International Journal of Medical Physics, Clinical Engineering and Radiation Oncology
Vol.03 No.04(2014), Article ID:50551,7 pages
10.4236/ijmpcero.2014.34027
Does Change in the Effect of Source Strength of the High Dose Rate 192Iridium Radio-Isotope on Local Control and Late Normal Tissue Toxicity (Bladder and Rectum) in the Treatment of Carcinoma Cervix
K. Sudhakar1, K. Gunaseelan1*, K. S. Reddy1, K. Saravanan2, N. V. Vinin1
1Department of Radiotherapy, JIPMER, Regional Cancer Centre, Puducherry, India
2Department of Medical Physics, JIPMER, Regional Cancer Centre, Puducherry, India
Email: *gunapgi@gmail.com
Copyright © 2014 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 8 August 2014; revised 6 September 2014; accepted 4 October 2014
ABSTRACT
Aim: To analyse and assess the effect of dose rate of 192ir-source strength on late complications and local control rate during treatment of carcinoma cervix. Materials and Methods: One hundred and two cases of carcinoma cervix were included in the study. All patients were treated with a curative intent with radical dose of radiation as per the department protocol. All patients were treated with both EBRT plus Brachytherapy with Inj. Cisplatin 40 mg/m2 weekly. Patients were divided into 2 groups based on activity i.e. group A (10-6Ci) and group B (5-2Ci). After brachytherapy, point doses were analysed based on ICRU 38 recommendations. During follow up, morbidities were evaluated using RTOG grading system. Results: There was no difference in local control and distant metastasis in both groups after six months of follow up. Late Complications were comparable in both groups irrespective of source strength. Bladder complications were minimal with no significant difference in both study groups. Further Patients were divided into four groups i.e. BED of ICRU rectal point (<100 Gy3 and ≥100 Gy3) and source strength (10-6Ci and 5-2Ci), when BED was >100 Gy3 resulted in higher late rectal complication rate (P < 0.05) compared to BED < 100 Gy3. Conclusion: This study suggests that change in source activity did not make a difference in local control, late rectal and bladder morbidities at 6 months of follow up. Longer follow up is required to assess long term results and morbidities.
Keywords:
Source Strength, Carcinoma Cervix, ICBT, Local Control, Distant Metastasis, Late Morbidity

1. Introduction
Some components, such as multi-leveled equations, graphics, and tables are not prescribed, although the various table text styles are Cancer of the cervix is the most common cancer in India [1] . Majority of patients present with locally advanced stage and nearly 70% belong to FIGO stage II b-or III. Concurrent Radiotherapy is the standard of treatment option in locally advanced cancers. External Beam Radiotherapy and Brachytherapy are widely practicing in many centers in the world as well as in India [2] [3] . Over the years the external beam radiotherapy has been well standardized and uniform but the brachytherapy component has experienced tremendous variation from LDR to HDR Intracavitary radiation therapy.
While there are four decades of published literature on the efficacy of HDR brachytherapy over LDR brachytherapy, variation in fractionation schedules and its effect of change in dose rate on treatment outcome and normal tissue complications is well reported but very few reports on the effect of source strength of HDR brachytherapy on local control and late rectal and bladder morbidity is available. The probable reason for such under reporting is due to variation in the fractionation schedules between various institutions.192Ir Radioisotope which is commonly used as HDR Brachytherapy source and has very short half-life of 78.3 days. In India, source is being utilized even when the activity is less than 2Ci mainly to economize the source cost. At the same time efficacy of low source activity in relation to disease control is still remain unanswered in clinical settings. Hence this study was undertaken to compare and understand the radiobiological relationships of Iridium source activity on local control and late rectal, bladder morbidities.
2. Materials and Methods
2.1. External Beam Radiotherapy (EBRT)
For EBRT treatment was delivered using 6-MV linear accelerator. For all the patients, simulation of the pelvic treatment fields was done on Acuity Varian simulator machine. Total dose of external beam radiation therapy (EBRT) to the whole pelvis was 46 Gy in 23 fractions over 5 weeks. Dose delivered to pelvis by two field technique (anterior-posterior fields) and patients with wider separation were considered for four cross field technique. Midline shielding was used up to 50 Gy. All patients received concurrent weekly I.V Cisplatin dose of 40 mg/m2.
