Paper Menu >>
Journal Menu >>
 Materials Sciences and Applications, 2010, 1, 118-126 doi:10.4236/msa.2010.13020 Published Online August 2010 (http://www.SciRP.org/journal/msa) Copyright © 2010 SciRes. MSA Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating Virpi Ääritalo1,5, Ville Meretoja1, Teemu Tirri1, Sami Areva2, Timo Jämsä3, Juha Tuukkanen4, Ari Rosling5, Timo Närhi1 1Department of Prosthetic Dentistry, Institute of Dentistry, University of Turku, Lemminkäisenkatu, Turku, Finland; 2Turku Centre for Biomaterials, Itäinen Pitkäkatu 4B, Turku, Finland; 3Department of Medical Technology, University of Oulu, Oulu, Finland; 4Department of Anatomy and Cell Biology, University of Oulu, Oulu, Finland; 5Laboratory of Polymer Technology, Åbo Akademi University, Biskopsgatan, Turku, Finland. Email: virpi.aaritalo@abo.fi Received May 20th, 2010; revised June 13th, 2010; accepted June 28th, 2010. ABSTRACT Objective of this study was to develope low temperature sol-gel coatings for shape memory metal (NiTi) and evaluate their biocompatibility on NiTi suture material. A series of low temperature TiO2 and TiO2-SiO2 sol-gel coatings were prepared on glass substrates. The silica content of TiO2-SiO2 coatings ranged from 0 to 30 mol%. The coatings were also prepared with polyethyleneglycol (PEG). The contact angle and photocatalytic activity measurements were used to evaluate the surface properties of the coatings. Stability of the coatings was tested in simulated body fluid (SBF). The TiO2-SiO2 90/10 film made with PEG was more hydrophilic, showed photocatalytic activity and was crack-free after the SBF test, thus it was chosen to animal experiment as a new experimental coating. Uncoated NiTi suture and the suture coated with high temperature TiO2 were used as reference materials. NiTi sutures were inserted subcutaneously on the back of rat for four weeks. In routine histological examinations all materials showed good biocompatibility with mild inflammatory cell reaction. No significant differences in the soft tissue response among the materials were observed. Both the high and new low temperature processed sol-gel coatings remained attached on the sutures confirming the suitability of the coating technique on thin NiTi sutures. Keywords: Sol-Gel Technique, Titania-Silica, Thin Film, Bioactive Coating, NiTi, Soft Tissue 1. Introduction Sol-gel technology is a promising manufacturing method to produce bioactive materials for biomedical applicati- ons [1,2]. The growing interest towards sol-gel materials is based on their ability to form a tight contact with the surrounding tissues, providing a strong chemical bond with them [3-5]. The silicon has shown to have several important roles in material preparation and materials bio- logical response. The addition of the silicon into the ma- terials structure has shown positive effect on osteoblast response on medical implant surfaces, e.g. on hydroxya- patite [6-8] and sol-gel titania films [9-11]. The TiO2- SiO2 sol-gel coatings have been shown to be biocompati- ble in vitro [9] and in vivo [12]. The nickel-titanium shape memory alloys (NiTi, Niti- nol) are promising materials for surgical implants in rec- onstructive medicine, because of their unique shape me- mory effect and super-elasticity [13]. However, some ad- verse effects such as inferior osteogenesis process, im- paired osteonectin synthesis and increased cell death rate have also been reported [14-16]. The biocompatibility of nikel-titanium alloys may be enhanced by the protective film e.g. by thickening the natural TiO2 layer at high tem- peratures [17], by hydroxyapatite coating [18] or by ion implantation [19]. A sol-gel derived titania-silica coating has been found to increase the bone to implant contact and biocompatibility of NiTi intramedullary nails [12]. The sol-gel materials can be processed and applied at room temperature, but the prepared materials often need a consolidation and densification step, by which the opt- imal material structure and surface properties can be tail- ored [20-22]. The conventional methods to consolidate the sol-gel titania are heat treatment at above 400˚C and/ or laser densification, but with these techniques the sub- strate material is limited to ceramics and metals. These temperatures are far too high for thermally sensitive mat- erials, such as most polymers, thus there is a striking ne- ed for bioactive sol-gel coatings prepared at lower tem- peratures.  Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating119 The purpose of this study was to evaluate the possibil- ity to lower the processing temperature of bioactive sol- gel derived implant coatings and to explore biologic res- ponse of the most promising coatings in soft tissue envi- ronment on NiTi suture materials. 