Open Journal of Pathology
Vol. 2 No. 2 (2012) , Article ID: 18564 , 3 pages DOI:10.4236/ojpathology.2012.22006
Wegener’s Granulomatosis Presenting with Bilateral Excavated Nodules
![]()
1Department of Pathology, Abderrahmen Mami Hospital, Ariana, Tunisia; 2Department of Pneumology, Abderrahmen Mami Hospital, Ariana, Tunisia.
Email: *emnabraham@yahoo.fr
Received December 23rd, 2011; revised January 5th, 2012; accepted March 21st, 2012
Keywords: Vasculitis; Wegener; Pathology; Lung; Granulomatous Inflammation
ABSTRACT
Wegener’s granulomatosis (WG) is a systemic inflammatory disease whose histopathologic features often include necrosis, granuloma formation, and vasculitis of small-to-medium-sized vessels. We report a new case of Wegener’s granulomatosis occurring in a 41-year-old man who was admitted for respiratory symptoms, fever, asthenia, night sweats and weight loss since one month. Chest X-ray and computed tomography showed multiple bilateral pulmonary excavated lesions. A trransparietal lung biopsy was performed. Histological examination showed an area of necrosis, surrounded by a palisade of histiocytes. Some of the histiocytes were multinucleated and formed true granulomas within the wall of the adjacent pulmonary artery. Serology was strongly positive for ANCA. A diagnosis of Wegener granulomatosis was conducted and the patient was started on cyclophosphamide and methylprednisolone as an initial treatment, with a favorable evolution.
1. Introduction
Wegener’s granulomatosis (WG) is a rare disease of uncertain cause characterized by necrotizing granulomatosis vasculitis of small and medium-sized vessels [1]. It is distinguished clinically by its predilection for affecting the upper and lower respiratory tracts and kidneys and by the histologic presence of necrosis, granulomatous inflammation, and vasculitis [2].
2. Case Report
A 41-year-old man, smoker (10 pack-years), with family history of tuberculosis, was admitted for cough, hemoptysis, dysphagia, fever, asthenia, night sweats and weight loss since one month. At admission, the temperature was 38.3˚C, his throught was erytematous and his eyes were red.
The white blood cell count was 15,200/mm3, eosinophils were increased. Renal function was normal. CRP level was increased. Chest X-ray and showed multiple bilateral pulmonary opacities of variable size witch some are excavated (Figure 1). Computed tomography revealed diffuse bilateral nodules and parenchymal masses some with excavation, the largest measuring 5 cm in diameter (Figure 2). He was first treated with antibiotics without any improvement. The diagnoses of tuberculosis, hydatidosis, metastatic carcinoma to lung and vasculitis were proposed.
Fibreoptic bronchoscopy was performed, with bronchial washings and bronchial biopsies. No bacilli, including acid fast bacilli or fungal hyphae, were detected and the cultures remained negative. Cytology of washings and pathological examination of bronchial biopsies did not reveal malignancy, infection, or vasculitis; only slight, aspecific inflammation was noticed, and these results were regarded nondiagnostic.
Hydatidosis serology was negative. Serology was strongly positive for Anti-neutrophil cytoplasmic antibodies (ANCA).
A computed tomography guided lung biopsy was performed. Histological examination showed an area of necrosis, surrounded by a palisade of histiocytes. Some of the histiocytes were multinucleated and formed true granulomas within the wall of the adjacent pulmonary artery (Figures 3(a) and (b)). A diagnosis of Wegener granulomatosis was made based of the histopathology and ANCA positivity.
Laryngeal nasofibroscopy showed purulent rhinitis and spotting and urine analysis reveals hematuria.
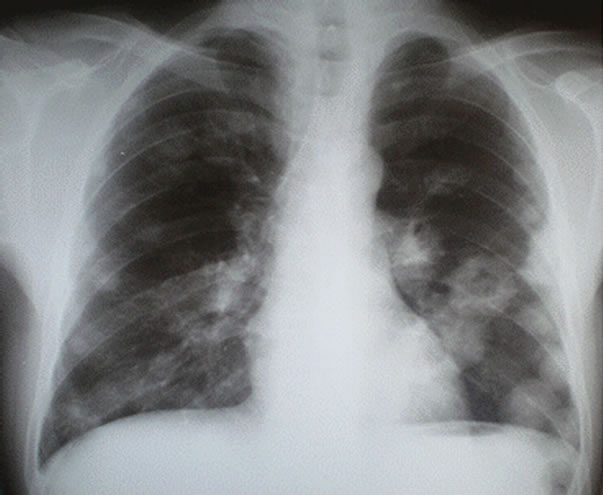
Figure 1. Chest radiograph showing multiple bilateral pulmonary opacities of variable size witch some are excavated.
