Health
Vol. 4 No. 2 (2012) , Article ID: 17479 , 6 pages DOI:10.4236/health.2012.42011
Correlation between waist circumference and other factors in menopausal women in Thailand*
![]()
Menopause Clinic, Department of Obstetrics and Gynecology, Faculty of Medicine, Chiang Mai University, Chiang Mai, Thailand; #Corresponding Author: spongsat@mail.med.cmu.ac.th
Received 26 September 2011; revised 19 November 2011; accepted 29 November 2011
Keywords: Waist Circumference; Hip Circumference; Metabolic Syndrome; Modified National Cholesterol Education Program Adult Treatment Panel III
ABSTRACT
Objective: To find the correlation between waist circumference and other factors such as lipid profiles, fasting blood glucose and blood pressure in healthy menopausal women attending menopause clinic. Material and Methods: A cross sectional study was carried out at the Menopause clinic, Faculty of Medicine, Chiang Mai University, Thailand. Four-hund-red healthy menopause women who had no medication for hypertension, dyslipidemia, diabetes mellitus and other medical conditions were enrolled. Waist circumference, hip circumference, body weight, height, blood pressure were measured and their blood samples were taken for lipid profiles and fasting blood glucose level after 12 hours fasting. Results: The mean age of participants was 53.4 ± 5.8 years. Mean waist and hip circumference were 76.2 ± 8.0 and 95.9 ± 6.7 cm, respectively. Mean body mass index was 23.3 ± 3.1 kg/m2. Positive correlations were found between waist circumference and other factors: triglyceride level, fasting blood glucose and blood pressure. There was a negative correlation between waist circumference and HDL-Cholesterol level. The prevalence of metabolic syndrome among participants by modified National Cholesterol Education Program Adult Treatment panel III (NCEP ATP-III) with Asian waist circumference was 21.0%. Conclusion: Waist circumference had a positive correlation with triglyceride level, fasting blood glucose and blood pressure and a negative correlation with HDL-C.
1. INTRODUCTION
Similar to waist circumference (WC), blood pressure (BP), fasting blood glucose (FBG), triglyceride (TG) and HDL cholesterol (HDL-C) is one of the factors used in the diagnosis of metabolic syndrome (MS).Waist circumference measurement is a simple method at no cost while waist hip ratio (WHR) reflects the fat distribution and can predict the MS and other cardiovascular risks. However WHR is more difficult than WC measurement.
Currently MS is more frequently diagnosed because of increasing concern of this problem, the lifestyle change and more aging population. Metabolic syndrome patients carry a higher risk for cardiovascular disease and diabetes mellitus and also for a mortality rate associated with these causes [1,2].
The prevalence of MS is higher when women going through menopausal period [3,4]. However, at the present there is a trend that both men and women of all age group have abnormal cholesterol level and more abdominal obesity [5].
The criteria for diagnosis of MS varies due to the definition (modified National Cholesterol Education Program Adult treatment Panel III: modified NCEP ATP-III or International diabetes federation: IDF criteria) including WC, BP, FBG, TG and HDL-C. Both criteria share the common issues for WC (≥80 cm for Asian women), high BP (BPs ≥ 130 mmHg or BPd ≥ 85 mmHg or on drug treatment ), TG ≥ 150 mg/dL, FBG ≥ 100 mg/dL and HDL-C < 50 mg/dL in women or on drug treatment. Diagnosis of MS by modified NCEP ATP-III requires at least 3 of 5 parameters [6] and by IDF is WC in combination with 2 of 4 parameters [7].
The prevalence of dyslipidemia in Asian is gradually increased including Thai population. In the menopausal transition more dyslipidemia is detected. The previous report of the prevalence of dyslipidemia in Thai menopausal women was very high (TC ≥ 200 mg/dL 91.25%, LDLC ≥ 190 mg/dL 48.75%, TG ≥ 150 mg/dL 10% and HDL –C < 50 mg/dL 38.75% ) [8].
