Open Journal of Gastroenterology
Vol.3 No.2(2013), Article ID:32177,6 pages DOI:10.4236/ojgas.2013.32019
Virological profile of hepatitis B infection in Black African HBsAg chronic carriers
![]()
1Service de Médecine et d’Hépato-Gastroentérologie, CHU Yopougon, Abidjan, Côte d’Ivoire
2Clinique Médicale Danga, Cocody, Abidjan, Côte d’Ivoire
Email: *attia_alain@yahoo.fr
Copyright © 2013 Koffi Alain Attia et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 4 February 2013; revised 26 March 2013; accepted 2 May 2013
Keywords: Hepatitis B Virus; Virological Profile; Cirrhosis
ABSTRACT
Aims: 1) Describe virological profile of patients followed-up for chronic Hepatitis B virus (HBV); 2) Search for a correlation between cirrhosis and virological profile of patients. Patients and Methods: Retrospective study about 75 HBsAg positive patients followedup for at least one year in two medical structures of Abidjan. Studied parameters: clinical signs, biological check-up (serum transaminases every 3 months for at least one year, platelets count and prothrombin rate), abdominal echography, virological check-up (HBsAg, HBeAg, anti-HBe, total anti-HBc, anti-VHC and antiHIV Ab, HBV DNA biannual quantification during at least one year). Histological or biochemical evaluation of hepatic activity and fibrosis were realized in case of transaminases elevation or HBV DNA > 2000 IU/ml. Results: The mean age of our 75 patients (54 men) was 42.1 ± 11.54 years. HBV was fortuitously discovered in most of our patients (74.7% of the cases). The HBV inactive chronic carriage was 50.7%; HBeAgpositive and HBeAg-negative chronic hepatitis represented respectively 9.3% and 40% of the cases. Mean B viral load was 327.5 IU/ml in HBV inactive chronic carriers, 44,047,663 IU/ml in HBeAg-positive chronic HBV and 20,231,822 IU/ml in HBeAg-negative chronic HBV. Cirrhosis prevalence was significantly higher in positive or negative HBeAg chronic HBV than in HBV inactive chronic carriers (32.4% vs. 5.3%, p = 0.008; OR = 8.6). Conclusion: Our patients’ virological profile was dominated by HBeAg-negative chronic HBV and HBV inactive chronic carriage. The risk of having cirrhosis was multiplied by 8.6 in case of active chronic hepatitis compared with HBV inactive chronic carriage.
1. INTRODUCTION
Hepatitis B Virus (HBV) infection is a real-world problem of public health and more particularly in high-prevalence areas such as sub-Saharan Africa [1-4] owing to its evolutionary complications (cirrhosis and hepatocellular carcinoma) and management difficulties in the particular context of our country with limited financial resources. Though there are numerous works on HBV infection prevalence in sub-Saharan Africa, we get fewer data on the virological profile of HBsAg-positive patients with an informed consent longitudinal follow-up. The present study aimed at describing the HBV virological profile in 75 HBsAg positive patients followed-up in two medical structures of Abidjan, Côte d’Ivoirefor at least one year and searching for a correlation between the existence of cirrhosis and patients’ virological profile.
