Journal of Tuberculosis Research
Vol.1 No.2(2013), Article ID:36720,3 pages DOI:10.4236/jtr.2013.12004
Evaluation of the ParaLens™ LED microscope attachment versus standard fluorescence microscopy for detection of Mycobacteria
![]()
1The Johns Hopkins Medical Institutions, Baltimore, Maryland; *Corresponding Author: nparrish@jhmi.edu
2Regional Hospital, Bamenda, Cameroon
3The University of Missouri-Kansas City, Kansas City, Missouri
4Mezam Polyclinic HIV/AIDS Treatment Center, Bamenda, Cameroon
Copyright © 2013 Clara Lema et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 30 May 2013; revised 2 July 2013; accepted 11 July 2013
Keywords: Paralens™; Tuberculosis; Microscopy; Diagnostics
ABSTRACT
The Paralens™ (PL) microscope attachment converts a light microscope into an epi-fluorescence microscope. We compared the PL to standard fluorescence microscopy for detection of Mycobacteria in clinical and spiked samples. Overall agreement between the two systems was 100%. Quantitative and qualitative performance was comparable. The PL is an acceptable alternative to standard fluorescence microscopy for detection of Mycobacteria.
1. INTRODUCTION
Mycobacterial infection continues to be a global scourge. Currently, sputum smear microscopy remains the most widely used method for detection of acid fast bacilli (AFB) in respiratory specimens. It has been demonstrated that the sensitivity of standard bright field microscopy can be increased by 10% through the use of fluorescence technology [1]. However, widespread implementation of fluorescence microscopy has been hindered often where it is needed most, due to the high costs associated with purchase and maintenance of fluorescence microscopes.
Recently, the World Health Organization (WHO) issued a policy statement recommending that “conventional fluorescent microscopy be replaced by LED microscopy, and that LED microscopy be phased in as an alternative for conventional Ziehl-Neelsen light microscopy” [2]. Current LED technology has resulted in development of LED microscopes or LED attachments used in conjunction with standard light microscopes. The ParaLens™ (PL) microscope attachment (QBC Diagnostics, Inc., Port Matilda, Pennsylvania) is a portable, LED-based technology which combines the light source and filters of an epi-fluorescent microscope in a compact, single objective, transforming any light microscope into an epifluorescent microscope. We compared the performance characteristics of the new and improved PL with a stateof-the-art fluorescence microscope for detection of Mycobacteria in clinical specimens.
2. METHODS
A total of 244 clinical specimens were used for this study. These included 115 prospective, clinical specimens from the Mycobacteriology Laboratory at the Johns Hopkins Hospital (JHH) encompassing a range of specimen types (sputum, bronchoalveolar lavage, tissue and sterile fluids), 48 sputum samples from suspected patients with tuberculosis from the Regional Hospital and Mezam Polyclinic HIV/AIDS Center, Bamenda, Cameroon, and 81 spiked sputum samples. All sputum specimens were digested and decontaminated using standard mycobacteriology procedures [3]. All smears were prepared using a rapid, 2 minute, fluorescent stain (Scientific Device Laboratories, Des Plaines, Illinois) as previously described [4]. A different medical technologist from the one performing the microscopy processed the samples, prepared the slides and blinded them prior to reading. All slides were scanned with an Olympus model BX41 fluorescent microscope (OM, Olympus America Inc., Center Valley, Pennsylvania) and the PL at 20x and 40x magnification according to manufacturer instructions and the results were compared [5]. A total of 15 fields were observed before a slide was resulted as negative. Results included quantitation of acid-fast bacilli (AFB) using the current WHO-International Union against Tuberculosis and Lung Disease guidelines (rare, 1 to 9 AFB per 100 fields), 1+, 10 to 99 AFB per 100 fields, 2+, 1 to 10 AFB per individual field, 3+, 10 to 100 AFB per individual field, and 4+, more than 100 AFB per individual field) [6]. The brightness of both AFB and background debris were also determined using a similar scale as previously described [4]. Brightness was graded ranging from dull (1+), to bright (2+), very bright (3+), or brilliant (4+). Results were stratified by either 20x or 40x such that a direct comparison could be made between equivalent magnifications on both the OM and the PL. Spiking studies were performed to determine the lower limit of detection for both the OM and the PL and to account for variation in performance relative to morphological differences between mycobacterial species. All spiking studies were conducted using pooled, processed, smear negative sputum which was divided into aliquots and inoculated with a dilution series (ranging from 107 to 102 CFU/ml) of the following mycobacterial species: Mycobacterium tuberculosis, M. avium, M. gordonae, M. kansasii, M abscessus, M. chelonae, M. fortuitum, M. mucogenicum, M. lentiflavum, M. scrofulaceum, and M. szulgai. Viable cell counts were used to confirm the actual number of bacilli per ml for each spiked sample tested.
