, is a group of small islands located in the Arabian Gulf. A Directorate of Health Centres, has a network of 21 primary-care health centres which provide free curative and preventive care services to both citizens and expatriates, including dispensing of essential drugs. Any patient requiring special investigations or specialist consultation or admission is referred to Salmaniya Medical Complex, a secondary-tertiary care facility. There is a Psychiatric Hospital, five Maternity Hospitals, and one Geriatric Hospital under the Ministry of Health. There are several private hospitals as well.
This prescription-based study was carried out at the psychiatric hospital, the only psychiatric facility that offers comprehensive services in Bahrain. This public hospital with 201 beds also provides the exclusive facility for substance abuse rehabilitation.
2.2. Data Source and Collection
All prescriptions issued by psychiatrists and dispensed for outpatients during September 2007 were collected. In order to ensure that dose-titration has been achieved and prescription duplication is avoided, prescriptions with a refill period of minimum six weeks were included.
2.3. Drugs
Antidepressants included on the psychiatric hospital essential drug list at the time of data collection were: TCAs (amitriptyline, clomipramine, doxepin, imipramine, maprotiline and trimipramine); SSRIs (escitalopram, fluoxetine, fluvoxamine, paroxetine); SNRI (venlafaxine), atypical antidepressants (mirtazapine, tianeptine); and monoamine oxidase inhibitor [MAOI] (tranylcypromine). Antipsychotics listed were typical antipsychotics with high potency (haloperidol, trifluoperazine), moderate potency (zuclopenthixol), and low potency (chlorpromazine, thioridazine and sulpiride). Atypical antipsychotics included clozapine, olanzapine and risperidone.
2.4. Operational Definitions
Antidepressant associated sexual dysfunction was graded based on evidence-based criteria [2] as negligible (0), moderate (2+), moderately severe (3+) and uncertain (U) adverse effect. Grade (0) category includes mirtazapine; grade (2+) include amitriptyline, doxepin, imipramine and maprotiline; grade (3+) include clomipramine, escitalopram, fluoxetine, fluvoxamine, paroxetine and venlafaxine; and uncertain grade (U) that includes tianeptine. In this study, we used the degree of antipsychotic-induced hyperprolactinaemia as an indirect indicator for sexual function impairment severity [6,14,15]. According to evidence-based criteria [16] antipsychotics effect on prolactin level was categorized as follows: no effect (0) for clozapine, very low (1+) for olanzapine, a dose-dependent no effect-to-moderately severe effect (0 to 3+) for risperidone, moderate (2+) for high potency (haloperidol, trifluoperazine), moderate potency (zuclopenthixol), and low potency (chlorpromazine, thioridazine) antipsychotics, and uncertain grade (insufficient data) for sulpiride.
2.5. Statistical Analysis
Data were analyzed using statistical package for the social sciences (SPSS/PC+, version 15). Chi-square (c2) and Fisher’s exact tests, if appropriate, were used to test differences between proportions and two-tailed t-test was used for continuous variables. A p-value of <0.05 was considered statistically significant.
3. Results
Patient characteristics and pattern of antidepressant therapy prescribed are shown (Table 1). Among 1089 prescriptions included in this study, 679 (62.4%) were for male and 410 (37.6%) were for female patients. The proportion of antidepressant as monotherapy, two-drug combinations, and augmented with antipsychotics were
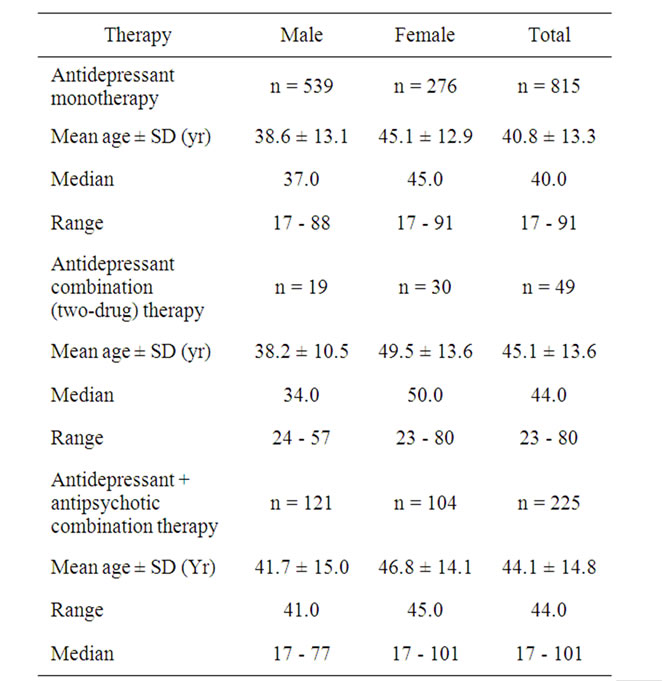
Table 1. Patient characteristics and drug therapy used.
