 Psychology 2013. Vol.4, No.2, 111-117 Published Online February 2013 in SciRes (http://www.scirp.org/journal/psych) http://dx.doi.org/10.4236/psych.2013.42016 Copyright © 2013 SciRes. 111 Screening for Personality Disorders: A Comparison of the Dimensional NEO-FFI with the Categorical SAPAS-SR* Sara Germans1#, Alexander Rath2, Guus L. Van Heck3, Paul P. G. Hodiamont4 1Departement of Psychiatry, Hospital of Namsos, Namsos, Norway 2Department of Psychology, University Nijmegen, Nijmegen, The Netherlands 3Department of Psychology, Tilburg University, Tilburg, The Netherlands 4Department of Psychiatry, Radboud University Nijmegen, Nijmegen, The Netherlands Email: #sara.germans@helse-nordtrondelag.no Received November 20th, 2012; revised December 18th, 2012; accepted January 10th, 2013 In psychiatric outpatients, the usefulness of the dimensional NEO-FFI as a screening instrument for per- sonality disorders (PDs) was compared with the categorical screening instrument SAPAS-SR using the SCID-II as the gold standard. Major research questions are: 1) is the NEO-FFI a useful screening instru- ment for PDs? 2) does the NEO-FFI outperform a categorical screening instrument (SAPAS-SR)? 3) does combining both instruments improve the screening results? Extreme raising on Big Five personality trait domains (NEO-FFI) domain scores were examined in relation to the presence and the number of PDs as diagnosed, with to the SCID-II. Additionally, the NEO-FFI, in conjunction with a short self-report screening instrument (SAPAS-SR), was analysed with respect to sensitivity and specificity for screening of PDs. According to the SCID II, 97 patients (50%) were suffering from a PD. The majority of them had no (35.9%) or only one (40%) extreme score on one of the Big Five personality domains. There were no significant relationships between separate extreme traits on PD or five factor profiles, as proposed in the literature, and the presence of a SCID-II PD. Comparisons of the NEO-FFI with the SAPAS-SR showed no significant relationships. Using both screeners in conjunction resulted in an increase in specificity and the number of correctly classified cases at the expense, however, of the sensitivity. Correlation and re- gression analyses showed that personality traits are statistically significant predictors for each of the12 PDs. However, the associations between NEO-FFI scores and the DSM-VI-TR PD criteria were rather modest. Support could not be obtained for the view that separate extreme scores on basic personality traits or combinations of such scores in five-factor profiles will provide adequate screening possibilities for PDs. The SAPAS-SR has better screening potential than the NEO-FFI or the SAPAS-SR and the NEO-FFI to- gether. Keywords: Personality Disorders; Big Five; Personality Screening Instrument Introduction Co-morbid personality disorders (PD) not only adversely af- fect the outcome of mental illnesses, but are also important factors in the choice of treatment options (Moran, Walsh, Tyrer, Burns, Creed, & Fahy, 2003; Newton-Howes, Tyrer, & Johnson, 2006). For this reason, assessment of the personality status should be a part of each initial psychiatric examination. Diag- nostic instruments with an adequate psychometric profile, like the Structured Clinical Interview for DSM-IV Personality Dis- orders (SCID-II) (Spitzer, Williams, Gibbon, & First, 1990) and the Structured Interview for DSM-IV Personality Disorders- revised (SIDP-R) (Reich 1989), are well-known and accessible, but when it comes to daily reality, it is not always feasible to use these instruments in a clinical setting. Major reasons are that they are rather time-consuming and require trained per- sonnel with a profound knowledge of psychopathology. To reduce the time, inherent in full scale interviews, one might resort to one of the available short structured interviews for PD. Examples include the Standardized Assessment of Per- sonality-Abbreviated Scale (SAPAS) (Moran, Leese, Lee, Wal- ters, Thornicroft, & Mann, 2003), the Iowa Personality Disorder Screen (IPDS) (Langbehn, Pfohl, Reynolds, Clark, Battaglia, Bellodi et al., 1999), the Rapid Personality Assessment Sched- ule (PAS-R) (Van Horn, Manley, Leddy, Cicchetti, & Tyrer, 2000), and the Quick Personality Assessment Schedule (PAS-Q) (Germans, Van Heck, & Hodiamont, 2011) which all have screening capacity for PD in terms of the DSM-IV and ICD-10. However, it should be noted that even such short interviews require a great deal of specific clinical training. An alternative for interviews are self-report measures. Ex- amples include the Personality Diagnostic Questionnaire— Revised (PDQ-R) (Hyler, Skodol, Kellman, Oldham, & Ros- nick, 1990) and the Assessment of DSM-IV Personality Disor- ders (ADP-IV) (Schotte, Doncker, Vankerckhoven, Vertommen, & Cosyns, 1998). While saving time, these self-report questionnaires require patients who are able to read and write properly and maintain an adequate level of concentration, because questionnaires of- ten contain over 100 items. Furthermore, self-report question- naires generally tend to overrate the prevalence of PDs and to have poor specificity (Verheul &Van Den Brink, 1999). To overcome concentration problems some of the relatively short structured interviews, like the Self-Report Standardized *Acknowledgements and Disclosure of Interest: None. #Corresponding author.  