2. PATIENTS AND METHODS
It is about a transversal retrospective study (January 1st, 2002 through August 31st, 2011). All the records of chronic carrier patients with HBsAg and ambulatory follow-ups in two hospital structures of Abidjan (Teaching Hospital of Yopougon and Clinique Médicale Danga of Cocody) were analyzed. A systematic minimal biological check-up was realized for every patient included in the study; this check-up included HIV serology (Screening by DetermineÒ and confirmation by Genie IIÒ), transaminases quarterly determination for at least one year (CobasÒIntegra 400 plus; Roche diagnostics, Mannheim, Germany), a search for HBe antigen (Ag), anti-HBe, anti-HBc and anti-HCV antibodies (Ab), (Mini VidasÒ; Biomerieux, Marcy l’Etoile, France), biannual quantitative measure of the HBV DNA for at least one year by a real-time PCR (CobasÒ Amplicor HBV Monitor assay, threshold of detectability 35 copies/ml or 6 IU/ml; Roche Diagnostics). Besides this minimal check-up, the result of the hemogram (number of Platelets) and prothrombinrate were taken into account. A hepatic echography was realized in all patients included in the study. Percutaneous liver biopsy for a histological examination or determination of biochemical indirect markers of activity and fibrosis (ActitestÒ and FibrotestÒ or InflaMètreÒ and FibroMètreÒ) were made in the patients who had biochemical and virological signs of viral replication (elevated transaminases and HBV DNA > 2000 IU/ml). Liver activity grade and fibrosis stage were estimated through Metavir score [5]. We distinguished various HBV infection virological profiles inpatients according to the results of the biological check-up. HBeAg positive patients were considered as wild virus-infected (HBeAgpositive hepatitis), HBeAg negative patients with normal transaminases and viremialess than 2000 IU/ml after one-year follow-up was considered as HBV inactive carriers, HBeAg negative patients with elevated transaminases at least once and viremia higher than 2000 IU/ml after one-year follow-up was considered as mutant precore virus-infected (HBeAg-negative hepatitis). Cirrhotic patients had an upper digestive endoscopy in search for portal hypertension (PHT) signs. Esophageal varices grade was noted according to the classification of the French society of digestive endoscopy [6]. Cirrhotic patients also had a prothrombin rate determination to assess hepatic function, Alpha-foeto-protein (AFP) determination and hepatic echography as part of the screening for hepatocellular carcinoma (HCC) in cirrhosis.
We searched for the existence of a correlation between the presence of cirrhosis and virological profile of our patients in univariate analysis (comparison of percentages) through Fisher’s exact test. Alpha threshold was set at 5% for bilateral formulation
3. RESULTS
After analysis of 151 records of HBsAg-positive patients seen in consultation during the study period, 75 (49.7%) met inclusion criteria and were retained for the study. Out of 76 patients excluded from the study, 30 were excluded for incomplete information in records and 46 other patients had a drop of insufficient follow-up (less than one year). Median duration of follow-up was 3 years with brackets from 1 to 9 years and an interquartile interval from 2 to 5 years. Our patients’ mean age was 42.1 ± 11.54 years with brackets from 17 to 77 years. Motives for consultation were physical asthenia in 5 patients (6.7%), pseudo-flu-like syndrome in 6 patients (8%), fortuitous discovery on the occasion of blood donation or medical check-up in 55 patients (73.3%), screening in subjects contacts of a patient infected in 9 patients (12%). Clinical and biological characteristics of 75 patients are summarized in Table 1. In the inclusion, none of 75 patients had clinical signs of hepatocellular failure (HCF) or portal Hypertension (PHT). We noted a clinical hepatomegaly in a single patient (1.3%). At abdominal echography, the liver was normal in 60 patients (80%), cirrhotic in 9 patients (12%) and steatosic in 6 patients (8%). Fibrosis stage and activity grade were established according to Metavir score in 32 patients (42.7%) who had a transaminases rise and viremia higher than 2000
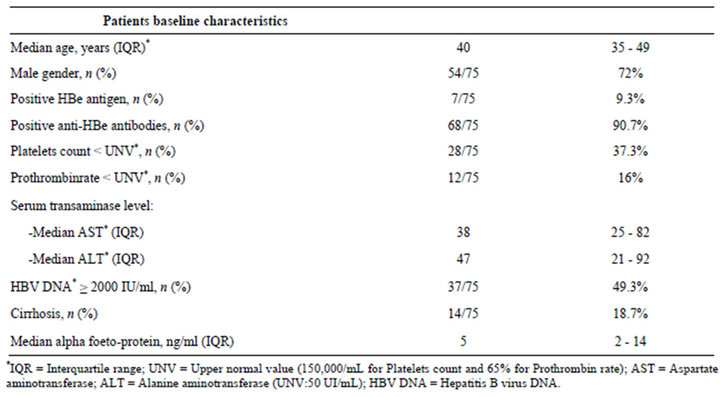
Table 1. Study population baseline characteristics (75 patients).