3. RESULTS and DISCUSSION
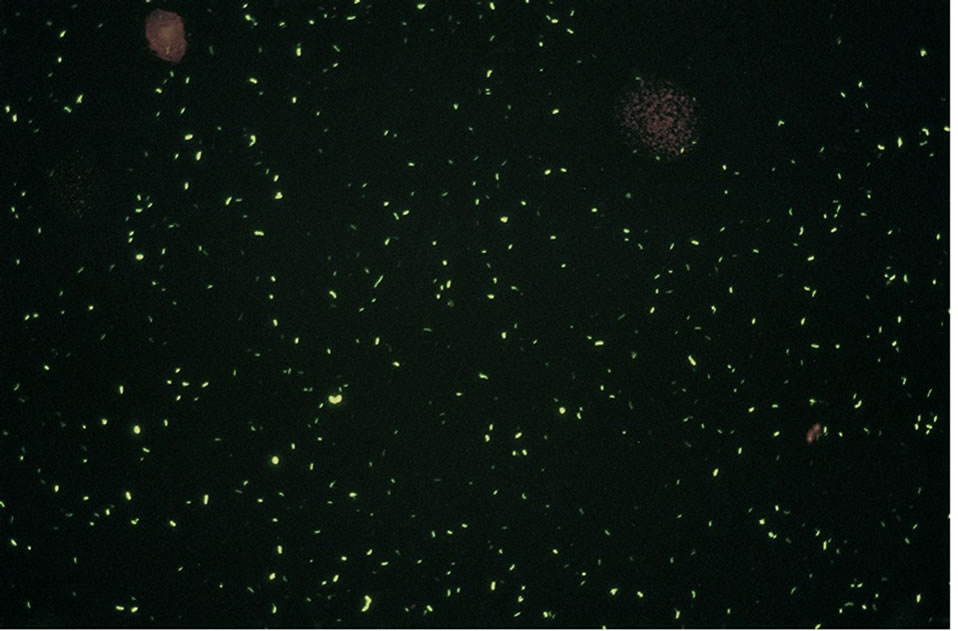
Overall agreement between the PL versus the OM was 100% for detection of smear positive (n = 94) versus smear negative (n = 150) specimens. AFB quantitation did not differ between the PL and the OM at either 20x or 40x (Table 1). Background and debris appearance and quantity did not differ between the PL and OM at either magnification (Table 1). AFB brightness was slightly less with the PL than the OM, however, this difference did not impact correct interpretation of the smear (Figures 1(a) and (b)). In spiking studies, agreement between the PL and OM was 100% for detection of smear positive versus smear negative sputum. AFB morphology was not affected using the PL versus the OM and detection limits were comparable (~104 CFU/ml). Agreement between the PL and OM for AFB detection in real-time samples was 100%.
