Open Journal of Pathology
Vol.05 No.04(2015), Article ID:60401,7 pages
10.4236/ojpathology.2015.54018
Gastric Cancer in Bahrain: A Retrospective Study of Histologically Confirmed Tumours between 2001 and 2007 from the Two Main Bahraini Referral Hospitals
Bedoor Al Omran, Naseem Ansari*
Department of Pathology, RCSI Bahrain, Busaiteen, Kingdom of Bahrain
Email: *ansarnas@gmail.com
Copyright © 2015 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 12 September 2015; accepted 17 October 2015; published 20 October 2015
ABSTRACT
Objective: Few data are available describing the epidemiology and pathology of stomach cancer in Bahrain. Methods: A retrospective study examining all histologically confirmed cases of gastric cancer at the two main referral hospitals in Bahrain during the period 2001-2007. Results: 116 cases of gastric cancer were histologically confirmed in this seven-year period. There were 94 cases (81%) of adenocarcinoma, 10 (8.6%) lymphoma, 7 (6.0%) gastrointestinal stromal tumour, and 5 (4.3%) neuroendocrine tumour. Of the 94 patients with adenocarcinoma 65 (69.1%) were male (p < 0.01). 24 out of 43 intestinal type adenocarcinomas were positive for intestinal metaplasia (p < 0.001). Between 2004 and 2006 when total annual numbers of gastric cancers overall and gastric adenocarcinoma decreased the total numbers of lymphoma increased. Conclusions: The most common type of gastric cancer in
Keywords:
Gastric Cancer, Adenocarcinoma, Helicobacter pylori, Intestinal Metaplasia, Lymphoma, Epidemiology, Pathology

1. Introduction
Stomach cancer is the fourth most common cancer worldwide. As such it is a significant cause of morbidity and mortality globally, and therefore accurate characterization of its epidemiology should lead to the way towards understanding its pathogenesis, risk factors involved and likely behavior and perhaps should indicate methods to prevent or treat the disease. Although there are several different histological types of stomach cancer including lymphoma, neuroendocrine tumours, gastrointestinal stromal tumour and sarcomas, by far the most common subtype of stomach cancer is adenocarcinoma, and it is largely this subtype being referred to when the term “stomach cancer” is used in unqualified manner.
The global variation in prevalence of gastric cancer is well known as its epidemiological characteristics in many countries and regions and the risk factors (established and putative) are well described. Little is known about stomach cancer in relation to the small island
2. Material and Methods
A retrospective study examining all histologically confirmed cases of gastric tumour diagnosed at the two main referral hospitals in Bahrain, Salmaniya Medical Complex and Bahrain Defence Force Royal Medical Services, during the period January 2001-December 2007. All cases of gastric tumour were identified by a combination of computer search and manual search of archived histopathology reports. All gastric tumour histopathology reports were retrieved from the pathology departments of the two study centres, collected and filed for inclusion in the study. Various epidemiological and pathological data were abstracted from the reports and recorded. Statistical analysis of data was performed using the SPSS software program.
3. Results
During the seven year period from January 2001 to December 2007 a total of 96,336 specimens were received in the histopathology departments of Salmaniya Medical Complex and Bahrain Defence Force Hospital for histological evaluation. Of these 11,435 were gastric specimens including 11,402 endoscopic biopsies and 33 gastrectomy specimens. A total of 116 gastric tumours were diagnosed in this seven year period. All 116 patients with gastric tumours presented to the gastroenterology clinic with one or more clinical symptoms including abdominal pain, weight loss, abdominal swelling, persistent vomiting and dysphagia.
