 Open Journal of Gastroenterology, 2013, 3, 328-336 OJGas http://dx.doi.org/10.4236/ojgas.2013.38058 Published Online December 2013 (http://www.scirp.org/journal/ojgas/) A randomized controlled trial of lifestyle self-monitoring for irritable bowel syndrome in female nursing school students Yukiko Okami1,2*, Gyozen Nin2, Kiyomi Harada2,3, Masayo Iwasa4, Kaori Kitaoka2,5, Ayako Saruwatari4, Wataru Aoi4, Sayori Wada4, Misaka Kimura6, Hiroaki Asano3, Yusuke Okuyama7, Susumu Takakuwa8, Motoyori Kanazawa9, Shin Fukudo9, Tomiko Tsuji1, Akane Higashi4 1Department of Health and Nutrition, Nagoya Bunri University, Inazawa, Japan 2Ex-Graduate School of Life and Environmental Sciences, Kyoto Prefectural University, Kyoto, Japan 3School of Nursing, Kyoto Prefectural University of Medicine, Kyoto, Japan 4Graduate School of Life and Environmental Sciences, Kyoto Prefectural University, Kyoto, Japan 5Department of Health and Nutrition, Kyoto Koka Women’s University, Kyoto, Japan 6Faculty of Bioenvi r o n m e n t al Science, Kyoto Gakuen University, Kameoka, Japan 7Department of Gas t r o e nterology, Japan Red C ro ss Kyoto Dai ichi Hospital, Kyoto, Japan 8Department of Education, Kyoto Women’s University, Kyoto, Japan 9Department of Beha v i o ral Medicine, Tohoku University Graduate School of Medicine, Sendai, Japan Email: *okami.yukiko@nagoya-bunri.ac.jp Received 1 November 2013; revised 5 December 2013; accepted 16 December 2013 Copyright © 2013 Yukiko Okami et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. In accor- dance of the Creative Commons Attribution License all Copyrights © 2013 are reserved for SCIRP and the owner of the intellectual property Yukiko Okami et al. All Copyright © 2013 are guarded by law and by SCIRP as a guardian. ABSTRACT Background: The aim of this study was to verify the efficacy of lifestyle self-monitoring for the improve- ment of the IBS and reveal what has been changed due to the intervention. Methods: A total of 111 nurs- ing school students were randomized into three groups, two intervention groups (a two-month intervention group, n = 34, and a four-month intervention group, n = 35) and a control group (n = 34). The intervention groups conducted lifestyle self-monitoring in con- junction with a 15-minutes group work for either two or four months. The primary outcome measure was Rome II criteria for IBS. Other outcome measures were the Hospital Anxiety and Depression Scale (HADS) and the Gastrointestinal Symptom Rating Scale (GSRS). They were assessed at the baseline and the end of both of the intervention periods. Analysis was conducted as intention-to-treat. Results: The pre- valence of IBS did not change significantly after the intervention in any of the groups. The HAD-A score, a subscale of the HADS score for anxiety, decreased 1.4 points in the two-month intervention group (p = 0.02) and 2.3 points in the four-month intervention group of (p = 0.01) after intervention. The average GSRS decreased 0.2 points in the control group (p = 0.05) and 0.3 points in the four-month intervention group (p < 0.01). Conclusions: Lifestyle self-moni- toring for two or four months did not reduce the pre- valence of the IBS significantly, but it did decrease anxiety and improved the QOL related to gastroin- testinal symptoms in female nursing school students. Keywords: Lifestyle; Self-Monitoring; Irritable Bowel Syndrome; Hospital Anxiety and Depression Scale; Gastrointestinal Symptom Rating Scale; Nursing School 1. INTRODUCTION Irritable bowel syndrome (IBS) is a functional gastroin- testinal disorder associated with abdominal pain, ab- dominal discomfort, and disordered defecation [1]. The number of people with IBS has increased recently, espe- cially in developed countries [2]. The prevalence and incidence of IBS are 10% - 15% and 1% - 2% per year in the general population, respectively [2]. IBS is one of the most common disorders in digestive medical care [3,4]. The mechanism of IBS remains unk nown. However, it has been clarified that most of the reported disorders, like dysregulation of the nervous system, altered intesti- nal motility, and increased visceral sensitivity, result *Corresponding autho . OPEN ACCESS  Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 329 from dysregulation of the bidirectional communication between the gut with its enteric nervous system and the brain (the brain-gut axis) [5]. In Japan and