 World Journal of Cardiovascular Diseases, 2013, 3, 419-427 WJCD http://dx.doi.org/10.4236/wjcd.2013.37066 Published Online October 2013 (http://www.scirp.org/journal/wjcd/) Percutaneous treatment of de novo unprotected left main stenosis in unselected consecutive patients: Experience of a high volume center Elisabetta Varani, Sabine Vecchio, Matteo Aquilina, Giuseppe Vecchi, Marco Balducelli, Valeria Frassineti, Massimo Margheri Department of Cardiology, S. Maria delle Croci Hospital, Ravenna, Italy Email: ra.hocardioemo@ausl.ra.it Received 25 July 2013; revised 25 August 2013; accepted 12 September 2013 Copyright © 2013 Elisabetta Varani et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: Percutaneous coronary intervention (PCI) has been increasingly employed to treat unpro- tected left main (ULM) stenosis, with hard endpoints similar to by-pass surgery, in patients selected by a Heart Team. Methods: From January 2008 to De- cember 2011, 317 unselected and consecutive patients with de novo ULM stenosis underwent PCI with both bare metal (BMS) and drug-eluting (DES) stents. Major adverse cardiovascular events, target lesion (TLR) and vessel (TVR) revascularization were eva- luated over a mean period of 590 ± 371 days. Results: Our population was characterized by a mean age 72 ± 10 years, high rate of acute coronar y syndrome (ACS ) (either with ST or non-ST elevation myocardial in- farction, 15.5% and 35% respectively), severe co- morbidity 16%, mean Euroscore 7 ± 3, mean Syntax Score 25 ± 9. In-hospital mortality was 6%. During the follow-up period, all-cause mortality was 16.7%, falling to 7% at the end of the follow-up, excluding patien ts pr esent ing with ACS . TLR wa s obser ved a nd treated in 15% of patients. BMS utilization, age >75 years, ACS indication, Syntax Score >32 and associ- ated peripheral artery disease were independent pre- dictors of mortality at multivariate analysis. Conclu- sions: Stenting of ULM stenosis appears to be associ- ated with a favorable mid-term outcome, even in an unselected population. Keywords: Unprotected Left Main; Percutaneous Coronary Intervention 1. INTRODUCTION Unprotected left main (ULM) percutaneous coronary intervention (PCI) has recently become a valid alterna- tive to coronary artery bypass graft (CABG) showing similar mid-term results for hard endpoints (death and myocardial infarction) even if still penalized by a higher rate of repeated revascularization in the drug-eluting stent (DES) era. Four randomized studies [1-4], 1 metanalysis [5], and several mono and multicentre registries [6-15] support these conclusions and 2010 ESC/EACT guidelines on myocardial revascularization have recognized a class IIa or IIb level of indication for ULM PCI [16] and probably they will be updated to a level of evidence A. In the metanalysis of Capodanno [5], where 1611 patients from 4 randomized clinical trials were evaluated, there were no significant differences between PCI and CABG in 1- year death (PCI 3.0% vs CABG 4.1%, p = 0.29) or myo- cardial infarction (2.8% vs 2.9%, p = 0.95), with in- creased target vessel revascularization (11.4% vs 5.4%, p < 0.001) and less frequent stroke (0.1% vs 1.7%, p = 0.013) in PCI group. A potentially higher procedural risk due to the fre- quent involvement of the bifurcation with the majority of myocardium being jeopardized has been balanced by the relative easiness of ULM PCI due to the vessel shortness and big dimensions. DES development and diffusion, the experience gained by intravascular ultrasound (IVUS) use, the benefits of post-dilation and kissing techniques and the protection given by a prolonged dual antiplatelet therapy have all led to the growth and diffusion of this procedure. The purpose of the present paper is to report the ULM PCI results of a single centre without on-site cardiac surgery, in consecutive “all comers” patients from 2008 until 2011. In all patients with de novo ULM lesions, PCI option was evaluated by clinical and interventional car- OPEN ACCESS  E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 420 diologists, and preferred over CABG, whenever a com- plete or at least a functionally complete revascularization was feasible or in presence of a high surgical risk deter- mined by comorbidities. 