Open Journal of Gastroenterology
Vol.4 No.3(2014), Article ID:43768,11 pages DOI:10.4236/ojgas.2014.43020
Laryngopharengeal Reflux in Gastroesophageal Reflux Disease: Does “Silent Laryngopharengeal Reflux” Really Exist?
Iman Ramzy1, Mohamed El Shazly2, Raghda Marzaban1, Tamer Elbaz1, Mina Safwat2, Botros Latif3
1Endemic Medicine and Hepatogastroenterology, Faculty of Medcinie, Cairo University, Cairo, Egypt
2Otorhinolaryngeology, Faculty of Medicine, Cairo University, Cairo, Egypt
3Hepatogastroenterology, Police Recruits Hospital, Cairo, Egypt
Email: won10@uga.edu, rsd7@psu.edu
Copyright © 2014 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/


Received 20 January 2014; revised 24 February 2014; accepted 2 March 2014
ABSTRACT
Background: Gastroesophageal reflux disease (GERD) is a disorder resulting from the reversed flow of gastroduodenal contents into the esophagus, and producing different symptoms, while laryngopharyngeal reflux (LPR) is a disorder resulting from the reversed flow of gastric contents into the hypopharynx. The aim of this work is to evaluate LPR in cases of GERD. Methods: The present study was performed on fifty GERD patients diagnosed by gastroscope. LPR was assessed by reflux symptoms score (RSI) and reflux finding score (RFS). Accordingly, patients are classified into: Group I = 25 patients with manifest LPR, and Group II = 25 control patients without LPR symptoms. Results: GERD accounts for 17.4% of attendants of gastroscope unit, where manifest LPR accounts for 29.1% of GERD cases recording mean RSI and RFS 16.48 and 8.44 respectively. Silent LPR accounts for 8% recording mean RFS 7. Conclusion: There is a significant direct proportional relationship between severity of GERD and the RSI and RFS (p = 0.015 and 0.005 respectively).
Keywords:Gastroesophageal Reflux Disease (GERD); Laryngopharyngeal Reflux (LPR); Reflux Symptoms Index (RSI); Reflux Finding Score (RFS)

1. Introduction
Gastroesophageal reflux disease (GERD) is diagnosed clinically or histologically due to abnormal exposure of the oesophagus to gastric contents [1] . Extraesophageal manifestations are the complicated GERD primarily involving the neighboring organs [2] . Laryngopharyngeal reflux (LPR) is common, but its diagnosis may be difficult, for its symptoms are nonspecific and its laryngoscopic signs are not always correlated with symptom severity [3] . Little gastric content can induce laryngitis as laryngeal tissue is more vulnerable to such injury than oesophageal one [4] . There is neither pathognomonic symptom nor sign for LPR, but both reflux symptoms index (RSI) and reflux finding score (RFS) were validated for its diagnosis [5] .
2. Patients and Methods
This study was conducted on adult patients with GERD diagnosed at Gastrointestinal Endoscopy Unit, Faculty of Medicine, Cairo University. Exclusion criteria: a) Patients giving history of peptic ulcer disease or anti ulcer medications or previous anti ulcer surgery, b) Patients having local laryngopharyngeal affection and those having causes inducing GERD like allergy, alcohol, tobacco, drugs.
The selected patients were divided into 2 groups: Group I: patients complaining of any of the LPR symptoms, and Group II: control cases who were not complaining of any of the LPR symptoms.