Of these 116 gastric tumours 94 (81.0%) were carcinomas (adenocarcinoma), while 22 (18.8%) were tumours other than carcinoma. This latter group of “non-carcinoma” gastric tumours comprised 10 (8.6%) lymphomas, 7 (6.0%) gastrointestinal stromal tumours (GIST), and 5 (4.3%) neuroendocrine tumours (NET). By far the commonest type of gastric tumour encountered in
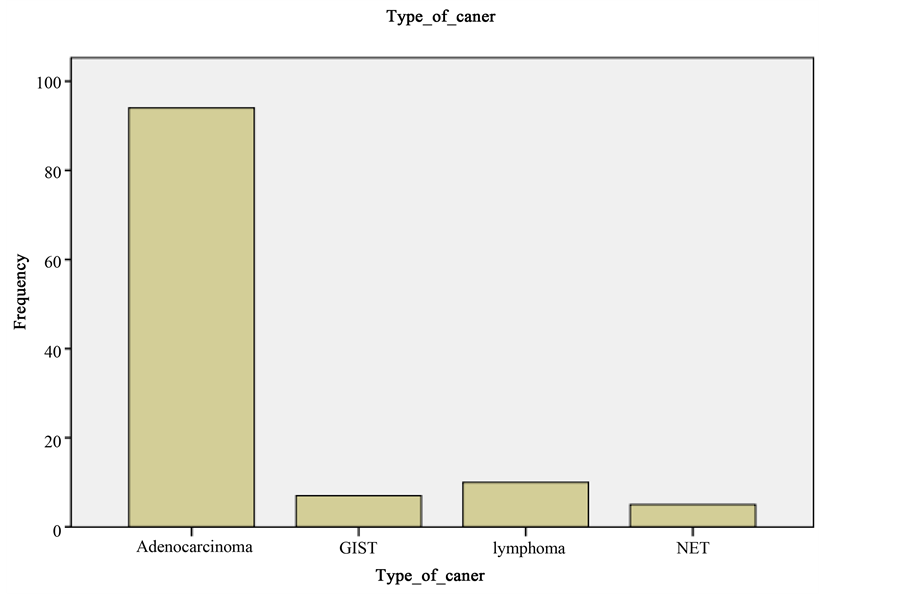
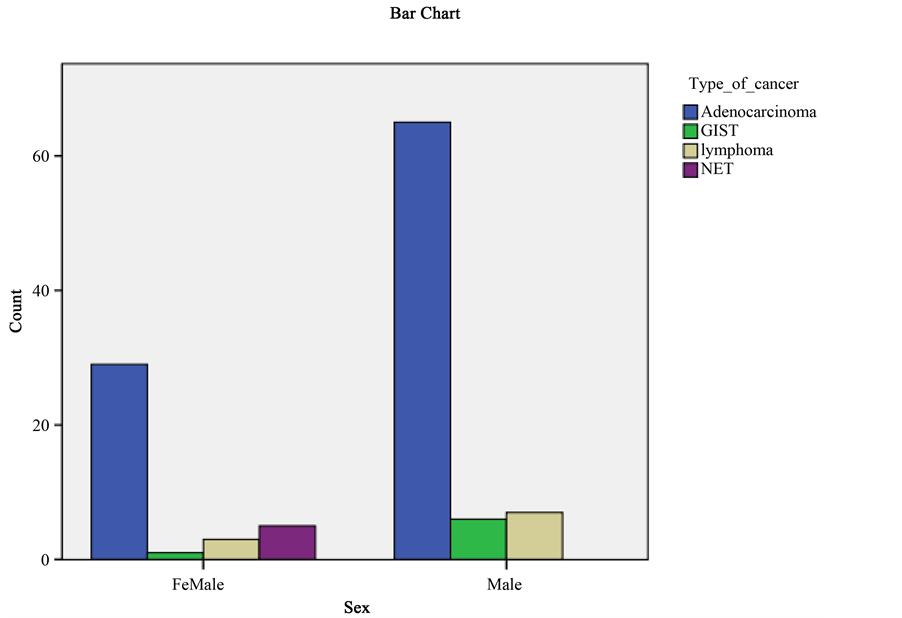
Figure 1 shows the numbers of each type of gastric tumour encountered in the study. Adenocarcinoma was the commonest type of gastric tumour disgnosed in Bahrain during the study period and the predominance of gastric adenocarcinoma in relation to other gastric tumours was a significant finding (p = 0.0001). The vast majority of adenocarcinoma cases (72/94, 76.6%) were Bahraini patients. The rest were mostly from other Gulf nations or expatriates from the Indian Subcontinent and The Philippines. Table 1 shows the relationship of patient age with incidence of different types of gastric tumour. In the case of adenocarcinoma 73 out of 94 (77.7%) patients were aged between 40 and 80. Figure 2 shows the relationship between patient gender and type of gastric tumour. A significant finding was that 65 of the 94 (69.1%) adenocarcinoma cases were male (p < 0.01).