Since WC is a simple method to reflect the central obesity and one of the criteria for diagnosis of MS, many authors recommend its use to predict the risk and give the advice for patients. However, there is a limited number of study in menopausal women concerning the correlation between WC and lipid profile, FBG and BP.
The aim of the present study was to find the correlation between WC, and also WHR, and other metabolic profiles such as lipid profiles, FBG and BP. A positive correlation with these parameters may lead to its use to predict the risk factors for MS. As it is simple with no cost, WC can be applied on a wide scale to promote health in mass population.
2. MATERIALS AND METHODS
All women attending menopause clinic at Department of Obstetrics and Gynecology, Faculty of Medicine, Chiang Mai University were recruited. Participants were 400 women with menopausal symptoms age at least 40 years old with no medication for diabetes mellitus, hypertension, dyslipidemia, autoimmune disease and other medical problems. Participants included both non-hormone use (no hormone use before or discontinue hormone for at least 6 months before enrollment, N 200) and hormone use (currently under hormone therapy, N 200). Participants were measured for body weight, height, WC, HC and BP with written inform consent. Waist hip ratio (WHR) and BMI were then calculated.
All anthropometry was measure by trained author (KS) with standard technique. Body weight and height was measure by standard equipment. Waist circumference was measure with plastic tape at midway between the lower costal margin and the iliac crest while women is standing without clothes at this region. Hip circumference was measure at the hip level at the widest part of buttocks without excess clothes. All parameters were then calculated such as BMI, WHR.
Venous blood sample was also taken for FBG and lipid profiles (TG, TC, LDL-C and HDL-C) after 12 hours fasting. Blood was analyzed by the Central Laboratory of the hospital. All assays were performed using automatic machine Unicel DXC 800 Synchrone clinical system, Beckman Couter Inc. Fasting blood glucose levels were assayed using glucose oxidase method, while TC with cholesterol oxidase, esterace, peroxidase method, TG with enzymatic method and LDL-C, HDL-C with direct measure method.
The sample size was calculated base on the prevalence of dyslipidemia in Thai menopausal women. The author predicts the difference not more than 10% and then the sample size was calculated to be 138 women per group (for non hormone and hormone use).Statistic analysis was performed by SPSS version 14.0 program. Descriptive data was presented by mean ± SD or percent. Student t test was used to compare the difference of characteristics between groups. Pearson correlation was performed to test the correlation between WC, WHR, age, BW and BMI with the following parameters such as BP, FBG and lipid profiles. Chi square test was used to test the difference between groups in terms of BP, FBG and lipid profiles.
The present study was approved by the research ethic committee of the Faculty of Medicine, Chiang Mai University, Chiang Mai, Thailand.
3. RESULTS
The characteristics of all participants are presented in Table 1. Mean age of all participants was 53.4 ± 5.8 years. Mean waist and hip circumference were 76.2 ± 8.0 and 95.9 ± 6.7 cm, respectively. Mean BMI was 23.3 ± 3.1 kg/m2. Systolic and diastolic hypertension were found in 36.8% and 17.8% of participants, respectively. The prevalence of hypertriglyceridemia (≥150 mg/dL), hypercholesterolemia (≥200 mg/dL), high LDL-C (≥130 mg/dL) and low HDL-C (<50 mg/dL) were 18.3%,73.3%, 54.8% and 35.0%, respectively. Among participants undergone hormone therapy, mean duration of hormone use was 52.1 ± 47.5 months. Table 2 compares the characteristics of participants classified by WC at cut-off level at 80 cm and by WHR at cut-off level at 0.8. Age and TC were not different between groups classified by WC. While BMI, BP, FBG, TG, LDL-C and HDL-C were significantly different between groups. All parameters were higher in participants with WC ≥ 80 cm except HDL-C was vice versa. Table 2 also demonstrates the characteristics of participants classified by WHR. Age, BP and TC levels were not significant different between groups, while BMI, FBG, TG, LDL-C and HDL-C were significantly different. All parameters, except HDL-C, were higher in the group of WHR ≥ 0.8.
