 Open Journal of Ophthalmology, 2012, 2, 71-77 http://dx.doi.org/10.4236/ojoph.2012.23015 Published Online August 2012 (http://www.SciRP.org/journal/ojoph) 71 Childhood Glaucoma: An Overview Parul Singh, Yogesh Kumar, Manoj Tyagi, Krishna Kuldeep, Parmeshwari Das Sharma Department of Ophthalmology, Veer Chandra Singh Garhwali Government Medical Sciences and Research Institute, Srinagar, India. Email: parulophtha@gmail.com Received March 16th, 2012; revised April 27th, 2012; accepted May 28th, 2012 ABSTRACT Several types of childhood glaucoma exist, and the terminology is based on the time of onset of disease and its potential cause. Though childhood glaucoma occurs less commonly than adults but can lead to permanent visual damage due to amblyopia, optic neuropathy or refractive error. A detailed evaluation should be done to establish diagnosis. Medical therapy has a limited role and surgery remains main modality for treatment. Childhood glaucoma is a treatable disease, if early diagnosis is established and therapeutic intervention done in time. In children with low vision efforts should be there to maintain residual vision and visual rehabilitation with low vision aids should be done. Keywords: Childhood Glaucoma; Goniotomy; Trabeculotomy 1. Introduction Glaucoma is less common in children than in adults. Al- though glaucoma can lead to permanent visual damage at any age, the consequences of the disease are more often severe in children due to additional damage that can happen to the developing visual system. Associated am- blyopia and secondary refractive errors are common. Primary congenital glaucoma (PCG) is hereditary child- hood glaucoma secondary to abnormal development of the filtration angle. Nonetheless, most ophthalmologists usually encounter the wide range of secondary forms of glaucoma in this age group. Glaucoma surgery has dras- tically improved the visual prognosis of children afflicted with glaucoma. However, late diagnosis of the condition can result in permanent and severe visual morbidity. Its affliction of young children makes glaucoma control a life-long goal requiring motivation and perseverance by patients, their parents and doctors. This article is in- tended to provide an overview of the disease at genetic levels, newer technological tools assisting in diagnosis, IOP lowering medications and refined surgical tech- niques. 1.1. Definition and Terminology Relating to age of onset 1) Congenital glaucoma: The glaucoma that exists at birth, and usually before birth; 2) Infantile glaucoma: Glaucoma that occurs from birth until 3 years of age; 3) Juvenile glaucoma: Occurs after the age of three to teenage years. Relating to deve lopment pattern 1) Developmental glaucoma: This term broadly en- compasses all glaucomas resulting from abnormal de- velopment of the aqueous outflow system. This may or may not be associated with systemic anomaly; 2) Primary developmental glaucoma: This is the glau- coma resulting from maldevelopment of aqueous outflow system; 3) Secondary developmental glaucoma: This refers to glaucoma resulting from damage to aqueous outflow system due to maldevelopment of some other portion of the eye, e.g. eye with microspherophakia or dislocated lens. Relating to anatomy Hoskins classified developmental glaucoma anatomi- cally by the structures involved: 1) Trabecular meshwork: Trabeculodysgenesis; 2) Iris and trabecular meshwork: Iridotrabeculodys- genesis; 3) Cornea and trabecular meshwork: Corneotrabecu- lodysgenesis [1]. 1.2. Classification of Congenital and Infantile Glaucoma Primary congemital glaucoma (Trabeculodysgenesis) Secondary congenital glaucoma 1) Iridocorneotrabeculodysgenesis a) Rieger’s anamoly; b) Axenfeld anamoly; c) Peter’s anamoly. 2) Iridotrabeculodysgenesis Copyright © 2012 SciRes. OJOph  Childhood Glaucoma: An Overview 72 a) Stromal defects: Hypoplasia, hyperplasia; b) Anomalous iris vessels: Persistence of tunica vas- culosa lenti; c) Structural anamolies: Holes, coloboma, aniridia; Acquired glaucomas 1) Aphakia; 2) Corticosteroid induced; 3) Retinoblastoma; 4) Traumatic; 5) Uveitis. 