IU/ml. Hepatic lesions assessment was obtained in histological examination after percutaneous liver biopsy (PLB) in 17 of them and by biochemical indirect markersof fibrosis and activity (ActitestÒ and FibrotestÒ or InflaMètreÒ and FibroMètreÒ) in 15 others. Thus, 25 of 32 patients (78.1%) had clinically significant hepatic lesions (activity grade or fibrosis stage ³2) and cirrhosis was found in 10 patients out of 32 (31.3%). Upper digestive endoscopy realized in 14 patients (18.7%) highlighted PHT signs in 7 patients (50%) among whom 3 had grade 1 esophageal varices and 4 with grade 2 esophageal varices. Cirrhosis diagnosis was made in these 14 patients, either in the histology, or by biochemical indirect markers, or upon existence of a cirrhotic liver on abdominal echography with presence of PHT endoscopic signs. AFP mean level in these 14 patients was 7.6 ± 6.21 ng/ml with brackets from 1 to 21 ng/ml. We noted no new case of cirrhosis or hepatocellular carcinoma (HCC) during the follow-up of the patients included in the study. HIV serology was negative in all the 75 patients.
Table 2 represents various virological profiles of HBV infection in our patients and quantitative values of HBV DNA according to HBV infection type. HBV mean load was 327.45 ± 453.82 IU/ml in inactive chronic carriers of HBV, 44,047,663 ± 60,205,983 IU/ml in patients having HBeAg-positive chronic HBV and 20,231,822 ± 37,475,619 IU/ml in patients having HBeAg-negative chronic HBV. Transaminases were elevated in the 7 HBeAgpositive patients. Table 3 represents correlation between the existence of cirrhosis and virological profile of our patients.
4. DISCUSSION
Though HBV is a real-world problem of public health, there are big regional variations of this infection prevalence and virological profiles often differ according to geographical zones [3,4]. In our study about adults whose mean age was 42.1 ± 11.54 years, HBeAg-positive chronic hepatitis was found in less than 10% of the cases. No patient was at the immune tolerance stage. Most of our patients were HBV inactive chronic carriers (50.7%) or had HBeAg-negative chronic hepatitis (40%). These results confirm those of several studies carried out in sub-Saharan Africa (areas of high HBV endemicity); in those studies, prevalence of HBeAg-positive chronic hepatitis varied from 5% to 25% [7-14]. Besides in the Mediterranean Basin (mean HBV endemicity areas), HBeAg-negative chronic hepatitis (precore mutant) is also more frequent than HBeAg-positive chronic hepatitis (wild-type) [15-19]. On the contrary, in areas of high endemicity of South-East Asia, HBeAg-positive chronic hepatitis is much more frequent and represents 30% to 50% of the cases [4,20-23]. This difference of virological profile would partially explain the differences of HBV contamination modalities. Indeed, in HBV high endemicity countries of South-East Asia, owing to high prevalence of HBeAg-positive chronic hepatitis with generally a high-level HBV viremia, perinatal vertical transmission is the main contamination way. The risk of evolution towards chronicity is very high in infected newborns (about 90%); very contagious chronic forms at the stage of immune tolerance may last for two or three decades and are the sustainability origin of this vertical transmission from young women with sexual activity [4,24,25]. In HBV high endemicity countries of sub-Saharan Africa, owing to the lowest prevalence of wild-type chronic HBV, intra-family horizontal transmission in the early childhood seem to be the main mode of contamination [4,24, 25], such as HBV medium endemicity areas. The risk of evolution towards chronicity varies from 30% to 50% if contamination occurs before the age of 5 years and HBeAg clearance arises earlier, generally during life first decade [25,26]. However certain works suggest that in sub-Saharan Africa, vertical transmission is considerable
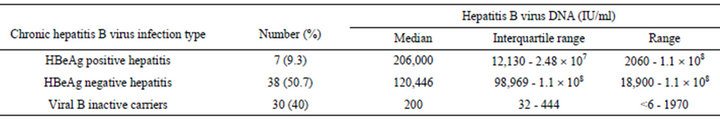
Table 2. Hepatitis B virus DNA quantitative values by hepatitis B virus infection type.
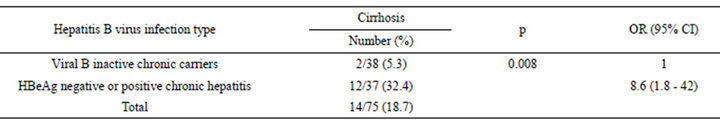
Table 3. Relationship between presence of cirrhosis and hepatitis B virus infection type.
