Journal of Cancer Therapy
Vol.08 No.05(2017), Article ID:76492,12 pages
10.4236/jct.2017.85039
Evaluation of the CO2 Laser Therapy on Vulvo-Vaginal Atrophy (VVA) in Oncological Patients: Preliminary Results
Isabella Pagano1, Stefania Gieri2, Francesca Nocera1, Giuseppe Scibilia1, Filippo Fraggetta3, Antonio Galia3, Mauro Gioè2, Basilio Pecorino1*, Paolo Scollo1
1Department of Obstetrics and Gynecology, Cannizzaro Hospital, Catania, Italy
2Institute of Molecular Bioimaging and Physiology, National Research Council (IBFM-CNR)-LATO, Cefalù (PA), Italy
3Pathology Unit, Cannizzaro Hospital, Catania, Italy

Copyright © 2017 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY 4.0).
http://creativecommons.org/licenses/by/4.0/



Received: April 10, 2017; Accepted: May 21, 2017; Published: May 26, 2017
ABSTRACT
Objective: To evaluate the impact of fractionated CO2 laser therapy on vaginal atrophy and mild/moderate stress urinary incontinence (SUI) symptoms in patients with physiological or surgically-induced menopause. Materials and Methods: Post-menopausal patients (n = 33) presenting vaginal atrophy and/or SUI, underwent three vaginal CO2 laser treatment sessions, performed at 1-month intervals. Vaginal symptoms were evaluated using the Vaginal Health Index Score (VHI-S), Visual Analogue Scales (VAS) for dyspareunia and global patient satisfaction. The impact of urinary incontinence on patient quality of life was evaluated using the International Consultation on Incontinence Questionnaire (ICIQ). Symptoms were evaluated before treatment and at every subsequent treatment session, as well as 3 months following the last treatment session. RESULTS: The three-session treatment series led to a significant improvement in both subjective symptoms (dryness, burning, dyspa- reunia) and clinical signs (VHI-S) (P < 0.01). In addition, reductions in the frequency and severity of SUI symptoms (P < 0.01) were noted during the treatment period, and were maintained after for at least 3 months after completion of the treatment course. Improvements in VHI-S were significantly greater in patients with surgically-induced menopause, as compared to those with physiological menopause. The vast majority of patients (90%) were satisfied with the procedure, and reported a significant improvement in quality of life. No adverse events were recorded throughout the study period. Conclusions: Fractionated CO2 laser therapy is a safe, effective and easy-to-perform treatment modality for menopause-related vaginal atrophy and SUI.
Keywords:
Laser CO2, Vaginal Atrophy, Urinary Incontinence, Menopause

1. Introduction
Genitourinary syndrome of menopause (GSM) is a condition affecting appro- ximately 50% of postmenopausal women, and to have significant impacts in the sexual sphere [1] [2] [3] . GSM develops as a direct result of reduced ovarian function and circulating hormone levels [4] . The syndrome is characterised by an involution of the genitourinary mucosa and adjacent vulvo-vaginal tissues and by histologically and clinically apparent changes in type I versus type III collagen ratios and in a reduction in both the quantity of elastic fibres and in vascularisation of the genitourinary tissues [5] . Consequently, the diameter of the vagina is reduced and the vaginal epithelium becomes pale and tends to develop infections. Clinically, these changes present as dryness, burning sensation, severe dyspareunia, dysuria and stress urinary incontinence (SUI) [6] [7] . Considering the progressive rise in the age of the general population, many women face this problem for more than one third of their adult life [1] .
A variety of therapeutic options, including topical and systemic hormonal therapies and non-hormonal lubrication provide relief of GSM symptoms [8] . Topical hormonal therapy is the gold standard treatment approach, however, patient compliance remains poor and is contraindicated in patients with a history of breast cancer [9] [10] .