74.8%, 4.5% and 20.7%, respectively. The mean age of patients treated with various antidepressant therapies are shown (Table 1).
As antidepressant monotherapy, there was a significant trend in prescribing SSRIs and SNRI to females more than to males (77.6% vs 30.6%, p < 0.0001) and tricyclics to males more than females (59.2% vs 14.8%; p < 0.0001) (Table 2). Despite a propensity to cause significantly less sexual dysfunction, mitrazapine was less often prescribed (males 8.3% and females 6.5%).
Prescribing mitrazapine with SSRIs or SNRI was the most common two-antidepressant drug combinations in male and female patients (47.5 vs 56.6%, p = 0.568, Table 2), followed by tricyclics along with TCAs or with SSRIs, and with SNRI (42.2% for males and 26.6% for females; p = 0.351, Table 2).
Patterns of antidepressants augmentation strategy with antipsychotics are presented (Table 3). Antidepressants were augmented with atypical and typical antipsychotics at a rate of 59.1% and 40.9%, respectively. Risperidone was the most popular antipsychotic used to augment antidepressant response, that accounted for 72.9% of all atypical antipsychotics and 43.1% of overall antipsychotics prescribed. Atypical antipsychotics such as clozapine and olanzapine were less often prescribed to augment antidepressant therapy (13.3% for males vs. 19.3% for females; p = 0.274).
4. Discussion
The trend to prescribe SSRIs or SNRIs as monotherapy in females (which are known to produce a moderately severe sexual dysfunction) in contrast to TCA monotherapy in males (which are known to produce moderate sexual dysfunction) was apparent (p < 0.0001, Table 2). Perhaps, this trend may be due to the perception of the prescriber that the risk for sexual dysfunction is significantly less for women than men. A further data analysis (data not shown) demonstrated that prescribing TCA monotherapy, notably amitriptyline and doxepin, accounted for 59.0% of overall prescribed TCAs. These TCAs were prescribed to male patients who were prison inmates or for those in police custody who required psychiatric intervention (26.9%), and to outpatients at Drug and Alcohol Rehabilitation unit (73.1%). It is likely that overt prescription of TCAs to male patients may be related to doctors prescribing behavior, patient characteristics and cost considerations. The therapeutic reasoning for prescribing amitriptyline and doxepin to inmates may be to relieve agitation and anxiety because these drugs have an additional sedative property.
This study also revealed that mirtazapine and tianeptine, as monotherapy, were less often prescribed to both males and females. Mirtazapine, produces benign
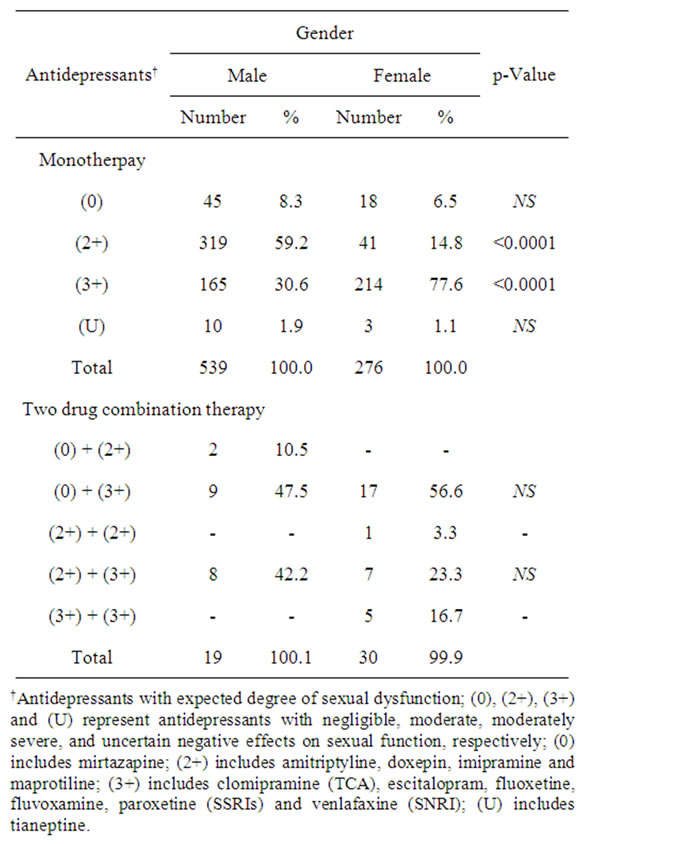
Table 2. Gender-based prescribing pattern of antidepressants and degree of sexual dysfunction expected: a comparison of monotherapy versus two drug combination therapy.
sexual dysfunction as a side effect [12,17,18], has the potential to reverse SSRI-induced sexual dysfunctions [17,19-23] without compromising therapeutic response to other antidepressants [22] and can improve baseline performance in certain subjects [19,20]. Tianeptine is at least as effective as SSRIs, with further advantage of better patient acceptability [24]. Treatment with tianeptine was reported to be associated with a lower incidence of sexual dysfunction than with TCAs or with SSRIs [25,26], and is effective in men with depression and erectile dysfunction [27]. As antidepressant monotherapy, mirtazapine and tianeptine were rarely prescribed despite the tendency to cause significantly less sexual dysfunction than other antidepressants. However, mirtazapine can produce significant weight gain as an adverse effect.