China, we co nducted comparativ e studies on lifestyles and IBS for nursing and medical school students who were busy and had a relatively high amount of stress related to their daily duties [6,7]. The diagnosis of IBS was based on Rome II criteria. The results of those studies showed that the prevalence of the IBS was 25.2% in males and 41.5% in females in Japan [6], and 26.6% in males and 33.6% in females in China [7]. In both countries, more females had IBS than males. In ad- dition, relationships were shown between IBS and anxi- ety, depression, sleep disorders, skipping meals and ir- regular meal times. In females of both countries, the IBS group showed a frequency for the intake of vegetables that was lower than that of the non-IBS group. Based on these results, we focused attention on lifestyle, including the daily habits of students with IBS. Accordingly, this study was conducted in order to intervene in the daily lives of the subjects an d assess the effect of the interven- tion on the improvement of the IBS symptoms. Treatment methods for patients with IBS vary widely depending on the individual subject concerned, due to individual character, genetics and environment differ- ences [8-14]. How matters related to IBS and its symp- toms are perceived results in a considerable disparity in the treatment of IBS, since IBS is a representative disor- der of the brain-gut axis [15]. On the other hand, self-monitoring has been widely understood as one of the self-health management meth- ods like the recording of weight, steps, blood pressure, the number of cigarettes smoked, and so on, because it is an easy and economical method [16-21]. Even for IBS patients, self-monitoring has had wide spread attention due to this cost-saving benefit [22,23]. Some studies have already reported the effect of self-monitoring for IBS, but most of those studies were fundamentally based on medication, and the self-monitoring was supplemen- tary [24-26]. Besides, self-monitoring was focused on the mental side of the patients in those studies. Accordingly, this study was conducted to verify the effect of lifestyle self-monitoring for the improvement of IBS. 2. METHODS 2.1. Study Population A total of 116 female freshmen at nursing schools in Kyoto prefecture participated in this study. Among these 116 students, two classes (39 and 38 students) were ran- domly chosen as the two-month and four-month inter- vention groups. Another class (39 students) was assigned as a control group. Among the 116 students, a total of 111 students (control group; n = 36, two-month interven- tion group; n = 37, four-month intervention group; n = 38) answered self-administered questionnaires (95.7%) after writing informed consent. According to our eligibil- ity criteria, males, subjects with no diagno sis of inflame- matory bowel disease, and no data inadequacy, 103 stu- dents (control group; n = 34, two-month intervention group; n = 34, four-month intervention group; n = 35) aged 18- to 26-years-old (mean ± SD: 18.6 ± 1.3) were considered ineligible (88.8 %). Study participants were asked to sign an informed consent form before they participated in the study. This study was approved by the Ethical Board of Kyoto Pre- fectural University. 2.2. Questionnaire Information In order to obtain a questionnaire suitable for our pur- pose, we combined well-known criteria with some origi- nal items. The self-recording questionnaire contained 65 items, with the following sections; bowel habits (15 items), QOL related to gastrointestinal symptoms (15 items), psychological factors (14 items), dietary habits and lifestyle (16 items), physical characteristics (4 items) and treatment for disease (1 item). The time required to complete the questionnaire was 10 minutes. After all of the subjects answered the questionnaires, the two inter- vention groups monitored their own lifestyles for two or four months. After the intervention, everyone answered the same questionnaire again. 2.3. IB Definitions This was the primary outcome measure. Patients with IBS were diagnosed with Rome II criteria [27]. Subjects were classified into three subgroups as follows: Diar- rhea-predominant IBS (IBS-D), constipation-predomi- nant IBS (IBS-C), and alteration type IBS (IBS-A). We used a Japanese version of the Rome II modular ques- tionnaire, including 15 items complied by Shinozaki et al. [28]. 