S. GERMANS ET AL. Assessment of Personality-Abbreviated Scale (SAPAS-SR) (Germans, Van Heck, Moran, & Hodiamont, 2008), and the self-report version of the Iowa Personality Disorder Screen (IPDS) (Germans, Van Heck, Langbehn, & Hodiamont, 2010), are transformed into short self-report questionnaires. Both ques- tionnaires correctly classify 81% of the patients. Therefore, they are, in spite of limitations, such as the inability to dis- criminate between different PDs, quite useful as quick screens for PDs. All these instruments are based on the Diagnostic and Statis- tical Manual of Mental Disorders (DSM) (American Psychiatric Association, 2000) and the International Classification of Dis- eases and Related Health Problems (ICD) (World Health Or- ganization, 1992). Consequently, they reflect the categorical approach. The criteria for diagnosing PD in DSM-5 and ICD-11, however, will almost certainly change dramatically (DSM-5, 2010). Besides the categorical approach, a dimensional com- ponent will be introduced. In view of the hypothesis that PDs are sharing the same dimensions as normal personality, just with extreme “values”, it follows that one might identify PD using assessment instruments for basic personality dimensions. One of the best known models for defining personality, using a dimensional approach, is the Big Five model (e.g. Costa & McCrae, 1992; Goldberg, 1990). This model is a general com- prehensive framework for structuring individual differences. The five dimensions, which are seen as pervasive across cul- tures, reflect sociability (Extraversion), interpersonal interac- tion (Agreeableness), self-discipline and impulse control (Con- scientiousness, describing task- and goal-directed behavior), personal adjustment (Neuroticism, contrasting emotional stabil- ity with anxiety, anger, and other negative feelings), and open- ness to new experiences (Openness, reflecting the breadth, depth, and complexity of mental and experiential life). Costa and McCrea (1990) have suggested that the five-factor model of personality is highly relevant to the conceptualization and assessment of PDs. They have proposed to let the Big-Five model replace the categorical system for identifying PD in DSM-IV, because, in their view, the broad five supertrait di- mensions offer adequate information to identify PDs that are traditionally diagnosed by categorical means. Several authors support these claims (Wiggins & Pincus, 1989; Costa & Mc Crae, 1992). Widiger, Costa, & McCrae (2002) have de- scribed how PD can be understood in terms of the Big-Five dimensions. They also present a four-step process that shows how the 12 PDs of the DSM-IV could be diagnosed using the five-factor model. The first step consists of formulating patterns of Big Five extremes that correspond to particular PDs. This should be based on a thorough understanding and a systematic conceptualization of how the five factors are defined in terms of content. Good examples of this first step can be found in the NEO-PI-R, which includes additional facet scores for each domain (Costa & McCrae, 1992), and in the review of Digman (1990). Costa and McCrae (1990) give an excellent overview of each domain along with their characteristic trait-descriptive terms (adjectives) and corresponding facet scores as used in the NEO-PI-R. The facet scores combined with the descriptions of the domains give a good idea not only of all what is encom- passed by a certain domain, but also which PD should correlate substantially with extremely high or low scores on these do- mains. To present an overview of the 12 PDs in DSM-IV and their corresponding five-factor profiles for quick and easy use in a clinical setting, a reference sheet was compiled on the basis of the information gathered by Rottman, Ahn, Sanislow, and Kim (2009) and Shedler and Westen (2004), taking into account the correlations computed by Trull (1992) between NEO-PI scores and scores on the PDQ-R, a scale with high sensitivity and moderate specificity for most axis-II disorders (Hyler, Skodol, Oldham, Kellman, & Doidge, 1992), and the MMPI-Personality Disorder scales (Morey, Waugh, & Blashfield, 1985), as well as the meta-analytic study of Samuel and Widiger (2008) (See Table 1). The Revised NEO Personality Inventory (NEO-PI-R) (Costa & McCrea, 1992) contains 240 items and takes approximately 40 minutes to complete. The NEO-FFI (Dutch version by Hoekstra, Ormel, & De Fruyt, 2003) is grounded on the same theoretical foundations as the NEO-PI-R but has only 60 items. Because it has less items the latter scale provides more general information at the domain level, not at the level of more spe- cific facets. Taking into account that the NEO-PI-R is con- ceived of as a potential framework to assess PD, the NEO-FFI might be a screener for PD. The research hypothesis and focus of this article is that ex- treme scores on the NEO-FFI, alone or in combination with a categorical screening instrument like the SAPAS-SR, is a good screener in an outpatient psychiatric population. Table 1. Five-factor model profiles and DSM-IV personality disorders. DSM-IV Personality disorder N E O A C Paranoid H L Schizotypal H L L Schizoid L Histrionic H Narcissistic L Borderline H L L Antisocial L L Avoidant H L Dependent H Obs.