[27-29]. In a study carried out in Côte d’Ivoire, motherto-child transmission rate at birth was 32.8% [27]; this rate was higher when the mother was HBeAg positive than when the mother was HBeAg negative (66.7% versus 26.9%; p = 0.03). In that study, the risk of motherto-child transmission was more than 20% in the absence of HBeAg, very likely owing to a high-level viremiain mothers (this parameter not having been taken into account in the study). Indeed, in a more recent Ghanaian study [28], mother-to-child transmission prevalence was 8.3%. Independently of the HBeAg status, the risk of mother-to-child transmission passed from 3.3% when HBV DNA of the mother was less than 10,000 IU/ml to 55% when HBV DNA was higher than 10,000 IU/ml (p = 0.0008). Viremia in patients of our study was often very high in case of active chronic hepatitis, with big variations yet; it was a mean of 44,047,663 IU/ml in case of HBeAg-positive chronic hepatitis (interquartile range = 98,969 - 1.1 ´ 108) and of 20,231,822 IU/ml in case of HBeAg-negative chronic hepatitis (interquartile range = 12,130 - 2.48 ´ 107). HBV DNA median value was 200,000 IU/ml in the patients who had HBeAg-negative chronic hepatitis. It is well demonstrated that the risk of vertical transmission is more correlated to HBV DNA load than to the HBeAg presence, even though HBV DNA is much more considerable in the presence of HBeAg [30-32]. Thus, independently of the HBeAg status, vertical transmission risk is very high when HBV viremia is ³200,000 IU/ml.
Most of our patients were asymptomatic; the diagnosis was made on the occasion of blood donationor medical check-up (73.3% of the cases) and on the occasion of screening in subjects contacts of infected patients (12% of the cases). Cirrhosis was present at the diagnosis time of chronic HBV infection in 18.7% of the patients. We noted an endoscopic portal hypertension in half of these cirrhotic patients but no case of hepatocellular carcinoma. Cirrhosis was found more frequently in the patients who had a chronic active hepatitis with HBeAg positive or with HBeAg negative than in the inactive chronic HBV carriers (32.4% versus 5.3% respectively, p = 0.008, OR = 8.6). Our results are in accordance with the literature data on the evolutionary risks of hepatic disease according to the evolutionary stage of HBV infection [3,4,33- 35]. Virological and morphological check-up is important for specifying the evolutionary stage of chronic HBV infection. This check-up has a double interest: a prognosis interest by identifying evolutionary complications and their management (cirrhosis, hepatocellular failure, portal hypertension and hepatocellular carcinoma); a therapeutic interest of the identifying patients for whom an antiviral treatment is indicated to durably surround the viral replication, prevent the appearance of cirrhosis or stabilize and improve hepatic lesions when the cirrhosis is already constituted. Recommendations elaboration by the American, Asia-Pacific and European consensus allowed to better codifying of the management of the subjects infected by HBV [36-38]. In patients at decompensate cirrhosis stage, prescription of nucleosidic or nucleotidic analogues to the viremic patients allows to improve hepatic functions and to propose hepatic transplantation in better conditions [36-38]. European consensus even recommends an antiviral treatment in case of cirrhosis compensated with viral replication for whatever viremia level [38]. In our area (sub-Saharan Africa) of high HBV endemicity, it is important to estimate through prospective cohort studies the risk of cirrhosis and hepatocellular carcinoma occurrence according to VHB DNA level and other factors such as viral genotype and quantitative determination of HBsAg. Such studies’ results should allow us to formulate recommendations adapted to our context, following the example of other consensus.
5. CONCLUSION
Most of our patients were often asymptomatic young adults. Their virological profile was dominated by HBeAgnegative chronic hepatitis and inactive chronic HBV carriage. A HBV antiviral treatment was indicated in approximately one patient out of two. The risk of having cirrhosis was multiplied by 8.6 in case of active chronic hepatitis compared with inactive chronic HBV carriage.
REFERENCES
- Wright, T.L. and Lau, J.Y.N. (1993) Clinical aspects of hepatitis B virus infection. Lancet, 342, 1340-1344. doi:10.1016/0140-6736(93)92250-W
- Murray, C.J. and Lopez, A.D. (1997) Mortality by cause for eight regions of the world: Global burden of disease study. Lancet, 349, 1269-1276. doi:10.1016/S0140-6736(96)07493-4
- Lai, C.L., Ratziu, V., Yeun, M.F. and Poynard, T. (2003) Viral hepatitis B. Lancet, 362, 2089-2094. doi:10.1016/S0140-6736(03)15108-2
- Goldstein, S.T., Zhou, F., Hadler, S.C., et al. (2005) A mathematical model to estimate global hepatitis B disease burden and vaccination impact. International Journal of Epidemiology, 34, 1329-1339. doi:10.1093/ije/dyi206
- Trabut, J.B. (2009) The METAVIR scoring system. Hepato-Gastro, 16, 219-220.
