Health
Vol.5 No.7(2013), Article ID:34591,7 pages DOI:10.4236/health.2013.57147
The effects of application of an ancient type of acupuncture needle on increase in urination of hospitalized oldest-old people
![]()
1Department of Medical Informatics, Niigata University Medical & Dental Hospital, Niigata, Japan; #Corresponding Author: watanabem62@gmail.com
2Department of Health, Faculty of Health Science, Tsukuba University of Technology, Tsukuba, Japan
3Urahigashi Veterinary Clinic, Osaka, Japan
4School of Health Sciences, Faculty of Medicine, Niigata University, Niigata, Japan
5Shaanxi University of Chinese Medicine, Shaanxi, China
6Department of Immunology, Niigata University School of Medicine, Niigata, Japan
Copyright © 2013 Mayumi Watanabe et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 13 May 2013; revised 14 June 2013; accepted 30 June 2013
Keywords: Di-Zhen (DZ); Acupuncture; Oldest-Old; Autonomic Nervous System (ANS); Leukocyte; Urination; Terminal Care
ABSTRACT
The di-zhen (DZ) is an ancient type of acupuncture needle with a history dating back to more than 2000 years. Unlike modern acupuncture needles, the DZ is not inserted subcutaneously and is considered to be safe for common use, even at the bedside of terminally ill patients. In this case study, DZ application was selected and applied 14 times on a 92-year-old patient who had suffered severe oliguria along with administration of diuretics. Urine volume increased 12 out of 14 times following DZ treatment; however, the other two times it was ineffective. To investigate the reason and the differences in effective/ineffective DZ application, two internal conditions (effective vs ineffective) were compared by analyzing daily nursing reports (vital signs such as blood pressure, urine volume and body temperature) and weekly clinical data (including renal, liver and immune function, urea nitrogen, creatinine, ALT, AST, the ratio and number of leukocytes, erythrocytes). DZ application increased urine volume via a transient modification of the autonomic nervous system when internal homeostasis was maintained. Aging populations, who often have several diseases and medications, are rapidly increasing in developed countries. Therefore, the study and application of DZ may contribute to a reduction in medical costs, which have been rapidly and heavily expanding recently.
1. INTRODUCTION
It is known that acupuncture as a therapeutic intervention is widely practiced. Acupuncture is said to be useful as an adjunct application included in a comprehensive management program application, which is known to reduce physical and psychological pain and improve the quality of life [1-3]. However, in cases of hospitalized patients who are the oldest-old or terminally ill, it is very difficult to insert acupuncture needles, which might cause problems such as infection and tissue breakdown [4,5]. The study of new approaches to the oldest-old, including terminally ill patients, addressed current needs given that aging populations are rapidly increasing in developed countries [6-9]. Recently, we studied the basal mechanism of di-zhen (DZ) application. DZ is an ancient type of acupuncture needle without subcutaneous insertion, the effects of which are very similar to those of modern needles inserted subcutaneously [10].
In this study, we applied DZ application for oliguria to a 92-year-old patient in the hospital, which resulted in an increase in urine output. The nursing team recorded vital signs (blood pressure, urine volume and body temperature) several times each day, and doctors weekly examined renal, liver and immune function (including urea nitrogen [UN], creatinine [CRE], ALT, AST, the ratio and number of leukocytes, erythrocytes). Therefore, we analyzed these data to quantify the effect of DZ applications. These results suggested a possibility that urine volume was increased after DZ application. At the same time, the findings indicated a difference between its effective and ineffective stages.
2. MATERIALS AND METHOD
2.1. Subject
2.1.1. Patient
A 92-year-old male, an active president of a local metal-processing company, was hospitalized because of aspiration pneumonia, under shock conditions (blood pressure: 20 - 70 mmHg), anuria and high fever. Written informed consent and all data were obtained from the patient and his family, and the study was approved by the institutional review board of Niigata University.
2.1.2. Clinical History
He recovered from brain infarction at the age of 82. He had suffered from arteriosclerosis for the past 2 years, and he routinely underwent acupuncture applications.
2.1.3. Conventional Application
The temperature in the hospital room was kept at 26˚C. Conventional therapy, the existing prescription and the existing quantity of administration of antibiotics, diuretic, fluid infusion, and nutrition were maintained during his hospitalization. DZ application was tried for the purpose of urination. The nursing team recorded vital signs, such as blood pressure, urine volume and body temperature several times each day, and doctors examined venous blood and urine every week to check clinical conditions of renal, liver and immune function.
