International Journal of Clinical Medicine
Vol.5 No.2(2014), Article ID:42449,4 pages DOI:10.4236/ijcm.2014.52013
Strangulated Femoral Hernia: A Challenging Surgical Vignette —Case Report and Review of Literature
Ketan Vagholkar
Ketan Vagholkar Department of Surgery, Dr. D.Y. Patil Medical College, Navi Mumbai, India.
Email: kvagholkar@yahoo.com
Received October 18th, 2013; revised November 15th, 2013; accepted December 10th, 2013 Copyright © 2014 Ketan Vagholkar. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. In accordance of the Creative Commons Attribution License all Copyrights © 2014 are reserved for SCIRP and the owner of the intellectual property Ketan Vagholkar. All Copyright © 2014 are guarded by law and by SCIRP as a guardian.
ABSTRACT
External hernia is one of the commonest causes of intestinal obstruction. Femoral hernia is a relatively uncommon hernia. It has a very high complication rate due to delayed diagnosis caused by deceptive symptomatology and subtle signs. CT scan enables a prompt diagnosis. Rigorous resuscitation followed by prompt surgical intervention is the mainstay of treatment. A case of a strangulated femoral hernia in a patient with complicated co morbid medical disorders is presented to highlight the pitfalls in initial clinical assessment.
Keywords: Strangulated Femoral Hernia Diagnosis Surgical Treatment
1. Introduction
Acute intestinal obstruction is one of the commonest surgical emergencies. Incarcerated external hernia is one of the leading causes of intestinal obstruction [1]. Clinically overt hernias may be easy to diagnose. However, rare types of hernias such as complicated femoral hernias are at times difficult to diagnose and may pose a surgical dilemma while deciding the cause for obstruction. A case of strangulated femoral hernia in a 78-year-old lady suffering from sick sinus syndrome with features of intestinal obstruction is presented with a view to highlight the wide range of clinical and diagnostic deception.
2. Case Report
A 78-year-old lady who was a known case of sick sinus syndrome presented with symptoms of abdominal pain, vomiting and inability to pass flatus and stools. Patient was initially admitted to a peripheral medical centre. During the course of treatment at that centre, she was administered conservative treatment for suspected intestinal obstruction in addition to the treatment for persistent bradycardia and hypertension. She was then transferred to a tertiary care centre. On admission to hospital she had one episode of generalised tonic-clonic convulsions which lasted for about four minutes followed by the prolonged post-ictal phase. On examination she was unconscious, not responding to oral commands. Her pulse was 56/min and her blood pressure was 160/100 mm of Hg. She had a naso-gastric tube and a per-urethral catheter already inserted. The nature of naso-gastric tube aspirate was bilious. Per abdominal examination did not reveal any distension. It was soft with no evidence of tenderness or rebound tenderness. Per rectal examination revealed an empty rectum. She had a swelling in the right groin situated below and lateral to the pubic tubercle measuring four cms in diameter. There was no tenderness or redness over the swelling. As the patient was unconscious, details pertaining to the groin swelling were not available. Details pertaining to the onset, duration and progress of the groin swelling were known from the patient only after the surgery. Laboratory investigations revealed haemoglobin of 13 gm%, haematocrit of 35, total count of 16000/mm3, Sodium 120 mEq/L, Potassium 2.2 mEq/L, Chloride 90 mEq/L, Calcium 7.5 mg%, Serum Creatinine 0.5 mg%. Correction of fluid and electrolyte balance was done aggressively. Plain X ray abdomen revealed a few gas filled bowel loops without any air fluid levels. Blood pressure was controlled by a nitroglycerine drip. After correction of fluid and electrolyte depletion which took two days, a CT scan of the abdomen was done which revealed an irreducible right-sided femoral hernia (Figure 1). Patient was taken up immediately for inguinal exploration under general anaesthesia.
The swelling was dissected. It was a hernia sac originating from the femoral ring. The appearance of bowel in the sac was gangrenous (Figure 2). In view of the difficulty in releasing the gangrenous contents by virtue of the severe tension in the sac a laparotomy was done through a lower midline incision in order to achieve reduction of the contents in the hernia sac. With great difficulty the contents were reduced into the abdominal cavity. A segment of intestine, measuring approximately 6 cm. in length was completely gangrenous (Figure 3). A resection anastomosis was done. The peritoneal cavity was closed in layers. A high herniotomy was done for the femoral sac. The femoral ring was very wide (Figure 4). In view of strangulated contents, a decision not to use a mesh was taken. The femoral ring was obliterated by approximating the inguinal ligament to the Cooper’s ligament with non absorbable sutures (Figure 5). Post-operatively, recovery of bowel function took approximately 5 days. There were no wound complications. Patient has been following up for approximately 4 month with no complaints.