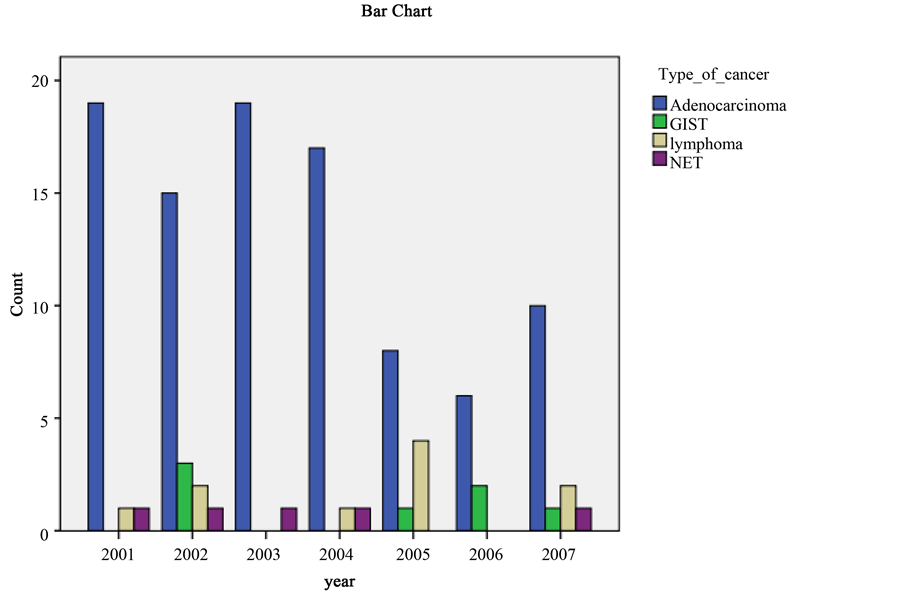
Figure 3 shows the numbers of each type of gastric tumour seen in each year of the study period. While the total number of gastric tumours remained fairly stable for each year from 2001 to 2004, there was a definite reduction in the total numbers for 2005 which remained at lower levels in 2006 before increasing again in 2007. Adenocarcinoma was the predominant tumour type in each year studied. Mirroring the trend for all tumours described above, the number of adenocarcinoma cases fell suddenly in 2005, remained low in 2006, and rose again
Figure 1. Bar chart showing numbers of each type of gastric cancer encountered in the study. GIST: Gastrointestinal Stromal Tumor; NET: Neuroendocrine Tumours.
Figure 2. The relationship of patient gender with type of gastric cancer.
Figure 3. Bar chart showing the numbers of each type of gastric cancer encountered in each year of the study.
Table 1. Age distribution for gastric cancers.