2.2. HDR Intracavitary Brachytherapy
Intracavitary application was done on outpatient basis under I.V sedation. Applicator insertion followed by place- ment of posterior vaginal wall retractor to displace the rectum. Finally, vaginal packing was done to stabilize the applicator and displace the bladder. Radiopaque rectal tube and dye was used to identify rectum and bladder. Then orthogonal X-rays antero-posterior and lateral X-rays taken with the dummy source in the applicator. Dosimetric computations was done in the treatment planning system using the orthogonal films and dose was calculated to point A, Point B, ICRU rectal and bladder points. Ir-192 Microselectron HDR remote control brachytherapy machine (Figure 1 shows microselectron equipment) was used to deliver Intracavitary brachytherapy. All patients received HDR brachytherapy 2 fractions of 9.0 Gy each (one week apart), dose specified to Bladder and Rectum were defined according to ICRU 38 (International Commission on Radiation Units and Measurements).
Figures 1(a)-(d): Brief description of brachytherapy steps: (Department of radiation oncology, jipmer, pudu- cherry, India). a) Ring and tandem applicator; b) orthogonal X-ray with dwell positions; c) isodose curves showing pear shaped dose distribution; and d) micro selectron brachytherapy equipment.


Figure 1. (a)-(d) steps of brachytherapy: (a) Ring and Tandem applicator provided rectal retractor; (b) orthogonal lateral X-ray; (c) isodose curves showing pear shaped dose; (d) micro selectron brachytherapy equipment.
2.3. Study Design
Ca cervix IIA-IIIB
(N = 102)
Whole Pelvis External Beam Radiotherapy (EBRT)
46 Gy/23# @ 200 cGy/#, 5days/week
+
Concurrent weekly chemotherapy with I/V Cisplatin 40 mg/m2
Followed by
Parametrial EBRT boost 4 Gy/2# @ 200 cGy/# with central shielding
7 days gap
Intracavitary High Dose Rate Brachytherapy using Ir-192 source
(9 Gy/# ×2 sessions, at weekly interval)
Group A: 50 patients were recruited in whom source had activity of 10-6Ci (Air Kerma Strength −2.857 cGy∙m2∙h−1 to 4.082 cGy∙m2∙h−1).
Group B: 52 patients were recruited in whom source had activity of 5 to 2Ci (Air Kerma Strength −0.8164 cGy∙m2∙h−1 - 2.041 cGy∙m2∙h−1).
Study design:
· Inclusion Criteria:
· Histological proven squamous cell carcinoma cervix patients, FIGO stage IIB to IIIB with less than upper 1/3rd of vagina involvement, who are suitable for radical radiotherapy by EBRT to pelvis followed by HDR Intracavitary brachytherapy.
· Age < 55 years.
· ECOG (0 - 2).
· Normal Haemogram, kidney function and liver function.
· No evidence of distant metastasis.
· No prior treatment for carcinoma cervix in form of radiation, surgery or chemotherapy.
· Clinical and dosimetric Parameters Studied.
· Local control of the disease.
· Distant metastasis.
· Bladder and rectal complications.
· Mean BED Bladder dose/maximum bladder dose.
· Mean BED Rectal dose/maximum rectal dose.
· Average dose at Point A.
· Average dose at Point B.
Strength calculated by using the formula: 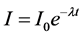
where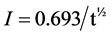 ;
;
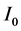 = Initial activity;
= Initial activity;
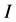 = Remaining activity at time
= Remaining activity at time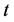 ;
;
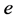 = Number denoting the base of natural logarithm;
= Number denoting the base of natural logarithm;
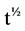 = Half-life of radioisotope;
= Half-life of radioisotope;
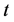 = time period.
= time period.
BED
Biological effective dose 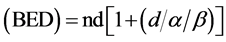
n—Number of fractions;
d—Dose per fraction;
 —10 for Tumor and 3 for Rectum and Bladder.
—10 for Tumor and 3 for Rectum and Bladder.
3. Statistical Analysis
Variables were expressed as mean and standard deviation. Chi square test, Man Whitney test was used for analysis of parameters P value of <0.05 was considered significant. SPSS software was utilized to complete the statistical analysis.
4. Results
Total of 102 patients enrolled in this study. In group A, 3 patients had residual disease and in group B, 4 patients had residual disease at 6 months of follow up. We analyzed the incidence distant metastasis between both groups; remarkably we observed significant incidence of distant metastasis after 6 months of follow up. Table 1 shows incidence of local, distant metastasis at 6 months. There was no apparent dose rate effect on local control and distant metastasis when source activity was stratified as high and low source activity.