2. METHODS 2.1. Clinical Procedure All consecutive unselected patients treated with PCI for de novo lesions of ULM from 1.1.2008 to 31.12.2011 in our catheterization laboratory (CL) were collected in this registry. Our laboratory is a province based CL in a region with almost 400.000 inhabitants and 3 hospitals (1 hub and 2 spoke centres), with a yearly volume of more than 2000 total procedures and 1300 - 1400 PCI, resulting the high- est volume CL in the Emilia-Romagna Region and one of the most productive in Italy. All clinical, angiographic and procedural data, hospital discharge and clinical follow-up data were recorded in a retrospective/prospective database. Data relative to the clinical conditions of the last available follow-up were collected by means of clinical examinations, telephone interviews or from civil registries. All patients gave written informed consent to the pro- cedure after full discussion of the risk/benefit profile of PCI and of the surgical alternative. Indication and timing of the procedure (one stage or subsequent steps in case of multivessel coronary disease) were evaluated by an expert team (at least 2 expert interventional and one clinical cardiologists), while all procedural techniques (arterial access, provisional/in- tended two stents, type of stent, intra-aortic balloon pump (IABP), IVUS, etc.) were left to the discretion of the first operator with a strong recommendation for sec- ond generation DES utilization. All patients were pre-treated with aspirin and clopido- grel (at least 300 mg in the previous 24 hours and 75 mg the morning of the procedure). They also received aspirin 100 mg daily indefinitely and clopidogrel 75 mg daily for at least 12 months post-procedure. Angiographic follow-up 7 ± 1 months after PCI was strongly recommended and it was performed whenever possible. 2.2. Definitions Cardiac death: all deaths due to cardiac causes (ischemic and non ischemic), or all deaths without a known cause. Vascular death: all deaths due to cerebral or peripheral artery disease. Post procedural non Q myocardial infarction (MI): CKMB elevation >3 times upper normal level (UNL), without clinical or electrocardiographic (ECG) signs of ischemia. Spontaneous MI: every post-discharge elevation of CKMB or troponin above UNL associated with clinical or ECG signs of ischemia. Target Lesion Revascularization (TLR): every new target lesion (left main) revascularization comprehensive of the 5 mm pre and post target (also left anterior de- scendent artery and circumflex artery ostia). Target Vessel Revascularization (TVR): every new in- dex target vessel/s revascularization also outside the tar- get lesion. Major vascular complications: every ischemic or he- morrhagic in-hospital complications requiring surgery or transfusions. Euroscore: 30 days death risk was stratified according to the additive Euroscore, evaluating clinical, cardiac and surgical parameters [17]. Syntax Score: anatomic complexity of the patients was evaluated with the Syntax Score algorithm, which is available on the SYNTAX Score Website (www.syn taxscore.com) [18]. Complete revascularization: left main (LM) PCI and of every >70% stenosis of major epicardial coronary arteries. Functionally complete revascularization: LM PCI and of every >70% stenosis of major epicardial vessels with a vital/ischemic bed. Stent thrombosis (ST): defined on the basis of Aca- demic Research Consortium criteria [19], as definite in case of angiographic or pathologic confirmation of ST, probable in case of any unexplained death within 30 days or target vessel myocardial infarction without angiogra- phic confirmation, and possible ST defined as unex- plained death after 30 days. 2.3. Statistical Analysis Statistical analysis was performed with SAS statistical package. All continuous variables were expressed as mean ± SD and categorical variables as percentages. Comparison between groups was performed using chi-square test for categorical variables and the unpaired Student’s T test for continuous data. A two-side p value < 0.05 was considered statistically significant. Logistic regression analysis was performed to identify independent predictors of mortality, adjusted for baseline confounding characteristics that were identified on the basis of univariate analysis. The odds ratios (OR) and 95% confidence intervals (CI) were reported with two tailed probability values. 3. RESULTS From the beginning of 2008 until the end of 2011, 383 LM PCI were performed in our CL; excluding 35 proce- dures of protected LM and 31 procedures for in-stent LM Copyright © 2013 SciRes. OPEN ACCESS  E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 Copyright © 2013 SciRes. 421 OPEN ACCESS 238 (75%) restenosis, 317 were procedures on de novo ULM and were considered for this analysis. 3.1. Clinical Characteristics Clinical characteristics of treated patients are described in Table 1. Mean age was 72.6 years, with 49.5% of patients aged ≥75 years and 27% aged ≥80 years. The unselected and consecutive population is com- posed by 201 patients with acute coronary symdrome (ACS) (63%); 49 of whom (15.5% of total) with ST ele- vation myocardial infarction (STEMI) and 22 (7%) pre- senting with cardiogenic shock. Fifty patients (16%) presented severe comorbidity (39 neoplasia, 7 severe valvular disease, 2 dialysis, 2 severe cognitive deterioration), various degrees of associated peripheral artery disease (PAD) (cerebral or at the legs level) was seen in 56% of patients, mean left ventricle ejection fraction (LVEF) was 50% ± 11% and ≤40% in 20% of patients; mean additive Euroscore was 7 ± 3 (range 0 - 17). 