Health
Vol.07 No.09(2015), Article ID:59463,8 pages
10.4236/health.2015.79123
The Impact of Hospital Accreditation System: Perspective of Organizational Learning
Yu H. Yan1, Chih M. Kung2*
1Department of Medical Research, Tainan Municipal Hospital, Tainan City, Chinese Taipei
2Department of Information Technology and Communication, Shih Chien University Kaohsiung Campus, Kaohsiung City, Chinese Taipei
Email: *alex@cvig.org
Copyright © 2015 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 3 August 2015; accepted 5 September 2015; published 8 September 2015
ABSTRACT
Objectives: Organizational learning is used to being a very important topic about hospital mana- gement and even is identified as the source of a hospital’s competitive strength. The study tries to explore the correlation between organizational learning and hospital accreditation awareness from the medical institution operation management’s point of view. Methods: We designed the questionnaire based on the cross-section survey, which included a total of 498 hospitals through- out Taiwan as the subjects (1922 copies of questionnaire were distributed, 4 copies per hospital). As a result, 306 returned the questionnaire (995 copies of valid questionnaire), a valid response rate was 49.94%. Then, we conducted the multiple regression analysis. Results: The factors critical to the operations management accreditation awareness include age, hospital ownership, hospital lever and team learning (p < 0.001). The factors critical to the medical care accreditation aware- ness include age, education level and team learning (p < 0.001). The team learning will produce positive effect to the hospital accreditation awareness. Conclusions: The organizational continuous learning may enhance the team learning through hospital accreditation operations to ensure that the medical treatment system may provide safe, valid and reliable healthcare and found the hospitals’ competitive strength.
Keywords:
Hospital Accreditation, Organizational Learning, Medical Care

1. Introduction
Internationally, dating from 1970s, health care accreditation programs and accrediting organizations emerged and developed [1] . Hospital accreditation is an internationally recognized evaluation process used to assess and improve the quality, efficiency, and effectiveness of health care organizations. Simply put, accreditation is based on the premise that adherence to evidence-based standards will produce higher quality health care services in an increasingly safe environment [2] , The Taiwan Joint Commission on Hospital Accreditation and Quality Improvement (TJCHA) began to reform the hospital accreditation system in 2003 to improve health care quality with emphasis on patient-centredness and safety. Hospital accreditation in Taiwan started in 1978. Over the years, the accreditation system has improved the hospital structure significantly. Yet TJCHA realized the urgent need of reforming the accreditation system after the SARS outbreak to focus on process and outcomes [3] .
The new system has revised accreditation standards, survey methods and the surveyors’ system to evaluate the entire process of patient care for better quality and safety [3] - [5] . The accreditation structure is divided into 2 volumes, Operations Management and Medical Care, with a total of 17 chapters and 238 guidelines. In Hospital Operation and Management, the accreditation includes: Hospital Operation Strategy, Employee Management and Supporting System, Human Resource Management, Employee Education & Training, Medical History, Information and Communication Management, Safe Environment and Facility, Patient-Oriented Service and Management, Risk Management, and Emergency Disaster Response. In Medical Care, the accreditation includes: Patient and Family Member Power & Responsibility, Medical Care Quality Management, Medical Care Conduct and Assessment, Special Care Service, Drug Safety, Anesthesia & Surgery, Infection Control, Testing, Pathology and Radiation Operation, Discharge Preparation, and Persistent Care Service [6] .
The hospital accreditation is a tool for quality enhancement. The accreditation process is anticipated to ensure that the medical care system provides safe, effective, and reliable health care [7] [8] , strengthens interdisciplinary team (medical team) effectiveness, promotes capacity-building, professional development, and organizational learning [9] , sustains improvements in quality and organizational performance [10] - [13] , and supports the efficient and effective use of resources in health care services [14] [15] .
The hospital accreditation is part of the organizational learning system. To facilitate the integration of the accreditation mechanism in the fundamental structure and practices of the hospital, the well-planned and persistent accreditation is applied and the outcome- and process-oriented goals were efficiently utilized to link the accreditation outcome and organizational learning goals as the driving force for hospital advancement [16] [17] . The organizational learning includes Promotes professional development and organizational learning [1] [2] [9] [18] - [22] , Stimulates sustainable quality improvement efforts and continuously raises the bar with regard to quality improvement initiatives, policies, and processes [1] [9] [13] [23] - [26] .