-Comp. H Passive-Agrr. H L L Depressive H L Note: H = extreme score in the direction of the given Big Five dimension, L = extreme score opposite to the direction of the given Big Five dimension. N: Neuroticism; E:Extraversion; O: Openness ; A: Agreeableness; C: Conscientiousness. Copyright © 2013 SciRes. 112  S. GERMANS ET AL. Methods Study Sampl e The subjects for the present study were all patients referred to GGZ Midden-Brabant, a Community Mental Health Centre in Tilburg, The Netherlands. The study was approved by the Regional Medical Ethical Committee. From a total of 2116 patients that were referred to this institute between March 2004 and March 2005, 207 patients were recruited at random. The process of randomization contained one daily blind draw out of the full set of referrals. This was executed by the secretary of the intake desk. After drawing, inclusion and exclusion criteria were checked and in case of eligibility the invitation letter was sent. In case of non-eligibility, there was no second draw that day. The criteria for recruitment were: Dutch origin and being non-illiterate. All recruited patients gave informed consent prior to participation. From the 207 patients recruited, 12 patients had to be excluded because they did not, after the first session, complete subsequent assessments, resulting in a study sample of 195 patients. Hundred-and-twelve individuals were female (57.4%), while 83 were male (42.6%). The mean age in the total group was 32.7 years (SD = 8.9). The primary reasons for psychiatric referral were: anxiety problems (n = 62; 31.8%), affective problems (n = 29; 14.9%), conduct disorders (n = 33; 16.9%), partner-relational problems (n = 23; 11.8%), somatic problems (n = 12; 6.2%), labour or school problems (n = 10; 5.1%), identity problems (n = 7; 3.6%), social problems (n = 4; 2.1%), addiction problems (n = 1; .5%), and cognitive problems (n = 2; 1.0%). No specific psychiatric problem was mentioned by the referring physician in the case of five patients (2.5%). Measures The NEO Five-Factor Inventory (NEO-FFI) Because of its brevity, comprehensiveness, and ease of ad- ministration, the 60-item NEO Five-Factor Inventory (NEO-FFI) was employed. In contrast to its “big brother”, the NEO-PI-R, calculation of facet scores is not possible. Subsequently, the focus lies on the broad domains: Extraversion, Agreeableness, Conscientiousness, Neuroticism, and Openness. Each of these five domains is represented by 12 items that must be scored on 5-point Likert scales. Consequently, scores range from 12 to 60. The NEO-FFI has good psychometric properties (Costa & McCrae, 1992). Since the present study compares the dimensional five-factor model of personality, used in the NEO-FFI, with the categorical approach of identifying PD, as used in the DSM-IV, scores on the Big Five were transformed into dichotomous scores reflect- ing extreme scoring. As threshold levels the upper and lower bound 10% of all observed scores within the dataset were used [1 = score in the lowest (0% - 10%) or highest (90% - 100%) decile; 0 = score in the deciles in between]. This method not only yielded a categorical score for each Big Five domain, but also a total score for extremity of rating made up of the number of Big Five domains with a score in the lowest (0% - 10%) or highest (90% - 100%) decile. The Structured Clinical Interview for DSM-IV-TR Personality Disorders (SCID-II) The SCID-II (First, Spitzer, Gibbon, & Williams, 1995) (Dutch version by Weertman, Arntz, & Kerkhof, 1997) is a semi- structured interview for diagnosing DSM-IV personality disor- ders. Translated into many different languages and used in clinical as well as research settings all over the world, it was chosen as the gold standard in the present study. The SCID-II consists of two parts. The first part contains eight open ques- tions which address broad general behavior interpersonal rela- tionships, and introspective ability of the patient. The second part holds 140 items divided into 12 sections, according to the PDs listed in the DSM-IV including the Depressive Personality Disorder and the Passive-Aggressive Personality Disorder (American Psychiatric Association, 2000). The content of each question bears a strong resemblance to every criterion as it is listed as typical and/or necessary for a specific PD within the DSM-IV. Items are scored as follows: ? (inadequate), 1 (absent), 2 (sub-threshold), or 3 (threshold). Interviewers need prior for- mal training in using the SCID-II and a quite profound knowl- edge of psychopathology