In recent years, a novel therapeutic fractionated CO2 laser-elicited vaginal mucosa-regenerating treatment option has been introduced, and has demon- strated positive effects on collage nogenesis-driven tissue remodelling. The treat- ment exploits a unique combination of minimal superficial ablation and deeper thermal deposition of the fractionated CO2 laser energy, delivered via a probe designed specifically for the vaginal anatomy. In response, collagen and elastic fibre remodelling, glycogen synthesis and transudate production are induced, yielding a state typical of the reproduction age. In parallel, the microablative action of the fractionated CO2 laser stimulates the interaction of heat shock proteins, which activate fibroblasts to produce other components of the extra- cellular matrix, such as proteoglycans, glycosaminoglycans [11] . A fundamental role is played by transforming growth factor-beta (TGF-β), and epidermal growth factor (FGF and EGF), that stimulate angiogenic activity [12] [13] [14] . Overall, the resulting light-induced eutrophication process involves early thermal damage (within 48 - 72 h of treatment), which is followed by a proliferation phase, with production of collagen and extracellular matrix (in the subsequent 30 days). Lastly, the remodelling phase (after 40 days) involves the apposition of mature collagen fibres and new elastic fibres [15] .
The purpose of this study was to evaluate the efficacy of CO2 laser therapy in treating vulvo-vaginal atrophy (VVA) and mild-to-moderate SUI symptoms in postmenopausal women.
2. Materials and Methods
2.1. Patients
Postmenopausal patients, between the ages of 33 - 71, presenting vaginal atrophy, and/or type 1 or type 2 SUI symptoms, with a negative cervical smear test within 12 months of the study, were eligible to participate in this study. Key exclusion criteria included active genitourinary cancer, active genitourinary infections, urge or mixed urinary incontinence, pelvic organ prolapse > Stage II, and history of anamnestic allergic reactions to laser energy.
2.2. Study Design
After providing informed, signed consent, the patients were treated between February and December 2015 in the outpatient clinic of the Azienda Ospedaliera “Cannizzaro” in Catania, Italy, Department of Obstetrics and Gynaecology. Pre-treatment assessments included a physical examination, assessment of quality of life, dyspareunia and global wellness. Patients who complained of isolated urinary incontinence or urinary incontinence associated with a genital disorder, underwent additional tests, including urine microscopy and culture, and completed questionnaires designed to evaluate the SUI (type 1-2). In addition, a pretreatment biopsy sample was collected from all patients who provided informed consent.
Once the need for treatment was confirmed, patients underwent three CO2 laser treatment sessions, performed at one-month intervals. The FemiLift CO2 laser (Alma Laser, Israel) was focused through holographic lenses to deliver microablative CO2 laser energy (30 Watts, 60 - 100 mJ/ppxl, high laser mode, 0.5 Hz), with an 81-pixel beam in a 9 × 9 mm template. Three passes were performed at each treatment session, where the probe was rotated and retracted 1 cm after completion of each rotation, in order to cover the entire vaginal canal. Energy for first application was between 60 mJ or 100 mJ, depending patient’s menopausal age and comfort, while energy in the second and third sessions was 20% lower (e.g., 100 mJ in first session and 80 mJ in second and third sessions). In patients with SUI only, laser energy was delivered at three positions only: 11-12-1 ‘o clock positions, 1 cm beyond the mid-urethra level, directly under the mid urethra, and 1 cm before the midurethral level.
2.3. Evaluations
At the first follow-up visit (FU1), performed 3 months after the third treatment session, symptoms were evaluated using validated quality of life questionnaires, devised to assess the reported condition and SUI. More specifically, the intensity of dyspareunia was evaluated using a pain visual analogue scale (VAS) (0: complete absence of symptoms, 10: worst symptoms) and satisfaction with global wellness of the patient was evaluated with a different VAS (0 to 10 scale). The impact of urinary incontinence on quality of life was evaluated with the International Consultation on Incontinence modular Questionnaire short form [16] (ICIQ-UI: 0 to 18 scale). Subjective patient evaluations were obtained before 1st treatment session and then after 3 months from 3rd treatment session (FU1 visit), in order to monitor their evolution. In parallel, the Vaginal Health Index Score (VHI-S: 5 to 25 scale) was recorded before 1st laser treatment and after 3 months from the 3rd treatment session (FU1 visit). As part of this visit, a biopsy vaginal mucosa sample was collected.
2.4. Biopsies
Vaginal biopsy samples were taken from the right or left lateral walls, under local anaesthesia, using a punch needle with a 2 mm diameter, and then embedded in paraffin. Histological analyses included assessment of mucosal thickness, collagen type and content, and morphology. The thickness of the epithelial layer was measured at the thinnest, middle and thickest points, averaged and then compared to the average measures for the same patient at baseline. Formalin-fixed tissue sections were stained with anti-collagen III (clone HDW1.1 (Biogenex), diluted 1:400) and anti-collagen IV antibodies (clone COL-94 (Biogenex) diluted 1:50), to enable qualitative evaluation of the concentration of type III and IV collagens. Stainings were carried out using a polymeric detection system: Kit Bond Polymer Refine Detection Leica and immune-stainer Leica Bond (Leica Biosystems-Wetzlar, Germany)
At time of submission of this paper, 20 of 33 samples were analysed.