All patients were subjected to: a) History taking, including evaluation of GERD symptoms as heart burn, regurgitation, halitosis, dysphagia and dyspepsia, and LPR symptoms, defined as RSI, including hoarseness, throat clearing, postnasal drip, dysphagia, irritant cough, dyspnea, and globus, as designed by Belafsky et al. (2002) [6] , and shown in Table1 Score > 13 is suggestive of LPR. b) Oesophagogastroduodenoscope using Olympus endoscopy for evaluating GERD, where Los Angeles classification was applied [7] and GERD oesophagitis was graded as follows: A: One (or more) mucosal break ≤ 5 mm, that does not extend between the tops of two mucosal folds, B: One (or more) mucosal break > 5 mm long that does not extend between the tops of two mucosal folds, C: One (or more) mucosal break that is continuous between the tops of ≥2 mucosal folds but which involves ˂75% of the circumference, and D: One (or more) mucosal break which involves ≥ 75% of the esophageal circumference. It was also done to examine the presence of contributing factors of GERD as hiatus hernia, and the presence of any complications as Barrett’s esophagus, stricture, and esophageal carcinoma. c) Direct fiberoptic laryngoscopy for examination of LPR signs defined as RFS and designed by Belafsky et al. (2002) [6] , and shown in Table2 Score > 5 is considered abnormal.
The study was approved by the institutional ethical committee, and all patients provided an informed consent.
3. Results
This study was a cross sectional study, conducted on attendants of Gastrointestinal Endoscopy Unit, Faculty of
Medicine, Cairo University from May 2012 to June 2013.
GERD was diagnosed in 17.4% of attendants (86/494 patients). GERD patients were then divided into 2 groups: Group I: constituted of 25 patients (29.1%) having LPR. All reported by symptoms and were confirmed by laryngoscope, therefore termed as “Manifest LPR”, and Group II: GERD patients without LPR symptoms which constituted of 61 patients (70.9%), however, 25 patients where further examined by laryngoscope to serve as control group. Most of the control group (23/25 patients; 92%) were laryngoscopically free while 2 only (8%) had LPR. Accordingly, group II is subdivided into IIA who are “LPR-free”, and IIB who are defined as “Silent LPR” respectively.
Demographic features of the studied groups are shown in Table3 None of the demographic features showed a statistical difference between the 2 groups. Obesity was higher in Group I than in Group II but without recording a statistical difference, however, it is worth noting that obesity was reported by most of the studied patients (39/50 patients; 78%).
Gastrointestinal symptoms of the studied groups are shown in Table4 Heart burn and regurgitation were the commonest symptoms (80% each) however, halitosis, dysphagia and nausea, which were less common, were significantly higher in Group I than in Group II (p = 0.01, 0.01 and 0.037 respectively).
LPR symptoms in manifest LPR (Group I) are illustrated in Figure 1. The mean score was 16.48.
Oesophagogastroduodenoscopic examination of the studied groups is shown in Table5 Laryngoscopic examination (RFS) of the studied groups is shown in Table6 Laryngoscopy detected positive signs of LPR in 2 patients in Group II (Group IIB). Both recorded erythema, vocal fold edema and diffuse laryngeal edema, while ventricular obliteration, posterior commissure hypertrophy and thick endolaryngeal mucus were detected in one of them. They recorded mean RFS = 7. Therefore termed as silent LPR.
Correlation between GERD grade and LPR symptom index and LPR finding score are illustrated in Figures 2(a) and (b) respectively. Predictability of RSI according to RFS is illustrated in Figure 3.
4. Discussion
GERD is a common disease that may present with disabling symptoms [8] . GERD was defined as backflow of gastric contents causing disturbing symptoms and/or complications. It was classified into esophageal and extraesophageal syndromes. Recently, it became patient-centered approach independent of the laryngoscopic examination, subclassification of the disease into discrete entities e.g. laryngitis, cough, etc. and also Barrett’s esophagus [9] .
In this study, GERD accounts for 17.4% among attendants of gastroscope unit. This figure is intermediate. It was higher than that recorded in Asia (˂5%) [10] , and lower than that recorded in USA, being the 3rd digestive disease, and with the highest economic burden [11] . However, it was variably recorded in the western world as reported by Farrokhi et al. and Hershcovici et al. i.e. approximately 35% - 40% and 10% - 20% respectively [4] [12] .
In this study, neither sex nor age predilection was recorded in GERD. This is similar to Dent [10] . However
LPR: Laryngopharyngeal reflux, GERD: Gastroesophageal reflux disease, BMI: Body mass index.
LPR: Laryngopharyngeal reflux, GERD: Gastrooesophageal reflux disease.
LPR: Laryngopharyngeal reflux, GERD: Gastroesophageal reflux disease.