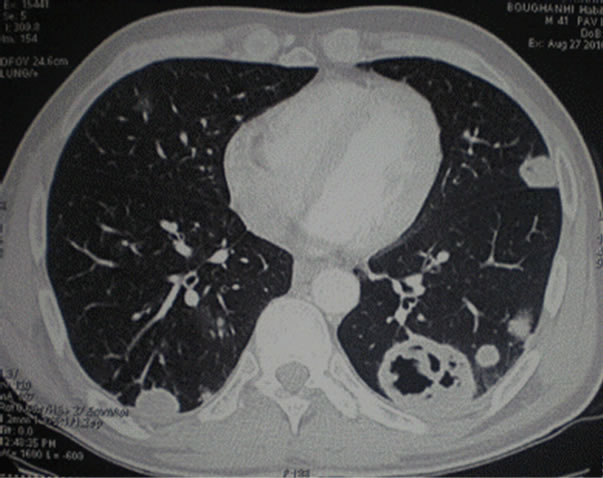
Figure 2. Computed chest tomography showing diffuse bilateral pulmonary nodules and masses of variable size with excavation.
Initial treatment consisted of intravenous methylprednisolone followed by oral prednisolone and cyclophos phamide. The treatment was well tolerated with clinical and radiological improvement 3 months after (Figure 4).
3. Discussion
Wegener’s granulomatosis is a systemic vasculitic syndrome, which affects mainly the upper and lower airways [3]. It was first described by Klinger in 1933, followed by other investigators, including Rossle in 1933, Wegener in 1936 and 1939, and Ringertz in 1947 [2].
Most patients are white, the sex distribution is equal, and most present in the fourth-fifth decade, although the age range extends to both extremes [2,4,5].
Pulmonary involvement is one of the cardinal features of WG. It occurs in 45% of patients at presentation and
 (a)
(a) (b)
(b)
Figure 3. (a) The pulmonary nodule was centered by an area of necrosis, surrounded by a palissade of histiocytes sometimes are giant and multinucleated; (b) Granulomas within the wall of the adjacent pulmonary artery (original magnification ×200).

Figure 4. Radiological improvement with reduction of number and size of pulmonary opacities.
87% during the course of the disease [2,5]. Cough, hemoptysis, and pleuritis are the most common pulmonary symptoms. Fever and weight loss may be reported at the onset of the disease and more frequently during the course of the illness [1,2,5].
Renal disease also may be seen as the initial presentation or during the course of the disease. Ocular manifestations have been reported to occur in 28% to 58% of patients with WG [2]. Other unusual presentations of WG include salivary gland, cutaneous, gastrointestinal, and cardiac involvement [2,5].
Imaging features are the result of an immunologically mediated necrotizing vasculitis that results in several different findings. The usual radiological pattern of WG in the lung is the presence of multifocal nodules, widely distributed over both lungs which are mostly cortical and excavated, with irregular margins varying from a few millimeters up to 10 centimeters. Other less frequent imaging manifestations include lung consolidation and ground-glass opacities, mosaic attenuation, tree-in-bud opacities, and interlobular septal thickening and pleural involvement. Alveolar hemorrhage usually accounts for the consolidation and ground-glass opacities, while the mosaic attenuation and tree-in-bud manifestations often relate to arteriolar involvement [1,3,4].
Anti-neutrophil cyctoplasmic antibodies (ANCA) are detected in almost all patients with active WG [3]. The presence of ANCA is not required to make a diagnosis of WG by either the American College of Rheumatology (ACR) or the Chapel Hill Consensus Conference (CHCC) definitions [2]. Recent reports suggest that ANCA in WG patients are produced in the respiratory tract, but the possible role of BAL as a diagnostic method has not been addressed in published studies [3].