Theorists of organization learning believe that new knowledge and ability may be gained through organizational learning and the organizational behavior may be improved accordingly [27] . Organizational learning is defined as that all of the members in an organization dedicated to learning and sharing with each other the experience generated by themselves or the organization when performing their functions. This improves their personal or organizational behavior [28] - [30] , so as to enable employees to achieve the entire organizational learning by self transcendence or team learning [31] . Therefore, in order to achieve the shared vision, it is necessary to inspire employees’ competence and specialty to gather the organization members’ competence and common agreement and to work hard for the organization’s permanent objectives through the teamwork learning mechanism and sharing of resources among the organization members [32] .
In the recent years, the topic about organizational learning is being valued increasingly, and even identified as the source of a hospital’s competitive strength. Notwithstanding, in this regard, there are still few empirical studies conducted from the point of view of a hospital organization domestically or overseas. The study hopes to comprehend the intention of the hospital accreditation system toward organizational learning more profoundly, in order to provide the governments, hospital operation management with a more macroscopic point of view toward the policies dedicated to boosting organizational learning. The study is intended to explore the correlation between the organizational learning and hospital accreditation awareness. In summary, there are two specific research questions in this research:
1) What is the effect of organizational learning and Operations Management?
2) What is the effect of organizational learning and Medical Care?
2. Methods
2.1. Participants
The Study collected the data through a structural questionnaire designed and based on the cross-section survey, which included the hospitals throughout Taiwan as the subjects. According to the statistic data published by Ministry of Health and Welfare in 2011, there were a total of 498 hospitals throughout the nation. The questionnaire was distributed to the hospitals throughout the nation, and the interviewees were the hospital employees in the areas of medical treatment, medical technology, nursing and administration. The questionnaire was sent to each hospital in the form of official document, i.e. 4 copies per hospital. A total of 1992 copies of questionnaire were distributed. The interviewees of the questionnaire must be the subjects included in the Study and the hospital employees (including physicians, registered nurses, pharmacists, clinical laboratory examiners, radiologists and executive officers). As a result, 306 hospital returned the questionnaire, and 995 copies of the returned questionnaire were valid, i.e. a valid response rate of 49.94% (995 divided by 1922 equals 49.94%).
The authors did extra analysis to check the small sample concern. According to Dillman the number of sample size can be estimated by the following formula:
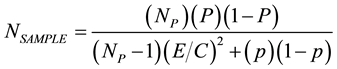
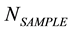 means the number of sample size; NP means the number of population size; E means tolerance error; C means Z value (=1.96) of 95% confidence interval; p, 1 − p means population variance. Under the consideration of normal distribution and fitting expected characteristic, the maximum population variance is 50%. According to the above formula, the minimum standard of sample size is 322. The number of our sample is 995. The result (995) is over the minimum standard (322). Hence, the number of sample is acceptable in this study.
means the number of sample size; NP means the number of population size; E means tolerance error; C means Z value (=1.96) of 95% confidence interval; p, 1 − p means population variance. Under the consideration of normal distribution and fitting expected characteristic, the maximum population variance is 50%. According to the above formula, the minimum standard of sample size is 322. The number of our sample is 995. The result (995) is over the minimum standard (322). Hence, the number of sample is acceptable in this study.
The questionnaire included a goodness-of-fit test of hospital level and hospital location. The test result showed that p values of the hospital level and hospital location were both more than 0.11. Apparently, there was no significant error between the sample and population. Meanwhile, with respect to the nonresponse error, the Study adopted the suggestion from Armstrong and Overton [33] , and used the Independent-Samples T Test and Chi-square Test to test the error between the questionnaires responded by the hospitals successively. The test result showed no significant statistic error (p > 0.19). With respect to the common method variance, the Study applied Harman’s one-factor test. The test result showed that the largest variance factor could only afford to explain 17% of the variance. Apparently, the common method variance in the questionnaire was minor.