as a whole, since clinical judgment plays an essential role in translating the wide range of possible patient reactions to each question into one of the response choices. The SCID-II is primarily designed to make a categori- cal diagnosis of PD. The interrater reliability and internal con- sistency of the SCID-II are adequate (Maffei, Fossati, Agostini, Barraco, Bagnato, Deborah et al., 1997; Westen & Shelder, 1999; Westen & Shelden 1999). The interrater reliability of the most recent Dutch version for the presence or absence of any PD is fair to good (Weertman, Arntz, Dreessen, Velzen, & Vertommen, 2003). Before undertaking fieldwork for the pre- sent study, the first author (S.G.) was formally trained in the use of the SCID-II. The Self Report Standardized Assessment of Personality-Abbreviated Scale (SAPAS-SR) The authors translated the items of the original SAPAS (Moran, Leese, Lee, Walters, Thornicroft, & Mann, 2003) and created a self-report questionnaire, the SAPAS-SR (Germans, Van Heck, Moran, & Hodiamont, 2010). The SAPAS was origi- nally developed by Moran et al. (2003) as a structured inter- view with eight dichotomous items. The original instrument was validated in a sample of clinical and polyclinical patients. The alpha coefficient for the total score of the SAPAS was .68. A cut-off score of 3 correctly classified over 80% of the pa- tients with a sensitivity of .94 and a specificity of .85 (Moran, Leese, Lee, Walters, Thornicroft, & Mann, 2003). The 8-item SAPAS-SR is an instrument that measures three broader do- mains, approximately reflecting the clusters A, B, and C as distinguished in the DSM-IV. Psychometric properties were studied, showing a test-retest coefficient of .89 for the total score. Factor analysis revealed that the three domains ac- counted for 53.8% of the total variance. When using a cut-off score of 4, the SAPAS-SR correctly classified 81% of the pa- tients, while showing a sensitivity of .83 and a specificity of .80, which is only slightly lower than the results obtained with the original English interview version (Germans, Van Heck, Moran, & Hodiamont, 2010). Procedure The NEO-FFI and the SAPAS-SR were completed during the initial clinical appointment. The SCID-II interview took place one week after the initial clinical appointment. The first author (S.G.) was blind for the NEO-FFI and SAPAS-SR re- sults prior to the SCID-II interview session. Copyright © 2013 SciRes. 113  S. GERMANS ET AL. Statistical Analyses All statistical analyses were performed using the SPSS 17 for Windows package. First, all personality domain scores were transformed into dichotomous scores (extremity of rating ver- sus no extremity of rating) that contrasted the top 10% and the bottom 10% scores, on the one hand, with the scores reflecting the less extreme range (11% - 89%), on the other hand. Then, scores on a new variable, Extremity of Rating (EoR0vs12345), were calculated: 0 (no extremity of rating on any of the five basic personality domains) versus 1 (extremity of rating on one or more traits). Subsequently, another dichotomous variable was created, reflecting the positive (1) or negative (0) outcome of the PD SCID-II diagnosis. Subsequently, Chi-square tests were performed. As a next step in the analysis, a set of new dichotomous variables was calculated, contrasting 1) EoR01vs2345; extrem- ity of rating on 0 traits or 1 trait versus extremity of rating on 2 or more traits; 2) EoR012vs345; extremity of rating on 2 or less than 2 traits versus extremity of rating on 3 or more traits; and 3) EoR0123vs45; extremity of rating on 3 or less than 3 traits versus extremity of rating on 4 or 5 traits. Three Chi-square tests were employed in order to examine whether different lev- els of extremity of rating were linked to caseness (i.e., any PD) in terms of SCID-II diagnosis (yes/no). Thereafter, for each participant the number of five-factor domains with extreme scoring was calculated. No participant had extreme scores on all five basic personality traits. This yielded a range of 1 (no extremity of rating) to 4 (extremity of rating on four traits). Additionally, a Pearson correlation coefficient was calculated to examine a possible relationship between the number of extreme five-factor scores and the number of PDs as diagnosed by the SCID-II interview. Finally, dichotomous variables were created to distinguish participants who did not have a particular profile as described in Table 1 (score = 0) and participants who actually did (score = 1). Again Chi-square analyses were used to test the associations between the 12 dichotomous variables [e.g., Paranoid Big-Five Profile (yes/no), Schizotypal Big-Five profile (yes/no), Schiz- oid Big-Five profile (yes/no), etc.) and the PD diagnoses, ac- cording to the SCID-II. Then, we compared the NEO-FFI with the SAPAS-SR. A dichotomous variable, using the SAPAS-SR cut-off score of 4 (Germans, Van Heck, Moran & Hodiamont, 2008) was compared with (EoR0vs12345). For a final analysis, a variable was examined that combined (EoR0vs12345) with a positive screening