2.4. QOL Definitions The QOL points related to gastrointestin al disorders were applied according to the Gastrointestinal Symptom Rat- ing Scale (GSRS) criteria [29]. The QOL of the subjects was assessed in five subscales of symptoms, acid reflux, abdominal pains, dyspepsia, diarrhea and constipation. The points applied for each of the items was the average point of the symptoms; for acid reflux it was the average of heartburn and regurgitation, for abdominal pains it was the average of epigastralgia, hunger pains and nau- sea, for dyspepsia it was it was the average of bor- borygmus, the feeling of fullness, eructation and ab- dominal wind, for diarrhea it was the average of a multi- tude of bowel movements, loose bowel movements, and Copyright © 2013 SciRes. OPEN ACCESS  Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 330 urgent bowel movements, for constipation it was the av- erage of few bowel movements, hard bowel movements and the feeling of incomplete evacuation, and for QOL related to gastrointestinal symptoms, it was the average point of these five subscales of symptoms. In each sub- scale, the minimum score of 1 indicated that the symp- tom did not affect the QOL at all. The maximum score of 7 indicated that the symptom had a harmful influence on the QOL. We used a modified Japanese version of the GSRS, including 15 items complied by Hongo et al. [30]. 2.5. Psychological Factors The hospital anxiety and depression scale (HADS) [31] was employed, a scale proven to be reliable and valid when screening for mood disorders. HADS can be di- vided into a subscale for anxiety (HAD-A) and a sub- scale for depression (HAD-D). In either of the HAD subscales, a score above 10 indicates definite clinically significant anxiety or depression, respectively, up to a maximum score of 21. Respectively, a score of more than 11 points is regarded as a definite type, a score between 8 and 10 is doubtful and a score of less than 7 points indi- cates no mood disorder. 2.6. Contents of Intervention 2.6.1. Self-Monitorin g Subjects in the intervention groups recorded their daily habits every day for two or four months, including the contents of breakfast (staple dish, main dish and side dish), their awakening time, bedtime, hours of sleep, frequency of bowel movements, and mood of the day. 2.6.2. Group Work In order to enhance the effectiveness of the self-moni- toring, a fifteen-minute group work session was con- ducted every week as one of the basic subjects of the nursing course. The members of the group work session were the same 3 or 4 students for the interventio n period. Each student set a goal to improve her lifestyle every week and wrote some messages in the self-monitoring sheet for the other members. Some groups made a pres- entation about their goals. After one week, they circu- lated the sheet in the group and assessed each other. The assessment points were as follows; “Have you remem- bered your goal for this week?”, “Have you made any efforts to accomplish that goal?”, “How much action have you taken toward you r goal?”. Figure 1 shows a flow chart for the intervention. Each intervention group continued the cycle of self-monitoring and the group work activity for two or four months. On the other hand, the control group did not conduct self- monitoring or group work activity. 2.6.3. Statistical Analysis All statistical computations were performed using the statistical software SPSS Ver.18 for windows. Wilcoxo n’s signed-rank test or McNemar ’s test was used to compare values obtained before and after intervention in each group. The Kruskal-Wallis test was u sed for comparisons among the three groups. Intention-to-Treat (ITT) analy- ses were employed for all of the analyses. A two-sided p value of less than 0.05 (p < 0.05) was considered statis- tically significant. 3. RESULTS 3.1. Characteristics of the Subjects (Table 1) There were no statistically significant differences in age, height, weight and BMI between the three groups. 3.2. Prevalence of IBS (Figures 2 and 3) There was an 11.8 point decrease in IBS prevalence in the two-month interventio n group. Meanwhile, there was only an 8.9 point decrease in the co ntrol group and a 5.8 point decrease in the four-month intervention group. In regard to the IBS-C subgroups, there were decreases of 8.8 and 2.8 points in the two-month and four-month in- tervention groups, respectively, but no change in the control gr oup. 3.3. The Relationship between Psychological Factors and IBS (Figure 4) The anxiety scores decreased 1.1 points in the two-month intervention group (p = 0.02) and 2.0 points in the four- month intervention group (p < 0.01), although there was only a 0.2 point decrease in the con trol group. 