2.2. Data Analysis
For the current study, descriptive and regression analyses were conducted in 2009 using SPSS 18.0. Descriptive analysis compared proportions of available characteristics with number of completed. Study participants were more often public hospitals (52.6%) or proprietary hospitals (36.2%), Regional hospitals (58.3%), female (83.2%), aged 31 to 40 years (43.6%), nursing department (49.5%), college (54.7%) or junior college (29.7%) (Table 1).
The construct about organizational learning and hospital accreditation awareness referred to herein was developed based on scholars’ past theories and scale. Therefore, the Study applied the confirmatory factor analysis (CFA) to test the construct validity and composite reliability. After completion of the CFA, we tested the various effects of hospital accreditation awareness through the regression analysis. In order to avoid excessive questions in the questionnaire resulting in interruption in the goodness-of-fit of measurement model, the Study conducted the test through 22 questions including Personal Mastery (X1), Team Learning (X2) and Building Shared Vision (X3) when designing the questions based on the original construct, and tested the hospital accreditation awareness through 45 questions including Operations Management and Medical Care. The other fit statistics indicated good fit as GFI = 0.785, AGFI = 0.764, RMSEA = 0.060, CFI = 0.886, IFI = 0.886, NNFI = 0.879 and Norm-chi = 4.426. Table 2 shows that the CR value of Building shared vision was only 0.2957 and average variance extracted (AVE) 0.1795, the lowest. According to the suggestion from Fornell & Larcker [34] , if the CR value was more than 0.60 and AVE higher 0.50, it meant that the internal consistency reliability of the model was good. Therefore, the Study deleted the option for Building shared vision, and after that, the GFI of the measurement model was 0.794. Therefore, its internal consistency reliability was held acceptable.
For the convergent validity, the loads of the questions about organizational learning or hospital accreditation awareness all attained the statistical significant level. Apparently, the measurement model has good convergent validity. For the discriminant validity, the Study conducted the χ2 difference test. According to the test result, when the coefficient for the organizational learning and hospital accreditation awareness was set as 1, the
Table 1. Participant demographics (n = 955).
Table 2. CR, AVE & Inter-construct correlations.
Note: ***p < 0.001, **p < 0.01, *p < 0.05.
chi-square test value increased from 58.3 to 79.2, and the chi-square difference 20.9, more than 3.84. Apparently, the discriminant validity of the organizational learning and hospital accreditation awareness was held acceptable. Further, the CR of organization learning and hospital accreditation awareness was also held good.
3. Results
The Study conducted the multiple regression analysis on variables about the effect of organizational learning and Operations Management Accreditation Awareness. The analysis result showed that after controlling the other variables, the Study forecast that R2 of Operations Management regression model attained 49.8% and F = 58.210, p < 0.001, reflecting the statistical significant difference. The factors of significant difference included Age, Hospital Ownership, Hospital Level and Team learning. The level of awareness of hospital employees more than 50 years old was more than that of hospital employees less than 30 years old (β = 0.064, t = 2.448, p < 0.01). The level of hospital management accreditation awareness of a private hospital was more than that of a public hospital (β = 0.122, t = 4.699, p < 0.001). The level of hospital management accreditation awareness of a district hospital was lower than that of a regional hospital (β = −0.065, t = −2.341, p < 0.01). The team learning and hospital management accreditation awareness showed significant positive correlation (β = 0.626, t = 23.806, p < 0.01). There was no significant primary effect of Educational level, Department and Personal Mastery toward the hospital management accreditation awareness, and β value failed to attain the statistical significant difference (p > 0.05).
The Study conducted the multiple regression analysis on the variables to forecast the effect of organizational learning and Medical Care Accreditation Awareness. R2 of the regression model attained 39.58% and F = 38.316, p < 0.001, reflecting the statistical significant difference. The factors of significant difference included Age, Education Level and Team learning. The level of medical care accreditation awareness of employees more than 41 years old was more than that of employees less than 30 years old (β = 0.083, 0.095; t = 2.690, 3.326; p < 0.01). The level of medical care accreditation awareness of junior college was lower than that of college (β = −0.062, t = −2.244, p < 0.01). The team learning and medical care accreditation awareness showed significant positive correlation (β = 0.552, t = 19.105, p < 0.001). There was no significant primary effect of Department, Hospital Ownership, Hospital level and Personal Mastery toward the medical care accreditation awareness, and β value failed to attain the statistical significant difference (p > 0.05, see Table 3).