result on the SAPAS-SR. This composite score was compared with the SCID-II diagnosis of any PD (yes/no PD). Hereafter, correlation analyses and regression analyses were performed to examine the associations between personality traits and PD. Results According to the SCID-II, at least one PD was present in 97 (50%) of the 195 patients. The mean number of PDs in patients diagnosed with any PD was 1.8 (SD = .87). The overall total number of SCID-II diagnoses was 172. The highest scoring personality factors of the study sample were Neuroticism and Agreeableness and the lowest scoring was Extraversion (see Table 2). A Chi-square test, examining the relation between Extremity of Rating on one or more basic personality traits, on the one hand, (yes/no) and a PD diagnosis, according to the SCID-II (yes/no), on the other hand, revealed no significant relationship (χ2(1, N = 195) = .072, p = .79). Among all 195 participants, there were 70 patients (35.9%) that showed no extreme score on any of the five-factor domains. Seventy-eight patients (40%) showed an extreme score on one of the domains, 31 (15.9%) on two domains, 14 (7.2%) on three domains, and two patients (1%) on four domains. Chi-square analyses, scrutinizing the relationships between the dichoto- mous variables EoR01vs2345, EoR012vs345, and EoR0123vs45 and caseness, according to SCID-II, did not result in significant associations (χ2(1, N = 195) = .942, p = .33; χ2(1, N = 195) = .172, p = .68; χ2(1, N = 195) = .001, p = .97). The correlation between the number of five-factor extremes and the number of PDs, identified with the use of SCID-II was non-significant and very weak, r = −.05, p = .47. For all participants with a specific PD, according to the SCID-II interview, it was examined whether or not they had the specific NEO-FFI profile as specified in Table 1. For instance, it was found that none of the 44 patients with a Borderline PD scored on the NEO-FFI the specific profile for Borderline syn- drome (high on Neuroticism, low on Agreeableness and Con- scientiousness) (see Table 3). In addition, values for sensitivity, specificity, and correctly classified cases were calculated. Table 4 gives an overview. Twelve Chi-square tests comparing SCID-II diagnoses with the presence or absence of a particular Big-Five profile were performed. The majority of these analyses failed to find sig- nificant associations. Exceptions were the analyses for the schizotypal PD profile, c2(1, N = 195) = 96.99, p < .001, and the schizoid PD profile, c2(1, N = 195) = 12.06, p = .001. The Chi-square test comparing the presence or absence of Extremity of Rating on at least one five-factor domain, on the one hand, with a positive or negative screening result on the SAPAS-SR, on the other hand, did not provide empirical sup- port for a significant relationship (χ2(1, N = 195) = .072, p = .79. A final analysis, combining SAPAS-SR and Big-Five profile information, both resulted in a significant relation between this composed score and the gold standard: c2(1, N = 195) = 34.52, Table 2. Dimensional scores for the five NEO-FFI personality factors. Factor Minimum score Maximum score Median Mean SD Neuroticism 16 58 45.0 43.7 8.3 Extraversion 16 57 35.0 35.1 8.2 Openness 22 54 36.0 36.7 6.7 Agreeableness 26 58 42.0 41.3 5.9 Conscientiousness 22 53 39.5 38.8 6.3 Copyright © 2013 SciRes. 114 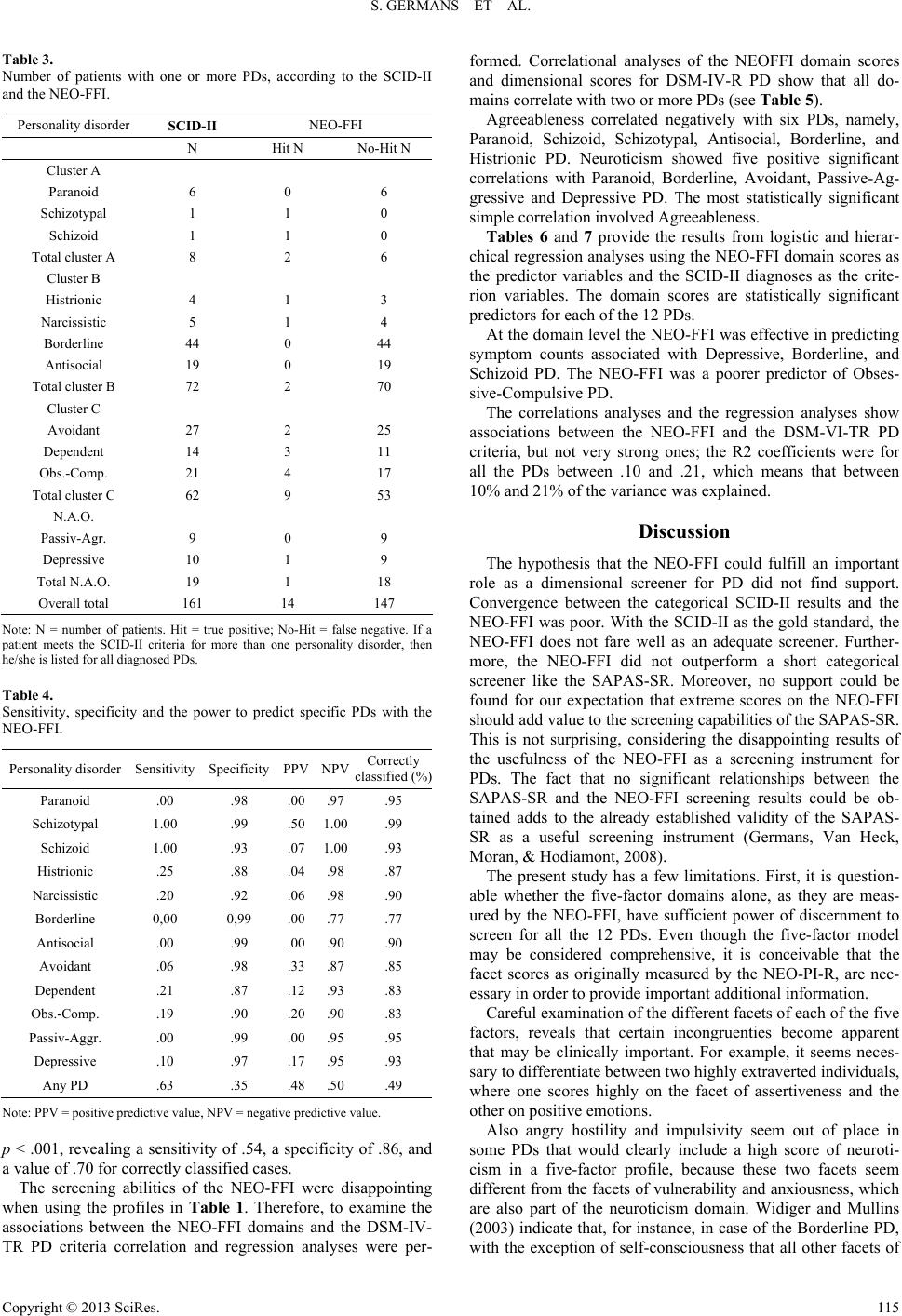 S. GERMANS ET AL. Table 3. Number of patients with one or more PDs, according to the SCID-II and the NEO-FFI. Personality disorder SCID-II NEO-FFI N Hit N No-Hit N Cluster A Paranoid 6 0 6 Schizotypal 1 1 0 Schizoid 1 1 0 Total cluster A 8 2 6 Cluster B Histrionic 4 1 3 Narcissistic 5 1 4 Borderline 44 0 44 Antisocial 19 0 19 Total cluster B 72 2 70 Cluster C Avoidant 27 2 25 Dependent 14 3 11 Obs.-Comp. 21 4 17 Total cluster C 62 9 53 N.A.O. Passiv-Agr. 9 0 9 Depressive 10 1 9 Total N.A.O. 19 1 18 Overall total 161 14 147 Note: N = number of patients. Hit = true positive; No-Hit = false negative. If a patient meets the SCID-II criteria for more than one personality disorder, then he/she is listed for all diagnosed PDs. Table 4. Sensitivity, specificity and the power to predict specific PDs with the NEO-FFI. Personality disorder Sensitivity Specificity PPV NPV Correctly classified (%) Paranoid .00 .98 .00 .97 .95 Schizotypal 1.00 .99 .50 1.00 .99 Schizoid 1.00 .93 .07 1.00 .93 Histrionic .25 .88 .04 .98 .87 Narcissistic .20 .92 .06 .98 .90 Borderline 0,00 0,99 .00 .77 .77 Antisocial .00 .99 .00 .90 .90 Avoidant .06 .98 .33 .87 .85 Dependent .21 .87 .12 .93 .83 Obs.