Camouflage Therapy for Post-Inflammatory Hyperpigmentation on the Face Caused by Fixed Drug Eruption 9
so we did not perform patch tests with compon ents of the
analgesic and instructed her not to take it in the future.
She tried to camouflage the bluish pigmentation on her
face by herself, however, she found it was difficult to
cover and her camouflage easily came off. Therefore, she
decided to participate in a medical camouflage lesson at
our camouflage clinic.
In the camouflage lesson, she first covered the hyper-
pigmentation with “Perfect Cover” (Shiseido, Tokyo,
Japan), an easy-to-use liquid foundation currently avail-
able only in Japan. It con tains a special thin film material
(titanium oxide coated by ultrafine iron oxide particles)
called Light-Filter-Powder. Next, she stabilized the co ver
with “d program smooth up foundation” (Shiseido, To-
kyo, Japan), and covered her lips with lipstick. The pa-
tient was satisfied with the results. The figures show her
face both before (Figure 1(a)) and after the application
of camouflage (Figure 1(b)).
3. Discussion
The hyperpigmentation caused by fixed drug eruption is
due to melanophages in the dermis, and is known as
dermal hypermelanosis. It also occurs in lichen planus,
cutaneous lupus erythematosus, and other post-inflam-
matory hyperpigmented dermatoses. In dermal hyperme-
lanosis, there is a destruction of basal keratinocytes [6].
These degenerating keratinocytes contain large amounts
of melanin which are eventually phagocytosed by macro-
phages (melanophages) in the upper dermis [6]. These
melanophages accumulate at the site of injury producing
a blue-gray discoloration [6].
Post-inflammatory hyperpigmentation can have a
negative impact on a patient’s qu a lity of life. Camouflage
therapy is used to conceal lesions that are not amenable
to medical or surgical treatments. A good cosmetic cover
must appear natural, greaseless, opaque, waterproof,
long-lasting, 100% fragrance free and easy to apply [1].
