Open Journal of Orthopedics
Vol.4 No.3(2014), Article ID:43680,7 pages DOI:10.4236/ojo.2014.43010
Lateral Intra-Articular Transposition of the Anterior Tibialis Tendon for the Treatment of Relapsed Clubfoot in Toddlers: A Previously Unreported Surgical Technique
Dayton Opel1, Samuel Abrams2, Matthew Halanski2, Kenneth Noonan2
1University of Wisconsin School of Medicine and Public Health, Madison, USA
2Department of Orthopedics and Rehabilitation, University of Wisconsin, Madison, USA
Email: noonan@ortho.wisc.edu
Copyright © 2014 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/


Received 24 January 2014; revised 28 February 2014; accepted 10 March 2014
ABSTRACT
Dynamic supination of the foot is a common residual deformity in children with clubfeet treated with the Ponseti method. Transfer of the anterior tibialis tendon (ATT) to the lateral cuneiform is an effective method for correcting this deformity when the cuneiform is ossified in children who are 3 to 5 years of age. We describe two cases of a previously unreported method of ATT transposition for correction of bilateral residual dynamic supination in a 26-month-old and a 19-monthold patient. Both patients presented shortly after birth with bilateral congenital idiopathic clubfoot and were initially treated with the Ponseti method. Both had residual deformity following initial treatment that included posterior contracture and metatarsus adductus with dynamic forefoot supination. This was surgically corrected with a posterior release and medial release of the 1st metatarsal/1st cuneiform joint. To correct dynamic supination, the ATT was transplanted laterally into the released midfoot joint. These two patients were followed post-operatively for 7.5 years and have correction of their residual deformity in both feet based on subjective functioning, appearance, range of motion, strength, and gait. Both have excellent lateral pull of their ATT, which functions as a strong foot dorsiflexor. No residual supination is present. This is the first report of lateral transposition of the ATT as an interposition graft at the released 1st metatarsal/1st cuneiform joint in patients with relapsed clubfoot. We suggest that this method should provide a high level of functioning in children with relapsed supination deformity and whose 3rd cuneiform has not yet ossified.
Keywords:Clubfoot; Clubfoot Relapse; Idiopathic Clubfoot; Anterior Tibialis Tendon Transfer; Ponseti; Residual Foot Deformity; Talipes Equinovarus

1. Introduction
The Ponseti technique of clubfoot correction is an internationally utilized method to correct congenital clubfoot. Depending on the institution and the published report, the ability to provide full and permanent correction varies. In some series, the rate of reoperation for recurrent or residual deformity may approach 35 percent of patients treated with the Ponseti method [1] -[5] . Relapse can occur due to scarring, muscle imbalance, loss of reduction, or inadequate correction of the original deformity [6] [7] . Typical residual deformity may include variable combinations of metatarsus adductus, posterior joint or Achilles contracture, as well as forefoot supination in the swing phase of gait.
It has been hypothesized by Ponseti that residual medial displacement of the navicular on the head of the talus will essentially translate the anterior tibialis tendon (ATT) insertion medially and thus transform the function of the ATT from foot dorsiflexor to foot supinator [3] . ATT transfer for the treatment of relapsed congenital clubfoot was first described by Garceau in 1940 and has since become a common and important form of surgical correction for relapsed clubfoot treated in the manner of Ponseti [1] [5] [6] [8] -[10] . This deformity is treated with transfer of the ATT into the third cuneiform and is indicated when the ossific nucleus has developed radiographically into a size sufficient for drilling, and through which the ATT can then be transferred. Unfortunately, this method precludes its use in children younger than 3 to 4 years of age, when the ossific nucleus has not yet developed.
Fortunately, most children with residual or recurrent deformity have forefoot supination and mild equinus contracture; in these children, it is acceptable to wait until sufficient ossification before tendoachilles lengthening and ATT transfer. Yet, occasionally a child who is less than 3 years may have a combination of deformity that is recalcitrant to repeat casting and becomes indicated for surgical “à la carte” approach of the residual deformity. In these operations on young patients with severe equinus, we have treated the functional medial displacement of the ATT with lateral translation of the ATT tendon into a midfoot capsulotomy, which also serves to correct metatarsus adductus. In this paper we describe the method and present midterm results of this method of lateralization in 4 feet of 2 children with residual clubfoot deformity.