-Comp. .19 .90 .20 .90 .83 Passiv-Aggr. .00 .99 .00 .95 .95 Depressive .10 .97 .17 .95 .93 Any PD .63 .35 .48 .50 .49 Note: PPV = positive predictive value, NPV = negative predictive value. p < .001, revealing a sensitivity of .54, a specificity of .86, and a value of .70 for correctly classified cases. The screening abilities of the NEO-FFI were disappointing when using the profiles in Table 1. Therefore, to examine the associations between the NEO-FFI domains and the DSM-IV- TR PD criteria correlation and regression analyses were per- formed. Correlational analyses of the NEOFFI domain scores and dimensional scores for DSM-IV-R PD show that all do- mains correlate with two or more PDs (see Table 5). Agreeableness correlated negatively with six PDs, namely, Paranoid, Schizoid, Schizotypal, Antisocial, Borderline, and Histrionic PD. Neuroticism showed five positive significant correlations with Paranoid, Borderline, Avoidant, Passive-Ag- gressive and Depressive PD. The most statistically significant simple correlation involved Agreeableness. Tables 6 and 7 provide the results from logistic and hierar- chical regression analyses using the NEO-FFI domain scores as the predictor variables and the SCID-II diagnoses as the crite- rion variables. The domain scores are statistically significant predictors for each of the 12 PDs. At the domain level the NEO-FFI was effective in predicting symptom counts associated with Depressive, Borderline, and Schizoid PD. The NEO-FFI was a poorer predictor of Obses- sive-Compulsive PD. The correlations analyses and the regression analyses show associations between the NEO-FFI and the DSM-VI-TR PD criteria, but not very strong ones; the R2 coefficients were for all the PDs between .10 and .21, which means that between 10% and 21% of the variance was explained. Discussion The hypothesis that the NEO-FFI could fulfill an important role as a dimensional screener for PD did not find support. Convergence between the categorical SCID-II results and the NEO-FFI was poor. With the SCID-II as the gold standard, the NEO-FFI does not fare well as an adequate screener. Further- more, the NEO-FFI did not outperform a short categorical screener like the SAPAS-SR. Moreover, no support could be found for our expectation that extreme scores on the NEO-FFI should add value to the screening capabilities of the SAPAS-SR. This is not surprising, considering the disappointing results of the usefulness of the NEO-FFI as a screening instrument for PDs. The fact that no significant relationships between the SAPAS-SR and the NEO-FFI screening results could be ob- tained adds to the already established validity of the SAPAS- SR as a useful screening instrument (Germans, Van Heck, Moran, & Hodiamont, 2008). The present study has a few limitations. First, it is question- able whether the five-factor domains alone, as they are meas- ured by the NEO-FFI, have sufficient power of discernment to screen for all the 12 PDs. Even though the five-factor model may be considered comprehensive, it is conceivable that the facet scores as originally measured by the NEO-PI-R, are nec- essary in order to provide important additional information. Careful examination of the different facets of each of the five factors, reveals that certain incongruenties become apparent that may be clinically important. For example, it seems neces- sary to differentiate between two highly extraverted individuals, where one scores highly on the facet of assertiveness and the other on positive emotions. Also angry hostility and impulsivity seem out of place in some PDs that would clearly include a high score of neuroti- cism in a five-factor profile, because these two facets seem different from the facets of vulnerability and anxiousness, which are also part of the neuroticism domain. Widiger and Mullins (2003) indicate that, for instance, in case of the Borderline PD, with the exception of self-consciousness that all other facets of Copyright © 2013 SciRes. 115 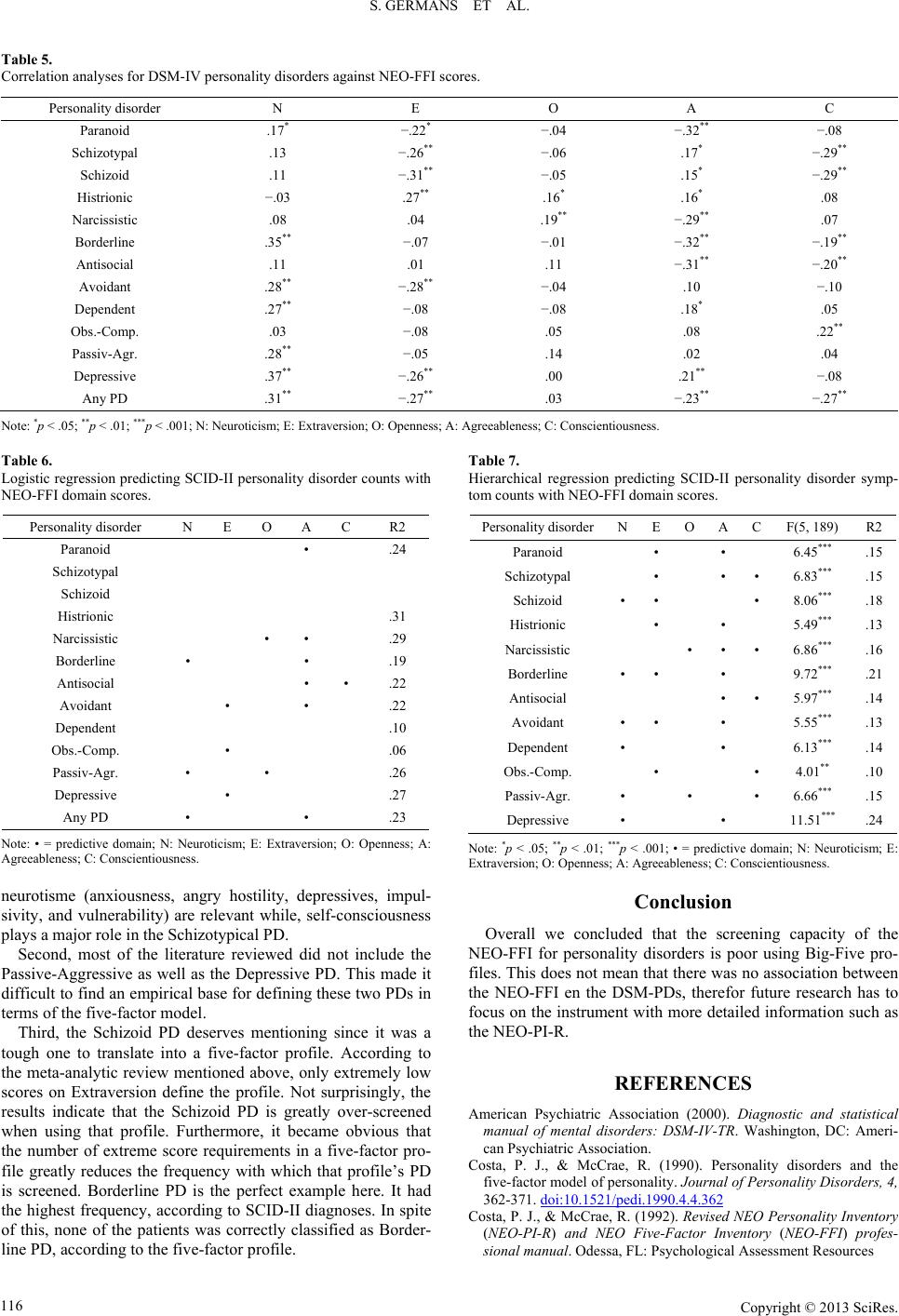 S. GERMANS ET AL. Table 5. Correlation analyses for DSM-IV personality disorders against NEO-FFI scores. Personality disorder N E O A C Paranoid .17* −.22* −.04 −.32** −.08 Schizotypal .13 −.26** −.06 .17* −.29** Schizoid .11 −.31** −.05 .15* −.29** Histrionic −.03 .27** .16* .16* .08 Narcissistic .08 .04 .19** −.29** .07 Borderline .35** −.07 −.01 −.32** −.19** Antisocial .11 .01 .11 −.31** −.20** Avoidant .28** −.28** −.04 .10 −.10 Dependent .27** −.08 −.08 .18* .05 Obs.-Comp. .03 −.08 .05 .08 .22** Passiv-Agr. .28** −.05 .14 .02 .04 Depressive .37** −.26** .00 .21** −.08 Any PD .31** −.27** .03 −.23** −.27** Note: *p < .05; **p < .01; ***p < .001; N: Neuroticism; E: Extraversion; O: Openness; A: Agreeableness; C: Conscientiousness. Table 6. Logistic regression predicting SCID-II personality disorder counts with NEO-FFI domain scores. Personality disorder N E O A C R2 Paranoid • .24 Schizotypal Schizoid Histrionic .31 Narcissistic • • .29 Borderline • • .19 Antisocial • • .22 Avoidant • • .22 Dependent .10 Obs.