Paper Menu >>
Journal Menu >>
 J. Biomedical Science and Engineering, 2009, 2, 239-244 doi: 10.4236/jbise.2009.24037 Published Online August 2009 (http://www.SciRP.org/journal/jbise/ JBiSE ). Published Online August 2009 in SciRes. http:// www.scirp.org/journal/jbise Detection ischemic episodes from electrocardiogram signal using wavelet transform Mohammad Karimi Moridani, Majid Pouladian Biomedical Engineering Department, Science and Research Branch, Islamic Azad University, Tehran, Iran Email: Karimi.m@srbiau.ac.ir Received 19 November 2008; revised 16 March 2009; accepted 16 April 2009. ABSTRACT In this paper, we propose an algorithm for de- tection of myocardial ischemic episodes from electrocardiogram (ECG) signal using the wavelet transform technique. The algorithm was tested on data from the European ST-T change database. Results show that this algorithm is effective for distinguishing normal ECGs from ischemic. We developed a method that uses wavelets for extracting ECG patterns that are characteristic for myocardial ischemia. Keywords: Myocardial Ischemic; Wavelet Trans- form; ECG 1. INTRODUCTION The formulation and properties of an electrical impulse through the heart muscle result in time-varying poten- tials on the surface of the human body, which are known as the ECG signals. The signal represents various activi- ties of the heart [1]. Wavelet Transformation (WT) has shown to be substantially noise-proof in ECG segmenta- tion, and thus very appropriate for ST-T segment extrac- tion (Figure 1). An initial downward deflection after the P-wave is termed as, ‘Q’, the dominant upward deflec- tion is the ‘R’ and the terminal part is denoted as ‘S’. The T-wave represents ventricular recovery or repolari- zation [1,2]. The ST segment usually merges smoothly and imper- ceptibly with the T-wave. Having a simple estimate of whether an ECG re- cording which includes segments is characteristic for ischemic heart or not, is one of the most interesting top- ics for cardiologists. Our aim in this research is to develop an algorithm using WT for identification of myocardial ischemic epi- sodes. 2. METHOD For ECG parameters estimation, it is desirable that the Figure 1. ECG waveform. basis functions (wavelets), be symmetric/antisymmetric Asymmetric basis will enable to detect the extreme of wave’s peak [4]. In case of antisymmetric basis, the peak of the wave is detected as a zero crossing. In order to have a computationally simple analysis, the peaks should be detected as zero crossings (which is provided by antisymmetric basis) or local extreme (symmetric basis) [4]. It is also desirable that basis have a minimum number of sign changes. In practice, QRS complex is usually considered to be symmetrical, while T wave is less so. However, it has been shown, PR and ST points can be estimated using biorthogonal wavelets under the assumption of QRS complex and T wave symmetry [2]. Moreover, having as an aim proposed quantitative analysis, it is quite plausible to suppose ba- sic QRS complex and T wave symmetry [4]. Biorthogo- nal wavelets satisfy both