 Advances in Bioscience and Biotechnology, 2013, 4, 304-315 ABB http://dx.doi.org/10.4236/abb.2013.42A041 Published Online February 2013 (http://www.scirp.org/journal/abb/) Seco-limonoid 11α,19β-dihydroxy-7-acetoxy-7- deoxoichangin promotes the resolution of Leishmania panamensis infection Diana Granados-Falla1,2, Carlos Coy-Barrera3, Luis Cuca3, Gabriela Delgado1* 1Immunotoxicology Research Group, Department of Pharmacy, Sciences Faculty, Universidad Nacional de Colombia Bogotá, Bo- gotá, Colombia 2Biotechnology Doctorate Program, School of Sciences, Universidad Nacional de Colombia, Medellin, Colombia 3Natural Products Group, School of Sciences, Universidad Nacional de Colombia, Bogotá, Colombia Email: *lgdelgadom@unal.edu.co Received 3 January 2013; revised 3 February 2013; accepted 10 February 2013 ABSTRACT The high morbidity generated by the infection caused by parasites of the genus Leishmania, make of this infection into one of the vector-borne infectious dis- eases most relevant worldwide, which added to the fact that the drugs used for its treatment are far from be optimal and considering that prophylactic appro- aches (such as the development of a vaccine) still seems far from being achieved, make of the search for new therapeutic alternatives for safe and effective treatment of this disease one of the most accurate ap- proaches to the control of this disease. In this study we evaluated the antileishmanial and immunomodu- latory activity of the compound 11α,19β-dihydroxy- 7-acetoxy-7-deoxoichangin (a seco-limonid molecule) through: 1) evaluation of its cytotoxicity over pro- mastigotes and axenic amastigo tes of L. (V) panamen- sis, 2) determination of its ability to induce the con- trol of in vitro infection, using infected murine cells (J774.2) and human dendritic cells (hDCs), 3) quan- tifying the levels of pro-inflammatory cytokines, (iv) evaluating the expression of cell markers associated with hDCs maturation, and (v) determinating the production of nitric oxide free radicals (NO). In this regard, this seco-limonoid exhibited an antileishma- nial activity represented in the reduction of in vitro infection in J774.2 cells and hDCs, with a EC50 of 7.9 µM (4.48 µg/mL) and 25.5 µM (14.39 µg/mL), respec- tively, and additionally, we observed an increase on the production of IL-12p70, TNF-α and NO, as also, in the number of hDCs HLA-DR-positive in treated infected hDCs. These findings suggest that anti-leish- manial activity of this compound could be associated with the potential “reactivation” of phagocytic cell that is “paralyzed” by the infection, generating an immune phenotype associated with protection. Keywords: Leishmaniasis; Treatment; Immunomodulation; Seco-Limonoid 1. INTRODUCTION Leishmaniasis is a parasitic disease of global public relevance, which is transmitted by the bite of sandfly species belonging to the genus Lutzomyia or Phleboto- mus, infected with promastigotes of the genus Leishma- nia. According to reports getting for the World Health Organization (WHO), the transmission of the pathogens responsible for this disease occurs endemically in at least 98 countries, primarily affecting developing countries located in tropical and subtropical regions around the world [1,2]. Annually, at least 1.5 million of new cases of the cutaneous form of the disease (CL) and approxima- tely 500,000 new cases of the visceral leishmaniasis (VL) are reported around the world, being the VL form the clinical presentation responsible for the deaths associated with the pathogen and the CL form the responsible of its high levels of morbidity [3]. Chemotherapy against leishmaniasis is based on the administration of pentavalent antimonial salts (as first- choice drugs) or the use of formulations of pentamidine®, pa ro momyc i n ®, miltefosine® or amphotericin B®, as second-choice drugs. However, the mechanism of action of these drugs has not been well clarified yet, and this added to the fact that none of them was originally de- signed for the treatment of this disease and limitations associated with their administration routes [4,5], high costs and duration of the treatment, the emergence of parasites resistant to these drugs [3,6] and the high toxic- ity of some formulations, make necessary and urgent the develop of safer and more effective therapeutic alterna- *Corresponding author. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 305 tive to the better control this disease [1,7]. Among the elucidated to date in relation to the mechanism of action postulated for the drugs mentioned above, it have been found that the formulations of pentavalent antimony salts act as pro-drugs, needing for that, their reduction to tri- valent form to perform their action, which is proposed to be directed against the trypanothione reductase and zinc- finger protein (proteins that are related with the protec- tion of the parasites from oxidative damage and toxic heavy metals, and with the process of replication and repair of DNA, respectively) [8,9]. On the other hand, the mechanism of action of pentamidine (second drug of choice for the treatment of this disease, used when pa- tients cannot tolerate the antimonial drugs, or in cases of resistance to these drugs) is associated with the accumu- lation and altering of the function of the kinetoplast, as well as the collapse of the membrane potential of the microorganism [10,11], while the mechanism of action of amphotericin B (a macrolide used for treatment of mu- cocutaneous and visceral leishmaniasis) is associated with its capability to bind to the ergosterol molecule (the major sterol of the Leishmania parasite membrane), lead- ing to the formation channels that would alter the per- meability of the cell membrane [12]. Recently, the study of compounds derived from plant species has become in a major tool for the developed of novel therapeutic agents against several infectious dis- eases, such as leishmaniasis [13-15], and in this regard, several research groups have screened a large number of natural compounds, with the aim of find potential che- mical entities (prototypes) that can be used for the de- velopment of more effective and safer alternative thera- pies against these pathogens [16-18]. In previous studies, our research group demonstrated that the compound 11α,19β-dihydroxy-7-acetoxy-7-de- oxoichangin (a seco-limonoid) exhibits an