2. Epidemiology Primary congenital glaucoma is hereditary with a vari- able incidence in different populations, but an overall occurrence of 1 in 10,000 births is seen [2]. A greater incidence occurs in populations with higher rates of con- sanguinity [3,4]. Boys are more commonly affected in United States and Europe with boys to girls ratio of 3:2. Whereas, in Japan more girls are seen having this condi- tion [5,6]. The majority (about 75%) of PCG cases are bilateral and asymmetric expression should be suspected in clinically apparent unilateral cases. More than 80% patients present within the first year of life, with 25% diagnosed in the neonatal period and 60% within the first 6 months of life [7]. 3. Genetics The majority of PCG cases are sporadic but 10% - 40% are familial with frequent association with consanguinity [8]. In the most familial cases, transmission is autosomal recessive with variable expression and penetrance of 40% - 100% [8]. Genetic heterogenicity of PCG confirmed by linkage studies explain discrepancies like unequal sex distribu- tion, lower than expected number of affected siblings in familial cases, and transmission of the disease to success- sive generations [8]. Three loci for PCG have been found [8-10]. The initial locus on chromosome 2p21 (GLC3A) was described in 1995 by Sarfarazi et al. who identified significant genetic linkage to this region in 11 of 17 turk- ish families [8,11]. Genetic heterogenicity was confirmed when a second locus on chromosome 1p36 (GLC3B) was found [9]. Genetic family analysis identified a third locus GLC3C on chromosome 14q24.3 [10]. Although three chromosomal loci have been linked to PCG, only CYP1B1 in locus GLC3A has been identified [12]. Mu- tations in these genes have been described as the pre- dominant cause of PCG in Turkish and Saudi arabian families [13]. It has been reported that 87% of familial and 27% sporadic case are due to mutation in this gene [8]. Approximately 45 mutations of this gene have been identified and include deletion, insertion, point mutation, mis-sense, non-sense, frameshift and terminator mutation [14]. From all mutations studied, frameshift and R390C homozygous mutations were associated with severe phe- noltype and very poor prognosis. Primary juvenile glau- coma can be inherited in an autosomal dominant fashion. A mutation in the chromosome 1q23-25 region has been linked to this disease [15,16]. Genetic studies have also been conducted on few other glaucomas. In Axenfeld, Rieger anomaly, the gene has been mapped to chromo- some 6p25 [17]. In aniridia, the most common inheri- tance pattern is autosomal dominant. The genetic locus for aniridia has been established as the PAX6 gene, lo- cated on 11p13 [18]. 4. Pathogenesis The exact mechanism involved in pathophysiology of primary infantile glaucoma is not known. One theory said that a pathologic membrane (known as Barkan’s membrane) [19] covered and blocked the trabecular meshwork in primary infantile glaucoma. Clinical and histopathologic observations of the anterior chamber in infantile glaucoma have revealed that the anatomic rela- tionship between the iris, trabecular meshwork and ciliary body are immature. The principal defect in pri- mary infantile glaucoma is a failure of one or more steps in the normal development of the anterior chamber angle. As the genes associated with primary infantile glau- coma are characterized further and the physiological or developmental role of the proteins they encode become better understood; the molecular, cellular and embryo- logical pathophysiology of this rare disorder will become clear [12]. Among the secondary glaucomas of childhood, the underlying pathophysiology is as varied as that in adults. Occurrence at or shortly after birth indicates a profound developmental abnormality of anterior