El-Serag found GERD increased with age (highest in the 60 - 69 years range, with a slight decrease afterwards), meanwhile, women had a slightly higher risk at age >50 years [13] . Similarly, Lee attributed this to the progressive decrease in abdominal lower eosophageal sphincter length and esophageal clearance and motility [14] . Also, Johnson recorded severe erosive esophagitis ranging from 12% in patients aged <21 years to 37% in patients
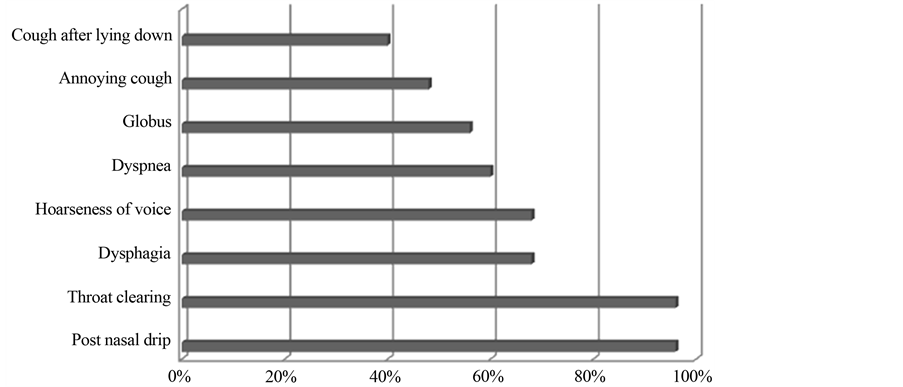
Figure 1. LPR symptoms of Group I.
LPR: Laryngopharyngeal reflux, GERD: Gastrooesophageal reflux disease, RFS: Reflux Finding Signs.
aged >70 years, and conversely, found heartburn ranging from 82% in patients aged <21 years to 34% of those aged >70 years [15] .
In the current study, 39 patients (78.0%) were obese (mean BMI = 31.8). Obesity was confirmed to be a strong predictor (95%) [16] , link to GERD-related symptoms [17] -[19] , and its complication up to esophageal adenocarcinoma [20] .
Heartburn was reported by 3/4 of the studied patients (38/50 patients; 76%), comparably present in Groups I and II (20 patients; 80% and 18 patients; 72% respectively), meanwhile grade A was more in Group II than in Group I (19 patients; 76% versus 15 patients; 60% respectively), while grades B, C & D (moderate & severe) are more in the Group I than in Group II. This confirmed the fact that heartburn was the only symptom related to GERD and LPR severity [21] .
Haematemesis was reported by 4 patients (8%), comparably present in Groups I and IIA. It is worth noting that they were following up their underlying oesophageal varices, complication of cirrhosis. This agrees with El-Serag who related history of haematemesis to positive GERD endoscopic examination [13] .
Regarding LPR, manifest LPR was present in 25 patients (29%) which is lower than that reported in an international survey (60%) [22] . Also, Merati documented significant relation between acid reflux events and LPR (p = 0.003) [23] .
 (a)
(a) (b)
(b)
Figure 2. (a) Correlation between GERD grade and RSI, GERD: Gastroesophageal reflux disease, RSI: Reflux symptom index (R = 0.482, p value = 0.015); (b) Correlation between GERD grade and RF; GERD: Gastroesophageal reflux disease, RFS: Reflux finding score (R = 0.544, p = 0.005).
LPR was not significantly related to either sex or age. On the contrary, Patigaroo et al. in their LPR study, found gender and age predilection (male:female = 2:3, and patients mostly-40%-belonged to age range 31 - 40 yrs) [24] . Mean age recorded in manifest LPR was slightly higher than GERD (40.4 versus 40.1 years). This was higher than that recorded by previous studies i.e. 38 and 32.4 years [24] [25] .

Figure 3. Predictability of RSI according to RFS. Overall accuracy = 98%, R2 = 0.86, p-value = 0.00. Sensitivity = 100%, specificity = 95.8%, PPV = 96.3%, NPV = 100%.