2.5. Statistical Analysis
Mean (± standard deviation) scores were calculated. An ANOVA model was used for repeated measurements and an “ad hoc” T-test was used to evaluate the efficacy of each treatment session on symptoms.
3. Results
The 33 participating patients presented symptoms of vaginal atrophy only (48.5%, n = 16) or both vaginal atrophy and SUI (51.5%, n = 17). Patients were of a mean age of 52.3 ± 9.9 years, and after an average 7.0 ± 5.8 years from menopause onset. Fifteen of the 33 patients (45.4%) had a history of cancer, with a distribution of 20% ovarian, 27% cervical, 7% breast and 46% endometrial cancer. Patient baseline characteristics are summarized in Table 1.
Progressive improvements in SUI symptoms were noted between the first and last treatment sessions, as manifested by a mean 2.6-point reduction in SUI scores (p-value < 0.05, Table 2), and an increase in VHI scores (p-value < 0.05, Table 2). Improved moisture and objective characteristics of the vaginal mucosa, as expressed by a mean 6-point rise in VHI-S, were recorded as well (Table 2). In parallel, dyspareunia VAS scores significantly declined over the course of treatment and stood at 4.3 at the 3-month follow-up visit (p-value < 0.05 Table 2). Slightly greater improvements in subjective assessments and clinical signs were observed among patients with surgery-induced menopause, as compared to those who underwent physiological menopause (Figures 1-3 and Table 2). No adverse events were reported during the study period. All the patients were satisfied with the procedure, and reported a significant improvement in their quality of life (VAS scale).
Before treatment, the stratified squamous epithelium appeared atrophic and thin, with no evidence of the crests of the Malpighian layer and epithelial papillae, and with a flattened sub-epithelial junction (Figure 4(a), Figure 5(a), Figure 6(a)). Post-treatment histology samples showed restoration of the epithelial and subepithelial structures, characteristic of reproductive-age vaginal mucosa
Table 1. Patient baseline characteristics.
Table 2. Patient-evaluated symptom severity.
*Difference between treatment sessions P < 0.05.
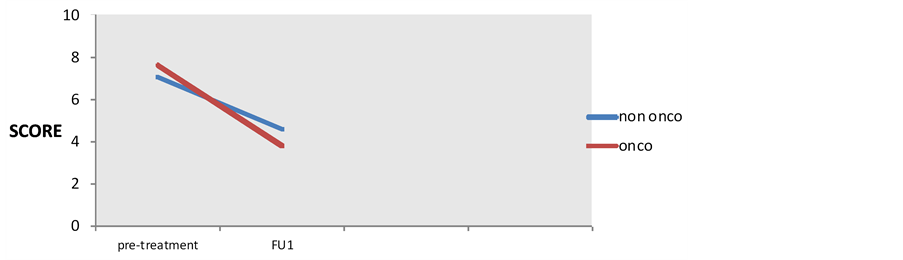
Figure 1. ICIQ: incontinence questionnaire in patients with surgery-induced menopause (onco) and In patients with physiological menopause (non onco).
Figure 2. VHI: vaginal health index in patients with surgery-induced menopause (onco) and In patients with physiological menopause (non onco).
Figure 3. VAS: visual analogique scale in patients with surgery-induced menopause (onco) and In patients with physiological menopause (non onco).
(Figure 4(b), Figure 5(b), Figure 6(b)). Immunostaining for collagen III and IV demonstrated a visible post-treatment enhancement. Microscopic examination of the biopsy sections revealed a striking increase in the thickness of epitelium, with resurfacing of the Malpighian layer and epithelial papillae. The median improvement from baseline in epithelium thickness was 97% (range: 9% - 203%).
