Open Journal of Pediatrics
Vol.3 No.4(2013), Article ID:40105,6 pages DOI:10.4236/ojped.2013.34056
Intussusception in Japanese infants: Analysis of health insurance claims database
![]()
1Department of Pediatrics, Toyama City Hospital, Toyama, Japan
2Healthoutcomes Department, GlaxoSmithKline K.K., Tokyo, Japan
3Biostatistics Department, GlaxoSmithKline Pharmaceuticals, Bangalore, India
4Health Economics Department, GlaxoSmithKline Vaccines, Wavre, Belgium
Email: *keiko.2.sato@gsk.com
Copyright © 2013 Masayoshi Miura et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 23 September 2013; revised 20 October 2013; accepted 28 October 2013
Keywords: Hospitalized; Incidence; Intussusception; Japan; Rotavirus
ABSTRACT
In order to better understand the possible impact of second-generation rotavirus vaccines on the incidence of intussusception (IS), robust knowledge of the baseline childhood epidemiology of IS from various sources is essential. This study estimated the overall and agespecific baseline incidence of IS among young Japanese children. Data on 57 IS cases from 42,438 screened children aged less than 12 months, born between January 2005 and April 2011 and covered by the health insurance claims database were retrospectively extracted (NCT01479491). IS cases were identified using the International Classification of Diseases, 10th revision (K56.1), with relevant examination and procedural codes. The extracted data were used to estimate the incidence of IS. Among all IS cases extracted, 51 (94.4%) were confirmed IS, of which 49/51 (96.1%) were hospitalized, 2/51 (3.9%) visited outpatient wards; 26/51 (51.0%) were males. The overall incidence of confirmed IS and IS hospitalizations among children aged less than 12 months was 143.5 (95% CI: 106.8 - 188.6) and 137.8 (95% CI: 102.0 - 182.2) per 100,000 children-years, respectively. Three (5.9%) IS cases were identified in children aged below 3 months. IS cases peaked between 6 - 11 months of age (40/51 [78.4%]) with the highest incidence (321.5 [95% CI: 138.8 - 633.4] per 100,000 children-years) observed at 10 months of age. The overall recurrence rate of IS was 3.7% (95% CI: 0.5 - 12.7). The baseline incidence of IS in Japanese children aged less than 12 months was higher than that observed in other countries prior to the introduction of second-generation rotavirus vaccines.
1. INTRODUCTION
Intussusception (IS) is the most common cause of intestinal obstruction among infants and young children [1,2]. The most common symptoms include vomiting, abdominal pain, abdominal mass and passage of bloody stool [2]. IS may lead to death if left untreated [3], therefore early diagnosis and disease management are essential. In Japan, the management guidelines mainly focus on enema reduction in mild and moderate cases and operative reduction/resection in more severe cases [4].
Rotavirus is the leading cause of severe gastroenteritis causing considerable morbidity and mortality worldwide [5]; however, it can be substantially prevented with available rotavirus vaccination [6]. Following a temporal association between first generation rotavirus vaccines and IS [7], all second-generation rotavirus vaccines required additional safety assessment [7]. Results to date suggest that the benefits of the currently available rotavirus vaccines: Rotarix™ (GlaxoSmithKline, Belgium) and Rotateq® (Merck & Co., NJ, USA) outweigh the risk of IS [7]. Therefore it is important to generate robust baseline data on the incidence of IS before the introduction of second-generation rotavirus vaccines into Japan.
So far, several studies on the incidence of IS have been conducted using hospital databases in Japan. One study reported the incidence of IS to be 185.1 per 100,000 children-years between 1978 and 2002 [2]. Other more recent studies have estimated the incidence to be between 179.0 - 191.0 during 2007-2008 [8] and 158.0 per 100,000 person-years between 2001 and 2010 [9].
Despite the previous assessment of the epidemiology and incidence of IS in Japanese children [2,8,9], further research using various data sources is warranted. In addition, although the majority of IS cases are treated at hospitals in Japan, it is nevertheless important to consider those cases treated on an outpatient basis.
This study was designed to estimate the overall and age-specific baseline incidence of IS among Japanese children aged less than 12 months, prior to the introduction of rotavirus vaccines in Japan.
2. SUBJECTS AND METHODS
2.1. Study Design and Study Population
This observational, database surveillance study retrospectively collected IS data from children born between January 2005 and April 2011, prior to the implementation of rotavirus vaccines in Japan (NCT01479491).