Combination therapy with different classes of antidepressants has become a preferred approach [28], used successfully in the treatment of refractory depression [29]. However, such strategy may result in more adverse reactions due to drug interactions [29,30]. It may also
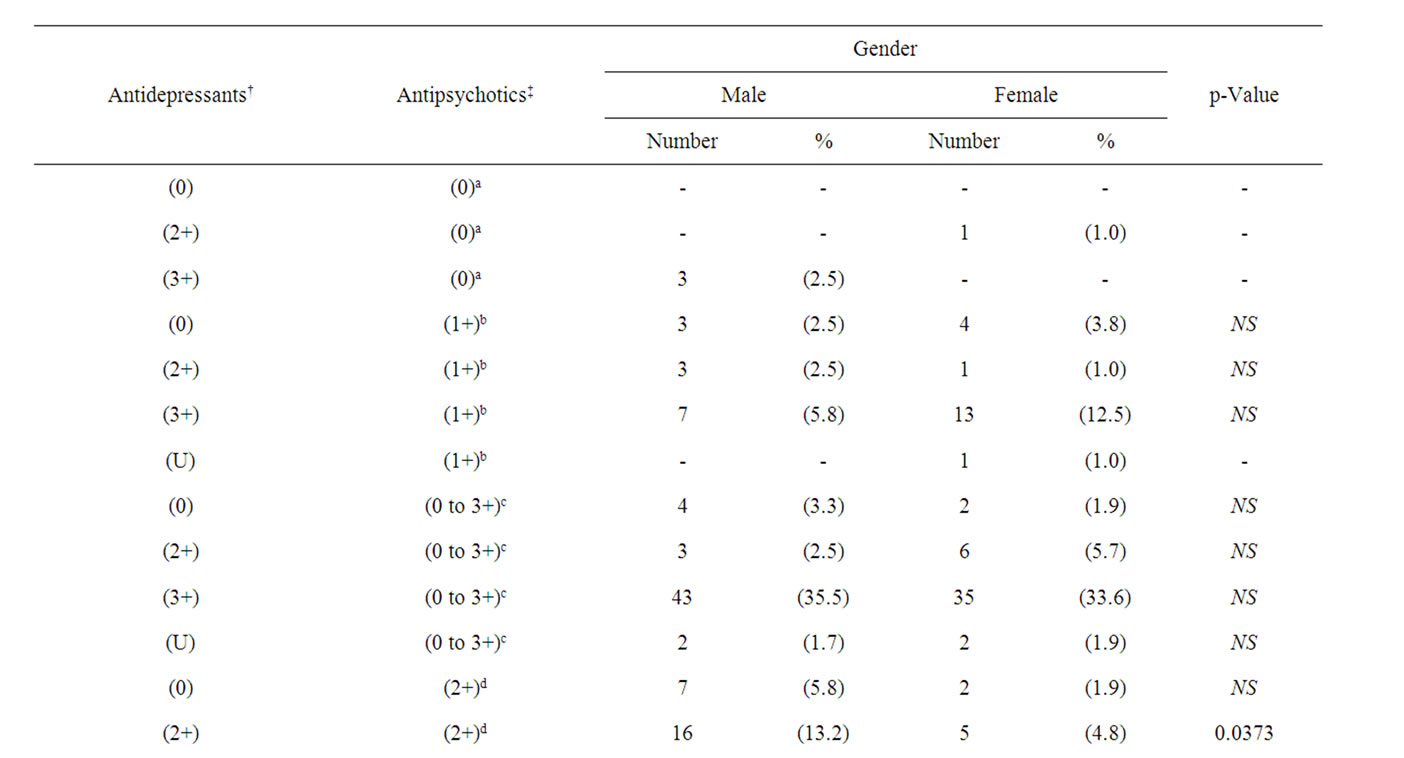
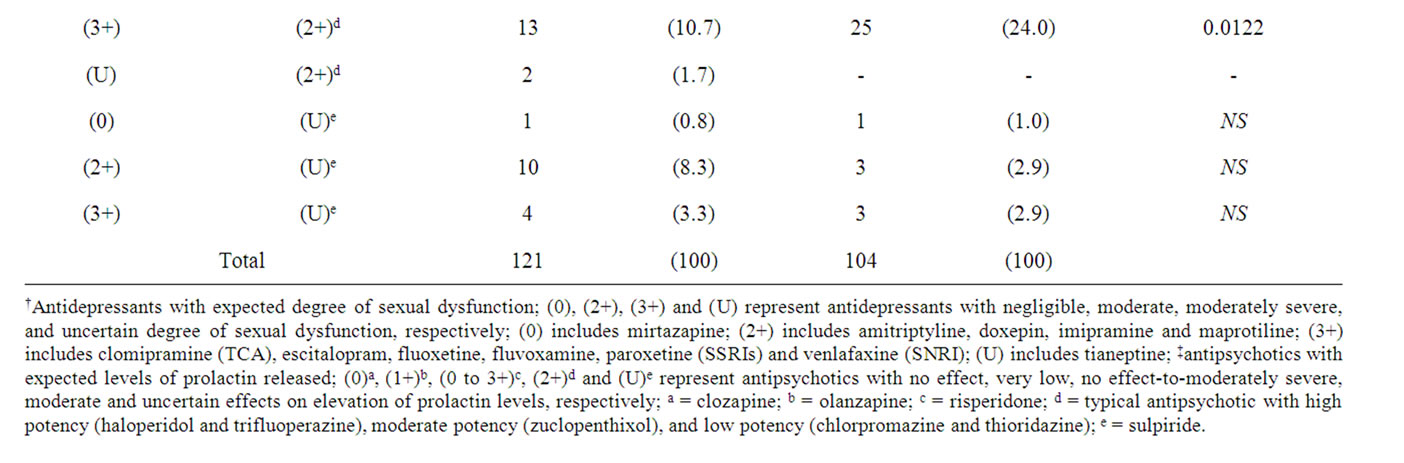
Table 3. Pattern of antidepressant augmentation strategies with antipsychotic and their potential for sexual dysfunction according to gender.
escalate the cost of therapy and result in unclear dosing strategies [31]. A combination of mirtazapine with various SSRIs or SNRI (venlafaxine) was the most often prescribed antidepressant two-drug therapy (Table 2). The lack of statistical difference between genders may be attributed to the small sample size of two antidepressant drug combinations in this study.
Mirtazapine as an add-on therapy to augment SSRIs or SNRI has gained popularity [28] since it seems to improve core depressive symptoms, reduce anxiety and ameliorate sleep disorders [32]. There is evidence that combination of antidepressants such as SSRIs or SNRI with mirtazapine that possess a negligible to low level of adverse effect on sexual function, may alleviate, and perhaps reverse SSRIand SNRI-induced sexual dysfunction [17,19-23]. Combinations such as TCA with another TCA or with SSRI or SNRI, and SNRI with SSRI accounted for 42.9% of overall two-drug antidepressant therapy (Table 2). Co-prescription of antidepressants having a moderate adverse effect on sexual function (TCA) with others having moderate to severe impact (SSRIs and SNRI) should be weighed carefully since such a therapeutic strategy can aggravate sexual problems.
The rationale for antidepressant augmentation strategy is to accelerate antidepressant response, to treat refractory depression, to increase the remission rate, and to avoid adverse effects of index antidepressant [28]. Available data suggest that atypical antipsychotics may be useful for augmentation particularly in non-psychotic