4. Discussion
The first use of CO2 laser in gynaecologic surgery was reported in 1973 [17] . The technique involves transformation of light energy into heat, which then causes
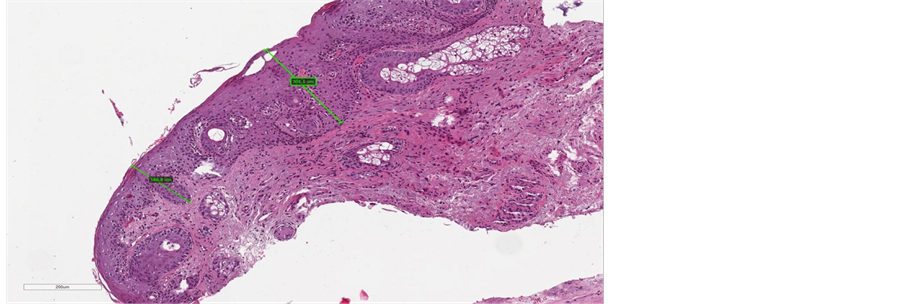
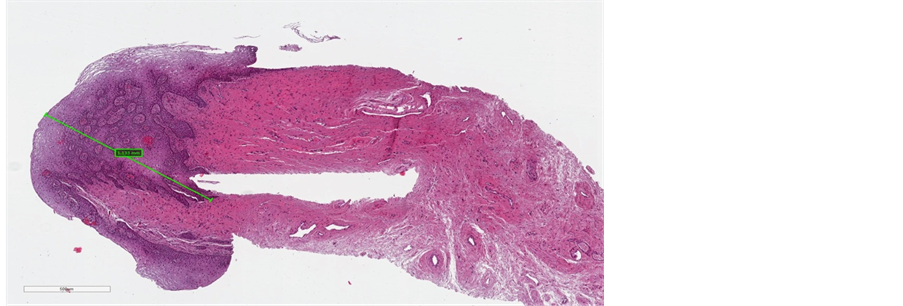
Figure 4. (a) pre-treatment section of epithelium (maximum measure of 300 µm); (b) post-treatment section of epithelium (maximum measure of 1133 µm).
evaporation of water from within the target cells. The fractionated/pixel CO2 laser treatment used in this study triggers superficial thermo-ablation, and deep thermal cell activation to stimulate tissue remodelling. The process involves a small family of proteins, known as heat shock proteins (HSP), which is activated, [18] [19] leading to a change in cell metabolism and selective induction of ex- pression of certain receptors on the surface of the cells of the treated tissue [20] [21] . Among these, sub-types 43, 47 and 70 are overexpressed, and act as chaperones to collagen, and also play a predominant role in the induction of growth factors, such as TGF-β, a key cytokine in the inflammatory and fibrogenetic processes that produce collagen and extracellular matrix [22] [23] . This cascade of events stimulates restoration of metabolic trophism of the vaginal mucosa, which improves its elasticity and moisture, and provides relief from discomfort in menopausal women. The present findings demonstrated that fractional/pixel CO2 laser treatment stimulated tissue remodelling, neocollageno genesis and reconstruction of the trabecular architecture typical of collagen. The thickened epithelial papillae, with enhanced production of glycogen, contributed to improved moisture and objective characteristics of the vaginal mucosa, as expressed in improved VHI-S and histologically evident qualitative and quantitative changes
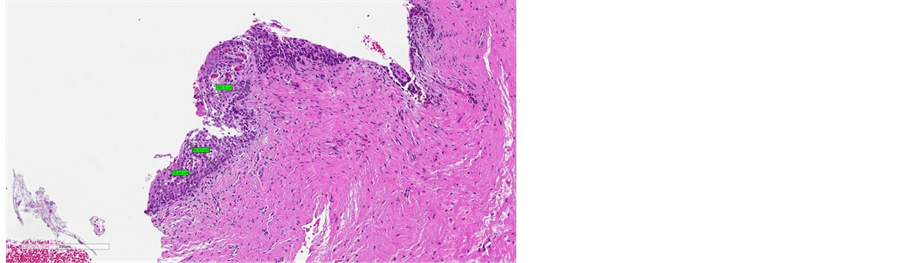
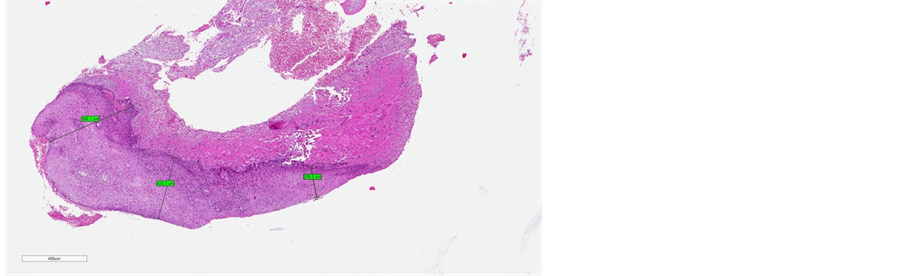
Figure 5. (a) pre-treatment measures (from minimum measure of 79 µm to maximum measure of 103 µm); (b) post-treatment measures (from minimum measure of 200 µm to maximum measure of 560 µm).