Data were collected from the Japan Medical Data Center Company Limited Medical Data Bank (JMDCMDB). This database is maintained by the Japan Medical Data Center Company Limited (JMDC, Tokyo, Japan) and consists of medical claim data from nearly 1,000,000 Japanese individuals (approximately 1% of the entire population) included in health insurance systems. Data from hospital receipts were collected from all the regions and included encrypted personal information; diagnostic codes according to International Classification of Disease and Related Health Outcomes 10th Revision (ICD- 10) codes; examination codes; procedural codes and hospitalization details [10].
Children born during this surveillance period, who were aged less than 12 months, diagnosed with IS and covered by the JMDC-MDB were included in the study. All children included in the database were retrospectively followed up until an event of IS occurred or until the end of the surveillance period. Aggregated data of age and gender and the individual-level data for IS cases were extracted. Children with a discrepancy between birth month and month of enrolment to the insurance society were excluded from the study analyses.
IS cases were identified using ICD-10 diagnostic code-K56.1, its uncertain disease flag, examination codes (Ultrasound examination [D215.2], radiological examination [E001], computer tomography (CT) scan [E002], magnetic resonance imaging (MRI) [E202] and radio-logical examination with liquid contrast enema [E003.6]) and procedural codes (non-invasive repositioning [K715.1], invasive re-positioning [K715.2], laparoscopically-assisted surgery [K714.2] and bowel resection [K716]). In addition, the presence of a characteristic lesion, shown by diagnostic imaging examinations, is a mandatory criterion for establishing the diagnosis of IS [11]. The uncertain disease flag is a unique variable in the reimbursement system in Japan, whereby when diagnosis is unclear, physicians flag the disease as “uncertain”, and later specify the disease after examination or treatment. The age (month) of IS onset was calculated from date of first diagnosis. All receipt data from birth to onset of IS were reviewed and the underlying diseases ascertained. All IS cases were grouped as confirmed, possible and suspected based on the case definitions given in Table 1.
2.2. Statistical Analyses
The per-protocol cohort included all eligible children with identified IS (from ICD-10 diagnostic, examination and procedural codes). All stat analyses were performed using Statistical Analysis System (SAS®) version 9.2 and all the graphs were generated using Microsoft excel. Categorical data like the gender, summary and the seasonal distribution of IS cases and the diagnostic procedures and the examinations are presented as proportions with one decimal. Incidence rate of intussusception cases by gender, age groups and overall incidence rates are expressed in terms of 100,000 children-years with 95% Exact Poisson confidence interval (CI). Since physicians sometimes kept the disease flag as “uncertain” even after diagnosis, the incidence of confirmed plus possible cases was also calculated.
3. RESULTS
3.1. Demographic Characteristics
From 42,438 screened children, data from 57 children with ICD-10 K56.1 codes were extracted from the database. Of these, 54 children were included in the study (51 [94.4%] as confirmed IS, one [1.9%] possible and two [3.7%] suspected IS [Figure 1]). The mean age (standard deviation) of these children was 7.64 (±2.62); 27 children (50%) were male.
Of the children with confirmed IS, 49 (96.1%) were hospitalized and two (3.9%) visited outpatient wards. The mean age (standard deviation) of the hospitalized children was 7.91 (±2.52) months, of whom 24 (49.0%) were male. Both outpatients were male and had a mean age of 4.32 (±2.91) months.
The youngest child with IS was one month old. Three (5.9%) children under the age of three months were hospitalized for confirmed IS. The age at which the highest number of children (17.6% [9/51]) had confirmed that IS cases were six months.