3.4. Sleep Time, Defecation Habits, Dietary Habits and Contents of Meals (Table 2) In the two-month intervention group, time of sleep be- came irregular after the intervention (p = 0.01), since the awakening time (p < 0.01) and bedtime (p < 0.01) be- came irregular after the intervention. In the four-month intervention group, the percentage of students using laxatives decreased 17.2 percentage points after the in- tervention (p = 0.01), although there were just 8.8 point and 5.9 point decreases in the control group and the two- month intervention group, respectively. The percent of students taking meals regularly de- creased after the intervention in th e con trol group and th e four-month intervention group. In both of the interven- tion groups, the percent of students having three dishes at breakfast increased after the intervention. On the other hand, students having three dishes at lunch decreased significantly after intervention in the four-month inter- vention grou p (p = 0.01). Copyright © 2013 SciRes. OPEN ACCESS  Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 Copyright © 2013 SciRes. 331 Figure 1. Flow chart of this study. Tab l e 1 . Characteristics of the subjects in the intervention and the control grou p s. Control group Intervention gr oup (2 months) Intervention gr oup (4 months) p1 n = 34 n = 34 n = 35 Age 18.3 ± 0.618.9 ± 1.5 18.5 ± 1.5 0.09 Height (cm)158.3 ± 4.4158.7 ± 6.4 157.6 ± 5.1 0.72 Weight (kg)51.6 ± 6.050.6 ± 5.7 51.1 ± 5.5 0.79 BMI 20.6 ± 2.520.3 ± 1.9 20.6 ± 2.3 0.97 Data are presented as mean ± SD Figure 2. The prevalence of IBS in the intervention and the control groups IBS irritable bowel syndrome. n.s.: not signifi- cant. McNemar’s test. B MI: weight (kg)/height ( m)2; 1Kruskal Wallis’ tes t . OPEN ACCESS  Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 332 Table 2. Sleep time, defecat i o n habits, dietary habits and conten t s of meals in the intervention and the co nt rol groups. Control group Intervention group (2 months) Intervention group (4 months) before after p1 before after p1 before after p1 n = 34 n = 34 n = 34 n = 34 n = 35 n = 35 Awakening time 0.69 0.01* 0.45 Regular 27 (79.4) 29(85.3) 32(94.1)23(67.6) 29 (82.9) 26 (74.3) Irregular 7 (20.6) 5(14.7) 2 (5.9)11(32.4) 6 (17.1) 9 (25.7) Bedtime 1.00 <0.01** 0.58 Regular 19 (55.9) 19(55.9) 25(73.5)16(47.1) 18 (51.4) 15 (42.9) Irregular 15 (44.1) 15(44.1) 9 (26.5)18(52.9) 17 (48.6) 20 (57.1) Time of sleep 0.55 <0.01** 0.55 Regular 21 (61.8) 18(52.9) 25(73.5)17(50.0) 21 (60.0) 18 (51.4) Irregular 13 (38.2) 16(47.1) 9 (26.5)17(50.0) 14 (40.0) 17 (48.6) Use of laxatives 0.10 0.16 0.01* Nothing 26 (76.5) 29(85.3) 29(85.3)31(91.2) 27 (77.1) 33 (94.3) Sometimes 7 (20.6) 5(14.7) 5 (14.7)3(8.8) 7 (20.0) 1 (2.9) Everyday 1 (2.9) 0(0) 0 (0) 0(0) 1 (2.9) 1 (2.9) Time of meal 0.16 0.16 0.01* Regular 11 (32.4) 9(26.5) 7 (20.6)7(20.6) 14 (40.0) 8 (22.9) Sometimes irregular 21 (61.8) 21(61.8) 23(67.6)19(55.9) 16 (45.7) 20 (57.1) Irregular 2 (5.9) 4(11.8) 4 (11.8)8(23.5) 5 (14.3) 7 (20.0) Contents of breakfast 0.32 0.41 0.71 Three dishes 1 (2.9) 1(2.9) 6 (17.6)8(23.5) 2 (5.7) 3 ( 8.6) One or two dishes 31 (91.2) 32(94.1) 27(79.4)25(73.5) 31 (88.6) 28 (80.0) No breakfast or only confectionaries 2 (5.9) 1(2.9) 1 (2.9)1(2. 9) 2 (5.7) 4 (11.4) Contents of lunch 0.66 0.26 0.01* Three dishes 20 (58.8) 20(58.8) 17(50.0)21(61.8) 16 (45.7) 8 (22.9) One or two dishes 14 (41.2) 13(38.2) 17(50.0)12(35.3) 19 (54.3) 26 (74.3) No lunch or only confectionaries 0 (0) 1(2.9) 0 (0) 1(2. 9) 0 (0) 1 ( 2.9) Contents of dinner 0.16 0.05 0.48 Three dishes 22 (64.7) 20(58.8) 27(79.4)23(67.6) 21 (60.0) 20 (57.1) One or two dishes 12 (35.3) 14(41.2) 7 (20.6)11(32.4) 13 (37.1) 13 (37.1) No dinner or only confectionaries 0 (0) 0(0) 0 (0) 0(0) 1 (2.9) 2 (5.7) Data are presented as the number of cases (%) *p < 0.05, **p < 0.01; 1McNemar's test (for t wo catego r i es) or Wilcoxon’s signed-rank test (for three or more categ o r i es). 