these properties, so they are used for DWT (discrete wavelet transform) decomposi- tion. Hence used in this work. The filter coefficients of both the symmetric low pass (LP) H and the antisym- metric high pass (HP) filters G and K are given in Table 1 [2]. Decomposition and reconstruction filters satisfy further equations: 1)()()( 2 wKwGwH (1) where, w is frequency piw wewH ))2/(cos()( 2 (2) )2/sin(4)( 2wiewGiw (3)  240 M. K. Moridani et al. / J. Biomedical Science and Engineering 2 (2009) 239-244 SciRes Copyright © 2009 JBiSE )( )(1 )( 2 wG wH wK (4) 1i and p=3,5,7,… For compact support ‘p’ should be as small as possible. Hence, it was chosen to be equal to 3. The filter coeffi- cients corresponding to p=3 are given in Table 1. 2.1. Parameters Estimation The parameters of the ECG signal are obtained by the wavelet decomposition dyadic tree. This tree decom- poses the signal initially into the smooth (low pass) and detail (high pass) constituents [1]. The low pass compo- nent is further decomposed into low pass and high pass. This process is repeated over the desired number of scales. When an ECG signal is passed through each of the wavelet filters whose scales range from 21 to 24, as shown in Figure 2, the detailed d1, k, d2 ,k, d3, k d4, k and the smooth s1, k, s2, k, s3, k, s4, k filtered outputs are obtained as shown in Figure 3. The following algo- rithm is suggested for estimating the said ECG parame- ters [1]. This initial filter is also based upon WT. The denois- ing procedure is performed in three steps (MATLAB wavelet toolbox) [2]: 1) decomposition with sym8 wavelet at level 5, 2) detailed coefficients threshold- choosing a thresh- old for each level, 3) reconstruction. In order to obtain ST and PR points’ values, each de- composed ECG is segmented (Figure 1). At the first and the second levels, QRS starting, ending and peak point are Table 1. Filter coefficients of symmetric Low Pass (LP), anti- symmetric High Pass (HP) and their reconstruction filters. H G K L 0.1768 0.5303 0.5303 0.1768 0.3536 1.0607 -1.0607 -0.3536 0.1768 -0.5303 0.5303 -0.1768 -0.3536 1.0607 1.0607 -0.3536 G, decomposition high pass filter coefficients; H, decomposition low pass filter coefficients; K, reconstruction high pass filter coefficients; L, reconstruction low pass filter coefficients. Figure 2. Wavelet decomposition of ECG signal. Decomposi- tion per-formed over 4 scales. extracted. Let us denote as -the R peak point, nl, and n, 2 the beginning and ending points of QRS complex respectively [2]. PR point is thus calculated as: R n 2 int 12 ll R nn nPRpo (5) At the fourth level, ST-T characteristic points are ob- tained: - the T peak point, nt1 and nt2 the beginning and ending points of T wave, respectively [1]. ST point is calculated as: T n 2 int 12 ll T nn nSTpo (6) Wavelet decomposition introduces scale-dependent phase delay into signals. For example, each zero cross- ing point which corresponds to the peak of a symmetric uniphase wave is delayed for exactly 121 J points, where represents the scale [1]. 