3.2. Incidence of IS
Among children aged less than 12 months, the incidences of confirmed IS and confirmed IS hospitalizations were
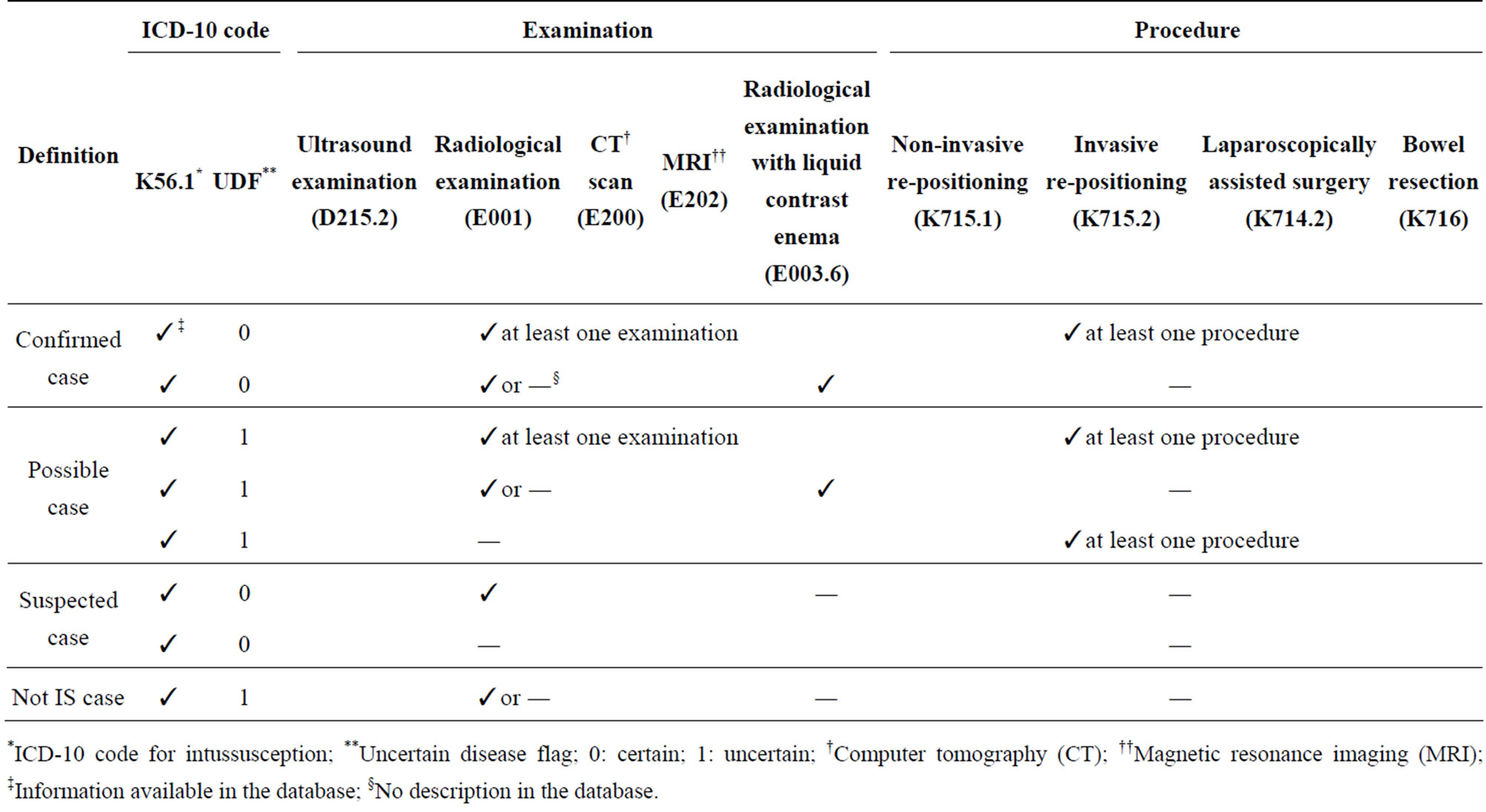
Table 1. Case definitions of IS cases.
*ICD-10 code for intussusception; **Uncertain disease flag; 0: certain; 1: uncertain; †Computer tomography (CT); ††Magnetic resonance imaging (MRI); ‡Information available in the database; §No description in the database.
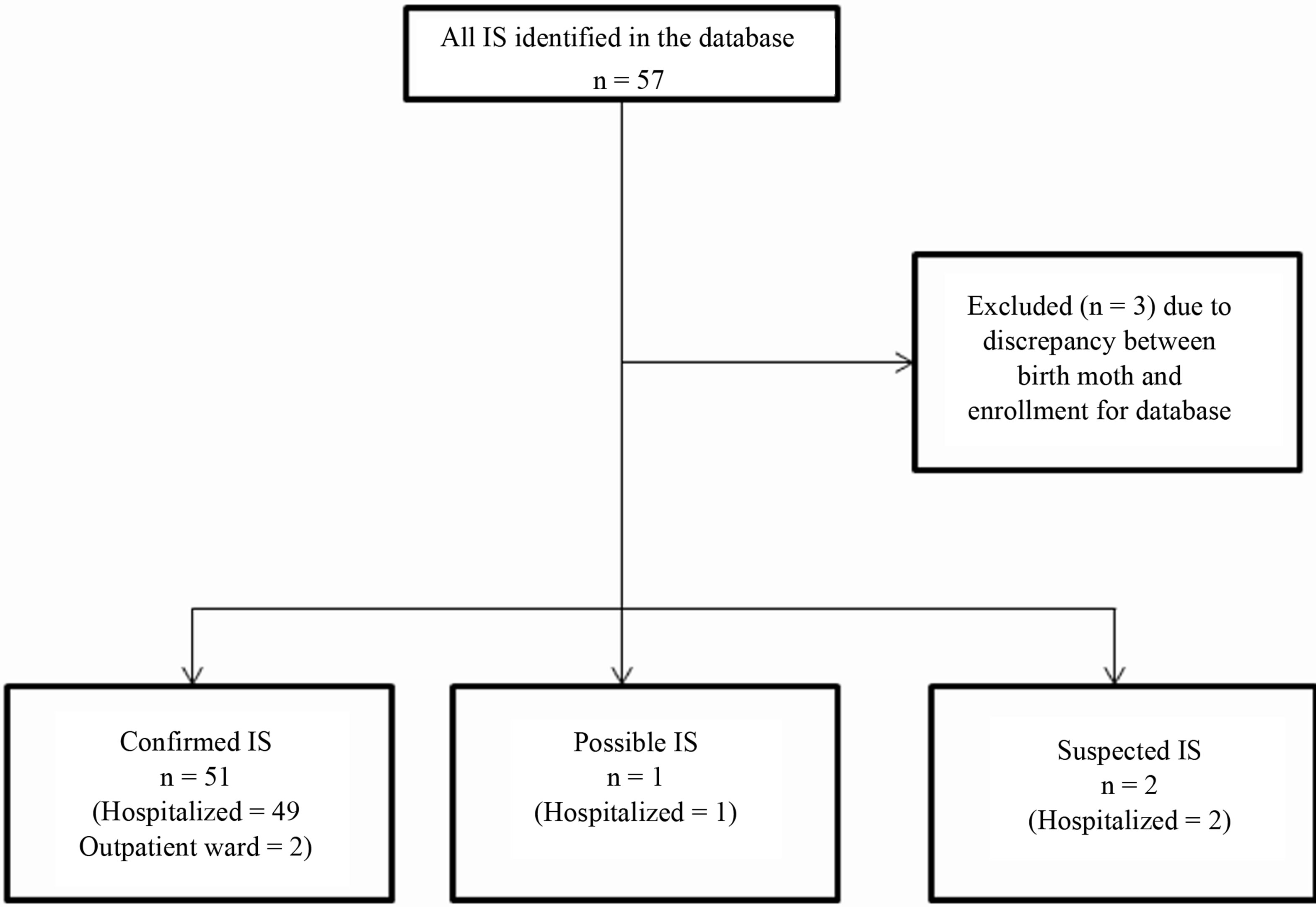
Figure 1. Study flow diagram.
143.5 (95% CI: 106.8 - 188.6) and 137.8 (95% CI: 102.0 - 182.2) per 100,000 children-years, respectively. The incidence of confirmed plus possible IS was 146.3 (95% CI: 109.2 - 191.8) per 100,000 children-years (Table 2).
The ageand gender-specific incidence of confirmed IS hospitalizations are shown in Table 3. Peak in the incidence of IS cases was observed in children between the age group 6 and 11 years (40/51 [78.4%]). The highest incidence of IS (321.5 [95% CI: 138.8 - 633.4] per 100,000 children-years) was observed in children aged 10 months (Table 3).
Two children suffered recurrent IS; an overall recur-
