Lichen Planopilarisis a Common Scarring Alopecia among Iraqi Population
38
Figure 5. Erythematous scarring alopecia in female patient
with discoid lupus erythematosus.
Irregular scarring areas that simulate moth eaten
alopecia are characteristic feature of LPP scarring and
can be considered as the most important differentiat-
ing point between DLE and LPP.
The activity of the disease is mainly central in DLE
lesions while the activity of LPP is mainly at the pe-
riphery of the scarring patch in the form of hyperk-
eratotic follicular papules [6].
The associated manifestation of other body regions
also can help approach the diagnosis; The lesions in
DLE commonly affect the sun exposed parts, particu-
larly on the cheeks, nose and the ears [13,14] with
typical discoid lesions, while LPP lesions, as demon-
strated by the present work, commonly present with a
symptomatic truncal follicular papules which might be
scarring or not (Figure 2).
Although both conditions sh are lichenod lymphocytic
infiltration of basal ep ithelium and follicular structure
with vacuolar interface dermatitis, but DLE lesions
are characterized by deeper follicular inflammation
and perieccrine lymphocytic infiltration while the
perifollicular inflammation in LPP is more superficial
and limited to the upper segment of the hair follicle [8]
(Figure 6).
The pathologic changes in active LPP are mainly fol-
licular without affection of the epidermis while in
DLE the changes are both epidermal (vacuolar inter-
face dermatitis) and dermal (interfollicular mucin
deposition) [15]. We also noticed an important ob-
servation where the inflammatory process involved
the area of bulge region causing fibrosis and leaving
the lower segment of the hair follicle intact. This
pathologic finding may be responsible for the perma-
nent damage to the hair organ and support the theory
that the bulge region is the site of hair regeneration
[16].
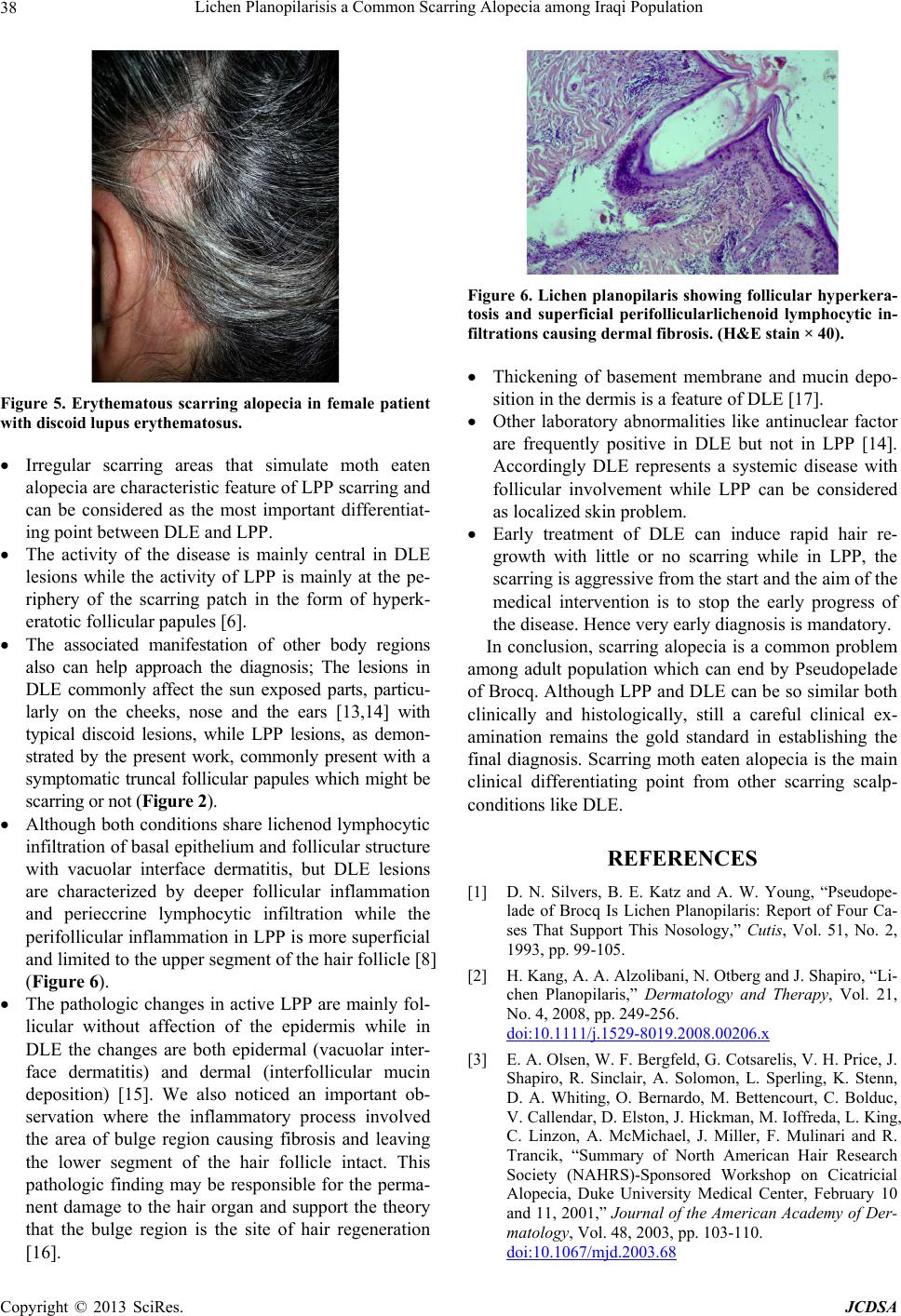
Figure 6. Lichen planopilaris showing follicular hyperkera-
tosis and superficial perifollicularlichenoid lymphocytic in-