4. Discussion
Prior research shows that teams are effective vehicles for organizational learning [35] [36] . Thus, increasingly, hospitals-including those we studied-use multidisciplinary teams to implement new practices [37] [38] . The team learning literature examines how such teams create organizational learning by improving their work practices [39] [40] .
The Study analyzed and certified the correlation between organizational learning and hospital accreditation awareness, and concluded that the hospital accreditation awareness may be raised through team learning. Such conclusion matched the study of Wu [41] , which believed that the organizational learning value derived from medical care might achieve the purpose of upgrading the medical treatment quality. The stronger organization learning is, the more is it likely to integrate with the hospital accreditation objectives and promote the professional development [1] [2] [9] [18] - [23] . The study of Hirose, Imanaka, Ishizaki, Evans [42] also believed that the medical team learning cohesion could mitigate the possibility of adverse events in the medical care. Reeve & Peerbhoy [43] indicated that team learning could promote the awareness toward organizational learning and hospital accreditation. We might find that though the current medical treatment environment and social, educational and political factors produce much pressure on hospital employees, they are still able to integrate with the hospital accreditation objectives planned by the government through complete team learning.
According to the study results, significant differences existed different ages and education levels toward the accreditation awareness. The awareness of the elder (>50 years old) is higher than that of the younger (<30 years old). The medical care accreditation awareness of college is higher than that of junior college. This result matches that of the study conducted by Chen [8] to explore the hospital accreditation criteria under the new system and execution of the accreditation operation, which believed that such demographic characteristics as age and education level would affect the execution of accreditation operation significantly. The study of Shih [44] also believed that differences existed in organizational learning by age and education level. The reason might be
Table 3. Organizational learning and hospital Accreditation awareness were analyzed.
Note: ***p < 0.001, **p < 0.01, *p < 0.05.
that hospital employees would have different opinion toward their working environment or the hospital accreditation policy to be followed by them following the increase in their age and work experience. More experienced employees would have stronger motive to have team learning. Since the hospital accreditation was forced in Taiwan, hospital employees have kept learning with their peers and their identification with the accreditation has been raised gradually. The study result showed that age, education level and team learning are important factors critical to the hospital accreditation, which is one of the contributions generated by the Study.
Further, the awareness of hospital management accreditation of a private hospital is higher than that of a public hospital, and the awareness of hospital management accreditation of a regional hospital is higher than that of a district hospital. This result matches the relevant study results in Taiwan, reflecting the significant difference in hospital administration by hospitals under different jurisdictions. This matches the concept about agency theory, holding that the public hospital’s management mechanism is more lenient because of lack of incentives and, therefore, its team learning is weaker. In addition, the Study result is also similar to the study of Chen [45] , which believed that there was significant positive correlation between the team learning and organizational characteristic level. The awareness of a larger scale hospital is higher than that of a smaller scale hospital. In the studies related to the medical treatment industry in Taiwan, there is no literature analyzing the organizational learning in hospitals. From the hospital employees’ point of view and based on the hospital accreditation awareness, the empirical result showed that the hospital accreditation awareness varies depending on Hospital level and Hospital Ownership, which are important factors affecting the organizational learning, and also one of the contributions generated by the Study.
The medical care is the essence of a hospital’s operation, which has been expressly disclosed in the hospital accreditation benchmarks. The management shall comply with the hospital’s purpose, vision and objective, and draft plans and strategies to form the culture for pursuing patients’ safety and medical care quality and to establish the patient’s safety and quality promotion and management mechanism and provide patients with the medical care that they really need and to avoid wasting the health care. Therefore, the management should not deviate from the thought and requirement about quality, and the ultimate purpose of quality management is intended to upgrade the hospital management’s performance. The both are indeed complementary for each other. The empirical result showed that there was some correlation between organization learning and hospital accreditation awareness. It may not only promote the dialogue with theories but also help the organization explore important issues and, therefore, meets the need for hospital accreditation reform. Finally, the hospital accreditation shall not be only a temporary organizational behavior. It shall explore the important organizational issues through the focused study, execution and application, and feed the accreditation result back to the hospital’s entire objectives, to enable the continuing learning to be the power of hospital accreditation to boost the upgrading of quality and upgrade the effect of organizational learning and seek competitive strength.