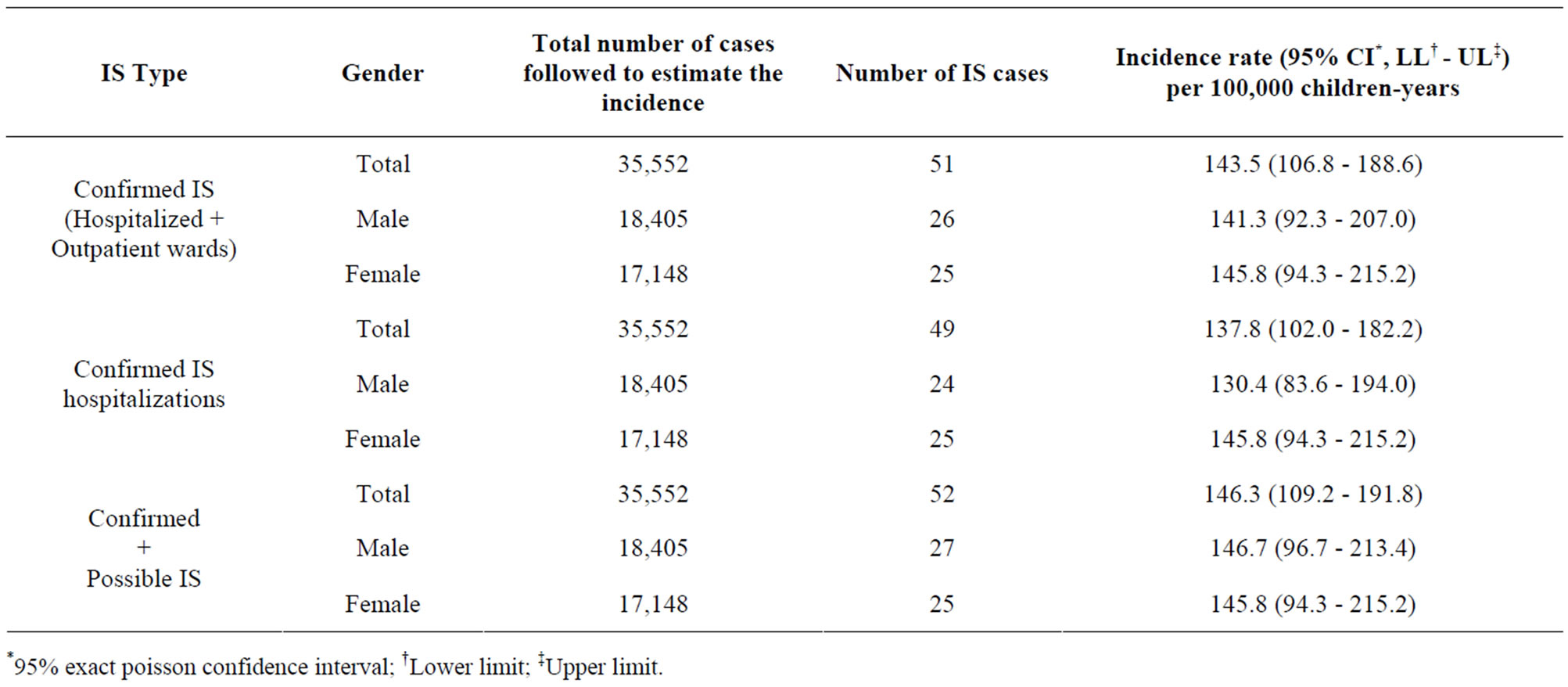
Table 2. Incidence of IS among children aged less than 12 months (per-protocol cohort).
*95% exact poisson confidence interval; †Lower limit; ‡Upper limit.
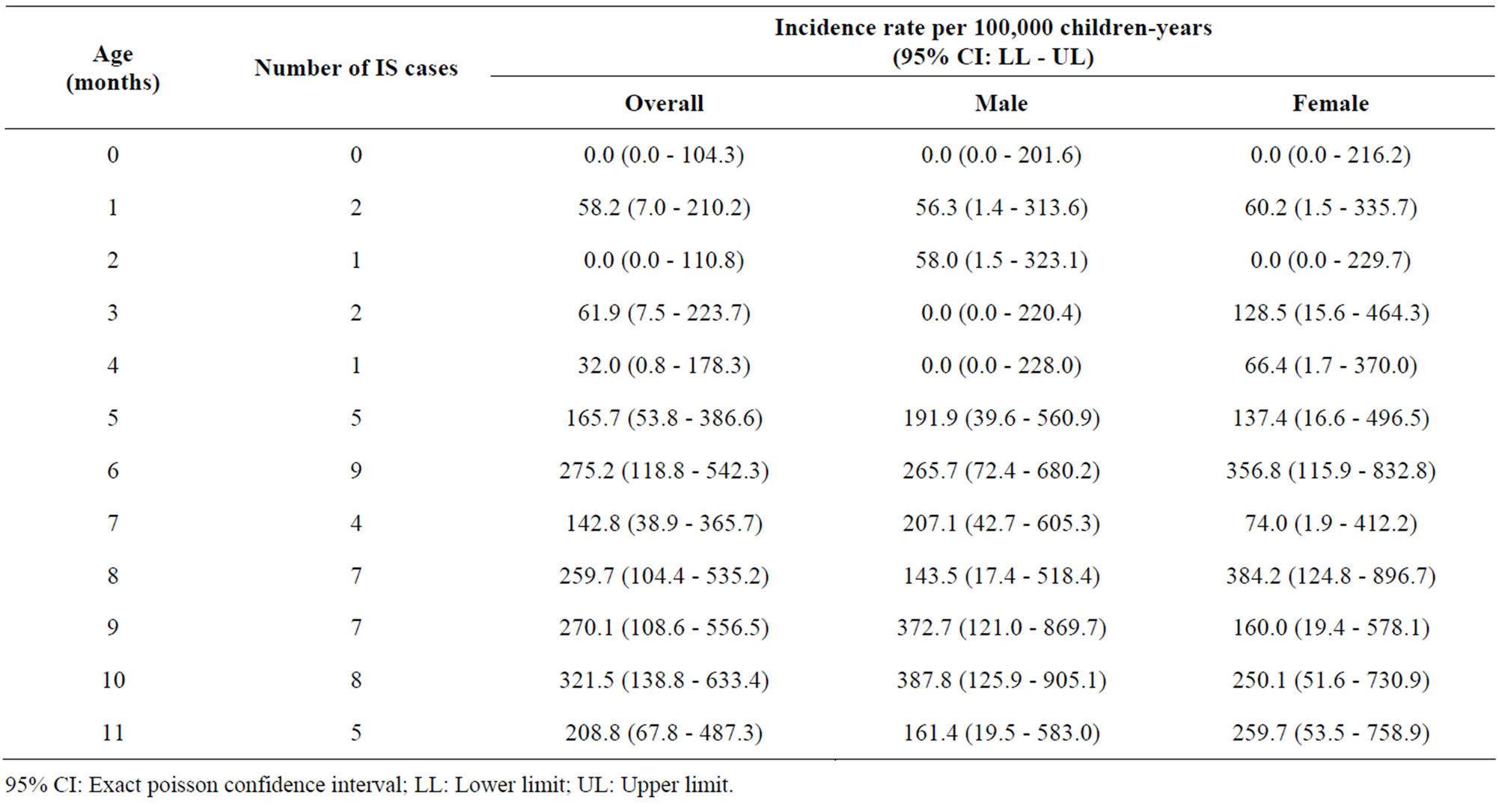
Table 3. Incidence of confirmed IS hospitalization cases by age and gender.
95% CI: Exact poisson confidence interval; LL: Lower limit; UL: Upper limit.
rence rate of 3.7% (95% CI: 0.50 - 12.7).
3.3. Management
Among the 49 confirmed IS cases which were treated in hospitals, one child (2.0%) underwent invasive repositioning. Non-invasive repositioning was performed in 46 children (93.9%), among whom bowel resection and laparoscopically-assisted surgery were performed in three children (6.5%) and one child (2.2%), respectively. Both children who were treated in the out-patient setting underwent non-invasive repositioning.
3.4. Underlying Diseases
Among the hospitalized children, Meckel’s diverticulum was observed in one case, but no other underlying disease was specified.
4. DISCUSSION
