Journal of Cancer Therapy
Vol.3 No.3(2012), Article ID:19938,4 pages DOI:10.4236/jct.2012.33026
Cardiac Mass and Hypertrophic Cardiomyopathy as Aggressive Presentation of Primary Cardiac Lymphoma: A Case Report*
![]()
1Department of Critical Care Medicine, Maimonides Medical Center, New York, USA; 2Department of Medicine, Maimonides Medical Center, New York, USA; 3Department of Cardiology, Maimonides Medical Center, New York, USA.
Email: #evbuenakpene@gmail.com
Received February 23rd, 2012; revised March 25th, 2012; accepted April 7th, 2012
Keywords: Primary Cardiac Lymphoma; Asymmetric Left Ventricular Hypertrophy; Chemotherapy
ABSTRACT
Primary cardiac lymphoma is very rare. This disease occurs mainly in immunocompromised patients and rarely in the immunocompetent. With the advent of echocardiogram, computed tomography and magnetic resonance imaging, more cases are being diagnosed ante-mortem although the prognosis still remains poor. These cardiac tumors provide unique diagnostic and therapeutic challenges. We present an interesting case of primary cardiac lymphoma diagnosed antemortem in an 81 year old immunocompetent female presenting as a large mass in the right atrium, right ventricle and encasing the right coronary artery; and asymmetric left ventricular hypertrophy, a variant of hypertrophic cardiomyopathy. Patient responded very well to chemotherapy with subsequent regression of the cardiac mass and ventricular hypertrophy.
1. Introduction
Primary malignant cardiac tumors are rare, with the most common being sarcomas. Primary cardiac lymphoma (PCL) comprises about 0.5% of all lymphomas and occurs generally in the right atrium and ventricle [1]. PCL most commonly are diffuse B-cell lymphomas and are more common in males with a mean age of 67 years at presentation [2]. With the advent of echocardiogram, computed tomography and magnetic resonance imaging more cases are being diagnosed ante-mortem although the prognosis still remains poor [2]. The incidence has also increased in immunocompromised patients especially with Acquired Immunodeficiency Syndrome (AIDS) and have a poorer outcome. PCL patients can present with chest pain, shortness of breath, pulmonary edema, arrythymias, atrioventricular blocks, left ventricular hypertrophy [3,4]. We present an interesting case of PCL diagnosed antemortem in an 81 year old immunocompetent female presenting as a large mass in the right atrium, right ventricle and encasing the right coronary artery; and asymmetric left ventricular hypertrophy, a variant of hypertrophic cardiomyopathy.
2. Case Report
An 81-year-old female with no significant past medical history presented with 2 week history of increasing dyspnea on exertion and fatigue. She denied any chest pain, palpitations, fever, cough or recent travel. She had lost about 8 pounds over the last 1 month. Human Immunodeficiency Virus (HIV) test was negative. An echocardiogram (Figure 1) revealed a lobulated mass 5 × 4 × 3 cm attached to the tricuspid valve, extending into the right atrium, right ventricle, asymmetric left ventricular hypertrophy, moderate pericardial effusion and ejection fraction of 65%. Magnetic resonance imaging (MRI), (Figure 2) showed similar findings with the mass attached to the tricuspid valve, projecting into the right atrium and right ventricle, infiltrating the walls of the right atrium and right ventricle, and the mass surrounding the coronary sinus, atrioventricular groove and encasing the right coronary artery. An enlarged lymph node was also noted in the anterior mediastinum. Computed tomography (CT) scan and Positron Emission Tomography (PET) scan showed no other focus. Diagnosis of diffuse large B cell Lymphoma was made with the biopsy and immunohistochemical staining of the lymph node. Patient was started on cyclophosphamide, doxorubicin, vincristine, prednisone and rituximab (R-CHOP) regimen and followed with serial echocardiograms. She received 6 cycles of chemotherapy with regression of disease and remains in remission for 13 months. Serial echocardiograms were used for documenting the regression of mass
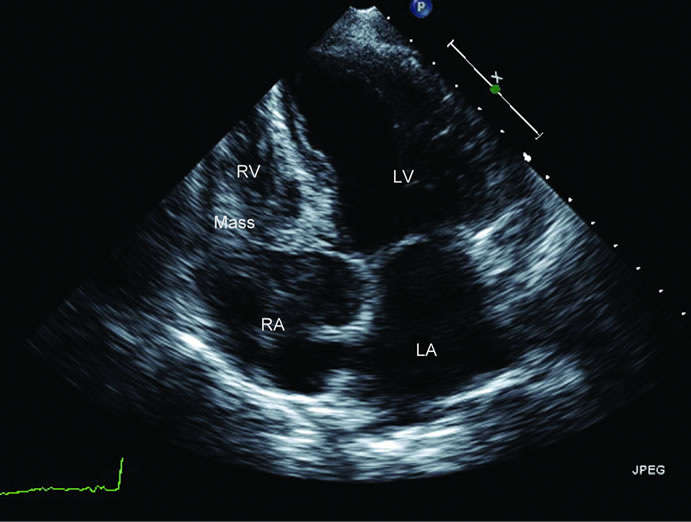
Figure 1. Transthoracic Echocardiography showing large irregular inhomogeneous mass measuring 5 × 4 × 3 cm in right heart adjacent to tricuspid valve and infiltrating the walls of RA and RV. (RA—right atrium, RV—right ventricle, LA—left atrium, LV—left ventricle).