3. Discussion
Femoral hernia is commonly seen in the female population. It is a hernia which is most prone to complications due to the narrowness of the femoral ring and the intricate relationship with neuro-vascular structures. The diagnosis of uncomplicated femoral hernias may at times be very difficult. However diagnosis of complicated femoral hernias may be easy. This is due to the fact that a sudden onset of a groin swelling, followed by symptoms of obstruction is almost confirmatory. Many a times, the history may be deceptive, as in the case presented, where in the patient had a history of a right groin swelling for a few weeks preceding this emergency. However the patient never acknowledged the presence of this swelling until after surgery. Commonest complication associated with the femoral hernia is irreducibility followed by obstruction and in most cases strangulation. [2] The peculiarity of this hernia is that it can manifest with symptoms of strangulation without obstruction. This condition is most commonly seen in middle aged women. Many a time’s co-morbid medical conditions over-ride the symptomatology of the complications arising from this hernia. In the case presented the patient was already suffering

Figure 1. Contrast CT showing the intestinal loop as the content of the right femoral sac medial to the femoral vessels.
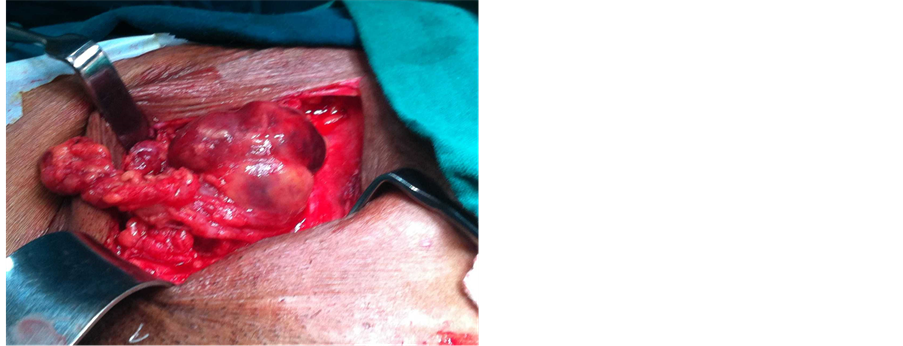
Figure 2. Intraoperative photograph showing the complicated femoral hernia sac with devitalized contents.

Figure 3. Extent of the full circumference gangrenous segment of the small intestine after trans abdominal reduction of the contents of the sac.
from sick sinus syndrome, had severe electrolyte depletion eventually leading to an episode of convulsion. These haemodynamic and metabolic complications

Figure 4. Widened right femoral ring after completion of a high right femoral herniotomy.

Figure 5. Femoral ring obliterated or closed by approximating the inguinal ligament with the Cooper’s ligament.
create compelling circumstances for a prompt and aggressive treatment taking a priority over other symptoms [2,3]. In the present case it took quite some time to bring all these derangements under control before surgical intervention could be contemplated. A contrast enhanced CT scan of the abdomen is an excellent tool to identify the cause for obstruction in the abdomen [4]. The right sided contents of the sac were clearly picked up and documented in the CT scan (Figure 1). CT scan therefore is an excellent investigation for diagnosing the aetiology of obstruction after having corrected the fluid and electrolyte depletion [5].
As soon as the diagnosis of an incarcerated femoral hernia is made, surgical treatment should be initiated immediately. Various approaches have been described in literature [6]. These are femoral approach, inguinal approach and a combined femoral and inguinal approach.
The choice of approach is dictated by the ease with which the surgeon can manage the damaged intestines and offer a safe and definitive repair. In the case presented as the sac was extremely tense and the contents gangrenous, any attempt to reduce the contents through a femoral approach could have caused more damage adding to the difficulty in reducing the contents. Carrying out the resection anastomosis of the strangulated loop would have been almost a technical impossibility through the femoral approach. It is always safe to add on a lower midline laparotomy in such complex situations as was done in the case presented. This not only adds to the manual dexterity in reducing the contents but also enables comfortable resection and anastomosis of the damaged intestines [7]. The laparotomy incision can then be safely closed after having explored every inch of the intestine. An added laparotomy approach may also be useful in those femoral hernias which contain a variety of rare abdominal contents such a caecum, ascending colon, Meckel’s diverticulum, ovary, fallopian tube and a bladder diverticulum [8-12]. Difficult situations may arise when any part of the colon gets trapped in the incarceration [11]. Clear identification of the proximal and distal end is pivotal in safe reduction and optimum decision making in strangulated femoral hernias. Therefore it is a safe practice to add a midline laparotomy to an inguinal or femoral approach in order to achieve safe and optimum surgical cure. The choice of repair for a femoral hernia again raises a few questions. The mesh plug technique is undoubtedly a good option for uncomplicated femoral hernias. But in the situation, where there are strangulated loops, this may heighten the chances of infection leading to failure of the repair [13]. Therefore it is advisable that in the situation of a strangulated femoral hernia the traditional McEvedy’s technique of approximating the inguinal ligament to the Cooper’s ligament be adopted after a high herniotomy.