1.1. Case #1
DW was a 6-day-old boy who presented for evaluation of bilaterally stiff idiopathic clubfoot. He underwent Ponseti casting, and was noted to have good correction with bilateral percutaneous tendoachilles lengthening at age of 5 weeks; 3 weeks later his casts were removed and he was fitted with a foot abduction orthosis. He was additionally prescribed physical therapy for heel cord and foot abduction stretching. At 8 months of age, the left foot demonstrated recurrence of the equinus deformity, some forefoot supination, metatarsus adductus, and the inability to dorsiflex past neutral. The right foot maintained better correction. Repeat casting of the left foot was performed for an additional month, followed with a brief and unsuccessful attempt at bracing with the abduction orthosis. At age 19 months, physical exam demonstrated left foot dorsiflexion to 5 degrees past neutral, very tight plantar fascia with a cavus deformity, and metatarsus adductus deformity.
Surgical correction for residual deformity was undertaken at 26 months of age (Figure 1). On the left foot, this consisted of a posterior release whereby the Achilles tendon and the flexor hallucis longus (FHL) tendons were Z-lengthened. The ankle joint was identified and incised to allow for further foot dorsiflexion. An incision was then made on the medial aspect of the distal calcaneus. The fascia of abductor hallucis was incised off of the calcaneus; the plantar fascia was transected and stripped distally. The foot was then maximally dorsiflexed and a 2 mm K-wire was used to pin the subtalar and tibiotalar joints in a position of dorsiflexion.
Through a medial incision, the ATT was identified, dissected free, and a Bunnell-type tendon suture was placed with #1 Vicryl suture. This suture would eventually be used for later transplantation and stabilization of the ATT into a midfoot capsulotomy. Release of the 1st cuneiform/navicular joint and 1st metatarsal/1st cuneiform joint was performed to correct the metatarsus adductus. While the forefoot was abducted and held in a corrected position, the joints were pinned with 0.046 and 0.062 K-wires. The ATT was then transplanted into the lateral aspect of the 1st metatarsal/1st cuneiform capsulotomy and the anchoring sutures were directed through the sole of the foot with Keith needles for later anchoring on the bottom of the cast. The suture ends in the ATT were left free during wound closures and would later pull the ATT into the capsulotomy and hold it there as the suture was finally tightened and tied on the bottom of the cast with a button (Figure 2).
On the right foot, Achilles Z-lengthening and posterior release was not performed because the foot was easily corrected. Through a medial incision, the ATT was identified and dissected free; similar capsulotomies were performed and the adductus was reduced and pinned as described above. The ATT was transplanted in a similar fashion into the 1st metatarsal/1st cuneiform capsulotomy, with later fixation to the bottom of the long-leg cast with a button. Both feet were immobilized in a non-weight bearing long-leg cast for 6 weeks at which time pins were pulled and the child was transitioned into a short leg weight bearing cast for a month; afterwards, bilateral ankle-foot orthoses (AFOs) were worn for 6 months.
At the latest visit, the patient was 9 years old (7.5 years after reconstruction), and was subjectively doing very well with no pain or problems. He can walk on his tiptoes and heels without difficulty and can dorsiflex his ankles to 10 degrees past neutral. During heel walking, his ATT is clearly palpable and functioning as an ankle dorsiflexor (Figure 3). There is no supination and his gait is considered normal. X-rays at 7.5 years post-op show normal alignment in the right foot and stable alignment without altered midfoot development (Figure 4).