Table 3 represents the Pearson correlation between WC, WHR, age, body weight, BMI with the following parameters such as BP, FBG and lipid profiles. Waist circumference had the positive correlation with BP (both systolic and diastolic), FBG and TG and the negative correlation

Table 1. Characteristics of all participants (Mean ± SD): N 400.
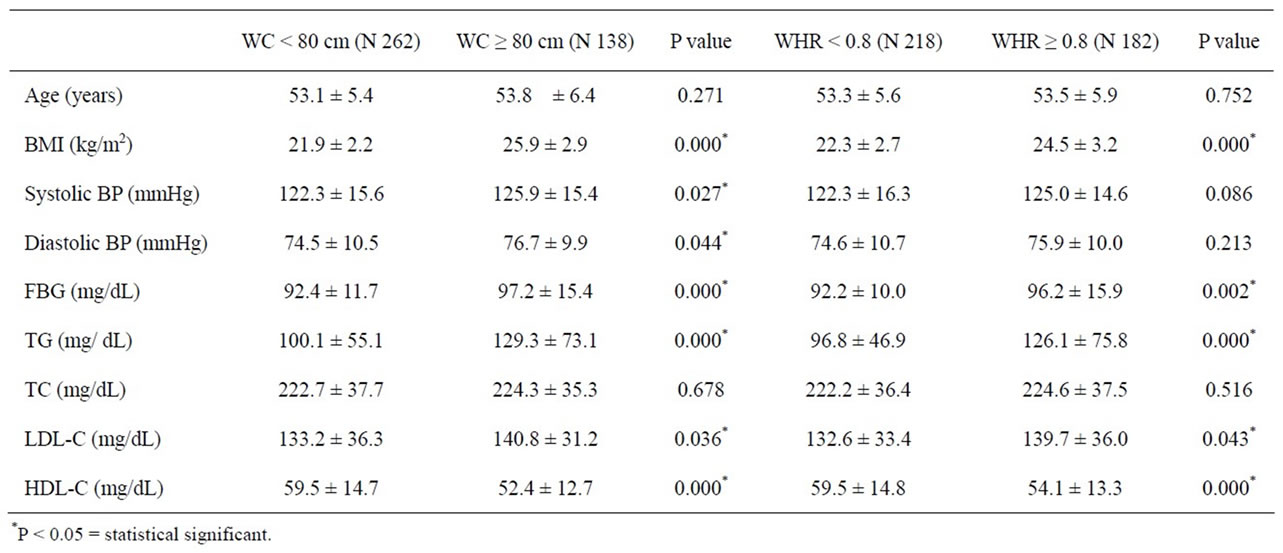
Table 2. Characteristic of participants classified by waist circumference (WC) or waist hip ratio (WHR) (mean ± SD) (student’s t test).
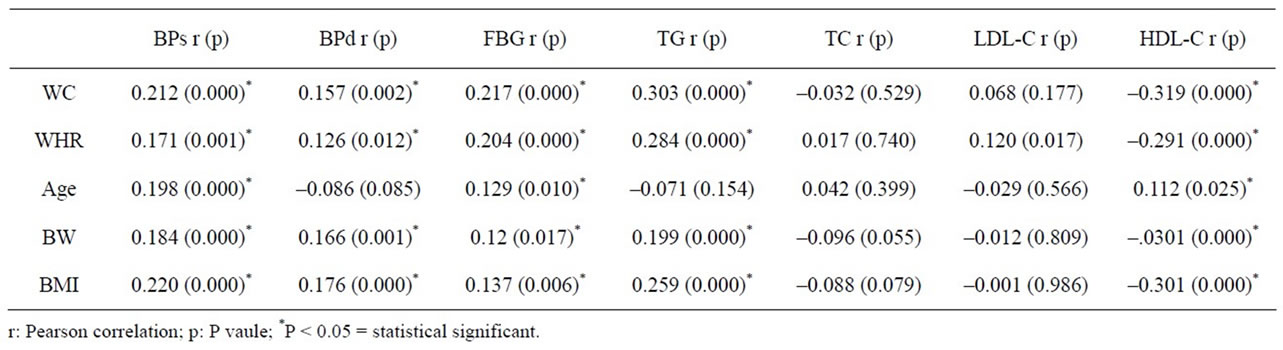
Table 3. The pearson correlation between waist circumference/waist-hip ratio/age/body weight/BMI with the following parameters (blood pressure, fasting blood glucose and lipid profiles).