major depressive disorders and treatment-resistant depression [33]. However, antipsychotic associated sexual dysfunction and the potential negative impact on quality of life and patient compliance to drug therapy need to be weighed [34,35]. In this study, antidepressant therapy was augmented with atypical and typical antipsychotics at a rate of 59.1% and 40.9%, respectively. Risperidone comprised 43.1% of all antipsychotics prescribed to both male and female patients (Table 3). Based on our data, it is apparent that antidepressant augmentation strategy with an antipsychotic needs further evaluation: 1) a lack of gender-based difference with respect to prescribing risperidone as an augmenting agent (43.0% for male vs 43.1% for female; p = 1.000, Table 3) which causes greater elevation in prolactin level than with typical antipsychotics per se [7,36]; 2) infrequent prescribing of clozapine and olanzapine which rarely elevate prolactin levels or produce sexual dysfunction [7,15,37,38]. The reluctance to prescribe clozapine can be due to the need for haematological monitoring of patients [39]. Additionally, only consultants in public psychiatric hospital in Bahrain were authorized to prescribe clozapine at the time of data collection for this study. However, less frequent use of olanzapine appears to be associated with its metabolic adverse effects and weight gain [38,40], although olanzapine has been reported to be somewhat more efficacious than other atypical antipsychotics [40]; 3) risperidone which produces at least as much sexual dysfunction as typical antipsychotics [15] was extensively prescribed to augment SSRIs, SNRI and TCA (clomipramine), known to have moderately severe sexual dysfunction potential (Table 3); and 4) the mean daily dose in mg ± SD of risperidone (3.4 ± 2.0 for males vs 2.6 ± 1.3 for females; p = 0.0109; data not shown) was significantly larger than the recommended dose (0.5 mg - 2.0 mg/day) [41,42], despite the fact that hyperprolactinemia induced by risperidone is dose-dependent [16].
