Paper Menu >>
Journal Menu >>
 Vol.2, No.8, 878-889 (2010) doi:10.4236/health.2010.28131 Copyright © 2010 SciRes. Openly accessible at http://www.scirp.org/journal/HEALTH/ HEALTH Depression in adult males with lower extremity amputa- tion and its bio-social correlates Arupendra Mozumdar1, Subrata K. Roy2* 1Department of Health, Nutrition and Exercise Sciences, North Dakota State University, Fargo, USA; arupendra.mozumdar@ndsu.edu 2Biological Anthropology Unit, Indian Statistical Institute, Kolkata, India; *Corresponding Author: rsubrata@isical.ac.in Received 23 March 2010; revised 30 April 2010; accepted 2 May 2010. ABSTRACT Depression is often associated with many adverse health conditions and lower socio-economic status. Stressful conditions like presence of disability coupled with traditional negative so- cietal attitude towards disability may result in higher level of depression in the individuals with disability than in general population and can cause other health problems as well. There- fore, the purposes of this study are to explore the association of depression with its biosocial correlates among individuals with lower ex- tremity amputations (LEA) living in Kolkata, In- dia. Eighty-five participants with traumatic LEA and 105 control participants with no amputation participated in this study. The depression levels of the participants were measured with Beck Depression Index (BDI). All participants were also measured with the following sets of health traits, using standard techniques-1) physical: body weight, stature, body mass index (BMI), blood pressure, total cholesterol, triglycerides, blood glucose, hemoglobin%, 2) functional: functional outcome or degree of independence in daily activities, and 3) social: economic con- dition, and social discomfort. No significant difference was found in mean BDI scores for individuals with LEA and control participants. Higher BDI scores were associated with chronic energy deficiency. None of the other physical health traits was associated with depression level. Higher depression was associated with poor socio-economic conditions like low eco- nomic condition, dependency on others for daily activity, occupational constraints due to disabil- ity and perceived problems in conjugal life. Therefore, economic development with a posi- tive social attitude toward people with disability is essential for the mental wellbeing of the indi- viduals with LEA. Keywords: Depression; Biosocial Health Factors; Lower Extremity Amputation 1. INTRODUCTION Depression is a mental state characterized by feelings of sadness, with downturn mood in despair and discour- agement, loss of interest or pleasure, a pessimistic sense of inadequacy and a despondent lack of activity, feelings of guilt or low self-worth, disturbed sleep or appetite, low energy, and poor concentration [1]. However, de- pression is often considered as a medical disorder, like any other physical disorder, which affects human thoughts, feelings, behaviors and even physical health (e.g. weight loss, loss of appetite, loss of sleep, loss of libido, etc) [2]. Symptoms of depression may be the outcomes of pro- longed exposure to the stressful life conditions. Negative consequences in life (like disease and disability) not only make life stressful, but also adversely affect the adaptive resources (which is very much dependent on the socio-economic condition of a given individual). Lower extremity amputation (LEA) cause serious physical dis- ability and it is intuitive that adjustment to the conditions of amputation is impulsive to psychological distress. Depression in individuals with LEA was well investi- gated and many studies reported the prevalence rate of depression up to 45% among the study samples [2-8]. The individuals with LEA showed relatively higher mortality rates due to cardiovascular diseases than the general population [9-12]. A number of studies investi- gated and inferred a close relationship of depression with high blood pressure [13-15], diabetic condition [16], high cholesterol level [17-21], and obesity [22,23]. From the above-mentioned studies, it may be argued that the individuals with LEA generally suffer from greater car- diovascular risks, and may also suffer from depression, although there is a dearth of empirical study among the individuals with LEA in this regard.  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 879 879 Several studies revealed that major depressive disor- ders and greater depressive symptomatology were more prevalent at lower levels of socioeconomic status [24, 25]. However, income levels of people with an amputa- tion were not related to depressive symptoms [26]. A number of studies showed that people generally avoid interaction or are likely to terminate an interaction sooner with a person who has visually detectable dis- ability, when a socially acceptable excuse is available [27,28]. People with an amputation also reported the same experiences. Therefore, the individuals with LEA have to adjust to the reality that they appear ‘different’ from other people [29]. The social problem often en- hances due to movement restriction, coupled with poor health, which in turn often limits opportunities for social participation such as regular walking outside, keeping contact with loved ones and acquaintances, and in- volvement in social ceremonies [30]. The findings of earlier studies regarding the impact of an amputation on social functioning were mixed. Some studies reported no significant difference in social functioning or levels of social discomfort between those with and without am- putations [31-34]. Contrary to these finding, several quantitative studies demonstrated the association of in- creased social isolation and lower levels of perceived social support with lower perceived quality of life and higher levels of depressive symptomatology among peo- ple with amputation [5-7,35]. Amputation level appears to be an important factor predicting successful rehabilitation [36]. Williamson [37], and Williamson and Walters [38] reported the dif- ference in the levels of activity among individuals with different levels of LEA. Many authors studied the rela- tionship of levels of amputation and the mental health of the individuals with LEA [26,35,39-41]. Gerhards et al. [42], and Cansever et al. [43] indicated association of depression with the cause of the amputation. Horgan and MacLachlan [44] studied the relationship of depression of the individuals with LEA with their functional out- come as well as their duration of disability. The mental health of the individuals with a physical disability is often influenced by the attitude of the soci- ety towards physical disability. The attitude of the soci- ety towards people with disability is different in tradi- tional society from