- Florent, C., Meary, N., Abdini, E. and Mostefa-Kara, N. (1995) The natural history of oesophageal varices. Acta Endoscopica, 25, 319-326. doi:10.1007/BF02963250
- Rapicetta, M., Stroffolini, T., Ngatchu, T., et al. (1991) Ageand sex related study of HBV-DNA in HBs Ag asymptomatic children from an endemic area (Cameroon). Annals of Tropical Paediatrics, 11, 325-329.
- Abiodun, P.O., Olomu, A., Okolo, S.N., et al. (1994) The prevalence of hepatitis Be antigen and anti-HBE in adults in Benin City. West African Journal of Medicine, 13, 171-174.
- Harry, T.O., Bajani, M.D. and Moses, A.E. (1994) Hepatitis B virus infection among blood donors and pregnant women in Maiduguri, Nigeria. East African Medical Journal, 71, 596-597.
- Pawlotsky, J.M., Belec, L., Gresenguet, G., et al. (1995) High prevalence of hepatitis B, C, and E markers in young sexually active adults from the Central African Republic. Journal of Medical Virology, 46, 269-272. doi:10.1002/jmv.1890460318
- Tswana, S., Chetsanga, C., Nystrom, L., et al. (1996) A sero-epidemiological cross-sectional study of hepatitis B virus in Zimbabwe. South African Medical Journal, 86, 72-75.
- Abebe, A., Nokes, D.J., Dejene, A., et al. (2003) Seroepidemiology of hepatitis B virus in Addis Ababa, Ethiopia: Transmission patterns and vaccine control. Epidemiology & Infection, 131, 757-770. doi:10.1017/S0950268803008574
- Otegbayo, J.A., Fasola, F.A. and Abja, A. (2003) Prevalence of hepatitis B surface and e antigens, risk factors for viral acquisition and serum transaminase among blood donors in Ibadan, Nigeria. Tropical Gastroenterology, 24, 196-197.
- Fujiwara, K., Tanaka, Y., Orito, E., et al. (2005) Distribution of HBV genotypes among HBV carriers in Benin: Phylogenetic analysis and virological characteristics of HBV genotype E. World Journal of Gastroenterology, 11, 6410-6415.
- Hadziyannis, S.J. and Vassilopoulos, D. (2001) Hepatitis B e antigen-negative chronic hepatitis B. Hepatology, 34, 617-624. doi:10.1053/jhep.2001.27834
- Funk, M.L., Rosenberg, D.M. and Lok, A.S. (2002) World-wide epidemiology of HBe Ag negative chronic hepatitis B and associated precore and core promoter variants. Journal of Viral Hepatitis, 9, 52-61. doi:10.1046/j.1365-2893.2002.00304.x
- Zarski, J.P., Marcellin, P., Leroy, V., et al. (2005) Quelles différences existe-t-il entre un porteur chronique inactif et un malade atteint d’hépatite virale chronique B antigène HBe négatif? Gastroentérologie Clinique et Biologique, 29, A177.
- Hadziyannis, S.J. and Papatheodoridis, G.V. (2006) Hepatitis B e antigen-negative chronic hepatitis B: Natural history and treatment. Seminars in Liver Disease, 26, 130-141. doi:10.1055/s-2006-939751
- Fattovich, G., Bortolotti, F. and Donato, F. (2008) Natural history of chronic hepatitis B: Special emphasis on disease progression and prognostic factors. Journal of Hepatology, 48, 335-352. doi:10.1016/j.jhep.2007.11.011
- Xu, Z.Y., Liu, C.B., Francis, D.P., et al. (1985) Prevention of perinatal acquisition of hepatitis B virus carriage using vaccine: Preliminary report of a randomized double-blind placebo-controlled and comparative trial. Pediatrics, 76, 713-718.
- Lo, K.J., Tsai, Y.T., Lee, S.D., et al. (1985) Combined passive and active immunization for interruption of perinatal transmission of hepatitis B virus in Taiwan. Hepatogastroenterology, 32, 65-68.