In this study, postnasal drip and throat clearing were the most prevalent symptoms (96% each). Throat clearing is the most related symptom to LPR [21] . They were followed by dysphagia, hoarseness (68% each), and globus (56%). This agrees with other studies which stated that sore throat, hoarseness, and choking cough are the most reliable symptoms of LPR [26] [27] . While annoying cough and post prandial/positional cough were the least symptoms (48% and 40% respectively). This figure is close to that recorded in previous studies e.g. Irwin et al. (48%) who stated that chronic cough can be the sole symptom of GERD [28] , and Patigaroo et al. (56%). GERD is generally considered one of the three main causes of chronic cough [29] . Also, 70% of LPR are found in patients with dysphagia [30] .
These figures are less than that recorded by Kouffman; throat clearing (98%), persistent cough (97%), globus (95%), and hoarseness (95%) [22] , and Said; persistent irritative cough (92%), sore throat (85%), globus (83%) [31] . On the contrary, Patigaroo et al.; clearing of throat (64%), globus (74%) [24] , and less figures reported by Youssef and Ahmed recorded; cough (49%), followed by globus (46%), throat clearing (36%), and hoarseness (25%) [25] , and Qadeer et al.; sore throat (40%), hoarseness (30%), and cough (20%) [27] .
Meanwhile, hoarseness was intermediate to previous studies e.g. >50 [32] , 62.8% [33], and 78.8% [34] .
Accordingly, the mean (RSI) score in manifest LPR was 16.48, while Patigaroo et al. reported higher score i.e. 24.75 [24] .
All of the studied GERD patients in this study had oesophagitis at variable degrees, as all of them were enrolled already diagnosed endoscopically, not on clinical suspect. Many other studies reported normal oesophogoscopy (62.7%, 59.6%, 60% - 70%, and 50% [31] [35] -[37] . It was even found in the minority of patients [38] for poor correlation between GERD clinically and histopathologically [35] . Gastroscope revealed inverse relation between grade of GERD and its incidence i.e. A (68%), B (28%), while C & D (4%). This is almost similar to Mearin et al. findings; A (32%), B (38.8%), C (25%), and D (4.2%) [39] .
Hiatus hernia was present in 11 patients (22%), comparably detected in both groups (6 and 5 patients in Groups I and II respectively). It was documented for its high specificity (95%) in predicting GERD [16] , even stated as a sine qua non for GERD, and that both were formerly considered synonyms [40] . Also, Fein et al. detected it in 75.6% of GERD [41] .
Barrett’s esophagus was detected in 2 patients of GERD (4%), both belonged to Group I. It was lower than that recorded previously e.g. 7.4% [42] , 10% [43] , and 5% - 15% [44] . However, other studies reported extreme values e.g. 1% [13] , and Koop who found it frequently in GERD patients [45] .
None of the patients showed esophageal carcinoma. This agrees with the fact its risk is low despite being strongly associated with GERD [44] .
The commonest laryngoscopic signs were vocal fold oedema, diffuse laryngeal oedema, erythema and posterior commisure hypertrophy (50%, 46%, 44%, 40% respectively). All were significantly higher in Group I than in Group II (92%, 84%, 80% and76% versus 8%, 8%, 8% and 4% respectively). This is lower than that recorded in an international survey i.e. arytenoid erythema (97.5%), vocal cord erythema (95.7%) and edema (95.7%), posterior commissure hypertrophy (94.9%), and arytenoid edema (94.0%) [22] . However, they were higher than that recorded by Qadeer et al.; medial arytenoid wall erythema/edema (60%), interarytenoid erythema (50%), and arytenoid complex erythema/edema (50%) [27] , Youssef and Ahmed; arytenoids erythema (54%), vocal cord oedema (27%) [25] , and Said; posterior commissure injection 82%, vocal cord edema (74%), laryngeal erythema (77%) and subglottic edema (24%) [31] .
Thick endolaryngeal mucus was detected in 14 patients (28%); mostly (13/14 patients; 92.8%) in Group I (52%), the left patient was nonsymptomatized. This is higher than that recorded by Ylitalo and Ramel; 50% - 60% in LPR [46] .