The present study provides overall and age-specific baseline IS incidence data prior to the introduction of rotavirus vaccines in Japan. We observed an incidence of confirmed IS among Japanese children aged less than 12 months 143.5 per 100,000 children-years. Assessment of confirmed IS incidence according to age during first year of life showed that the highest incidence occurred at six months of age. The majority of confirmed IS cases (96.1%) were hospitalized and non-invasive repositioning was the most commonly recorded diagnostic procedure (in 93.9%).
So far three hospital-based, retrospective studies have assessed the incidence of IS in Japan [2,8,9] and have shown similar results to those in our study. One study retrieved hospital-based data on IS from the last 25 years, showing the incidence of IS hospitalizations among children aged less than 12 months to be 185.1 per 100,000 children-years [2]. Another study which utilized the Diagnosis Procedure Combination inpatient database, reported similar findings and incidence rates of 179.0 (95% CI: 165.0 - 203.0) per 100,000 infants in 2007 and 191.0 (95% CI: 165.0 - 216.0) per 100,000 infants in 2008 [8]. The most recent study, which reviewed in-patient medical charts calculated an incidence of 158.0 (95% CI: 131.0 - 188.0) per 100,000 person-years during 2001- 2010 [9].
Although the exact reason for the lower IS incidence rate observed in our present study, as compared to previous studies in Japan is unknown, possible reasons include differences in source data collection, case identification and study design. Another reason could be a true decrease in the incidence of IS itself over time. Indeed, in an epidemiological study undertaken in Denmark a reduction in IS-associated hospitalizations was observed over time [12], despite the Danish physicians reporting no changes in hospitalization practices, diagnostic criteria, or the process of nationwide hospital registration during the entire study period. The decrease in IS incidence in Denmark was therefore considered as a true decrease in the occurrence of IS over time [12]. Furthermore, improvements in environmental hygiene and a decrease in intestinal viral infection in developed countries might be contributing to a decrease in the number of IS cases [3].