3.2. Angiographic Characteristics Angiographic characteristics of the population are sum- marized in Table 2. LM disease was associated with multivessel coronary artery disease in more than 87% of patients, and in 28% of cases there was a chronic total occlusion (CTO), in 54 patients (17%) of the right coronary artery. Syntax Score was calculated in 311 patients; it was ≤22 in 125, between 23 and 32 in 120, and >32 in 66 patients. LM stenosis was distal in 75% of cases, with bifurcation involvement in 227 patients (72%). Procedural characteristics are summarized in Tab le 3. LM PCI was “ad hoc” in 54% of cases, with femoral access in 81% and with stent implantation in 99%, bare metal stents (BMS) 16%, DES 84%, first generation in 15 patients and second generation (mainly Xience and Biomatrix) in 249 patients. Isolated LM PCI was per- formed in 80 patients, LM and other vessel/s PCI in 237 in a unique or staged procedure; in 21 patients also an associated CTO was tempted. Mean number of implanted stents was 2.6 ± 1.5 per patient (range 0 - 10). Revascu- larization was complete in 177 patients (56%). Bifurcation LM lesions were treated as follows: provi- sional stenting strategy was adopted in 183 patients, a two stent strategy in 41 (18%), with a minicrush tech- nique in 20, T-stenting in 15, and V-stenting in 6 patients. Final kissing-balloon was performed in 92% of cases. Table 1. Clinical characteristics of 317 patients treated with PCI for de novo unprotected left main lesions. Males Age 72 ± 10 (39 - 92); 157 (49.5%) ≥ 75 y; 86 (27%) ≥ 80 y Indication to PCI STEMI 49 (15.5%) NSTEMI 111 (35%) Unstable angina 41 (14%) Stable ischemic heart disease 116 (37%) Hypertension 229 (72%) Diabetes mellitus 89 (28%) Hypercholesterolemia 234 (74%) Smoking 161 (51%) Chronic obstructive pulmonary disease 31 (10%) Peripheral artery disease 178 (56%) Previous myocardial infarction 77 (24%) Chronic kidney disease (creatinine >2 mg/dl) 22 (7%) Severe comorbidity 50 (16%) Cardiogenic shock 22 (7%) Left ventricle ejection fraction 50 ± 11; ≤35% 42 (13%) Euroscore 7 ± 3 N STEMI = non-ST elevation myocardial infarction; PCI = percutaneous coronary intervention; STEMI = ST elevation myocardial infarction.  E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 422 Table 2. Angiographic characteristics of the studied population. Coronary disease LM alone 39 (12%) LM + 1 vessel 83 (26%) LM + 2 vessels 102 (32%) LM + 3 vessels 93 (29%) Associated CTO 89 (28%) RCA CTO 54 (17%) Syntax score 25 ± 9 < 22 125 (40%) 22-32 120 (38.5%) >32 66 (21%) Left main Ostial 61 (19.2%) Body 17 (5.4%) Distal 239 (75.4%) Calcium 79 (25%) Thrombus 15 (5%) CTO = chronic total occlusion; LM = left main; RCA = right coronary artery. 3.3. In-Hospital Events There were 20 in-hospital deaths (6%), of which 16 (5%) were cardiac deaths, 24 (7.5%) post-procedural non Q MI, 7 urgent repeated PCI (2.2%); 5 of these were per- formed for residual dissection (1 of LM, 3 of circumflex artery, and 1 of left anterior descendent artery) and 2 for sub-acute ST of left anterior descendent artery (LAD) (in a patient after urgent intestinal resection). Furthermore, 1 patient presented a hemorrhagic stroke, and 10 (3%) major ischemic or hemorrhagic vascular complications. 3.4. Follow-Up Two hundred ninety seven patients were discharged alive; they were given statin therapy in 77%, beta-blocker in 67.5%, and ACE-inhibitor in 59% of cases; moreover 23 (7%) of them were on oral anticoagulant therapy (war- farin) together with aspirin 100 mg and clopidogrel 75 mg daily. Mean duration of clinical follow-up was 590 ± 371 days (range 23 - 1516) median of 525 days (i.q. 25 - 75: 281 - 881 days). One hundred and ninety patients (64%) had an an- giographic follow-up, routinely performed in 138 and clinically driven in 52 patients. Table 4 depicts clinical events at follow-up. Total mortality was 16.7%, cardiac mortality was 10% (7.9% at 1 year); excluding patients with ACS (either Table 3. Procedural characteristics. Ad hoc PCI 172 (54%) Femoral vascular access 257 (81%) Debulking 17 (5%) IVUS 44 (14%) IABP 61 (19%) GP IIb/IIIa inhibitors 33 (10%) Stent 314 (99%) BMS 50 (16%) DES 264 (84%) Biforcation technic POBA 3 Provisional stenting 183 2 stents 41 (18%) Final kissing 209/227 (92%) Stent postdilatation 254 (80%) Treated lesions LM alone 80 (25%) LM + 1 vessel 120 (38%) LM + 2 vessels 90 (28%) LM + 3 vessels 27 (8.5%) CTO 21 Total stents/patient 2.6 ± 1.5 (0 - 10) Complete