Laryngeal granuloma was detected in 8 patients (16%), all belonged to Group I (32%). This figure is intermediate to other studies e.g. Maronian et al. found GERD in all patients with organic subglottic stenosis and 71% with idiopathic subglottic stenosis. They concluded GERD a synergistic factor that stimulates laryngeal granulomatous reaction that may result in stenosis [47] . Also, Ylitalo and Ramel, and Ohman et al.; 65% - 74% respectively [46] [48] . On the contrary, Youssef and Ahmed (2%) [25] in LPR.
Pseudosulcus was detected in 6 patients (12%), all belonged to Group I. It is confirmed as a strong predictor (90%) for LPR [49] .
Accordingly, mean RFS of Group I was 8.44, which is lower than that recorded by Patigaroo; 12 [24] . Moreover, 2 patients of Group II (Subgroup IIB = 8%), had positive laryngoscopic signs of LPR and both recorded RFS 6 and 8 (mean RFS = 7), therefore defined as “Silent LPR”.
In this study, both RSI and RFS were significantly correlated with GERD grade (p = 0.015 and 0.005 respectively), and RSI was a significant predictor for RFS (p = 0.00), despite the stated fact that the endoscopic laryngeal signs do not correlate with LPR symptom severity, and treatment is recommended to continue for ≥6 months or until complete resolution of signs [3] [50] . Also accurate clinical assessment of LPR is likely to be difficult because laryngoscopic signs may show inter-observer variation [51] . Meanwhile, mild LPR can be confused with other laryngeal conditions [5] . LPR was detected in healthy people [33] , reaching up to 86% of asymptomatic GERD volunteers [52] .
5. Conclusion
RSI is a significant predictor for RFS, and both, RSI and RFS, are significantly proportionate to GERD, yet Silent LPR did exist among control patients.
References
References
DeVault, K.R. and Castell, D.O. (2005) Updated Guidelines for the Diagnosis and Treatment of Gastroesophageal Reflux Disease. American Journal of Gastroenterology, 100, 190-200. http://dx.doi.org/10.1111/j.1572-0241.2005.41217.x
Wong, W.-M. and Fass, R. (2004) Extraesophageal and Atypical Manifestations of GERD. Journal of Gastroenterology and Hepatology, 19, S33-S43. http://dx.doi.org/10.1111/j.1440-1746.2004.03589.x
Belafsky, P.C., Postma, G.N. and Koufman, J.A. (2001) Laryngopharyngeal Reflux Symptoms Improve before Changes in Physical Findings. Laryngoscope, 111, 979-981. http://dx.doi.org/10.1097/00005537-200106000-00009
Farrokhi, F. and Vaezi, M. (2007) Laryngeal Disorders in Patients. Minerva Gastroenterologica e Dietologica, 53, 181-187.
Ford, C.N. (2005) Evaluation and Management of Laryngopharyngeal Reflux. JAMA 294, 1534-1540. http://dx.doi.org/10.1001/jama.294.12.1534
Belafsky, P.C., Postma, G.N. and Koufman, J.A. (2002) Validity and Reliability of the Reflux Symptom Index (RSI). Journal of Voice, 16, 274-277. http://dx.doi.org/10.1016/S0892-1997(02)00097-8
American Society for Gastrointestinal Endoscopy (1999) The Role of Endoscopy in the Management of GERD: Guidelines for Clinical Application. Gastrointestinal Endoscopy, 49, 834-835. http://dx.doi.org/10.1016/S0016-5107(99)70313-5
Gorecki, P. (2001) Gastro-Esophageal Reflux Disease (GERD). Surgical Treatment: Evidence-Based and ProblemOriented. Zuckschwerdt, Munich.