chamber angle whereas, manifestation later usually suggests a different process. Secondary open angle also occur in young children. Both corticosteroid-induced and chronic uveitic glauco- mas are described [20]. It is difficult to classify the un- derlying cause of glaucoma, that frequently follows pe- diatric cataract extraction. Walton examined 65 children in whom, pre-operative gonioscopy revealed no consis- tent angle defect but post-operative gonioscopy revealed filtration angle deformity [21]. Retained lens material was one of the risk factor known another cause may be presence of small cornea. 5. Presentation The signs and symptoms of PCG are variable dependent on child’s age and severity of glaucoma; and secondary corneal abnormalities. PCG is characterized by clinical triad of epiphora, blepharospasm and photophobia, but Copyright © 2012 SciRes. OJOph  Childhood Glaucoma: An Overview 73 these symptoms are often missed until the more alarming corneal edema becomes apparent. The corneal edema, may be subtle, especially in bilateral cases; or profound with enlarged corneal diameter and globe, breaks in De- scemet’s membrane (Haab’s striae) and sometimes even acute hydrops. Myopia is typical finding in infantile glaucoma. In older children, astigmatism and progressive axial myopia cause symptomatic decreased uncorrected visual acuity and refractive amblyopia. Optic neuropathy is the most concerning consequence from glaucoma, because the neuropathy is irreversible once axonal death has occurred. While cupping of the optic nerve in glaucoma is gen- erally a gradual process in older children and adults, it can occur rapidly in infants. Reversibility of the cupping with normalization of the intra-ocular pressure (IOP) in young children occurs due to suspected relative immatur- ity and elasticity of lamina cribrosa. Less common pre- senting signs in infantile glaucoma include conjunctivitis, blepharitis and cellulitis. 6. Diagnosis and Ancillary Testing It is important to do a complete ophthalmic examination in a child suspected of glaucoma. This includes IOP measurement, gonioscopy, optic nerve head examination and refraction. Check for the child’s ability to fix and follow; and for the presence of nystagmus. Examination of the cornea is crucial with respect to size and clarity of the cornea and the presence of Haab’s striae. This examination can be done in clinic. With some practice, IOP can be measured in a conscious, swaddled infant using perkin’s tonometer or tonopen. Usually IOP in infants with normal eyes is in the range of 11 - 14 mm Hg using these devices. The measurement of IOP greater than 20 mmHg in a calm, resting infant is suspicious for glaucoma when other signs and symptoms also suggest the disease. Measurements of IOP undertaken while a child cries and resists efforts to hold the eye open are invalid. Examination of the optic nerve is attempted, because obvious cupping confirms the diagnosis. Shaffer and Hetherington noted a cup to disc ratio (C/D ratio) greater than 0.3 in 68% of 126 eyes affected by primary infantile glaucoma [22], whereas C/D ratio greater than 0.3 was found in less than 2.6% of newborns with normal eyes [23]. A Koeppe infant diagnostic lens offers good visu- alization of disc using direct ophthalmoscope. Gonio- scopy can also be performed with it even in a conscious infant. In the normal newborn eye, the iris usually inserts posterior to the scleral spur. In PCG, the iris commonly inserts anteriorly directly into the trabecular meshwork. This iris insertion is most commonly flat, although con- cave insertion may be rarely seen. If the diagnosis of glaucoma is confirmed or strongly suspected based on clinical examination, an examination under anaesthesia is required. Unfortunately, most anes- thetic agents and sedatives have lowering effect on IOP [24]. Tonometry should be best performed as soon as possible after induction of anesthesia. Corneal diameters are measured with