2.2. ST Deviation Analysis In our analysis, we have used European ST-T change database with ischemic ECG signals sampled at 250 Hz, two hours in duration each. The most elementary differ- entiate/threshold algorithm has been applied to extract each beat. Obtained signals were decomposed as de- scribed in section 2.1 and for each beat/separate signal, an ST deviation value was calculated as [2]: int)(int)( STpoECGvaluePRpoECGvalue nSTdeviatio (7) where ECG value(x) denotes an amplitude at the point x of a given ECG. Cases with specific ECG beats, that is to say with in- distinguishable ECG features (thus impossible segmen- tation), were excluded from further analysis. In this way, an ST deviation value was obtained for each beat that could be analyzed [2]. The final report might include the comment that some beats were excluded from analysis as well as the number of the beats omitted, and therefore suggest a manual observation where required [2]. 2.3. QRS Onset and Offset Detection Some of the existing techniques use a series of band- pass filters to extract QRS complexes from the ECG signal, which under severe baseline drift and other high frequency noises, fails to detect the characteristic points to an acceptable accuracy. And some techniques use neural network based adaptive identification algorithms [3,5], which can be used for only a particular type of pattern. The wavelet transform based technique can be used to identify the characteristic points of the ECG sig- nal to a fairly good accuracy, even with the presence of severe high frequency and low frequency noises [6,7,8]. Our aim is to describe an elegant algorithm, which uses  M. K. Moridani et al. / J. Biomedical Science and Engineering 2 (2009) 239-244 241 SciRes Copyright © 2009 JBiSE WT to identify the characteristic points of the ECG sig- nal, and identifying the myocardial ischemic episodes. As an alternative to the normal filtering techniques, which use different narrow-band filters to extract the frequency contents of the signal, wavelet transform technique can be used [3]. In wavelet transform tech- nique, the signal is analyzed at different frequencies with different resolutions. It is called multi resolution analysis (MRA) (Figure 4). The wavelet used in this work is the quadratic spline wavelet [9]. The reasons for choosing this particular wavelet for the analysis purpose are as follows: It has a very compact support and a generalized linear phase, so there is a determinate relationship between ECG characteristic points and the modulus maxima, or the zero-crossing points of the WTs. The Fourier transform (FT) of the quadratic spline wavelet is given as: 4 ) 4 4 sin ()( w w iww (8) The FIR(Finite Impulse Response) filter coefficients that make up the decomposition and reconstruction filter banks and the Lipschitz coefficients for the decomposi- tion algorithm are given in Tables 2 and 3 [3]. Figure 4. Block diagram of the entire process. Table 2. FIR filter coefficients for quadratic spline wavelet. N H G K L -3 -2 -1 0 1 2 3 0.125 0.375 0.375 0.125 -2.0 2.0 0.0078125 0.054685 0171875 -0.171875 -0.054685 -0.0078125 