It should be emphasized that choice of any drug is usually made based primarily on expected effect of the drug as well as its side effects. This is because symptoms of psychotropic-associated sexual dysfunction, for instance, may affect the patient’s quality of life and may compromise compliance with treatment as well. We therefore suggest, in addition to mirtazapine and tianeptine, newer antidepressants and antipsychotics with proven efficacy, safety and with negligible adverse effect on sexual function should be added to the essential drugs list to expand the therapeutic options for improving core depressive symptoms, without concerns about compromising the quality of life as a result of sexual dysfunction.
Different strategies have been proposed for the treatment of psychotropic-induced sexual dysfunction. For example, alternative psychotropic without significant sexual adverse effects, can be substituted. Other approaches involve drug holidays or adjunctive therapy with phosphodiesterase-5 inhibitors [17]. Recent reports have confirmed that sildenafil is effective in the management of antipsychotic-induced sexual dysfunction in men [35,43], and in women [44]. Perhaps the effectiveness of sildenafil in managing antidepressant (SSRI)— induced sexual dysfunction, either in male or in female, is less convincing [45-47]. The lack of robust, placebo controlled studies limit our ability to draw firm conclusion on the efficacy of such intervention. Moreover, it is unclear as to the adverse effects of antidepressant augmentation with antipsychotic on sexual functions, and whether sildenafil is beneficial in ameliorating such adverse effects. Adjunctive therapy with atypical antipsychotic, such as aripiprazole, did not adversely affect sexual functioning [48]. There is considerable evidence that bupropion can be usefully combined with SSRIs to ameliorate SSRI-induced sexual dysfunction [49]. Further studies on the effects of antidepressants and antipsychotic drugs on sexual function are needed.
4.1. Conclusion
The prescribing of psychotropics by psychiatrists in Bahrain needs further attention to optimize achieving the therapeutic goal with minimal adverse impact on sexual function.
4.2. Limitations of the Study
Since the psychiatric diagnosis is not stated in prescriptions, the therapeutic rationale for psychotropic drugs prescribed is uncertain. Moreover, factors that determine the antidepressant selection such as history of previous treatment response, drug safety in overdose, overall adverse effect profiles, comorbid conditions and non-psychotropic medications used, and patient preference if any, are unknown. Therefore the observations of this study need to be interpreted with caution.
4.3. Strength of the Study
The prescription audit approach provides an unbiased insight about the prescribers’ actual practicing behavior with respect to iatrogenic sexual dysfunction due to psychotropic medications in psychiatric practice.
5. Conflict of Interest
There is no conflicts of interest to declare. This work is not supported or funded by any drug company.
REFERENCES
- S. H. Kennedy and R. Sakina, “Sexual Dysfunction, Depression and the Impact of Antidepressants,” Journal of Clinical Psychopharmacology, Vol. 29, No. 2, 2009, pp. 157-164. doi:10.1097/JCP.0b013e31819c76e9
- R. J. Baldessarini, “Drug Therapy of Depression and Anxiety Disorders,” In: L. L. Brunton, J. S. Lazo and K. L. Parker, Eds., Goodman and Gilman’s the Pharmacological Basis of Therapeutics, McGraw-Hill, New York, 2006, pp. 429-459.