a millimeter ruler or caliper and re- corded. Detailed hand slit lamp examination of anterior segment is followed by gonioscopy and fundus examina- tion. Visual field defects are similar to those seen in adults with initial predilection for loss in arcuate areas, but child should be able to follow directions for field exami- nation (perimetry). Although the technology has been around and algorithm is getting better and better, it is still difficult to apply them in children as they may not follow instructions or may not cooperate. Optical coherence tomography may be a better option and much easier as compared to visual field examination in young and non- cooperative patients. 7. Differential Diagnosis Signs and symptoms Condition Tearing, discharge, conjunctival injection Nasolacrimal duct obstruction infections Allergic conjunctivitis Cloudy cornea, loss of corneal lusture, Haab’s striae Corneal dystrophy e.g. CHED, PPMD Forcep trauma Cysticercosis Sclerocornea Mucopolysaccharidosis I, Is, II, III infectious keratitis Enlarged cornea, apparent asymmetry of globe size Primary megalocornea Unilateral high myopia Proptosis lid retraction Contralateral microphthalmos Enopthalmos ptosis Photophobia, blepharospasm Uveitis corneal infection, abrasion or dystrophy Retinal cone dystrophy High myopia Pathologic myopia Vitreo-retinal degeneration e.g. Stickler’s syndrome Enlarged cup to disc ratio Physiologic optic nerve cupping optic nerve atrophy or anomaly Copyright © 2012 SciRes. OJOph 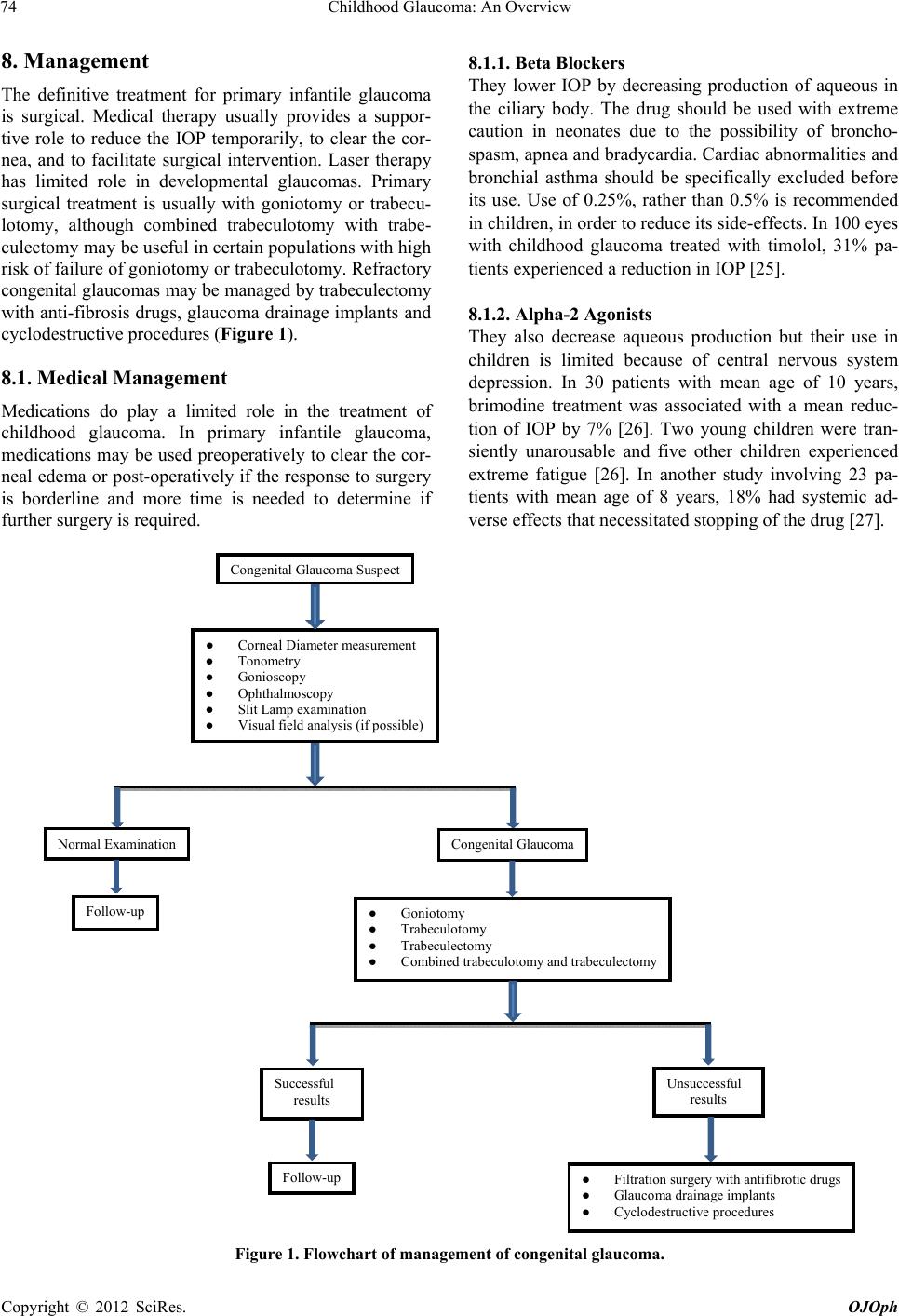 Childhood Glaucoma: An Overview Copyright © 2012 SciRes. OJOph 74 8. Management 8.1.1. Beta Blockers They lower IOP by decreasing production of aqueous in the ciliary body. The drug should be used with extreme caution in neonates due to the possibility of broncho- spasm, apnea and bradycardia. Cardiac abnormalities and bronchial asthma should be specifically excluded before its use. Use of 0.25%, rather than 0.5% is recommended in children, in order to reduce its side-effects. In 100 eyes with childhood glaucoma treated with timolol, 31% pa- tients experienced a reduction in IOP [25]. The definitive treatment for primary infantile glaucoma is surgical. Medical therapy usually provides a suppor- tive role to reduce the IOP temporarily, to clear the cor- nea, and to facilitate surgical intervention. Laser therapy has limited role in developmental glaucomas. Primary surgical treatment is usually with goniotomy or trabecu- lotomy, although combined trabeculotomy with trabe- culectomy may be useful in certain populations with high risk of failure of goniotomy or trabeculotomy. Refractory congenital glaucomas may be managed by trabeculectomy with anti-fibrosis drugs, glaucoma drainage implants and cyclodestructive procedures (Figure 1). 8.1.2. Alph a- 2 Ago n i sts They also decrease aqueous production but their use in children is limited because of central nervous system depression. In 30 patients with mean age of 10 years, brimodine treatment was associated with a mean reduc- tion of IOP by 7% [26]. Two young children were tran- siently unarousable and five other children experienced extreme fatigue [26]. In another study involving 23 pa- tients with mean age of 8 years, 18% had systemic ad- verse effects that necessitated stopping of the drug [27]. 8.1. Medical Management Medications do play a limited role in the treatment of childhood glaucoma. In primary infantile glaucoma, medications may be used preoperatively to clear the cor- neal edema or post-operatively if the response to surgery is borderline and more time is needed to determine if further surgery is required. Con enital Glaucoma Sus ect Normal Examination Congenital Glaucoma ● Corneal Diameter measurement ● Tonometry ● Gonioscopy ● Ophthalmoscopy ● Slit Lamp examination ● Visual field analysis (if possible) Follow-up ● Goniotomy ● Trabeculotomy ● Trabeculectomy ● Combined trabeculotomy and trabeculectomy Successful results Follow-up Unsuccessful results ● Filtration surgery with antifibrotic drugs ● Glaucoma drainage implants ● Cyclodestructive procedures Figure 1. Flowchart of management of congenital glaucoma.  