0.0078125 0.046875 0.1171875 0.65625 0.1171875 0.046875 0.0078125 G, decomposition High Pass filter coefficient; H, decomposition Low Pass filter coefficients; K, reconstruction High Pass filter coefficients; L, reconstruction Low Pass filter coefficients. Table 3. Normalization coefficients j for the quadratic spline wavelet. j j 1 2 3 4 5 1.5 1.12 1.03 1..01 1.00 There is a relation between the characteristic points of the signal and their WT at different levels [10,11,12]. For example, for the wave in Figure 5, the wavelet transform at scale 21 is given. The wave’s rising edge corresponds to a negative min- ima and the dropping edge corresponds to a positive maxima. The moduli of these maxima or minima corre- sponding to the same edge are named as the modulus maxima line. If the uniphase wave is symmetric to its peak, then its peak corresponds to the zero-crossing point of the positive maxima negative minima pair with a delay of exactly 12 1 J points, where j represents the scale [3]. After obtaining the wavelet transform coeffi- cients at different scales, the next step is to find out the ECG characteristic points from these coefficients [3]. 2.4. T and P Wave Detection T and P waves are normally low frequency, so WT at high scale is used to locate these waves. In this work, WT up to four scales are taken and the scale 24 is used to locate T and P waves. T wave creates a pair of modulus maxima with a dif- ferent sign on W2jf (n) at scale, 24 within a time window after the detected R-peak [3]. Since the wave is almost symmetric to its peak, the peak of T-wave corresponds to the zero crossing point of the modulus maximum pair with a delay of 24-1-1 points. The peak, onset and offset of the P-wave are detected in a way similar to those of the T before the detected R-wave [3]. 2.5. R-peak Detection For detecting the R-peak, the modulus maxima–minima pair is located at lowest scale, which is done by fixing a threshold for detection [13]. So maxima–minima pairs for other scales are located within the neighborhood of these maxima-minima pairs. If the amplitudes of the maxima-minima pairs, compared to those are at lower scale, are consistent or increasing, the corresponding Figure 5. The uniphase wave and its WT at scale 21. Filter Bank Digitized ECG WT Analysis algorithm ST-T detection Characteristic Points ST-T events 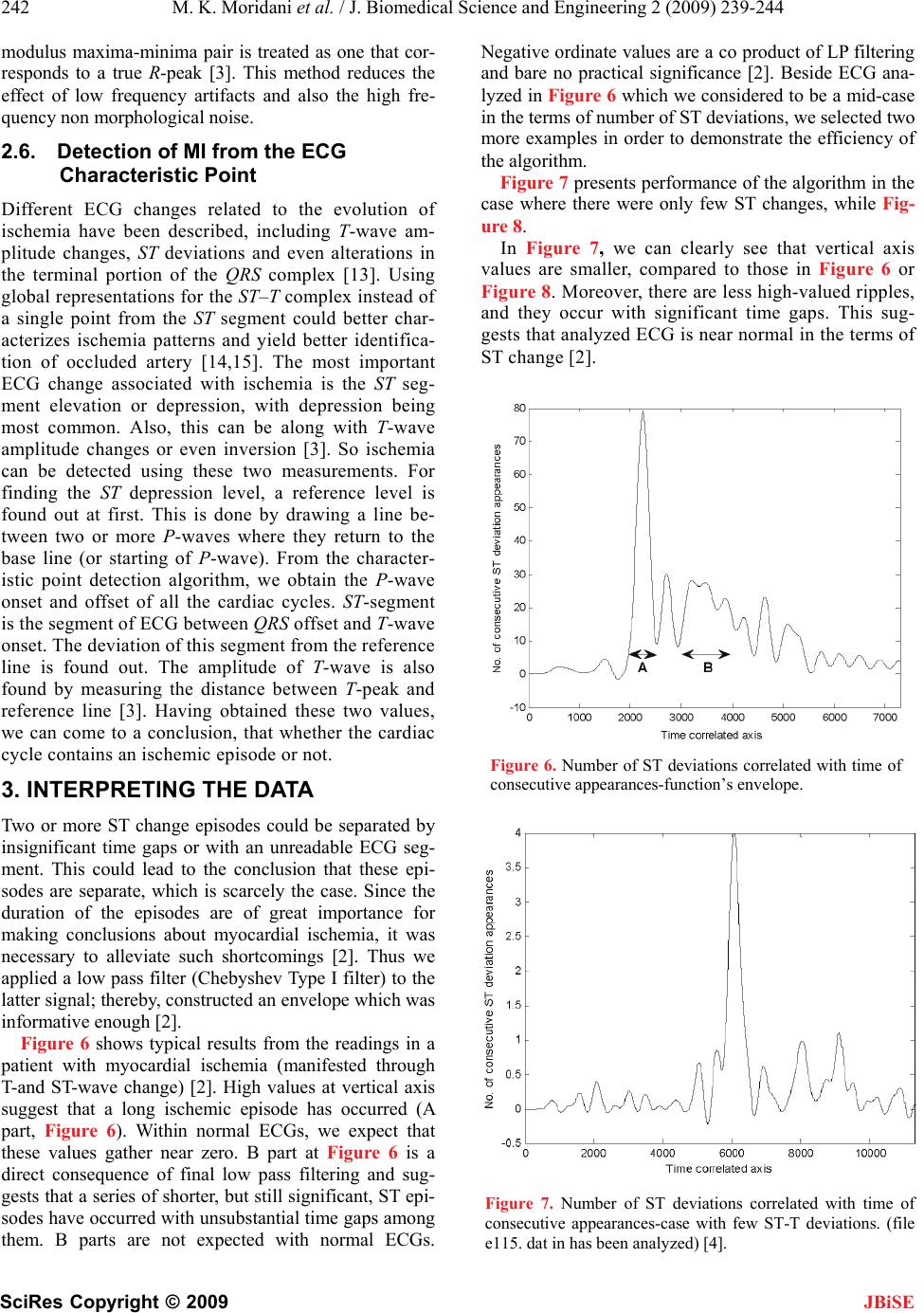 242 M. K. Moridani et al. / J. Biomedical Science and Engineering 2 (2009) 239-244 SciRes Copyright © 2009 JBiSE modulus maxima-minima pair is treated as one that cor- responds to a true R-peak [3]. This method reduces the effect of low frequency artifacts and also the high fre- quency non morphological noise. 