5. Limitations of the Study
The study still tends to collect data from the questionnaire completed by hospital employees. Though all questions in the questionnaire were supported by theories and they went through reliability and validity tests, the study still failed to collect objective data. We suggest that if an in-depth interview with hospitals may be conducted in the future, the subjective and objective diversified indicators may be attended simultaneously to help measure the approach of organizational learning and organization learning ability. This would provide more complete analysis and more plentiful discoveries.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interests with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Tainan municipal hospital funding for the conduct of this study.
Cite this paper
Yu H.Yan,Chih M.Kung, (2015) The Impact of Hospital Accreditation System: Perspective of Organizational Learning. Health,07,1081-1089. doi: 10.4236/health.2015.79123
References
- 1. Greenfield, D. and Braithwaite, J. (2008) Health Sector Accreditation Research: A Systematic Review. International Journal for Quality in Health Care, 20, 172-183.
http://dx.doi.org/10.1093/intqhc/mzn005 - 2. Pomey, M.P., Fran?ois, P., Contandriopoulos, A.P., Tosh, A. and Bertrand, D. (2005) Paradoxes of French Accreditation. Quality & Safety in Health Care, 14, 51-55.
http://dx.doi.org/10.1136/qshc.2004.011510� - 3. Wung, C.H. (2008) The Reform of the Hospital Accreditation System in Taiwan. World Hosp Health Serv., 44, 14-18.
- 4. Wang, J.W., Yeh, T.F. and Tseng, K.Y. (2003) The Meta-Analysis for the Trend of Hospital Accreditation in Taiwan. Chung Shan Medical Journal, 14, 513-522. (Original work published in Chinese)
- 5. Wei, Y., Chung, K.P. and Cheng, S.H. (2005) The Evolution of Healthcare Quality Assessment: From Accreditation to Report Card System. Taiwan Journal of Public Health, 24, 275-283. (Original work published in Chinese)
- 6. Chiu, S.H., Chung, H.J. and Huang, L.J. (2011) Reform Direction and Preliminary Results of the 2011 Edition of the Hospital Accreditation Standards. Journal of Healthcare Quality, 5, 58-62. (Original work published in Chinese)
- 7. Su, C.H., Tsai, A. and Wang, Z.M. (2008) The Application of Project Management in the Hospital Accreditation Early. Journal of Project Management and System Engineering, 3, 1-16. (Original work published in Chinese)
- 8. Chen, L.H. and Tsai, C.Y. (2009) External Audit of Hospital Facilities—With the ISO 9001 Quality Management System and Hospital Accreditation as Examples. St. Joseph’ Hospital Medical & Nursing Journal, 3, 38-42. (Original work published in Chinese)
- 9. Lanteigne, G. (2009) Case Studies on the Integration of Accreditation Canada’s Program in Relation to Organizational Change and Learning: The Health Authority of Anguilla and the Ca’Focella Ospetale di Treviso. Doctorat en administration des services de santé: Faculté de médicine, Université de Montréal. Montréal, QC.
- 10. Pomey, M.P., Lemieux-Charles, L., Champagne, F., Angus, D., Shabah, A. and Contandriopoulos, A.P. (2010) Does Accreditation Stimulate Change? A Study of the Impact of the Accreditation Process on Canadian Health Care Organizations. Implementation Science, 5, 31-44.
http://dx.doi.org/10.1186/1748-5908-5-31 - 11. Simons, R., Kasic, S., Kirkpatrick, A., Vertesi, L., Phang, T. and Appleton, L. (2002) Relative Importance of Designation and Accreditation of Trauma Centers during Evolution of a Regional Trauma System. The Journal of Trauma, 52, 827-833.
http://dx.doi.org/10.1097/00005373-200205000-00002 - 12. Shaw, C.D. (2003) Evaluating Accreditation. International Journal for Quality in Health Care, 15, 455-456.
http://dx.doi.org/10.1093/intqhc/mzg092 - 13. El-Jardali, F., Jamal, D., Dimassi, H., Ammar, W. and Tchaghchaghian, V. (2008) The Impact of Hospital Accreditation on Quality of Care: Perception of Lebanese Nurses. International Journal for Quality in Health Care, 20, 363-371.
http://dx.doi.org/10.1093/intqhc/mzn023 - 14. Wiebe, V.A. and Hoskins, S. (2010) Accountability, Accreditation, and Quality in Health Care. Qmentum Quarterly, 4, 10-13.