- S. MacDonald, J. Halliday, T. MacEwan, V. Sharkey, S. Farrington, S. Wall and R. G. McCreadie, “Nithsdale Schizophrenia Surveys 24: Sexual Dysfunction. CaseControl Study,” British Journal of Psychiatry, Vol. 182, No. 1, 2003, pp. 50-56. doi:10.1192/bjp.182.1.50
- E. O. Laumann, A. Paik and R. C. Rosen, “Sexual Dysfunction in the United States: Prevalence and Predictors,” Journal of American Medical Association, Vol. 281, 1999, pp. 537-544. doi:10.1001/jama.281.6.537
- A. Ucok, C. Incesu, T. Aker and S. Erkoc, “Sexual Dysfunction in Patients with Schizophrenia on Antipsychotic Medication,” European Psychiatry, Vol. 22, No. 5, 2007, pp. 328-333. doi:10.1016/j.eurpsy.2007.01.001
- H. Liu-Seifert, B. J. Kinon, C. J. Tennant, J. Sniadecki and J. Volavka, “Sexual Dysfunction in Patients with Schizophrenia Treated with Conventional Antipsychotics or Risperidone,” Journal of Neuropsychiatric Disease and Treatment, Vol. 5, 2009, pp. 47-54. doi:10.1016/j.eurpsy.2007.01.001
- B. J. Kinon, J. A. Gilmore, H. Liu-Seifert and U. M. Halbreich, “Prevalence of Hyper-Prolactinemia in Schizophrenic Patients Treated with Conventional Antipsychotic Medications or Risperidone,” Psychoneuroendocrinology, Vol. 28, Suppl. 2, 2003, pp. 55-68. doi:10.1016/S0306-4530(02)00127-0
- M. Hummer and J. Hubber, “Hyperprolactinemia and Antipsychotic Therapy in Schizophrenia,” Current Medical Research and Opinion, Vol. 20, 2004, pp. 189-197. doi:10.1185/030079903125002865
- M. J. Gitlin, “Psychotropic Medications and Their Effects on Sexual Dysfunction: Diagnosis, Biology, and Treatment Approaches,” Journal of Clinical Psychiatry, Vol. 55, 1994, pp. 406-413.
- M. H. Pollack, S. Reiter and P. Hammerness, “Genitourinary and Sexual Adverse Effects of Psychotropic Medication,” International Journal of Psychiatry in Medicine, Vol. 22, No. 4, 1992, pp. 305-327.
- R. C. Rosen and H. Marin, “Prevalence of Antidepressant-Associated Erectile Dysfunction,” Journal of Clinical Psychiatry, Vol. 64, Suppl. 10, 2003, pp. 5-10.
- A. L. Montejo, G. Llorca, J. A. Izquierdo and F. RicoVillademoros, “Incidence of Sexual Dysfunction Associated with Antidepressant Agents: A Prospective Multicentre Study of 1022 Outpatients,” Journal of Clinical Psychiatry, Vol. 62, Suppl. 3, 2001, pp. 10-21.
- A. L. Montejo, S. Majadas, F. Rico-Villademoros, G. Llorca, J. de la Gandara, M. Franco, M. Martin-Carrasco, L. Aquera, N. Prieto and Spanish Working Group for the Study of Psychotropic-Related Sexual Dysfunction, “Frequency of Sexual Dysfunction in Patients with a Psychotic Disorder Receiving Antipsychotics,” Journal of Sexual Medicine, Vol. 7, No. 10, 2010, pp. 3404-3413. doi:10.1111/j.1743-6109.2010.01709.x
- J. Buvat, “Hyperprolactinemia and Sexual Function in Men: A Short Review,” International Journal of Impotence Research, Vol. 15, No. 5, 2003, pp. 373-377. doi:10.1038/sj.ijir.3901043
- M. L. Crismon, T. Argo, and P. F. Buckley, “Schizophrenia,” In: J. T. Dipiro, R. L. Talbert, G. C. Yee, G. R. Matzke, B. G. Wells and L. M. Posey, Eds., Pharmacotherapy: A Pathophysiologic Approach, McGraw-Hill Companies Inc., Beijing, 2008, pp. 1099-1122.
- R. A. Endow-Eyer, M. M. Mitchell and J. P. Lacro, “Schizophrenia,” In: M. A. Koda-Kimble, L. Y. Young, B. K. Aldredge, R. L. Corelli, B. J. Guglielmo, W. A. Kradjan and B. R. Williams, Eds., Applied Therapeutics—The Clinical Use of Drugs, Lippincott Williams and Wilkins, Philadelphia, 2009, pp. 78.1-78.34.
- G. L. Stimmel and M. A. Gutierrez, “Sexual Dysfunction and Psychotropic Medications,” CNS Spectrums, Vol. 11, 2006, pp. 24-30.
- K. U. Lee, Y. M. Lee, J. M. Nam, H. K. Lee, H. K. Kweon, C. T. Lee and T. Y. Jan, “Antidepressant-Induced Sexual Dysfunction among Newer Antidepressants in a Naturalistic Setting,” Psychiatry Investigations, Vol. 7, 2010, pp. 55-59. doi:10.4306/pi.2010.7.1.55
- A. J. Gelenberg, C. McGahuey, C. Laukes, G. Okayli, F. Moreno, L. Zentner and P. Delgado, “Mirtazapine Substitution in SSRI-Induced Sexual Dysfunction,” Journal of Clinical Psychiatry, Vol. 61, No. 5, 2000, pp. 356-360. doi:10.4088/JCP.v61n0506
- R. S. Gregorian, K. A. Golden, A. Bahce, C. Goodman, W. J. Kwong and Z. M. Khan, “Antidepressant-Induced Sexual Dysfunction,” Annals of Pharmacotherapy, Vol. 36, No. 10, 2002, pp. 1577-1589. doi:10.1345/aph.1A195
- A. H. Clayton and A. L. Montejo, “Major Depressive Disorder, Antidepressants, and Sexual Dysfunction,” Journal of Clinical Psychiatry, Vol. 67, Suppl. 60, 2006, pp. 33-37.