1.2. Case #2
NL was a 10-day-old boy who was referred for moderately stiff bilateral idiopathic clubfeet. He was born at 37 weeks without complications. He underwent weekly Ponseti manipulation and long-leg casting, and percutaneous tendoachilles lengthening was performed at 6 weeks age; 3 weeks later the casts were removed and foot abduction orthoses were worn until 5 months of age. Similar to the previous patient, he was recasted for a month due to difficulties with bracing. He was transitioned back into bracing, but continued to have difficulties with
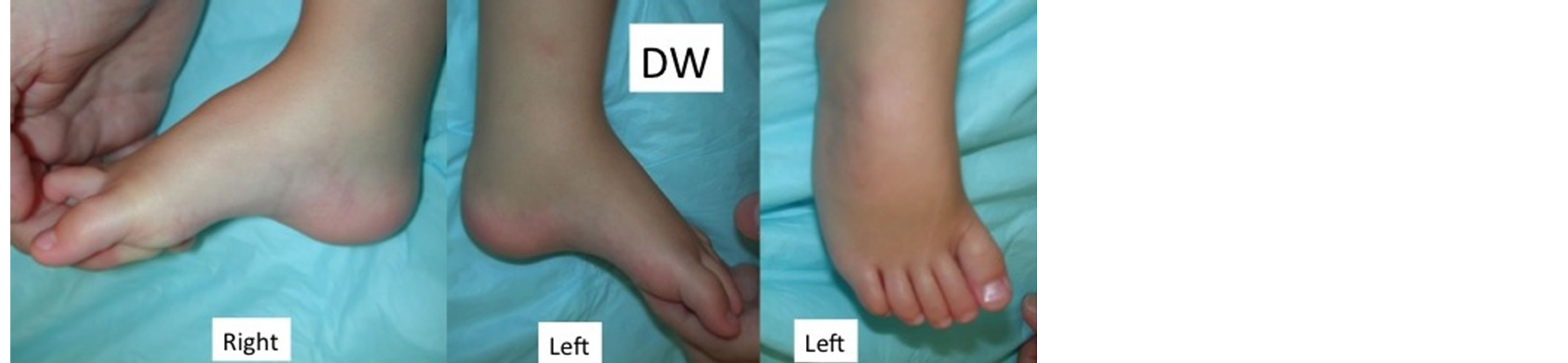
Figure 1. 26-month-old with recurrence of clubfoot deformity. The right foot demonstrates metatarsus adductus. The left foot demonstrates recurrence of the equinus deformity, forefoot supination, metatarsus adductus, very tight plantar fascia with a cavus deformity, and the inability to dorsiflex past neutral.
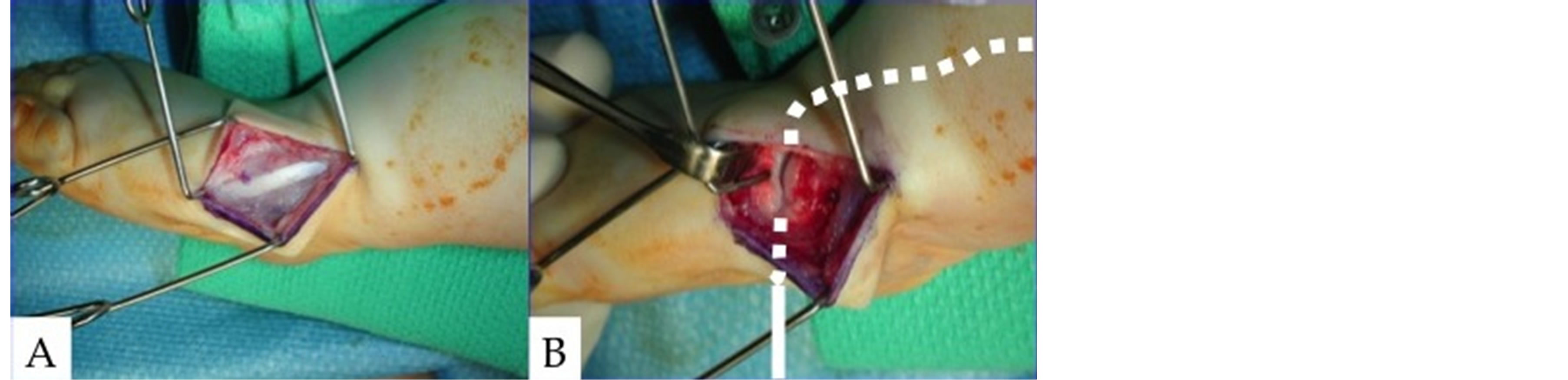
Figure 2. Intraoperative photographs taken during ATT transfer at 26 months of age. (A) ATT was identified and dissected free through a medial incision. (B) The ATT has been transplanted laterally into the lateral aspect of the 1st metatarsal/1st cuneiform capsulotomy. The white dotted line shows the path of the ATT from the leg through the capsulotomy and out the sole of the foot. The suture ends in the ATT were tied on the bottom of the cast with a pull-out button.


Figure 3. Photographs taken at 9 years old (7.5 years after reconstruction). (A) During heel-walking, ATT is clearly functioning as an ankle-dorsiflexor and easily palpated. (B) During toe-walking, there is no residual deformity of supination or adductus.