with HDL-C. This correlation was similar when WHR, BW and BMI were analyzed. Although WC, WHR, BW and BMI had similar correlation with such parameters but the correlation was not strong. Age was the poor indicator because it had a weak correlation with only systolic BP, FBG and HDL-C.
Waist circumference, WHR, age, BW and BMI had the negative correlation with HDL-C.
The Chi square test comparing WC and WHR and such parameters are shown in Table 4. When WC was used (cutoff level at 80 cm), high FBG, high TG, high LDL-C and low HDL-C were found to be significantly higher in large WC compared to small WC. When WHR was used (cutoff level at 0.8), high FBG, high TG and low HDL-C were found significantly more prevalent in large WHR, the same as large WC.
Table 5 compares BP, FBG, TG, TC, LDL-C and HDLC between hormone use and non-hormone use.Both groups were not different un terms of BP, FBG, TG, LDL-C and HDL-C. Total cholesterol was significant higher in nonhormone use.
4. DISCUSSION
The authors found the positive correlation with WC and BP (systolic and diastolic), FBG and TG and the negative correlation with HDL-C. Similar correlation can be demonstrated for WHR, BW and BMI. However, the correlation was weak. Waist circumference represents similar picture as BMI since high WC reflects high BMI. Then either WC, WHR, BW or BMI can be used to predict the relationship. Despite the usefulness of any method, WC is a preferable choice.
Waist hip ratio is more complicated in practice and can predict the same as WC. The present study showed that the value of WHR was similar to BMI.
Waist circumference of ≥80 cm was found to be more significantly high BP (systolic and diastolic), FBG, TG, LDL-C and low HDL-C than less WC. Similarly, high WHR (≥0.8) was found to be more significantly prevalent among participants with high FBG, TG, LDL-C and low HDL-C. However TC was not significant different between groups either WC or WHR was used.
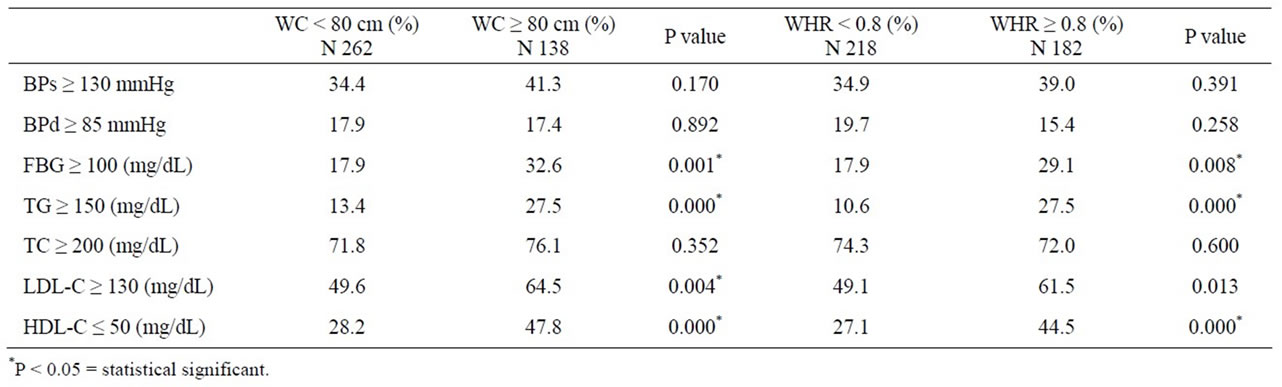
Table 4. Chi square test between WC and WHR and the following parameters (blood pressure, fasting blood glucose and lipid profiles).