2.2. DZ Application
The DZ needles made of stainless steel with a columnlike body and flat head (Tumujikaze-kun SNM type, Soken Medical Co. Ltd., Toshima, Japan) were selected to avoid any problems such as infection or tissue breakdown. An autoclaved DZ was softly pressed vertically onto the body surface for 5 minutes (diameter 5.0 mm, 37.3 g/mm2) at approximately 120 points from the head to the feet on both sides of the spine as mentioned in our previous study [10]. DZ application points corresponding to the Bladder Meridian as defined by the World Health Organization were selected. This meridian anatomically passes near the bladder and kidneys, and the aim of DZ application was to enhance function of these organs to increase urine volume [11,12]. The application was applied by nationally licensed, experienced Japanese acupuncturists.
2.3. Statistical Analysis
The statistical significance of differences between values was tested using Wilcoxon signed-rank test. P-values of less than 0.05 were considered to be statistically significant.
3. RESULTS
3.1. Systolic Blood Pressure (SBP) Elevated after DZ Application before Day 50
The kidneys filter out waste products from the blood, combining them with water to make urine and control blood pressure [13,14]. Because the volume of urine affects blood pressure, two kinds of blood pressures (diastolic blood pressure and systolic blood pressure: DBP and SBP) were studied. Compared to DBP, SBP showed an increasing trend after DZ application, although there were no statistically significant differences. After Day 50 of hospitalization, DBP did show elevation (Figure 1, upper panel).
3.2. Urine Volume Increased after DZ Application before Day 50
The urine volume of the patient, who had suffered from oliguria, showed a step-like increase (103 → 300 → 850 → 1900 mL) after the first DZ application (Figure 1, lower panel). Particularly, on all days when urine volume exceeded 1000 mL, SBP showed an elevation. Urine volume significantly increased with DZ application compared to without DZ application (P < 0.05) (Figure 2). However, after day 50, urine volume was not increased (Figure 1, lower panel).
3.3. Body Temperature, Total Protein, Erythrocytes and Hemoglobin Decreased
As mentioned, DZ application might have an effect on blood pressure, which is one of several vital signs. Therefore, kinetic changes in body temperature, another type of vital sign, were also studied; body temperature returned to the normal range. At the same time, total protein, erythrocytes and hemoglobin were investigated. All of these measures were consistently below the normal range and showed a decrease (Figure 3).
The number of leukocytes, which had severely exceeded the normal range, began to decrease after Day 10 (Figure 4). The ratio of leukocytes to granulocytes was outside of the normal range. The number of granulocytes and lymphocytes largely decreased after Day 10. The latter showed a sudden decrease after Day 50.
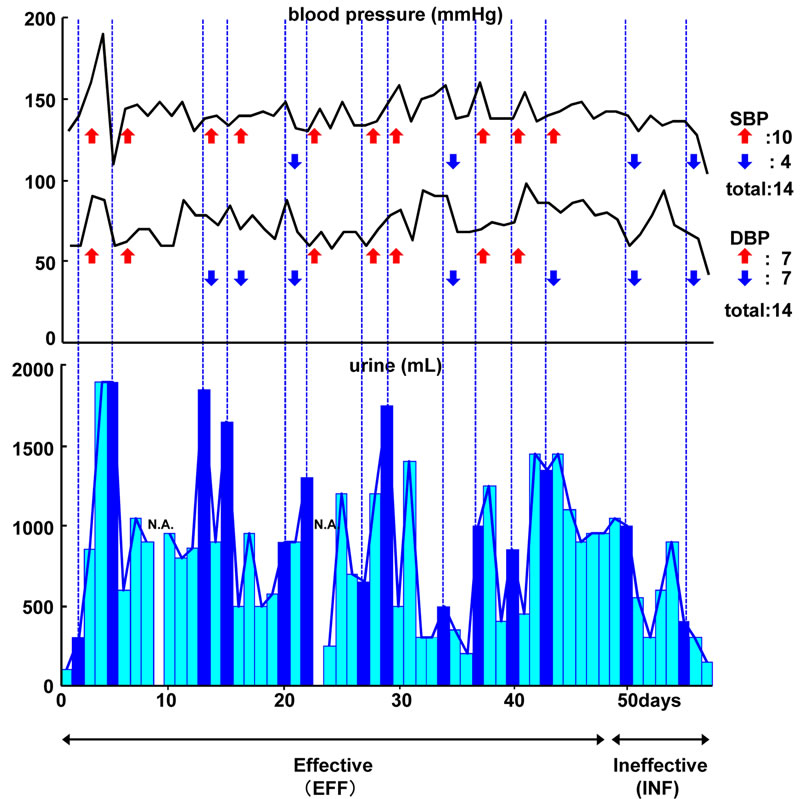
Figure 1. Kinetic record of blood pressure, urine volume and the cross relationship. Upper panel: kinetic record of DBP (diastolic blood pressure) and SBP (systolic blood pressure). Comparison of DBP with SBP showed an increasing trend after DZ application (SBP↑10, ↓4 vs DBP↑7, ↓7). After Day 50, DBP did show elevation. Lower: kinetic record of urine volume. Dark blue = days with DZ application; Light blue = days without DZ application. After Day 50, no increase was observed. On days when urine volume exceeded 1000 mL, SBP was elevated.