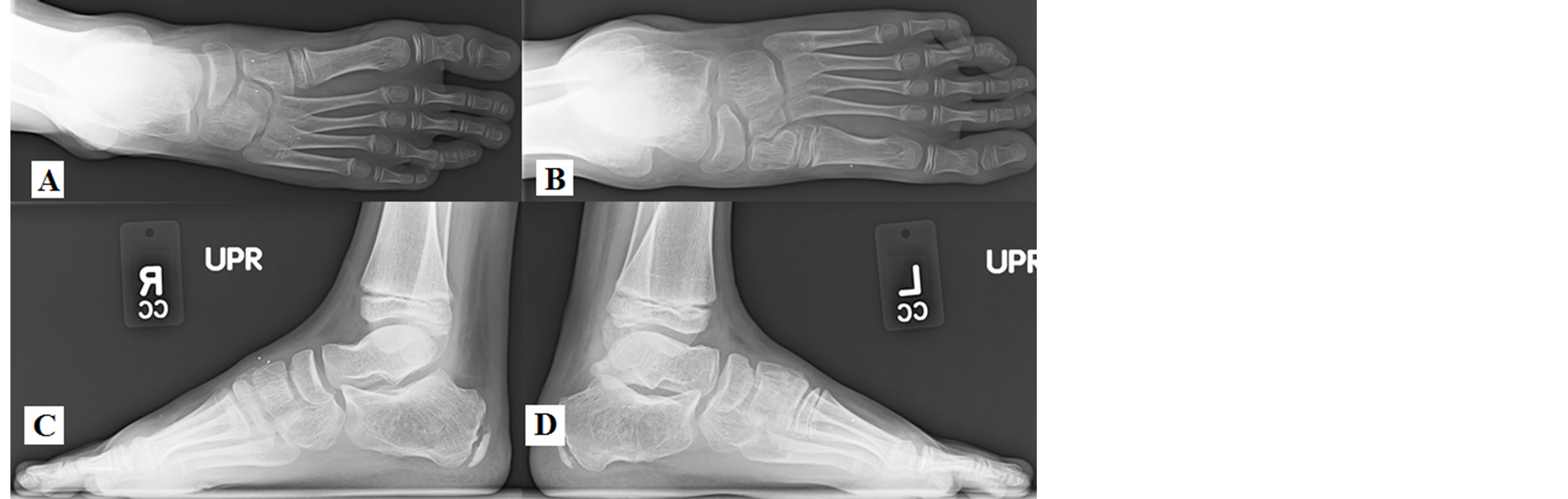
Figure 4. Radiographs taken of DW at 9 years old (7.5 years after reconstruction). AP (A) and lateral (C) views of the right foot show normal foot and ankle alignment. AP (B) and lateral (D) views of the left foot show stable alignment with minimal hind foot varus. Both feet demonstrate normal midfoot without evidence of growth arrest or dysplasia.
brace wear and developed recurrence of clubfoot deformity that included cavus, adductus, and equinus.
Surgical correction was undertaken at age 19 months for residual clubfeet deformities (Figure 5). The procedures on the left foot included posterior tibiotalar release with Z-lengthening of the tendoachilles, FHL, flexor digitorum longus (FDL), and posterior tibialis tendons, medial column release with 1st ray pinning, and ATT lateral transplantation into the capsulotomy (as described above). On the right foot, a tendoachilles lengthening was performed and a medial midfoot release and an ATT lateralization were performed. His post-operative course was similar to that above with the exception of night time AFO wear for 2 years.
At the most recent visit, he is 8 years old (7.5 years postoperatively) and has had good correction of his deformity. He is pain free and is able to walk and run without difficulty. He has 15 degrees of active and passive dorsiflexion bilaterally, and during ankle testing and gait evaluation his ATT dorsiflexes both feet without supination (Figure 6). X-rays at 7.5 years post-op show stable alignment of the hindfoot and midfoot with continued pes cavus of the left foot, and no sign of radiographic abnormality where the AT was transposed (Figure 7).
2. Discussion
Residual clubfoot deformity following the Ponseti method is a common occurrence. Many of these patients have incomplete correction and may have non-compliance with the foot abduction orthosis as a result of, or contributing cause of, the residual deformity. These children can be treated with variable combinations of different bracing strategies, use of physiotherapy, repeat casting, and surgical procedures. When non-operative methods to correct residual deformity fail, implementation of differing surgical procedures depends on degree and type of residual deformity and the age of the patient.