Biopsy is usually needed to confirm clinical suspicion but it is not always diagnostic. Histologic changes tend to be patchy, requiring a lot of tissue for a positive yield. In our case, diagnosis was made on fine needle biopsy which shows charatcteristic lesions.
Histologically, classic lesion involves necrosis of medium size vessels with infiltration by neutrophils and multinucleated giant cells. In the lung, the necrosis takes on a “geographic” pattern and the classic necrotizing granulomatous vasculitis is found. A small vessel capillaritis and intraalveolar hemorrhage may also be seen. In the kidney, the ischemic injury is seen predominantly in the glomeruli where there is a crescentic glomerulonephritis. Glomerulonephritis is typically focal and segmental with few or no immune deposits [6,7].
The differential diagnosis of necrotizing granulomas includes infectious etiologies such as tuberculosis, aspergillosis, as well as foreign body type granulomatous inflammation or sarcoidosis. Like Wegener granulomatosis, infection can also cause necrosis, granulomatous inflammation, and vasculitis histologically, so microorganisms must be ruled out with special stains [8].
Traditionally, initial therapy of WG consists of daily oral cyclophosphamide-corticosteroid combination therapy. This treatment has been quite effective in inducing remission in more than 90% of patients who adhere to this regimen [2,5].
Other therapies for WG include methotrexate and prednisone, which is another alternative for patients with active but not immediately lifethreatening disease and normal or near-normal renal function [2,6]. In our case, the patient began therapy with monthly intravenous cyclophosphamide pulse therapy with clinical and radiological improvement.
In conclusion, Wegener granulomatosis should be considered in patient with respiratory and general symptoms presenting with multiple bilateral cavitary pulmonary nodules when infectious and malignant disease have been ruled out. Typical criteria found on histopathogical examination of lung nodule in association with ANCA positivity confirm the diagnosis.
REFERENCES
- A. C. Toffart, F. Arbib, S. Lantuejoul, J. F. Roux, V. Bland, G. Ferretti and S. Diab, “Wegener Granulomatosis Revealed by Pleural Effusion,” Case Report in Medicine, Vol. 2009, 4 February 2009, 3 p. doi:10.1155/2009/164395
- K. Shafiei, E. Luther, M. Archie, J. Gulick and M. R. Fowler, “Wegener Granulomatosis: Case Report and Brief Literature Review,” Journal of the American Board Family Medicine, Vol. 16, No. 6, 2003, pp. 555-559. doi:10.3122/jabfm.16.6.555
- T. Van Der Werf, C. Stegeman, K. Meuzelaar and W. Timens, “Late Recurrence of Wegener’s Granulomatosis Presenting as Solitary upper Lobe Pulmonary Mass,” European Respiratory Journal, Vol. 7, No. 7, 1994, pp. 1365-1368. doi:10.1183/09031936.94.07071365
- G. William and M. D. Schucany, “Wegener’s Granulomatosis Presenting as a Large Solitary Cavitary Mass,” Proceedings of Baylor University Medical Center, Vol. 23, No. 2, 2010, pp. 171-172.
- G. S. Hoffman, G. S. Kerr, R. Y. Leavitt, et al., “Wegener Granulomatosis: An Analysis of 158 Patients,” Annals of Internet Medicine, Vol. 116, No. 6, 1992, pp. 488-498.
- C. A. Langford, M. C. Sneller and G. S. Hoffman, “Methotrexate Use in Systemic Vasculitis,” Rheum Disease Clinics of North America, Vol. 23, No. 4, 1997, pp. 841-853. doi:10.1016/S0889-857X(05)70363-X
- C. A. Langford, “Update on Wegener Granulomatosis,” Cleveland Clinic Journal of Medicine, Vol. 72, No. 8, pp. 689-690, 693-697. doi:10.3949/ccjm.72.8.689
- R. J. José, J. P. Dilworth, J. Cleverley, M. Young, R. Stratton and M. Lipman, “Wegener’s Granulomatosis with Multiple Pulmonary Nodules—Diagnostic Difficulties,” JRSM Short Reports, Vol. 1, No. 34, 2010, pp. 469-470. doi:10.1258/shorts.2010.010043
NOTES
*Corresponding author.

