Journal of Cancer Therapy
Vol. 4 No. 5 (2013) , Article ID: 33774 , 4 pages DOI:10.4236/jct.2013.45107
Cholangiocarcinoma Arising 38 Years after Surgical Resection of Hepatocellular Carcinoma*
![]()
1Qidong Liver Cancer Institute and Qidong People’s Hospital, Qidong, China; 2Nantong University Liver Cancer Institute and Tumor Hospital of Nantong University, Nantong, China; 3Department of Pharmaceutical Sciences, Eugene Applebaum College of Pharmacy and Health Sciences, Wayne State University, Detroit, USA.
Email: #chenjg@vip.sina.com, #fchen@wayne.edu
Copyright © 2013 Jianguo Chen et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received May 18th, 2013; revised June 16th, 2013; accepted June 23rd, 2013
Keywords: HCC; ICC; Liver Cirrhosis; Cancer Surveillance; Earlier Detection
ABSTRACT
Background: Most of the reports on tumor relapse are recurrence of the same type of tumor after months to few years of a successful initial cancer treatment. It is generally unusual and unexpected that a different type of the second tumor occurs after several decades of the curative treatment of the original tumor. Case Presentation: We report a case of 74-year-old man with intrahepatic cholangiocarcinoma (ICC) diagnosed 38 years after curative resection of hepatocellular carcinoma (HCC). In addition to the uniqueness of longer survival and developed a new type of tumor, both the original HCC and the later occurred ICC were detected through a cancer surveillance program by screening alpha-fetoprotein (AFP) and ultrasonography of the liver for the general population and/or high risk group of people who were asymptomatic. Conclusion: This report provides evidence demonstrating occurrence of new type of tumor following initial curative therapy of the original tumor. In addition, this case report also highlights the importance of cancer surveillance program for earlier detection of the tumors to achieve a remarkably improved prognosis of the cancer patients for a prolonged cancer free survival time.
1. Introduction
Primary liver cancer is the fifth most common cancer in men and the eighth most common cancer in women worldwide. Previous epidemiologic studies have revealed that the incidence rate of liver cancer is much higher in East Asia and sub-Saharan Africa than in North America and most of Europe [1]. This variation in the incident rate of liver cancer is largely resulted from the complex of different risk factors. In countries of East Asia and Africa, primarily infection of hepatitis B virus (HBV) or exposure to aflatoxin B is considered as the major etiological factor of liver cancer, whereas infection of hepatitis C virus (HCV), alcoholic and non-alcoholic liver diseases might be responsible for driving liver cancer in the regions of North America and Europe. The majority of primary liver malignancies are hepatocellular carcinoma
(HCC), which is accounted for more than 90% of liver cancers. In contrast, only about 6% and 2% of liver tumors are intrahepatic cholangiocarcinoma (ICC) and combined HCC and ICC (HCC-ICC), respectively [2].
HCC is the most common cancer in men in some areas of China. In recent years, more than 360,000 new HCC cases diagnosed and about 350,000 patients died from this malignancy annually. The overall one year and five year survival rate of HCC in China is less than 20% and 10%, respectively. Since only few patients are eligible for surgical resection and the ineffectiveness of HCC chemotherapy or radiation therapy, screening of serum alpha-fetoprotein (AFP) in combination with liver ultrasonography for the high risk population, such as HBV carriers and cirrhotic patients, has been confirmed as an important strategy for the early detection and surgical resection of HCC. We had established a regional cancer registration program with emphasis on HCC surveillance since 1970s and screened more than 2 million people since then [3]. In a recent screening of 26,355 people, 64 cases of earlier stage HCC were identified, among which 28 cases were then subjected to curative treatment by surgical resection and 20 cases received transcatheter arterial chemoembolization therapy [4]. Most recently, we re-screened 90 patients who had been survived for more than 10 years after HCC resection and identified a case of ICC from a patient who had been survived for 38 years since the curative HCC resection.
2. Case Presentation
2.1. The First Diagnosis of HCC in 1974
The research project of cancer surveillance program on human population has been approved by the institutional review board of Qidong Liver Cancer Institute. Statements of written consents were obtained from the individuals included in the screening program and follow-up studies. The patient, male, was first diagnosed with HCC on January 8th, 1974 when he was 35 years old (born in March, 1938) and was included in a HCC screening program for general population in Qidong, China. The serum AFP level was large than 1000 unit as determined by haemagglutination assay and then rocket immunoelectrophoresis. Additional laboratory testing did not show any other abnormalities. Radioisotope scanning revealed a well-defined tumor mass 8.5 cm in diameter in the hepatic hilar region. The patient was a farmer, non-smoker and alcohol drinker. He was not aware of any familialassociated liver, gastrointestinal, or lung malignancy.