- B. K. Yang and C. F. Donatucci, “Drugs That Effect Male Sexual Dysfunction,” In: J. J. Mulcahy, Ed., Male Sexual Dysfunction: A Guide to Clinical Management, Humana Press Inc., Totowa, 2006, p. 170.
- N. K. Ozmenler, T. Karlidere, A. Bozkurt, S. Yetkins, A. Doruk, L. Sutcigil, A. Cansever, O. Uzun, F. Ozgen and A. Ozsahin, “Mirtazapine Augmentation in Depressed Patients with Sexual Dysfunction Due to Selective Serotonin Reuptake Inhibitors,” Human Psychopharmacology, Vol. 23, No. 4, 2008, pp. 321-326. doi:10.1002/hup.929
- S. Kasper and J. P. Olie, “A Meta-Analysis of Randomized Controlled Trials of Tianeptine versus SSRI in the Short-Term Treatment of Depression,” European Journal of Psychiatry, Vol. 17, 2002, pp.331-340. doi:10.1016/S0924-9338(02)00651-X
- M. Bonierbale, C. Lancon and J. Tignol, “The ELIXIR Study: Evaluation of Sexual Dysfunction in 4557 Depressed Patients in France,” Current Medical Research and Opinion, Vol. 19, No. 2, 2003, pp. 114-124.
- M. Atmaca, M. Kuloglu, E. Tezcan and A. Buyukbayram, “Switching to Tianeptine in Patients with Antidepressant-Induced Sexual Dysfunction,” Human Psychopharmacology, Vol. 18, 2003, pp. 277-280. doi:10.1002/hup.479
- H. El-Shafey, A. Atteya, S. Abu-el-Magd, A. Hassanein, A. Fathy and R. Shamloul, “Tianeptine Can Be Effective in Men with Depression and Erectile Dysfunction,” Journal of Sexual Medicine, Vol. 3, No. 5, 2006, pp. 910- 917. doi:10.1111/j.1743-6109.2005.00141.x
- R. S. McIntyre, A. Muller, D. A. Mancini and E. S. Silver, “What to Do if an Initial Antidepressant Fails,” Canadian Family Physician, Vol. 49, No. 4, 2003, pp. 449-457.
- I. Schweitzer and V. Tuckwell, “Risk of Adverse Events with the Use of Augmentation Therapy for the Treatment of Resistant Depression,” Drug Safety, Vol. 19, No. 6, 1998, pp. 455-464. doi:10.2165/00002018-199819060-00003
- Martindale, “The Complete Drug Reference,” In: S. C. Sweetman, Ed., Pharmaceutical Press, London, 2007, pp. 333-336.
- D. O. Antonuccio, D. Burns and W. G. Danton, “Antidepressant: A Triumph of Marketing over Science?” Prevention and Treatment, 2002. http://www.Antidepressantsfacts.com/2002-07-15-Antonucciotherapy-vs-med.htm/
- L. L. Carpenter, Z. Jocic, J. M. Hall, S. A. Rasmussen and L. H. Price, “Mirtazapine Augmentation in the Treatment of Refractory Depression,” Journal of Clinical Psychiatry, Vol. 60, No. 1, 1999, pp. 45-49. doi:10.4088/JCP.v60n0110
- N. S. Philip, L. L. Carpenter, A. R. Tyrka and L. H. Price, “Augmentation of Antidepressants with Atypical Antipsychotics: A Review of the Current Literature,” Journal of Psychiatric Practice, Vol. 14, No. 1, 2008, pp. 34-44. doi:10.1097/01.pra.0000308493.93003.92
- S. Smith and A. Gillam, “Sexual Dysfunction—The Forgotten Taboo,” Mental Health Nursing, Vol. 25, No. 1, 2005, pp. 6-9.