3.5. QOL Related to Gastrointestinal Symptoms (Table 3) In the four-month intervention group, the QOL points related to all gastrointestinal disorders decreased after the intervention. Especially, the points for acid reflux (p = 0.01), abdominal pains (p = 0.01) and dyspepsia (p < 0.01) decreased significantly after the intervention. Due to these subscales, the average points decreased 0.3 oints (p < 0.01) in the four-month intervention group. p Copyright © 2013 SciRes. OPEN ACCESS 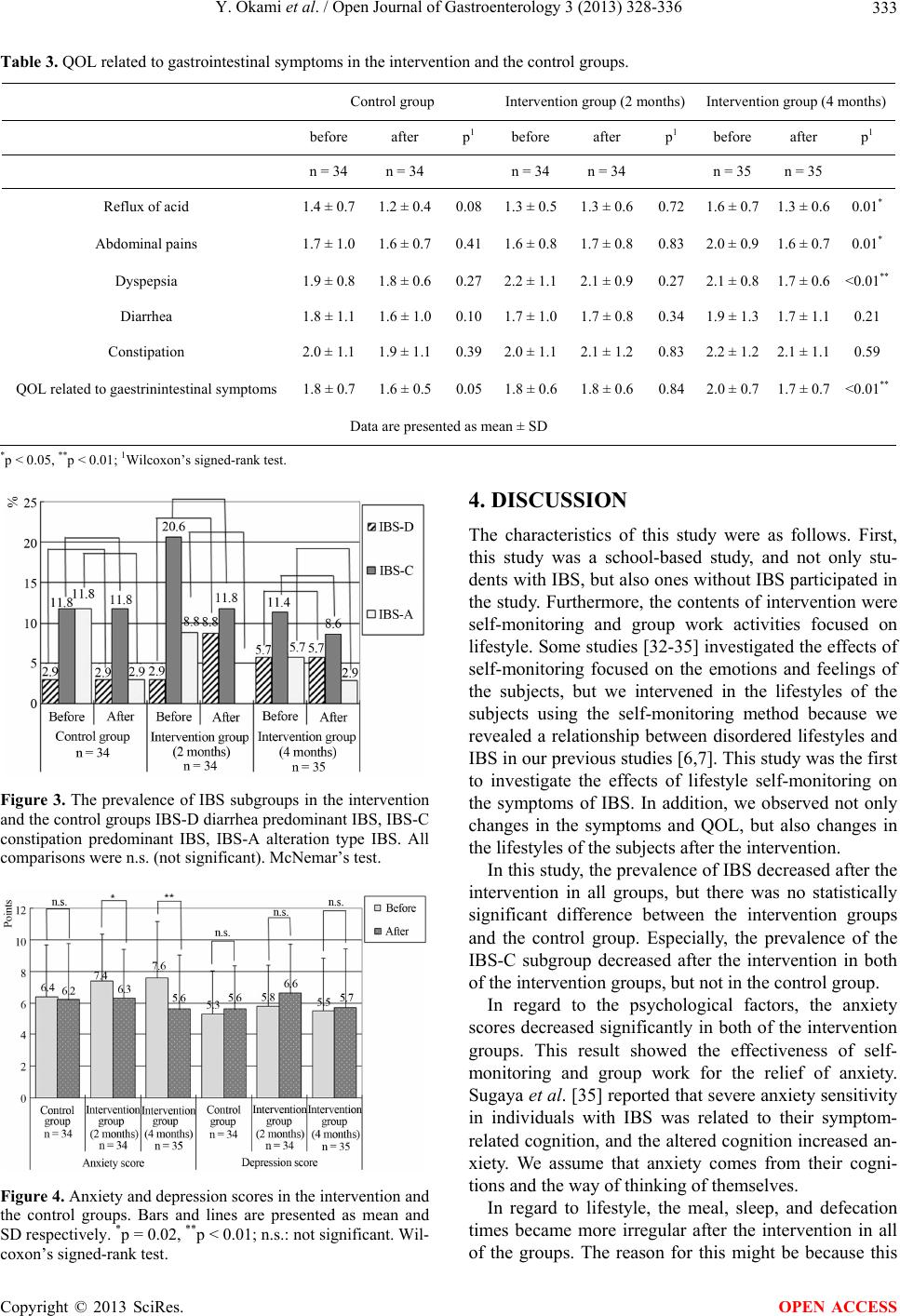 Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 333 Table 3. QOL related to gastrointestinal symptoms in the intervention and the control groups. Control group Intervention group (2 months) Intervention group (4 months) before after p1 before after p1 before after p1 n = 34 n = 34 n = 34 n = 34 n = 35 n = 35 Reflux of acid 1.4 ± 0.71.2 ± 0.40.081.3 ± 0.51.3 ± 0.60.72 1.6 ± 0.7 1.3 ± 0.60.01* Abdominal pain s 1.7 ± 1.01.6 ± 0.70.411.6 ± 0.81.7 ± 0.80.83 2.0 ± 0.9 1.6 ± 0.70.01* Dyspepsia 1.9 ± 0.81.8 ± 0.60.272.2 ± 1.12.1 ± 0.90.27 2.1 ± 0.8 1.7 ± 0.6<0.01** Diarrhea 1.8 ± 1.11.6 ± 1.00.101.7 ± 1.01.7 ± 0.80.34 1.9 ± 1.3 1.7 ± 1.10.21 Constipation 2.0 ± 1.11.9 ± 1.10.392.0 ± 1.12.1 ± 1.20.83 2.2 ± 1.2 2.1 ± 1.10.59 QOL related to gaestrinintestinal symptoms 1.8 ± 0.71.6 ± 0.50.051.8 ± 0.61.8 ± 0.60.84 2.0 ± 0.7 1.7 ± 0.7<0.01** Data are presented as mean ± SD *p < 0.05, **p < 0.01; 1Wilcoxon’s signed-rank test. Figure 3. The prevalence of IBS subgroups in the intervention and the control groups IBS-D diarrhea predominant IBS, IBS-C constipation predominant IBS, IBS-A alteration type IBS. All comparisons were n.s. (not significant). McNemar’s test. Figure 4. Anxiety and depression scores in the intervention and the control groups. Bars and lines are presented as mean and SD respectively. *p = 0.02, **p < 0.01; n.s.: not significant. Wil- coxon’s signed-rank test. 4. DISCUSSION The characteristics of this study were as follows. First, this study was a school-based study, and not only stu- dents with IBS, but also ones without IBS participated in the study. Fu rthermore, the contents of in tervention were self-monitoring and group work activities focused on lifestyle. Some studies [32-35] investigated the effects of self-monitoring focused on the emotions and feelings of the subjects, but we intervened in the lifestyles of the subjects using the self-monitoring method because we revealed a relationship between disordered lifestyles and IBS in our previou s studies [6 ,7]. This study w as the fir st to investigate the effects of lifestyle self-monitoring on the symptoms of IBS. In addition, we observed not only changes in the symptoms and QOL, but also changes in the lifestyles of the subjects after the intervention. In this study, the prevalence of IBS decreased after the intervention in all groups, but there was no statistically significant difference between the intervention groups and the control group. Especially, the prevalence of the IBS-C subgroup decreased after the intervention in both of the intervention groups, but no t in the control group. In regard to the psychological factors, the anxiety scores decreased significantly in both of the intervention groups. This result showed the effectiveness of self- monitoring and group work for the relief of anxiety. Sugaya et al. [35] reported that severe anxiety sensitivity in individuals with IBS was related to their symptom- related cognition, and the altered cognition increased an- xiety. We assume that anxiety comes from their cogni- tions and the way of thinking of themselves. In regard to lifestyle, the meal, sleep, and defecation times became more irregular after the intervention in all of the groups. The reason for this might be because this Copyright © 2013 SciRes. OPEN ACCESS  Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 334 study was conducted with first-year college students as the subjects. When the subjects were high school stu- dents, they regularly spent time stud ying for their college entrance examinations, but their lifestyles changed after entering college. At college, they can choose the classes they take by themselves, and most of the subjects worked part-time after classes. Their meal, sleeping, and defeca- tion times tended to be very irregular along with these changes in lifestyle. The number of students who took three dishes at lunch decreased significantly after the intervention in the four-month intervention group. The number of students who took three dishes at dinner also decreased after the