The patient was hospitalized on June 18th, 1974, in a local hospital for liver tumor and gallbladder resection by surgeon specialists from the Jiangsu Medical Team in Qidong. At laparotomy, a solitary tumor behind the portal hilar structure was found. The tumor showed a well-defined pseudocapsule formed by fibrotic tissue surrounded the tumor and a size of 8.5 × 8.5 × 4.5 cm3. The non-cancerous liver tissue exhibited some scattered cirrhotic nodules. The liver tumor was surgically removed along with an expanded inferior right and left hepatectomies. Pathological and histological examination revealed that the tumor had some segmental structures with interfused nodules and featured with abnormal architecture of thickened hepatic cords. The tumor also showed infiltration of inflammatory cells and necrotic lesions in the central region (Figure 1(A)). The patient was diagnosed as primary HCC with grade II differentiation, chronic hepatitis and mild liver cirrhosis, based on the final report given by pathologist. After surgical resection of the tumor, the patient was fully recovered without chemotherapy, radiation therapy or adjuvant treatment.
2.2. The Diagnosis of ICC in 2012, 38 Years after HCC Resection
Since the last surgical operation to remove the liver tumor in 1974, the patient, now is 74 years old, has been working as a farmer without any physical limitation or symptoms of illness. The patient was subjected to follow-up studies of post-surgery during the past decades and showed normal liver function and serum negative of AFP in several laboratory tests, except serum positives of HBsAg and anti-HBc.
The patient was recruited to an undergoing research project monitoring cancer recurrence by screening serum AFP along with ultrasonography for a group of patients who had been survived for more than 10 years after HCC resection. The patient was presented for this research project on June 7th, 2012. On physical examination, he was an elderly man with proper nutrition and mostly normal physical signs. Superficially, there were no visible signs of jaundice, anemia and febrile. His pulse was 72 beats per minute and blood pressure 140/80 mm·Hg. His chest was clear under X-ray. Other systems were unremarkable.
Although laboratory test showed undetectable level of serum AFP, ultrasonography and CT scan revealed a tumor mass with a diameter of 2.5 cm in the medial segment of left lobe of the liver and dilated intrahepatic biliary ducts (Figure 1(B)). Additional blood test showed marginal increase of CEA (5.75 ng/ml), HBsAg (+), anti-HBc (+) HCV (−), HIV (−). No other abnormalities were noted. The patient was tentatively diagnosed as HCC recurrence and was hospitalized in Qidong Liver Cancer Institute on June 8th, 2012, for scheduling HCC resection.
Surgical operation on this patient was performed on June 14th, 2012. A solid tumor with a size of 3.5 × 2.5 × 3.0 cm3 was seen at the left lobe of the liver. The tumor mass showed gray to gray-white color and compressive growth without notable encapsulation in the hepatic parenchyma. The tumor was removed along with an expanded partial left lobe hepatectomy. Additional pathological evaluation revealed that the tumor has no evident fibrous capsule and exhibited bud-like growth of the cancerous tissues into the surrounding liver tissue that was severely cirrhotic. The tumor also showed variable sized tubular structures, acini formation, papillary configurations and mild desmoplastic reaction. The tumor cells exhibited cord-like growth pattern with variable cellular and nuclear pleomorphism. The majority of cancer cells have a small nucleus and a pale, eosinophilic, or vacuolated cytoplasm. Mucin production was visible on cut surfaces and the luminal sides of the tubular structures (Figure 1(C)). Based on these findings, the patient was diagnosed as ICC in the left liver robe, chronic hepatitis and liver cirrhosis.
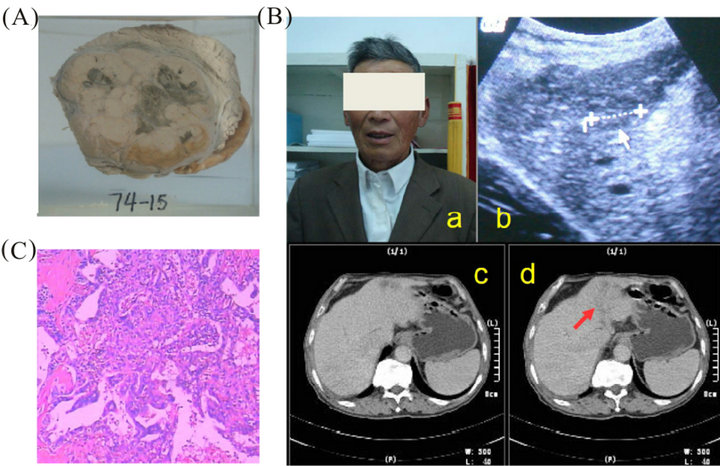
Figure 1. (A) Formaldehyde-fixed HCC specimen from the patient who was subjected to surgical resection of the liver tumor on June 18th, 1974; (B) Panel (a) photo of the patient taken on the day of screening on June 7th, 2012; Panel (b) a tumor mass was detected by ultrasonography; Panels (c) and (d) computed tomography (CT) scan from 2 of the series (00745025) showing location and size of the tumor; (C) Photomicrograph of ICC stained by hematoxylin-eosin (HE). Original magnification: 10 × 10.