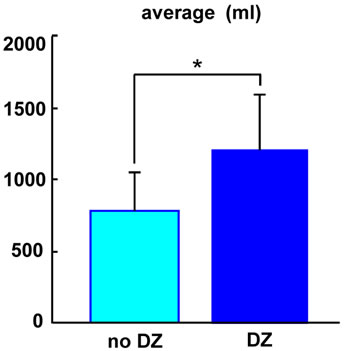
Figure 2. Statistical analysis of days with and without DZ application. Compared to days without DZ application (light blue; no DZ), urine volume significantly increased on days with DZ application (dark blue; DZ) (P < 0.05).
3.4. Comparison of the Internal Condition of the Two Points: The Effective and Ineffective
Although urine volume with DZ application increased until Day 49, it did not show an increase after Day 50.
Therefore, the period of hospitalization was divided into two stages: the effective period when DZ application could increase urine volume and the ineffective period when it did not. In other words, DZ application was effective from Day 1 through Day 49 (effective period) and was ineffective after Day 50 (ineffective period) (Figure 5). To investigate this reason, the internal clinical conditions of the former period and that of the latter were compared. The former was represented by data from Day 22 and the latter by that of Day 50. These days were selected because DZ applications were given soon after the clinical medical checks on these 2 days.
The plasma levels of Na and Cl were lower than the normal range during both periods. The volume of potassium (K) in the plasma was out of the normal range during ineffective period. The plasma level of C-reactive protein during the effective period had been severely high and decreased during the ineffective period; however, it remained over the normal range. UN and CRE were lower during the effective period compared to the ineffective. GPT (ALT) and GOT (AST) were elevated during the ineffective period compared to the effective, during which GOT/GPT decreased inside of the normal range.
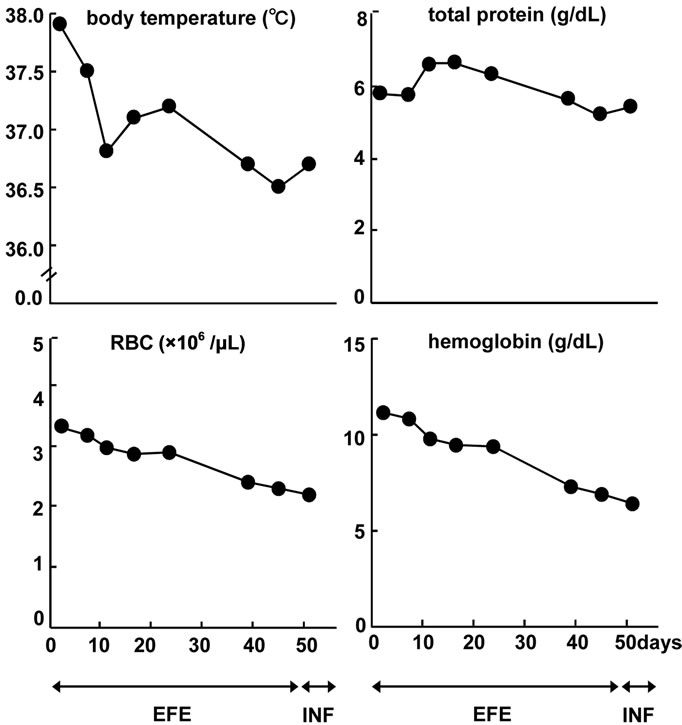
Figure 3. Kinetic change of body temperature, total protein, erythrocytes and hemoglobin. These measures were consistently below the normal range and showed a decrease.