Vakil, N., van Zanten, S.V., Kahrilas, P., Dent, J. and Jones, R. (2006) The Montreal Definition and Classification of Gastroesophageal Reflux Disease: A Global Evidence-Based Consensus. American Journal of Gastroenterology, 101, 1900-1920. http://dx.doi.org/10.1111/j.1572-0241.2006.00630.x
Dent, J., El-Serag, H.B., Wallander, M.-A. and Johansson, S. (2005) Epidemiology of Gastro-Oesophageal Reflux Disease: A Systematic Review. Gut, 54, 710-717. http://dx.doi.org/10.1136/gut.2004.051821
Sandler, R.S., Everhart, J.E., Donowitz, M., Adams, E., Cronin, K., Goodman, C., et al. (2002) The Burden of Selected Digestive Diseases in the United States. Gastroenterology 122, 1500-1511. http://dx.doi.org/10.1053/gast.2002.32978
Hershcovici T. and Fass, R. (2011) Pharmacological Management of GERD: Where Does It Stand Now? Trends in Pharmacological Sciences, 32, 258-264. http://dx.doi.org/10.1016/j.tips.2011.02.007
El-Serag, H., Hill, C. and Jones, R. (2009) Systematic Review: The Epidemiology of Gastro-Oesophageal Reflux Disease in Primary Care, Using the UK General Practice Research Database. Alimentary Pharmacology & Therapeutics 29, 470-480. http://dx.doi.org/10.1111/j.1365-2036.2008.03901.x
Lee, J., Anggiansah, A., Anggiansah, R., Young, A., Wong, T. and Fox, M. (2007) Effects of Age on the Gastroesophageal Junction, Esophageal Motility, and Reflux Disease. Clinical Gastroenterology and Hepatology 5, 1392-1398. http://dx.doi.org/10.1016/j.cgh.2007.08.011
Johnson, D.A. and Fennerty, M.B. (2004) Heartburn Severity Underestimates Erosive Esophagitis Severity in Elderly Patients with Gastroesophageal Reflux Disease. Gastroenterology, 126, 660-664. http://dx.doi.org/10.1053/j.gastro.2003.12.001
Lien, H.C., Wang, C.C., Hsu, J.Y., Sung, F.C., Cheng, K.F., Liang, W.M., et al. (2011) Classical Reflux Symptoms, Hiatus Hernia and Overweight Independently Predict Pharyngeal Acid Exposure in Patients with Suspected Reflux Laryngitis. Alimentary Pharmacology & Therapeutics 33, 89-98. http://dx.doi.org/10.1111/j.1365-2036.2010.04502.x
Eusebi, L.H., Fuccio, L. and Bazzoli F. (2012) The Role of Obesity in Gastroesophageal Reflux Disease and Barrett’s Esophagus. Digestive Diseases, 30, 154-157. http://dx.doi.org/10.1159/000336668
Moayyedi, P. (2008) Barrett’s Esophagus and Obesity: The Missing Part of the Puzzle. American Journal of Gastroenterology, 103, 301-303. http://dx.doi.org/10.1111/j.1572-0241.2007.01618.x
Nocon, M., Labenz, J., Jaspersen, D., Meyer-Sabellek, W., Stolte, M., Lind, T., et al. (2007) Association of Body Mass Index with Heartburn, Regurgitation and Esophagitis: Results of the Progression of Gastroesophageal Reflux Disease study. Journal of Gastroenterology and Hepatology 22, 1728-1731. http://dx.doi.org/10.1111/j.1440-1746.2006.04549.x
Hampel, H., Abraham, N.S. and El-Serag, H.B. (2005) Meta-Analysis: Obesity and the Risk for Gastroesophageal Reflux Disease and Its Complications. Annals of Internal Medicine 143, 199-211. http://dx.doi.org/10.7326/0003-4819-143-3-200508020-00006
Noordzij, J.P., Khidr, A., Desper, E., Meek, R.B., Reibel J.F. and Levine, P.A. (2002) Correlation of pH Probe-Measured Laryngopharyngeal Reflux with Symptoms and Signs of Reflux Laryngitis. Laryngoscope, 112, 2192-2195. http://dx.doi.org/10.1097/00005537-200212000-00013
Koufman, J.A. (1991) The Otolaryngologic Manifestations of Gastroesophageal Reflux Disease (GERD): A Clinical Investigation of 225 Patients Using Ambulatory 24-Hour pH Monitoring and an Experimental Investigation of the Role of Acid and Pepsin in the Development of Laryngeal. Laryngoscope 101, 1-78.