filtrations causing dermal fibrosis. (H&E stain × 40).
Thickening of basement membrane and mucin depo-
sition in the dermis is a feature of DLE [17].
Other laboratory abnormalities like antinuclear factor
are frequently positive in DLE but not in LPP [14].
Accordingly DLE represents a systemic disease with
follicular involvement while LPP can be considered
as localized skin problem.
Early treatment of DLE can induce rapid hair re-
growth with little or no scarring while in LPP, the
scarring is aggressive from the start and the aim of the
medical intervention is to stop the early progress of
the disease. Hence very early diagnosis is mandatory.
In conclusion, scarring alopecia is a common problem
among adult population which can end by Pseudopelade
of Brocq. Although LPP and DL E can be so similar both
clinically and histologically, still a careful clinical ex-
amination remains the gold standard in establishing the
final diagnosis. Scarring moth eaten alopecia is the main
clinical differentiating point from other scarring scalp-
conditions like DLE.
REFERENCES
[1] D. N. Silvers, B. E. Katz and A. W. Young, “Pseudope-
lade of Brocq Is Lichen Planopilaris: Report of Four Ca-
ses That Support This Nosology,” Cutis, Vol. 51, No. 2,
1993, pp. 99-105.
[2] H. Kang, A. A. Alzolibani, N. Otberg and J. Shapiro, “Li-
chen Planopilaris,” Dermatology and Therapy, Vol. 21,
No. 4, 2008, pp. 249-256.
doi:10.1111/j.1529-8019.2008.00206.x
[3] E. A. Olsen, W. F. Bergfeld, G. Cotsarelis, V. H. Price, J.
Shapiro, R. Sinclair, A. Solomon, L. Sperling, K. Stenn,
D. A. Whiting, O. Bernardo, M. Bettencourt, C. Bolduc,
V. Callendar, D. Elston, J. Hickman, M. Ioffreda, L. King,
C. Linzon, A. McMichael, J. Miller, F. Mulinari and R.
Trancik, “Summary of North American Hair Research
Society (NAHRS)-Sponsored Workshop on Cicatricial
Alopecia, Duke University Medical Center, February 10
and 11, 2001,” Journal of the American Academy of Der-
matology, Vol. 48, 2003, pp. 103-110.
doi:10.1067/mjd.2003.68
Copyright © 2013 SciRes. JCDSA