The patient was recovered after operation and discharged from the hospital on June 22nd, 2012. No additional chemotherapy or adjuvant treatment was administrated.
3. Conclusions
HCC is one of the most malignant cancers that have the lowest five-year survival rate after diagnosis. The data from population-based cancer registration suggested that the current five-year survival rate of HCC is less than 10% in China or 15% worldwide. In fact, more than 80% of HCC patients died within 6 to 12 months after diagnosis. The lack of earlier detection and effective chemotherapies has long been ascribed to the poorest prognosis of HCC [5]. Accordingly, earlier detection of HCC, such as AFPand ultrasonography-based screening for the high risk population, is pivotal to achieve an improved outcome. The case reported here may provide the strongest support to this notion, which showed that the patient has survived for more than 38 years after a screeningbased earlier detection and the subsequent surgical resection of the HCC.
ICC is considered as a malignant tumor with characteristics of adenocarcinoma that arises from the bile duct epithelium, which accounts for only about 4% - 7% of all liver cancers [6]. The rarity of ICC relative to HCC may simply reflect the fact that the number of cholangiocytes is far less then the number of the hepatocytes in the total population of liver epithelial cells. It was believed that both HCC and ICC are derived from the same bipotential hepatic progenitor cell niches located in the canals of Hering and peribiliary glands of the livers. Indeed, this notion was supported by our recent gene profiling study that indicated a shared molecular signature between higher JNK1 HCC and ICC that showed overlapping gene expression spectrum between them, such as those genes important for self renewal of the progenitor/stem cells and phenotypic identities of the cells, including CD24, SPP1, KRT7, and KRT19 [7,8]. Although a number of studies suggested that HCC and ICC do not share the major risk factors, several lines of evidence indicated presence of common risk factors for both HCC and ICC [9].
To the best of our knowledge, there is no reported case of ICC that occurred several years after HCC resection. The case presented here is not the recurrence of HCC after resection, nor a mixture of HCC and ICC, but rather, a new type of malignant tumor developed following the curative therapy of the previous cancer 38 years ago. It is unclear whether the previous HCC and the later developed ICC caused by the same etiological factors, such as HBV infection and liver cirrhosis. One of the possible mechanisms of the subsequent development of ICC is compensatory proliferation of the biliary epithelium or the bipotential hepatic progenitor cells induced by the neighboring cirrhotic lesions that were consistent after the surgical resection of HCC. It is not unlikely that the cirrhotic cells release paracrine factors, such as Wnt signaling proteins and cytokines to influence the growth of the biliary epithelial cells, progenitor cells or the associated myofibroblast cells [10]. An additional possibility that cannot be ruled out is that the altered biliary duct structure due to previous resection of HCC, gallbladder and partial hepatectomy, may enhance the level of shear stress on hepatobiliary tract, leading to chronic inflammation, proliferation and transformation of the intrahepatic biliary epithelial cells.
Similar to HCC, ICC is a devastating malignancy with very dismal prognosis due to the fact that majority of ICCs are growth aggressively, invasiveness and unresectable when diagnosed. For the resectable ICC, surgical resection of the tumor along with the histologically negative surrounding liver segments is the only existing curative measure. Depending on location and the degree of intrahepatic metastasis, the 5-year disease free survival rate of post-ICC surgery varied from 8% to 47%. Most studies have concluded that chemotherapy of ICC has no benefit in improving survival in either resected or unresected ICC [11]. Because of lack of reliable tumor markers, it is difficult to make earlier detection of ICC, esp., in those asymptomatic patients. Despite this, several circulating proteins can be useful as diagnosis guide, such as the widely used carbohydrate antigen (CA) 19-9 and carcinoembryonic antigen (CEA).
The HCC of this case reported here was detected through cancer screening by serum AFP test for the general population in 1974. Intriguingly, the ICC of the same patient was detected also through a follow-up screening for a high risk population 38 years late by using the same screening tactics in combination of ultrasonography, although this time the serum AFP was negative. Thus, this brief report highlights the importance of screening for either a general population or a high risk population by the mutually compensatory procedures for earlier detection of the tumor and a remarkably prolonged survival of the patients.