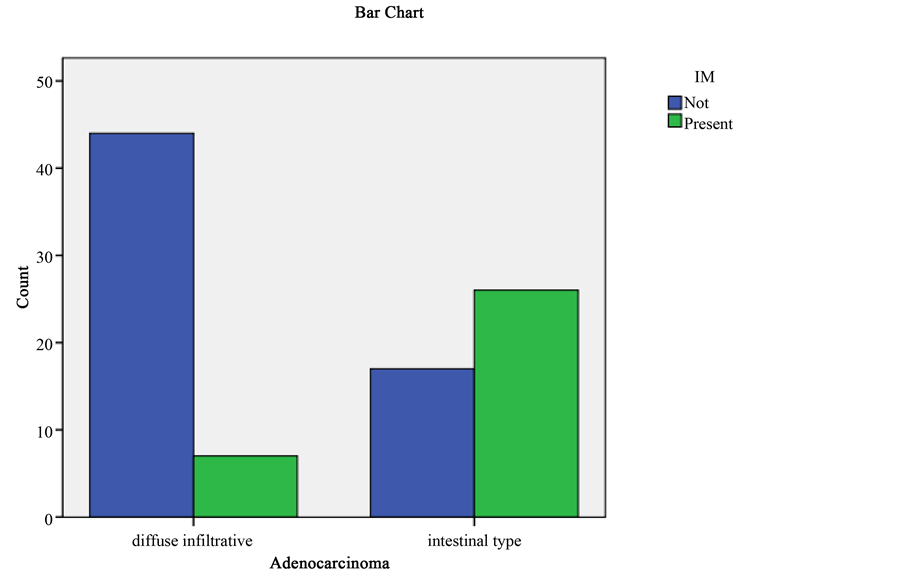
in 2007 (since the vast proportion of tumours identified were adenocarcinoma it is no surprise that yearly trend changes for adenocarcinoma are reflected almost exactly in the yearly trend changes for all tumours as a group). Despite this overall trend, interestingly from 2004 to 2006 (while total tumour numbers were falling) there was a reverse trend for the “non-carcinoma” group of tumours which increased in number (especially gastric lymphoma). H. pylori was identified in 28 cases of adenocarcinoma (29.8%) which overall did not support a significant association. Of these 28 H. pylori-positive cases, 15 (29.4%) were seen in the diffuse infiltrative subtype and 13 (30.2%) in the intestinal subtype, and for each of these subtypes a significant association with H. pylori was not apparent. Intestinal metaplasia was identified in 33 cases of adenocarcinoma (35.1%) which overall did not support a significant association. However, 26 of these intestinal metaplasia positive cases were patients with intestinal subtype of adenocarcinoma (60.5%) while only 7 cases of diffuse infiltrative adenocarcinoma had concurrent or preceding intestinal metaplasia (13.7%). These results shown in Figure 4 indicate a significant association between intestinal metaplasia and intestinal subtype gastric adenocarcinoma (p < 0.001). Interestingly 3 out of the 5 neuroendocrine tumour (carcinoid) cases (60%) were positive for intestinal metaplasia identified in biopsies predating the development of tumour in the context of autoimmune gastritis. Among the 55
Figure 4. Bar chart showing numbers of each subtype of adenocarcinoma that were positive and negative for intestinal metaplasia.
cases of adenocarcinoma in which the exact site of tumour within stomach was documented, 34 of these were located in the antrum and or pylorus (61.8%). Eleven out of 94 cases (11.7%) of adenocarcinoma had metastasized at the time of primary site histological diagnosis. All of these metastatic cases were diffuse infiltrative (signet ring) type adenocarcinoma.
4. Discussion
Primary tumours of the stomach are classified into those that are benign or malignant. The large majority are malignant and include carcinoma (adenocarcinoma), lymphoma, neuroendocrine tumours and mesenchymal tumours incorporating sarcoma and gastrointestinal stromal tumour (GIST). Of these, as confirmed in this study, adenocarcinoma is the most prevalent accounting for as many as 95% of all gastric cancers in some studies. Comparable with this figure we found that adenocarcinoma comprises 81% of all gastric cancers in Bahrain. Since the vast majority of gastric cancer is adenocarcinoma much of the epidemiological literature on the subject refers to gastric cancer, stomach cancer and gastric carcinoma (adenocarcinoma) interchangeably.
Stomach cancer is the fourth most common cancer worldwide with 989,600 new cases in 2010 and as it is a poor prognosis tumour its mortality rate is correspondingly high at 738,000 deaths per year [1] . The incidence of stomach cancer shows considerable variation globally, being especially high in countries like Japan (31.1/ 100,000/yr) [2] , Chile, Portugal and Bulgaria, lowest in countries like Egypt (2.3/100,000/yr), India (3.8), USA (4.1), UK (5.5), and showing intermediate levels in countries such as Turkey (13.5), Iran (15.6) and Israel (8.6). This variation is usually attributed to, but cannot be entirely explained by factors such as 1) socio-economic status, as Japan and USA have hugely different levels of stomach cancer and are both amongst the most affluent nations, 2) geographic location, as neighbouring countries such as Iraq and Iran show marked variance in incidence, 3) diet, since there is significant variation in incidence among Mediterranean countries which share similar dietary habits, and 4) Helicobacter seroprevalence, as countries with similar HP seroprevalence levels can show vastly different stomach cancer levels [3] [4] .