antileishma- nial specific activity against the intracellular form of the parasite (corresponding to the most relevant stage for studying and designing possible therapeutic targets against this pathogen) [19,20]. This compound was iso- lated from the vegetal species Raputia heptaphylla, a spe- cies belonging to the family Rutaceae, and whose geo- graphical distribution is concentrated in tropical areas of Central and South America (mainly reports its location in Costa Rica, Panama, Colombia, and forested areas of Brazil and Peru). Species belonging to the genus Rapu- tia have been characterized by the present of abundant secondary metabolites (primarily alkaloids and limonoid), being an example of this, the studies carried out in Rapu- tia prateermisa (other species of the genus Raputia), whose leaves have been used in decoction for treatment of cutaneous leishmaniasis and chagas disease in selvatic areas of Brazil, and whose phytochemical study showed that limonoids compounds are an important part of its composition to the secondary metabolites level [21], be- ing them possibly responsible for some of the biological activities attributed to these plants. In this study, we sought to confirm the antileishmanial activity of this seco-limonoid using for in vitro assays, murine macrophages and human dendritic cells (hDCs) infected with this protozoan, as also, we wanted to char- acterize its possible immunomodulatory effect on anti- gen-presenting cells (APCs), which are a critical popula- tion for the resolution of natural infections by parasites of the genus Leishmania, observing that the compound pre- sents an antileishmanial activity associated with an im- munomodulatory effect, that it is evident by the differen- tial induction on the increase in the production of soluble pro-inflammatory mediators, such as IL-12p70 and TNF- α, and a significant increase in the expression of MHC class II molecules as also in the levels of nitric oxide (NO) on infected cells exposed to the seco-limonoid compared with infected cells without treatment. 2. MATERIALS AND METHODS 2.1. Cells RPMI 1640 (Gibco BRL-Life Technologies Inc., Grand Island, NY, USA) medium was used for culturing the phagocytic cell line J774.2 (a murine macrophage cell line derived from the murine J774A.1 cells, which are monocyte/macrophage cells, obtained from reticulum cell sarcoma of ascites in BALC/c mouse, which are sus- ceptible to the infection with Leishmania parasites), hu- man dendritic cells (hDCs) derived from peripheral blood monocytes (obtained from healthy volunteers) and the promastigotes of Leishmania (Viannia) panamensis (L. (V) panamensis), which were either untransfected (MHOM/88CO/UA140) or transfected (MHOM/88/CO/ UA140irGFP) with a plasmid (ir) encoding green fluo- rescent protein (GFP) (kindly donated by Dr. Sara Robledo from the Program for the Study and Control of Tropical Diseases; PECET-Programa de Estudio y Con- trol de Enfermedades Tropicales, of the Universidad de Antioquia, Colombia [22]). The RPMI medium was sup- plemented with 2 mM L-glutamine (Gibco BRL-Life Technologies Inc.), 1% non-essential amino acids, 1000 U/ml penicillin, 0.1 mg/ml streptomycin, 0.25 ug/ml amphotericin B (Sigma Chemical Co., St. Louis, MO, USA), 24 mM sodium bicarbonate (Sigma Chemical Co.), and 25 mM HEPES (Gibco BRL-Life Technologies Inc.). The culture media were enriched with 10% fetal bovine serum (FBS) (Microgen, Bogotá, Colombia) for the J774.2 cells and parasites or with AB negative human plasma that was filtered and inactivated (Lonza Walkers- ville, MD, USA) for the culture of hDCs. The mammalian cells were incubated at 36˚C - 37˚C in Copyright © 2013 SciRes. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 306 an atmosphere of 5% CO2 and 90% humidity, whereas the promastigotes of L. (V) panamensis were grown at 25˚C - 26˚C. The axenic amastigotes were produced from the cul- ture of promastigotes of L. (V) panamensis in RPMI me- dium enriched with 20% FBS at pH 5.4, and differentia- tion was achieved by the gradual exposure of the cells to increases in temperature (29˚C, 32˚C, and 34˚C). It should be note that depending on the assay, the monocytes used to differentiate hDCs were derived from 2 different sources of peripheral blood taken, either of them, from healthy donors. For the in vitro infection as- says, the monocytes were obtained by leukopheresis and density gradient centrifugation of a single donor sample (that was screened for HIV-1, hepatitis B, hepatitis C, HTLV-1 and HTLV-2) (Lonza Walkersville, MD, USA), whereas to evaluate the compound-induced immuno- modulation, the monocytes were obtained from he- parinized blood samples from healthy volunteers without and with a medical history of active cutaneous presenta- tion of the disease prior the treatment of the disease (six (6) and seven (7) individuals, respectively), and whose samples were taken after the explanation and subsequent signing of the informed consent (approval by the Ethics Committee, act 04 of June 2009 at the Faculty of Sci- ences of the Universidad Nacional de Colombia). Briefly, for the monocytes derived from blood of vol- unteers without and with a medical history of leishmani- asis, the samples were centrifuged at 2500 rpm for 15 minutes, and the leuko-platelet layer (buffy coat) was collected and diluted in RPMI-1640 (Gibco BRL-Life Technologies Inc.). Subsequently, the cell suspension was used to prepare the density gradient by adding 1 volume of the ficoll-hypaque reagent (Invitrogen, USA) to 2 volumes of diluted blood sample, and the gradients were centrifuged for 30 minutes at 3000 RPM at room temperature, producing a layer of peripheral blood mononuclear cells (PBMCs), which was collected and washed by centrifugation at 2000 RPM for 10 minutes and at 2000 RPM for 7 minutes. Then, the PBMCs were cultured for 2 h at 37˚C in sterile Petri dishes (TPP, Techno Plastic Products, Switzerland) using the previ- ously described culture medium. Ended the incubation time, the non-adherent cells were removed, and the ad- herent cells were incubated in RPMI-1640 medium sup- plemented with recombinant human GM-CSF at 1ng/mL (BD Biosciences, San Diego, USA) and human recom- binant IL-4 at 1 ng/mL (BD Biosciences) for 5 - 7 days. The differentiation process of the hDCs, was monitored by evaluation of the cell morphology using an inverted microscope and the purity of hDCs was evaluated using flow cytometry. Finally, the yield and the cell viability were determined using trypan blue dye staining, and the cells were counted in a Neubawer chamber [23]. 