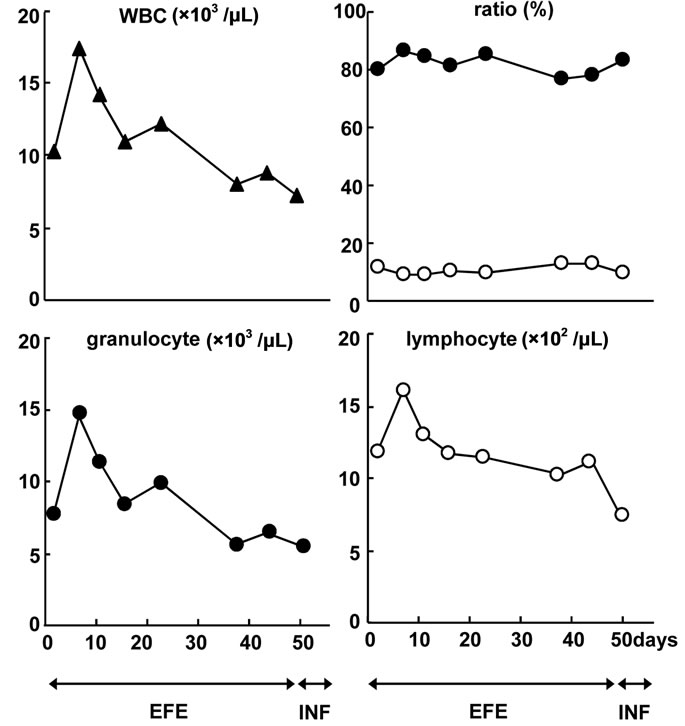
Figure 4. Kinetic change of the number and the ratio of leukocytes. The number of granulocytes (●) largely decreased after Day 10, while lymphocytes (○) showed a sudden decrease on Day 50. (▲): leukocytes.
4. DISCUSSION
4.1. DZ Application Increased Urine Volume
Because the urine volume was higher on days with DZ application compared to days without, it was suggested
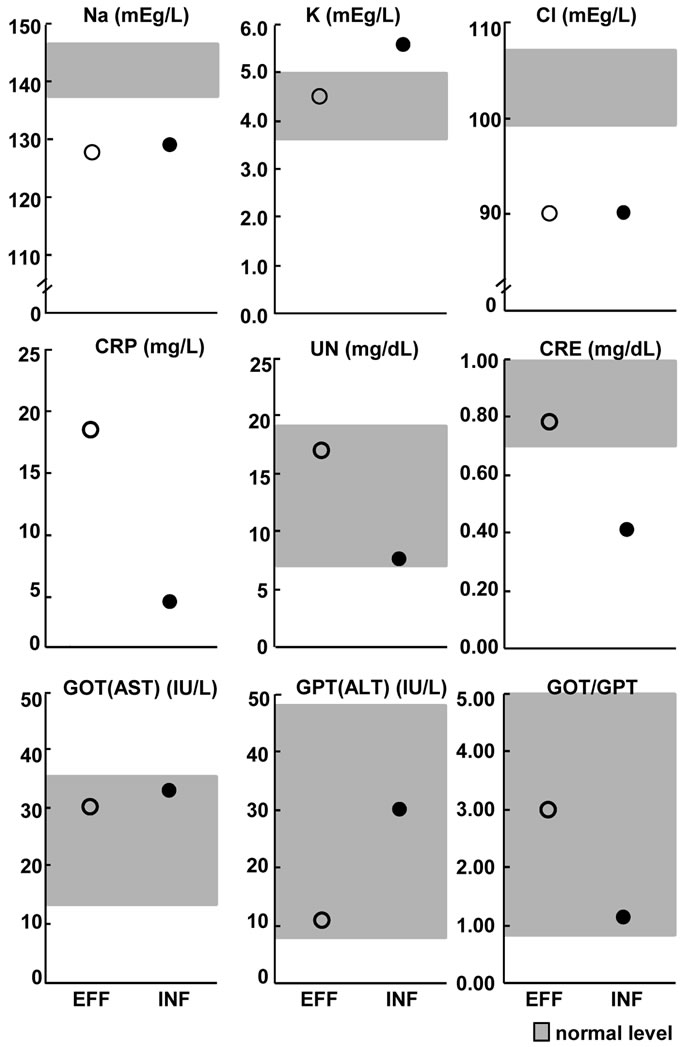
Figure 5. Comparison of the internal clinical conditions of the effective and ineffective stages. Effective: Day 22, representing the effective period from Day 1 to 49. Ineffective: Day 50, representing the ineffective period after Day 50. UN (urea nitrogen) and CRE (creatinine) are lower during the effective stage compared to the ineffective.