It has been recognized that the traditional extensive posterior and medial release for a partially treated club-
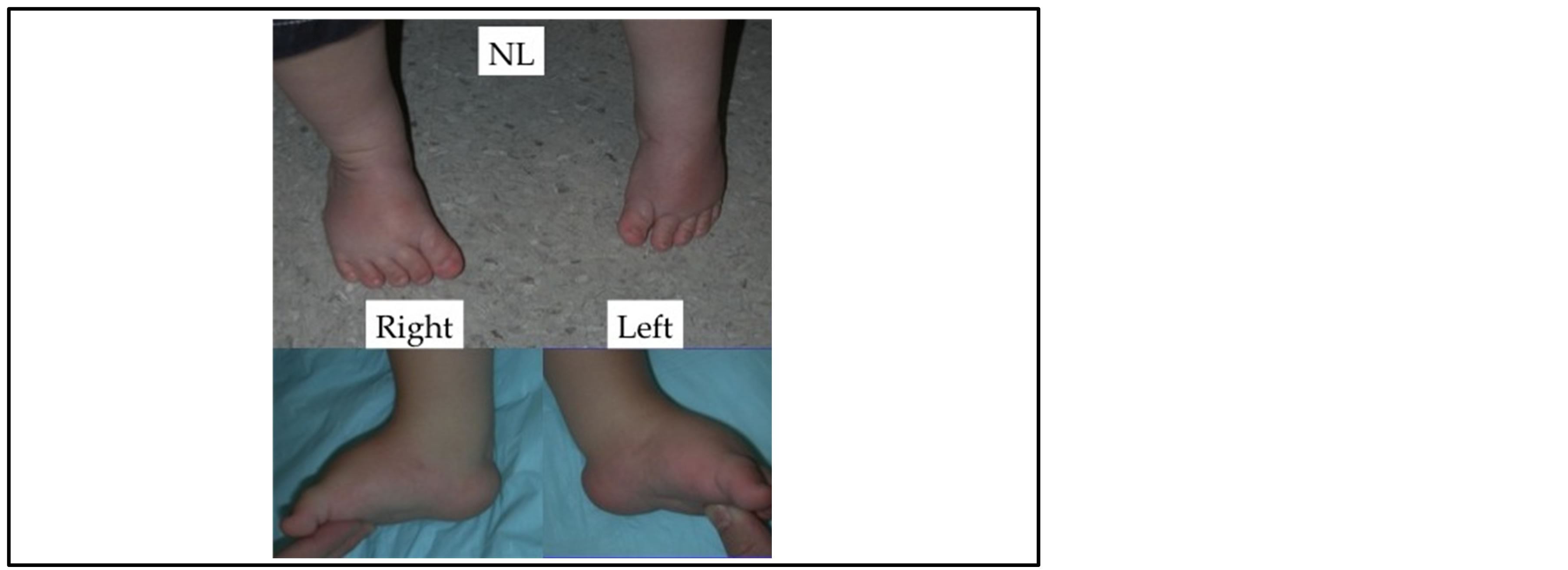
Figure 5. 19-month-old with recurrence of clubfoot deformity. Both feet demonstrate cavus, metatarsus adductus, and equinus.