2.2. Compound The plant material from the bark of Raputia heptaphylla used in this study was collected in Albán (Cundinamarca) in Colombia (a specimen of this species rests in the Na- tional Herbarium of Colombia, Institute of Natural Sci- ences, Universidad Nacional de Colombia, under the code COL. 511102). Briefly, to obtain the crude ethano- lic extract, the dried plant material was subjected to ex- traction by percolation in 96% ethanol at room tempera- ture, and the organic solvent was removed by distillation under reduced pressure in a rotavapor. Next, the metabo- lites were extracted from the ethanolic extract, and the purification of the seco-limonoid was performed using conventional chromatographic methods [18]. To eluci- date the structure of this seco-limonoid compound (Fig- ure 1(a)), spectroscopic methods were used (including ultraviolet, infrared (IR), nuclear magnetic resonance (NMR) of hydrogen and carbon, circular dichroism, and nuclear Overhauser enhancement spectroscopy (NOESY) experiments), as also data reported in the literature of related seco-limonoid. Furthermore, the extracts, fractions, and the com- pounds isolated from the plant material as well, the cul- ture medium used were subjected to evaluation for the presence of endotoxins using the LAL test and the re- agent Pyrogent™ Plus Gel Clot LAL assay (Lonza Walkersville, MD, USA). This procedure was performed to ensure that any functional regulation of the hDCs in- fected with L. (V) panamensis and treated with the com- pound was due to the treatment and not to the presence of contaminating lipopolysaccharide (LPS) in the mate- rial. For this purpose, the experimental procedures were made according to the instructions recommended by Lonza. 2.3. Assays to Evaluate the Effects of the Cytotoxic Activity on Mammalian Phagocytic-Cell Targets of Infection with L. (V) panamensis Using the resazurin test for cell metabolism detection, the toxicity of the seco-limonoid was evaluated accord- ing to its ability to damage murine macrophage cells (J774.2) and hDCs [24]. Briefly, 2 × 104 J774.2 cells or 3 × 104 hDCs were exposed to different concentrations of the compound [sequential 1:4 dilutions were used, using as maximum concentration 354.5 μM (200 μg/mL) and a minimum of 22 μM (12.5 ug/mL)] for 72 h at 36˚C - 37˚C in an atmosphere containing 5% CO2 and 90% hu- midity. The controls included cells exposed to the re- agents that were used to solubilize the seco-limonoid [dimethylsulfoxide (DMSO), ethanol, and chloroform] and cells cultured in the absence of the compound. After the 72 h of incubation period, the resazurin solution was Copyright © 2013 SciRes. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 307 (a) (b) Figure 1. (a) correspond to the seco-limonoid compound struc- ture (11α,19β-dihydroxy-7-acetoxy-7-deoxoichangin-C28H36 O12, 565.2285) and (b) shows the cytotoxic activity of the seco-limonoid on monocyte/macrophage cells derived from mice-J774.2 cells (open circles) and hDCs (filled circles). The graph depicts the average percentage viability ± SEM of the cells exposed to different concentrations of the compounds. added at a final concentration per well of 44 μM (Sigma- Aldrich), and after 4 h of incubation at 36˚C - 37˚C, the plates were read using a spectrofluorometer at λexc 535 nm and λemi 590 nm (Tecan, Genios, Salzburg, Austria). The lethal concentration 50% (LC50) of the seco-limo- noid which corresponds to the concentration at which 50% of the cells die, was determined using the statistical software package GraphPad Prism version 5.00 Demo (GraphPad Software, USA). Each assay was performed in duplicate in at least three independent experiments. 2.4. Antileishmanial Activity E valuation 2.4.1. Antileis hmanial Activi ty a gainst P romastigotes of L. (V) panamensis The in vitro antileishmanial effect of seco-limonoid on the extracellular flagellar form of the parasite was evalu- ated by culturing promastigotes of L. (V) panamensis (expressing GFP) in the presence of different concentra- tions of the compound, using for this experiment, seco- limonoid concentrations lower than the LC50 (that had previously been determined in cytotoxicity assays over cells of mammals). Briefly, 2 × 105 promastigotes were incubated for 72 h at 25˚C - 26˚C in the presence of 106.3 μM (60 μg/mL), 26.6 μM (15 μg/mL), 6.6 μM (3.75 μg/mL), 1.1 μM (0.63 μg/mL), 0.55 μM (0.31 μg/mL) or 0.28 μM (0.16 ug/mL) of seco-limonoid. As a positive control for the direct cytotoxicity of the com- pound against the extracellular form of the parasite, the promastigotes were exposed to different concentrations of pentamidine isethionate (Pentacarinat®, Sanofi-Av- entis, France) at 1:4 dilutions starting at a maximum concentration of 5 μg/mL to a minimum concentration of 1 × 10−5 μg/mL, using the same experimental conditions as those used in the evaluation tests of the activity of the compound. Next, the viability of the parasites was de- termined by flow cytometry (FacsCantoII) (BD Biosci- ences) and resazurin metabolic assay (Sigma Chemical Co.), where the reduction in the fluorescence emission from the promastigotes and the decrease in their meta- bolic activity, was associated with non-viable parasites. 2.4.2. Antileishmanial Activity agains t the Intracellular Form of the Parasite The antileishmanial effect on intracellular amastigotes was determined by in vitro APC infection assays using J774.2 cells and hDCs. 2 × 105 cells were infected with promastigotes of L. (V) panamensis (constitutively ex- pressing GFP) at ratios between 1:40 and 1:50 (cell per parasites) for 6 h, time after which the non-internalized parasites were removed by washing with RPMI-1640 medium, and once the infection was established, the cells were exposed to various concentrations of seco-limonoid [consecutive 1:4 dilutions were used starting from a maximum concentration of 53.2 μM (30 μg/mL) down to a minimum concentration of 0.81 μM (0.47 μg/mL)] for 48 h at 36˚C in an atmosphere of 5% CO 2. Similarly, infected cells treated with 2000 μg/mL, 500 μg/mL, 250 μg/mL, 125 μg/mL, 40 μg/mL, and 20 μg/mL of sodium stiboglucon ate® (Ryan Laboratories, Colombia) were used as positive