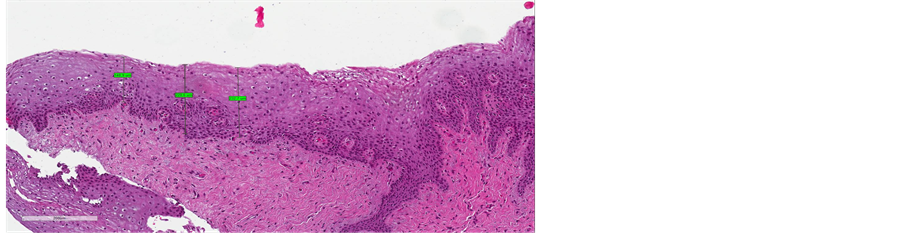
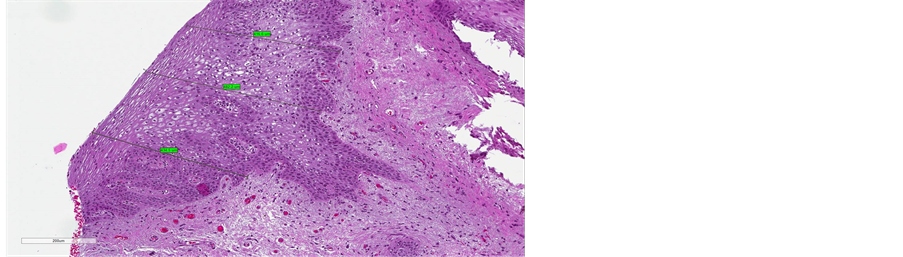
Figure 6. (a) pre-treatment measure (from minimum measure 148 µm to maximum measure of 232 µm); (b) post-treatment measures (from minimum measure of 416 µm to maximum measure of 482 µm).
in vaginal tissue. Overall, the treatment regimen provided effective relief from the predominant GSM symptoms, improved vaginal health and improved control of urination. Future urodynamic studies will be necessary to better quantify these improvements.
The laser therapy applied here induced neo-collagenogenesis, up regulated collagen type 3 expression, and increased epithelial papillae thickness, but due to limitations of the technique the degree of up regulation was not quantifiable. In addition. In addition, a significant enhancement of type III collagen production was observed in the lamina propria following treatment, likely to underlie its improved function, as well as the re-establishment of the physiological vaginal pH, probably due to the microbial lactobacillus flora (Figure 7 Figure 8). No side effects were observed and the procedure was well tolerated and did not require any local or systemic pharmacological or behavioural treatments. Of note, the ideal safety profile reported here can most likely be attributed to the stringent application of the study’s inclusion and exclusion criteria.
Women with surgically-induced menopause benefited from higher treatment efficacy, as compared to those with physiological menopause. The average patient age in the two subcohorts was significantly different, where patients with surgically-induced menopause were a mean 5 years younger than those with physiologic menopause, and the time from menopause was almost 4 years shor- ter compared to those who had experienced physiological menopause (Table 2). This interesting finding suggests that the rejuvenating prospects of fractional CO2 laser therapy on the vaginal wall increase with proximity to onset of meno- pause.