Childhood Glaucoma: An Overview 75 8.1.3. Carbonic Anhydrase Inhibitors (CAIs) They suppress aqueous production and are available as either an oral formulation or as topical drop. The oral formulation may be more effective in IOP lowering but also produces more side-effects of diarrhea, lethargy, poor appetite and metabolic acidosis [28]. The mean was reduced by 36% and 27% compared with baseline, after treatment with acetazolamide and topical dorzolamide, respectively. All eyes showed an increase in IOP when switched from acetazolamide to dorzolamide with mean increase of 3.7mmHg [29]. Topical CAI can be expected to have additive benefit when used in conjunction with beta-blockers [30]. 8.1.4. Pros t aglandins Ana logues These drugs reduce IOP by enhancing uveo-scleral out- flow [31]. Their side-effects include conjunctival hy- peremia, iris and skin pigmentation and accelerated eye- lash growth. High non-response rate has been reported in children with little IOP lowering in responders [32]. 8.1.5. Mio t i c s They are ineffective for PCG, but can be used pre- operatively before angle surgery. 8.2. Surgical Treatment Early surgical intervention is of prime importance in the management of patients with PCG. Either goniotomy or trabeculotomy is the procedure of choice; goniotomy requires clear cornea while trabeculotomy may be per- formed if cornea is hazy or opaque. When greater chances of failure are present, trabeculotomy may be combined with trabeculectomy. 8.2.1. Goni o to m y A blade is inserted through the peripheral cornea 180˚ across from meshwork to be incised (usually the nasal or the temporal portions) and is then guided across the ante- rior chamber into the chamber angle. With the aid of go- nioscopy lens, the trabecular meshwork is visualized, and the blade is used to make a linear incision through the meshwork for approximately one third of the circumfer- ence of eye. The reported rate of success of goniotomy in infantile glaucoma is 80% [33]. Endoscopic goniotomy has been successfully performed utilizing a co-axial ocu- lar endoscope in presence of corneal opacification, which prevented standard goniotomy procedure [34]. 8.2.2. Trabeculotomy A scleral flap is created over the area of network to be incised. Through this flap a dissection into schlemm’s canal is created. A trabeculotome is inserted into the ca- nal and the meshwork is then opened, as instrument is rotated into the anterior chamber. Considering congenital glaucoma of all grades of severity, trabeculotomy con- trols IOP in over 90% of eyes. The efficacy of this opera- tion compared favorably with goniotomy. The results of trabeculotomy and goniotomy for infantile glaucoma were compared and found equally effective and safe [35]. The significant advantage of trabeculotomy for those cases with a cloudy cornea limiting visualization of the angle was described [36]. A newer trabeculotomy tech- nique with protein suture passed 360˚ through Schlemm’s canal has been mentioned [37]. 8.2.3. Trabeculectomy A trabeculectomy involves creating a full thickness opening in the sclera (sclerotomy) for outflow of aqueous. A partial thickness scleral flap covers the opening and the conjunctiva overlies the flap. Intraocular pressure can be significantly lowered with this. Success rate in adults is usually around 70% - 80%. In children, long term suc- cess rate is lower being around 50% [38] due to more aggressive wound healing response in children, which scars down sclerotomy or scleral flap. Children are also more prone to complications such as infections due to eye rubbing. 8.3. Management of Refractory Pediatric Glaucomas (Figure 1) When the IOP is not controlled after the first surgery, the surgical options are filtration surgery with anti-fibrosis drugs; glaucoma drainage implants or cyclodestructive procedures. 