controls for the resolution of the in vitro infection. Completed the incubation times, the super- natants were collected and cryopreserved at −20˚C until they were required for quantification of the cytokines associated with inflammatory processes. The J774.2 cells were transferred to flow cytometry tubes to quantify the percentage of infected cells by flow cytometry (Fac- sCanto II, BD, San José, CA, USA), and thereby, the fluorescence emitted by the fluorescent parasites was captured in the green channel using a 530/30 nm filter, and was used to distinguish the infected cells from the uninfected population. Because of the complexity of hDCs, clear differences among the infected cells popula- tion and uninfected cells were not easily observed using flow cytometry, due mainly at the characteristic auto- fluorescence of this kind of cells, factor for which is lim- ited the analysis using this technique; therefore, light microscopy with slides containing Giemsa-stained cell preparations were used to evaluate infection on hDCs. For this assay, the protocol described above was used to evaluate the antileishmanial activity against the intracel- lular form of the pathogen; however, the hDCS were placed onto the chamber slides, containing 16 wells (Nunc, Rochester, NY, USA) instead of 96-well flat- bottom plates. Free parasites, uninfected cells, infected cells in the absence of the compound, and infected cells exposed to the conventional treatment (pentavalent an- timonials) were used as controls for each of the assays. In these assays, reductions in the percentage of infected cells and/or in the emitted fluorescence by the internal- ized parasites were the parameters that were indicative of the parasiticidal activity of the compounds. Antileishma- nial activity against the promastigotes and intracellular Copyright © 2013 SciRes. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 308 amastigotes was evaluated in at least three independent experiments. Using these assays, the effective concentration 50 (EC50), which corresponds to the concentration that re- duces the parasite burden by 50% in experimentally in- fected phagocytes, was determined, and the division of the values obtained from the cytotoxic antileishmanial activity on the intracellular pathogens [Lethal Concentra- tion 50 (LC50)/Effective Concentration 50 (EC50)] cor- responds to the selectivity index (SI), a parameter related to the selectivity and safety of the tested molecule. For the compounds with potential leishmanicidal activity, arbitrary SI values have been reported, considering a value ≥ 2 to be significant. 2.4.3. Antileishmanial Activity against Axenic Amastigotes The evaluation of antileishmanial activity against the axenic forms of the parasite was performed by seeding 2 - 5 × 105 axenic amastigotes per well in 96-well flat-bot- tom plates (TPP, Switzerland) which were exposed to different concentrations of the compound for 72 h at 36˚C, 5% CO2 and 90% humidity (using the concentra- tions mentioned previously for the evaluation of activity against intracellular amastigotes). Pentamidine isethi- onate® and sodium stibogluconate® were used as treat- ment controls, and cells that were not exposed to treat- ment or compounds were included in the assays, as nega- tive controls. After the incubation period, the viability of the cells was determined using the indirect resazurin metabolic assay (Sigma-Aldrich, St. Louis, USA), fol- lowing the protocol described in a previous section. 2.5. Immunomodulatory Activity Assessment 2.5.1. Determination of Nitric Oxide (NO) J774.2 cells or hDCs (4 × 105 cells) were infected at a ratio of between 1:40 and 1:50 with promastigotes of L. (V) panam ensis (not transfected parasites) for 6 h at 36˚C - 37˚C in an atmosphere with 5% CO2 and 90% humidity. Once the experimental infection was estab- lished, the non-internalized parasites were removed by gentle washes using a sterile saline solution, followed by treatment of the cells with the concentrations of the seco- limonoid mentioned previously (see protocols for the evaluation of antileishmanial activity). Sodium stiboglu- conate® was used as control drug (as described previ- ously). Similarly, a sample of cells was treated with 10 μg/mL phorbol myristateacetate for 24 h as a positive control for the induction of NO, as also, a sample of cells not exposed to any type of treatment (with and without infection) was used to determine the basal levels of NO production for each population. The NO production was monitored after 48 h of treatment with the seco-limonoid or the control drug, and latter, the cells was transferred to flow cytometry tubes and staining with 4 μM DAF-FM diacetate solution (Invitrogen, USA) for 1 h at 36˚C - 37˚C. Subsequently, the cells were washed, with the aim to remove the unincorporated probe and the readings were performed in a BD FacsCanto II flow cytometer using the blue laser (λexc 488 nm) as the excitation source and the 530/30 nm filter for detection. 2.5.2. Quantification of Cy tokines in Supernatants Cultures Briefly, 15 µL of a mixture comprising capture beads for each of the cytokines to be evaluated (IL-6, IL-10, MCP-1, IFN-γ, TNFα, and IL-12p70 for the J774.2 cells or IL-8, IL-1β, IL-6, IL-10, TNF and IL-12p70 for the hDC) was mixed with 15 µL of the PE detection reagent and 50 µL of the culture supernatants. The mixtures were incubated at ambient temperature for 2 - 3 h protected from the light, and after this incubation period, the sam- ples were washed to remove the unbound PE detection antibody. On the other hand, using the same conditions mentioned before, standards for each cytokine were run simultaneously. The readings were performed using the FacsCanto II flow cytometer (BD Biosciences, San Diego, CA, USA) and the BD FACSDiva (BD Biosci- ences) acquisition software. The data were analyzed us- ing the FCAP ArrayTM (Soft Flow) software. 2.5.3. Evaluation of Cell Surface Marker Expression For the phenotypic analysis of the hDCs, the surface marker expression was evaluated using the following antibodies: clone L243, (APC-conjugated anti-HLA-DR), clone DCN46 (FITC-conjugated anti-CD209), clone MφP9 (PerCP-conjugated anti-CD14), clone HB15e (PE- conjugated anti-CD83), and clone L307.4 (PE-conju- gated anti-CD80). The acquisition and analysis were performed using a FacsCanto II (BD, Biosciences) flow cytometer and the acquisition software FACSDiva (BD Biosciences). 