that DZ application could affect urine volume. Several researchers and clinical doctors reported acupuncture and other skin stimulating applications regulated urine volume [15-19]. Recently, we reported that DZ application increases catecholamine (adrenaline, noradrenaline and dopamine) levels. Moreover, there are many clinical reports of the ability of various skin stimulating applications, such as acupuncture, moxibustion and massage, to elevate catecholamine levels [10,20,21], which indicates an effect on the autonomic nervous system (ANS). As SBP was elevated the day after DZ application, there is a possibility that the circulatory system is affected as well (Figure 1, upper panel). Given that the maintenance of blood pressure and urination is commonly regulated by the kidneys, the relationship between the urine volume and the blood pressure must be considered. In fact, on all days when the urine volume exceeded 1000 mL, SBP also was elevated (Figure 1).
4.2. DZ Application Affected Urine Volume via Changes in ANS Balance from SNS to PNS Dominance
4.2.1. Urination Was Observed after Transient SNS Dominance
Recently, we reported that DZ application affected the level of adrenaline and noradrenaline, and that it induced a transient sympathetic nervous system (SNS) dominance (20 - 40 min) [10]. In fact, urination was observed 20 - 40 minutes after DZ application in the current study (data not shown). The same mechanism was indicated in a transient cutaneous hypothermia, which showed recovery within 20 - 40 minutes [10]. These observations agree with the fact that adrenaline and noradrenaline have a short half-life [22,23]. In this way, it is expected that urination was observed after the end of the transient SNS dominance.
4.2.2. DZ Application Affected Urination, Changing the ANS Balance from SNS to PNS Dominance
The detrusor urinae muscle (smooth muscle) contracts in response to the pelvic nerve, a parasympathetic nerve, to cause urination. In short, urination is controlled by the parasympathetic nervous system (PNS) and is suppressed under SNS dominance [24,25]. Therefore, it is thought that urine volume increased after DZ application because of changes in ANS balance from SNS to PNS dominance.
4.2.3. Transient SNS Dominance Was Followed by PNS Dominance
The image of the relationship between transient SNS dominance and the onset of PNS dominance is illustrated in Figure 6. DZ application was stronger than other skin stimulation [10] and brought about a transient (rapid appearance and disappearance of) SNS dominance. Such a rapid and strong change in ANS balance could induce a kind of rebound, such as the yin-yang like reaction. In other words, SNS suppression was related to PNS dominance [26]. Thus, there is the possibility that the transient SNS dominance was followed by a PNS dominance. Further studies with precise measurements are needed to support this hypothesis.
4.3. DZ Application Was Ineffective When Internal Homeostasis Failed
First, UN and CRE, renal function indicators, largely decreased during the ineffective stage compared to the effective stage (Figure 5). Therefore, it may be plausible to consider that DZ application was ineffective when renal function failed. Second, the number of lymphocytes remained over 1000/μL until suddenly dropping after day
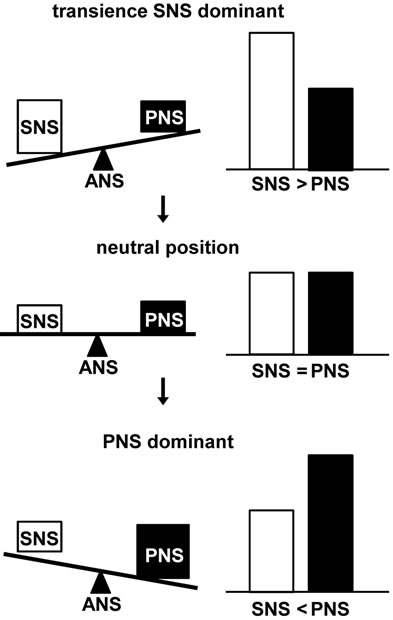
Figure 6. Image of the power balance between the SNS and PNS. Sympathetic Nervous System (SNS) dominant status induced by DZ application was transient. When the SNS was suppressed, either it was in a neutral state or the parasympathetic nervous system (PNS) was induced.