When ICRU rectal point BED was analysed in 50 patients in group A, BED ranged from 85 Gy - 154 Gy3 and majority of patients BED was between 100 - 130 Gy3.. In group B, ICRU rectal point BED ranged from 83 Gy - 164 Gy3 and majority of patients BED is between 110 - 130 Gy3. When ICRU bladder point BED was analysed in group A, BED ranged from 85 Gy3 - 175 Gy3 and majority of patients BED was between 100 - 140 Gy3. One patient had received Dose > 170 Gy3. In group B, Doses were ranged from 86 Gy3 - 169 Gy3 and majority of Patients BED between 90 - 150 Gy3. Three patients had received Dose >160 Gy3. We found there was no significant difference between BED between two groups.
The Mean BED of rectum in group A and B were 115 Gy3 and 121 Gy3 (P < 0.05) respectively with EBRT plus brachytherapy. It was observed that rectal BED was received by patients in group B which was statistically significant (P < 0.05) (Table 2).
Table 1. Incidence of local, distant metastasis.
Table 2. Comparing the incidence of complications with ICRU rectum point mean dose in both groups.
On further sub group analysis in (rectal BED i.e. ≤100 Gy3 and ≥100 Gy3) 32 patient had received ≤100 Gy3 and 70 patients had received dose ≥ 100 Gy3. It was also observed that stage IIIB (63) patients had received high
rectal BED ≥ 100 Gy3 dose in comparison of other stage of presentation. This implies that there was increase in probability of late rectal complications as the disease advances (Table 3).
5. Strength
The incidence of rectal complications and occurrence of different grades of toxicity with respect to the BED Twenty nine patients (28.4%) had no complications. No grade IV complications were observed in both groups. Twenty seven cases (26.4%), 35 cases (34.3%), and 11 cases (10.7%) had Grade I, II and III late rectal complications respectively (Table 4).
6. Discussion
Manning et al. postulated a model showing that cell killing was dependent on source activity, especially in cells with a short repair time. There are several factors that affect local control or complications in HDR-ICBT for cervical cancer such as stage, fractionation scheme, biological dose, and optimization strategy and insertion technique, are extremely complex. The dose-rate effect of an HDR 192Ir source is a strange factor which is currently being investigated [4] . Very few studies have assessed the effect of source activity on local control rate and late normal tissue morbidity. Different applicators can be used to deliver HDR Brachytherapy like Fletcher suit and Ring and Tandem. The advantage of Tandem and Ring applicator over Tandem and Ovoid applicator is it provides a rectal retractor which displaces the ant rectal wall sufficient enough that vaginal packing can be avoided. It also has been reported to have advantages of better spatial reproducibility and fixed applicator geometry [5] .
Shang-Wen Chen et al., reported 5-year overall survival was 75% for all patients. The pelvic relapse-free survival was 88% for all patients, 90% for stage IIB, and 79% for stage III. They stated that there was no apparent dose-rate effect on pelvic control for stage IIB and stage III tumors when source activity was stratified with activity of 2.4 cGy∙m2∙h−1 [6] . In this study group A, 3 patients (6%) had residual disease and in group B, 4 patients (8%) had residual disease. Though the results are comparable with Shang et al. study, longer follow up is required to assess local control rate, and survival rate.
Das D. et al. from India reported the incidence of distant metastasis in cancer cervix. In their study 6 patients developed distant metastasis after 2 years follow up. Nelson et al. reported on 104 patients with stage II and III cancer cervix, who underwent exploratory laparotomy and Para-aortic lymph node biopsies. They observed
Table 3. Sub group analysis of rectal BED with source activity and stage of presentation.
Table 4. Frequency and grade of rectal bleeding in each group stratified by bed and source strength.
12.5% of patients with stage IIA disease, 14.9% with stage IIB, and 38.4% with stage III disease had Para-aortic lymph node metastases. [7] Grigsby et al. study in 43 patients with cervical cancer and biopsy-proven positive
para-aortic lymph nodes treated with external irradiation to the pelvis and para-aortic regions (45 to 50 Gy) combined with brachytherapy. They found tumor recurrence occurred in 20 patients (3 pelvis, 9 pelvis and distant metastasis, and 8 distant metastasis only) [8] . Current study the results were comparable with the Grigsby et al.
Suzuki and Isohashi et al. calculated rectal dose based on ICRU recommendations and GECESTRO, DVH parameters. They observed that rectal BED range was 37.5 Gy3 - 195.5 Gy3 and majority was within the range 85 - 125 Gy3 in majority of cases [9] [10] . Shang Wen Chen et al. the median total rectal BED was 104.5 Gy3 (range, 81.7 to 174.8), and the median total bladder BED 109.3 Gy3 (range, 82.5 to 170.6) [6] . With the present study, the results were comparable with Shang study. Mean dose and maximum dose of rectum and bladder BED results were reproducible with Suzuki et al. study. In contrast to Suzuki study, the minimum BED dose observed in this study was 74 Gy3. The reason may be attributed to institutional variations in following different fractionation schemes and ICBT insertion techniques. In Suzuki et al. most patients received less than 40 Gy of EBRT without central shielding with a larger prescribed dose of 6.8 to 7.2 Gy to point A with fletcher suit applicator. In contrast, all patients in the present study had received 50 Gy of EBRT with two sessions of ICBT of 9 Gy to point A with Ring and Tandem applicator.