2.6. Statistical Analyses The results from each experimental protocol were ana- lyzed according to the parameters for each technique and were validated by comparison with the established con- trols for each assay. Therefore, the data obtained allowed the determination of the lethal concentration 50 (LC50) and the effective concentration 50 (EC50) as expected according to the technique used. Using nonparametric tests, it was possible to evaluate differences between the experimental groups, according to the parameters of the technique employed. For these analyses, the statistical software package GraphPad Prism version 5.00 Demo (GraphPad Software, USA) was used. Copyright © 2013 SciRes. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 309 3. RESULTS 3.1. Cytotoxic Activity on Mammalian Cells Targeted by L. (V) panamensis Infection The cytotoxic activity of the seco-limonoid on cells of the murine monocyte/macrophage lineage (the murine macrophage cell line J774.2) and hDCs was determined using the resazurin metabolic assay, which indirectly demonstrates the viability of a cell population through evaluating of the metabolism of the non-fluorescent in- dicator (resazurin) to a fluorescent molecule (resorufin) [25]. In these assays, we observed a decreased suscepti- bility of the murine cells to the toxicity induced by the seco-limonoid, determining an LC50 of 368.5 µM (207.9 µg/mL) for the J744.2 cells versus 116.8 µM (65.89 µg/mL) for the hDCs. The cytotoxic effect induced by the greatest concentration of the compound observed in both cell lines was statistically significant (P value < 0.0001). The cell viability results in these cell populations ex- posed to varying concentrations of the seco-limonoid are shown in Figure 1(b), where it’s shows that to achieve similar death levels in the hDCs (filled circles) as in the J774.2 cells (empty circles) a lower concentration of the compound is required. Moreover, pentavalent antimony- als (sodium stibogluconate) did not induce toxicity, as demonstrated by the resazurin metabolic assay, which could not determine an LC50 for the two cell populations evaluated (LC50 > 2000 µg/mL). 3.2. Antileishmanial Activity With the aim of evidencing whether previously demon- strated activity of seco-limonoid was conserved in the different stages of the pathogen, tests were developed on the extracellular form (promastigotes), as well as the intracellular and axenic amastigotes forms. The parasites used in the present study belong to the genus Leishmania, subgenus Viannia, specie L. panamensis, which is one of the most important epidemiological species in South America, being the primarily responsible for the cases of cutaneous leishmaniasis in Colombia. The data obtained show that the activity of the seco-limonoid compound observed here appears to be directed specifically against the intracellular form of the pathogen (intracellular amastigotes) determining an EC50 of 7.9 µM (4.48 µg/mL) and 25.5 µM (14.39 µg/mL) using the in vitro infection model of J774.2 cells and hDCs, respectively. Figure 2 shows the representative results of the in vitro infection assays using infected murine cells (panel 2a) or hDCs (panels 2b and 2c). In the panel a of the Figure 2, the broken line of the histogram, and panel b, are the infected cells without treatment, while, the solid lines in panel 2a and the panel c correspond to cells exposed to 30 µg/mL of the seco-limonoid. Here, we show that the in vitro infection is controlled when cells were treated with compound, as demonstrated, by the decrease in the percentage of fluorescent cells (62.5% in untreated infected cells versus 10.32% in in- fected cells treated with seco-limonoid at 30 µg/mL) as also, was observed in the slides stained with Giemsa so- lution a decrease in uninfected cells in relation to the total cell population (Figures 2(d) and (e)). Similarly, Figure 3(a) shows the antileishmanial effect on axenic amastigotes of L. (V) panamensis, with an EC50 of 86.3 µM (48.7 µg/mL), demonstrating a concentration depen- dent response, which was not observed on the flagellar form of the pathogen (statistically significant differ- ences were found when comparing the response obtained in both stages with 60 µg/ml of the compound, being most susceptible to the effect of the compound the axenic amastigotes form that promastigotes with a P value of 0.0024) (Figure 3(b)). Figure 3(c) shows the results obtained with pentamidine drug on the flagellar ex- tracellular form of the pathogen (promastigotes) deter- mining an EC50 of 0.6 µg/ml Table 1 shows a summary of the cytotoxicity results and the efficacy observed in the tests described. In this respect, an antileishmanial effect was demon- strated for the amastigote forms of the parasite (being mostly susceptible the intracellular form that the axenic); finding that the concentration of compound required to control 50% of the population for the intracellular stage of the parasite was lower (4.48 and 14.39 µg/mL for the infected J774.2 and hDCs that were treated with the compound, respectively) than for the axenic stage (48.7 µg/mL), which allows us to suggest that the compound, in addition to exhibiting antiparasitic activity capable of controlling the pathogen, may be acting on some meta- bolic pathways of APCs, leading to the complete resolu- tion of the infection, possibly by the recovery of the an- timicrobial activity that was silenced by the pathogen. The data indicate that this compound needs to be me- tabolized to carry out its activity or its antileishmanial activity is associated with an event caused by the immu- nomodulation of APCs by this molecule. 3.3. Immunomodulatory Activity 3.3.1. Nitric Oxi d e (NO) Production Given the importance of the free nitrogen radicals in the control of intracellular infectious agents (such as Leishmania spp.) in this study, we determined the levels of NO in infected murine J774.2 macrophages and hDCs treated with the seco-limonoid by flow cytometry using the indicator DAF-FM diacetate (4-amino-5-methyl- amino- 2’,7’-difluorofluorescein diacetate) as a probe. In both in vitro infection models (J774.2 and hDCs) the seco-limonoid induced an increase in NO production in nfected and treated cells (with significant differences for i Copyright © 2013 SciRes. OPEN ACCESS 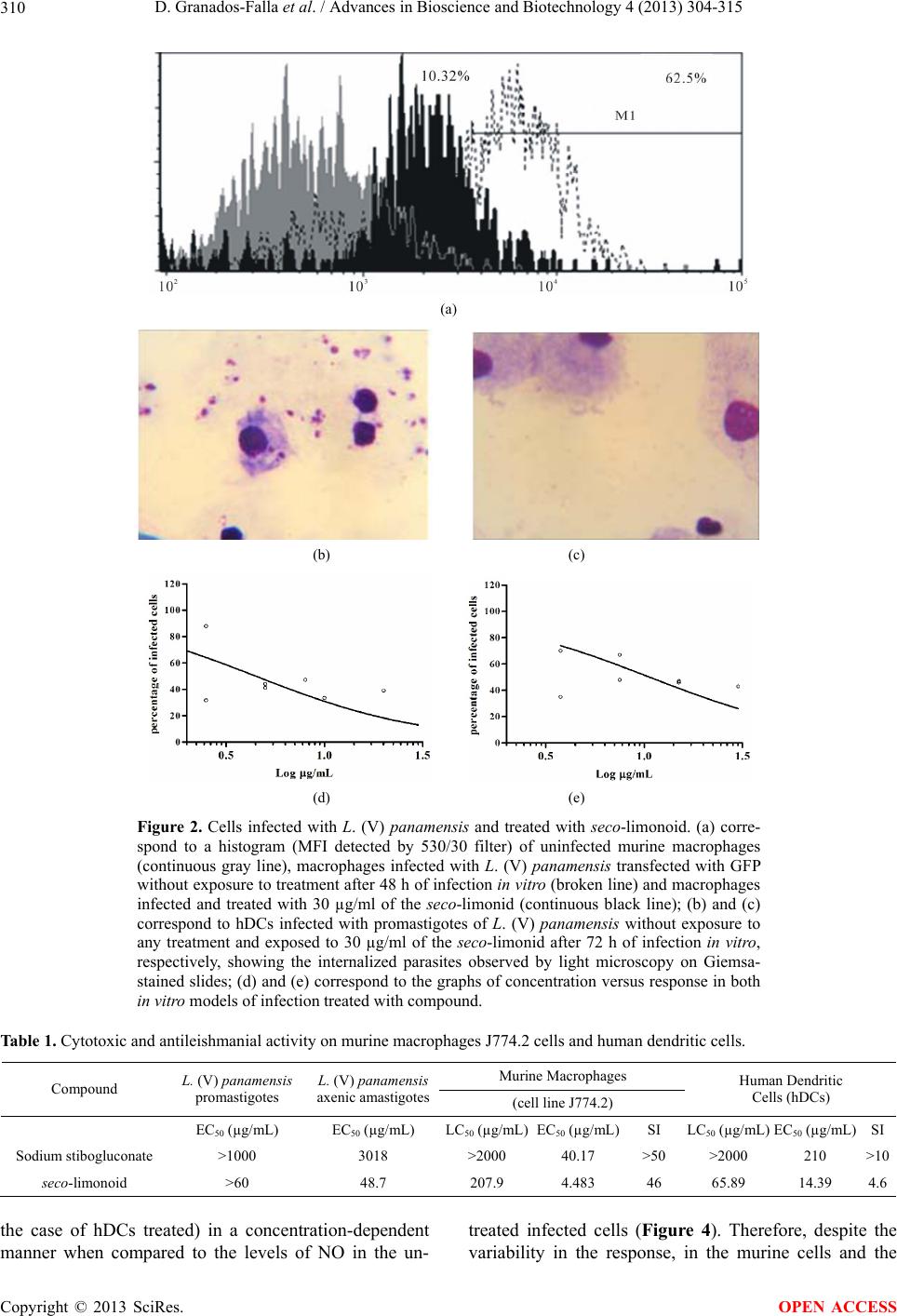 D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 Copyright © 2013 SciRes. 