- Merican, I., Guan, R., Amarapuka, D., et al. (2000) Chronic hepatitis B virus infection in Asian countries. Journal of Gastroenterology and Hepatology, 15, 1356-1361. doi:10.1046/j.1440-1746.2000.0150121356.x
- Chen, H.L., Lin, L.H., Hu, F.C., et al. (2012) Effects of maternal screening and universal immunization to prevent mother-to-infant transmission of HBV. Gastroenterology, 142, 773-781. doi:10.1053/j.gastro.2011.12.035
- Hoffmann, C.J. and Thio, C.L. (2007) Clinical implications of HIV and hepatitis B co-infection in Asia and Africa. Lancet Infectious Diseases, 7, 402-409. doi:10.1016/S1473-3099(07)70135-4
- Hadziyannis, S.J. (2011) Natural history of chronic hepatitis B in Euro-Mediterranean and African Countries. Journal of Hepatology, 55, 183-191. doi:10.1016/j.jhep.2010.12.030
- Kramvis, A. and Kew, M.C. (2007) Epidemiology of hepatitis B virus in Africa, its genotypes and clinical associations of genotypes. Hepatology Research, 37, S9- S19. doi:10.1111/j.1872-034X.2007.00098.x
- Lohouès-Kouacou, M.J., Touré, M., Hillah, J., et al. (1998) Materno-fetal transmission of hepatitis B virus in Ivory Coast. Plea for mass vaccination. Sante, 8, 401-404.
- Candotti, D., Danso, K. and Allain, J.P. (2007) Maternofetal transmission of hepatitis B virus genotype E in Ghana, West Africa. Journal of General Virology, 88, 2686-2695. doi:10.1099/vir.0.83102-0
- Sangaré, L., Sombié, R., Combasséré, A.W., et al. (2009) Antenatal transmission of hepatitis B virus in an area of HIV moderate prevalence, Burkina Faso. Bulletin de la Société de Pathologie Exotique, 102, 226-229.
- Del Canho, R., Grosheide, P.M., Mazel, J.A., et al. (1997) Ten-year neonatal hepatitis B vaccination program, The Netherlands, 1982-1992: Protective efficacy and longterm immunogenicity. Vaccine, 15, 1624-1630. doi:10.1016/S0264-410X(97)00080-7
- Pan, C.Q., Duan, Z., Bhamidimarri, K.R., et al. (2012) An algorithm for risk assessment and intervention of mother to child transmission of hepatitis B virus. Clinical Gastroenterology and Hepatology, 10, 452-459. doi:10.1016/j.cgh.2011.10.041
- Zou, H., Chen, Y., Duan, Z., et al. (2012) Virologic factors associated with failure to passive-active immunoprophylaxis in infants born to HBsAg-positive mothers. Journal of Viral Hepatitis, 19, e18-e25. doi:10.1111/j.1365-2893.2011.01492.x
- Pol, S. (2007) Epidemiology and natural history of HBV infection. Hepato-Gastro, 14, 6-15.
- Fattovich, G., Bortolotti, F. and Donato, F. (2008) Natural history of chronic hepatitis B: Special emphasis on disease progression and prognostic factors. Journal of Viral Hepatitis, 48, 335-352. doi:10.1016/j.jhep.2007.11.011
- Chu, C.M. and Liaw, Y.F. (2009) Incidence and risk factors of progression to cirrhosis in inactive carriers of hepatitis B virus. Journal of Viral Hepatitis, 104, 1693- 1699. doi:10.1038/ajg.2009.187
- Lok, A.S. and McMahon, B.J. (2009) Chronic hepatitis B: Update 2009. American Association for the Study of Liver Diseases Practice Guidelines. Hepatology, 50, 661- 662. doi:10.1002/hep.23190
- Liaw, Y.F., Kao, J.H., Piratvisuth, T., et al. (2012) AsianPacific consensus statement on the management of chronic hepatitis B: A 2012 update. Hepatology International, 6, 531-561. doi:10.1007/s12072-012-9365-4
- European Association for the Study of the Liver (2012) EASL Clinical Practice Guidelines: Management of chronic hepatitis B virus infection. Journal of Hepatology, 57, 167-185.
NOTES
*Corresponding author.