the modern Western world, where the attitude mostly changed after World War II. The welfare efforts for people with a disability were changed from providing the life sustenance, towards improving all- round social well-being, considering people with dis- abilities as productive members of the society. In the developing world, particularly in traditional societies, attitudes are changing at a much slower pace [45]. In India, traditionally the rehabilitation of people with a disability was considered to be a responsibility of the family and local communities. The1980s changed the scenario significantly. As a signatory to the World Pro- gramme of Action Concerning Disabled Persons, India had also developed the Persons with Disabilities Act 1995 [46]. The objectives of the act are directed towards creating a barrier-free environment for people with a disability; and towards their self-reliance and socio- economic development. Along with other efforts, a per- centage of public sector job are also reserved for the persons with a physical disability. However, still the Indian society is in a crossroad between the positive and negative attitude towards physical disability. This paves a unique consequence for the mental and social health status of the people with a disability, certainly different from that of modern Western society. In view of these, the objectives of the present study are the following in the individuals with lower extremity amputation (LEA) from Kolkata, India-1) Can the condition of locomotor disability enhances depression? 2) What is the relationship of depression with selected health traits? 3) What is the relationship of socio- eco- nomic condition with depression? and 4) Is there any relationship of disability related factors (e.g. duration of disability, level of disability, and use of prosthesis, etc.) with depression? 2. MATERIALS AND METHODS 2.1. Population and Sample The data were collected as a part of a larger bio-medical program involving individuals with a lower extremity amputation from Kolkata and its adjoining areas. Two national level rehabilitation centers, the National Insti- tute for the Orthopedically Handicapped and Mahavir Seva Sadan were contacted for a list of addresses of the individuals with an amputation. A statement of purpose of the study and a consent form seeking their participa- tion were mailed to about 1000 adult male individuals with unilateral LEA. It is well documented that the pre- valence rate of locomotor disability in adult males is higher than females in India [47], which was one of the reasons for considering only males as participants. Re- spondents (109 individuals), with written consent, were included in the study. Although the response rate was very low, it was the most convenient way to recruit the samples, as maintenance of hospital records was very poor and absence of any data-bank for people with dis- ability. Due to death or severe illness or migration, there were few dropouts during data collection, leaving 102 individuals with LEA. Most of the study participants experienced traumatic amputation (82.6%). Degenera- tive diseases like diabetes (11.0%) and cancer (6.4%)  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 880 were the other two common causes for amputation. For this study only the individuals with traumatic amputation (n = 85) was considered, because the depression level of individuals with LEA due to diabetes or cancer may not have a similar level of depression from that of an indi- viduals with a traumatic amputation. Out of 85 individuals with traumatic amputation, 27 individuals had above-knee amputation and 58 individu- als had below-knee amputation. The mean age of the study participants (individuals with traumatic LEA) was 42.58 ± 14.81 years. All participants had prosthesis and all of them had been amputated at least approximately 2 years prior to the study. As there is a lack of any estab- lished population norm for depression level in the study population, a number of 105 non amputated healthy males, matched for age and socio-economic status (mostly from among the close-kins of the individuals with LEA) were studied as control group. All the study participants i.e. individuals with limb amputation and all the control group participants, were Bengali-speaking Hindus. All data were collected by a single investigator (AM) through multiple home visits. The study was done in accordance with the responsible committee on human experimenta- tion (Scientific Ethical committee for Protection of Re- search Risks to Humans) at the Indian Statistical Insti- tute, Kolkata. 2.2. Data Types 2.2.1. Measurement of Depression All participants were screened for the presence of de- pression using the Beck Depression Inventory-II (BDI) [48]. The BDI is one of the most commonly used meas- ure of depression, and its reliability and validity has been assessed in a variety of study populations [48] including individuals with disability [49-52]. The Beck Depression Inventory is a self-report questionnaire consisting of 21- items/ questions. Each question has a set of at least four answer choices, ranging in intensity. For example, the item concerning mood had five answers: (0) I do not feel sad. (1) I feel sad. (2a) I am blue or sad all the time and I can’t snap out of it. (2b) I am so sad or unhappy that it is very painful. (3) I am so sad or unhappy that I can't stand it. While completing the BDI, for each item the partici- pants were asked to select at least one answer from the list of given answers. Upon completion of the answering all items, a value of 0 to 3 was assigned for each answer and the scores of all 21 answers were summed up. Therefore, every individual had a theoretical possibility of scoring 0 to 63. If a participant selected more than one answer for any item, then the highest scoring answer was considered. As the participants of this study were from a non-English speaking population, a translated and well- tested Bengali version of the BDI scale was used [53]. Regarding the BDI test scores and interpretation, the following scores and interpretive labels were used to characterize scores on the BDI-II as: 0-13 (minimal), 14 -19 (mild), 20-28 (moderate), and 29-63 (severe) as suggested by Beck et al. [48]. Since there is no cut-off value specifically for the study population the cut-off values proposed by Beck et al. [48] was used. 2.2.2. Measurement of Physical Health Traits The traits considered in the present study for biological response of the depression were systolic and diastolic blood pressure, hemoglobin %, blood glucose, total cho- lesterol, triglycerides and body mass index. Data on all the measurements were collected following standard techniques as recommended by the International Bio- logical Program (IBP) [54]. Body weight of the indi- viduals with an amputation was calculated using the formulae of Mozumdar and Roy [55]. Body mass index was calculated using the formula bodyweight (Kg)/ height (M)2. Waist circumference measurement was taken at the iliac crest level. Blood pressure measure- ments, systolic blood pressure (SBP) and diastolic blood pressure (DBP), were taken after a 15 minute rest period, in a sitting position on the left hand by the auscultatory method using a mercury sphygmomanometer and a ste- thoscope. The traits involving blood analysis were done by collecting blood samples by finger pricking, followed by putting the blood drops on different strips meant for different traits. All the blood parameters were analyzed immediately after collecting the blood samples from the participants with a dry autoanalyzer (Accutrend-GCT manufactured by Borhinger-Mannheim, 1999) and the respective results were recorded subsequently. 