310 (a) (b) (c) (d) (e) Figure 2. Cells infected with L. (V) panamensis and treated with seco-limonoid. (a) corre- spond to a histogram (MFI detected by 530/30 filter) of uninfected murine macrophages (continuous gray line), macrophages infected with L. (V) panamensis transfected with GFP without exposure to treatment after 48 h of infection in vitro (broken line) and macrophages infected and treated with 30 µg/ml of the seco-limonid (continuous black line); (b) and (c) correspond to hDCs infected with promastigotes of L. (V) panamensis without exposure to any treatment and exposed to 30 µg/ml of the seco-limonid after 72 h of infection in vitro, respectively, showing the internalized parasites observed by light microscopy on Giemsa- stained slides; (d) and (e) correspond to the graphs of concentration versus response in both in vitro models of infection treated with compound. Table 1. Cytotoxic and antileishmanial activity on murine macrophages J774.2 cells and human dendritic cells. Murine Macrophages Compound L. (V) panamensis promastigotes L. (V) panamensis axenic amastigotes(cell line J774.2) Human Dendritic Cells (hDCs) EC50 (µg/mL) EC50 (µg/mL) LC50 (µg/mL)EC50 (µg/mL)SI LC50 (µg/mL) EC50 (µg/mL)SI Sodium stibogluconate >1000 3018 >2000 40.17 >50 >2000 210 >10 seco-limonoid >60 48.7 207.9 4.483 46 65.89 14.39 4.6 the case of hDCs treated) in a concentration-dependent manner when compared to the levels of NO in the un- treated infected cells (Figure 4). Therefore, despite the variability in the response, in the murine cells and the OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 311 (a) (b) (c) Figure 3. (a) shows the cytotoxic activity of seco-li- monoid on axenic amastigotes (the graph shows the average percentage viability ± SD); while (b) and (c) correspond to cytotoxic activity of the seco-limonoid and Pentacarinat® against the extracellular flagellar form of the parasite (promastigotes). The graphs show the average percentage mortality ± SD. hDCs, there is a marked tendency toward NO production at the highest concentration of seco-limonoid, which reinforces the concept of its potential immunomodula- tory activity. It should be noted that the compound used in this study, as well the culture media used here for the maintenance of the cell populations described before, did not yield positive results in the determination of endo- (a) (b) Figure 4. The diagrams correspond to nitric oxide (NO) production by murine macrophages (J774.2) (a) and human dendritic cells (hDCs) (b) The graph depicts the mean of the mean fluorescence intensity (MFI) and its SEM. toxin assay (commercial kit which present a sensibility range of 0.06 EU/mL) 3.3.2. Quantification of Cytokines by Flow Cytometry To evaluate the possible immunomodulatory effect of the seco-limonoid, we quantified cytokines associated with inflammatory processes using the cytometric bead array (CBA) method for flow cytometry. Thereby, IL-6, IL-10, MCP-1, IFN-γ, TNF, and IL-12p70 were assayed in the supernatants of the J774.2 cells, and IL-8, IL-1β, IL-6, IL-10, TNFα, and IL-12p70 were assayed in the super- natants of the hDCs from patients with active disease (cutaneous presentation) and control volunteers with no history of the disease. In this regard, we determined that the seco-limonoid modulates cytokine secretion selec- tively in cells infected with L. (V) pan amensis in the two in vitro infection models used (see Figures 5 and 6) Copyright © 2013 SciRes. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 Copyright © 2013 SciRes. 312 Figure 5. Correspond to levels of cytokines present in the supernatans of murine cells J774.2. Figure 6. Correspond to cytokines levels in the supernatans of hDCs. preferentially to the pro-inflammatory phenotype. Nota- bly, despite the trend observed, significant differences between the two in vitro models when compared to the untreated infected cells were not observed. Furthermore, the evaluation on the production of solu- ble mediators involved in inflammatory processes in cells derived from active leishmaniasis patients and the control volunteers demonstrated that the hDCs derived from patients with active disease produced more of these cytokines compared with the control group of unexposed patients; however, because of the variability of the re- sults, significant differences were not observed. 3.3.3. E valuation o f Cell Surfa ce Markers by Flow Cytometry To explore the possible immunomodulatory effect of the seco-limonoid on hDCs (critical cell population for the development of adequate immune response for the reso- lution of this disease) the expression of cell surface markers associated with the maturation of the hDCs was OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 313 assessed. The cells were labeled with commercial mono- clonal antibodies in the presence of HLA-DR, DC-SIGN, and the co-stimulatory molecule human CD83, allowing, in this way the evaluation of the basic phenotypic char- acteristics of the hDCs population of infected that was treated with the compound. The results demonstrate that in infected cells treated with 15 µg/mL of the seco-li- monoid, the expression of HLA-DR was enhanced (sig- nificant differences between the untreated infected cells and the infected cells treated with the compound in the two experimental groups, P value < 0.05) (Figure 7). Similar results were obtained when evaluating the ex- pression of the DC-SIGN molecule and CD83 (data not shown); however, no significant differences were ob- served for these molecules, when comparing the un- treated infected cells with the treated cells. It is notewor- thy that the number of positive events in the hDCs de- rived from patients with active disease was less than the number of positive events in the hDCs derived from the control volunteers for the three molecules tested; how- ever, despite this marked tendency, significant differ- ences between the two experimental groups of individu- als were not observed. 