The incidence of histologically confirmed stomach cancer in Bahrain, derived from the current study figures of 116 cases out of a population of 1 million over a period of seven years, is 1.7/100,000/yr. This figure is likely to be an underestimate as there are presumably a number of surgical specimens received and reported at some of the smaller Bahraini hospitals (although this is certainly only a small number). Other factors that can help explain the apparently low incidence of stomach cancer in Bahrain are: firstly, the population of Bahrain is very small at approximately 1 million and therefore low numbers would be expected; secondly, there is a cultural tendency among some, especially in the small townships and villages, to rely on herbal practitioners and complementary medicine. These patients are likely to die of their disease before it is confirmed histologically or presentation at tertiary health centres only happens at a late stage when the disease is deemed inoperable; thirdly, there is also a tendency for patients to seek medical and surgical advice/treatment overseas and therefore diagnosis and management takes place abroad; fourthly, postmortem examination in Bahrain is restricted to medico-legal cases only, and there are undoubtedly cases of gastric cancer that escape detection on account of death intervening before prominent symptoms arise, and the non-existence of routine autopsies; and finally, some of the “occult” cases described above would still be recorded as gastric cancer cases if there were an effective local cancer registry (which is not the case at present but is an urgent requirement to record cases diagnosed in and outside Bahrain). In relation to these described factors the sudden fall in gastric carcinoma (and stomach cancer overall) that we discovered between 2004 and 2006 might be attributable to more patients seeking treatment overseas and therefore escaping detection in Bahrain. The increase in incidence in 2007 probably results from a real increase in the rate of stomach cancer despite patients traveling abroad for medical care.
It was noted that while overall stomach cancer rates were falling between 2004 and 2006, the incidence of gastric lymphoma rose during this same period. We postulate that this could be a response to the increase of potentially lymphomagenic factors released into the ecosystem a few years earlier during the Gulf War in 2003.
Almost thirty years after its discovery in 1983, the important role played by Helicobacter pylori in the pathogenesis of several gastric diseases is firmly established [5] . These diseases include gastritis, peptic ulcer and gastric malignancy. In the context of gastric cancer it is known to be an aetiological factor for gastric carcinoma (adenocarcinoma) and gastric marginal zone B cell lymphoma (maltoma). Contrary to expectations the present study did not reveal a significant association between histologically identified H. pylori and subsequent or concurrent existence of gastric adenocarcinoma (or either of the two broad subtypes). Proposed explanations for this apparent lack of association are: firstly, H. pylori numbers may have been low and the pathogen consequently missed; secondly, in small biopsy material which is extensively infiltrated by tumour it can be difficult to identify non-neoplastic gastric mucosa which harbours the organism or there might not be any non-neoplastic gastric mucosa included in the biopsy; thirdly, more sensitive special stain techniques for the detection of H. pylori employing silver-based reagents such as the Warthin-Starry technique were not performed, largely because they are lengthy and require considerable histotechnical dexterity; fourthly, H. pylori detection rates decrease with the progression of intestinal metaplasia and atrophy; fifthly, during the process of surgical biopsy sign out once the main diagnosis of cancer was established other biopsy features, e.g presence/absence of H. pylori may have been overlooked or not mentioned in the report; and lastly, effective anti helicobacter medical therapy may have been instituted well in advance of the biopsy resulting in eradication of the organism and H. pylori negative biopsies.
Studies on the prevalence of H. pylori in various Gulf state populations presenting with dyspepsia show variation according to (to some degree) which tests are used to identify the microbe. For example, a study from Bahrain [6] demonstrated a H. pylori prevalence of 75% when biopsy culture was used and 54% when serology was used in the same patients. In a Kuwaiti study [7] utilizing the urea breath test 50% of their dyspeptic patients were found to be H. pylori positive. The sensitivity of light microscopy for the detection of H. pylori, even with special stains, is lower than these figures especially when microbe density in the biopsy is low. We expect that correlation of biopsy findings with other H. pylori detection tests, if done, e.g. serology would reveal a higher H. pylori infection rate in these Bahraini gastric adenocarcinoma cases.