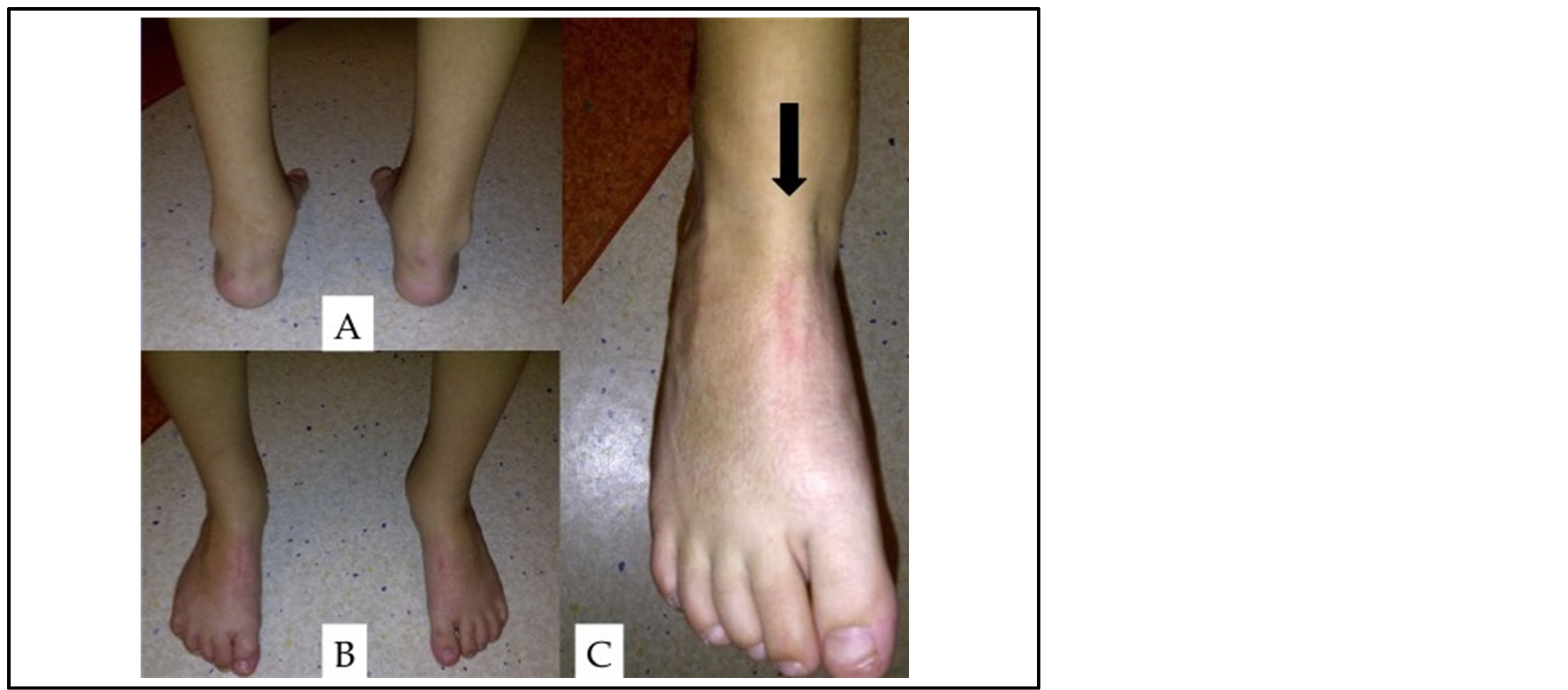
Figure 6. Photographs taken at age 8 years (7.5 years postoperatively). (A) Posterior view demonstrates no deformity. (B) Anterior view demonstrates continued resolution of the previous cavus, metatarsus adductus, and equinus deformities. (C) The ATT functions as a dorsiflexor to 15 degrees past neutral without supination.
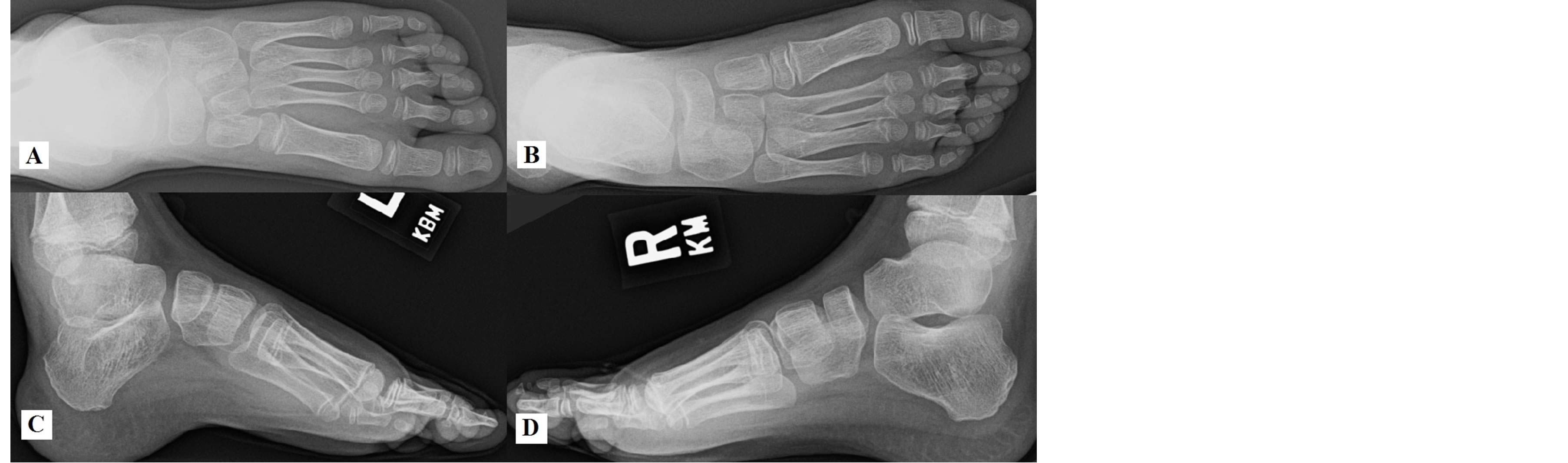
Figure 7. X-rays taken of NL at 9 years old (7.5 years after reconstruction). AP (A) and lateral (C) views of the left foot show stable alignment of the hindfoot and midfoot, with continued pes cavus and mild flattening of the talar dome. AP (B) and lateral (D) views of the right foot show stable hindfoot and midfoot relationships.