2. Materials and Methods 2.1 Preparation of Coatings A series of titania and titania-silica coatings were prepa- red on glass slides by dip-coating method. Before the co- ating process the glass slides were ultrasonically cleaned in acetone and in ethanol, five minutes in both solvents. TiO2-SiO2 sols were prepared by mixing the following TiO2 and SiO2 sols so that the TiO2-SiO2 molar ratios 100/0, 90/10, 80/20 and 70/30 were obtained. SiO2 sol was prepared by mixing tetraethyl orthosilicate [TE-OS, (Si(OC2H5)4], ethanol and water at room temperature having the EtOH: Si(OR)4 and H2O: Si(OR)4 molar ratios of 1.9 and 1.0, respectively. The prepared sol was hydr- olyzed at 40˚C for one hour. TiO2 was prepared by mix- ing titanium tetraisopropoxide [TIPT, (Ti(OC3H7)4)], eth- anol, nitric acid (65%), and water at room temperature and hydrolyzed at 40˚C for 30 min having the EtOH: Ti(OR)4, H2O: Ti(OR)4 and HNO3: Ti(OR)4 molar ratios 18.0, 1.2 and 0.33, respectively. The prepared sols are mixed rapidly under stirring. The mixed TiO2-SiO2 sols were aged at 40˚C for 24 hours and cooled to room temp- erature before the dipping process. Sols were also prepa- red with polyethylene glycol PEG (Mw 600 g/mol). PEG is added into the mixed sol (mPEG = moxides) before aging. The compositions of the prepared mixed sols are shown in Table 1. The dipping process was carried out at amb- ient atmosphere at room temperature. The substrate pl- ates were dipped into the sol and withdrawn at a speed of 0.3 mm/s. The dip-coated plates were dried at 60˚C for one hour. The dried coatings were further treated in aut- oclave, 60 minutes at 121˚C. The TiO2-SiO2 90/10 PEG containing coatings were also post-treated under UV-lig- ht (254 nm) for three hours. Table 1. The compositions of the prepared TiO2-SiO2 sols Material EtOH/alk H2O/alk HNO3/alk TiSi 70/30 13.2 1.14 0.23 TiSi 70/30 PEG 13.2 1.14 0.23 TiSi 80/20 14.8 1.16 0.27 TiSi 80/20 PEG 14.8 1.16 0.27 TiSi 90/10 16.4 1.18 0.30 TiSi 90/10 PEG 16.4 1.18 0.30 TiO2 18.0 1.20 0.34 TiO2 PEG 18.0 1.20 0.34 2.2 Surface Characterization The transmittance through the dip coated glass substrates was measured using the UV-Vis spectrometer in the wa- velength range 300-600 nm [Shimadzu UV-1601]. Water contact angle of the coatings was measured by sessile drop method at room temperature by using contact angle meter CAM100 [KSV instruments Ltd., Helsinki, Finland]. The contact angle was established from six parallel measurements taken from each sample. Photocatalytic activity of the specimens was given by the degradation of methylene blue (MB). The coated glass substrates (2.5 cm × 2.5 cm) were immersed into MB aqueous solution (10-5 M). The substrates were irradiated with UV light and the changes in concentrations of MB in the aqueous solution were examined as a function of time from ab- sorption spectra measured on a UV-Vis spectrophotome- ter [Shimadzu UV-1601] at a wavelength of 660 nm. The concentration of methylene blue was measured over a 5-hour period, at intervals of one hour. The reaction rate constant for photocatalytic degradation of methylene blue was obtained graphically from the relationship bet- ween natural logarithm of the normalized absorbance, ln(A/A0), and reaction time [23]. The kinetic may be ex- pressed as follow, kt A A)ln( 0 (1) where k is the apparent reaction rate constant (1/hours), A0 and A are the initial absorbance and the reaction abs- orbance of methylene blue, respectively and t is time. The initial absorbance value is measured from the meth- ylene blue solution after one hour immersion in dark. The rate for the decomposition reaction of the MB aqueous so- lutions was obtained one time for each coating. An exa- mple for absorbance curves is shown in Figure 1. The resulted decomposition rates (1/hours) are given per area Figure 1. Calculation of the photocatalytic activity (k) (hour-1cm-2) from methylene blue time-absorbance curves. Curves are only shown for TiO2-SiO2 90/10 films; original and PEG containing, though in figure 4 all k-values are presented Copyright © 2010 SciRes. MSA  Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating 120 (cm2), because the specimens are cut from the glass sli- des (average size 2.5 cm × 2.5 cm). The stability of the coatings was tested by immersing the samples (10 × 10 mm2) into 15 ml of simulated body fluid (SBF) [24] at 37˚C for three weeks. Two parallel samples were immer- sed in closed polyethylene tubes under a shaking water bath at a constant temperature of 37˚C. After immersion the samples were