The current version of the PL is significantly improved over earlier versions (non-QBC) which encouraged us to evaluate performance characteristics versus a state-ofthe-art fluorescence microscope [7]. Improvements include addition of two scanning objectives (20x and 40x) and a second oil immersion objective (100x), the ability
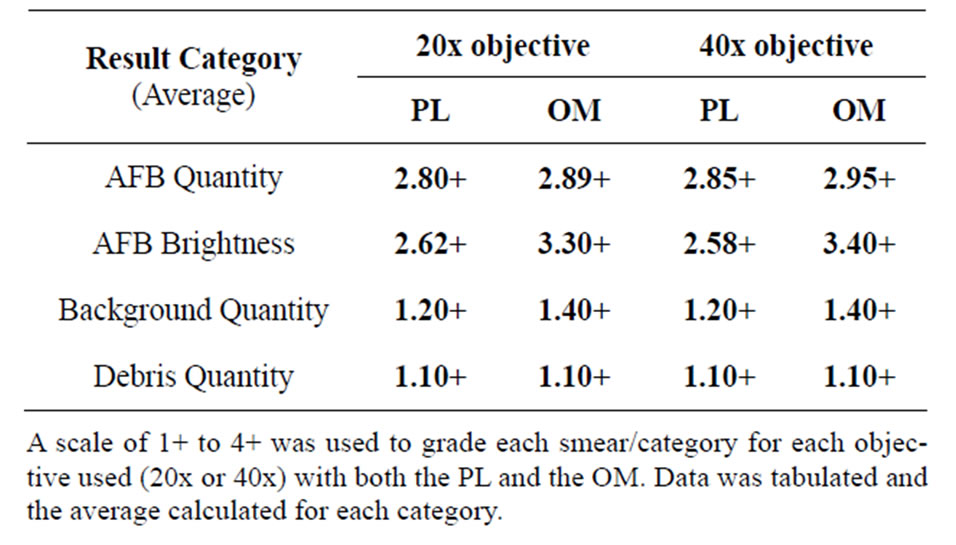
Table 1. Overall quantitative and qualitative comparison of the PL versus the OM.
 (a)
(a)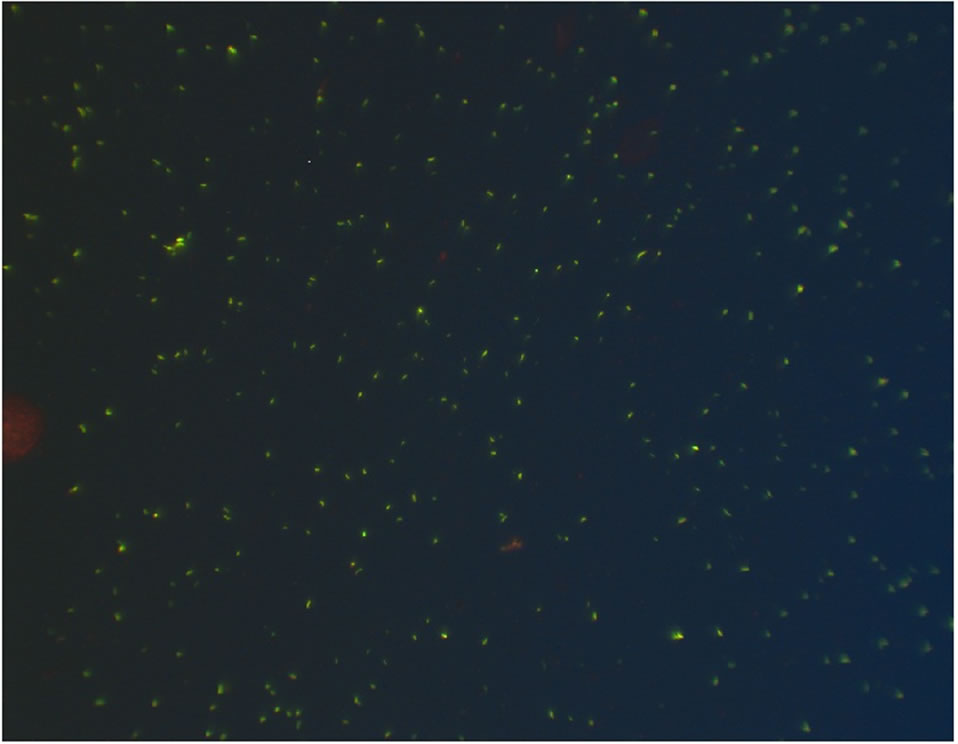 (b)
(b)
Figure 1. (a) Representative 4+ Auramine-O stained smear as seen through the 20x objective of the OM. (b) Representative 4+ Auramine-O stained smear as seen through the 20x objective of the PL.