foot in an infant or young toddler may result in severe stiffness and overcorrection. As a result, it may be more prudent to employ an “à la carte” approach to residual deformity in the older infant or young toddler. For instance, equinus can be treated with repeat tenotomy, Achilles lengthening or posterior release. Cavus may be treated by plantar fascia release. Metatarsus adductus in the past has been treated by extensive mid foot release with variable results and high rates of stiffness. This deformity may be better treated with osteotomy of the midfoot when the child ages.
A very common residual deformity in ambulatory children is forefoot adduction and dynamic supination in the swing phase of gait. It is thought to be due to residual medial displacement of the navicular on the head of the talus with resultant medial displacement of the forefoot and the ATT insertion, which results in supination as opposed to straight dorsiflexion [1] [5] [7] [8] [10] -[12] . In order to correct this deformity the ATT is detached from its medial insertion and is usually transferred into the third or lateral cuneiform when it is sufficiently ossified on preoperative radiographs. In humans, the lateral cuneiform, which has been accepted as the best option for transfer of the ATT for surgical correction of residual clubfoot deformity [13] -[16] , does not begin to ossify until age 3.
When dynamic supination occurs as a component of recurrence between ages 3 - 5 years [3] -[6] , these patients can be treated with the ATT transfer as a portion of their surgical treatment. Yet, there is a small population of clubfoot patients who experience recurrence and persistence of significant equinus interfering with ambulation before 3 years of age. In order to address any dynamic supination and metatarsus adductus at this time, we have used lateral transplantation of the ATT. To the best of our knowledge there are no scientific reports of this surgical technique in the English literature; these case reports are the first to describe lateral transfer of the ATT as an interposition graft at the released 1st metatarsal/1st cuneiform joint in patients with relapsed clubfoot whose 3rd cuneiform has not yet ossified.
Our two patients had significant equinus as a component of their residual deformity in at least one of their feet that merited surgical intervention at 26 and 19 months. All four of the feet had residual metatarsus adductus and supination during the swing phase of gait that we chose to treat with limited capsule release and ATT transposition. It is possible that the capsular release could lead to midfoot stiffness as a complication of this procedure; however, this was not appreciated at follow-up and may be less likely than the stiffness seen in the historical release of the entire midfoot. In addition, it is possible that correction of the equinus and cavus deformities would have been sufficient in these patients to mitigate the supination or delay its treatment until the lateral cuneiform was ossified. Yet we chose to correct all of the deformity at one surgical setting by lateral transposition of the ATT. At 6 years follow-up this tendon acts as a pure dorsiflexor without apparent weakness, overt stiffness, or painful decrease in function. As a result of our experience in these 4 feet, we now consider this a viable option for the child with residual supination deformity that, in the opinion of the treating surgeon, requires surgical treatment for the relapsed clubfoot in a child less than 3 years of age.
3. Conclusion
Later displacement of the anterior tibialis tendon can be accomplished in immature feet with residual clubfoot deformity. In these children, displacement of the tendon into the metatarsal-cuneiform joint will correct dynamic supination deformity
References
- Abdelgawad, A.A., Lehman, W.B., van Bosse, H.J., Scher, D.M. and Sala, D.A. (2007) Treatment of Idiopathic Club Foot Using the Ponseti Method: Minimum 2-Year Follow-Up. Journal of Pediatric Orthopedics. Part B, 16, 98-105.