Suzuki et al., analyzed rectal complications based on ICRU recommendations in 132 patients, 39 patients (30%) developed rectal complications, including 25 patients (19%) with Grade 1 toxicity, 9 (7%) with Grade 2, 3 (2%) with Grade 3, and 2 (2%) with Grade 4. They concluded that there was definitive correlation between the source strength and rectal complications. Shang-Wen Chen et al. reported rectal complications in 42 patients developed grade 1 to 4 late rectal complications (13 grade 1, 23 grade 2, 4 grade 3, 2 grade 4). The cumulative rate of rectal complications was 19.8% for grade 1% - 4%, 13.7% for grade 2% - 4% and 2.8% for grade 3% - 4%. The median time for the development of rectal complications was 12 months (range, 3 - 35 months) [6] .
Ogino, et al. found that the rectal BED was significantly correlated with the incidence of late rectal complications. They reported 50% of complications and the calculated incidence of grade 3 - 4 complications ranged from 5% to 10% at a BED of 119 to 146 Gy. There was no correlation of complications with source activity, and the calculated incidence of grade 3 - 4complications ranged from 5% to 10% at BED of 119 to 146 Gy [11] . Toita et al. reported that there was increase in probability of occurrence in the incidence complications as the BED increases. They suggested cumulative rectal BED should be kept below 100 to 120 Gy3 to prevent grade 1 - 4 rectal complications [12] . Ferrigno et al. treated 138 patients with EBRT of 45 Gy combined with 4 weekly fractions of 6 Gy to point A. They reported that a cumulative BED at the rectum greater than 110 Gy3 had higher actuarial rates of grade 1 to 4 rectal complications than those with lower values (18% vs. 12%, P = 0.49) [13] . In the present study the cumulative percentage of rectal complications were almost 55%. As mentioned above, this discrepancy might be attributed to several confounding factors, especially institutional variations in dose and fractionation schemes and insertion techniques.
Present study as well as several other studies described rectal bleeding rate was greater in cases where rectal BED exceeds >100 Gy3. The BED were compared with late rectal and bladder complications in both group A and group B. it was observed that with the BED increase, the incidence of late rectal complications increased [14] . Very few studies reported bladder complications using HDR brachytherapy. Das D. et al. from India reported 6 cases had bladder complication after 6 months follow up [7] . Nakoni et al. [15] reported 0.9% bladder complication rate in carcinoma cervix after radiotherapy in 1968 to 1986. Montana et al. [16] analyzed bladder complications in 517 patients who received EBRT alone and documented 10% bladder complications. Shang Wen Chen et al. [6] reported Twenty-seven patients had grade 2 and higher late bladder complications (14 grade 2, 12 grade 3, 1 grade 4). The mean time to bladder complications was 27 months (range, 3 - 49 months). The cumulative rate of bladder complications was 12.7% for grade 2% - 4% and 6.1% for grade 3% - 4%. Present study it was observed in group A, 3 patients (grade 1), 3 patients (grade 2) and in group B, 3 patients (grade 1), 2 patients (grade 2) delayed late bladder complications which had no statistical significance with ICRU bladder point doses.
7. Conclusion
This study demonstrated no obvious dose-rate effect of the 192Ir source in HDR ICBT for cervical cancer in terms of pelvic control or radiation morbidity. However, longer study group with longer follow up is required to substantiate the results. Thus, there was no evidence that the practice of HDR should be modified when considering the dose rate effect. Careful monitoring of the biological doses i.e. BED for both the rectum and bladder is required, since it act as a good predictor for development of late sequelae. Further research and clinical trials should be focusing on the impact of source strength on the clinical outcome and a common consensus has to be developed based on evidence.
References
- ICMR Report on Incidence and Epidemiology of Cancer in India 2001-2004.