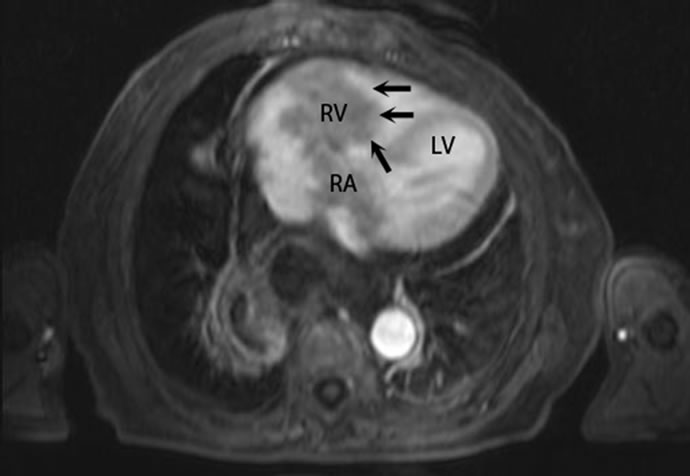
Figure 2. Magnetic resonance imaging showing large lobulated mass attached to the tricuspid valve. Mass projects into right atrium and right ventricle. (RA—right atrium, RV—right ventricle, LV—left ventricle.
and asymmetric left ventricular hypertrophy which completely resolved after chemotherapy.
3. Discussion
Primary cardiac lymphoma is classically defined as an extranodal non-Hodgkin’s lymphoma exclusively located in the heart and/or pericardium and is extremely rare. This disease occurs mainly in immunocompromised patients [5,6] and rarely in the immunocompetent. [3,7,8]. It accounts for 1.3% - 2% of all cardiac tumours and 0.5% of all extranodal lymphomas [1,7,9], but it has been encountered with increasing frequency in patients with Acquired Immune Deficiency Syndrome (AIDS) or other severe immunodepressive syndromes. Most of the reported primary cardiac lymphoma cases are of B-cell origin, while T-cell cardiac lymphomas are much rarer.
Thirty-five cases of primary cardiac non-Hodgkin’s lymphoma were reviewed by Chalabreysse et al. [10], of which twenty-two of these cases were diffuse, large B-cell lymphoma (DLBCL) [10]. Similarly, Pertrich et al. [3] reviewed 197 cases of PCL, with half of all cases reported since 1995. The study is the largest analysis of PCL to date. Diffuse large B-cell lymphoma constituted a majority, and survival in PCL was affected mainly by 4 factors: immune status, left ventricular involvement, presence of extra-cardiac disease, and arrhythmia. Prognosis generally remains poor, however, lack of left ventricular involvement and presence of arrhythmias were associated with improved survival. Mayayo Artal et al. [11] also described PCL among immunocompentent hosts, in which it was observed that Ebstein Barr Virus appears to play no role in the development of PCL, and this finding was also observed in a review by Lee et al. [12].