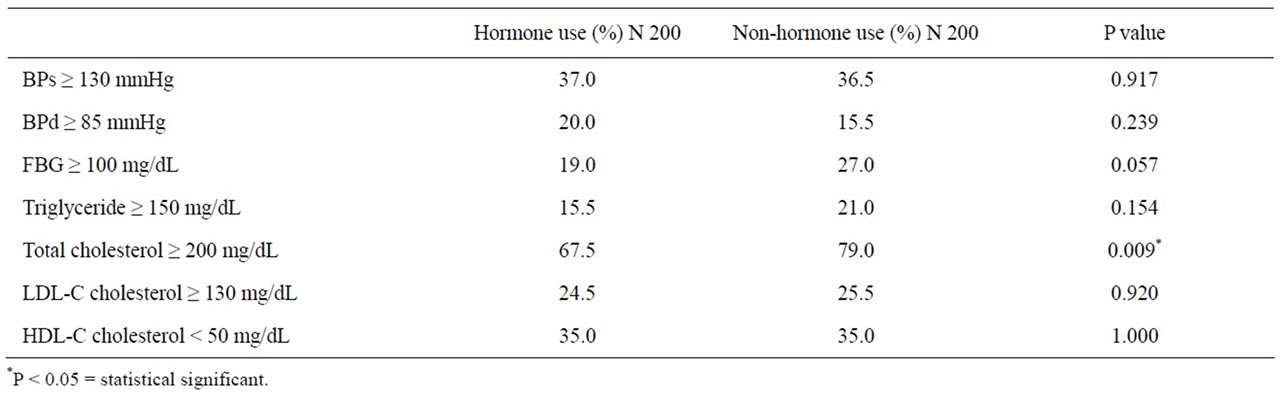
Table 5. Chi square test between hormone use and non hormone use with the following parameters (blood pressure, fasting blood glucose and lipid profiles).
Data from Iran [9] demonstrates that WC showed significant correlation with TG, TC and LDL-C. Previous data shows different results from the present study (except for TG and LDL-C) that may be explained by racial difference of studied population and participants in Iran’s were only overweight and obese. However, other data from adult healthy population in Iran demonstrates the correlation of WC as same as previous data with the strongest correlation with TG [10]. Moreover, WC had no correlation with FBG [10]. Jeong showed that WC, WHR, BMI and weight/height ratio had a positive correlation with dyslipidemia (TC/HDL > 4) in Korean women (age > 50 yrs) [11].
The prevalence of MS in Thai menopausal women in Bangkok (perimenopause, post menopause and surgical menopause) was 14.9% - 16.0% by modified NCEP ATPIII criteria (WC for Asian women) [12]. In the present study higher prevalence (21.0%) was found. This difference can be partly explained by the fact that participants were from different regions, Northern vs. central. The lifestyle may be influential factor. However, when compare the prevalence with other studies we found much lower in this study. The prevalence of MS in postmenopausal women in China is 33.7% [13], Brazil (34.7%) [14] and Ecuador (41.5%) [15].