- 15. Martin, L.A., Neumann, C.W., Mountford, J., Bisognano, M. and Nolan, T.W. (2009) Increasing Efficiency and Enhancing Value in Health Care. Institute for Healthcare Improvement, Cambridge, MA.
- 16. Cousins, J.B., Goh, S., Clark, S. and Lee, L. (2004) Integrating Evaluative Inquiry into the Organizational Culture: A Review and Synthesis of the Knowledge Base. Canadian Journal of Program Evaluation, 19, 99-141.
- 17. Owen, J.M. (2007) Program Evaluation: Forms and Approaches. 3rd Edition, Guilford, New York.
- 18. Pagliarulo, M.A. (1986) Accreditation: Its Nature, Process, and Effective Implementation. Physical Therapy, 66, 1114-1118.
- 19. Baldi, G., Burani, M., Ghirelli, L. and De Pietri, S. (2000) Certification of an Emergency Department According to UNI EN ISO 9002 Criteria. European Journal of Emergency Medicine, 7, 61-66.
http://dx.doi.org/10.1097/00063110-200003000-00012 - 20. Gluck, J.C. and Hassig, R.Z. (2001) Raising the Bar: The Importance of Hospital Library Standards in the Continuing Medical Education Accreditation Process. Bulletin of the Medical Library Association, 89, 272-276.
- 21. Newhouse, R.P. (2006) Selecting Measures for Safety and Quality Improvement Initiatives. The Journal of Nursing Administration, 36, 109-113.
http://dx.doi.org/10.1097/00005110-200603000-00002 - 22. Touati, N. and Pomey, M.P. (2009) Accreditation at a Crossroads: Are We on the Right Track? Health Policy, 90, 156-165.
http://dx.doi.org/10.1016/j.healthpol.2008.09.007 - 23. Chen, J., Rathore, S.S., Radford, M.J. and Krumholz, H.M. (2003) JCAHO Accreditation and Quality of Care for Acute Myocardial Infarction. Health Affairs, 22, 243-254.
http://dx.doi.org/10.1377/hlthaff.22.2.243 - 24. Leatherman, S., Berwick, D., Iles, D., Lewin, L.S., Davidoff, F., Nolan, T. and Bisognano, M. (2003) The Business Case for Quality: Case Studies and an Analysis. Health Affairs, 22, 17-30.
http://dx.doi.org/10.1377/hlthaff.22.2.17 - 25. Baskind, R., Kordowicz, M. and Chaplin, R. (2010) How Does an Accreditation Programme Drive Improvement on Acute Inpatient Mental Health Wards? An Exploration of Members’ Views. Journal of Mental Health, 19, 405-411.
http://dx.doi.org/10.3109/09638230903531118 - 26. Peer, K.S. and Rakich, J.S. (2000) Accreditation and Continuous Quality Improvement in Athletic Training Education. Journal of Athletic Training, 35, 188-193.
- 27. Fiol, C.M. and Lyles, M. (1985) Organizational Learning. Academy of Management Review, 10, 803-813.
- 28. Mulholland, P., Zdrahal, Z., Domingue, J., Hatala, M. and Bernardi, A. (2001) A Methodological Approach to Supporting Organizational Learning. International Journal of Human-Computer Studies, 55, 337-367.
http://dx.doi.org/10.1006/ijhc.2001.0494 - 29. Chou, S.W. (2003) Computer Systems to Facilitating Organizational Learning: IT and Organizational Context. Expert Systems with Applications, 24, 273-280.
http://dx.doi.org/10.1016/S0957-4174(02)00155-0 - 30. Lopez, S.P., Peon, J.M.M. and Ordas, C.J.V. (2005) Organizational Learning as a Determining Factor in Business Performance. The Learning Organization, 12, 227-245.