It should also be applicable to all skin types, non-irritat-
ing, non-sensitizing, non-photosensitizing, and non-co-
medogenic [1]. The camouflage technique used with this
patient employs the theory of complementary colors of
light. Complementary colors are pairs of colors that are
of “opposite” hue. For example, red and cyan, green and
magenta, or blue and yellow are complementary colors
and when mixed in the proper propor tion, they produce a
neutral color such as white (especially when in light)
(Figure 2(a)). The Light-Filter-Powder contained in the
liquid foundation selectively allowed yellow light to
penetrate and thereby faded the bluish melanin deposi-
tion [7] (Figure 2(b)).
Our camouflage clinic typically treats patients with
vitiligo (and also atrophic scars, burn scars, telangiecta-
sias, nevus of Ota, etc.) and provides them with camou-
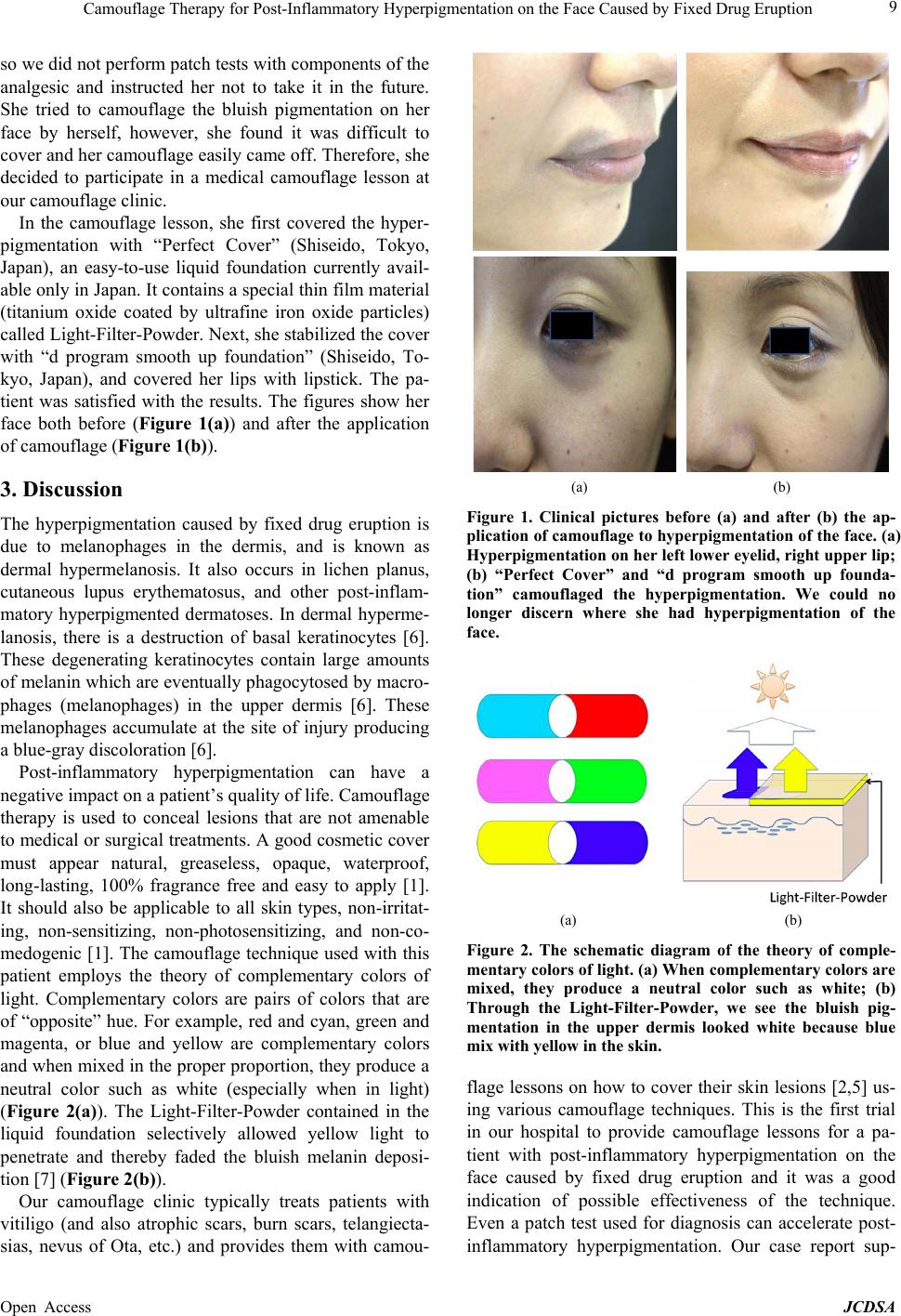
(a) (b)
Figure 1. Clinical pictures before (a) and after (b) the ap-
plication of camouflage to hyperpigmentation of the face. (a)
Hyperpigmentation on her left lower eye lid, right upper lip;
(b) “Perfect Cover” and “d program smooth up founda-
tion” camouflaged the hyperpigmentation. We could no
longer discern where she had hyperpigmentation of the
face.
(a) (b)
Figure 2. The schematic diagram of the theory of comple-
mentary colors of light. (a) When complementary colors are
mixed, they produce a neutral color such as white; (b)
Through the Light-Filter-Powder, we see the bluish pig-
mentation in the upper dermis looked white because blue
mix with yellow in the skin.
flage lessons on how to cover their skin lesions [2,5] us-
ing various camouflage techniques. This is the first trial
in our hospital to provide camouflage lessons for a pa-
tient with post-inflammatory hyperpigmentation on the
face caused by fixed drug eruption and it was a good
indication of possible effectiveness of the technique.
Even a patch test used for diagnosis can accelerate post-
inflammatory hyperpigmentation. Our case report sup-
Open Access JCDSA