Figure 7. Post-treatment immunohistochemical evalu- ation of type III and IV collagen

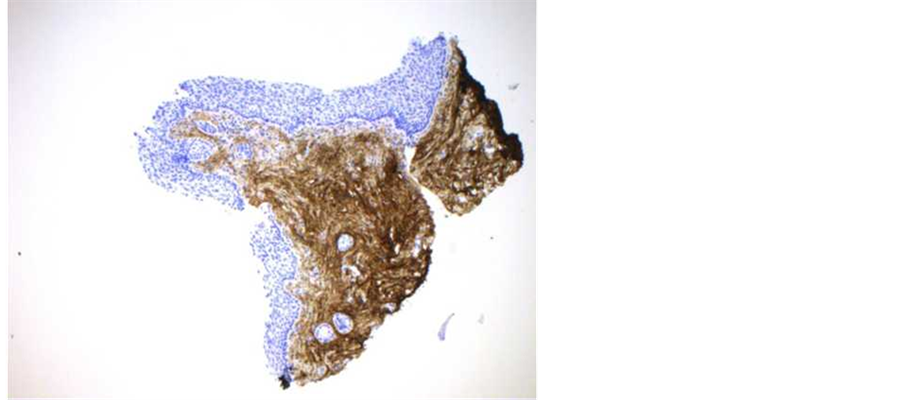
Figure 8. (a)-(b) Evaluation of type III collagen using monoclonal antibody. (a) Vaginal mucosa before treatment. (b) vaginal mucosa after treatment: significant increase in the thickness and staining of the epithelium.
These preliminary results warrant further assessments in a larger sample size and over a longer follow-up period, later to be followed by validation in randomised studies. These studies must consider the longevity of both subjective and objective improvements, as well as the need for maintenance treatments.
5. Conclusion
The fractional/pixel CO2 laser is a minimally invasive precision tool, which provides for a novel, outpatient approach to treat GSM symptoms. The approach is bound to pave the way toward a new, safe and efficacious therapeutic modality for rejuvenation of the vaginal mucosa and improved urinary control. This approach provides particular hope for oncology patients with treatment-induced menopause and subsequent genitourinary atrophy and SUI, for whom hormonal therapy is contraindicated, as well as for women who are mutation carriers (e.g., BRCA1-2 mutations) who suffer from GSM or SUI, for whom hormonal therapy is contraindicated. Further scientific data will be necessary to validate the therapeutic efficacy of the presented laser therapy for genitourinary atrophy, SUI and sexual-dysfunction-related symptoms. Moreover, longer follow-up periods will establish the duration of the treatment effect.
Cite this paper
Pagano, I., Gieri, S., Nocera, F., Scibilia, G., Fraggetta, F., Galia, A., Gioè, M., Pecorino, B. and Scollo, P. (2017) Evaluation of the CO2 Laser Therapy on Vulvo-Vaginal Atrophy (VVA) in Oncological Patients: Preliminary Results. Journal of Cancer Therapy, 8, 452- 463. https://doi.org/10.4236/jct.2017.85039
References
- 1. (2013) Management of Symptomatic Vulvovaginal Atrophy: 2013 Position Statement of The North American Menopause Society. Menopause, 20, 888-902; quiz 3-4.
- 2. Portman, D.J. and Gass, M.L. (2014) Genitourinary Syndrome of Menopause: New Terminology for Vulvovaginal Atrophy from the International Society for the Study of Women’s Sexual Health and The North American Menopause Society. Climacteric, 17, 557-563.
https://doi.org/10.3109/13697137.2014.946279 - 3. Sturdee, D.W. and Panay, N. (2010) Recommendations for the Management of Postmenopausal Vaginal Atrophy. Climacteric, 13, 509-522.
https://doi.org/10.3109/13697137.2010.522875 - 4. Iosif, C.S., Batra, S., Ek, A. and Astedt, B. (1981) Estrogen Receptors in the Human Female Lower Uninary Tract. American Journal of Obstetrics and Gynecology, 141, 817-820.
https://doi.org/10.1016/0002-9378(81)90710-9 - 5. Fadare, O. (2011) Vaginal Stromal Sclerosis: A Distinctive Stromal Change Associated with Vaginal Atrophy. International Journal of Gynecological Pathology, 30, 295-300.
- 6. Nappi, R.E. and Kokot-Kierepa, M. (2010) Women’s Voices in the Menopause: Results from an International Survey on Vaginal Atrophy. Maturitas, 67, 233-238.
- 7. Nappi, R.E. and Kokot-Kierepa, M. (2012) Vaginal Health: Insights, Views & Attitudes (VIVA)—Results from an International Survey. Climacteric, 15, 36-44.
https://doi.org/10.3109/13697137.2011.647840 - 8. Johnston, S.L., Farrell, S.A., Bouchard, C., et al. (2004) The Detection and Management of Vaginal Atrophy. Journal of Obstetrics and Gynaecology Canada, 26, 503-515.