8.3.1. Trabeculectomy with Anti-Fibrotic Agents Mitomycin-C and 5-Florouracil are the two most com- monly used anti-metabolites in glaucoma surgery. Al- though each of these medications decrease the scarring of blebs, they also create more potential for complications such as infection (endopthalmitis) [39-42]. 8.3.2. Aqueous Drainage Implants Implant surgery is an important treatment alternative for PCG patients who are poor candidates for angle incision therapy and trabeculectomy or who have proven to be refractory to these procedures. Glaucoma drainage im- plants may be characterized as non-restrictive devices such as Molteno and Baerveldt implants or valved such as krupin implants or Ahmed glaucoma valve. Reported complications of implants include hypotony with shallow anterior chamber, choroidal detachments, tube cornea touch, obstructed tube or plate, endophthalmitis and reti- nal detachment. The surgical procedure is same for all implants [43]. The superior temporal quadrant is the preferred site. Fol- lowing periotomy, the implant device is placed with its anterior edge approximately 8mm from limbus. The tube Copyright © 2012 SciRes. OJOph  Childhood Glaucoma: An Overview 76 is shortened and beveled and an incision is made into the anterior chamber to allow entry of tube parallel to iris. The tube is then protected with autologous sclera or pericardium and limbal peritomy is closed. 8.3.3. Cyclode s tructive Procedures These are selectively used for PCG which has proven refractory to medical therapy and to conventional surgi- cal procedures to improve aqueous outflow and work by decreasing aqueous production. The required ciliary epithelial ablation is produced by trans-scleral cyclocryo- therapy or by endoscopic diode laser cyclophotocoagula- tion. The ocular indications include a blind painful eye, a blind eye with high pressure, rapidly deteriorating cornea refractory to all treatment alternatives and, an eye with anatomic defect which preclude other glaucoma proce- dures. 8.4. Low Vision Rehabilitation Regrettably, children with congenital glaucoma may end up with low vision despite treatment. Various low vision aids such as magnifiers, binoculars, telescopes are avail- able for such patients to improve their quality of life. Some non-optical devices such as close circuit televi- sions, large print books exist for their help. Such patients should receive special care and vocational training from trained professionals, working specifically for visually impaired patients, in order to help them develop their abilities to maximum potential [44]. 9. Conclusion The main goal in managing primary congenital glaucoma is early diagnosis and therefore early surgical interven- tion. Following successful surgery, glasses should be prescribed and care must be taken to manage amblyopia for optimal visual rehabilitation. REFERENCES [1] D. H. Hoskins, R. N. Shaffers and J. Hetherington, “Ana- tomical Classification of the Developmental Glaucomas,” Archives of Ophthalmology, Vol. 102, No. 9, 1984, pp. 1331-1336. doi:10.1001/archopht.1984.01040031081030 [2] S. J. H. Miller, “Genetic Aspects of Glaucoma,” Transac- tions of the Ophthalmological Society of the UK, Vol. 86, 1966, pp. 425-434. [3] S. C. Debnath, K. D. Teichmann and K. Salamah, “Tra- beculectomy versus Trabeculotomy in Congenital Glau- coma,” British Journal of Ophthalmology, Vol. 73, No. 8, 1989, pp. 608-611. doi:10.1136/bjo.73.8.608 [4] A. Gencik, “Epidemiology and Genetics of Primary Con- genital Glaucoma in Slovakia. Description of a Form of Primary Congenital in Gypsies with Autosomal-Reces- sive Inheritance and Complete Penetrance,” Develop- ments in Ophthalmology, Vol. 16, 1989, pp. 76-115. [5] V. P. DeLuise and D. R. Anderson, “Primary Infantile Glaucoma (Congenital Glaucoma),” Survey of Ophthal- mology, Vol. 28, No. 1, 1983, pp. 1-19. doi:10.1016/0039-6257(83)90174-1 [6] R. N. Shaffer, “Genetics