The morbidity and mortality associated with complicated femoral hernias is very high as most of the patients are of an advanced age. Fluid, electrolyte imbalance and septicaemia are the commonest causes for morbidity and mortality [7]. Initial resuscitation should be initiated promptly and aggressively in order to enable a CT diagnosis and immediate surgical treatment.
4. Conclusion
Complicated femoral hernia can give rise to a wide spectrum of clinical features. Prompt and aggressive primary resuscitation followed by a contrast enhanced CT scan of the abdomen will enable confirmation of the diagnosis. No sooner is the diagnosis confirmed than prompt surgery should be performed. It is a safe practice to combine a groin incision with a lower midline laparotomy not only to ease but also to enhance the quality of surgical care.
Acknowledgements
I would like to thank Dr. Shirish Patil, Dean, Dr, D.Y.
Patil Medical College, Navi Mumbai, MS, India for allowing me to publish this case report. I would also like to thank Mr. Parth Ketan Vagholkar for his help in typesetting the manuscript.
[1] REFERENCES
[2] U. Ihedioha, A. Alani, P. Modak, P. Chong and P. J. O’Dwyer, “Hernias Are the Most Common Cause of Strangulation in Patients Presenting with Small Bowel Obstruction,” Hernia, Vol. 10, No. 4, 2006, pp. 338-340. http://dx.doi.org/10.1007/s10029-006-0101-7
[3] S. Kadirov, J. Sayfan, S. Friedman and R. Orda, “Richter’s Hernia—A Surgical Pitfall,” Journal of the American College of Surgeons, Vol. 182, No. 1, 1996, pp. 60- 62.
[4] L. S. Bizer, R. W. Liebling, H. M. Delany and M. L. Gliedman, “Small Bowel Obstruction: The Role of Non Operative Treatment in Simple Intestinal Obstruction and Predictive Criteria for Strangulation Obstruction,” Surgery, Vol. 89, No. 4, 1981, pp. 407-413.
[5] D. H. Frager and J. W. Baer, “Role of CT in Evaluating Patients with Small Bowel Obstruction,” Seminars in Ultrasound, CT, and MRI, Vol. 16, No. 2, 1995, pp. 127- 140. http://dx.doi.org/10.1016/0887-2171(95)90005-5
[6] R. Vinca, G. Angelelli, A. A. Stabilelanora, A. Gabello and A. Rotundo, “Vascular Complications in Intestinal Obstructions. The Role of Computed Tomography,” Radiologia Medica, Vol. 98, No. 3, 1999, pp. 157-161.
[7] O. Alimoglu, B. Kaya, I. Okan, F. Dasiran, D. Guzey, G. Bas and M. Sahin, “Femoral Hernia: A Review of 83 Cases,” Hernia, Vol. 10, No. 1, 2006, pp. 70-73. http://dx.doi.org/10.1007/s10029-005-0045-3
[8] N. Kurt, M. Oncel, Z. Ozkan and S. Bingul, “Risk and Outcome of Bowel Resection in Patients with Incarcerated Groin Hernias: Retrospective Study,” World Journal of Surgery, Vol. 27, No. 6, 2003, pp. 741-743. http://dx.doi.org/10.1007/s00268-003-6826-x
[9] A. H. Omari and M. A. Alghazo, “Urinary Bladder Diverticulum as Content of Femoral Hernia: A Case Report and Review of Literature,” World Journal of Emergency Surgery, Vol. 8, No. 1, 2013, p. 20. http://dx.doi.org/10.1186/1749-7922-8-20
[10] M. Mifsud and E. Ellul, “Meckel’s Diverticulum in a Strangulated Femoral Hernia. Case Report and Review of Literature,” Annali Italiani di Chirurgia, Vol. 82, No. 4, 2011, pp. 305-307.
[11] A. Ay, A. Agac Ay, B. Kaptanoglu, S. Ozer and C. Akalin, “Femoral Hernia Containing Strangulated Ileum along with the Uterus and Both Ovaries: A First Case Report,” Hernia, Vol. 16, No. 3, 2012, pp. 351-353. http://dx.doi.org/10.1007/s10029-010-0758-9
[12] R. B. Patel, N. Vasava and S. Hukkeri, “Non Obstructed Femoral Hernia Containing Ascending Colon, Caecum, Appendix and Small Bowel with Concurrent Bilateral Recurrent Inguinal Hernia,” Hernia, Vol. 16, No. 2, 2012, pp. 211-213. http://dx.doi.org/10.1007/s10029-010-0726-4
[13] A. H. Omari and M. A. Alghazo, “Urinary Bladder Diverticulum as Content of Femoral Hernia: A Case Report and Review of Literature,” World Journal of Emergency Surgery, Vol. 8, No. 1, 2013, p. 20. http://dx.doi.org/10.1186/1749-7922-8-20
[14] T. Hachinsuka, “Femoral Hernia Repair,” Surgical Clinics of North America, Vol. 83, No. 5, 2003, pp. 1189- 1205. http://dx.doi.org/10.1016/S0039-6109(03)00120-8