revascularization 177 (56%) BMS = bare metal stent; CTO = chronic total occlusion; DES = drug eluting stent; GP = glicoprotein; IABP = intra-aortic balloon pump; IVUS = intravascular ultrasound; LM = left main; PCI = percutaneous coronary intervention; POBA = plein old balloon angioplasty. with ST or non ST elevation myocardial infarction) as indication for the index procedure, total mortality falls to 3.8% at 1 year and 7% at the end of follow-up. Among cardiac deaths, 4 were undetermined possibly due to ST: 1 at 185 days in a patient with moderate to severe mitral regurgitation, 1 at 417 days, 1 at 487 days after a red blood cells transfusion for acute anemia and 1 at 231 days for a documented ventricular fibrillation, while no cases of definite ST were documented an- giographically or anatomically. A repeated revascularization procedure for a LM le- sion was necessary in 15% of cases (47/48 cases were treated with a repeated PCI and only one case with CABG), in 13 patients this was due to a LM edge restenosis, in 16 to a distal LM or LAD and circumflex artery ostial lesion, in 17 to an isolated circumflex ostial Copyright © 2013 SciRes. OPEN ACCESS  E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 423 Table 4. Clinical events at follow up. 12 months At follow-up (median 525 days) Total death 41 (12.9%) 53 (16.7%) Cardiac death 25 (7.9%) 31 (10%) Vascular death 7 (2.2%) 8 (2.5%) Other causes death 9 (2.8%) 14 (4.4%) Total death excluding patients with STEMI 30/268 (11%) 40/268 (14.9%) Total death excluding patients with STEMI/NSTEMI 6/157 (3.8%) 11/157 (7%) Myocardial infarction (all NSTEMI) 18 (5.7%) 20 (6.3%) LM TLR 43 (13.6%) 48 (15%) Other vessel TVR 35 (11%) 42 (13.2%) De novo lesion PCI 29 (9.1%) 41 (12.9%) Stroke 2 (0.6%) 3 (0.9%) Definite stent thrombosis 0 0 Possible stent thrombosi 2 (0.6%) 4 (1.2%) LM = left main; NSTEMI = Non ST elevation myocardial infarction; PCI = percutaneous coronary intervention; STEMI = ST elevation myocardial infarction; TLR = target lesion revascularization; TVR = target vessel revascularization. lesion and in 2 to an isolated LAD ostial lesion. TLR was clinically driven only in 25 patients, with an angiographic follow-up due to symptoms or inducible ischemia. Clinically driven TLR was performed at a mean time of 208 days from the index procedure, a mean of 30 days before TLR performed during a routine an- giographic follow-up (233 days). Forty-two patients (13.2%) had a repeated procedure on an already treated vessel and 41 (12.9%) had a PCI of another vessel/de nov o lesion. At univariate analysis, variables correlated to total mortality were age, ACS as indication for coronary an- giography, ad hoc PCI, serum creatinine, presence of chronic obstructive pulmonary disease and PAD, LVEF, Killip class 3-4, associated 1 - 3 vessel disease, Syntax Score, presence of thrombus, IABP utilization, BMS implantation, pre-PCI TIMI flow <3, an incomplete re- vascularization. Independent predictors of mortality at multivariate analysis were: BMS utilization (<0.001), age >75 years (p = 0.006), ACS indication (either STEMI and non ST elevation MI-NSTEMI) (p = 0.017), Syntax Score >32 (p = 0.010), and associated PAD (p = 0.042) (Table 5). Comparisons between patients treated with DES or BMS and between the three Syntax Score groups are shown in Table 6 and 7. 4. DISCUSSION The population studied represents a real world scenario, being composed by unselected, consecutive patients ad- mitted to a high volume hub centre without on-site car- diac surgery. Most of the patients were admitted with an ACS, who had frequent comorbidities and a complex anatomic situation frequently associated with multivessel disease (Tables 1 and 2). The peculiarity of our LM PCI experience lies in the absence of a proper “heart team” and in the presence of experienced operators leading to the preferred choice of the percutaneous revascularization option if possible (at least a functionally complete revascularization) without employing more than 4 - 5 stents, and in the absence of absolute contraindications to DES. The main intent was to avoid adverse events related to CABG, even those less known or not routinely reported (i.e., sequelae of surgical wounds, psycho-intellective deterioration) that signifi- cantly impact on morbidity and on the quality of life and costs [20]. Our results show a satisfactory short-term outcome, with an acceptable in-hospital mortality considering the type of patients (15% STEMI, comorbidity, age, mean Euroscore 7 ± 3); moreover, also at 12 months, excluding patients with acute MI (STEMI and NSTEMI) total mor- tality results 3.8% (Table 4), similar to the 12-month mortality of the LM subgroup of the Syntax trial that did not enroll patients with acute MI (2). Our results also do well in