50, when DZ application became ineffective. It has been reported that the number and ratio of lymphocytes controlled by the PNS [27,28]. The volume of urine, which is also regulated by the PNS, did not increase after DZ application when the number of leukocytes dropped (Figure 4, upper right panel). Therefore, the number of leukocytes might be considered to be an indicator of the effectiveness of DZ application.
The urination reflex is a local reflex and is controlled by centers in the spinal cord and central nervous system [15,24]. However, increased urine volume was not observed after DZ application under a severe and systemic condition. It may be understood that DZ application was ineffective when internal homeostasis failed.
4.4. Specific and Historical Compatibility of DZ and the Bladder Meridian
In this study, DZ was selected because it was practiced during the end-of-life care of an oldest-old patient in a general hospital; it was needed to avoid infection and tissue damage. Because the main purpose of the application was the application of oliguria, the Bladder Meridian, which is said to run through and stimulate the kidneys and the bladder [11,12], was selected.
The specific compatibility of DZ, the ancient type of acupuncture needle, with the stimulation of acupuncture points along the Bladder Meridian was not negligible. If this historically reported compatibility, which was indicated from the era of the Tyrolean Iceman [29], is more significant than other applications, it should be possible to observe effects that are specific to DZ application. Further research is required to support this hypothesis.
5. CONCLUSION
DZ showed effectiveness at the bedside during endof-life care of the oldest-old. In cases when the effects of administered diuretics are not sufficient, DZ application, with adequate knowledge and appropriate technique, could help improve the quality of life of patients as complementary medicine. The oldest-olds often have several diseases and medications [30,31]. DZ application may contribute to reduce medical costs, which have been rapidly and heavily expanding recently.
6. ACKNOWLEDGEMENTS
The authors thank all the medical staff, the patient and his family, and Ms. Hiromi Ishiwatari (Soken Medical Co. Ltd.) and Ms. Ryoko Karasawa for assistance with this study.
![]()
![]()
REFERENCES
- National Institutes of Health Office of the Director (1997) Acupuncture. NIH Consensus Statement, 15, 1-34. http://consensus.nih.gov/1997/1997Acupuncture107PDF.pdf
- NIN Consensus Development Panel on Acupuncture (1998) Acupuncture. JAMA, 280, 1518-1524. doi:10.1001/jama.280.17.1518
- Ernst, E., Pittler, M.H. and Wider, B. (2006) Acupuncture. In: Ernst, E., Pittler, M.H. and Wider, B., Eds., The Desktop Guide to Complementary and Alternative Medicine, 2nd Edition, Mosby Ltd, London, 292-296.
- Walsh, B. (2001) Control of infection in acupuncture. Acupuncture in Medicine, 19, 109-111. doi:10.1136/aim.19.2.109
- Woo, P.C., Lin, A.W., Lau, S.K. and Yuen, K.Y. (2010) Acupuncture transmitted infections. British Medical Journal, 340, 1147-1152. doi:10.1136/bmj.c1268
- Roush, W. (1996) Live long and prosper? Science, 273, 42-46.
- Christensen, K., Doblhammer, G., Rau, R. and Vaupel, J.W. (2009) Ageing populations: The challenges ahead. Lancet, 374, 1196-1208. doi:10.1016/S0140-6736(09)61460-4
- United Nations Department of Economic and Social Affairs Population Division (2012) Population facts 2012/4. http://www.un.org/esa/population/publications/popfacts/popfacts__2012-1.pdf
- Statistics and Information Department Minister’s Secretariat, Ministry of Health, Labour and Welfare Japan (2010) Vital statistics, life expectancy at birth. http://www.mhlw.go.jp/english/database/db-hw/dl/81-1a2en.pdf
- Watanabe, M., Takano, O., Tomiyama, C., Matsumoto, H., Urahigashi N., Kainuma, E., Madarame, T., Fukuda, M. and Abo, T. (2012) The effects of application of an ancient type of acupuncture needle on body temperature, immune function and the autonomic nerve system. Health, 4, 775-780. doi:10.4236/health.2012.410120
- World Health Organization Western Pacific Region (2008) WHO standard acupuncture point locations in the western pacific region. World Health Organization Western Pacific Regional Office, Manila.