- R. Gopalakrishnan, K. S. Jacob and A. Kuruvilla, “Sildenafil in the Treatment of Antipsychotic-Induced Erectile Dysfunctions: A Randomized, Double-Blind, Placebo-Controlled, Flexible Dose, Two-Way Crossover Trial,” American Journal of Psychiatry, Vol. 163, No. 3, 2006, pp. 494-499. doi:10.1176/appi.ajp.163.3.494
- J. Volavka, P. Czobor, T. B. Cooper, B. Sheitman, J. P. Lindenmayer, L. Citrome, J. P. McEvoy and J. A. Lieberman, “Prolactin Levels in Schizophrenia and Schizoaffective Disorders Patients Treated with Clozapine, Olanzapine, Risperidone, or Haloperidol,” Journal of Clinical Psychiatry, Vol. 65, No. 1, 2004, pp. 57-61. doi:10.4088/JCP.v65n0109
- D. M. Gardner, R. J. Baldessarini and P. Waraich, “Modern Antipsychotic Drugs: A Critical Overview,” Canadian Medical Association Journal, Vol. 172, No. 13, 2005, pp. 1703-1711. doi:10.1503/cmaj.1041064
- D. Novivk, J. M. Haro, E. Perrin, D. Suarez and J. M. Texeria, “Tolerability of Outpatient Antipsychotic Treatment: 36-Month Results from the European Schizophrenia Outpatient Health Outcomes (SOHO) Study,” European Neuropsychopharmacology, Vol. 19, No. 7, 2009, pp. 542-550. doi:10.1016/j.euroneuro.2009.03.003
- S. Miyamoto, G. E. Duncan, C. E. Marx and J. A. Lieberman, “Treatment for Schizophrenia: A Critical Review of Pharmacology and Mechanisms of Action of Antipsychotic Drugs,” Molecular Psychiatry, Vol. 10, 2005, pp. 79-104. doi:10.1038/sj.mp.4001556
- K. Komossa, C. Rummel-Kluge, H. Hunger, F. Schmid, S. Schwarz, L. Duggan, W. Kissling and S. Leucht, “Olanzapine versus Other Atypical Antipsychotics for Schizophrenia,” Cochrane Database System Review, Vol. 17, No. 3, 2010, Article ID: CD006654
- K. Tani, N. Takei, M. Kawai, K. Suzuki, Y. Sekine, T. Toyoda, Y. Minabe and N. Mori, “Augmentation of Milnacipran by Risperidone in Treatment for Major Depression,” International Journal of Neuropsychopharmacology, Vol. 7, No. 1, 2004, pp. 55-58. doi:10.1017/S146114570300381X
- R. A. Mahmoud, G. I. Pandina, I. Turkoz, C. Kosik-Gonzalez, C. M. Canuso, M. J. Kujawa and G. M. GharabawiGaribaldi, “Risperidone for Treatment—Refractory Major Depressive Disorder. A Randomized Trial,” Annals of Internal Medicine, Vol. 147, No. 9, 2007, pp. 593-602.
- M. M. Berner, M. Hagen and L. Kriston, “Management of Sexual Dysfunction Due to Antipsychotic Drug Therapy,” Cochrane Databse Systemic Reviews, Vol. 24, 2007, Article ID: CD003546.
- L. A. Labbate, “Psychotropics and Sexual Dysfunction: The Evidence and Treatments,” Advances in Psychosomatic Medicine, Vol. 29, 2008, pp. 107-130. doi:10.1159/000126627
- A. J. Salerian, W. E. Deibler, B. J. Vittone, S. P. Geyer, L. Drell, N. Mirmirani, J. A. Mirczak, W. Byrd, S. B. Tunick, M. Wax and S. Fleisher, “Sildenafil for Psychotropic-Induced Sexual Dysfunction in 31 Women and 61 Men,” Journal of Sexual and Marital Therapy, Vol. 26, No. 2, 2000, pp. 133-140. doi:10.1080/009262300278533
- H. G. Nurenberg, P. L. Hensley, A. J. Gelenberg, M. Fava, J. Lauriello and S. Paine, “Treatment of Antidepressant-Associated Sexual Dysfunction with Sildenafil: A Randomized Controlled Trial,” Journal of American Medical Association, Vol. 289, No. 1, 2003, pp. 56-64. doi:10.1001/jama.289.1.56
- H. G. Nurenberg, P. L. Hensley, J. R. Heiman, H. A. Croft, C. Debattista and S. Paine, “Sildenafil Treatment of Women with Antidepressant-Associated Controlled Trial,” Journal of American Medical Association, Vol. 300, No. 4, 2008, pp. 395-404. doi:10.1001/jama.300.4.395
- R. N. Marcus, R. D. McQuade, W. H. Carson, D. Hennicken, M. Fava, J. S. Simon, M. H. Trivedi, M. E. Thase and R. M. Berman, “The Efficacy and Safety of Aripiprazole as Adjunctive Therapy in Major Depressive Disorder: A Second, Multicenter, Randomized, DoubleBlind Placebo—Controlled Study,” Journal of Clinical Psychopharmacology, Vol. 28, No. 2, 2008, pp. 156-165. doi:10.1097/JCP.0b013e31816774f9
- D. Baldwin and A. Mayers, “Sexual Side-Effects of Antidepressant and Antipsychotic Drugs,” Advances in Psychiatric Treatment, Vol. 9, No. 3, 2003, pp. 202-210. doi:10.1192/apt.9.3.202
NOTES
*Corresponding author.