- Laaveg, S.J. and Ponseti, I.V. (1980) Long-Term Results of Treatment of Congenital Club Foot. The Journal of Bone and Joint Surgery. American Volume, 62, 23-31.
- Ponseti, I.V. and Smoley, E.N. (2009) The Classic: Congenital Club Foot: The Results of Treatment. 1963. Clinical Orthopaedics and Related Research, 467, 1133-1145. http://dx.doi.org/10.1007/s11999-009-0720-2
- Singer, M. and Fripp, A.T. (1958) Tibialis Anterior Transfer in Congenital Club Foot. The Journal of Bone and Joint Surgery. British Volume, 40, 252-255.
- Thompson, G.H., Hoyen, H.A. and Barthel, T. (2009) Tibialis Anterior Tendon Transfer after Clubfoot Surgery. Clinical Orthopaedics and Related Research, 467, 1306-1313. http://dx.doi.org/10.1007/s11999-009-0757-2
- Farsetti, P., Caterini, R., Mancini, F., Potenza, V. and Ippolito, E. (2006) Anterior Tibial Tendon Transfer in Relapsing Congenital Clubfoot: Long-Term Follow-Up Study of Two Series Treated with a Different Protocol. Journal of Pediatric Orthopedics, 26, 83-90. http://dx.doi.org/10.1097/01.bpo.0000188999.21427.fb
- Tarraf, Y.N. and Carroll, N.C. (1992) Analysis of the Components of Residual Deformity in Clubfeet Presenting for Reoperation. Journal of Pediatric Orthopedics, 12, 207-216. http://dx.doi.org/10.1097/01241398-199203000-00011
- Critchley, J.E. and Taylor, R.G. (1952) Transfer of the Tibialis Anterior Tendon for Relapsed Club-Foot. The Journal of Bone and Joint Surgery. British Volume, 34, 49-52.
- Garceau, G.J. (1940) Anterior Tibial Tendon Transposition in Recurrent Congenital Club-Foot. The Journal of Bone & Joint Surgery, 22, 932-936.
- Kuo, K.N., Hennigan, S.P. and Hastings, M.E. (2001) Anterior Tibial Tendon Transfer in Residual Dynamic Clubfoot Deformity. Journal of Pediatric Orthopedics, 21, 35-41. http://dx.doi.org/10.1097/01241398-200101000-00009
- Garceau, G.J. and Palmer, R.M. (1967) Transfer of the Anterior Tibial Tendon for Recurrent Club Foot. A Long-Term Follow-Up. The Journal of Bone and Joint Surgery. American Volume, 49, 207-231.
- Masrouha, K.Z. and Morcuende, J.A. (2012) Relapse after Tibialis Anterior Tendon Transfer in Idiopathic Clubfoot Treated by the Ponseti Method. Journal of Pediatric Orthopedics, 32, 81-84. http://dx.doi.org/10.1097/BPO.0b013e31823db19d
- Garceau, G.J. (1972) Anterior Tibial Tendon Transfer for Recurrent Clubfoot. Clinical Orthopaedics and Related Research, 84, 61-65. http://dx.doi.org/10.1097/00003086-197205000-00012
- Huang, Y.T., Lei, W., Zhao, L. and Wang, J. (1999) The Treatment of Congenital Club Foot by Operation to Correct Deformity and Achieve Dynamic Muscle Balance. The Journal of Bone and Joint Surgery. British Volume, 81, 858- 862. http://dx.doi.org/10.1302/0301-620X.81B5.9354
- Hui, J.H., Goh, J.C. and Lee, E.H. (1998) Biomechanical Study of Tibialis Anterior Tendon Transfer. Clinical Orthopaedics and Related Research, 349, 249-255. http://dx.doi.org/10.1097/00003086-199804000-00031
- Lampasi, M., Bettuzzi, C., Palmonari, M. and Donzelli, O. (2010) Transfer of the Tendon of Tibialis Anterior in Relapsed Congenital Clubfoot: Long-Term Results in 38 Feet. The Journal of Bone and Joint Surgery. British Volume, 92, 277-283. http://dx.doi.org/10.1302/0301-620X.92B2.22504