2.2.3. Measurement of Economic Condition Data on monthly family expenditure were collected from the participants and monthly per capita expenditure (MPCE) was calculated. However, MPEC was not used in this study to indicate the economic condition of the participants as other studies among the general popula- tion of the study location had experienced some un- avoidable errors of under- or over-reporting of MPCE. Therefore, an alternative and more objective method was used to assess the economic condition of the participants. This method had widely been used by Bhattacharya, Chattopadhyay, and Rudra [56] and Chattopadhyay [57] in many published literatures. In this method, the ratio between the number of living rooms in the household and number of family members (household size) (i.e. number of living rooms in the household/household size) were calculated. Then the participants’ families were  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 881 881 classified into three economic categories: low, middle, or high. If the ratio was 0.25 or less, i.e. at least four household members were living in one family living room (in most cases a couple with their two children), the economic category of the family was classified as ‘low’. Similarly, if the ratio was higher than 0.25 but less than or equal to 0.5, i.e. at most two household members were living in a single room, the economic category of the family was considered as ‘middle’. If the ratio was higher than 0.5, i.e. on average rooms in the house were shared by less than two persons, the economic categories of the family were considered as ‘high’. This classifica- tion of economic condition was also in agreement with MPCE of the participants. Out of 85 participants with amputation, 29 individuals belonged to the low eco- nomic group, 30 individuals belonged to the middle economic group and 26 individuals belonged to high economic group. 2.2.4. Measurement of Social Discomfort The social discomfort level for each participant was measured using the Social Discomfort Scale (SDS) as used by Rybarezyk et al. [5] in their study. SDS is a 3-item questionnaire and each question focused on the extent of discomfort in social interactions associated with an individual with an amputation. For example: “Does it bother you to have an adult you don’t know ask you about your amputation or prosthesis?” Each SDS item has three answers-‘1–not at all’, ‘2–somewhat’, and ‘3–definitely’, assigned scoring was 1 to 3. There is a possibility of scoring 3 to 9 in SDS. Score ‘3’ indicates absence of any social discomfort and score ‘9’ indicates the highest degree of social discomfort. 2.2.5. Measurement of Functional Outcome The Locomotor Index (LI) was used to measure the mo- bility and personal independence of a participant with an amputation. LI has widely been used for its reliability and sensitiveness for the measurement of personal inde- pendence of an individual with an amputation [9,58]. LI is a 14-item questionnaire with 4-multiple choice an- swers for each item, regarding the nature and extent of dependency in movement as well as daily activities. The scale ranges from 0 to 3 for each item/question, giving the possible range of scoring from 0 to 42 for all 14 items/questions. The scoring of ‘42’ indicates the indi- vidual is fully independent in daily activities, while a score of ‘0’ indicates a total dependence of the individual with an amputation on others. It is worthy to mention that if a participant with LEA reported to perform certain daily activities with the help of his rehabilitative aid (e.g. prosthesis or crutch), he was still considered independent for such activities, unless he was reported to take help from another person. 2.3. Statistical Analysis Demographic characteristics of the participants with LEA and the control participants were presented and compared by calculating Chi-square tests. The distribu- tion of the levels of depression among the individuals with LEA and controls were presented using the standard cut-off values for BDI scores [48]. The descriptive sta- tistics of the BDI scores were calculated for the indi- viduals with LEA and for the control group as well. Fur- ther, the comparisons between the two groups were done using independent sample t-tests. As there were a lack of published literatures reporting comparison of BDI score between individuals with traumatic amputation and con- trol population, no pre-test power analysis was done. Therefore, a post hoc power analysis was done by cal- culating the effect size (Cohen’s d) and the statistical power. The participants with LEA were classified according to the presence or absence of a number of health risk factors. The different risk factors with their respective cut-off values were presented. The descriptive statistics of the BDI scores were calculated for the participants with LEA separated by presence or absence of the health risk factors. Subsequently, comparisons of BDI scores between the two groups have been done for each health risk factor. The relationship between the presence of locomotor disability and the physical health traits were examined by a two-way analysis of variance of BDI scores, using the presence of LEA as a fixed factor and each physical health trait as a covariate. The same analysis was also done to determine the relationship between depression level and the economic condition (ratio between number of rooms in household and household size) of the indi- viduals with LEA. The relationships between depression level and various disability related factors were exam- ined by applying logistic regression analysis. All statis- tical analyses were done using the software SPSS for Windows version 14.0. 