intervention in all of the groups. The reason for this is because most of the students started to live alone and cook by themselves. On the other hand, the contents of breakfast improved after the intervention in both of the intervention groups. This means that they recognized the importance of breakfast and were more aware of that importance due to the self-monitoring and the group work activities. The frequency of using laxa- tives decreased significantly in the four-month interven- tion group . The QOL points related to gastrointestinal symptoms decreased 0.4 points after the intervention in the four- month intervention group. This depended on three items, acid reflux, abdominal pain and dyspepsia. Previous studies [33,34] conducted psychoeducation for patients with IBS, showing a direct effect on global IBS symptom improvement and improvement in QOL, independent of its effects on distress [34]. In our study, there was an improvement of QOL related to gastrointes- tinal symptoms, but not any significant reduction of the IBS prevalence. Moss-Morris et al. [36] showed that symptomatic relief due to self-management was observ- ed after an interven tion and that the relief con tinued until six months later. They also reported that a clinically sig- nificant change in the IBS severance score was ob- served six months later. Kennedy et al. [24] also reported that the effect of cognitive behavioral therapy in addition to the intake of mebeverine continued until six month later. These studies showed the possibility that the effects of self-management continued for a while after the in- tervention or that it became visible some months after the intervention. This study was limited for the following reasons. First, the persons who conducted this study were not special- ists in self-monitoring. Second, we didn’t compare self- monitoring with other therapeutic approaches in this study. Third, the subjects of th is study also included stu- dents who did not have any IBS symptoms. As a whole, there were only 28 students identified with IBS versus 75 students without before intervention. The more severe symptoms of IBS are, the more rapidly the effects of improvement surface [37]. Considering the fact, it was difficult to obtain a rapid response to the self-monito ring in this school-based study. Forth, we didn’t follow up on the subjects until some time after the intervention. And lastly, this study was conducted with first-grade college students as the subjects in spring. The intervention period was during a time when the lifestyle of students under- went a lot of changes. This study might be regarded as an exploratory re- search since the number of subjects was adjusted ac- cording to the number of classes and there were several primary outcome measures (Rome II, HADS and GSRS) . These limitations must be considered in our future re- search. Future research should also include long-term follow-up studies of IBS patients treated with self-moni- toring, and it might be more appropriate if the subjects were second or third year students. Overall, this study showed that lifestyle self-moni- toring intervention for two or four months didn’t reduce the prevalence of the IBS significantly, but related to gastrointestinal symptoms, it did decrease anxiety and improved QOL. 5. ACKNOWLEDGEMENTS We would like to express our thanks to the staff and all of the students that collaborated in this research at the Kyoto Prefectural University of Medicine and the nursing school at the Japan Red Cross Kyoto Daiichi Hospital. REFERENCES [1] Fujii, Y. and Nomura, S. (2006) The effects of psychoso- cial factors and daily habits of irritable bowel syndrome carriers on the symptoms and disease-specific QOL. Shokaki Shinshin Igaku, 13, 14-25. [2] Talley, N.J. (1999) Irritable bowel syndrome: definition, diagnosis and epidemiology. Best Practice & Research Clinical Gastroenterology, 13, 371-384. http://dx.doi.org/10.1053/bega.1999.0033 [3] Russo, M.W., Gaynes, B.N. and Drossman, D.A. (1999) A national survey of practice patterns of gastroenterolo- gists with comparison to the past two decades. Journal of Clinical Gastroenterology, 29, 339-343. http://dx.doi.org/10.1097/00004836-199912000-00009 [4] Thompson, W.G., Heaton, K.W., Smyth, G.T., et al. (2000) Irritable bowel syndrome in general practice: pre- valence, characteristics, and referral. Gut, 46, 78-82. http://dx.doi.org/10.1136/gut.46.1.78 [5] Fukudo, S., Nomura, T. and Hongo, M. (1998) Impact of corticotropin-releasing hormone on gastrointestinal mo- tility and adrenocorticotropic hormone in normal controls and patients with irritable bowel syndrome. Gut, 42, 845- 849. http://dx.doi.org/10.1136/gut.42.6.845 [6] Okami, Y., Kato, T., Nin, G., et al. (2011) Lifestyle and psychological factors related to irritable bowel syndrome in nursing and medical school students. Journal of Gas- Copyright © 2013 SciRes. OPEN ACCESS  Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 335 troenterology, 46, 1403-1410. http://dx.doi.org/10.1007/s00535-011-0454-2 [7] Okami, Y., Nin, G., Harada, K., et al. (2013) Irritable bowel syndrome in Chinese nursing and medical school students—Related lifestyle and psychological factors. Open Journal of Gastroenterology, 3, 55-63. http://dx.doi.org/10.4236/ojgas.2013.31009 [8] Chang, L., Toner, B.B., Fukudo, S., et al. (2006) Gender, age, society, culture, and the patient’s perspective in the functional gastrointestinal disorders. Gastroenterology, 130, 1435-1446. http://dx.doi.org/10.1053/j.gastro.2005.09.071 [9] Faresjö, A., Anastasiou, F., Lionis, C., et al. (2006) Health-related quality of life of irritable bowel syndrome patients in different cultural settings. Health and Quality of Life Outcomes, 4, 21. http://dx.doi.org/10.1186/1477-7525-4-21 [10] Farnam, A., Somi, M.H., Sarami, F., et al. (2007) Per- sonality factors and profiles in variants of irritable bowel syndrome. World Journal of Gastroenterology, 13, 6414- 6418. http://dx.doi.org/10.3748/wjg.13.6414 [11] Handa, M., Nukina, H., Hosoi, M., et al. (2008) Child- hood physical abuse in outpatients with psychosomatic symptoms. BioPsychoSocial Medicine, 2, 8. http://dx.doi.org/10.3748/wjg.13.6414 [12] Bengtson, M.B., Rønning, T., Vatn, M.H., et al. (2006) Irritable bowel syndrome in twins: Genes and environ- ment. Gut, 55, 1754-1759. http://dx.doi.org/10.1136/gut.2006.097287 [13] Saito, Y.A., Zimmerman, J.M., Harmsen, W.S., et al. (2008) Irritable bowel syndrome aggregates strongly in families: a family-based case-control study. Neurogas- troenterology & Motility, 20, 790-797. http://dx.doi.org/10.1111/j.1365-2982.2007.01077.x [14] Ali, A., Toner, B.B., Stuckless, N., et al. (2000) Emo- tional abuse, self-blame, and self-silencing in women with irritable bowel syndrome. Psychosomatic Medicine, 62, 76-82. [15] Drossman, D.A., Richter, J.E., Talley, N.J., et al. (1994) Functional gastrointestinal disorders. Little, Brown and Co., Boston, pp. 1-174. [16] Kamaura, M., Ohono, H., Takahashi, M., et al. (2007) Evaluation of a guidance method for reducing lifestyle- related diseases by the self-monitoring of blood collection in small- and medium-sized enterprises. Sangyo Eisei- gaku Zassh., 49, 89-97. http://dx.doi.org/10.1539/sangyoeisei.49.89 [17] Aittasalo, M., Miilunpalo, S., Kukkonen-Harjula, K., et al. (2006) A randomized intervention of physical activity promotion and patient self-monitoring in primary health care. Preventi ve Medicine, 42, 40-46. http://dx.doi.org/10.1016/j.ypmed.2005.10.003 [18] Halme, L., Vesalainen, R., Kaaja, M., et al. (2005) Self-monitoring of blood pressure promotes achievement of blood pressure target in primary health care. American Journal of Hypertension, 18, 1415-1420. http://dx.doi.org/10.1016/j.amjhyper.2005.05.017 [19] Soumerai, S.B., Mah, C., Zhang, F., et al. (2004) Effects of health maintenance organization coverage of self- monitoring devices on diabetes self-care and glycemic control. Archives of Internal Medicine, 164, 645-652. http://dx.doi.org/10.1001/archinte.164.6.645 [20] Mossavar-Rahmani, Y., Henry, H., Rodabough, R., et al. (2004) Additional self-monitoring tools in the dietary modification component of The Women’s Health Initia- tive. Journal of the American Dietetic Association, 104, 76-85. http://dx.doi.org/10.1016/j.jada.2003.10.017 [21] Sjöberg, S., Carlson, A., Rosenqvist, U., et al. (1988) Health attitudes, self-monitoring of blood glucose, meta- bolic control and residual insulin secretion in type 1 dia- betic patients. Diabetic Medicine, 5, 449-453. http://dx.doi.org/10.1111/j.1464-5491.1988.tb01026.x [22] Andersson, E., Ljótsson, B., Smit, F., et al. (2011) Cost- effectiveness of internet-based cognitive behavior therapy for irritable bowel syndrome: Results from a randomized controlled trial. BMC Public Health, 11, 