When focus on only lipid profiles, the authors also found the high prevalence of abnormal values either TG, TC, LDL-C and HDL-C. Hypercholesterolemia (73.3%) was the most prevalent follow by high LDL-C (54.8%). The most common indicators for MS in Thai menopausal women was by systolic hypertension followed by low HDL-C. Data from Brazil in climacteric women the most prevalent indicators are low HDL-C and hypertension [14]. Data from postmenopausal women from Brazil shows that WC > 88 cm is the most common indicator [16], similar to results of another study from Buenos Aires [17]. While study in Spanish perimenopausal women, hypertriglyceridemia is the most common factor in MS, followed by central obesity [18]. The different groups of participants give different results, the most common indicators for MS in cardiologic clinic in Brazil were hypertension and hypertriglyceridemia [19]. About one third of Thai menopausal women in the present study had systolic hypertension, low HDL-C and abdominal obesity. Even though Thai have a small body figure, but they often have abdominal obesity (34.5%).
The present study included women with hormone therapy for menopausal symptoms. At the present time, there is limited data of the effect of hormone use on MS. Hormone therapy may give a beneficial effects on lipid profiles that affect to the risk of MS [20,21]. The Chi square test in this study was shown that hormone therapy had no effect on lipid profiles parameters and FBG and also BP. But more favourable effect on TC was found in hormone use group.
The limitation of the present study is lacking in detail of lifestyle in participants such as diet and physical activity. However, all participants were in the quite similar background (including diet and habit) because their habitat and culture and none of them was smoking. It is the nature of Thai women that different from women in the Western countries. The authors do not describe the types of hormone therapy because there were a variety of regimens in the present study. Moreover, all participants had not continue to use the same regimen from the beginning till enrollment. However, the most common hormone regimen was oral route.
Even though some of our findings were different from others, we believed that WC is still a simple and valuable method to predict MS despite its weak correlation.
In conclusion, WC had a weak positive correlation with BP, FBG, TG and a negative correlation with HDL-C as same as WHR, BW and BMI. Waist circumference ≥ 80 cm was found to be significant different from those with WC < 80 cm in terms of higher BP, FBG, TG, LDL-C and lower HDL-C. The prevalence of MS in Thai menopausal women was 21.0%. The two most common indicators for MS in the present study were systolic hypertension and low HDL-C. Abdominal obesity was found in 34.5% and it was the third most prevalent indicator for MS.
Waist circumference measurement is beneficial in terms of prediction of the rest indicators for MS (BP, FBG, TG and HDL-C) but it can not predict TC and LDL-C.
![]()
![]()
REFERENCES
- Ford, E.S. (2004) The metabolic syndrome and mortality from cardiovascular disease and all-causes: Findings from the National Health and Nutrition Examination Survey II Mortality Study. Atherosclerosis, 173, 309-314. doi:10.1016/j.atherosclerosis.2003.12.022
- Ford, E.S. (2005) Risks for all-cause mortality, cardiovascular disease, and diabetes associated with the metabolic syndrome: A summary of the evidence. Diabetes Care, 28, 1769-1778. doi:10.2337/diacare.28.7.1769
- Ford, E.S., Giles, W.H. and Dietz, W.H. (2002) Prevalence of the metabolic syndrome among US adults: Findings from the third National Health and Nutrition Examination Survey. Journal of the American Medical Association, 287, 356-359. doi:10.1001/jama.287.3.356
- Lobo, R.A. (2008) Metabolic syndrome after menopause and the role of hormones. Maturitas, 60, 10-18. doi:10.1016/j.maturitas.2008.02.008
- Ford, E.S., Li, C., Zhao, G. and Tsai, J. (2010) Trends in obesity and abdominal obesity among adults in the United States from 1999-2008. International Journal of Obesity, 35, 736-743.
- Executive Summary of the Third Report of the National Cholesterol Education Program (NCEP) (2001) Expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). Journal of the American Medical Association, 285, 2486- 2497. doi:10.1001/jama.285.19.2486
- Alberti, K.G., Zimmet, P. and Shaw, J. (2006) Metabolic syndrome—A new world-wide definition. A consensus statement from the International Diabetes Federation. Diabetic Medicine, 23, 469-480. doi:10.1111/j.1464-5491.2006.01858.x
- Taechakraichana, N., Pasatrat, S., Ninlagarn, T., Panyakhamlerd, K., Chaikittisilpa, S. and Limpaphayom, K. (1999) Dyslipidemia among healthy postmenopausal Thai women. Journal of the Medical Association of Thailand, 82, 895- 899.