http://dx.doi.org/10.1108/09696470510592494 - 31. Sinkula, J.M., Baker, W.E. and Noordewier, T. (1997) A Framework for Market-Based Organizational Learning: Linking Values, Knowledge, and Behavior. Journal of the Academy of Marketing Science, 25, 305-318.
http://dx.doi.org/10.1177/0092070397254003 - 32. Lin, L.J. and Lee, H.L. (2008) Application of the Balanced Scorecard System in Healthcare Management in the Community Health Care Center. Taipei City Medical Journal, 5, 516-523.
- 33. Armstrong, J.S. and Overton, T.S. (1977) Estimating Nonresponse Bias in Mail Surveys. Journal of Marketing Research, 14, 396-402.
http://dx.doi.org/10.2307/3150783 - 34. Argote, L., Gruenfeld, D. and Naquin, C. (2001) Group Learning in Organizations. In: Turner, M.E., Ed., Groups at Work: Advances in Theory and Research, Lawrence Erlbaum Associates, Mahwah, 369-411.
- 35. Fornell, C. and Larcker, D.F. (1981) Evaluating Structural Equation Models with Unobservable Variables and Measurement Error. Journal of Marketing Research, 18, 39-50.
http://dx.doi.org/10.2307/3151312 - 36. Guzzo, R.A. and Dickson, M.W. (1996) Teams in Organizations: Recent Research on Performance and Effectiveness. Annual Review of Psychology, 47, 307-338.
http://dx.doi.org/10.1146/annurev.psych.47.1.307 - 37. Horbar, J.D., Rogowski, J., Plesk, P., Delmor, P., Edwards, W.H., Hocker, J., Kantak, A.D., Lewallen, P., et al. (2001) Collaborative Quality Improvement for Neonatal Intensive Care. Pediatrics, 107, 14-22.
http://dx.doi.org/10.1542/peds.107.1.14 - 38. Uhlig, P.N., Brown, J., Nason, A.K., Camelio, A., Kendall, E. and John, M. (2002) Eisenberg Patient Safety Awards. System Innovation: Concord Hospital. The Joint Com-mission Journal on Quality and Patient Safety, 28, 666-672.
- 39. Edmondson, A.C. (2002) The Local and Variegated Nature of Learning in Organizations: A Group-Level Perspective. Organization Science, 13, 128-146.
http://dx.doi.org/10.1287/orsc.13.2.128.530 - 40. Reagans, R., Argote, L. and Brooks, D. (2005) Individual Experience and Experience Working Together: Predicting Learning Rates from Knowing Who Knows What and Knowing How to Work Together. Management Science, 51, 869-881.
http://dx.doi.org/10.1287/mnsc.1050.0366 - 41. Wu, P.Y. (2013) The Relationship among Training of Nursing Staff, Organizational Learning and Quality of Nursing Care for Psychiatric Hospital Nurse. Unpublished Master’s Thesis, AISA University Department of Business Administration, Taichung City. (Original work published in Chinese)
- 42. Hirose, M., Imanaka, Y., Ishizaki, T. and Evans, E. (2003) How Can We Improve the Quality of Health Care in Japan? Learning from JCQHC Hospital Accreditation. Health Policy, 66, 29-49.
http://dx.doi.org/10.1016/S0168-8510(03)00043-5 - 43. Reeve, J. and Peerbhoy, D. (2007) Evaluating the Evaluation: Understanding the Utility and Limitations of Evaluation as a Tool for Organizational Learning. Health Education Journal, 66, 120-131.
http://dx.doi.org/10.1177/0017896907076750 - 44. Shih, H.Y. (2010) A Study of Organizational Learning and Teacher Career Development in Prim School. Chia-Nan Annual Bulletin, 36, 448-464. (Original Work Published in Chinese)
- 45. Chen, Y. (2011) An Exploration of Taiwan Health Care Organizations Perceived Learning Organization on Perceived Organizational Innovation and Organizational Performance. Unpublished Master’s Thesis, I-Shou University, Kaohsiung City. (Original work published in Chinese)
NOTES

*Corresponding author.


