Case Reports in Clinical Medicine
Vol.3 No.4(2014), Article ID:44509,4 pages DOI:10.4236/crcm.2014.34047
Gastric Malrotation Relieved by Pleural Effusion Drainage
Guy Dori1,2*, Rawi Hazzan1, Gregori Kushner1
1Department of Internal Medicine E, HaEmek Medical Center, Afula, Israel
2Faculty of Medicine, Technion-Israel Institute of Technology, Haifa, Israel
Email: *guydo@clalit.org.il, ravih@clalit.org.il, greg_ku@clalit.org.il
Copyright © 2014 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 8 January 2014; revised 7 February 2014; accepted 5 March 2014
ABSTRACT
Mr M., 55-year-old, with metastatic adenocarcinoma of lung (stage IV) was admitted to the hospital after an earlier visit to oncology, where he presented with abdominal pain and distention suspected of having ascites for the first time. After performing abdominal CT and gastric passage film, it was hypothesized that clinical manifestation was related to gastric malrotation. The latter was forced by the huge left pleural effusion. Draining the pleural effusion may be complicated by a trapped lung, an adverse effect where the lung does not expand post drainage. After considering the palliative therapeutic options the effusion was drained, the stomach recoiled to its anatomical position, gastric malrotation was relieved, and the patient resumed oral nutrition. Though gastric malrotation due to a huge, malignant left pleural effusion is rare, it should be considered as more patients are being treated for lung cancer.
Keywords:Malignant Pleural Effusion, Gastric Malrotation

1. Presentation
Mr M., 55-year-old, with metastatic adenocarcinoma of lung (stage IV) was admitted to the hospital after an earlier visit to oncology, where he presented with a distended abdomen suspected of having ascites for the first time. An attempt to drain the ascitic fluid provided 500 ml of dark brownish fluid. After the procedure, Mr. M. suffered severe left upper quadrant pain and nausea, and therefore hospitalized.
2. Assessment
Abdominal and chest computed tomography (CT) with intravenous contrast media performed on admission demonstrated many pathologies, however we focus on the following: 1) severe gastric distention and malrotation containing approximately 2 liters of fluid (Figure 1, *). 2) A huge encapsulated pleural effusion occupying most of the left hemithorax (Figure 1, **) (comparing with previous CT the volume of the fluid significantly increased), and 3) no signs of ileal dilatation, free air in the abdomen or ascites were demonstrated (not shown). Liver metastases were also demonstrated.
Nasogastric tube was inserted alleviating nausea. Drained gastric content demonstrated coffee ground.
Gastric passage film demonstrated a caudally depressed stomach (Figure 2, gastric fundus and pylorus are at
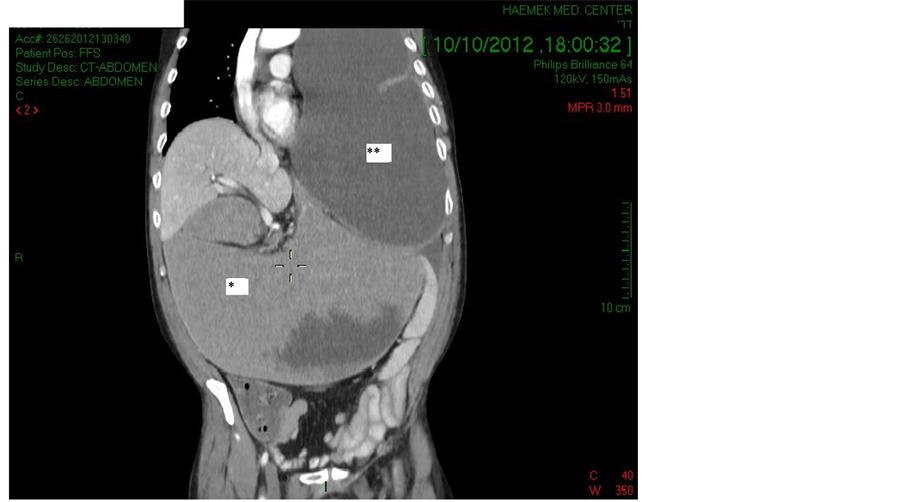
Figure 1. Abdominal and chest computed tomography (coronal plane) showing gastric dilatation (*) associated with left pleural effusion (**).
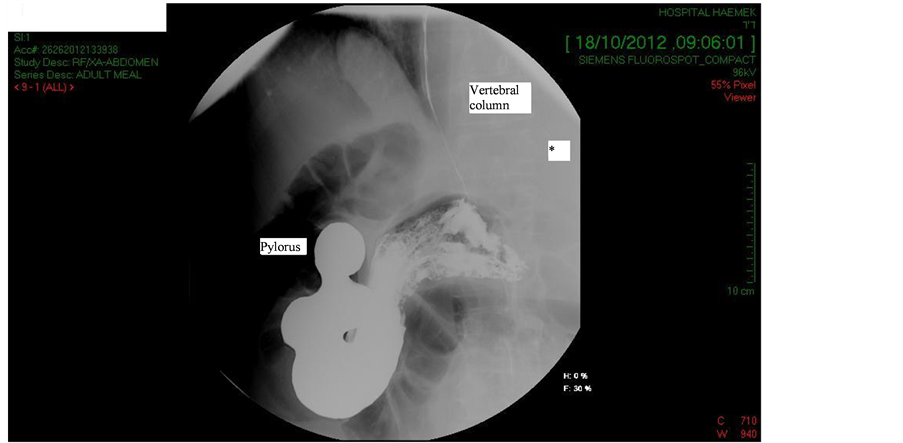
Figure 2. Gastric passage film before left pleural drainage showing a caudally depressed stomach.
the same level, deviating to the right of the vertebral column, pleural effusion marked by *).