removed from the fluid, gently rinsed with distilled water and dried at 40˚C before the surface analysis. The surfaces were analysed with optical micros- cope. 3. Animal Experiment 3.1 Implant Materials The NiTi (Ni 55.5-Ti 44.5 weight %) suture material was ground by silicon carbide papers having 1200 grits and the suture was ultrasonically washed 5 min in acetone and 5 min in ethanol before dipping. Two different sol- gel coated NiTi sutures were prepared: TiO2 heat treated at 500˚C and novel low temperature TiO2-SiO2 90/10 prepared with PEG, which exhibited the most suitable properties for implant coating (see materials characteri- zation section). The uncoated NiTi suture was used as reference. The average diameter of NiTi suture is 220 μm. The conventional TiO2 sol-gel coating was prepared by sol-gel dip-coating technique as described by Areva and co-workers [3]. Briefly, titanium tetraisopropoxide [TIPT, Ti((CH3)2CHO)4] was dissolved into ethanol and mixed with the solution containing ethyleneglycolmonoethyle- ther (C2H5OCH2OH), deionized water, fuming hydroch- loric acid (HCl, 37%) and ethanol. The sol was aged for 24 hours at 0˚C before dipping. The number of coating layers was five and every layer was heat treated 15 min- utes at 500˚C. The TiO2-SiO2 90/10 PEG sol was prep- ared as described in this work. The TiO2-SiO2 film was used as monolayer. The prepared film was autoclaved 60 minutes at 121˚C and UV-light treated for three hours. The implant sutures were sterilized with gamma radiation (minimum, 25 kGy). The morphology of implant surfa- ces was examined with SEM [JEOL Scanning Electron Microscope JSM-5500]. 3.2 Surgical Procedure Four adult Sprague-Dawley rats were used for the study. The experiment was accepted by The Ethical Committee for Animal Experiments at the Turku University, Finland (license #1420/04) and national guidelines for the care and use of laboratory animals were followed. Operations were performed under general anesthesia induced by sub- cutaneous injection of fentanyl citrate/fluanisone (Hypn- orm®, Janssen Pharmaceutica, Beerse, Belgium) and mi- datzolam (Dormicum®, Roche, Basel, Switzerland). The operation area was shaved and disinfected with chlorhex- idine gluconate solution (Klorhexol®, Leiras Ltd, Turku, Finland). The two centimeters long experimental materials were inserted subcutaneously on the back of each rat via six one centimeter skin incisions. Skin wound was closed with individual resorbable sutures (Vicryl 3-0, Johnson & Joh- nson Intl, Brussels, Belgium). Animals were sacrificed after four weeks using CO2 suffocation. Implants were retrieved with 2 to 4 mm soft tissue margin and fixed in 4% buffered formalin at 8˚C for two weeks. 3.3 Histological and Histomorphometrical Evaluation Fixed specimens were dehydrated in a graded series of ethanol and embedded in light curing resin (Technovit 7200, Exakt, Kulzer, Norderstedt, Germany). The specim- ens were cut and ground down to 20 μm and stained with haematoxylin and eosin (HE) for light microscope analy- sis. Sections were histologically evaluated for fibrous tis- sue capsule formation, inflammatory reaction and foreign body reaction using light microscope. Histomorphometrical grading was done according to the criteria by Jansen and co-workers [25]. Briefly, cap- sule thickness, tissue morphology and implant to tissue interface were rated from 0 (the least favorable) to 4 (the most favourable). The capsule thickness measurement was based on the observed number of fibroblasts. The qu- alitative rating of the capsule consisted of rating the tiss- ue morphology (fibrous tissue, maturity, presence of con- nective tissue or fat tissue) and cellularity (presence of fi- broblasts, macrophages, giant cells and other inflamma- tory cells). Direct contact was evaluated from four cross sectional sectors of the implants and graded according to the number of sectors from which immediate implant to tissue contact was detected. An implant was determined to be in direct contact if no visible gap could be observed between the connective tissue and implant surface at magnification × 200. Statistical analysis was performed with an SPSS v.11.0 software package (SPSS Inc., IL). Data were analyzed with one-way ANOVA followed by Tukey’s post-hoc test. Differences were considered sig- nificant at 95% confidence level. 