The incidence of IS in Japanese infants observed in the present and previous studies [2,8,9] remains consistently higher than that observed in other regions of Asia including Singapore (average incidence of 60 per 100,000 during 1997-2004) [13]; Taiwan (77.0 per 100,000 person-years during 1998-2007) [14] and Hong Kong (108.0 per 100,000 during 1997-2003) [15] and the world, including the USA (41.6 per 100,000 infants during 1997-2006) [16] and Germany (60.4 per 100,000 childyears during January 2006-December 2007) [17]. Since Japanese infants receive high quality medical care as part of the national health program, the number of IS cases are closely monitored. Such a program is more likely to identify all the IS cases. This may be one of the factors for the increased number of IS cases reported in Japan, however, the exact reason remains unclear.
Our observation of a peak in incidence at 6 - 11 months of age is consistent with the previously conducted studies in Japan [2,8] and Singapore [13]. Younger ages for the IS peak have, however, been recorded from a hospital-based study in the USA at 5 - 7 months of age [18] and a review of published studies conducted in Europe at 3 - 9 months of age [19].
The causes of recurrent IS are largely unknown, but could partly be due to anatomical causes including polyps or Meckel’s diverticulum [20]. Studies are scarce, but a recent Vietnamese trial reported that the incidence of recurrent IS in infants aged under 24 months was 14.0% during the six months follow-up period [20]. In our present study we observed a recurrence rate of 3.7% in Japanese children aged less than 12 months.
The strengths of the present study give credibility to the findings and substantiate the observed results. Firstly, the health insurance claims database also employed claim data from clinics and all hospital wards, including pediatric wards, where children with IS were diagnosed and treated. This enabled collection of IS data from all reported cases and also on the underlying diseases/conditions. Furthermore, the ability to follow up children from birth until the occurrence of IS allowed robust estimation of IS incidence and enabled analysis of other disease profiles among IS cases. Secondly, this was a relatively large study in which over 42,000 children were screened; representing nearly 1% of the entire population from various regions throughout Japan. Our results are therefore, more likely to be a true representation of the exact scenario of IS cases. Additionally as data on the incidence of IS were screened using ICD-10 diagnostic and procedural codes, case ascertainment was more robust and made the data on IS incidence more epidemicologically reliable. Lastly, annual assessment of IS among children on a monthly-basis, enabled the identification of the age group in which the risk of developing IS was the highest.
The possible limitations of this study may originate from the inherent limitations of the database and the use of ICD-10 codes which may suffer from lack of accuracy of disease diagnosis and lack of data completeness. This may have ultimately resulted in overestimation or underestimation of incidence of IS.
5. CONCLUSION
Analysis of a health insurance claims database indicated that before the introduction of rotavirus vaccines, the incidence of IS among Japanese children under 12 months of age was higher than that observed in other countries. IS cases were confirmed in infants younger than three months of age, the age at which the first dose of rotavirus vaccination is recommended, and the highest incidence was observed in children aged 10 months.
6. ACKNOWLEDGEMENTS
The authors acknowledge Harshith Bhat (employed by the GlaxoSmithKline group of companies) for manuscript writing and Dr. Roeland Van Kerckhoven (Consultant for Keyrus Biopharma) for manuscript coordination.
REFERENCES
- Peter, G. and Myers, M.G. (2002) Intussusception, rotavirus, and oral vaccines: Summary of a workshop. Pediatrics, 110, e67. http://dx.doi.org/10.1542/peds.110.6.e67
- Nakagomi, T., Takahashi, Y., Arisawa, K. and Nakagomi, O. (2006) A high incidence of intussusception in Japan as studied in a sentinel hospital over a 25-year period (1978- 2002). Epidemiology and Infection, 134, 57-61. http://dx.doi.org/10.1017/S0950268805004644
- World Health Organisation (2002) Acute intussusception in infants and children. Incidence, clinical presentation and management: A global perspective. In: Initiative for Vaccine Research Department of Vaccines and Biologicals, Vol. WHO/V&B/02.19, Geneva.