215. http://dx.doi.org/10.1186/1471-2458-11-215 [23] Everitt, H.A., Moss-Morris, R.E., Sibe lli, A., et al . (2010) Management of irritable bowel syndrome in primary care: Feasibility randomised controlled trial of mebeverine, methylcellulose, placebo and a patient self-management cognitive behavioural therapy website. (MIBS trial). BMC Gastroenterology, 10, 136. http://dx.doi.org/10.1186/1471-230X-10-136 [24] Kennedy, T.M., Chalder, T., McCrone, P., et al. (2006) Cognitive behavioural therapy in addition to antispas- modic therapy for irritable bowel syndrome in primary care: Randomised controlled trial. Health Technology As- sessment, 10, 1-67. [25] Mahvi-Shirazi, M., Fathi-Ashtiani, A., Rasoolzade-Ta- batabaei, S.K., et al. (2012) Irritable bowel syndrome treatment: cognitive behavioral therapy versus medical treatment. Archives of Medical Science, 8, 123-129. http://dx.doi.org/10.5114/aoms.2012.27292 [26] Reme, S.E., Stahl, D., Kennedy, T., et al. (2011) Media- tors of change in cognitive behaviour therapy and me- beverine for irritable bowel syndrome. Psychological Medicine, 41, 2669-2679. http://dx.doi.org/10.1017/S0033291711000328 [27] Thompson, W.G., Longstreth, G.F., Drossman, D.A., et al. (1999) Functional bowel disorders and functional ab- dominal pain. Gut, 45, 43-47. [28] Shinozaki, M., Kanazawa, M., Sagami, Y., et al. (2006) Validation of the Japanese version of the Rome II modu- lar questionnaire and irritable bowel syndrome severity index. Journal of Gastroenterology, 41, 491-494. http://dx.doi.org/10.1007/s00535-006-1799-9 [29] Dimenäs, E., Glise, H., Hallerbäck, B., et al. (1995) Well-being and g astrointestinal symptoms among patients referred to endoscopy owing to suspected duodenal ulcer. Scandinavian Journal of Gastroenterology, 30, 1046- 1052. http://dx.doi.org/10.3109/00365529509101605 [30] Hongo, M., Fukuhara, S. and Joseph, G. (1999) Evalua- tion of Japanese gastrointestinal symptom rating scale. Diagnosis and Treatment, 87, 731-736. [31] Hatta, H., Higashi, A., Yashiro, H., et al. (1998) A vali- Copyright © 2013 SciRes. OPEN ACCESS  Y. Okami et al. / Open Journal of Gastroenterology 3 (2013) 328-336 Copyright © 2013 SciRes. 336 OPEN ACCESS dation of the hospital anxiety and depression scale. Japanese Journal of Psychosomatic Medicine, 38, 309- 315. [32] Gros, D.F., Antony, M.M., McCabe, R.E. , et al . (2011) A preliminary investigation of the effects of cognitive be- havioral therapy for panic disorder on gastrointestinal distress in patients with comorbid panic disorder and irri- table bowel syndrome. Depression and Anxiety, 28, 1027- 1033. http://dx.doi.org/10.1002/da.20863 [33] Lackner, J.M., Jaccard, J., Krasner, S.S., et al. (2007) How does cognitive behavior therapy for irritable bowel syndrome work? A mediational analysis of a randomized clinical trial. Gastroenterology, 133, 433-444. http://dx.doi.org/10.1053/j.gastro.2007.05.014 [34] Lackner, J.M., Jaccard, J., Krasner, S.S., et al. (2008) Self-administered cognitive behavior therapy for moder- ate to severe irritable bowel syndrome: Clinical efficacy, tolerability, feasibility. Clinical Gastroenterology and Hepatology, 6, 899-906. http://dx.doi.org/10.1016/j.cgh.2008.03.004 [35] Sugaya, N., Nomura, S. and Shimada, H. (2012) Rela- tionship between cognitive factors and anxiety in indi- viduals with irritable bowel syndrome. International Journal of Behavioral Medicine, 19, 308-315. http://dx.doi.org/10.1007/s12529-011-9195-0 [36] Moss-Morris, R., McAlpine, L., Didsbury, L.P., et al. (2010) A randomized controlled trial of a cognitive be- havioural therapy-based self-management intervention for irritable bowel syndrome in primary care. Psycho- logical Medicine, 40, 85-94. http://dx.doi.org/10.1017/S0033291709990195 [37] Lackner, J.M., Gudleski, G.D., Keefer, L., et al. (2010) Rapid response to cognitive behavior therapy predicts treatment outcome in patients with irritable bowel syn- drome. Clinical Gastroenterology and Hepatology, 8, 426-432. http://dx.doi.org/10.1016/j.cgh.2010.02.007 ABBREVIATIONS BMI, body mass index; HADS, the hospital an xiety and depression scale; HAD-A, a subscale for anxiety; HAD-D, a subscale for de pr ession; GSRS, the Gastrointestinal Symptom Rating Scale; QOL, quality of life; IBS, irritable bowel syndrome; IBS-A, the alteration type IBS; IBS-C, the constipation-predominant IBS; IBS-D, the diarrhea-predominant IBS; SD, standard deviation.
|