4. Results 4.1 Surface Characteristics TiO2 and TiO2-SiO2 sols with 10, 20 and 30 mol% silica were successfully prepared and the sols produced clear crack free coatings on glass substrates (TiSi 70/30, TiSi 80/20, TiSi 90/10 and TiO2). The transmittance curves for the TiO2-SiO2 90/10 PEG coating after drying and after autoclaving of dried coating are seen in Figure 2. The figure shows the general trend seen in all the films with different compositions and no obvious difference in transmittance could be observed. All the prepared coat- ings were hydrophilic, contact angles varying from 60° to Copyright © 2010 SciRes. MSA 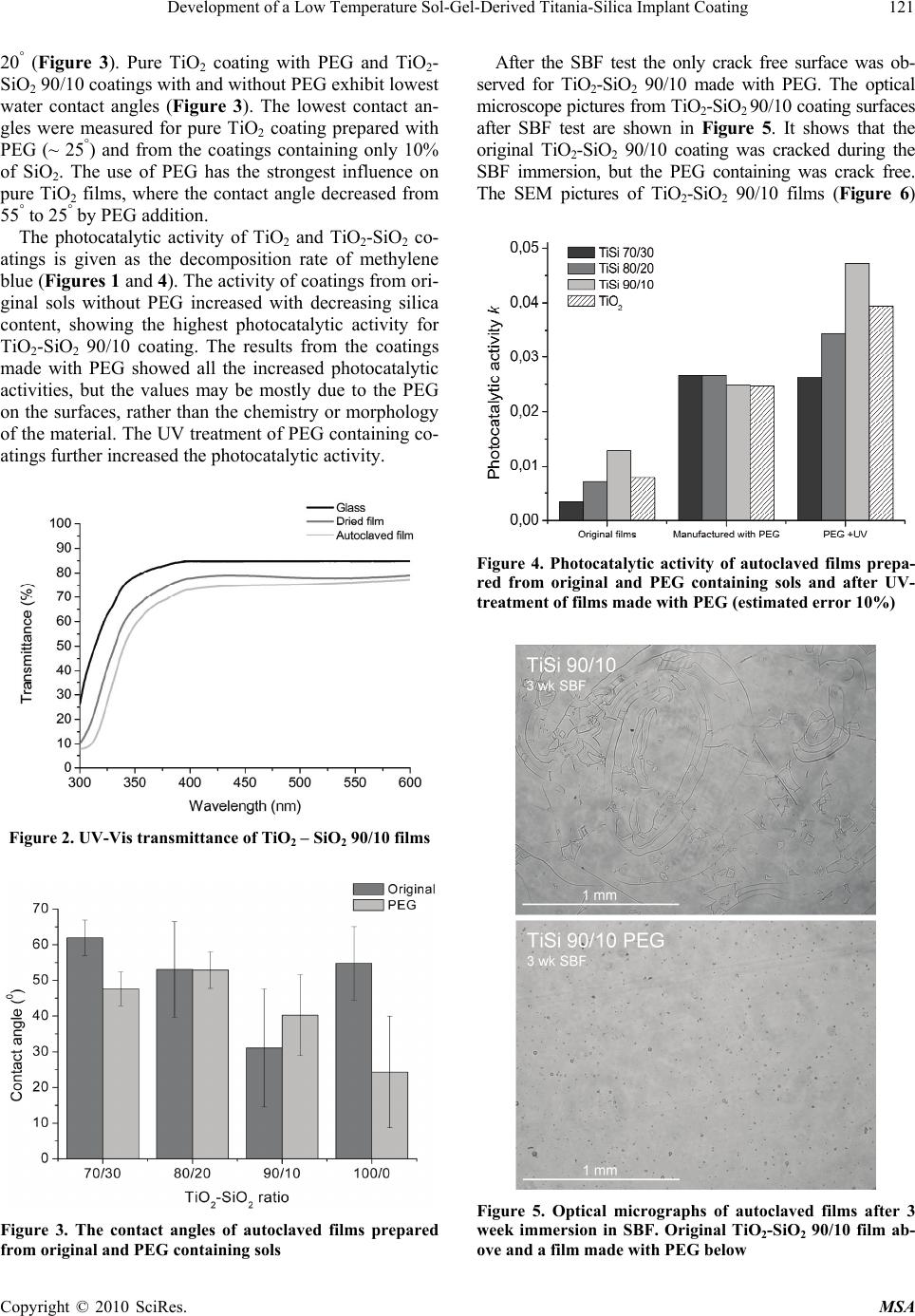 Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating121 20° (Figure 3). Pure TiO2 coating with PEG and TiO2- SiO2 90/10 coatings with and without PEG exhibit lowest water contact angles (Figure 3). The lowest contact an- gles were measured for pure TiO2 coating prepared with PEG (~ 25°) and from the coatings containing only 10% of SiO2. The use of PEG has the strongest influence on pure TiO2 films, where the contact angle decreased from 55° to 25° by PEG addition. The photocatalytic activity of TiO2 and TiO2-SiO2 co- atings is given as the decomposition rate of methylene blue (Figures 1 and 4). The activity of coatings from ori- ginal sols without PEG increased with decreasing silica content, showing the highest photocatalytic activity for TiO2-SiO2 90/10 coating. The results from the coatings made with PEG showed all the increased photocatalytic activities, but the values may be mostly due to the PEG on the surfaces, rather than the chemistry or morphology of the material. The UV treatment of PEG containing co- atings further increased the photocatalytic activity. Figure 2. UV-Vis transmittance of TiO2 – SiO2 90/10 films Figure 3. The contact angles of autoclaved films prepared from original and PEG containing sols After the SBF test the only crack free surface was ob- served for TiO2-SiO2 90/10 made with PEG. The optical microscope pictures from TiO2-SiO2 90/10 coating surfaces after SBF test are shown in Figure 5. It shows that the original TiO2-SiO2 90/10 coating was cracked during the SBF immersion, but the PEG containing was crack free. The SEM pictures of TiO2-SiO2 90/10 films (Figure 6) Figure 4. Photocatalytic activity of autoclaved films prepa- red from original and PEG containing sols and after UV- treatment of films made with PEG (estimated error 10%) Figure 5. Optical micrographs of autoclaved films after 3 week immersion in SBF. Original TiO2-SiO2 90/10 film ab- ove and a film made with PEG below Copyright © 2010 SciRes. MSA 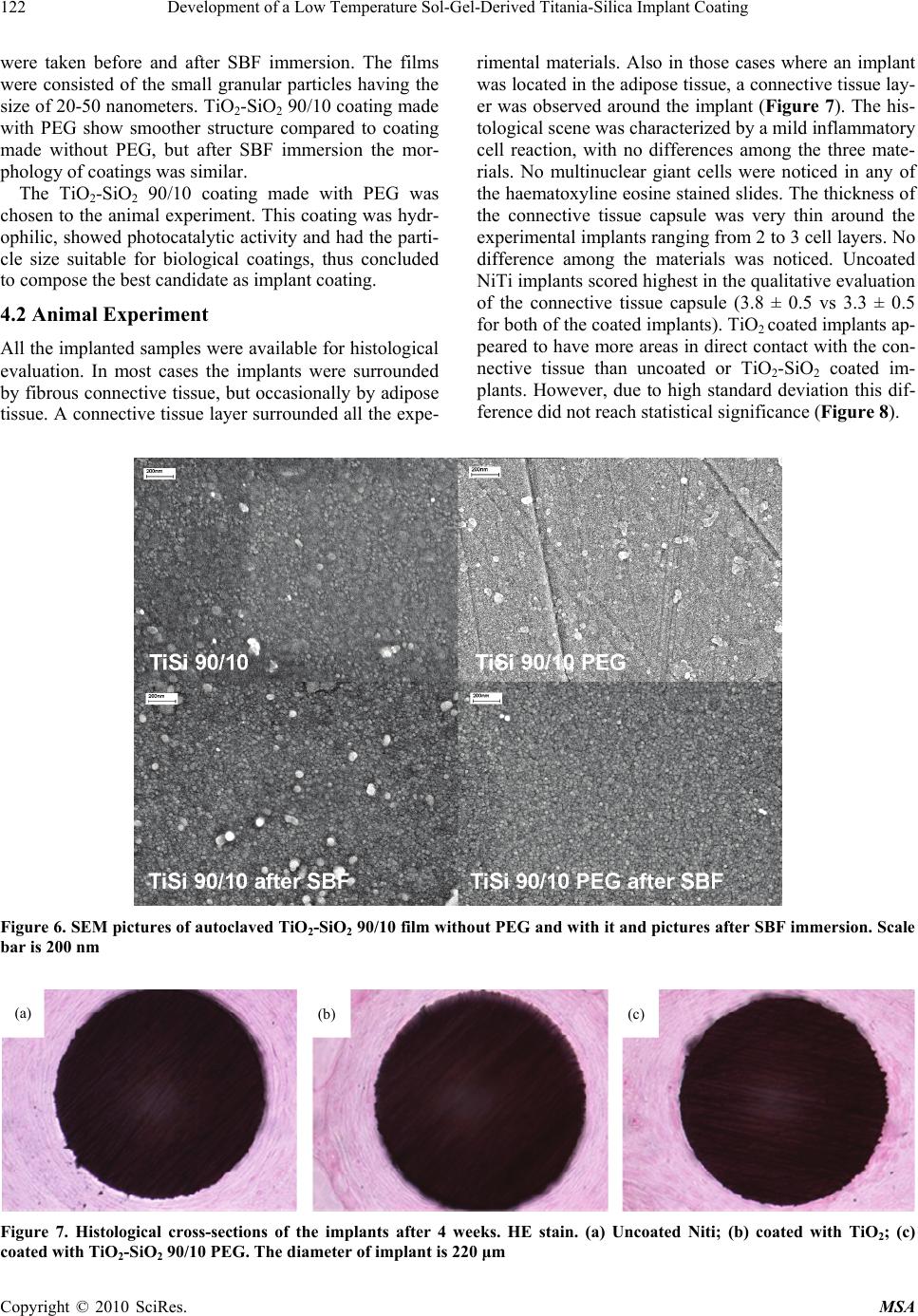 Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating Copyright © 2010 SciRes. MSA 122 were taken before and after SBF immersion. The films were consisted of the small granular particles having the size of 20-50 nanometers. TiO2-SiO2 90/10 coating made with PEG show smoother structure compared to coating made without PEG, but after SBF immersion the mor- phology of coatings was similar. The TiO2-SiO2 90/10 coating made with PEG was chosen to the animal experiment. This coating was hydr- ophilic, showed photocatalytic activity and had the parti- cle size suitable for biological coatings, thus concluded to compose the best candidate as implant coating. 4.2 Animal Experiment All the implanted samples were available for histological evaluation. In most cases the implants were surrounded by fibrous connective tissue, but occasionally by adipose tissue. A connective tissue layer surrounded all the expe- rimental materials. Also in those cases where an implant was located in the adipose tissue, a connective tissue lay- er was observed around the implant (Figure 7). The his- tological scene was characterized by a mild inflammatory cell reaction, with no differences among the three mate- rials. No multinuclear giant cells were noticed in any of the haematoxyline eosine stained slides. The thickness of the connective tissue capsule was very thin around the experimental implants ranging from 2 to 3 cell layers. No difference among the materials was noticed. Uncoated NiTi implants scored highest in the qualitative evaluation of the connective tissue capsule (3.8 ± 0.5 vs 3.3 ± 0.5 for both of the coated implants). TiO2 coated implants ap- peared to have more areas in direct contact with the con- nective tissue than uncoated or TiO2-SiO2 coated im- plants. However, due to high standard deviation this dif- ference did not reach statistical significance (Figure 8). Figure 6. SEM pictures of autoclaved TiO2-SiO2 90/10 film without PEG and with it and pictures after SBF immersion. Scale bar is 200 nm (a) (b) (c) Figure 7. Histological cross-sections of the implants after 4 weeks. HE stain. (a) Uncoated Niti; (b) coated with TiO2; (c) coated with TiO2-SiO2 90/10 PEG. The diameter of implant is 220 μm 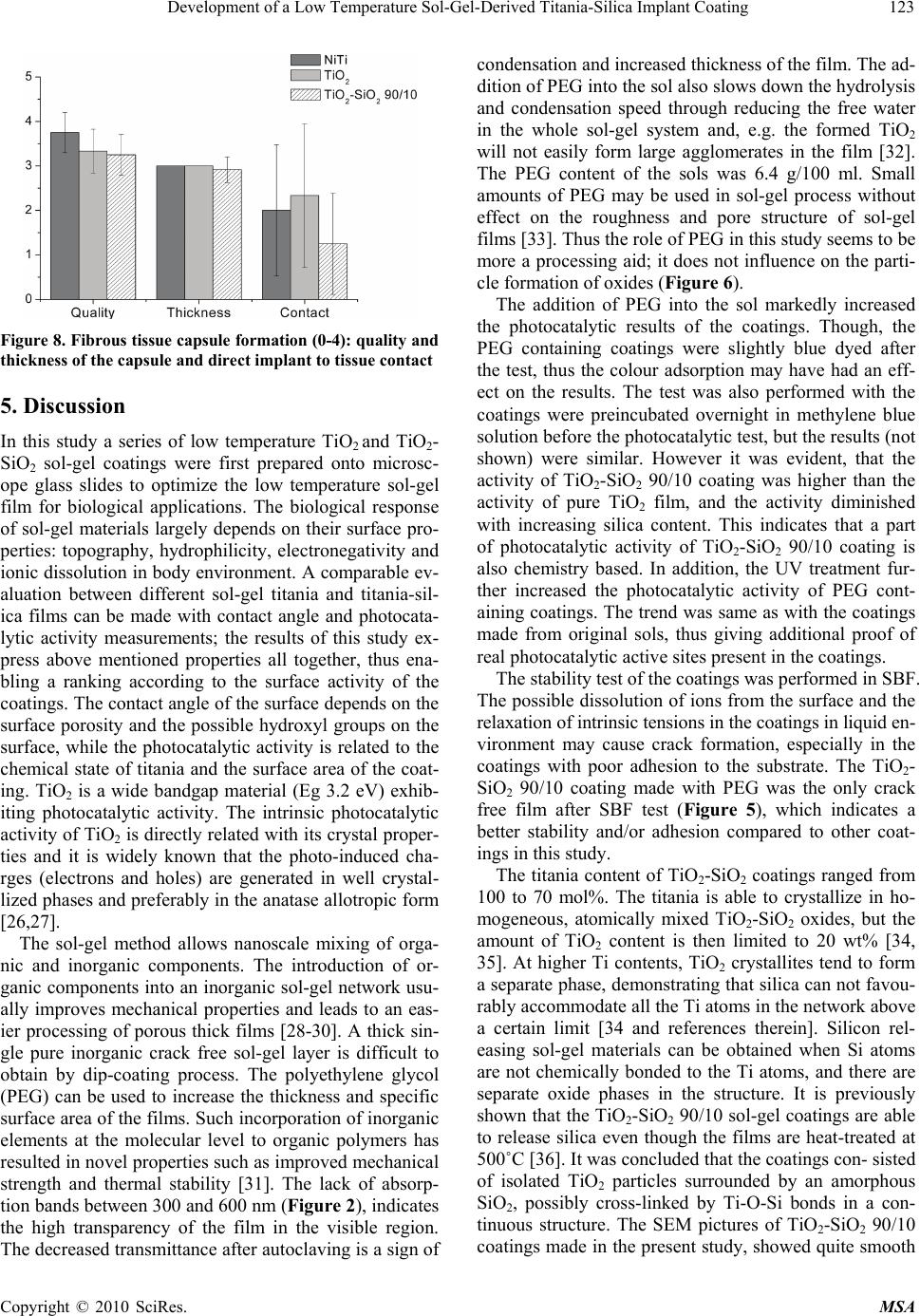 Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating123 