comparison with the experience of the large DELTA Registry (6), with cardiac mortality of 10% ver- sus 6.8%, if we considered that our patients were older (mean age 72 ± 10 vs 65.8 ± 1.1 years), and presented more frequently an ACS (STEMI 15% vs 2.9%, NSTEMI Copyright © 2013 SciRes. OPEN ACCESS 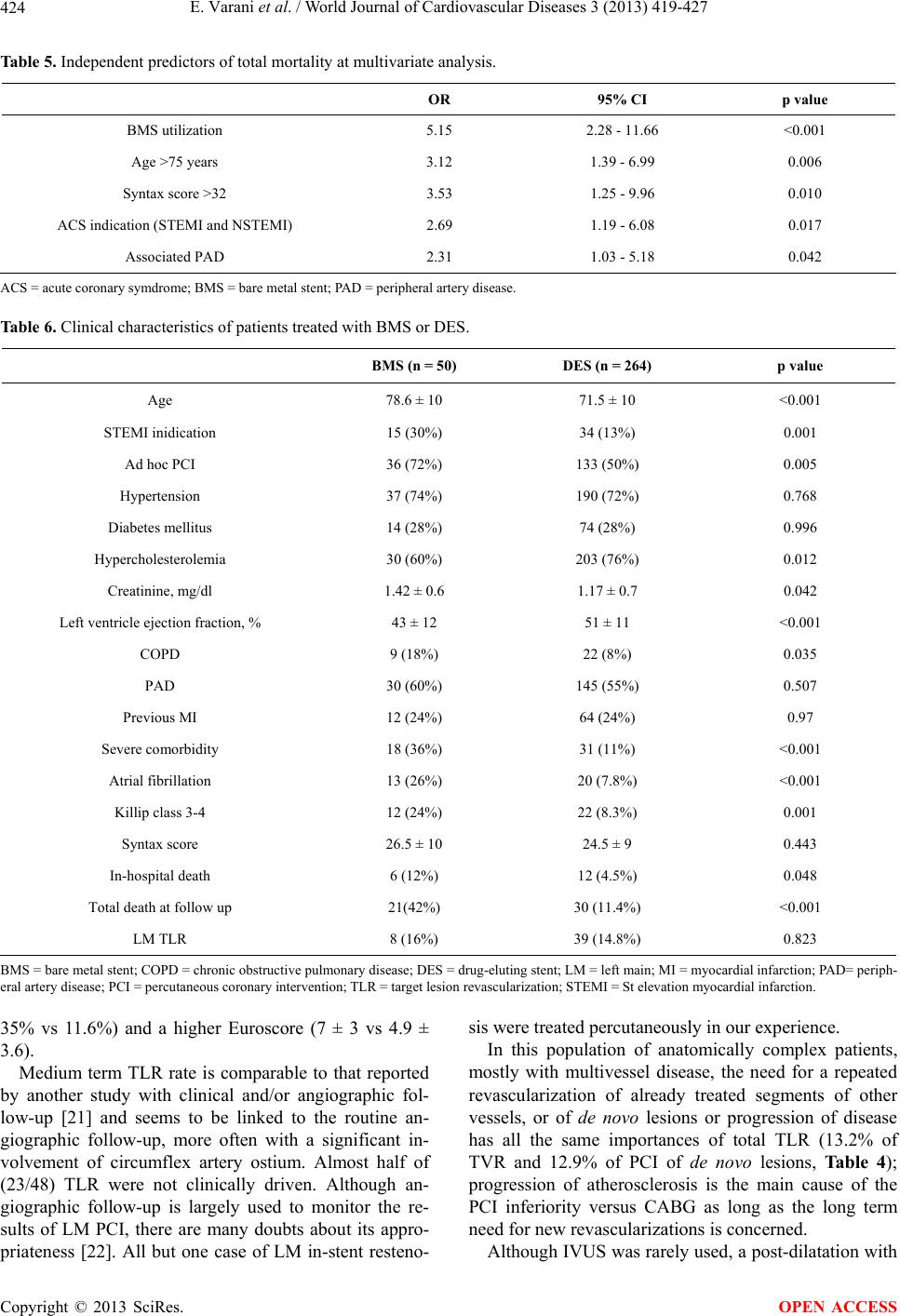 E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 424 Table 5. Independent predictors of total mortality at multivariate analysis. OR 95% CI p value BMS utilization 5.15 2.28 - 11.66 <0.001 Age >75 years 3.12 1.39 - 6.99 0.006 Syntax score >32 3.53 1.25 - 9.96 0.010 ACS indication (STEMI and NSTEMI) 2.69 1.19 - 6.08 0.017 Associated PAD 2.31 1.03 - 5.18 0.042 ACS = acute coronary symdrome; BMS = bare metal stent; PAD = peripheral artery disease. Table 6. Clinical characteristics of patients treated with BMS or DES. BMS (n = 50) DES (n = 264) p value Age 78.6 ± 10 71.5 ± 10 <0.001 STEMI inidication 15 (30%) 34 (13%) 0.001 Ad hoc PCI 36 (72%) 133 (50%) 0.005 Hypertension 37 (74%) 190 (72%) 0.768 Diabetes mellitus 14 (28%) 74 (28%) 0.996 Hypercholesterolemia 30 (60%) 203 (76%) 0.012 Creatinine, mg/dl 1.42 ± 0.6 1.17 ± 0.7 0.042 Left ventricle ejection fraction, % 43 ± 12 51 ± 11 <0.001 COPD 9 (18%) 22 (8%) 0.035 PAD 30 (60%) 145 (55%) 0.507 Previous MI 12 (24%) 64 (24%) 0.97 Severe comorbidity 18 (36%) 31 (11%) <0.001 Atrial fibrillation 13 (26%) 20 (7.8%) <0.001 Killip class 3-4 12 (24%) 22 (8.3%) 0.001 Syntax score 26.5 ± 10 24.5 ± 9 0.443 In-hospital death 6 (12%) 12 (4.5%) 0.048 Total death at follow up 21(42%) 30 (11.4%) <0.001 LM TLR 8 (16%) 39 (14.8%) 0.823 BMS = bare metal stent; COPD = chronic obstructive pulmonary disease; DES = drug-eluting stent; LM = left main; MI = myocardial infarction; PAD= periph- eral artery disease; PCI = percutaneous coronary intervention; TLR = target lesion revascularization; STEMI = St elevation myocardial infarction. 35% vs 11.6%) and a higher Euroscore (7 ± 3 vs 4.9 ± 3.6). Medium term TLR rate is comparable to that reported by another study with clinical and/or angiographic fol- low-up [21] and seems to be linked to the routine an- giographic follow-up, more often with a significant in- volvement of circumflex artery ostium. Almost half of (23/48) TLR were not clinically driven. Although an- giographic follow-up is largely used to monitor the re- sults of LM PCI, there are many doubts about its appro- priateness [22]. All but one case of LM in-stent resteno- sis were treated percutaneously in our experience. In this population of anatomically complex patients, mostly with multivessel disease, the need for a repeated revascularization of already treated segments of other vessels, or of de novo lesions or progression of disease has all the same importances of total TLR (13.2% of TVR and 12.9% of PCI of de novo lesions, Table 4); progression of atherosclerosis is the main cause of the PCI inferiority versus CABG as long as the long term need for new revascularizations is concerned. Although IVUS was rarely used, a post-dilatation with Copyright © 2013 SciRes. OPEN ACCESS  E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 425 Table 7. Clinical characteristics and events in the three Syntax score groups. <22 22 - 33 >33 p N˚ patients 125 120 66 Age 71 ± 10 74 ± 10 73 ± 10 0.086 LVEF, % 53 ± 11 49 ± 11 47 ± 12 0.005 Creatinine, mg/dl 1.04 ± 0.4 1.4 ± 1 1.17 ± 0.46 0.001 Killip class 3-4 10 (8%) 12 (10%) 13 (19%) 0.044 Previous MI 22 (17.6%) 34 (28%) 20 (30%) 0.067 Euroscore 6.4 ± 3.6 7.4 ± 3.2 7.5 ± 3.9 0.038 Associated CTO 6 (4.8%) 35 (29%) 35 (53%) <0.001 Other vessel treated 61 (49%) 100 (83%) 60 (91%) <0.001 Complete revascularization 101 (81%) 55 (46%) 20 (30%) <0.001 In-hospital death 6 (4.8%) 6 (5%) 7 (10.6%) 0.227 Total death at follow up 13 (10.4%) 20 (16.6%) 18 (27.3%) 0.011 LM TLR 19 (15%) 18 (15%) 11 (16.5%) 0.951 Other vessel TVR 14 (11%) 20 (16.5%) 8 (12%) 0.426 CTO = chronic total occlusion, LM = left main; LVEF = left ventricle ejection fraction, MI = myocardial infarction, TLR = target lesion revascularization, TVR = target vessel revascularization. a non-compliant balloon (254/317, 80%) and final kiss- ing-balloon in almost all bifurcation lesions were fre- quently performed (Ta b l e 3). This technical feature, de- rived from the results of IVUS-guided stenting studies [23], may account for the low prevalence of ST (no case of definite ST, 4 unknown cause death cases, possibly due to ST). Multivariate analysis shows a strong correlation of BMS utilization with total mortality. This result deserves a comment because it is likely due to the presence of a higher risk profile (older age, more often STEMI presen- tation, severe comorbidities, necessity for oral antico- agulation, lower LVEF and compromised hemodynamic status, Ta b