The present study revealed that two of the ten cases of gastric lymphoma showed presence of H. pylori organisms in either the same or preceding biopsy material from the patient. In agreement with the accepted causative association between H. pylori and gastric marginal zone B cell lymphoma, both H. pylori positive cases were marginal zone lymphomas. Interestingly, a proportion of these marginal zone lymphomas of the stomach completely regress in response to anti Helicobacter therapy. However, we do not have follow-up data on these cases. The eight H. pylori negative cases of gastric lymphoma were diffuse large B cell lymphoma, a tumour that is not causatively associated with H. pylori.
The present study showed that there was a significant association between intestinal metaplasia and concurrent or subsequent existence of intestinal subtype gastric adenocarcinoma. This is in concordance with the firmly accepted notion that intestinal metaplasia in the gastric mucosa is a histological precursor of intestinal subtype gastric adenocarcinoma [8] . As expected, there was no association demonstrated between intestinal metaplasia and diffuse infiltrative subtype gastric adenocarcinoma.
Three of the five cases of neuroendocrine tumour (carcinoid) also showed foci of intestinal metaplasia in the concurrent or preceding biopsy material from the patient. The intestinal metaplasia was detected as part of the histological picture of autoimmune gastritis in each of these three cases, a known precursor of gastric carcinoid. Autoimmune gastritis can lead to intestinal metaplasia and endocrine cell hyperplasia which eventually develops into carcinoid tumour [9] . Autoimmune gastritis can also cause mucosal atrophy and thereby lead to gastric adenocarcinoma [10] .
Eleven of the adenocarcinoma cases metastasized to lymph nodes and or distant organs. All such cases were histologically diffuse infiltrative in subtype, and this is consistent with the known high agressivity of this subgroup [11] .
The M:F gender ratio for our gastric cancers was 2:1 which is entirely consistent with established data from other parts of the world [12] .
Notably, in the present study there were seven GIST diagnosed by histological morphology, and the immunohistochemical profile of CD34+ve, smooth muscle actin (SMA)?ve, S100?ve. Since CD117 antibody has high specificity for GIST and imparts prognostic information in relation to likelihood of response to the biologic agent imatinib [13] , it is an antibody which should feature prominently in any diagnostic pathology laboratory.
5. Conclusion
The most common type of gastric cancer in Bahrain is adenocarcinoma, and the two main subtypes, intestinal and diffuse (Lauren classification), are encountered in approximately equal numbers although there is a slight predominance of diffuse subtype. While there was a broadly stable trend in the total number of gastric tumours and adenocarcinoma during the study period there was an overall reduction in these tumours during the middle two years of the study, and possible explanations for this were suggested. An association between histologically confirmed Helicobacter pylori and gastric adenocarcinoma (overall) and individual subtypes (intestinal or diffuse) was not demonstrated in this study and reasons for this apparent unexpected outcome were discussed. An association between intestinal metaplasia and intestinal subtype gastric adenocarcinoma was confirmed. On the basis of an increased association with metastasis at the time of presentation, the higher aggressivity of diffuse subtype as compared with intestinal subtype was demonstrated. The non-carcinoma gastric tumours in Bahrain comprise a small proportion of all gastric tumours and include lymphoma, neuroendocrine tumours and gastrointestinal stromal tumours. During the period when overall gastric tumour numbers in Bahrain were following a decreasing trend the numbers of gastric lymphoma cases increased. In keeping with the known aetiological association of Helicobacter pylori and gastric marginal zone B cell lymphoma (maltoma) all cases of gastric maltoma were H. pylori positive while the gastric diffuse large B cell lymphomas were H. pylori negative.
Acknowledgements
This study was funded by the RCSI Association of Graduates Undergraduate Medical Student Research Award, awarded to Bedoor Al Omran.