Patient’s nausea and pain were relieved by inserting a nasogastric tube, however Mr. M. could not eat. Nutrition administered via nasogastric tube was not absorbed even hours after administration. Differential diagnosis included: gastric outlet obstruction due to metastasis or a functional kink of the pylorus, edema of the pylorus, gastric vulvulus or malrotation. Multi-disciplinary discussion, with oncologists, gastroenterologists, pulmonologists, radiologists, surgeons and the authors resulted in a working diagnosis. It was hypothesized that the stomach is malrotated probably due to the space occupying effect of the huge left pleural effusion. Yet, we were reluctant to drain this effusion since we thought that the left lung will not expand, an adverse effect known as trapped lung [1] .
3. Management
Two palliative options were examined: 1) maintaining the nasogastric tube, relieving the nausea and pain however, accepting the nutritional deficit and the grave prognosis, versus 2) draining the pleural effusion, hoping the stomach will “recoil” to its anatomical position, resuming oral intake, however, considering the adverse outcome of a trapped left lung. Mr. M’s life expectancy was estimated to be weeks and therefore, after thoroughly discussing the palliative options with him, we proposed to drain the pleural effusion [2] .
A 16-gauge central venous catheter was introduced into the left pleural sac, draining 6.4 liters over 6 days. The stomach recoiled to its anatomical position. Nasogastric tube was removed and patient slowly began eating, without vomiting. Post drainage passage film (Figure 3) demonstrated repositioning of the stomach (fundus left to vertebral column and at higher position relative to pylorus, air is observed in the left lower lobe, marked by *).
The left lung expanded to some extent, pleural effusion began to re-accumulate, however, symptoms of pain and nausea did not recur.
Approximately, 2 months after discharge Mr. M. passed away.
Lessons taken: 1) Abdominal pain and distention in a patient with known metastatic malignancy requires a differential diagnosis and may not always be ascites. It is possible that the first attempt of abdominal paracentesis resulted in puncturing the stomach. 2) The clinical manifestation of abdominal distention, and vomiting, due to gastric malrotation is rare, however, previously described in children [3] . Gastric malrotation resulting from a space occupying effect of a huge malignant pleural fluid was, to the best of our knowledge, not described hitherto. Nevertheless, as more patients are treated for lung cancer such a complication may be expected. 3) Pal-
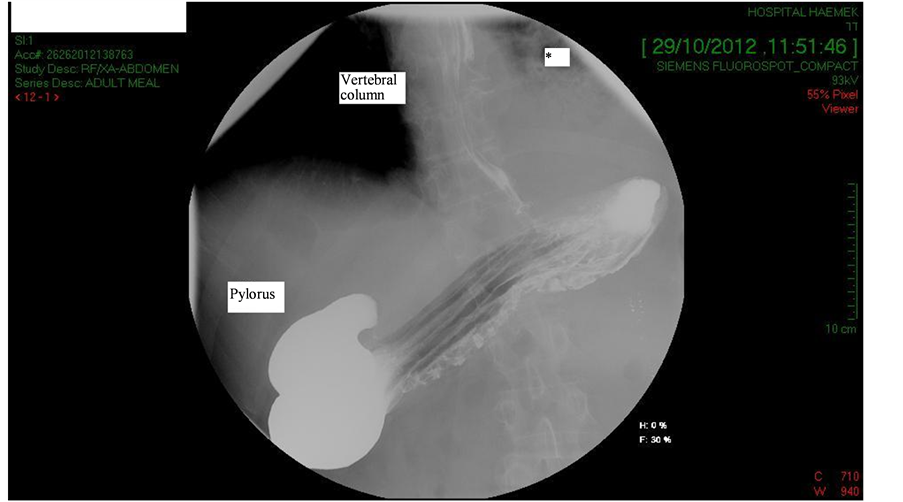
Figure 3. Gastric passage filmafter left pleural drainage showing repositioning of the stomach.
liative care aims to improve patient’s symptoms, while considering possible adverse outcomes. There is only a short window of opportunity to somewhat improve quality of life of a terminally-ill patient and this opportunity should not be missed on our behalf.
References
- Roberts, M.E., Neville, E., Berrisford, R.G., Antunes, G., Ali, N.J., BTS Pleural Disease Guideline Group (2010) Management of a Malignant Pleural Effusion: British Thoracic Society Pleural Disease Guideline 2010. Thorax, 65, ii32- ii40. http://dx.doi.org/10.1136/thx.2010.136994
- Beyea, A., Winzelberg, G. and Stafford, R.E. (2012) To Drain or Not to Drain: An Evidence-Based Approach to Palliative Procedures for the Management of Malignant Pleural Effusions. Journal of Pain Symptom Management, 44, 301-306. http://dx.doi.org/10.1016/j.jpainsymman.2012.05.002
NOTES

*Corresponding author.