le 6 ), which leads to the choice of BMS uti- lization in order to avoid prolonged dual antiplatelet therapy or is based on the supposedly worse cost/efficacy ratio in very compromised clinical conditions. Probably BMS utilization alone is not really an independent pre- dictor of mortality but rather an indicator of a worse clinical setting. This hypothesis is supported by the very high acute in-hospital mortality of this subset of patients (6/50, 12% vs 13/264, 4.5% in the BMS and DES group respectively), without a concomitant higher TVR versus DES group in patients who survived the in-hospital phase (Table 6). We cannot derive a difference between the first and sec- ond generations DES from our data, even if recent stud- ies showed no significant advantage of the latter one [24]. The presence of a Syntax Score >32 is also a predictor of mortality and this result is in line with the increased major adverse event rate at 3rd and 5th years in higher Syntax Score subgroup in Syntax trial [25,26]. Notably, our patients with Syntax Score >32 had lower LVEF, higher Euroscore, more frequent Killip class 3-4 (Table 6). All these features made us to prefer percutaneous coronary treatment over a surgical approach. In our experience, besides anatomical situation, clini- cal features (age, ACS presentation, PAD) are important determinants of prognosis. An integrated clinical judg- ment may be represented by the new risk scores (global and clinical Syntax Score) [27,28], and is mandatory to choose the right revascularization strategy for each indi- vidual patient in order to guarantee the best benefit-to- risk ratio and quality of life. REFERENCES [1] Buszman, P.E., Buszman, P.P., Kiesz, R.S., Bochenek, A., Trela, B., Konkolewska, M., Wallace-Bradley, D., Wilc- zynski, M., Banasiewicz-Szkrobla, I., Peszek-Przybyla, E., Kkrol, M., Kondys, M., Milewski, K., Wiernek, S., Debinski, M., Zurakowski, A., Martin, J.L. and Tendera, M. (2009) Early and long-term results of unprotected left main coronary artery stenting: The LEMANS (left main coronary artery stenting) registry. Journal of the Ameri- can College of Cardiology, 54, 1500-1511. http://dx.doi.org/10.1016/j.jacc.2009.07.007 [2] Morice, M.C., Serruys, P.W., Kappetein, A.P., Feldman, T.E., Stahle, E., Colombo, A., Mack, M.J., Holmes, D.R., Copyright © 2013 SciRes. OPEN ACCESS  E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 426 Torracca, L., van Es, G.-A., Leadley, K., Dawkins, K. and Mohr, F. (2010) Outcomes in patients with de novo left main disease treated with either percutaneous coro- nary intervention using paclitaxel-eluting stents or coro- nary artery bypass graft treatment in the synergy between percutaneous coronary intervention with taxus and car- diac surgery (SYNTAX) trial. Circulation, 121, 2645- 2653. http://dx.doi.org/10.1161/CIRCULATIONAHA.109.8992 11 [3] Boudriot, E., Thiele, H., Walther, T., Liebetrau, C., Boeckstegers, P., Pohl, T., Reichart, B., Mudra, H., Beier, F., Gansera, B., Neumann, F.-J., Gick, M., Zietak, T., Desch, S., Schuler, G. and Mohr, F.-W. (2011) Random- ized comparison of percutaneous coronary intervention with sirolimus-eluting stents versus coronary artery by- pass grafting in unprotected left main stem stenosis. Journal of the American College of Cardiology, 57, 538- 545. http://dx.doi.org/10.1016/j.jacc.2010.09.038 [4] Park, S.J., Kim, Y.H., Park, D.W., Yun, S.C., Ahn, J.M., Song, H.G., Lee, J.Y., Kim, W.J., Kang, S.J., Lee, S.W., Lee, C.W., Park, S.W., Chung, C.H., Lee, J.W., Lim, D.S., Rha, S.W., Lee, S.G., Gwon, H.C., Kim, H.S., Chae, I.H., Jang, Y., Jeong, M.H., Tahk, S.J. and Seung, K.B. (2011) Randomized trial of stents versus bypass surgery for left main coronary artery disease. New England Jour- nal of Medicine, 364, 1718-1727. http://dx.doi.org/10.1056/NEJMoa1100452 [5] Capodanno, D., Stone, G.W., Morice, M.C., Bass, T.A. and Tamburino, C. (2011) Percutaneous coronary inter- vention versus coronary artery bypass graft surgery in left main coronary artery disease. A meta-analysis of ran- domized clinical data. Journal of the American College of Cardiology, 58, 1426-1432. http://dx.doi.org/10.1016/j.jacc.2011.07.005 [6] Chieffo, A., Meliga, E., Latib, A., Park, S.-J., Onuma, Y., Capranzano, P., Valgimigli, M., Jegere, S., Makkar, R.R., Palacios, I.F., Kim, Y.-H., Buszman, P.E., Chakravarty, T., Sheiban, I., Mehran, R., Naber, C., Margery, R., Ag- nihotri, A., Marra, S. and Capodanno, D. (2012) Drug- eluting stent for left main coronary artery disease. The DELTA registry: A multicenter registry evaluating per- cutaneous coronary intervention versus coronary artery bypass grafting for left main treatment. JACC: Cardio- vascular Interventions, 5, 718-727. http://dx.doi.org/10.1016/j.jcin.2012.03.022 [7] Kim, Y.