3. RESULTS On average the participants were middle aged (nearly 44% between 40 years to 55 years), married (65.7%), and with a secondary level of education (58.8%) (Table 1). About 50% of the participants with LEA belonged to households with annual per capita expenditure between $200 and $400. Comparisons of the demographic char- acteristics between the participants with LEA and con- trol participants were done using chi-square tests. The distribution of the participants across age groups, per capita expenditure categories, economic conditions, marital statuses and education levels were similar be- 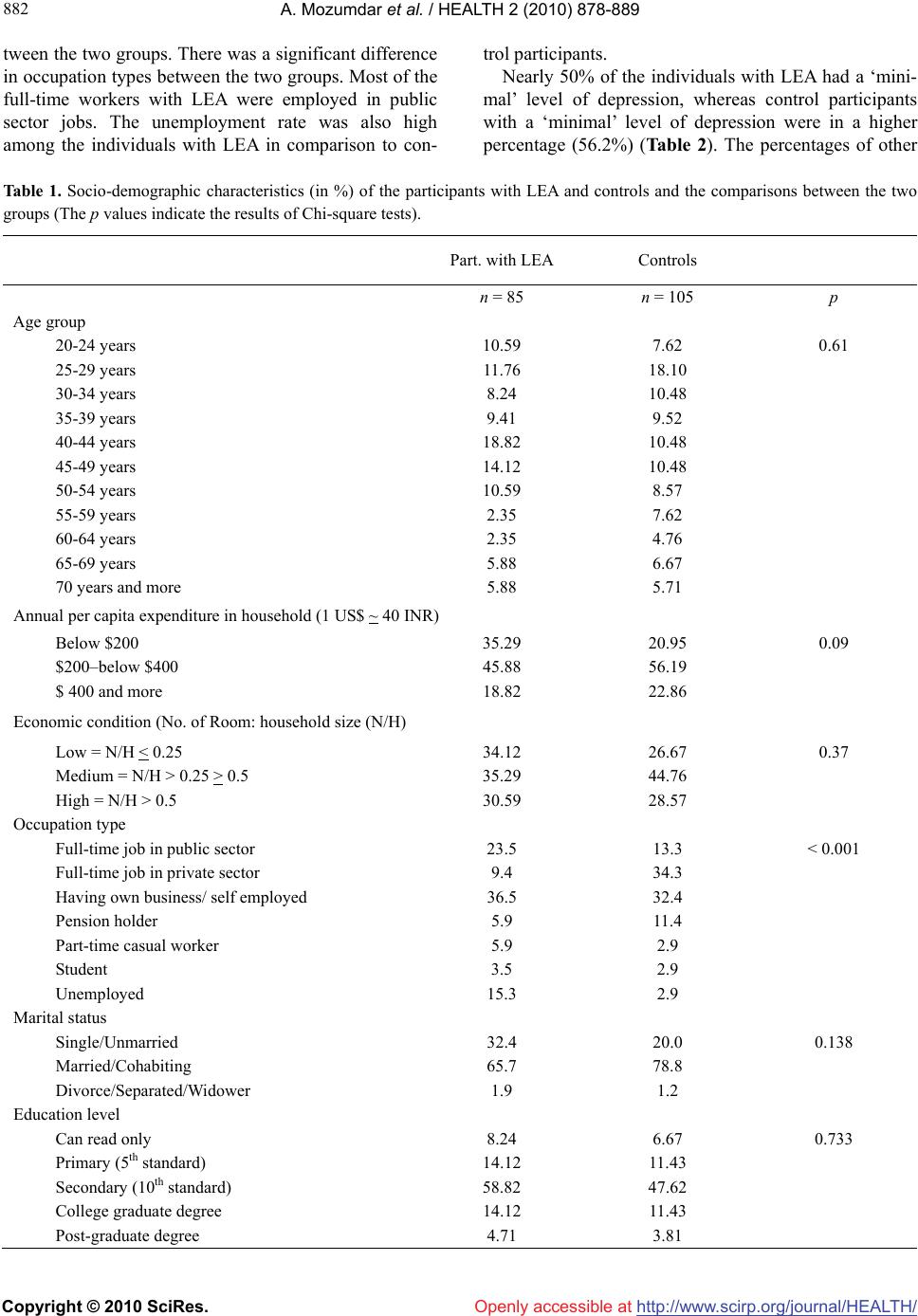 A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 882 tween the two groups. There was a significant difference in occupation types between the two groups. Most of the full-time workers with LEA were employed in public sector jobs. The unemployment rate was also high among the individuals with LEA in comparison to con- trol participants. Nearly 50% of the individuals with LEA had a ‘mini- mal’ level of depression, whereas control participants with a ‘minimal’ level of depression were in a higher percentage (56.2%) (Table 2). The percentages of other Table 1. Socio-demographic characteristics (in %) of the participants with LEA and controls and the comparisons between the two groups (The p values indicate the results of Chi-square tests). Part. with LEA Controls n = 85 n = 105 p Age group 20-24 years 10.59 7.62 0.61 25-29 years 11.76 18.10 30-34 years 8.24 10.48 35-39 years 9.41 9.52 40-44 years 18.82 10.48 45-49 years 14.12 10.48 50-54 years 10.59 8.57 55-59 years 2.35 7.62 60-64 years 2.35 4.76 65-69 years 5.88 6.67 70 years and more 5.88 5.71 Annual per capita expenditure in household (1 US$ ~ 40 INR) Below $200 35.29 20.95 0.09 $200–below $400 45.88 56.19 $ 400 and more 18.82 22.86 Economic condition (No. of Room: household size (N/H) Low = N/H < 0.25 34.12 26.67 0.37 Medium = N/H > 0.25 > 0.5 35.29 44.76 High = N/H > 0.5 30.59 28.57 Occupation type Full-time job in public sector 23.5 13.3 < 0.001 Full-time job in private sector 9.4 34.3 Having own business/ self employed 36.5 32.4 Pension holder 5.9 11.4 Part-time casual worker 5.9 2.9 Student 3.5 2.9 Unemployed 15.3 2.9 Marital status Single/Unmarried 32.4 20.0 0.138 Married/Cohabiting 65.7 78.8 Divorce/Separated/Widower 1.9 1.2 Education level Can read only 8.24 6.67 0.733 Primary (5th standard) 14.12 11.43 Secondary (10th standard) 58.82 47.62 College graduate degree 14.12 11.43 Post-graduate degree 4.71 3.81 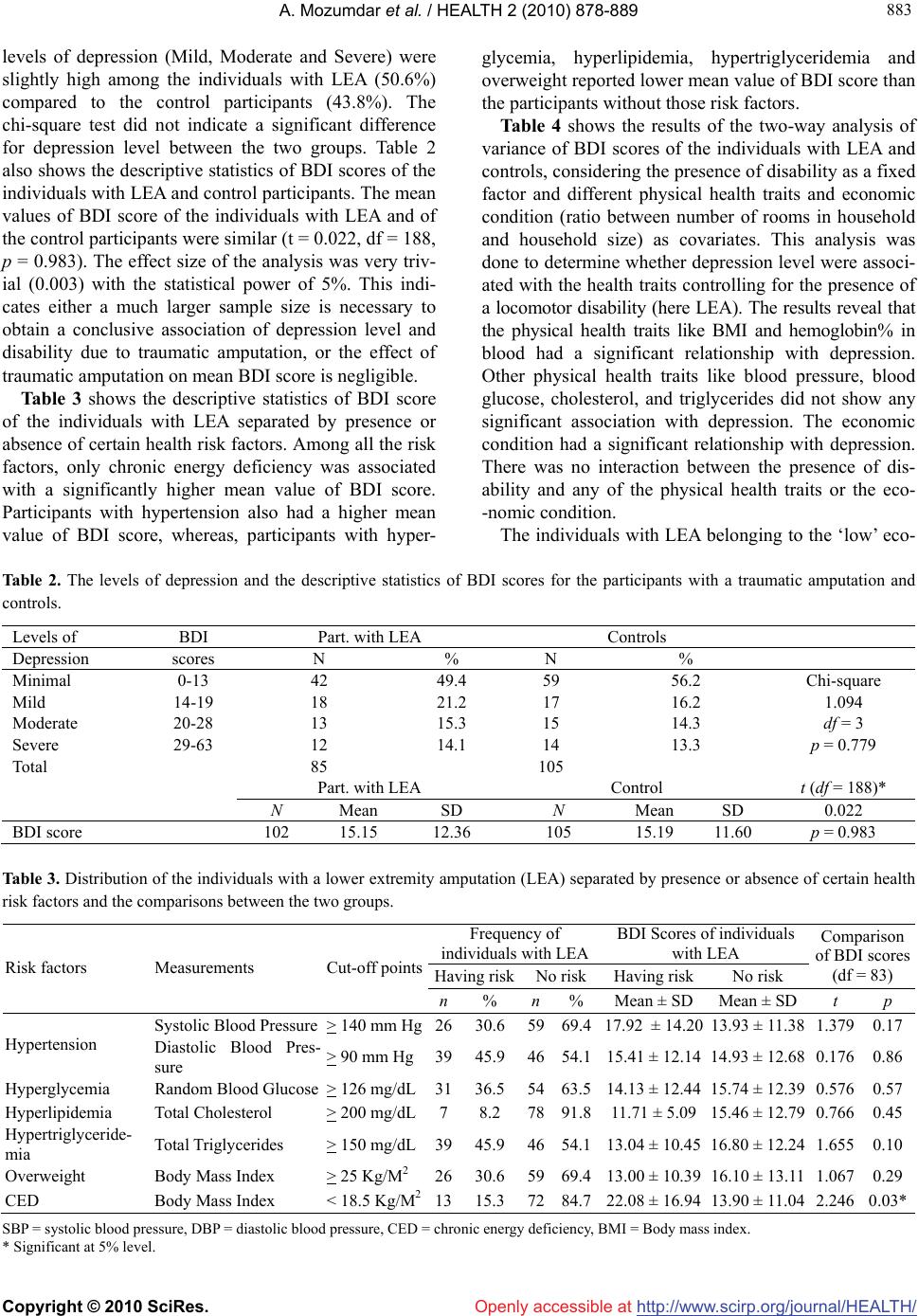 A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 883 883 levels of depression (Mild, Moderate and Severe) were slightly high among the individuals with LEA (50.6%) compared to the control participants (43.8%). The chi-square test did not indicate a significant difference for depression level between the two groups. Table 2 also shows the descriptive statistics of BDI scores of the individuals with LEA and control participants. The mean values of BDI score of the individuals with LEA and of the control participants were similar (t = 0.022, df = 188, p = 0.983). The effect size of the analysis was very triv- ial (0.003) with the statistical power of 5%. This indi- cates either a much larger sample size is necessary to obtain a conclusive association of depression level and disability due to traumatic amputation, or the effect of traumatic amputation on mean BDI score is negligible. Table 3 shows the descriptive statistics of BDI score of the individuals with LEA separated by presence or absence of certain health risk factors. Among all the risk factors, only chronic energy deficiency was associated with a significantly higher mean value of BDI score. Participants with hypertension also had a higher mean value of BDI score, whereas, participants with hyper- glycemia, hyperlipidemia, hypertriglyceridemia and overweight reported lower mean value of BDI score than the participants without those risk factors. Table 4 shows the results of the two-way analysis of variance of BDI scores of the individuals with LEA and controls, considering the presence of disability as a fixed factor and different physical health traits and economic condition (ratio between number of rooms in household and household size) as covariates. This analysis was done to determine whether depression level were associ- ated with the health traits controlling for the presence of a locomotor disability (here LEA). The results reveal that the physical health traits like BMI and hemoglobin% in blood had a significant relationship with depression. Other physical health traits like blood pressure, blood glucose, cholesterol, and triglycerides did not show any significant association with depression. The economic condition had a significant relationship with depression. There was no interaction between the presence of dis- ability and any of the physical health traits or the eco- -nomic condition. The individuals with LEA belonging to the ‘low’ eco- Table 2. The levels of depression and the descriptive statistics of BDI scores for the participants with a traumatic amputation and controls. Levels of BDI Part. with LEA Controls Depression scores N % N % Minimal 0-13 42 49.4 59 56.2 Chi-square Mild 14-19 18 21.2 17 16.2 1.094 Moderate 20-28 13 15.3 15 14.3 df = 3 Severe 29-63 12 14.1 14 13.3 p = 0.779 Total 85 105 Part. with LEA Control t (df = 188)* N Mean SD N Mean SD 0.022 BDI score 102 15.15 12.36 105 15.19 11.60 p = 0.983 Table 3. Distribution of the individuals with a lower extremity amputation (LEA) separated by presence or absence of certain health risk factors and the comparisons between the two groups. Frequency of individuals with LEA BDI Scores of individuals with LEA Having riskNo riskHaving risk No risk Comparison of BDI scores (df = 83) Risk factors Measurements Cut-off points n% n% Mean ± SD Mean ± SD t p Systolic Blood Pressure > 140 mm Hg2630.65969.417.92 ± 14.20 13.93 ± 11.38 1.3790.17 Hypertension Diastolic Blood Pres- sure > 90 mm Hg3945.94654.115.41 ± 12.14 14.93 ± 12.68 0.1760.86 Hyperglycemia Random Blood Glucose > 126 mg/dL3136.55463.514.13 ± 12.44 15.74 ± 12.39 0.5760.57 Hyperlipidemia Total Cholesterol > 200 mg/dL78.2 7891.811.71 ± 5.09 15.46 ± 12.79 0.7660.45 Hypertriglyceride- mia Total Triglycerides > 150 mg/dL3945.94654.113.04 ± 10.45 16.80 ± 12.24 1.6550.10 Overweight Body Mass Index > 25 Kg/M2 2630.65969.413.00 ± 10.39 16.10 ± 13.11 1.0670.29 CED Body Mass Index < 18.5 Kg/M21315.37284.722.08 ± 16.94 13.90 ± 11.04 2.2460.03* SBP = systolic blood pressure, DBP = diastolic blood pressure, CED = chronic energy deficiency, BMI = Body mass index. * Significant at 5% level.  