to utilize a variety of power sources (110 v/240 v, low voltage battery pack, solar power adapter or cigarette lighter), and a light source lamp of ~20,000 hours. In addition, the PL requires minimal space, is easily transported between locations, is easily stored, and can be used with standard microscope slides. In a recent study by Kuhn, et al., [8] the authors compared 20 positive smears and 5 negative control slides to assess performance of the PL using the original oil immersion objective of 60x. This study demonstrated 100% agreement between the PL versus a Nikon fluorescence microscope using the 60x oil immersion objective. In our study, the scanning objectives of 20x and 40x were selected since most Mycobacteriology laboratories typically scan Auramine-O stained slides at a lower power which permits visualization of more fields resulting in decreased overall turnaround-time for smear reporting. The current study demonstrates that the PL is a viable alternative to standard fluorescence microscopy for rapid detection of AFB in clinical specimens and can be used with either the 20x or 40x scanning objectives with no impact on smear interpretation and a more rapid turn-around-time. Not assessed in this study, was the use of the solar battery option for powering the PL, which may be of significant benefit in resource limited settings in which TB is endemic. Additional field studies are needed to determine the performance characteristics of the PL when operated solely by solar power.
4. ACKNOWLEDGEMENTS
Many thanks to the JHH Microbiology and staff for their support which made this study possible. Thanks also to Isaac Afwamba from KCMC Hospital in Tanzania for his assistance.
REFERENCES
- Steingart, K.R., Henry, M., Ng, V., et al. (2006) Fluorescence versus conventional sputum smear microscopy for tuberculosis: A systematic review. The Lancet Infectious Diseases, 6, 570-581. doi:10.1016/S1473-3099(06)70578-3
- World Health Organization (2010) Fluorescent light emitting diode (LED) microscopy for diagnosis of tuberculosis. WHO, Geneva.
- Pfyffer, G.E. (2007) Mycobacterium: General characteristics, laboratory detection, and staining procedures. In: Murray, P.R., Baron, E.J., Landry, M.L., Jorgensen, J.H. and Pfaller, M.A., Eds., Manual of Clinical Microbiology, 9th Edition, American Society for Microbiology Press, Washington DC, 543-572.
- Hendry, C., Dionne, K., Hedgepeth, A., et al. (2009) Evaluation of a rapid fluorescent staining method for detection of Mycobacteria in clinical specimens. Journal of Clinical Microbiology, 47, 1206-1208. doi:10.1128/JCM.02097-08
- (2010) Paralens microscope attachment operators manual. QBC Diagnostics, Port Matilda.
- World Health Organization (2006) Global tuberculosis control: Surveillance, planning, financing. WHO, Geneva.
- Patterson, K., Mcdonald, C., Miller, B., et al. (1995) Use of the ParaLens adapter for detection of acid-fast organisms. Journal of Clinical Microbiology, 33, 239-241.
- Kuhn, W., Armstrong, D., Atteberry, S., et al. (2010) Usefulness of the Paralens™ fluorescent adapter for the identification of Mycobacteria in both field and laboratory settings. The Open Microbiology Journal, 4, 30-33. doi:10.2174/1874285801004010030