- Eifel, P.J. (2000) Chemoradiation for Carcinoma of the Cervix: Advances and Opportunities. Radiation Research, 154, 229-236. http://dx.doi.org/10.1667/0033-7587(2000)154[0229:CFCOTC]2.0.CO;2
- Haie-Meder, C., de Crevoisier, R., Bruna, A., Lhomme, C., Pautier, P., Morice, P., et al. (2005) Concomitant Chemoradiation in Patients with Cervix Cancer. Bulletin du Cancer, 92, 1032-854.
- Manning, M.A., Zwicker, R.D., Arthur, D.W. and Arnfield, M. (2005) Biologic Treatment Planning for High-Dose- Rate Brachytherapy. International Journal of Radiation Oncology*Biology*Physics, 49, 839-845. http://dx.doi.org/10.1016/S0360-3016(00)01453-X
- Brooks, S, Bowens, P, Lowe, G, Brayant, L and Hoskin, P.J. (2005) Cervical Brachytherapy Utilizing Ring Applicator: Comparison of Standard and Conformal Loading. International Journal of Radiation Oncology*Biology*Physics, 63, 934-939. http://dx.doi.org/10.1016/j.ijrobp.2005.07.963
- Chen, S.W, Wang, C.J., Leung, S.W., et al. (1998) The correlation of acute toxicity and late rectal injury in radiotherapy for cervical carcinoma: Evidence suggestive of consequential late effect (CQLE). International Journal of Radiation Oncology*Biology*Physics, 40, 758-64.
- Das, D., Chaudhuri, S., Deb, A.R., Gangopadhay, S. and Ray, A. (2011) Treatment of Cervical Carcinoma with High Dose Rate Intracavitary Brachytherapy: Two Years Follow Up Study. Asian Pacific Journal of Cancer Prevention, 12, 807-810.
- Grigsby, P.W. and Perez, C.A. (1991) Radiotherapy Alone for Medically Inoperable Carcinoma of the Cervix: Stage IA and Carcinoma in Situ. International Journal of Radiation Oncology*Biology*Physics, 21, 375-378. http://dx.doi.org/10.1016/0360-3016(91)90785-3
- Suzuki, O., Yoshioka, Y., Isohashi, F., et al. (2008) Effect of High Dose Rate Ir-192 Source Activity on Late Rectal Bleeding after Intracavitary Radiation Therapy for Uterine Cervix Cancer. International Journal of Radiation Oncology*Biology*Physics, 71, 1329-1334. http://dx.doi.org/10.1016/j.ijrobp.2007.11.074
- Ishohashi, F., Yoshioka, Y., Koizumi, M., et al. (2010) Rectal Dose Source Strength of the High Dose Rate Iridium-192 Both Affect Late Rectal Bleeding after intracavitary Radiation Therapy For Uterine Cervical Carcinoma. International Journal of Radiation Oncology*Biology*Physics, 77, 758-764. http://dx.doi.org/10.1016/j.ijrobp.2009.05.030
- Ogino, I., Kitamura, T., Okamoto, N., et al. (1995) Late Rectal Complication Following High Dose Rate Intracavitary Brachytherapy in Cancer of the Cervix. International Journal of Radiation Oncology*Biology*Physics, 31, 725-734. http://dx.doi.org/10.1016/0360-3016(94)00547-8
- Toita, T. (2009) Current Status and Perspectives of Brachytherapy for Cervical Cancer. International Journal of Clinical Oncology, 14, 25-30.
- Ferrigno, R., Dos, P.E., Pellizzon, A.C., et al. (2001) High-Dose-Rate Brachytherapy in the Treatment of Uterine Cervix Cancer. Analysis of Dose Effectiveness and Late Complications. International Journal of Radiation Oncology*Biology*Physics, 50, 1123-1135. http://dx.doi.org/10.1016/S0360-3016(01)01533-4
- Chen, W.S., et al. (2003) High Dose Rate Brachytherapy for Elderly Patients with Uterine Cervical Cancer. Japanese Journal of Clinical Oncology, 33, 221-228. http://dx.doi.org/10.1093/jjco/hyg041
- Nakono, T., Kato, S., Ohno, T., et al. (2005) Long Term Results of High-Dose Rate Intracavitary Brachytherapy for Squamous Cell Carcinoma of the Uterine Cervix. Cancer, 103, 92-102. http://dx.doi.org/10.1002/cncr.20734
- Montana, G.S., Fowler, W.C., Varia, M.A., Walton, L.A., Mack, Y. and Shemanski, L. (1986) Carcinoma of the Cervix, Stage III. Results of Radiation Therapy. Cancer, 57, 148-154. http://dx.doi.org/10.1002/1097-0142(19860101)57:1<148::AID-CNCR2820570130>3.0.CO;2-7
NOTES
*Corresponding author.