Figure 8. Fibrous tissue capsule formation (0-4): quality and thickness of the capsule and direct implant to tissue contact 5. Discussion In this study a series of low temperature TiO2 and TiO2- SiO2 sol-gel coatings were first prepared onto microsc- ope glass slides to optimize the low temperature sol-gel film for biological applications. The biological response of sol-gel materials largely depends on their surface pro- perties: topography, hydrophilicity, electronegativity and ionic dissolution in body environment. A comparable ev- aluation between different sol-gel titania and titania-sil- ica films can be made with contact angle and photocata- lytic activity measurements; the results of this study ex- press above mentioned properties all together, thus ena- bling a ranking according to the surface activity of the coatings. The contact angle of the surface depends on the surface porosity and the possible hydroxyl groups on the surface, while the photocatalytic activity is related to the chemical state of titania and the surface area of the coat- ing. TiO2 is a wide bandgap material (Eg 3.2 eV) exhib- iting photocatalytic activity. The intrinsic photocatalytic activity of TiO2 is directly related with its crystal proper- ties and it is widely known that the photo-induced cha- rges (electrons and holes) are generated in well crystal- lized phases and preferably in the anatase allotropic form [26,27]. The sol-gel method allows nanoscale mixing of orga- nic and inorganic components. The introduction of or- ganic components into an inorganic sol-gel network usu- ally improves mechanical properties and leads to an eas- ier processing of porous thick films [28-30]. A thick sin- gle pure inorganic crack free sol-gel layer is difficult to obtain by dip-coating process. The polyethylene glycol (PEG) can be used to increase the thickness and specific surface area of the films. Such incorporation of inorganic elements at the molecular level to organic polymers has resulted in novel properties such as improved mechanical strength and thermal stability [31]. The lack of absorp- tion bands between 300 and 600 nm (Figure 2), indicates the high transparency of the film in the visible region. The decreased transmittance after autoclaving is a sign of condensation and increased thickness of the film. The ad- dition of PEG into the sol also slows down the hydrolysis and condensation speed through reducing the free water in the whole sol-gel system and, e.g. the formed TiO2 will not easily form large agglomerates in the film [32]. The PEG content of the sols was 6.4 g/100 ml. Small amounts of PEG may be used in sol-gel process without effect on the roughness and pore structure of sol-gel films [33]. Thus the role of PEG in this study seems to be more a processing aid; it does not influence on the parti- cle formation of oxides (Figure 6). The addition of PEG into the sol markedly increased the photocatalytic results of the coatings. Though, the PEG containing coatings were slightly blue dyed after the test, thus the colour adsorption may have had an eff- ect on the results. The test was also performed with the coatings were preincubated overnight in methylene blue solution before the photocatalytic test, but the results (not shown) were similar. However it was evident, that the activity of TiO2-SiO2 90/10 coating was higher than the activity of pure TiO2 film, and the activity diminished with increasing silica content. This indicates that a part of photocatalytic activity of TiO2-SiO2 90/10 coating is also chemistry based. In addition, the UV treatment fur- ther increased the photocatalytic activity of PEG cont- aining coatings. The trend was same as with the coatings made from original sols, thus giving additional proof of real photocatalytic active sites present in the coatings. The stability test of the coatings was performed in SBF. The possible dissolution of ions from the surface and the relaxation of intrinsic tensions in the coatings in liquid en- vironment may cause crack formation, especially in the coatings with poor adhesion to the substrate. The TiO2- SiO2 90/10 coating made with PEG was the only crack free film after SBF test (Figure 5), which indicates a better stability and/or adhesion compared to other coat- ings in this study. The titania content of TiO2-SiO2 coatings ranged from 100 to 70 mol%. The titania is able to crystallize in ho- mogeneous, atomically mixed TiO2-SiO2 oxides, but the amount of TiO2 content is then limited to 20 wt% [34, 35]. At higher Ti contents, TiO2 crystallites tend to form a separate phase, demonstrating that silica can not favou- rably accommodate