4. DISCUSSION The current first-choice treatment for leishmaniasis is based on the administration of pentavalent antimonial salts, which is still used despite their associated [7,11] adverse effects, as well as, the appearance of drug-re- sistant parasite [6,26] and the high cost associated with patient care. Also, despite the existence of second-line drugs (as amphotericin B, hexadecilphosphocholine, pen- tamidine isethionate, and paromomycin sulfate), these also have presented some drawbacks (such as adverse effects induced in the treated individuals and the high costs involved in the access to certain formulations). Considering this, it acquires even more relevance the ur- gent need for the development of new therapeutic agents for the treatment of this disease [5]. For many years, the study of compounds derived from natural products has been an important source of information for the design and/or discovery new therapeutic alternatives for the control of diverse diseases, such as leishmaniasis disease [13,17]. Therefore, various research studies have focused on the search for new, safer, and more effective bioactive molecules against leishmaniasis. In this study, we confirmed the antileishmanial activity (a) (b) hDCS Infected hDCS Treated infected hDCs Basal with 30 μg/mL of seco-limonoid compound (c) Figure 7. (a) and (b) shows the expression of the HLA-DR molecule in hDCs derived from individuals with and without clinical history of Leishmania infection, respectively. **correspond to significant differences finding when comparing the response found it with the basal response with a P value < 0.05, *significant differences with a P value < 0.01. (c) corresponds to histograms repre- senting the HLA-DR expression in hDCs. Copyright © 2013 SciRes. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 314 of a seco-limonoid (11α,19β-dihydroxy-7-acetoxy-7-de- oxoichangin), which was isolated from the bark of Rapu- tia heptaphylla (Rutaceae family), which was previously described by Coy and colleagues [18]. We suggest here a possible mechanism for the antiparasitic activity of this compound that is related to the immunomodulatory ef- fect on APCs. In this regard and taking into account the information currently available regarding the parasite responsible for leishmaniasis and the information regarding its verte- brate host [20,27-29] suggest that immunomodulation is an attractive and promising tool [7,30,31] for developing new therapies for the adequate control of intracellular pathogens, such as Leishmania spp. [32]. Here, we ob- served that the seco-limonoid exhibits a specific activity against intracellular amastigotes of Leishmania and that this activity is possibly mediated or promoted by the immunomodulatory effect that this compound induces only in infected cells (depending on their interaction with pathogen). Thereby, this seco-limonoid has been shown to be a bioactive molecule exhibiting an interesting spe- cific projection (because it would only modulate the mi- crobicidal activity of infected cells) that can be used for the design of a leishmanicidal therapy. The immunomodulatory potential of the seco-limonoid 11α,19β-dihydroxy-7-acetoxy-7-deoxoichangin is sup- ported by the production of nitric oxide and the expres- sion of HLA-DR, which is down-regulated following infection and exhibits a tendency to recover after expo- sure to this seco-limonoid. It is also important to high- light the importance of developing studies to confirm this activity in vivo (results using the hamster model Meso- cricetus auratus have demonstrated the resolution of experimental cutaneous lesions of leishmaniasis). Notably, for many years, numerous molecules exhibi- ting microbicidal activity has been reported; however, these molecules have not been developed into drug pro- totypes. One of the reasons for this delay is the difficulty in establishing the mechanism of action, which rein- forces the importance of this study with respect to the immunomodulatory potential of the seco-limonoid in in- fected cells. Furthermore, this study enhances the importance of considering the highly complex life cycle of the patho- gen responsible for leishmaniasis [33]. When developing in vitro screens to study bioactive molecules for the con- trol of this microorganism, there is a necessity for de- veloping assays to evaluate possible antiparasitic activi- ties against parasites of the genus Leishmania at the dif- ferent life cycle stages of this pathogen. It is particularly important to develop antiparasitic therapies against the form of the pathogen responsible for the disease in the vertebrate host during the clinical manifestations of the disease [34,35], and is in this way, that in the present study we confirmed the efficacy of a seco-limonoid (triterpene) [18] which exhibits activity against only the intracellular form of the parasite, leading to a decrease and subsequent resolution of the infection in treated in- fected cells. We demonstrated that this activity is related to an immunomodulatory mechanism of action in which the compound induces an apparent “reactivation” of the “paralyzed” APC caused by the survival mechanisms developed by the pathogen. 5. ACKNOWLEDGEMENTS We express our gratitude to the Immunotoxicology Research Group, the Natural Plant Products Group of the Universidad Nacional de Co- lombia, and the PECET of the Universidad de Antioquia. This project was financed by Bogotá Research Division (DIB) at the Universidad Nacional de Colombia (projects Hermes No. 15099 and No. 16105) and the Colombian Institute for the Development of Science and Technol- ogy “Francisco Jose de Caldas” (project No.110151928476). REFERENCES [1] WHO (2010) Control of the leishmaniases. Report of a meeting of the WHO Expert Committee on the control of Leishmaniases, World Health Organization, Geneva. [2] Desjeux, P. (2004) Leishmaniasis: Current situation and new perspectives. Comparative Immunology, Microbiol- ogy & Infectious Diseases, 27, 305-318. doi:10.1016/j.cimid.2004.03.004 [3] WHO (2004) TDR—Tropical disease research. World Health Organization, Geneva. [4] Mitropoulos, P., Konidas, P. and Durkin-Konidas, M. (2010) New World cutaneous leishmaniasis: Updated re- view of current and future diagnosis and treatment. Jour- nal of the American Academy of Dermatology, 63, 309- 322. doi:10.1016/j.jaad.2009.06.088 [5] Santos, D.O., Coutinho, C.E., Madeira, M.F., Bottino, C.G., Vieira, R.T., Nascimento, S.B., Bernardino, A., Bourguignon, S.C., Corte-Real, S., Pinho, R.T., Rodri- gues, C.R. and Castro, H.C. (2008) Leishmaniasis treat- ment—A challenge that remains: A review. Parasitology Research, 103, 