-H., Dangas, G.D., Solinas, E., Aoki, J., Parise, H., Kimura, M., Franklin-Bond, T., Dasgupta, N.K., Kir- tane, A.J., Moussa, I., Lansky, A.J., Collins, M., Stone, G.W., Leon, M.B., Moses, J.W. and Mehran, R. (2008) Effectiveness of drug-eluting stent implantation for pa- tients with unprotected left main coronary artery stenosis. American Journal of Cardiology, 101, 801-806. http://dx.doi.org/10.1016/j.amjcard.2007.10.052 [8] Lee, M.S., Kapoor, N., Jamal, F., Czer, L., Aragon, J., Forrester, J., Kar, S., Dohad, S., Kass, R., Neal, E., Trento, A., Shah, P.K. and Makkar, R.R. (2006) Com- parison of coronary artery bypass graft surgery with per- cutaneous coronary intervention with drug-eluting stents for unprotected left main coronary artery disease. Journal of the American College of Cardiology, 47, 864-870. http://dx.doi.org/10.1016/j.jacc.2005.09.072 [9] Palmerini, T., Marzocchi, A., Tamburino, C., Sheiban, I., Margheri, M., Vecchi, G., Sangiorgi, G., Santarelli, A., Bartorelli, A., Briguori, C., Vignali, L., Di Pede, F., Ra- mondo, A., Inglese, L., De Carlo, M., Bolognese, L., Be- nassi, A., Palmieri, C., Filippone, V. and Sangiorgi, D. (2008) Two-year clinical outcome with drug-eluting stents versus bare-metal stents in a real-world registry of un- protected left main coronary artery stenosis from the Ital- ian Society of Invasive Cardiology. American Journal of Cardiology, 102, 1463-1468. http://dx.doi.org/10.1016/j.amjcard.2008.07.030 [10] Sheiban, I., Meliga, E., Moretti, C., Biondi-Zoccai, G.G.L., Rosano, G., Sciuto, F., Grosso Marra, W., Omedè, P., Gerasimou, A. and Trevi, G.P. (2007) Long-term clinical and angiographic outcomes of treatment of un- protected left main coronary artery stenosis with siroli- mus-eluting stents. American Journal of Cardiology, 100, 431-435. http://dx.doi.org/10.1016/j.amjcard.2007.03.041 [11] Valgimigli, M., Malagutti, P., Aoki, J., Garcia-Garcia, H.M., Rodriguez Granillo, G.A., vanMieghem, C.A.G., Ligthart, J.M., Ong, A.T.L., Sianos, G., Regar, E., Van Domburg, R.T., De Feyter, P., de Jaegere, P. and Serruys, P.W. (2006) Sirolimus-eluting versus paclitaxel-eluting stent implantation for the percutaneous treatment of left main coronary artery disease: A combined RESEARCH and T-SEARCH long-term analysis. Journal of the Ame- rican College of Cardiology, 47, 507-514. http://dx.doi.org/10.1016/j.jacc.2005.09.040 [12] Brener, S.J., Galla, J.M., Bryant III, R., Sabik III, J.F. and Ellis, S.G. (2008) Comparison of percutaneous versus surgical revascularization of severe unprotected left main coronary stenosis in matched patients. American Journal of Cardiology, 101, 169-172. http://dx.doi.org/10.1016/j.amjcard.2007.08.054 [13] Chieffo, A., Magni, V., Latib, A., Maisano, F., Ielasi, A., Montorfano, M., Carlino, M., Godino, C., Ferraro, M., Calori, G., Alfieri, O. and Colombo, A. (2010) 5-year outcomes following percutaneous coronary intervention with drug-eluting stent implantation versus coronary ar- tery bypass graft for unprotected left main coronary le- sions: The Milan experience. JACC: Cardiovascular In- terventions, 3, 595-601. http://dx.doi.org/10.1016/j.jcin.2010.03.014 [14] Meliga, E., Garcia-Garcia, H.M., Valgimigli, M., Chieffo, A., Biondi-Zoccai, G., Maree, A.O., Cook, S., Reardon, L., Moretti, C., De Servi, S., Palacios, I.F., Windecker, S., Colombo, A., van Domburg, R., Sheiban, I. and Serruys, P.W. (2008) Longest available clinical outcomes after drug-eluting stent implantation for unprotected left main coronary artery disease: The DELFT (drug eluting stent for LeFt main) registry. Journal of the American College of Cardiology, 51, 2212-2219. http://dx.doi.org/10.1016/j.jacc.2008.03.020 [15] Park, D.-W., Seung, K.B., Kim, Y.H., Lee, J.-Y., Kim, W.-J., Kang, S.-J., Lee, S.-W., Lee, C.W., Park, S.-W., Yun, S.-C., Gwon, H.-C., Jeong, M.-H., Jang, Y.-S., Kim, H.-S., Kim, P.J., Seong, I.-W., Park, H.S., Ahn, T., Chae, I.-H. and Tahk, S.-J. (2010) Long-term safety and effi- cacy of stenting versus coronary artery bypass grafting for unprotected left main coronary artery disease: 5-year Copyright © 2013 SciRes. OPEN ACCESS  E. Varani et al. / World Journal of Cardiovascular Diseases 3 (2013) 419-427 Copyright © 2013 SciRes. 427 OPEN ACCESS results from the MAIN-COMPARE (revascularization for unprotected left main coronary artery stenosis: Compari- son of percutaneous coronary angioplasty versus surgical revascularization) registry. Journal of the American Col- lege of Cardiology, 56, 117-124. http://dx.doi.org/10.1016/j.jacc.2010.04.004 [16] Wijns, W., Kolh, P., Danchin, N., et al. (2010) Guidelines on myocardial revascularization: The task force on myo- cardial revascularization of the European Society of Car- diology (ESC) and the European Association for Cardio- Thoracic Surgery (EACTS). European Heart Journal, 31, 2501-2555. http://dx.doi.org/10.1093/eurheartj/ehq277 [17] Roques, F., Michel, P., Goldstone, A.R. and Nashef, S.A. (2003) The logistic Euro-SCORE. European Heart Jour- nal, 24, 881-882. http://dx.doi.org/10.1016/S0195-668X(02)00799-6 [18] Sianos, G., Morel, M.A., Kappetein, A.P., Morice, M.