all the Ti atoms in the network above a certain limit [34 and references therein]. Silicon rel- easing sol-gel materials can be obtained when Si atoms are not chemically bonded to the Ti atoms, and there are separate oxide phases in the structure. It is previously shown that the TiO2-SiO2 90/10 sol-gel coatings are able to release silica even though the films are heat-treated at 500˚C [36]. It was concluded that the coatings con- sisted of isolated TiO2 particles surrounded by an amorphous SiO2, possibly cross-linked by Ti-O-Si bonds in a con- tinuous structure. The SEM pictures of TiO2-SiO2 90/10 coatings made in the present study, showed quite smooth Copyright © 2010 SciRes. MSA  Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating 124 granular structures for coatings made with and without PEG (Figure 6). The slightly smoother structure of the PEG containing coating may derive from the applied PEG, because the original granular structure was re- vealed after a three week immersion in SBF. The coating structure consisted mainly of those granular particles having the size from 20 to 50 nm, thus exhibiting the morphology shown to favour bioactivity of sol-gel mate- rials (2-50 nm) [37-39]. The crystallinity of the studied materials was not ana- lysed in this work. X-ray diffraction (XRD) is a prefer- able method to analyse crystallinity of sol-gel films, but the sensitivity of the equipment is insufficient for analy- sing thin coatings with very small crystallites. It is shown that the incorporation of the silica onto the titania net- work can effectively inhibit the crystallite growth of tita- nia or even disrupt the phase transformation from amor- phous to anatase or rutile form [40-42]. In the present study different sol-gel derived coatings were fabricated on shape memory alloy sutures. Subcu- taneous implantation is often used method to examine bi- ocompatibility of new biomaterials. In terms of biocom- patibility both the test and control materials performed equally well in rat subcutaneous environment after a 4 weeks implantation period. The high temperature sol-gel titania coating studied in this work is previously shown to bond to the connective tissue [3,43]. In light of this, the new low temperature TiO2-SiO2 coating is a promi- sing implant coating material. Longer implantation time in more demanding conditions would be needed in order to be able to detect real differences in the biological res- ponse, e.g. in terms of the unwanted dissolution of nickel, from these experimental materials. 6. Conclusions Based on this study it can be concluded that biocompati- ble sol-gel derived coatings can be applied on memory metal sutures. The comparable study of different sol-gel surfaces by contact angle and photocatalytic activity measurements may be used to evaluate the surface activ- ity of the sol-gel biomaterials. The novel low temperature sol-gel TiO2-SiO2 90/10 coating was found to perform equally well with traditional high temperature TiO2 coat- ing in rat subcutaneous environment after a four weeks implantation period. 7. Acknowledgements This work was supported in part by the National Techn- ology Agency of Finland (40222/05, 40171/06). V. Ä. was supported by the Biomaterial and Tissue Engineer- ing Graduate School in Finland. REFERENCES [1] D. Pickup, K. Wetherall, J. Knowles, M. Smith and R. Newport, “Sol-Gel Preparation and High-Energy XRD Study of (CaO)x(TiO2)0.5−x(P2O5)0.5 Glasses (x = 0 and 0.25),” Journal of Materials Science: Materials in Medi- cine, Vol. 19, No. 4, April 2008, pp. 1661-1668. [2] P. Saravanapavan, J. R. Jones, S. Verrier, R. Beilby, V. J. Shirtliff, L. L. Hench and J. M. Polak, “Binary CaO–SiO2 Gel-Glasses for Biomedical Applications,” Bio-Medical Materials & Engineering, Vol. 14, No. 4, December 2004, pp. 467-486. [3] S. Areva, H. Paldan, T. Peltola, T. Närhi, M. Jokinen and M. Lindén, “Use of Sol-Gel-Derived Titania Coating for Direct Soft Tissue Attachment,” Journal of Biomedical Materials Research Part A, Vol. 70A, No. 2, August 2004, pp. 169-178. [4] C. P. A. T. Klein, P. Li, J. M. A. de Blieck-Hogervorst and K. de Groot, “Effect of Sintering Temperature on Silica Gels and their Bone Bonding Ability,” Biomate- rials, Vol. 16, No. 9, June 1995, pp. 715-719. [5] L. Meseguer-Olmo, M. Ros-Nicolás, V. Vicente-Ortega, M. Alcaraz-Baños, M. Clavel-Sainz, D. Arcos, C. V. Ragel, M. Vallet-Regí and Meseguer-Ortiz C., “A Bioac- tive Sol-Gel Glass Implant for In Vivo Gentamicin Re- lease. Experimental Model in Rabbit,” Journal of Ortho- paedic Research, Vol. 24, No. 3, March 2006, pp. 454- 460. [6] M. Houmard, D. Riassetto, F. Roussel, A. Bourgeois, G. Berthomé, J. C. Joud