-Comp. • .06 Passiv-Agr. • • .26 Depressive • .27 Any PD • • .23 Note: • = predictive domain; N: Neuroticism; E: Extraversion; O: Openness; A: Agreeableness; C: Conscientiousn ess . neurotisme (anxiousness, angry hostility, depressives, impul- sivity, and vulnerability) are relevant while, self-consciousness plays a major role in the Schizotypical PD. Second, most of the literature reviewed did not include the Passive-Aggressive as well as the Depressive PD. This made it difficult to find an empirical base for defining these two PDs in terms of the five-factor model. Third, the Schizoid PD deserves mentioning since it was a tough one to translate into a five-factor profile. According to the meta-analytic review mentioned above, only extremely low scores on Extraversion define the profile. Not surprisingly, the results indicate that the Schizoid PD is greatly over-screened when using that profile. Furthermore, it became obvious that the number of extreme score requirements in a five-factor pro- file greatly reduces the frequency with which that profile’s PD is screened. Borderline PD is the perfect example here. It had the highest frequency, according to SCID-II diagnoses. In spite of this, none of the patients was correctly classified as Border- line PD, according to the five-factor profile. Table 7. Hierarchical regression predicting SCID-II personality disorder symp- tom counts with NEO-FFI domain scores. Personality disorderNEO A C F(5, 189)R2 Paranoid • • 6.45*** .15 Schizotypal • • • 6.83*** .15 Schizoid • • • 8.06*** .18 Histrionic • • 5.49*** .13 Narcissistic • • • 6.86*** .16 Borderline • • • 9.72*** .21 Antisocial • • 5.97*** .14 Avoidant • • • 5.55*** .13 Dependent • • 6.13*** .14 Obs.-Comp. • • 4.01** .10 Passiv-Agr. • • • 6.66*** .15 Depressive • • 11.51*** .24 Note: *p < .05; **p < .01; ***p < .001; • = predictive domain; N: Neuroticism; E: Extraversion; O: Openness; A: Agreeableness; C: Conscientiousness. Conclusion Overall we concluded that the screening capacity of the NEO-FFI for personality disorders is poor using Big-Five pro- files. This does not mean that there was no association between the NEO-FFI en the DSM-PDs, therefor future research has to focus on the instrument with more detailed information such as the NEO-PI-R. REFERENCES American Psychiatric Association (2000). Diagnostic and statistical manual of mental disorders: DSM-IV-TR. Washington, DC: Ameri- can Psychiatric Association. Costa, P. J., & McCrae, R. (1990). Personality disorders and the five-factor model of personality. Journal of Personality Disorders, 4, 362-371. doi:10.1521/pedi.1990.4.4.362 Costa, P. J., & McCrae, R. (1992). Revised NEO Personality Inventory (NEO-PI-R) and NEO Five-Factor Inventory (NEO-FFI) profes- sional manual. Odessa, FL: Psychological Assessment Resources Copyright © 2013 SciRes. 116  S. GERMANS ET AL. Costa, P. J., & McCrae, R. (1992).The five-factor model of personality and its relevance to personality disorders. Journal of Personality Disorders, 4, 343-359. doi:10.1521/pedi.1992.6.4.343 Digman, J. (1990). Personality structure: Emergence of the five-factor model. Annual Review of Psychology, 41, 417-440. doi:10.1146/annurev.ps.41.020190.002221 DSM-5 Work Group (1990). Re: Personality and personality disorders. URL (last checked 12 December 2012). http://www.dsm5.org/Pages/Default.aspx First, M., Spitzer, R., Gibbon, M., & Williams, J. (1995). The struc- tured clinical interview for DSM-III-R personality disorders (SCID- II): Part I: Description. Journal of Personality Disorders, 9, 92-104. doi:10.1521/pedi.1995.9.2.92 Germans, S., Van Heck, G. L., & Hodiamont, P. P. G. (2011). The Quick Personality Assessment Schedule (PAS-Q): Validation of a brief screening test for personality disorders in a population of psy- chiatric outpatients. Australian and New Zealand Journal of Psy- chiatry, 45, 756-762. doi:10.3109/00048674.2011.595683 Germans, S., Van Heck, G. L., Langbehn, D. R., & Hodiamont P. P. G. (2010). The Iowa Personality Disorder Screen (IPDS): Preliminary results of the validation of a self-administered version in a Dutch population. European Journal of Psychological Assessment, 26, 11- 18. doi:10.1027/1015-5759/a000003 Germans, S., Van Heck, G. L., Moran. P., & Hodiamont, P. P. G. (2008). The self-report Standardized Assessment of Personality-Ab- breviated Scale; Preliminary results of a brief screening test for per- sonality disorders. Personality and Mental Health, 2, 70-76. doi:10.1002/pmh.34 Goldberg, L. R. (1990). An alternative “description of personality”: The big-five factor structure. Journal of Personality and Social Psychol- ogy, 59, 1216-1229. doi:10.1037/0022-3514.59.6.1216 Hoekstra, H. A., Ormel, J., De Fruyt, F. (1996). NEO-FFI big five per- soonlijkheidsvragenlijst (NEO-FFI big five personality question- naire). Lisse: Swets & Zeitlinger B.V. Hyler, S. E., Skodol, A. E., Kellman, H., Oldham, J. M., & Rosnick, L. (1990). Validity of the Personality Diagnostic Questionaire-Revised: Comparison with two structured interviews. American Journal of Psychiatry, 147, 1043-1048. Hyler, S., Skodol, A., Oldham, J. M., Kellman, H. D., & Doidge, N. (1992). Validity of the Personality Diagnostic Questionnaire-Revised: A replication in an outpatient sample. Comprehensive Psychiatry, 33, 73-77. doi:10.1016/0010-440X(92)90001-7 Langbehn, D. R., Pfohl, B. M., Reynolds, S., Clark, L. A., Battaglia, M., Bellodi, L., Cadoret, R., Grove, W., Pilkonis, P., & Links, P. (1999). The Iowa Personality Disorder Screen: Development and preliminary validation of a brief screening interview. Journal of Personality