2.6. Detection of MI from the ECG Characteristic Point Different ECG changes related to the evolution of ischemia have been described, including T-wave am- plitude changes, ST deviations and even alterations in the terminal portion of the QRS complex [13]. Using global representations for the ST–T complex instead of a single point from the ST segment could better char- acterizes ischemia patterns and yield better identifica- tion of occluded artery [14,15]. The most important ECG change associated with ischemia is the ST seg- ment elevation or depression, with depression being most common. Also, this can be along with T-wave amplitude changes or even inversion [3]. So ischemia can be detected using these two measurements. For finding the ST depression level, a reference level is found out at first. This is done by drawing a line be- tween two or more P-waves where they return to the base line (or starting of P-wave). From the character- istic point detection algorithm, we obtain the P-wave onset and offset of all the cardiac cycles. ST-segment is the segment of ECG between QRS offset and T-wave onset. The deviation of this segment from the reference line is found out. The amplitude of T-wave is also found by measuring the distance between T-peak and reference line [3]. Having obtained these two values, we can come to a conclusion, that whether the cardiac cycle contains an ischemic episode or not. 3. INTERPRETING THE DATA Two or more ST change episodes could be separated by insignificant time gaps or with an unreadable ECG seg- ment. This could lead to the conclusion that these epi- sodes are separate, which is scarcely the case. Since the duration of the episodes are of great importance for making conclusions about myocardial ischemia, it was necessary to alleviate such shortcomings [2]. Thus we applied a low pass filter (Chebyshev Type I filter) to the latter signal; thereby, constructed an envelope which was informative enough [2]. Figure 6 shows typical results from the readings in a patient with myocardial ischemia (manifested through T-and ST-wave change) [2]. High values at vertical axis suggest that a long ischemic episode has occurred (A part, Figure 6). Within normal ECGs, we expect that these values gather near zero. B part at Figure 6 is a direct consequence of final low pass filtering and sug- gests that a series of shorter, but still significant, ST epi- sodes have occurred with unsubstantial time gaps among them. B parts are not expected with normal ECGs. Negative ordinate values are a co product of LP filtering and bare no practical significance [2]. Beside ECG ana- lyzed in Figure 6 which we considered to be a mid-case in the terms of number of ST deviations, we selected two more examples in order to demonstrate the efficiency of the algorithm. Figure 7 presents performance of the algorithm in the case where there were only few ST changes, while Fig- ure 8. In Figure 7, we can clearly see that vertical axis values are smaller, compared to those in Figure 6 or Figure 8. Moreover, there are less high-valued ripples, and they occur with significant time gaps. This sug- gests that analyzed ECG is near normal in the terms of ST change [2]. Figure 6. Number of ST deviations correlated with time of consecutive appearances-function’s envelope. Figure 7. Number of ST deviations correlated with time of consecutive appearances-case with few ST-T deviations. (file e115. dat in has been analyzed) [4]. 