There have been other reports of immunocompetent patients with diffuse B-cell lymphoma presenting with SVC syndrome [8], cardiac tamponade, life threatening arrhythmias and intractable heart failure. Because of this rapid evolution, the situation represents an oncologic emergency, and therefore early diagnosis and treatment are crucial.
Most cases of cardiac lymphoma are solid, infiltrative nodule tumors in one or multiple chambers. Clinical series by Caresoli et al. [7], and Pertrich et al. and a clinicopathologic series by Chim et al. [13] revealed that primary cardiac lymphoma usually arise in the right chambers as a mass with or without pericardial effusion among >80% of the patients, and the most common presentation was unresponsive heart failure.
Lymphomatous infiltration of pericardium is also seen in a number of cases [2,13]. However the diffuse infiltration in all cardiac chambers along with intracardiac mass is rare and represents an aggressive presentation as seen in our patient. Massive infiltration of the myocardium results in irregular thickening of the walls mimicking hypertrophic cardiomyopathy and is generally associated with malignant lymphoma with spread to the myocardium [3,14]. A case of PCL presenting solely as hypertrophic obstructive cardiomyopathy was described by Lee et al. and diagnosed postmortem [12]. Similarly, Kadhim et al. [5] and Cabin et al. [15] in different case reports described extensive myocardial infiltration causing concentric left ventricular hypertrophy and mimicking hypertrophic cardiomyopathy. A substantial amount of the myocardium was replaced by infiltration of the tumor. The phenomenon of infiltration in these cases are similar to our case, in which there was extensive infiltration involving the right chambers and he right coronary and asymmetric left ventricular hypertrophy however, there was a good response to treatment in our case. We are presenting the first case with right sided large mass and diffuse wall infiltration in an immunocompetent subject, mimicking hypertrophic cardiomyopathy and with good response to chemotherapy.
The clinical symptoms of PCL are nonspecific and related to the location of the tumor. Presentations could be acute including dyspnea, edema, arrhythmias and rarely cardiac wall rupture [7]. Other clinical manifestation includes conduction defects leading to tachyor bradyarrhythmias [6], pericardial effusion and heart failure. Symptoms often include chest pain, exertional dyspnea, palpitations, syncope and other non-specific constitutional symptoms. Diagnosis can be made by echocardiogram, CT and MRI followed by tissue biopsy [7,9]. This case is also interesting as it emphasizes the advantage of echocardiogram for diagnosis and serial follow up.
Lymphomas should be considered in the differential diagnosis of cardiac mass and asymmetrical LV hypertrophy presenting as hypertrophic cardiomyopathy. Because the tumors are largely B-cell lymphomas, they are sensitive to chemotherapy with main regimen as CHOP (cyclophosphamide, doxurubicin, vincristine + prednisone) +/– rituximab [7,13].
The mortality is high due to delay in diagnosis and high relapse rate but survival up to 192 months also has been documented [16]. Extra care is required in the early stage of treatment as tumor lysis may lead to cardiac complications including rupture of the heart or asystole [17].
In conclusion, the diagnosis of primary cardiac lymphoma is difficult due to non-specific clinical manifestations and it should therefore be considered in patients with a cardiac mass with or without pericardial effusion. It is confirmed using imaging modalities such as transthoracic echocardiography and magnetic resonance imaging and certified using cytology or open biopsy. The most effective treatment is chemotherapy, but prognosis remains poor. Definitive approaches to obtain early histological diagnosis are important in order to initiate early treatment.
REFERENCES
- J. M Sarjeant, J. Butany and R. J. Cusimano, “Cancer of the Heart: Epidemiology and Management of Primary Tumors and Metastases,” American Journal of Cardiovascular Drugs, Vol. 3, No. 6, 2003, pp. 407-421. doi:10.2165/00129784-200303060-00004
- H. Ikeda, et al., “Primary Lymphoma of the Heart: Case Report and Literature Review,” Pathology International, Vol. 54, No. 3, 2004, pp. 187-195. doi:10.1111/j.1440-1827.2003.01606.x
- A. Petrich, S. I. Cho and H. Billett, “Primary Cardiac Lymphoma: An Analysis of Presentation, Treatment, and Outcome Patterns,” Cancer, Vol. 117, No. 3, 2.11, pp. 581-589. doi:10.1002/cncr.25444
- K. Tanoue, et al., “Malignant Lymphoma with Various Cardiac Manifestations: A Case Report,” Journal of Cardiology, Vol. 40, No. 3, 2002, pp. 117-123.