-C., Colombo, A., Dawkins, K., van den Brand, M., van Dyck, N., Russell, M.E. and Serruys, P.W. (2005) The SYN- TAX score: An angiographic tool grading the complexity of coronary artery disease. EuroIntervention, 1, 219-227. [19] Cutlip, D.E., Windecker, S., Mehran, R., Boam, A., Cohen, D.J., van Es, G.-A., Steg, P.G., Morel, M.-A., Mauri, L., Vranckx, P., McFadden, E., Lansky, A., Ha- mon, M., Krucoff, M.W. and Serruys, P.W. (2007) Clini- cal end points in coronary stent trials: A case for stan- dardized definitions. Circulation, 115, 2344-2351. http://dx.doi.org/10.1161/CIRCULATIONAHA.106.6853 13 [20] Varani, E., Balducelli, M., Vecchi, G., Aquilina, M. and Maresta, A. (2007) Comparison of multiple drug-eluting stent percutaneous coronary intervention and surgical re- vascularization in patients with multivessel coronary ar- tery disease: One-year clinical results and total treatment costs. Journal of Invasive Cardiology, 19, 469-475. [21] Lee, J.-Y., Park, D.-W., Kim, Y.-H., Yun, S.-C., Kim, W.-J., Kang, S.-J., Lee, S.-W., Lee, C.-W., Park, S.-W. and Park, S.-J. (2011) Incidence, predictors, treatment, and long-term prognosis of patients with restenosis after drug-eluting stent implantation for unprotected left main coronary artery disease. Journal of the American College of Cardiology, 57, 1349-1358. http://dx.doi.org/10.1016/j.jacc.2010.10.041 [22] Biondi-Zoccai, G.G., Giraudi, E., Moretti, C., Sciuto, F., Omedè, P., Sillano, D., Garrone, P., Treevi, G.P. and Sheiba, I. (2010) Impact of routine angiographic follow up after percutaneous coronary drug-eluting stenting for unprotected left main disease: The Turin registry. Clini- cal Research in Cardiology, 99, 235-242. http://dx.doi.org/10.1007/s00392-009-0112-3 [23] Puri, R., Kapadia, S.R., Nicholls, S.J., Harvey, J.E., Kataoka, Y. and Tuzcu, E.M. (2012) Optimizing out- comes during left main percutaneous coronary interven- tion with intravascular ultrasound and fractional flow re- serve: The current state of evidence. JACC: Cardiovas- cular Interventions, 5, 697-707. http://dx.doi.org/10.1016/j.jcin.2012.02.018 [24] Kim, Y.-H., Park, D.-W., Ahn, J.-M., Yun, S.-C., Song, H.G., Lee, J.-Y., Kim, W.-J., Kang, S.-J., Lee, S.-W., Lee, C.W., Park, S.-W., Jang, Y., Jeong, M.-H., Kim, H.-S., Hur, S.-H., Rha, S.-W., Lim, D.-S., Her, S.-H., Seung, K.B. and Seong, I.-W. (2012) Everolimus-eluting stent implantation for unprotected left main coronary artery stenosis. The PRECOMBAT-2 (premier of randomized comparison of bypass surgery versus angioplasty using sirolimus-eluting stent in patients with left main coronary artery disease) study. JACC: Cardiovascular Interven- tions, 5, 708-717. http://dx.doi.org/10.1016/j.jcin.2012.05.002 [25] Kappetein, A.P., Feldman, T.E., Mack, M.J., Morice, M.-C., Holmes, D.R., Stahle, E., Dawkins, K.D., Mohr, F.W., Serruys, P.W. and Colombo, A. (2011) Comparison of coronary bypass surgery with drug-eluting stenting for the treatment of left main and/or three-vessel disease: 3-year follow-up of the SYNTAX trial. European Heart Journal, 32, 2125-2134. http://dx.doi.org/10.1093/eurheartj/ehr213 [26] Mohr, F.W., Morice, M.-C., Kappetein, A.P., Feldman, T.E., Stahle, E., Colombo, A., Mack, M.J., Holmes, D.R., Morel, M.-A., Van Dyck, N., Houle, V.M., Dawkins, K.D. and Serruys, P.W. (2013) Coronary artery bypass graft surgery versus percutaneous coronary intervention in pa- tients with three-vessel disease and left main coronary disease: 5-year follow up of the randomized, clinical SYNTAX trial. Lancet, 381, 629-638. http://dx.doi.org/10.1016/S0140-6736(13)60141-5 [27] Serruys, P.W., Farroq, V., Vranckx, P., Girasis, C., Bru- galetta, S., Garcia-Garcia, H.M., Holmes, D.R., Kap- petein, A.-P., Mack, M.J., Feldman, T., Morice, M.-C., Stahle, E., James, S., Colombo, A., Pereda, P., Huang, J., Morel, M.-A., vanes, G.-A., Kawkins, K.D. and Mohr, F.W. (2012) A global risk approach to identify patients with left main or 3-vessel disease who could safely and efficaciously be treated with percutaneous coronary in- tervention. JACC: Cardiovascular Interventions, 5, 606- 617. http://dx.doi.org/10.1016/j.jcin.2012.03.016 [28] Garg, S., Sarno, G., Garcia-Garcia, H.M., Girasis, C., Wykrzykowska, J., Dawkins, K.D. and Serruys, P.W. (2010) A new tool for the risk stratification of patients with complex coronary artery disease: The clinical SYNTAX score. Circulation: Cardiovascular Interven- tions, 3, 317-326. http://dx.doi.org/10.1161/CIRCINTERVENTIONS.109.9 14051
|