Dis- orders, 13, 75-89. doi:10.1521/pedi.1999.13.1.75 Maffei, C., Fossati, A., Agostoni, I., Barraco, A., Bagnato, M., Deborah D. et al. (1997). Interrater reliability and internal consistency of the structured clinical interview for DSM IV axis II personality disorder (SCID II) version 2.0. Journal of Personality Disorders, 11, 85-92. doi:10.1521/pedi.1997.11.3.279 Moran, P., Leese, M., Lee, T., Walter, P., Thornicroft, G., & Mann, A. (2003). Standardised Assessment of Personality-Abbreviated Scale (SAPAS): Preliminary validation of a brief screen for personality disorder. British Journal of Psychiatry, 183, 228-232. doi:10.1192/bjp.183.3.228 Moran, P., Walsh, E., Tyrer, P., Burns, T., Creed, F., & Fahy, T. (2003). The impact of co-morbid personality disorder on violence in psycho- sis—Data from the UK700 trial. British Journal of Psychiatry, 182, 129-134. doi:10.1192/bjp.182.2.129 Morey, L. C., Waugh, M. H., & Blashfield, R. K. (1985). MMPI scales for DSM-III personality disorders: Their derivation and correlates. Journal of Personality Assessment, 49, 245-251. doi:10.1207/s15327752jpa4903_5 Newton-Howes, G., Tyrer, P., & Johnson, T. (2006). Personality disor- der and the outcome of depression: Meta-analysis of published stud- ies. British Journal of Psychiatry, 188, 13-20. doi:10.1192/bjp.188.1.13 Reich, J. (1989). Update on instruments to measure DSM-III and DSM-III-R personality disorders. Journal of Nervous and Mental Disease, 177, 366-370. doi:10.1097/00005053-198906000-00008 Rottman, B., Ahn, W., Sanislow, C., & Kim, N. (2009). Can clinicians recognize DSM-IV personality disorders from five-factor model de- scriptions of patient cases? American Journalof Psychiatry, 166, 427-433. doi:10.1176/appi.ajp.2008.08070972 Samuel, D., & Widiger, T. (2008). A meta-analytic review of the rela- tionships between the five-factor model and DSM-IV-TR personality disorders: A facet level analysis. Clinical Psychological, 28, 1326- 1342. doi:10.1016/j.cpr.2008.07.002 Schotte, C., De Doncker, D., Vankerckhoven, C., Vertommen, H., & Cosyns, P. (1998). Self-report assessment of the DSM-IV personality disorders. Measurement of trait and distress characteristics: The ADP-IV. Psychological Medicine, 28, 1179-1188. doi:10.1017/S0033291798007041 Shedler, J., & Westen, D. (2004). Refining personality disorder diagno- sis: Integrating science and practice. American Journal of Psychiatry, 161, 1350-1365. doi:10.1176/appi.ajp.161.8.1350 Spitzer, R., Williams, J., Gibbon, M., & First, M. (1990). Structured clinical interview for the DSM-III-R personality disorders (SCID-II). Washington, DC: American Psychiatric Press. Trull, T. (1992). DSM-III-R Personality disorders and the five-factor model of personality: An empirical comparison. Journal of Abnormal Psychology, 101, 553-560. doi:10.1037/0021-843X.101.3.553 Van Horn, E., Manley, C., Leddy, D., Cicchetti, D., & Tyrer, P. (2000). Problems in developing an instrument for the rapid assessment of personality status. European Psychiatry, 15, 29-33. doi:10.1016/S0924-9338(00)90497-8 Verheul, R., & Van den Brink, W. (1999) Persoonlijkheidsstoornissen (Personality disorders). In A. De Jong, W. Van den Brink, J. Ormel, & D. Wiersma (Eds.), Handboek psychiatrische epidemiologie (Handbook of psychiatric epidemiology) (pp. 355-359) Maarsen: Elsevier/De Tijdstroom. Weertman, A., Arntz, A., Dreessen, L., Van Velzen, C., & Vertommen, S. (2003). Short-interval test-retest interrater reliability of the Dutch version of the Structured Clinical Interview for DSM-IV personality disorders (SCID-II). Journal of Personality Disorders, 17, 562-567. doi:10.1521/pedi.17.6.562.25359 Weertman, A., Arntz, A., & Kerkhofs, M. (1997). Gestructureerd Klinisch Interview voor de DSM-III Persoonlijkheidsstoornissen (Structured clinical interview for the DSM-III personality disor- ders). Lisse: Swets Test Publisher. Westen, D., & Shelder, J. (1999). Revising and assessing Axis II, Part I: Development of a clinically and empirically valid assessment method. American Journal of Psychiatry, 156, 258-272. Westen, D., & Shelder, J. (1999). Revising and assessing Axis II, Part II: Toward an empirically based and clinically useful classification of personality disorders. American Journal of Psychiatry, 156, 273-285. Widiger, T., Costa, P., & McCrae, R. (2002). A proposal for Axis II: Diagnosing personality disorders using the five-factor model. In Personality disorders and the five-factor model of personality (2nd ed., pp. 431-456). Washington, DC: American Psychological Asso- ciation. doi:10.1037/10423-025 Widiger, T. A., & Mullins, S. (2003). Personality disorder. In A. Tas- man, J. Kay, & J. A. Lieberman (Eds.), Psychiatry (2nd ed., pp. 1603-1637). Chichester: John Wiley & Sons. Wiggins, J., & Pincus, A. (1989). Conceptions of personality disorders and dimensions of personality. Psychological Assessment: Journal of Consulting and Clinical Psychology, 1, 305-316. World Health Organization (1992). International classification of dis- eases (10th Revision) Geneva: World Health Organization Copyright © 2013 SciRes. 117
|