and M. Langlet, “Enhanced Persi- Stence of Natural Super-Hydrophilicity in TiO2-SiO2 Composite Thin Films Deposited via a Sol-Gel Route,” Surface Science, Vol. 602, No. 21, November 2008, pp. 3364-3374. [7] L. L. Hench, I. D. Xynos and J. M. Polak, “Bioactive Glasses for in Situ Tissue Regeneration,” Journal of Biomaterials Science - Polymer Edition, Vol. 15, No. 4, April 2004, pp. 543-562. [8] E. S. Thian, J. Huang, S. M. Best, Z. H. Barber and W. Bonfield, “Silicon-Substituted Hydroxyapatite: The Next Generation of Bioactive Coatings,” Materials Science and Engineering: C, Vol. 27, No. 2, March 2007, pp. 251- 256. [9] S. Areva, V. Ääritalo, S. Tuusa, M. Jokinen, M. Lindén and T. Peltola, “Sol-Gel-Derived TiO2-SiO2 Implant Coa- Tings for Direct Tissue Attachment. Part II: Evaluation of Cell Response,” Journal of Materials Science: Materials in Medicine, Vol. 18, No. 8, August 2007, pp. 1633-1642. [10] D. Böcking, J. Fiedler, R. E. Brenner and R. E. Hüsing. “Cultivation of Human Fibroblasts and Multipotent Mes- enchymal Stromal Cells on Mesoporous Silica and Mixed Metal Oxide Films,” Journal of Materials Science, Vol. 44, No. 24, December 2009, pp. 6786-6794. [11] A. Ochsenbein, F. Chai, S. Winter, M. Traisnel, J. Breme and H. F. Hildebrand. “Osteoblast Responses to Different Oxide Coatings Produced by the Sol–Gel Process on Ti- tanium Substrates,” Acta Biomaterialia, Vol. 4, No. 5, September 2008, pp. 1506-1517. [12] V. Muhonen, S. Kujala, A. Vuotikka, V. Ääritalo, T. Pel- tola, S. Areva, T. Närhi and J. Tuukkanen, “Biocompatib- Copyright © 2010 SciRes. MSA  Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating125 ility of Sol-Gel-Derived Titania-Silica Coated Intrame- dullary NiTi Nails,” Acta Biomaterialia, Vol. 5, No. 2, February 2009, pp. 785-793. [13] N. B. Morgan, “Medical Shape Memory Alloy Applica- tions–The Market and its Products,” Materials Science and Engineering A, Vol. 378, No. 1-2, July 2004, pp. 16- 23. [14] M. Es-Souni, M. Es-Souni and H. Fischer-Brandies, “On the Properties of Two Binary Niti Shape Memory Alloys. Effects of Surface Finish on the Corrosion Behaviour and in Vitro Biocompatibility,” Biomaterials, Vol. 23, No. 14, July 2002, pp. 2887-2894. [15] W. Jia, M. W. Beatty, R. A. Reinhardt, T. M. Petro, D. M. Cohen, C. R. Maze, E. A. Strom and M. Hoffman, “Nic- kel Release from Orthodontic Arch Wires and Cellular Immune Response to Various Nickel Concentrations,” Journal of Biomedical Materials Research Part B: Ap- plied Biomaterials, Vol. 48, No. 4, July 1999, pp. 488- 495. [16] C. Shih, S. Lin, Y. Chen, Y. Su, S. Lai, G. J. Wu, C. Kwok and K. Ching, “The Cytotoxicity of Corrosion Products of Nitinol Stent Wire on Cultured Smooth Mus- cle Cells,” Journal of Biomedical Materials Research Part A, Vol. 52, No. 2, November 2000, pp. 395-403. [17] Y. W. Gu, B. Y. Tay, C. S. Lim and M. S. Yong, “Chara- cterization of Bioactive Surface Oxidation Layer on NiTi Alloy,” Applied Surface Science, Vol. 252, No. 5, Dece- mber 2005, pp. 2038-2049. [18] C. Y. Li, X. J. Yang, L. Y. Zhang, M. F. Chen and Z. D. Cui, “In vivo Histological Evaluation of Bioactive NiTi Alloy after Two Years Implantation,” Materials Science and Engineering: C, Vol. 27, No. 1, January 2007, pp. 122-126. [19] N. Shevchenko, M.-T. Pham and M. F. Maitz, “Studies of Surface Modified NiTi Alloy,” Applied Surface Science, Vol. 235, No. 1-2, July 2004, pp. 126-131. [20] N. Moritz, S. Areva, J. Wolke and T. Peltola, “TF-XRD Examination of Surface-Reactive TiO2 Coatings Pro- duced by Heat Treatment and CO2 Laser Treatment,” Biomaterials, Vol. 26, No. 21, July 2005, pp. 4460-4467. [21] B. Yang, M. Uchida, H. Kim, X. Zhang and T. Kokubo, “Preparation of Bioactive Titanium Metal via Anodic Oxidation Treatment,” Biomaterials, Vol. 25, No. 6, March 2004, pp. 1003-1010. [22] T. Peltola, M. Pätsi, H. Rahiala, I. Kangasniemi and A. Yli-Urpo, “Calcium Phosphate Induction by Sol-Gel- Derived Titania Coatings on Titanium Substrates in Vi- tro,” Journal of Biomedical Materials Research Part A, Vol. 41, No. 3, September 1998, pp. 504-510. [23] J. Yu, X. Zhao and Q. Zhao, “Effect of Surface Structure on Photocatalytic Activity of TiO2 Thin Films Prepared by Sol-Gel Method,” Thin Solid Films, Vol. 379, No. 1-2, December 2000, pp. 7-14. [24] T. Kokubo, H. Kushitani, S. Sakka, T. Kitsugi and T. Ya- mamuro, “Solutions Able to Reproduce in vivo Surface- Structure Changes in Bioactive Glass-Ceramic A-W3,” Journal of Biomedical Materials Research, Vol. 24, No. 6, June 1990, pp. 721-734. [25] J. A. Jansen, W. J. Dhert, J. P. van der Waerden and A. F. von Recum, “Semi-Quantitative and Qualitative His- tologic Analysis Method for