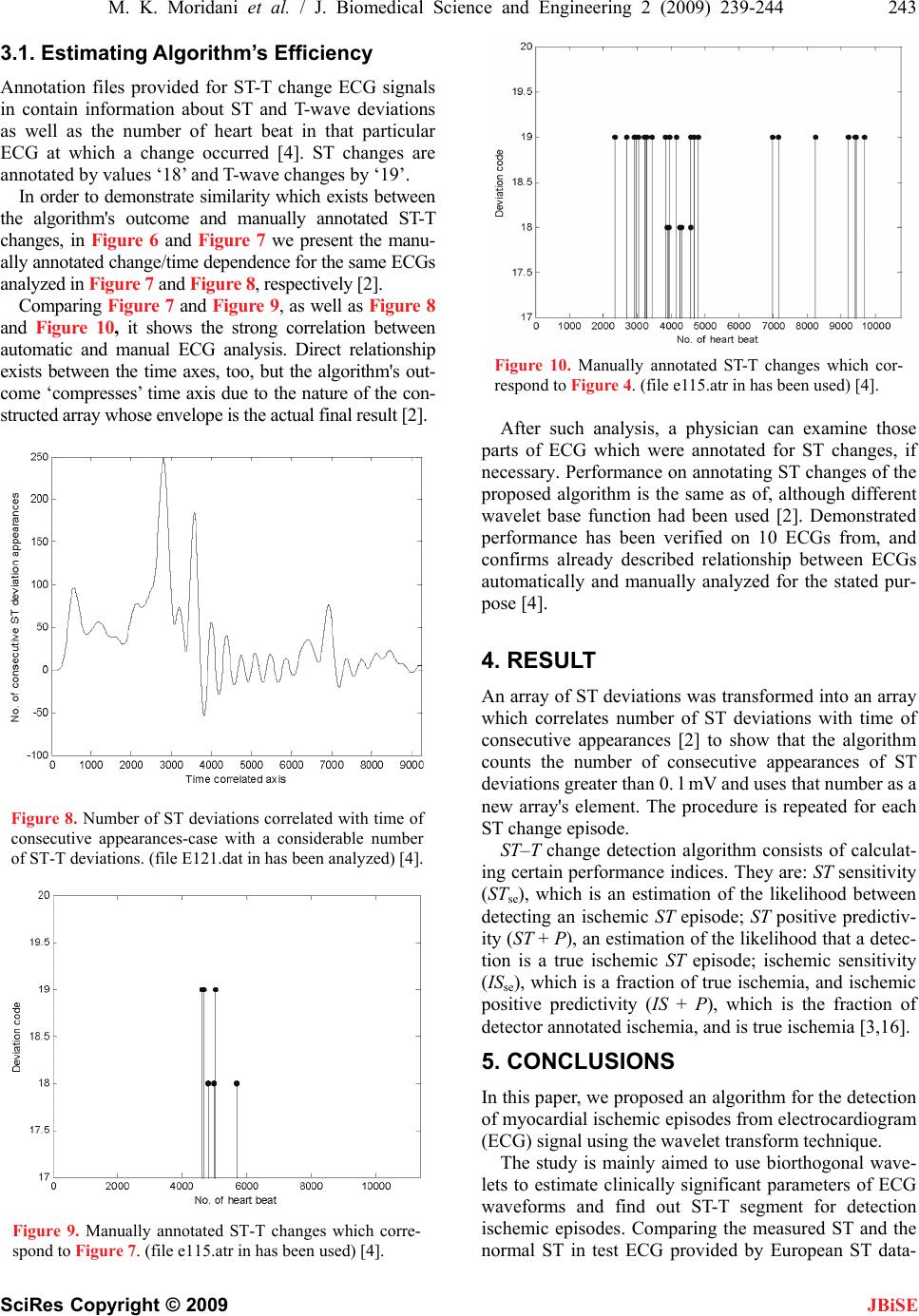 M. K. Moridani et al. / J. Biomedical Science and Engineering 2 (2009) 239-244 243 SciRes Copyright © 2009 JBiSE 3.1. Estimating Algorithm’s Efficiency Annotation files provided for ST-T change ECG signals in contain information about ST and T-wave deviations as well as the number of heart beat in that particular ECG at which a change occurred [4]. ST changes are annotated by values ‘18’ and T-wave changes by ‘19’. In order to demonstrate similarity which exists between the algorithm's outcome and manually annotated ST-T changes, in Figure 6 and Figure 7 we present the manu- ally annotated change/time dependence for the same ECGs analyzed in Figure 7 and Figure 8, respectively [2]. Comparing Figure 7 and Figure 9, as well as Figure 8 and Figure 10, it shows the strong correlation between automatic and manual ECG analysis. Direct relationship exists between the time axes, too, but the algorithm's out- come ‘compresses’ time axis due to the nature of the con- structed array whose envelope is the actual final result [2]. Figure 8. Number of ST deviations correlated with time of consecutive appearances-case with a considerable number of ST-T deviations. (file E121.dat in has been analyzed) [4]. Figure 9. Manually annotated ST-T changes which corre- spond to Figure 7. (file e115.atr in has been used) [4]. Figure 10. Manually annotated ST-T changes which cor- respond to Figure 4. (file e115.atr in has been used) [4]. After such analysis, a physician can examine those parts of ECG which were annotated for ST changes, if necessary. Performance on annotating ST changes of the proposed algorithm is the same as of, although different wavelet base function had been used [2]. Demonstrated performance has been verified on 10 ECGs from, and confirms already described relationship between ECGs automatically and manually analyzed for the stated pur- pose [4]. 4. RESULT An array of ST deviations was transformed into an array which correlates number of ST deviations with time of consecutive appearances [2] to show that the algorithm counts the number of consecutive appearances of ST deviations greater than 0. l mV and uses that number as a new array's element. The procedure is repeated for each ST change episode. ST–T change detection algorithm consists of calculat- ing certain performance indices. They are: ST sensitivity (STse), which is an estimation of the likelihood between detecting an ischemic ST episode; ST positive predictiv- ity (ST + P), an estimation of the likelihood that a detec- tion is a true ischemic ST episode; ischemic sensitivity (ISse), which is a fraction of true ischemia, and ischemic positive predictivity (IS + P), which is the fraction of detector annotated ischemia, and is true ischemia [3,16]. 