4. Author’s Contribution
JGC designed the cancer surveillance program, recruited participants of cancer screening project and data collection; WZL performed ultrasonography and CT scanning; LXW, YXZ, NJW, and YSC performed surgical resection of the tumor and other clinical services; JZ, HWZ and JY participated in the histopathological diagnosis of the patient; FC analyzed all the pathological and clinical data and wrote the manuscript.
5. Acknowledgements
The research projects in FC’s laboratory are supported by Wayne State University Fund 176417, NIH R01 ES01 7217 and NIH R01 ES020137.
REFERENCES
- F. Chen, K. Beezhold and V. Castranova, “JNK1, a Potential Therapeutic Target for Hepatocellular Carcinoma,” Biochimica et Biophysica Acta, Vol. 1796, No. 2, 2009, pp. 242-251.
- I. Ikai, S. Arii, T. Ichida, K. Okita, M. Omata, M. Kojiro, K. Takayasu, Y. Nakanuma, M. Makuuchi and Y. Matsuyama, et al., “Report of the 16th Follow-Up Survey of Primary Liver Cancer,” Hepatology Research, Vol. 32, No. 3, 2005, pp. 163-172. doi:10.1016/j.hepres.2005.04.005
- J. G. Chen, D. M. Parkin, Q. G. Chen, J. H. Lu, Q. J. Shen, B. C. Zhang and Y. R. Zhu, “Screening for Liver Cancer: Results of a Randomised Controlled Trial in Qidong, China,” Journal of Medical Screening, Vol. 10, No. 4, 2003, pp. 204-209. doi:10.1258/096914103771773320
- J. G. Chen and S. W. Zhang, “Liver Cancer Epidemic in China: Past, Present and Future,” Seminars in Cancer Biology, Vol. 21, No. 1, 2011, pp. 59-69. doi:10.1016/j.semcancer.2010.11.002
- T. W. Kensler, G. S. Qian, J. G. Chen and J. D. Groopman, “Translational Strategies for Cancer Prevention in Liver,” Nature Reviews Cancer, Vol. 3, No. 5, 2003, pp. 321-329. doi:10.1038/nrc1076
- C. H. Lee, C. J. Chang, Y. J. Lin, C. N. Yeh, M. F. Chen and S. Y. Hsieh, “Viral Hepatitis-Associated Intrahepatic Cholangiocarcinoma Shares Common Disease Processes with Hepatocellular Carcinoma,” British Journal of Cancer, Vol. 100, No. 11, 2009, pp. 1765-1770. doi:10.1038/sj.bjc.6605063
- Q. Chang, Y. Zhang, K. J. Beezhold, D. Bhatia, H. Zhao, J. Chen, V. Castranova, X. Shi and F. Chen, “Sustained JNK1 Activation Is Associated with Altered Histone H3 Methylations in Human Liver Cancer,” Journal of Hepatology, Vol. 50, No. 2, 2009, pp. 323-333. doi:10.1016/j.jhep.2008.07.037
- F. Chen, S. Li and V. Castranova, “Overlapping Signature Genes between Hepatocellular Carcinoma and Intrahepatic Cholangiocarcinoma,” European Journal of Gastroenterology & Hepatology, Vol. 21, No. 11, 2009, pp. 1320-1321. doi:10.1097/MEG.0b013e32832b2123
- T. M. Welzel, L. Mellemkjaer, G. Gloria, L. C. Sakoda, A. W. Hsing, L. El Ghormli, J. H. Olsen and K. A. McGlynn, “Risk Factors for Intrahepatic Cholangiocarcinoma in a Low-Risk Population: A Nationwide CaseControl Study,” International Journal of Cancer, Vol. 120, No. 3, 2007, pp. 638-641. doi:10.1002/ijc.22283
- F. Chen, “JNK-Induced Apoptosis, Compensatory Growth, and Cancer Stem Cells,” Cancer Research, Vol. 72, No. 2, 2012, pp. 379-386. doi:10.1158/0008-5472.CAN-11-1982
- S. A. Khan, H. C. Thomas, B. R. Davidson and S. D. Taylor-Robinson, “Cholangiocarcinoma,” Lancet, Vol. 366, No. 9493, 2005, pp. 1303-1314. doi:10.1016/S0140-6736(05)67530-7
List of Abbreviations
HCC: hepatocellular carcinoma; ICC: intrahepatic cholangiocarcinoma; AFP: alpha-fetoprotein; HBV: hepatitis B virus.
NOTES
*Competing interests: No any financial or non-financial competing interest to be disclosed by all the authors.
#Corresponding authors.