the Evaluation of Implant Biocompatibility,” Journal of Investigative Surgery, Vol. 7, No. 2, March-April 1994, 123-134. [26] H. Choi, E. Stathatos and D. D. Dionysiou, “Synthesis of Nanocrystalline Photocatalytic TiO2 Thin Films and Par- ticles Using Sol-Gel Method Modified with Nonionic Surfactants,” Thin Solid Films, Vol. 510, No. 1-2, July 2006, pp. 107-114. [27] M. Langlet, A. Kim, M. Audier and J. M. Herrmann, “Sol-Gel Preparation of Photocatalytic TiO2 Films on Polymer Substrates,” Journal of Sol-Gel Science and Technology, Vol. 25, No. 3, December 2002, pp. 223- 234. [28] A. Matsuda, Y. Matsuno, M. Tatsumisago and T. Minami, “Changes in Porosity and Amounts of Adsorbed Water in Sol-Gel Derived Porous Silica Films with Heat Treat- ment,” Journal of Sol-Gel Science and Technology, Vol. 20, No. 2, February 2001, pp. 129-134. [29] Y. Djaoued, S. Badilescu, P. V. Ashrit, D. Bersani, P. P. Lottici and R. Brüning, “Low Temperature Sol-Gel Pre- paration of Nanocrystalline TiO2 Thin Films,” Journal of Sol-Gel Science and Technology, Vol. 24, No. 3, July 2002, 247-254. [30] Z. Liu, Z. Jin, W. Li and J. Qiu, “Preparation of ZnO Porous Thin Films by Sol-Gel Method Using PEG Tem- plate,” Materials Letters, Vol. 59, No. 28, December 2005, pp. 3620-3625. [31] K. Kuraoka, T. Ueda, M. Sato, T, Okamoto and T. E. Yazawa. “Preparation and Properties of Organic-Inorganic Hybrid Flexible Hardcoat Films,” Journal of Materials Science, Vol. 40, No. 13, July 2005, pp. 3577-3579. [32] B. Guo, Z. Liu, L. Hong and H. Jiang, “Sol-Gel Derived Photocatalytic Porous TiO2 Thin Films,” Surface and Co- atings Technology, Vol. 198, No. 1-3, August 2005, pp. 24-29. [33] J. Yu, J. C. Yu, B. Cheng, X. Zhao, Z. Zheng and A. S. K. Li, “Atomic Force Microscopic Studies of Porous TiO2 Thin Films Prepared by the Sol-Gel Method,” Journal of Sol-Gel Science and Technology, Vol. 24, No. 3, July 2002, pp. 229-240. [34] X. Gao and I. E. Wachs, “Titania-Silica as Catalysts: Mo- lecular Structural Characteristics and Physicochemical Properties,” Catalysis Today, No. 51, No. 2, June 1999, pp. 233-254. [35] D. M. Pickup, F. E. Sowrey, R. J. Newport, P. N. Gun- awidjaja, K. O. Drake and M. E. Smith, “The Structure of TiO2-SiO2 Sol-Gel Glasses from Neutron Diffraction with Isotopic Substitution of Titanium and 17O and 49Ti Solid- state NMR with Isotopic Enrichment,” The Journal of Physical Chemistry B, Vol. 108, No. 30, July 2004, pp. 10872-10880. [36] V. Ääritalo, S. Areva, M. Jokinen, M. Lindén and T. Pelt- ola, “Sol-Gel-Derived TiO2-SiO2 Implant Coatings for Direct Tissue Attachment. Part I: Design, Preparation and Copyright © 2010 SciRes. MSA  Development of a Low Temperature Sol-Gel-Derived Titania-Silica Implant Coating Copyright © 2010 SciRes. MSA 126 Characterization,” Journal of Materials Science: Materi- als in Medicine, Vol. 18, No. 9, September 2007, pp. 1863-7183. [37] P. Sepulveda, J. R. Jones and L. L. Hench, “In Vitro Dis- solution of Melt-Derived 45S and Sol-Gel Derived 58S Bioactive Glasses,” Journal of Biomedical Materials Res- earch Part A, Vol. 61, No. 2, August 2002, pp. 301-311. [38] M. M. Pereira and L. L. Hench, “Mechanisms of Hydr- oxyapatite Formation on Porous Gel-Silica Substrates,” Journal of Sol-Gel Science and Technology, Vol. 7, No. 1-2, August 1996, pp. 59-68. [39] T. Peltola, M. Jokinen, H. Rahiala, M. Pätsi, J. Heikkilä, I. Kangasniemi and A. Yli-Urpo, “Effect of Aging Time of Sol on Structure and in Vitro Calcium Phosphate Forma- tion of Sol-Gel-Derived Titania Films,” Journal of Bio- medical Materials Research Part A, Vol. 51, No. 2, Au- gust 2000, pp. 200-208. [40] C. Kang, L. Jing, T. Guo, H. Cui, J. Zhou and H. Fu, “Mesoporous SiO2-Modified Nanocrystalline TiO2 with High Anatase Thermal Stability and Large Surface Area as Efficient Photocatalyst,” The Journal of Physical Chemistry C, Vol. 113, No. 3, January 2009, pp. 1006- 1013. [41] H. J. Lee, S. H. Hahn, E. J. Kim and Y. Z. You, “Influ- ence of Calcination Temperature on Structural and Opti- cal Properties of TiO2-SiO2 Thin Films Prepared by Sol-Gel Dip Coating,” Journal of Materials Science, No. 39, No. 11, June 2004, pp. 3683-3688. [42] C. Xie, Z. Xu, Q. Yang, B. Xue, Y. Du and J. Zhang, “Enhanced Photocatalytic Activity of Titania-Silica Mixed Oxide Prepared via Basic Hydrolyzation,” Materi- als Science and Engineering B, Vol. 112, No. 1, Septem- ber 2004, pp. 34-41. [43] H. Paldan, S. Areva, T. Tirri, T. Peltola, T. Lindholm, L. Lassila, L. Pelliniemi, R.-P. Happonen and T. Närhi, “Soft Tissue Attachment on Sol-Gel-Treated Titanium Implants In Vivo,” Journal of Materials Science: Materials in Medicine, Vol. 19, No. 3, March 2008, pp. 1283-1290. |