1-10. doi:10.1007/s00436-008-0943-2 [6] Croft, S.L., Sundar, S. and Fairlamb, A.H. (2006) Drug resistance in leishmaniasis. Clinical Microbiology Re- views, 19, 111-126. doi:10.1128/CMR.19.1.111-126.2006 [7] Croft, S.L., Seifert, K. and Yardley, V. (2006) Current scenario of drug development for leishmaniasis. Indian Journal of Medical Research, 123, 399-410. [8] Frezard, F., Demicheli, C. and Ribeiro, R.R. (2009) Pen- tavalent antimonials: New perspectives for old drugs. Molecules, 14, 2317-2336. doi:10.3390/molecules14072317 [9] Haldar, A.K., Sen, P. and Roy, S. (2011) Use of antimony in the treatment of leishmaniasis: Current status and fu- ture directions. Molecular Biology International, 2011, 1-23. doi:10.4061/2011/571242 [10] Bray, P.G., Barrett, M.P., Ward, S.A. and de Koning, H.P. Copyright © 2013 SciRes. OPEN ACCESS  D. Granados-Falla et al. / Advances in Bioscience and Biotechnology 4 (2013) 304-315 315 (2003) Pentamidine uptake and resistance in pathogenic protozoa: Past, present and future. Trends in Parasitology, 19, 232-239. doi:10.1016/S1471-4922(03)00069-2 [11] Croft, S.L., Barrett, M.P. and Urbina, J.A. (2005) Che- motherapy of trypanosomiases and leishmaniasis. Trends in Parasitology, 21, 508-512. doi:10.1016/j.pt.2005.08.026 [12] Paila, Y.D., Saha, B. and Chattopadhyay, A. (2010) Am- photericin B inhibits entry of Leishmania donovani into primary macrophages. Biochemical and Biophysical Re- search Communications, 399, 429-433. doi:10.1016/j.bbrc.2010.07.099 [13] Newman, D.J. and Cragg, G.M. (2007) Natural products as sources of new drugs over the last 25 years. Journal of Natural Products, 70, 461-477. doi:10.1021/np068054v [14] Harvey, A.L. (2008) Natural products in drug discovery. Drug Discovery Today, 13, 894-901. doi:10.1016/j.drudis.2008.07.004 [15] Rocha, L.G., Almeida, J.R., Macedo, R.O. and Barbosa- Filho, J.M. (2005) A review of natural products with an- tileishmanial activity. Phytomedicine, 12, 514-535. doi:10.1016/j.phymed.2003.10.006 [16] Mishra, B.B., Singh, R.K., Srivastava, A., Tripathi, V.J. and Tiwari, V.K. (2009) Fighting against leishmaniasis: Search of alkaloids as future true potential anti-leishma- nial agents. Mini Reviews in Medicinal Chemistry, 9, 107- 123. doi:10.2174/138955709787001758 [17] de Carvalho, P.B. and Ferreira, E.I. (2001) Leishmaniasis phytotherapy. Nature’s leadership against an ancient dis- ease. Fitoterapia, 72, 599-618. doi:10.1016/S0367-326X(01)00301-X [18] Coy Barrera, C.A., Coy Barrera, E.D., Granados Falla, D.S., Delgado Murcia, G. and Cuca Suarez, L.E. (2011) Seco-limonoids and quinoline alkaloids from Raputia heptaphylla and their antileishmanial activity. Chemical & Pharmaceutical Bulletin, 59, 855-859. doi:10.1248/cpb.59.855 [19] Handman, E. (1999) Cell biology of Leishmania. Ad- vances in Parasitology, 44, 1-39. doi:10.1016/S0065-308X(08)60229-8 [20] Basu, M.K. and Ray, M. (2005) Macrophage and Leish- mania: An unacceptable coexistence. Critical Reviews in Microbiology, 31, 145-154. doi:10.1080/10408410591005101 [21] Rosas, L.V. (2005) Phytochemistry, chemosystematic and searching of new antichagasic and antileishmaniasis drugs: Study of Raputia praetermissa (Rutaceae). Tese (Doutorado), Universidade Federal de São Carlos, São Carlos. [22] Pulido, S.A., Munoz, D.L., Restrepo, A.M., Mesa, C.V., Alzate, J.F., Velez, I.D. and Robledo, S.M. (2012) Im- provement of the green fluorescent protein reporter sys- tem in Leishmania spp. for the in vitro and in vivo screening of antileishmanial drugs. Acta Tropica, 122, 36-45. doi:10.1016/j.actatropica.2011.11.015 [23] Strober, W. (1997) Trypan blue exclusion test of cell viability. In: Coligan, J.E., Krusbeek, A.M., Margulies, D.H., Shevach, E.M. and Strober, W., Eds, Current Pro- tocols in Immunology, John Wiley & Sons, Inc., New York. [24] Buckner, F.S. and Wilson, A.J. (2005) Colorimetric assay for screening compounds against Leishmania amastigotes grown in macrophages. American Journal of Tropical Medicine and Hygiene, 72, 600-605. [25] O’Brien, J., Wilson, I., Orton, T. and Pognan, F. (2000) Investigation of the Alamar Blue (resazurin) fluorescent dye for the assessment of mammalian cell cytotoxicity. European Journal of Biochemistry, 267, 5421-5426. doi:10.1046/j.1432-1327.2000.01606.x [26] Chakravarty, J. and Sundar, S. (2010) Drug resistance in leishmaniasis. Journal of Global Infectious Diseases, 2, 167-176. doi:10.4103/0974-777X.62887 [27] Bogdan, C. and Rollinghoff, M. (1999) How do proto- zoan parasites survive inside macrophages? Parasitology Today, 15, 22-28. doi:10.1016/S0169-4758(98)01362-3 [28] Burchmore, R.J. and Barrett, M.P. (2001) Life in vacu- oles--nutrient acquisition by Leishmania amastigotes. In- ternational Journal for Parasitology, 31, 1311-1320. [29] Mougneau, E., Bihl, F. and Glaichenhaus, N. (2011) Cell biology and immunology of Leishmania. Immunological Reviews, 240, 286-296. doi:10.1111/j.1600-065X.2010.00983.x [30] El-On, J. (2009) Current status and perspectives of the immunotherapy of leishmaniasis. Israel Medical Associa- tion Journal, 11, 623-628. [31] Mansueto, P., Vitale, G., Di Lorenzo, G., Rini, G.B., Mansueto, S. and Cillari, E. (2007) Immunopathology of leishmaniasis: an update. International Journal of Im- munopathology and Pharmacology, 20, 435-445. [32] Saha, P., Mukhopadhyay, D. and Chatterjee, M. (2011) Immunomodulation by chemotherapeutic agents against leishmaniasis. International Immunopharmacology, 11, 1668-1679. doi:10.1016/j.intimp.2011.08.002 [33] Vermeersch, M., da Luz, R.I., Tote, K., Timmermans, J.P., Cos, P. and Maes, L. (2009) In vitro susceptibilities of Leishmania donovani promastigote and amastigote stages to antileishmanial reference drugs: Practical rele- vance of stage-specific differences. Antimicrobial Agents and Chemotherapy, 53, 3855-3859. doi:10.1128/AAC.00548-09 [34] De Muylder, G., Ang, K.K., Chen, S., Arkin, M.R., Engel, J.C. and McKerrow, J.H. (2011) A screen against Leishmania intracellular amastigotes: Comparison to a promastigote screen and identification of a host cell-spe- cific hit. PLOS Neglected Tropical Diseases, 5, e1253. doi:10.1371/journal.pntd.0001253 [35] Shukla, A.K., Singh, B.K., Patra, S. and Dubey, V.K. (2010) Rational approaches for drug designing against leishmaniasis. Applied Biochemistry and Biotechnology, 160, 2208-2218. doi:10.1007/s12010-009-8764-z Copyright © 2013 SciRes. OPEN ACCESS
|