- H. Kadhim, et al., “Cardiac Lymphoma Presenting as Concentric Pseudo-Hypertrophic Cardiomyopathy in a Previously Unrecognised Hiv Patient,” Pathology, Vol. 41, No. 7, 2009, pp. 706-709. doi:10.3109/00313020903306082
- Z. Frikha, et al., “Cardiac Tamponade and Paroxysmal Third-Degree Atrioventricular Block Revealing a Primary Cardiac Non-Hodgkin Large B-Cell Lymphoma of the Right Ventricle: A Case Report,” Journal of Medical Case Reports, Vol. 5, 2011, p. 433. doi:10.1186/1752-1947-5-433
- G. L. Ceresoli, et al., “Primary Cardiac Lymphoma in Immunocompetent Patients: Diagnostic and Therapeutic Management,” Cancer, Vol. 80, No. 8, 1997, pp. 1497- 1506. doi:10.1002/(SICI)1097-0142(19971015)80:8<1497::AID-CNCR18>3.0.CO;2-0
- K. P. Cohoon, W. Howe and T. Mc Kiernan, “Primary Cardiac Diffuse, Large B-Cell Lymphoma in an Immunocompetent Patient,” The Journal of Invasive Cardiology, Vol. 20, No. 2, 2008, pp. E59-E60.
- J. J. Monsuez, et al., “Non-Hodgkin’s Lymphoma with Cardiac Presentation: Evaluation and Follow-Up with Echocardiography and MR Imaging,” European Heart Journal, Vol. 12, No. 3, 1991, pp. 464-467.
- L. Chalabreysse, et al., “Primary Cardiac Lymphoma in Immunocompetent Patients: A Report of Three Cases and Review of the Literature,” Virchows Archiv, Vol. 441, No. 5, 2002, pp. 456-461. doi:10.1007/s00428-002-0711-0
- E. M. Artal, et al., “Primary Cardiac Lymphoma: Presentation of Two Cases in Immunocompetent Patients,” Anales de Medicina Interna, Vol. 19, No. 12, 2002, pp. 629-631.
- P. W. Lee, et al., “Images in Cardiovascular Medicine. Diffuse Infiltration of Lymphoma of the Myocardium Mimicking Clinical Hypertrophic Cardiomyopathy,” Circulation, Vol. 113, No. 12, 2006, pp. e662-e664. doi:10.1161/CIRCULATIONAHA.105.576306
- C. S. Chim, et al., “Primary Cardiac Lymphoma,” American Journal of Hematology, Vol. 54, No. 1, 1997, pp. 79- 83. doi:10.1002/(SICI)1096-8652(199701)54:1<79::AID-AJH13>3.0.CO;2-5
- R. Bambury, et al., “Primary Cardiac Lymphoma: Diagnostic Tools and Treatment Challenges,” Irish Journal of Medical Science, Vol. 180, No. 1, 2011, pp. 271-273. doi:10.1007/s11845-009-0446-x
- H. S. Cabin, et al., “Cardiac Lymphoma Mimicking Hypertrophic Cardiomyopathy,” American Heart Journal, Vol. 102, No. 3, 1981, pp. 466-468. doi:10.1016/0002-8703(81)90328-8
- A. F. Nascimento, G. L. Winters and G. S. Pinkus, “Primary Cardiac Lymphoma: Clinical, Histologic, Immunophenotypic, and Genotypic Features of 5 Cases of a Rare Disorder,” The American Journal of Surgical Pathology, Vol. 31, No. 9, 2007, pp. 1344-1350. doi:10.1097/PAS.0b013e3180317341
- J. M. Van Der Klooster, et al., “Asystole during Combination Chemotherapy for Non-Hodgkin’s Lymphoma: The Acute Tumor Lysis Syndrome,” The Netherlands Journal of Medicine, Vol. 56, No. 4, 2000, pp. 147-152. doi:10.1016/S0300-2977(99)00124-2
NOTES
*No grant or funding has been received by any author for this work.
#Corresponding author.