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 884 Table 4. Two-way analysis of variance of BDI scores using the presence of LEA as a fixed factor and each physical health trait and economic condition (ratio between number of rooms in the household and household size) as a covariate. Factor 1 Factor 2 (LEA) Interaction (fac- tor 1* factor 2)Corr. Model Intercept Error Name of the factor F df p F df p F dfp F dfp F df p dfMean sqr SBP 0.43 1 0.52 0.45 1 0.510.4610.500.253 0.869.09 1 < 0.01* 186143.72 DBP 1.53 1 0.22 0.61 1 0.440.6310.430.66 30.5812.29 1 < 0.01* 186142.77 Blood glucose 0.76 1 0.39 1.48 1 0.231.97 1 0.160.88 30.4549.81 1 < 0.01* 186142.28 Total cholesterol 1.95 1 0.17 0.29 1 0.590.45 10.510.79 30.5012.34 1 0.01* 186116.60 Triglycerides 1.71 1 0.19 0.87 1 0.350.64 10.420.82 30.4873.79 1 < 0.01* 186140.37 BMI 6.71 1 0.01* 1.24 1 0.720.1110.752.16 30.0929.16 1 < 0.01* 186139.43 Haemoglobin% 5.50 1 0.02* 1.38 1 0.241.42 1 0.242.21 30.0919.02 1 < 0.01* 186139.32 Economic con- dition 10.91 1 < 0.01* 0.45 1 0.510.44 1 0.513.70 30.01*34.10 1 < 0.01* 186136.17 SBP = systolic blood pressure, DBP = diastolic blood pressure, BMI = Body mass index. nomic category showed a higher mean value of BDI score (Table 5). The individuals with LEA in the ‘mid- dle’ economic group showed a lower mean value of BDI scores than those in the ‘low’ economic group. The par- ticipants in the ‘high’ economic group showed the lowest mean value of BDI scores than the other two groups of economic condition. Among participants of three eco- nomic categories a significant difference in BDI scores was determined (p = 0.023). The mean BDI scores of the individuals with LEA in different levels of the social discomfort were significantly different. The individuals with LEA having ‘extreme’ social discomfort reported a mean BDI score of 32.67, which was almost two times higher than the mean BDI scores of the other groups. The participants experiencing ‘some’ degree of discom- fort and the participants without any discomfort reported similar mean BDI scores. A number of participants (48.4%) had changed their occupation due to coping with the new situation of locomotor disability. The indi- viduals (with LEA), who had changed their occupation after an amputation showed a significantly higher BDI score than the participants (with LEA) who had not changed their occupation. Again, the individuals (with LEA), who perceived problems in conjugal life due to amputation, showed a significantly higher mean value of BDI scores than the individuals (with LEA) who re- ported no problem in their conjugal life. No significant difference in BDI scores was reported between the individuals with an above knee amputation (AKA) and the individuals with a below knee amputa- tion (BKA) (Table 6). The participants (with LEA), who were totally independent in their daily activities showed a lower mean value of BDI score than the participants who had some kind of dependency. The result of the t-test showed a marginal difference between the groups (p = 0.08). The duration of disability did not show a consistent trend with depression scores. Recently ampu- tated individuals (up to 2 years) had higher mean values of BDI score than all other groups. However, the par- ticipants with a duration of disability between 10 to 20 years showed significantly less depression in comparison to participants with recent experience of a traumatic amputation. Other categories showed more or less simi- lar mean values of BDI scores. 4. DISCUSSION The results of the present study showed that the depres- sion level of individuals with a traumatic amputation and control participants were similar. The association of higher depression were reported with hypertension, and chronic energy deficiency, whereas, the risk conditions like hyperglycemia, hyperlipidemia, hypertriglyceride- mia, and overweight had relationship with a lower de pression level among individuals with LEA. due to the dearth of the empirical studies on this area of research among individuals with LEA the findings of the present study was not compared to other published data. How- ever, similar studies of the general (non-amputated) population showed similar results of association between depression and hypertension [14,15] and lower choles- terol level [17-20]. Although few studies of the general population reported an association between higher de- pression level and higher blood glucose [16] as well as obesity [59], the findings of this study did not corrobo- rate with those findings of earlier studies. The results of this study also indicated that low eco- nomic condition had an association with higher depress- sion in participants with a traumatic amputation, which was corroborative to the finding of the studies by Ry- barczyk et al. [5,6]. The association of perceived social discomfort and high depression levels among the indi-  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 885 885 Table 5. Descriptive statistics of BDI scores by socioeconomic variables of the individuals with LEA. Socio-economic variables n (%) BDI score Mean ± SD Economic condition No. of room: House hold Size (N/H) ANOVA df (2, 82) Low N/H < 0.25 29 (34.1) 20.07 ± 14.04 F = 3.932 Middle N/H > 0.25 > 0.5 30 (35.3) 13.57 ± 9.67 p = 0.023 High N/H > 0.5 26 (29.5) 11.50 ± 11.81 Social discomfort Social discomfort scale (SDS) ANOVA df (2, 82) Extreme SDS = 9 3 (3.53) 32.67 ± 11.50 F = 3.735 Some SDS = 4 to 8 37 (43.53) 13.19 ± 9.04 p = 0.028 None SDS = 3 45 (52.94) 15.60 ± 13.95 Change of occupation t (df = 83) Yes 49 (43.53) 18.38 ± 14.85 t = 2.157 No 53 (56.47) 12.67 ± 9.47 p = 0.034 Perceived problems in the conjugal life due to a disability (among married participants only) t (df = 65) Yes 10 (14.93) 26.40 ± 18.06 t = 2.815 No 57 (85.07) 14.32 ± 11.38 p = 0.006 Table 6. Descriptive statistics of BDI scores of the individuals with LEA and its association with disability related factors. Disability related factors n (%) BDI score (Mean ± SD) Odds Ratio 95% CI Levels of amputation t = 0.19 Above knee amputation 27 (31.76) 13.81 ± 13.85 df = 83 Ref. - Below knee amputation 58 (68.24) 16.78 ± 11.68 p = 0.499 1.01 0.98-1.05 Functional outcome in daily activities (LI = locomotor index) t = 1.795 Totally independent (LI = 42) 59 (69.41) 13.58 ± 11.95 df = 83 Ref. - Some dependency (LI < 42) 26 (30.59) 18.73 ± 12.77 p = 0.076 1.03 0.996-1.07 Duration of disability Up to 2 years 4 (4.71) 27.00 ± 15.30 ANOVA Ref. - More than 2 to 10 years 40 (35.29) 16.23 ± 13.27 F = 1.809 0.95 0.88-1.02 More than 10 to 20 years 32 (31.76) 11.37 ± 9.53 df (4, 80) 0.91 0.84-0.97 More than 20 to 30 years 14 (15.29) 14.62 ± 8.77 p = 0.135 0.94 0.86-1.02 More than 30 years 12 (12.94) 17.82 ± 16.38 0.96 0.88-1.04 viduals with an amputation was also corroborative to the finding of Rybarczyk et al. [5,6]. The high mean BDI score for the participants who changed their occupation due to disability indicated the adverse effect of occupation change on their mental health. This may be due to the uncertainty in their work- site or starting a new job. This finding of the present study corroborates with the study of Whyte and Niven [4]. A significantly high degree of depression was re- ported among the participants (with LEA), who per- ceived problems in their conjugal life due to a disability. This finding was also corroborative with the earlier studies [5-7,35]. The results of this study showed a lower depression level in the individuals with AKA than in the individuals with BKA and this was corroborative with the findings of O’Toole et al. [39]. O’Toole et al. [39] explained that individuals with BKA are less severely disabled in terms of function and may be in a better position in respect to their functional abilities, which is more or less similar to their pre-amputation abilities (except a full-fledged body image), than those with AKA. As a result, the individuals with BKA are more sensitive to the differences between themselves and able-bodied individuals.  