Open Journal of Orthopedics
Vol.4 No.4(2014), Article ID:45091,4 pages DOI:10.4236/ojo.2014.44019
Giant Cell Tumour of Tendon Sheath in Thumb—A Case Report
Sankar Rao. P, Siddaram Patil, Sandeep Reddy
Mamata Medical College, Department of Orthopaedic, Khammam, India
Email: drsnp_2006@yahoo.co.in
Copyright © 2014 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/


Received 4 March 2014; revised 8 April 2014; accepted 15 April 2014
ABSTRACT
Giant cell tumor of the tendon sheath is the second most common tumor of the hand often referred to as xanthoma. Histologically these tumors are composed of multinucleated giant cells, polyhedral histiocytes, fibrosis and hemosiderin deposits. Marginal excision of giant cell tumor of the tendon sheath is the treatment of choice. We present a case of xanthoma of flexor pollicis longus tendon presented as a single enlarging mass in volar aspect of left thumb. After clinical diagnosis, work-up is done with ultrasound, FNAC and excision biopsy.
Keywords:Thumb, Tendon Sheath, Giant Cell Tumor, Flexor Tendon

1. Case Report
A 55-year-old female patient presented us with complaints of swelling over the palmar aspect of the left thumb since 3 years. The Swelling was insidious in onset, initial size being that of pea nut which gradually progressed to about 3 × 2 × 2 cm at the time of presentation (Figure 1). Patient did not give any history of trauma/prick injury. There was no history of any kind of immobilization or massage treatment, and no history of constitutional symptoms and any other similar swellings in the body. On examination proper, swelling extended from the Metacarpo-phalangeal joint to interphalangeal joint of left thumb. Swelling was globular in shape with the overlying skin being normal. Swelling was firm in consistency with mild tenderness and no local rise of temperature. It was non-reducible and non-translucent, mobile in horizontal direction and fixed in vertical direction. Movements are completely restricted at all joints of left thumb. She is unable to flex both MCP and IP joints of left thumb.
X-ray revealed no bony involvement. Serum calcium and serum phosphorus was 10.2 mg/dl and 3.0 mg/dl respectively. Serum ALP (127 IU/l), parathyroid hormone levels, creatinine kinase, aldolase levels, ANA, Vitamin D levels, 24 hours urinary calcium and inorganic phosphate were all within normal limits. Ultrasound of the swelling confirmed solid, homogenous, hypoechoic mass was adjacent to insertion of flexor pollicis longus tendon. Histopathological detailing was done with Fine Needle Aspiration Cytology (FNAC) which reported features suggestive of giant cell tumor of tendon sheath and excision biopsy that was planned for confirmative diagnosis and definitive treatment. Gross examination of the biopsy specimen revealed single nodular grey white mass of tissue measuring 3 × 2 × 1.5 cm, external surface nodular, cut section shows homogenous grey white nodular areas (Figure 2).
Microscopic examination smears showed moderate cellularity comprising of few dispersed plump fibrohistiocytic cells with oval vesicular nuclei and bland chromatin and moderate amount of cytoplasm, variable number of osteoclast like multinucleated giant cells are seen against hemorrhagic background (Figure 3). Biopsy findings confirmed the diagnosis of giant cell tumor of tendon sheath. Patient was followed up for a period of one year, where there were no signs of recurrence (Figure 4).

Figure 1. Clinical picture of swelling on volar aspect of thumb.

Figure 2. Gross specimen of resected tumour.