Merati, A.L., Lim, H.J., Ulualp, S.O. and Toohill, R.J. (2005) Meta-Analysis of Upper Probe Measurements in Normal Subjects and Patients with Laryngopharyngeal Reflux. Annals of Otology, Rhinology, and Laryngology 114, 177-182.
Patigaroo, S.A., Hashmi S.F., Hasan, S.A., Ajmal, M.R. and Mehfooz, N. (2011) Clinical Manifestations and Role of Proton Pump Inhibitors in the Management of Laryngopharyngeal Reflux. Indian Journal of Otolaryngology and Head & Neck Surgery, 63, 182-189. http://dx.doi.org/10.1007/s12070-011-0253-3
Youssef, T.F. and Ahmed, M.R. (2010) Treatment of Clinically Diagnosed Laryngopharyngeal Reflux Disease. Archives of Otolaryngology—Head and Neck Surgery 136, 1089-1092. http://dx.doi.org/10.1001/archoto.2010.165
Ahmad, I. and Batch, A. (2004) Acid Reflux Management: ENT Perspective. Journal of Laryngology & Otology 118, 25-30. http://dx.doi.org/10.1258/002221504322731583
Qadeer M.A., Swoger, J., Milstein, C., Hicks, D.M., Ponsky, J., Richter, J.E., et al. (2005) Correlation between Symptoms and Laryngeal Signs in Laryngopharyngeal Reflux. Laryngoscope, 115, 1947-1952. http://dx.doi.org/10.1097/01.mlg.0000176547.90094.ac
Irwin, R.S., French, C.L., Curley, F.J., Zawacki, J.K. and Bennett F.M. (1993) Chronic Cough Due to Gastroesophageal Reflux. Clinical, Diagnostic, and Pathogenetic Aspects. Chest, 104, 1511-1517. http://dx.doi.org/10.1378/chest.104.5.1511
Moore, J. and Vaezi, M. (2010) Extraesophageal Manifestations of Gastroesophageal Reflux Disease: Chronic Cough. Current Opinion in Gastroenterology 26, 389-394. http://dx.doi.org/10.1097/MOG.0b013e32833adc8d
Aviv, J.E., Liu, H., Parides, M., Kaplan, S.T. and Close, L.G. (2000) Laryngopharyngeal Sensory Deficits in Patients with Laryngopharyngeal Reflux and Dysphagia. Annals of Otology, Rhinology, and Laryngology, 109, 1000-1006.
Said, M.S. (2010) Manifestation and Response of Laryngopharygeal Reflux to Treatment in Kurdistan-IRAQ. Al-Kindy College Medical Journal 6, 1-8.
Hopkins, C., Yousaf, U. and Pedersen, M. (2006) Acid Reflux Treatment for Hoarseness. Cochrane Database of Systematic Reviews, 1, CD005054.
Ozturk, O., Oz, F., Karakullukcu, B., Oghan, F., Guclu, E. and Ada, M. (2006) Hoarseness and Laryngopharyngeal Reflux: A Cause and Effect Relationship or Coincidence? European Archives of Oto-Rhino-Laryngology, 263, 935-939. http://dx.doi.org/10.1007/s00405-006-0097-8
Wiener, G.J., Koufman J.A., Wu, W.C., Cooper, J.B., Richter, J.E. and Castell, D.O. (1989) Chronic Hoarseness Secondary to Gastroesophageal Reflux Disease: Documentation with 24-h Ambulatory pH Monitoring. American Journal of Gastroenterology, 84, 1503-1508.