5. CONCLUSIONS In this paper, we proposed an algorithm for the detection of myocardial ischemic episodes from electrocardiogram (ECG) signal using the wavelet transform technique. The study is mainly aimed to use biorthogonal wave- lets to estimate clinically significant parameters of ECG waveforms and find out ST-T segment for detection ischemic episodes. Comparing the measured ST and the normal ST in test ECG provided by European ST data-  244 M. K. Moridani et al. / J. Biomedical Science and Engineering 2 (2009) 239-244 SciRes Copyright © 2009 base, the algorithm could found the exactly time, that ST shape is changed into an abnormal shape. ST segment is the most important diagnostic parameter to finding myocardial ischemia therefore developed algorithm best coincidence with the database occurs in the determina- tion of the beginning of the ST episodes, and the worst in the calculation of the maximum deviation. Neverthe- less, this parameter is just used in the description of ischemia episodes, and its importance is relatively low with respect to the quantification of the number of epi- sodes and their duration. JBiSE REFERENCES [1] N. Sivannarayana, D. C. Reddy, (1999) Biorthogonal wavelet transforms for ECG parameters estimation, 167-174. [2] N. Milosavljevic and A. Petrovic, (2006) ST segment change detection by means of wavelets, 137-140. [3] P. Ranjith, P. C. Baby, and P. Joseph, (2003) ECG analy- sis using wavelet transform: application to myocardial ischemia detection, 44-47. [4] “European ST-T change database,” www. physionet.org. [5] N. Magaveras, T. Stamkopoulos, C. Pappas, and M. G. Strintzis, (1998) An adaptive backpropagation neural network for real-time ischemia episodes detection: De- velopment and performance analysis using the European ST-T database, IEEE Trans Biomed Eng, 45, 805-13. [6] M. Vetterly and J. Kovacevic, (1995) Wavelet and sub- band coding, First Edition, Upper Saddle River, NJ: Prentice Hall. [7] M. R. Raghuveer and S. Bopardikar, (1996) Wavelet transforms: Introduction to theory and applications, Sec- ond Edition, Boston, MA: Addison Wesley. [8] (1996) Special issue on wavelets, Proc IEEE, 84(4). [9] S. Mallat and S. Zhong, (1992) Characterization of sig- nals from multiscale edges, IEEE Trans PAMI, 14(7). [10] C. Li, C. Zheng, and C. Tai, (1995) Detection of ECG characteristic points using wavelet transform, IEEE Trans Biomed Eng, 42(1), 8-21. [11] D. P. Golden, R. A. Wolthuis, and G. W. Hoffler, (1973) A spectral analysis of the normal resting electrocardiogram, IEEE Trans Biomed Eng, 20(5), 366-72. [12] S. Mallat, (1991) Zero crossing of a wavelet transform, IEEE Trans Inf Theory, 37(4). [13] P. F. Cohn, (1993) Silent myocardial ischemia and infarc- tion, 8–18, NewYork: Marcel Dekker, 87-97. [14] F. Jager, G. B. Moody, and R. G. Mark, (1998) Detection of transient ST segment episodes during ambulatory ECG monitoring, Comput Biomed Res, 31(5), 305-22. [15] J. Garcia, L Sornmo, S. Olmos, P. Laguna, (2000) Auto- matic detection of ST–T complex changes on the ECG using filtered RMS difference series: Application to am- bulatory ischemia monitoring, IEEE Trans Biomed Eng; 47(9), 1195-201. [16] F. Jager, G. B. Moody, A. Taddei, R. G. Mark, (1991) Per- formance measures for algorithms to detect transient ischemic ST segment changes. Computers in Cardiology, Los Alamitos, CA: IEEE Computer Society Press, 372-96. |