- Shahraki, T., Shahraki, M. and Roudbari, M. (2009) Waist circumference: A better index of fat location than WHR for predicting lipid profile in overweight/obese Iranian women. Eastern Mediterranean Health Journal, 15, 899- 905.
- Chehrei, A., Sadrnia, S., Keshteli, A.H., Daneshmand, M.A. and Rezaei, J. (2007) Correlation of dyslipidemia with waist to height ratio, waist circumference, and body mass index in Iranian adults. Asia Pacific Journal of Clinical Nutrition, 16, 248-253.
- Jeong, S.K., Seo, M.W., Kim, Y.H., Kweon, S.S. and Nam, H.S. (2005) Does waist indicate dyslipidemia better than BMI in Korean adult population? Journal of Korean Medical Science, 20, 7-12. doi:10.3346/jkms.2005.20.1.7
- Indhavivadhana, S., Rattanachaiyanont, M., Wongvananurak, T., Kanboon, M., Techatraisak, K., Leerasiri, P., et al. (2011) Predictors for metabolic syndrome in perimenopausal and postmenopausal Thai women. Climacteric, 13, 58-65. doi:10.3109/13697137.2010.481735
- Ruan, X., Jin, J., Hua, L., Liu, Y., Wang, J. and Liu, S. (2010) The prevalence of metabolic syndrome in Chinese postmenopausal women and the optimum body composition indices to predict it. Menopause, 17, 566-570.
- Figueiredo Neto, J.A., Figueredo, E.D., et al. (2010) Metabolic syndrome and menopause: Cross-sectional study in gynecology clinic. Arquivos Brasileiros de Cardiologia, 95, 339-345. doi:10.1590/S0066-782X2010005000094
- Hidalgo, L.A., Chedraui, P.A., Morocho, N., Alvarado, M., Chavez, D. and Huc, A. (2006) The metabolic syndrome among postmenopausal women in Ecuador. Gynecological Endocrinology, 22, 447-454. doi:10.1080/09513590600890272
- Orsatti, F.L., Nahas, E.A., et al. (2010) Association between anthropometric indicators of body fat and metabolic risk markers in post-menopausal women. Gynecological Endocrinology, 26, 16-22. doi:10.3109/09513590903184076
- Mesch, V.R., Boero, L.E., et al. (2006) Metabolic syndrome throughout the menopausal transition: Influence of age and menopausal status. Climacteric, 9, 40-48. doi:10.1080/13697130500487331
- Aguilar, V.Z. and Garcia, L.L. (2009) Screening of metabolic syndrome in the perimenopause. Ginecología y Obstetricia de México, 77, 123-127.
- Barbosa, J.B., Silva, A.A., et al. (2010) Metabolic syndrome in outpatient cardiology clinics. Arquivos Brasileiros de Cardiologia, 94, 46-54. doi:10.1590/S0066-782X2010000100009
- Green, J.S., Stanforth, P.R., et al. (2004) The effects of exercise training on abdominal visceral fat, body composition, and indicators of the metabolic syndrome in postmenopausal women with and without estrogen replacement therapy: The HERITAGE family study. Metabolism, 53, 1192-1196. doi:10.1016/j.metabol.2004.04.008
- Shakir, Y.A., Samsioe, G., Nerbrand, C. and Lidfeldt, J. (2004) Combined hormone therapy in postmenopausal women with features of metabolic syndrome. Results from a population-based study of Swedish women: Women’s Health in the Lund Area study. Menopause, 11, 549-555. doi:10.1097/01.GME.0000133076.09175.6D
NOTES
*Conflict of interest: The authors report no conflict of interest. The authors alone are responsible for the content and writing of the paper.