- Ito, Y., Kusakawa, I., Murata, Y., Ukiyama, E., Kawase, H., Kamagata, S., et al. (2012) Japanese guidelines for the management of intussusception in children, 2011. Pediatrics International, 54, 948-958. http://dx.doi.org/10.1111/j.1442-200X.2012.03622_1.x
- Parashar, U.D., Gibson, C.J., Bresee, J.S. and Glass, R.I. (2006) Rotavirus and severe childhood diarrhea. Emerging Infectious Diseases, 12, 304-306. http://dx.doi.org/10.3201/eid1202.050006
- Patel, M.M., Glass, R., Desai, R., Tate, J.E. and Parashar, U.D. (2012) Fulfilling the promise of rotavirus vaccines: How far have we come since licensure? The Lancet Infectious Diseases, 12, 561-570. http://dx.doi.org/10.1016/S1473-3099(12)70029-4
- Patel, M.M., Lopez-Collada, V.R., Bulhoes, M.M., De Oliveira, L.H., Bautista Marquez, A., et al. (2011) Intussusception risk and health benefits of rotavirus vaccination in Mexico and Brazil. The New England Journal of Medicine, 364, 2283-2292. http://dx.doi.org/10.1056/NEJMoa1012952
- Takeuchi, M., Osamura, T., Yasunaga, H., Horiguchi, H., Hashimoto, H. and Matsuda, S. (2012) Intussusception among Japanese children: An epidemiologic study using an administrative database. BMC Pediatrics, 12, 36. http://dx.doi.org/10.1186/1471-2431-12-36
- Noguchi, A., Nakagomi, T., Kimura, S., Takahashi, Y., Matsuno, K., Koizumi, H., et al. (2012) Incidence of intussusception as studied from a hospital-based retrospective survey over a 10-year period (2001-2010) in Akita prefecture, Japan. Japanese Journal of Infectious Disease, 65, 301-305. http://dx.doi.org/10.7883/yoken.65.301
- Kimura, S., Sato, T., Ikeda, S., Noda, M. and Nakayama, T. (2010) Development of a database of health insurance claims: Standardization of disease classifications and Anonymous record linkage. Journal of Epidemiology, 20, 413-419. http://dx.doi.org/10.2188/jea.JE20090066
- Japanese Society of Emergency Pediatrics (2012) Evidence-based guidelines for the management of intussusception in children. Herusu-Shuppan, Tokyo.
- Fischer, T.K., Bihrmann, K., Perch, M., Koch, A., Wohlfahrt, J., Kare, M., et al. (2004) Intussusception in early childhood: A cohort study of 1.7 million children. Pediatrics, 114, 782-785. http://dx.doi.org/10.1542/peds.2004-0390
- Boudville, I.C., Phua, K.B., Quak, S.H., Lee, B.W., Han, H.H., Verstraeten, T., et al. (2006) The epidemiology of paediatric intussusception in Singapore: 1997 to 2004. Annals Academy of Medicine, 35, 674-679.
- Chen, S.C., Wang, J.D., Hsu, H.Y., Leong, M.M., Tok, T.S. and Chin, Y.Y. (2010) Epidemiology of childhood intussusception and determinants of recurrence and operation: Analysis of national health insurance data between 1998 and 2007 in Taiwan. Pediatrics and Neonatology, 51, 285-291. http://dx.doi.org/10.1016/S1875-9572(10)60055-1
- Chiu, S.S., Ip, K.S., Lau, D., Lau, Y.L., Ng, C.H., Ng, D.K., et al. (2007) Intussusception trends in Hong Kong children. Hong Kong Medical Journal, 13, 279-283.
- Zickafoose, J.S., Benneyworth, B.D., Riebschleger, M.P., Espinosa, C.M. and Davis, M.M. (2012) Hospitalizations for intussusception before and after the reintroduction of rotavirus vaccine in the United States. Archives of Pediatrics and Adolescent Medicine, 166, 350-355. http://dx.doi.org/10.1001/archpediatrics.2011.1501
- Jenke, A.C., Klaassen-Mielke, R., Zilbauer, M., Heininger, U., Trampisch, H. and Wirth, S. (2011) Intussusception: Incidence and treatment-insights from the nationwide German surveillance. Journal of Pediatric Gastroenterology and Nutrition, 52, 446-451. http://dx.doi.org/10.1097/MPG.0b013e31820e1bec
- Parashar, U.D., Holman, R.C., Cummings, K.C., Staggs, N.W., Curns, A.T., Zimmerman, C.M., et al. (2000) Trends in intussusception-associated hospitalizations and deaths among US infants. Pediatrics, 106, 1413-1421. http://dx.doi.org/10.1542/peds.106.6.1413
- Huppertz, H.I., Soriano-Gabarro, M., Grimprel, E., Franco, E., Mezner, Z., Desselberger, U., et al. (2006) Intussusception among young children in Europe. The Pediatrics Infectious Disease Journal, 25, S22-S29. http://dx.doi.org/10.1097/01.inf.0000197713.32880.46
- Justice, F.A., Nguyen, L.T., Tran, S.N., Kirkwood, C.D., Thi, N.T., Carlin, J.B., et al. (2011) Recurrent intussusception in infants. Journal of Pediatrics and Child Health, 47, 802-805. http://dx.doi.org/10.1111/j.1440-1754.2011.02029.x
NOTES
*Corresponding author.