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 886 The mean value of the BDI scores in individuals who had experienced LEA within last 2 years was much higher although only 4 participants were grouped in that category. The mean value of BDI score was much less in the participants who had an amputation 2 to 10 years ago. Earlier studies like Fisher and Hanspal [60], Furst and Humphrey [61] had similar findings. The participants with an experience of traumatic amputation 10 to 20 years ago showed the lowest mean BDI scores. The par- ticipants who had their amputation 30 years ago showed a slightly higher mean value of BDI scores than other categories (i.e. the individuals who had amputated 2-10 years, 10 to 20 years and 20-30 years ago). This result was consistent with the findings of a few studies [60,62], however it was in contrast to some studies as well [5,6, 26,38,63]. In an extensive review of studies regarding depression and time spent since amputation, Horgan and MacLachlan [44] commented that the findings of a higher depression level in some earlier studies might be due to the use of CES-D scales for diagnosing depres- sion, which usually overestimate depression in their study sample [64]. In explaining such associations of depression and time since amputation it can be theorized that there are three phases in adapting to change in body image, social discomfort and functional difficulties. The initial ‘shock’ is associated with a high level of depres- sion, followed by ‘adapting with the situation’ (the learning and adaptation phase of a new life with amputa- tion). When the time since amputation is long ago, the health deterioration with the advancing age and increas- ing difficulties due to physical immobility causes an increase in depression level. The inherent errors and limitations of the cross sec- tional data of the present study cannot be ruled out. The result of the present study should not be considered as any definitive finding in understanding depression and its bio-social correlates among individuals with LEA, but showed some trends which can not be ignored alto- gether. A possible and significant limitation for this finding is the 90% non-response rate in the sample. The level of depression may have influenced whether an in- dividual responded to the survey or not. Individuals with higher levels of depression may have been too depressed to agree to participate in the study. Conversely, individu- als who were depressed may have been more likely to respond so as to have the opportunity to discuss their feelings. However, due to a lack of maintenance of medical records it was difficult to control such con- founding factors for the present study. It is also worthy to mention that all the individuals with LEA had pros- thesis and therefore, they were to some extent rehabili- tated. This may help to reduce the depression level among the individuals with LEA. Possibly, because of these conditions, the post hoc power analysis revealed a trivial effect size for the difference in depression level between the individuals with a traumatic amputation and controls, suggesting a larger sample size is necessary to reveal a meaningful clinical result. Since the effect of rehabilitation on the depression and bio-social correlates can not be ruled out, it would have been better to repeat the study on non-rehabilitated individuals with LEA as well, to understand the effect of rehabilitation on mental health of the individuals with LEA. The levels of reha- bilitation, facilities and benefits available to individuals with LEA in developed countries are not comparable with developing countries like India. In view of these circumstances, although the present study showed some corroborative and contrasting findings to the other stud- ies from the western population, how far the other stud- ies were comparable was under question. Still, the com- parisons of the findings were done due to the lack of similar studies on the Indian population. The present study acknowledges these limitations but it is still rele- vant under limited resources, infrastructure, and con- venience. The results of the present study indicate how the indi- viduals with a traumatic LEA in Kolkata were finding themselves in the crossroads of changing societal atti- tude and its effects on their mental health. The individu- als with LEA did not show any effect of being amputated or physically impaired on their depression level. But the individuals with LEA were showing higher level of de- pression when they were experiencing social problems such as ‘social discomfort’, forced to change their occu- pations, facing trouble in their conjugal life or facing dependency in their daily activities. At the same time, it was also evident that the societal attitude towards people with a disability was still need to be changed, so that the individuals with a disability could get jobs in private sectors with equal proportions as general people. If that change happens in future, the dependency on job reser- vation in the public sector would be no longer necessary at all. The primary concern for most of the study par- ticipants was to earn for the basic need of life (food, dress and shelter) rather than maintaining a good health. It may be the reason that the sample population of the present study showed a positive relation of depression level with CED rather with overweight or high blood glucose level. To the participants, being overweight (body) was not a matter of illness but a symbol of abun- dance. The association of depression with other social correlates like change of occupation, and problems in conjugal life may also be because of economic instabil- ity of the study population. In developing countries like India, the physical, social and psychological well-being is incapacitated until and unless economic security is  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/ 887 887 Openly accessible at ensured. 