and the Congenital Glaucomas,” American Journal of Ophthalmology, Vol. 60, 1965, pp. 981-994. [7] A. E. Kolker and J. Hetherington, “Congenital Glau- coma,” In: Becker-Shaffer’s Diagnosis and Therapy of the Glaucomas, 5th Edition, CV Mosby, St Louis, 1983, p. 317 [8] M. Sarfarazi and I. Stoilov, “Molecular Genetics of Pri- mary Congenital Glaucoma,” Eye, Vol. 14, 2000, pp. 422- 428. doi:10.1038/eye.2000.126 [9] A. N. Akarsu, M. E. Turacli, S. G. Aktan, et al., “A Sec- ond Locus (GLC3C) for Primary Glaucoma (Buphthal- mos) Maps to the 1p36 Region,” Human Molecular Ge- netics, Vol. 5, No. 8, 1996, pp. 1199-1203. doi:10.1093/hmg/5.8.1199 [10] I. R. Stoilov and M. Sarfarazzi, “The Third Genetic Locus (GLC3C) for Primary Congenital Glaucoma (PCG) Maps to Chromosome 14q24.3,” Investigative Ophthalmology & Visual Science, Vol. 43, 2002, pp. 1820-1827. [11] M. Sarfarazi, A. N. Arkarsu, A. Hossain, et al., “Assign- ment of a Locus (GLC3A) for Primary Congenital Glau- coma (Buphthalmos) to 2p21 and Evidence for Genetic Heterogeneity,” Genomics, Vol. 30, No. 2, 1995, pp. 171- 178. doi:10.1006/geno.1995.9888 [12] I. Stoilov, A. Nurten and M. Sarfarazi, “Identification of Three Different Truncating Mutations in Cytochrome P4501B1 (CYP1B1) as the Principal Cause of Primary Congenital Glaucoma in Families Linked to the GLC3A on Chromosome 2p21,” Human Molecular Genetics, Vol. 6, No. 4, 1997, pp. 641-647. doi:10.1093/hmg/6.4.641 [13] B. A. Bejjani, R. A. Lewis, T. F. Tomey, et al., “Muta- tions in CYP1B1, the Gene for Cytochrome P4501B1, Are the Predominant Cause of Primary Congenital Glau- coma in Saudi Arabia,” American Journal of Human Ge- netics, Vol. 62, No. 2, 1998, pp. 325-333. doi:10.1086/301725 [14] S. G. Panicker, A. N. Mandal, A. B. M. Reddy, V. K. Gothwal and S. E. Hasnain, “Correlations of Genotype with Phenotype in Indian Patients with Primary Congeni- tal Glaucoma,” Investigative Ophthalmology & Visual Science, Vol. 45, No. 4, 2004, pp. 1149-1156. [15] A. T. Johnson, A. V. Drack, A. E. Kwitek, et al., “Clini- cal Features and Linkage Analysis of a Family Autosomal Dominant Juvenile Glaucoma,” Ophthalmology, Vol. 100, No. 4, 1993, pp. 524-529. [16] V. C. Sheffield, E. M. Stone, W. L. M. Alward, et al., “Genetic Linkage of Familial Open Angle Glaucoma to Chromosome 1q21-q31,” Nature Genetics, Vol. 4, No. 1, 1993, pp. 47-50. doi:10.1038/ng0593-47 [17] D. B. Gould, A. J. Mears, W. G. Pearce and M. A. Walter, “Autosomal Dominant Axenfeld-Rieger Anomaly Maps to 6p25,” American Journal of Human Genetics, Vol. 61, No. 3, 1997, pp. 765-768. Copyright © 2012 SciRes. OJOph  Childhood Glaucoma: An Overview Copyright © 2012 SciRes. OJOph 77 doi:10.1016/S0002-9297(07)64340-7 [18] T. Glaser, D. S. Walton and R. L. Mass, “Genomic Struc- ture, Evolutionary Conservative and Aniridia Mutations in the Human PAX6 Gene,” Nature Genetics, Vol. 2, No. 3, 1992, pp. 232-239. doi:10.1038/ng1192-232 [19] O. Barkan, “Pathogenesis of Congenital Glaucoma,” American Journal of Ophthalmology, Vol. 40, 1955, pp. 1-11. [20] I. Tugal-Tutkun, K. Havrlikova, W. J. Power and C. S. Foster, “Changing Patterns in Uveitis of Childhood,” Ophthalmology, Vol. 103, No. 3, 1996, pp. 375-383. [21] D. S. Walton, “Pediatric Aphakic Glaucoma: A Study of 65 Patients,” Transactions of the American Ophthal- mological Society, Vol. 93, 1995, pp. 403-413. [22] R. N. Shaffer and J. Hetherington Jr., “The Glaucomatous Disc in Infants. A Suggested Hypothesis for Disc Cup- ping,” Transactions of the American Academy of Oph- thalmology & Otolaryngology, Vol. 73, No. 5, 1969, pp. 923-935. [23] K. T. Richardson and R. N. Shaffers, “Optic-Nerve Cup- ping in Congenital Glaucoma,” American Journal of Ophthalmology, Vol. 62, No. 3, 1966, pp. 507-509. [24] R. N. Jaffar and A. K. Ghulamqadir, “Effect of Oral Cho- ral Hydrate on the Intraocular Pressure Measurement,” Journal of Pediatric Ophthalmology and Strabismus, Vol. 30, No. 6, 1993, pp. 372-376. [25] H. D. Hoskins