Figure 3. HPE showing scattered groups of mononuclear cells with occasional osteoclast like giant cell.
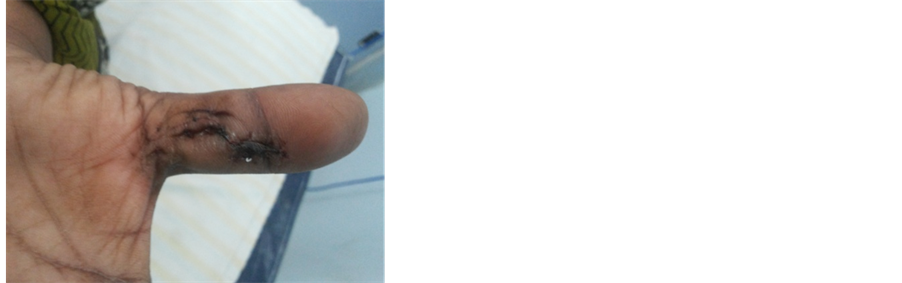
Figure 4. Post operative picture of the left thumb shows a healed surgical scar.
2. Discussion
GCT of tendon sheath is reactive lesions, not really tumors, which are similar to PVNS. They do not always arise from the tendon sheath but may arise from the synovium [1] -[13] . It is the second most common benign hand tumor next to ganglions. Despite recurrences of no malignant transformation has been reported [3] [14] [15] . Complete surgical excision remains the mainstay of treatment, assisted either with an operating microscope or a magnifying loupe. Radiotherapy has been suggested after inadequate excision and in patients with high mitotic activity to prevent recurrence [16] -[18] .
3. Conclusion
Giant cell tumors are benign conditions, appearing as asymptomatic nodules. In our case, it was presented as a single enlarging mass on volar aspect of left thumb (Figure 1). After clinical diagnosis, we proceeded with ultrasound, FNAC and excision biopsy. Microscopic examination revealed scattered groups of mononuclear cells as example, with occasional osteoclast like giant cell (Figure 3). After correlating the clinical history and presentation with the pathological findings, a diagnosis of Giant cell tumor of tendon sheath was concluded. We recommend complete excision of the lesion as it not only provides successful resolution without recurrence, but also establishes our diagnosis.
References
- Murphey, M.D., Rhee, J.H., Lewis, R.B., Fanburg-Smith, J.C., Flemming, D.J. and Walker, E.A. (2008) Pigmented Villonodular Synovitis: Radiologic-Pathologic Correlation. Radiographics, 28, 1493-1518. http://dx.doi.org/10.1148/rg.285085134
- Al-Qattan, M.M. (2001) Giant Cell Tumours of Tendon Sheath: Classification and Recurrence Rate. Journal of Hand Surgery (British Volume), 26, 72-75. http://dx.doi.org/10.1054/jhsb.2000.0522
- Reilly, K.E., Stern, P.J. and Dale, J.A. (1999) Recurrent Giant Cell Tumors of the Tendon Sheath. Journal of Hand Surgery, 24, 1298-1302. http://dx.doi.org/10.1053/jhsu.1999.1298
- Kotwal, P.P., Gupta, V. and Malhotra, R. (2000) Giant Cell Tumour of the Tendon Sheath. Is Radiotherapy Indicated to Prevent Recurrence after Surgery? The Bone & Joint Journal, 82, 571-573. http://dx.doi.org/10.1302/0301-620X.82B4.10328
- Rao, A.S. and Vigorita, V.J. (1984) Pigmented Villonodular Synovitis (Giant-Cell Tumor of the Tendon Sheath and Synovial Membrane): A Review of 81 Cases. The Journal of Bone & Joint Surgery, 66, 76-94.
- Choudhury, M., Jain, R. and Nangia, A. (2000) Localized Tenosynovial Giant Cell Tumor of Tendon Sheath. A Case Report. Acta Cytologica, 44, 463-466. http://dx.doi.org/10.1159/000328500
- Ciattaglia, G., Filosa, G. and Bugatti, L. (1991) Giant Cell Tumor of Tendon Sheath. Journal of the American Academy of Dermatology, 25,728-729. http://dx.doi.org/10.1016/S0190-9622(08)80680-9
- Suresh, S.S. and Zaki, H. (2010) Giant Cell Tumor of Tendon Sheath: Case Series and Review of Literature. Journal of Hand and Microsurgery, 2, 67-71. http://dx.doi.org/10.1007/s12593-010-0020-9
- Garg, B. and Kotwal, P.P. (2011) Giant Cell Tumour of the Tendon Sheath of the Hand. Journal of Orthopaedic Surgery (Hong Kong), 19, 218-220.
- Agarwal, P.K., Gupta, M. and Srivastava, A. (1997) Cytomorphology of Giant Cell Tumor of Tendon Sheath. A Report of Two Cases. Acta Cytologica, 41, 587-589. http://dx.doi.org/10.1159/000332562
- Iyer, V.K., Kapila, K. and Verma, K. (2003) Fine-Needle Aspiration Cytology of Giant Cell Tumor of Tendon Sheath. Diagnostic Cytopathology, 29, 105-110. http://dx.doi.org/10.1002/dc.10319
- Phalen, G.S., McCormack, L.J. and Gazale, W.J. (1959) Giant-Cell Tumor of Tendon Sheath (Benign Synovioma) in the Hand. Evaluation of 56 Cases. Clinical Orthopaedics, 15, 140-151.
- Moore, J.R., Weiland, A.J. and Curtis, R.M. (1984) Localized Nodular Tenosynovitis: Experience with 115 Cases. The Journal of Hand Surgery, 9, 412-417. http://dx.doi.org/10.1016/S0363-5023(84)80233-6
- Wright, C.J.E. (1951) Benign Giant-Cell Synovioma: An Investigation of 85 Cases. British Journal of Surgery, 38, 257-271. http://dx.doi.org/10.1002/bjs.18003815102
- Goda, J.S., Patil, P., Krishnappan, C. and Elangovan, D. (2009) Giant Cell Tumor of the Tendon Sheath Treated by Brachytherapy (Surface Mold) Technique-A Technical Illustration. Brachytherapy, 8, 79-83.
- Rodrigues, C., Desai, S. and Chinoy, R. (1998) Giant Cell Tumor of the Tendon Sheath: A Retrospective Study of 28 Cases. Journal of Surgical Oncology, 68, 100-103. http://dx.doi.org/10.1002/(SICI)1096-9098(199806)68:2<100::AID-JSO5>3.0.CO;2-A
- Darwish, F.M. and Haddad, W.H. (2008) Giant Cell Tumour of Tendon Sheath: Experience with 52 Cases. Singapore Medical Journal, 49, 879-882.
- Messoudi, A., Fnini, S., Labsaili, N., Ghrib, S., Rafai, M. and Largab, A. (2007) Giant Cell Tumors of the Tendon Sheath of the Hand: 32 Cases. Chirurgie de la Main, 26, 165-169. http://dx.doi.org/10.1016/j.main.2007.03.008