5. CONCLUSIONS We expected that the individuals with LEA will be at a higher level of depression than the general population, but the findings of this study did not show any such dif- ference. The depression level of the individuals with LEA also was not associated to most of the physical health factor. Whereas, presence of chronic energy defi- ciency and socio-economic problems were significantly associated to a higher level of depression among indi- viduals with LEA. That is why; the wellbeing of the in- dividuals with LEA can only be achieved by improving the economic condition with a positive societal attitude towards disability. 6. ACKNOWLEDGEMENTS The authors are grateful to the study participants for their kind help and cooperation. Financial and logistic support was given to this study by the Indian Statistical Institute, Kolkata. We thank Katie Gunter at Cen- ter for Writers, North Dakota State University for reviewing the manu- script. Both the authors participated in study design, data analysis and writing the manuscript. AM collected the field data for the present study. No author had any financial or personal conflict of interest in the organization supporting the research. REFERENCES [1] American Psychiatric Association (APA). (1994) Diag- nostic and statistical manual of mental disorders. 4th Edition, Washington, D.C. [2] Mathew, R.J., Largen, J. and Claghorn, J.L. (1979) Bio- logical symptoms of depression. Psychosomatic Medi- cine, 41(6), 439-443. [3] Kashani, J.H., Frank, R.G., Kashani, S.R., Wonderlich, S.A. and Reid, J.C. (1983) Depression among amputees. Journal of Clinical Psychiatry, 44(7), 256-258. [4] Whyte, A.S. and Niven, C.A. (2001) Psychological dis- tress in amputees with phantom limb pain. Journal of Pain and Symptom Management, 22(5), 938-946. [5] Rybarczyk, B.D., Nyenhuis, D.L., Nicholas, J.J., Schulz R, Alioto, R.J. and Blair, C. (1992) Social discomfort and depression in a sample of adults with leg amputations. Archives of Physical and Medical Rehabilitation, 73(12), 1169-1173. [6] Rybarczyk, B, Nyenhuis, D.L., Nicholas, J.J., Cash, S.M. and Kaiser, J. (1995) Body image, perceived social stigma, and the prediction of psychosocial adjustment to leg amputation. Rehabilitation Psychology, 40(2), 95- 110. [7] Williamson, G.M., Schulz, R., Bridges, M.W. and Behan, A.M. (1994) Social and psychological factors in adjust- ment to limb amputation. Journal of Social Behavior and Personality, 9(2), 249-268. [8] Carter, R. (2000) Coping and depression in older adults who have a lower limb amputation. Unpublished doctoral dissertation, University of Birmingham, England. [9] Condie, E., Jones, D., Treweek, S. and Scott, H. (1996) A one-year national survey of patients having a lower limb amputation. Physiotherapy, 82(1), 14-20. [10] Weiss, G.N., Gorton, T.A., Read, R.C., Neal, L.A. (1990) Outcomes of lower extremity amputations. Journal of American Geriatric Society, 38(8), 877-883. [11] Madan, M., Peles, E., Halkin, H., Nitzan, H., Azaria, M., Gitel, S., Dolfin, D. and Modan, B. (1998) Increased car- diovascular disease mortality rates in traumatic lower limb amputees. American Journal of Cardiology, 82(10), 1242-1247. [12] Mozumdar, A. and Roy, S.K. (2006) Validity of an alter- native anthropometric trait as cardiovascular diseases risk factor: Example from individuals with lower extrem- ity amputation. European Journal of Clinical Nutrition, 60(10), 1180-1188. [13] Joynt, K.E., Whellan, D.J. and O’Connor, C.M. (2003) Depression and Cardiovascular Disease: Mechanisms of Interaction. Biological Psychiatry, 54(3), 248-261. [14] Shinn, E.H., Poston, W.S., Kimball, K.T., St Jeor, S.T. and Foreyt, J.P. (2001) Blood pressure and symptoms of depression and anxiety: A prospective study. American Journal of Hypertension, 14(7), Part 1, 660-664. [15] Jonas, B.S. and Lando, J.F. (2000) Negative affect as a prospective risk factor for hypertension. Psychosomatic Medicine, 62(2), 188-196. [16] Anderson, R.J., Freedland, K.E., Clouse, R.E. and Lust- man, P.J. (2001) The prevalence of comorbid depression in adults with diabetes: A meta-analysis. Diabetes Care, 24(6), 1069-1078. [17] Horsten, M., Wamala, S.P., Vingerhoets, A., Orth-Gomer K. (1997) Depressive symptoms, social support, and lipid profile in healthy middle-aged women. Psychosomatic Medicine, 59(5), 521-528. [18] Olusi, S.O. and Fido, A.A. (1996) Serum lipid concentra- tions in patients with major depressive disorder. Biologi- cal Psychiatry, 40(11), 1128-1131. [19] Steegmans, P.H., Fekkes, D., Hoes, A.W., Bak, A.A., van der Does, E. and Grobbee, D.E. (1996) Low serum cho- lesterol concentration and serotonin metabolism in men. British Medical Journal, 312(7025), 221. [20] Steegmans, P.H., Hoes, A.W., Bak, A.A., van der Does, E. and Grobbee, D.E. (2000) Higher prevalence of depres- sive symptoms in middleaged men with low serum cho- lesterol levels. Psychosomatic Medicine, 62(2), 205-211. [21] Hyyppa, M.T., Kronholm, E., Virtanen, A., Leino, A. and Jula, A. (2003) Does simvastatin affect mood and steroid hormone levels in hypercholesterolemic men? A ran- domized double-blind trial. Psychoneuroendocrinology, 28(2), 181-194. [22] Istvan, J., Zavela, K. and Weidner, G. (1992) Body weight and psychological distress in NHANES I. Inter- national Journal of Obesity and Related Metabolic Dis- order, 16(12), 999-1003. [23] Carpenter, K.M., Hasin, D.S., Allison, D.B. and Faith, M.S. (2000) Relationships between obesity and DSM-IV major depressive disorder, suicide ideation, and suicide attempts: Results from a general population study. Ameri- can Journal of Public Health, 90(2), 251-257.  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 888 [24] Bruce, L., Seeman, T.E., Merrill, S.S., Blazer, D.G. (1994) The impact of depressive symptomatology on physical disability: MacArthur Studies of Successful Aging. American Journal of Public Health, 84(11), 1796-1799. [25] Stansfeld, S.A., Marmot, M.G. (1992) Social class and minor psychiatric disorder in British Civil Servants: A validated screening survey using the General Health Questionnaire. Psychological Medicine, 22(3), 739-749. [26] Behel, J.M., Rybarczyk, B., Elliott, T.R., Nicholas, N.J., Nyenhuis, D. (2002) The role of perceived vulnerability in adjustment to lower extremity amputation: A prelimi- nary investigation. Rehabilitation Psychology, 47(1), 92- 105. [27] Kleck, R., Ono, H. and Hastorf, A.H. (1966) The effects of physical deviance upon face-to-face interaction. Hu- man Relations, 19(4), 425-436. [28] Snyder, M.L., Kleck, R.E., Strenta, A. and Mentzer, S.J. (1979) Avoidance of the handicapped: An attributional ambiguity analysis. Journal of Personality and social Psychology, 37(12), 2297-2306. [29] Goffman, I. (1963) Stigma: Notes on the Management of Spoiled Identity. Prentice Hall, Englewood Cliffs. [30] Simonsick, E.M., Kasper, J.D. and Phillips, C.L. (1998) Physical disability and social interacion: Factors associ- ated with low social contacts and home cofinement in disabled older women (The women’s health and aging study). Journal of Gerontology: Social Sciences, 53B(4), S209-17. [31] Weinstein, C.L. (1985) Assertiveness, anxiety, and inter- personal discomfort among amputees: Implications for assertiveness training. Archives of Physical Medicine and Rehabilitation, 66(10), 687-689. [32] Smith, D.G., Horn, P., Malchow, D.R.N, et al. (1995) Prosthetic history, prosthetic charges, and functional outcome of the isolated, traumatic below-knee amputee. Journal of Trauma: Injury, Infection and Critical Care, 38(1), 44-47. [33] Kegel, B., Carpenter, M.L. and Burgess, E.M. (1977) A survey of lower-limb amputees: Prostheses, phantom sensations, and psychosocial aspects. Bulletin of Pros- thetics Research, 10(27), 43-60. [34] Peters, E.J.G, Childs, M.R., Wunderlich, R.P., Harkless, L.B., Armstrong, D.G. and Lavery, L.A. (2001) Func- tional status of persons with diabetes-related lower- extremity amputations. Diabetes Care, 24(10), 1799- 1804. [35] Thompson, D.M. and Haran, D. (1984) Living with an amputation: What it means for patients and their helpers. International Journal of Rehabilitation Research, 7(3), 283-293. [36] Hagberg, E., Berlin, Ö.K. and Renström, P. (1992) Func- tion after through-kneecompared with below-knee and above-knee amputation. Prosthetics and Orthotics Inter- national, 16(3), 168-173. [37] Williamson, G.M. (1995) Restriction of normal activities among older adult amputees: The role of public self- consciousness. Journal of Clinical Geropsychology, 1(3), 229-242. [38] Williamson, G. and Walters, A. (1996) Perceived impact of limb amputation on sexual activity: A study of adult amputees. Journal of Sex Research, 33(3), 221-230. [39] O’Toole, D.M., Goldberg, R.T. and Ryan, B. (1985) Functional changes in vascular amputee patients: Evalua- tion by Barthel Index, PULSES Profile, and ESCROW Scale. Archives of Physical Medicine and Rehabilitation; 66(8), 508-511. [40] Shukla, G.D., Sahu, S.C., Tripathi, R.P. and Gupta, D.K. (1982) A psychiatric study of amputees. British Journal of Psychiatry, 141(1), 50-53. [41] Tyc, V.L. (1992) Psychosocial adaptation of children and adolescents with limb deficiencies: A review. Clinical Psychology Review, 12(3), 275-291. [42] Gerhards, F., Florin, I. and Knapp, T. (1984) The impact of medical, reeducational, and psychological variables and rehabilitation outcome in amputees. International Journal of Rehabilitation Research, 7(4), 379-388. [43] Cansever, A., Uzun, O., Yildiz, C., Ates, A. and Atesalp, A.S. (2003) Depression in men with traumatic lower part amputation: a comparison to men with surgical lower part amputation. Military Medicine, 168(2), 106-109. [44] Horgan, O. and MacLachlan, M. (2004) Psychosocial adjustment to lower-limb amputation: A review. Disabil- ity and Rehabilitation, 26(14-15), 837-850. [45] Dalal, A.K. (2000) Social attitudes and rehabilitation of people with disability: The Indian experience. Arab Journal of Rehabilitation, 5(1), 15-21. [46] Ministry of Law, Justice and Company Affairs. (1996) The persons with disabilities (equal opportunities, pro- tection of rights and full participation) act 1995. Gov- ernment of India, New Delhi. [47] National Sample Survey Organization. (2003) A report on disabled persons, Report 485, 55th Round. Ministry of Statistics and Program Implementation, Government of India, New Delhi. [48] Beck, A.T., Steer, R.A. and Brown, G.K. (1996) Manual for beck depression inventory–II. Psychological Corp, San Antonio. [49] Hughes, R.B., Robinson-Whelen, S., Taylor, H.B., Peter- sen, N.J. and Nosek, M.A. (2005) Characteristics of de- pressed and nondepressed women with physical disabili- ties. Archives of Physical Medicine and Rehabilitation; 86(3), 473-479. [50] Platisa, N. and Devecerski, G. (2006) Types of psycho- logical reactions in patients with lower-extremity ampu- tations. Medicinski Pregled, 59(3-4), 149-154. [51] Bodenheimer, C., Kerrigan, A.J., Garber, S.L., Monga, T.N. (2000) Sexuality in persons with lower extremity amputations. Disability and Rehabilitation, 22(9), 409- 415. [52] Frank, R.B., Kashani, J.H., Kashani, S.R., Wonderlich, S.A., Umlauf, R.L. and Ashkanazi, G.S. (1984) Psycho- logical response to amputation as a function of age and time since amputation. British Journal of Psychiatry, 144(5), 493-497. [53] Basu, S., Chattopadhyay, D., Deb, A., Ash, S., Samajder, J., Deb, Z. and Basu, S. (1995) Adoption of beck depres- sion inventry into Bengali and its clinical validity. Bulle- tin of Indian Psychiatric Society, 5(1), 5-9. [54] Weiner, J.S. and Laurie, J.A. (1981) Practical Human Biology. Academic Press, London. [55] Mozumdar, A. and Roy, S.K. (2004) Method for estima- tion of body weight of lower extremity amputees and its implication on their nutritional assessment. American Journal of Clinical Nutrition, 80(4), 868-875.  A. Mozumdar et al. / HEALTH 2 (2010) 878-889 Copyright © 2010 SciRes. http://www.scirp.org/journal/HEALTH/Openly accessible at 889 889 [56] Bhattacharya, N., Chattopadhyay, M. and Rudra, A. (1987) Changes in level in rural West Bengal: Social con- sumption. Economic and Political Weekly, 22(1), 33. [57] Chattopadhyay, M. (1990) Perceptions of villages about changes in level of living in West Bengal. The Adminis- trator; 25(1), 97-113. [58] Treweek, S.P. and Condie, M.E. (1998) Three measures of functional outcome for lower limb amputees: A retro- spective review. Prosthetics and Orthotics International, 22(3), 178-185. [59] Wilson, P.W., D’Agostino, R.B., Levy, D., Belanger, A.M., Silbershatz, H. and Kannel, W.B. (1998) Predic- tion of coronary heart disease using risk factor categories. Circulation, 97(18), 1837-1847. [60] Fisher, K. and Hanspal, R.S. (1998) Phantom pain, anxi- ety, depression, and their relation in consecutive patients with amputated limbs: Case reports. British Medical Journal, 316(7135), 903-904. [61] Furst, L. and Humphrey, M. (1983) Coping with the loss of a leg. Prosthetics and Orthotics International, 7(3), 152-156. [62] Breakey, J.W. (1997) Body Image: The lower-limb am- putee. Journal of Prosthetics and Orthotics, 9(2), 58-66. [63] Hill, A., Niven, C.A., Knussen, C. and McCreath, S.W. (1995) Rehabilitation outcome in long-term amputees. British Journal of Therapy and Rehabilitation, 2(11), 593-598. [64] Papassotiropoulos, A. and Heun, R. (1999) Screening for depression in the elderly: A study on misclassification by screening instruments and improvement of scale per- formance. Progress in Neuro-Psychopharmacology and Biological Psychiatry, 23(3), 431-446. |