Jr., J. Hetherington Jr., S. D. Magee, R. Naykhin and C. V. Migliazzo, “Clinical Experience with Timolol in Childhood Glaucoma,” Archives of Ophthal- mology, Vol. 103, No. 8, 1985, pp. 1163-1165. doi:10.1001/archopht.1985.01050080075024 [26] L. B. Enyedi and S. F. Freedman, “Safety and Efficacy of Brimonidine in Children with Glaucoma,” Journal of AAPOS, Vol. 5, No. 5, 2001, pp. 281-284. doi:10.1067/mpa.2001.117571 [27] R. J, Bowman, J, Cope and K, K. Nischal, “Ocular and Systemic Side-Effects of Brimonidine 0.25% Eye Drops (Alphagan in Children),” Eye, Vol. 18, 2004, pp. 24-26. doi:10.1038/sj.eye.6700520 [28] L. I. Larsson and A. Alm, “Aqueous Humor Flow in Hu- man Eyes Treated with Dorzolamide and Different Doses of Acetazolamide,” Archives of Ophthalmology, Vol. 116, No. 1, 1998, pp. 19-24. [29] M. Portellos, E. G. Buckley and S. F. Freedman, “Topical versus Oral Carbonic Anhydrase Inhibitor for Pediatric Glaucoma,” Journal of AAPOS, Vol. 2, No. 1, 1998, pp. 43-47. doi:10.1016/S1091-8531(98)90109-4 [30] L. L. Wayman, L. I. Larsson, T. L. Maus and R. F. Bru- baker, “Additive Effect of Dorzolamide on Aqueous Hu- mor Flow in Patients Receiving Long Term Treatment with Timolol,” Archives of Ophthalmology, Vol. 116, No. 11, 1998, pp. 1438-1440. [31] R. K. Parrish, P. Palmberg and W. P. Sheu, “A Compari- son of Latanoprost, Bimatoprost and Travoprost in Pa- tients with Elevated Intraocular Pressure: A 12-Week, Randomized, Masked-Evaluator Multicenter Study,” Ameri- can Journal of Ophthalmology, Vol. 135, No. 5, 2003, pp. 688-703. doi:10.1016/S0002-9394(03)00098-9 [32] L. B. Enyedi, S. F. Freedman and E. G. Buckley, “The Effectiveness of Latanoprost for the Treatment of Pediat- ric Glaucoma,” Journal of AAPOS, Vol. 3, No. 1, 1999, pp. 33-39. doi:10.1016/S1091-8531(99)70092-3 [33] K. S. Morgan, B. Black, F. D. Ellis and E. M. Helveston, “Treatment of Congenital Glaucoma,” American Journal of Ophthalmology, Vol. 92, 1981, pp. 799-803. [34] K. M. Joos and J. H. Shen, “An Ocular Endoscope En- ables a Goniotomy Despite a Cloudy Cornea,” Archives of Ophthalmology, Vol. 119, No. 1, 2001, pp. 134-135. [35] S. D. McPherson Jr. and D. MacFarland, “External Tra- beculotomy for Developmental Glaucoma,” Ophthalmol- ogy, Vol. 87, No. 4, 1980, pp. 302-305. [36] S. D. McPherson Jr. and D. P. Berry, “Goniotomy vs External Trabeculotomy for Developmental Glaucoma,” American Journal of Ophthalmology, Vol. 95, No. 4, 1983, pp. 427-431. [37] A. D. Beck and M. G. Lynch, “360 Degrees Trabecu- lotomy for Congenital Glaucoma,” Archives of Ophthal- mology, Vol. 113, No. 9, 1995, pp. 1200-1202. doi:10.1001/archopht.1995.01100090126034 [38] G. R. Beauchamp and M. M. Parks, “Filtering Surgery in Children: Barriers to Success,” Ophthalmology, Vol. 86, No. 1, 1979, pp. 170-180. [39] A. K. Mandal, D. S. Walton, T. John, et al., “Mitomycin C Augmented Trabeculectomy in Refactory Congenital Glaucoma,” Ophthalmology, Vol. 104, No. 6, 1997, pp. 996-1003. [40] R. Susanna, E. W. Oltrogge, J. C. E. Carani, et al., “Mi- tomycin as Adjunct Chemotherapy with Trabeculectomy in Congenital and Developmental Glaucomas,” Journal of Glaucoma, Vol. 4, No. 3, 1995, pp. 151-157. doi:10.1097/00061198-199506000-00002 [41] S. Waheed, D. C. Ritterband and D. S. Greenfield, “Bleb- Related Ocular Infection in Children after Trabeculec- tomy with Mitomycin C,” Ophthalmology, Vol. 104, No. 12, 1997, pp. 2117-2120. [42] M. Zalish, H. Leiba and M. Oliver, “Subconjunctival Injection of 5-Fluorouracil Following Trabeculectomy for Congenital and Infantile Glaucoma,” Ophthalmic Surgery, Vol. 23, No. 3, 1992, pp. 203-205. [43] M. Akimato, H. Tamihara, A. Negi and M. Nagata, “Sur- gical Results of Trabeculotomy ab Externo for Develop- mental Glaucoma,” Archives of Ophthalmology, Vol. 112, No. 12, 1994, pp. 1540-1544. [44] A. K. Mandal and D. Chakrabarti, “Update on Congenital Glaucoma,” Indian Journal of Ophthalmology, Vol. 59, No. 7, 2011, pp. 148-157. doi:10.4103/0301-4738.73683
|