Cite this paper
Bedoor AlOmran,NaseemAnsari, (2015) Gastric Cancer in Bahrain: A Retrospective Study of Histologically Confirmed Tumours between 2001 and 2007 from the Two Main Bahraini Referral Hospitals. Open Journal of Pathology,05,129-136. doi: 10.4236/ojpathology.2015.54018
References
- 1. Jemal, A., Bray, F., Center, M.M., Ferlay, J., Ward, E. and Forman, D. (2011) Global Cancer Statistics. CA—A Cancer Journal for Clinicians, 61, 69-90.
- 2. Globocan (2008) World Health Organization. International Agency for Research on Cancer.
http://globocan.iarc.fr - 3. Kikuchi, S., Wada, O., Nakajima, T., Nishi, T., Kobayashi, O., Konishi, T. and Inaba, Y. (1995) Serum Anti-Helicobacter Pylori Antibody and Gastric Carcinoma among Young Adults. Research Group on Prevention of Gastric Carcinoma among Young Adults. Cancer, 75, 2789-2793.
http://dx.doi.org/10.1002/1097-0142(19950615)75:12<2789::AID-CNCR2820751202>3.0.CO;2-4 - 4. Nomura, A., Stemmermann, G.N., Chyou, P.H., Kato, I., Perez-Perez, G.I. and Blaser, M.J. (1991) Helicobacter pylori Infection and Gastric Carcinoma among Japanese Americans in Hawaii. The New England Journal of Medicine, 325, 1132-1136.
http://dx.doi.org/10.1056/NEJM199110173251604 - 5. Weck, M.N., Gao, L. and Brenner, H. (2009) Helicobacter pylori Infection and Chronic Atrophic Gastritis: Associations According to Severity of Disease. Epidemiology, 20, 569-574.
http://dx.doi.org/10.1097/EDE.0b013e3181a3d5f4 - 6. Kamath, R., Al-Qamish, J. and Yousif, A. (1995) Prevalence of Helicobacter pylori among Dyspeptic Patients in Bahrain. Bahrain Medical Bulletin, 17, 50-52.
- 7. Alazmi, W.M., Siddique, I., Alateeqi, N. and Al-Nakib, B. (2010) Prevalence of Helicobacter pylori Infection among New Outpatients with Dyspepsia in Kuwait. BMC Gastroenterology, 10, 14.
http://dx.doi.org/10.1186/1471-230X-10-14 - 8. Leung, W.K., Kim, J.J. and Kim, J.G. (2000) Microsatellite Instability in Gastric Intestinal Metaplasia in Patients with and without Gastric Cancer. The American Journal of Pathology, 156, 537-543.
http://dx.doi.org/10.1016/S0002-9440(10)64758-X - 9. Capella, C., Fiocca, R. and Cornaggia, M. (1999) Autoimmune Gastritis. In: Graham, D.Y., Genta, R.M. and Dixon, M.F., Eds., Gastritis, Lippincott Williams, Philadelphia, 79-96.
- 10. Whittingham, S. and Mackay, I.R. (2005) Autoimmune Gastritis: Historical Antecedents, Outstanding Discoveries, and Unresolved Problems. International Reviews of Immunology, 24, 1-29.
http://dx.doi.org/10.1080/08830180590884413 - 11. Piessen, G., Messager, M., Leteurtre, E., Jean-Pierre, T. And Mariette, C. (2009) Signet Ring Cell Histology Is an Independent Predictor of Poor Prognosis in Gastric Adenocarcinoma Regardless of Tumoural Clinical Presentation. Annals of Surgery, 250, 878-887.
http://dx.doi.org/10.1097/SLA.0b013e3181b21c7b - 12. Garcia, M., Jemal, A., Ward, E.M., Center, M.M., Hao, Y., Siegel, R.L. and Thun, M.J. (2007) Global Cancer Facts & Figures 2007. American Cancer Society, Atlanta.
https://www.cancer.org/acs/groups/content/@nho/documents/document/globalfactsandfigures2007re v2p.pdf - 13. Eisenberg, B.L. and Trent, J.C. (2011) Adjuvant and Neoadjuvant Imatinib Therapy: Current Role in the Management of Gastrointestinal Stromal Tumours. International Journal of Cancer, 129, 2533-2542.
http://dx.doi.org/10.1002/ijc.26234
NOTES

*Corresponding author.