- 9. de Villiers, T.J., Pines, A., Panay, N., et al. (2013) Updated 2013 International Menopause Society Recommendations on Menopausal Hormone Therapy and Preventive Strategies for Midlife Health. Climacteric, 16, 316-337.
https://doi.org/10.3109/13697137.2013.795683 - 10. Ronconi, L. and Galli, M. (2012) MonaLisa TouchTM. In: DEKA, Ed., The Latest Frontier in the Treatment of Vaginal Atrophy, Vol. 2, Scientific Series, September.
- 11. Kaufmann, R. and Hibst, R. (1996) Pulsed Erbium:YAG Laser Ablation in Cutaneous Surgery. Lasers in Surgery and Medicine, 19, 324-330.
https://doi.org/10.1002/(SICI)1096-9101(1996)19:3<324::AID-LSM7>3.0.CO;2-U - 12. Capon, A. and Mordon, S. (2003) Can Thermal Lasers Promote Skin Wound Healing? American Journal of Clinical Dermatology, 4, 1-12.
https://doi.org/10.2165/00128071-200304010-00001 - 13. Dafforn, T.R., Della, M. and Miller, A.D. (2001) The Molecular Interactions of Heat Shock Protein 47 (Hsp47) and Their Implications for Collagen Biosynthesis. Journal of Biological Chemistry, 276, 49310-49319.
https://doi.org/10.1074/jbc.M108896200 - 14. Prignano, F., Campolmi, P., Bonan, P., et al. (2009) Fractional CO2 Laser: A Novel Therapeutic Device upon Photobiomodulation of Tissue Remodeling and Cytokine Pathway of Tissue Repair. Dermatologic Therapy, 22, S8-S15.
https://doi.org/10.1111/j.1529-8019.2009.01265.x - 15. Salvatore, S., Leone Roberti Maggiore, U., Athanasiou, S., et al. (2015) Histological Study on the Effects of Microablative Fractional CO2 Laser on Atrophic Vaginal Tissue: An ex Vivo Study. Menopause, 22, 845-849.
- 16. Abrams, P., Avery, K., Gardener, N. and Donovan, J., ICIQ Advisory Board (2006) The International Consultation on Incontinence Modular Questionnaire: https://www.iciq.net. The Journal of Urology, 175, 1063-1066; Discussion 1066.
- 17. Kaplan, I., Goldman, J. and Ger, R. (1973) The Treatment of Erosions of the Uterine Cervix by Means of the CO2 Laser. Obstetrics & Gynecology, 41, 795-796.
- 18. Jiang, X., Ge, H., Zhou, C., Chai, X. and Deng, H. (2013) The Role of Transforming Growth Factor Beta1 in Fractional Laser Resurfacing with a Carbon Dioxide Laser. Lasers in Medical Science, 29, 681-687.
https://doi.org/10.1007/s10103-013-1383-5 - 19. Verrico, A.K., Haylett, A.K. and Moore, J.V. (2001) In Vivo Expression of the Collagen-Related Heat Shock Protein HSP47, Following Hyperthermia or Photodynamic Therapy. Lasers in Medical Science, 16, 192-198.
https://doi.org/10.1007/PL00011354 - 20. Chen, W.R., Liu, H. and Nordquist, R.E. (2002) Mechanism of Laser Immunotherapy: Role of Immunoadjuvant and Selective Photothermal Laser-Tissue Interaction. Proceedings of SPIE, 4536, 82-89.
- 21. Wang, S., Diller, K.R. and Aggarwal, S.J. (2003) Kinetics Study of Endogenous Heat Shock Protein 70 Expression. Journal of Biomechanical Engineering, 125, 794-797.
https://doi.org/10.1115/1.1632522 - 22. Snoeckx, L.H., Cornelussen, R.N., Van Nieuwenhoven, F.A., Reneman, R.S. and Van Der Vusse, G.J. (2001) Heat Shock Proteins and Cardiovascular Pathophysiology. Physiological Reviews, 81, 1461-1497.
- 23. Yamasaki, A., Tamamura, K., Sakurai, Y., Okuyama, N., Yusa, J. and Ito, H. (2008) Remodeling of the Rat Gingiva Induced by CO2 Laser Coagulation Mode. Lasers in Surgery and Medicine, 40, 695-703.
https://doi.org/10.1002/lsm.20712