Johansson, K.E., Ask, P., Boeryd, B., Fransson, S.G. and Tibbling, L. (1986) Oesophagitis, Signs of Reflux, and Gastric Acid Secretion in Patients with Symptoms of Gastro-Oesophageal Reflux Disease. Scandinavian Journal of Gastroenterology, 21, 837-847. http://dx.doi.org/10.3109/00365528609011128
Younes, Z. and Johnson, A. (1999) Diagnostic Evaluation in Gastroesophageal Reflux Disease. Gastroenterology Clinics of North America, 28, 809-830. http://dx.doi.org/10.1016/S0889-8553(05)70091-1
Meneghetti, A.T., Tedesco, P., Damani, T. and Patti, M.G. (2005) Esophageal Mucosal Damage May Promote Dysmotility and Worsen Esophageal Acid Exposure. Journal of Gastrointestinal Surgery, 9, 1313-1317.
Sontag, S.J. (2007) Rolling Review: Gastro-Oesophageal Reflux Disease. Alimentary Pharmacology & Therapeutics 7, 293-312.
Mearin, F., Ponce, J., Ponce, M., Balboa, A., González, M.A. and Zapardiel, J. (2012) Clinical Usefulness of Adherence to Gastro-Esophageal Reflux Disease Guideline by Spanish Gastroenterologists. World Journal of Gastroenterology, 18, 4885-4891.
Gordon, C., Kang, J.Y., Neild, P.J. and Maxwell, J.D. (2004) The Role of the Hiatus Hernia in Gastro-Oesophageal Reflux Disease. Alimentary Pharmacology & Therapeutics, 20 719-732.
Fein, M., Ritter, M.P., DeMeester, T.R., Oberg, S., Peters, J.H., Hagen, J.A. and Bremner, C.G. (2013) Role of the Lower Esophageal Sphincter and Hiatal Hernia in the Pathogenesis of Gastroesophageal Reflux Disease. Journal of Gastrointestinal Surgery, 3, 405-410. http://dx.doi.org/10.1016/S1091-255X(99)80057-2
Chandrasoma, P., Wickramasinghe, K., Ma, Y. and DeMeester T. (2007) Is Intestinal Metaplasia a Necessary Precursor Lesion for Adenocarcinomas of the Distal Esophagus, Gastroesophageal Junction and Gastric Cardia? Disease of Esophagus, 20, 36-41.
Watson, A. (2000) Barrett’s Oesophagus—50 Years on. British Journal of Surgery, 87 529-531.
Shaheen, N.J. and Richter, J.E. (2009) Barrett’s Oesophagus. Lancet, 373 850-861.
Koop, H. (2004) Gastroesophageal Reflux Disease and Barrett’s Esophagus. Endoscopy, 36 103-109.
Ylitalo, R. and Ramel, S. (2002) Extraesophageal Reflux in Patients with Contact Granuloma: A Prospective Controlled Study. Annals of Otology, Rhinology, and Laryngology, 111, 441-446.
Maronian, N.C., Azadeh, H., Waugh, P. and Hillel, A. (2001) Association of Laryngopharyngeal Reflux Disease and Subglottic Stenosis. Annals of Otology, Rhinology, and Laryngology, 110 606-612.
Ohman, L., Olofsson, J., Tibbling, L. and Ericsson, G. (1983) Esophageal Dysfunction in Patients with Contact Ulcer of the Larynx. Annals of Otology, Rhinology, and Laryngology, 92 228-230.
Hickson, C., Simpson, C.B. and Falcon, R. (2001) Laryngeal Pseudosulcus as a Predictor of Laryngopharyngeal Reflux. Laryngoscope, 111 1742-1745.
Khan, A.M., Hashmi, S.R., Elahi, F., Tariq, M. and Ingrams, D.R. (2006) Laryngopharyngeal Reflux: A Literature Review. Surgeon, 4, 221-225.
Branski, R.C., Bhattacharyya, N. and Shapiro, J. (2002) The Reliability of the Assessment of Endoscopic Laryngeal Findings Associated with Laryngopharyngeal Reflux Disease. Laryngoscope, 112 1019-1024.
Hicks, D.M., Ours, T.M., Abelson, T.I., Vaezi M.F. and Richter, J.E. (2002) The Prevalence of Hypopharynx Findings Associated with Gastroesophageal Reflux in Normal Volunteers. Journal of Voice, 16, 564-579.