- Lee, B.Y., LaRicca, P.J. and Newberg, A.B. (2004) Acupuncture in theory and practice physiologic effects. Hospital Physician, 11-18. http://turner-white.com/memberfile.php?PubCode=hp_apr04_theory.pdf11
- Osuji, C.U., Nwaneli, C.U., Onwubere, B.J., Onwubuya, E.I. and Ahaneku, G.I. (2012) Renal function in patients with hypertension associated congestive cardiac failure seen in a tertiary hospital. International Journal of Nephrology, 2012, 1-5. doi:10.1155/2012/769103
- Yee, J. (2008) Diabetic kidney disease: Chronic kidney disease and diabetes. Diabetes Spectrum, 21, 8-10. doi:10.2337/diaspect.21.1.8
- Sato, A., Sato, Y. and Uchida, S. (2002) Reflex modulation of visceral functions by acupuncture-like stimulation in anesthetized rats. International Congress Series, 1238, 111-123. doi:10.1016/S0531-5131(02)00418-1
- Sato, A., Sato, Y. and Suzuki, A. (1992) Mechanism of the reflex inhabitation of micturition contractions of the urinary bladder elicited by acupuncture-like stimulation in anesthetized rats. Neuroscience Research, 15, 189-198. doi:10.1016/0168-0102(92)90004-V
- Paterno, J.C., Freire, A.O., Soares, M.F., Franco, M.F., Schor, N. and Teixeira, V.P. (2008) Electroacupuncture and moxibustion attenuate the progression of renal disease in 5/6 nephrectomized rats. Kidney and Blood Pressure Research, 31, 367-373. doi:10.1159/000176189
- Yi, W.M., Pan, A.Z., Li, J.J., Luo, D.F. and Huang, Q.H. (2011) Clinical observation on the acupuncture application in patients with urinary retention after radical hysterectomy. Chinese Journal of Integrative Medicine, 17, 860-863. doi:10.1007/s11655-011-0800-5
- Radvanska, E., Kamperis, K., Kleif, A., Kovács, L. and Rittig, S. (2011) Effect of laser acupuncture for monosymptomatic nocturnal enuresis on bladder reservoir function and nocturnal urine output. Journal of Urology, 185, 1857-1861. doi:10.1016/j.juro.2010.12.068
- Mori, H., Nishijo, K., Kawamura, H. and Abo, T. (2002) Unique immunomodulation by electro-acupuncture in humans possibly via stimulation of the autonomic nervous system. Neuroscience Letters, 320, 21-24. doi:10.1016/S0304-3940(02)00012-5
- Watanabe, M., Takano, O., Tomiyama, C., Matsumoto, H., Kobayashi, T., Urahigashi, N., Urahigashi, N. and Abo, T. (2012) Skin rubdown with a dry towel, “kanpu-masatsu” is an aerobic exercise affecting body temperature, energy production, and the immune and autonomic nervous systems. Biomedical Research, 33, 243-248. doi:10.2220/biomedres.33.243
- Oonuki, D., Nagoh, T., Takahashi, Y. and Sano, K. (2009) The influence of local anesthetic injected by the pre-administration method on plasma catecholamine and hemodynamic responses. Oral Therapeutics and Pharmacology, 28, 117-123.
- Stiell, I. G., Hebert, P.C., Weitzman, B.N., Wells, G.A., Raman, S., Stark, R.M., Higginson, L.A., Ahuja, J. and Dickinson, G.E. (1992) High-dose epinephrine in adult cardiac arrest. The New England Journal of Medicine, 327, 1045-1050. doi:10.1056/NEJM199210083271502
- Tsuchida, S. (1989) Nervous control of micturition. Japanese Journal of Urology, 80, 1257-1277.
- Creasey, G.H. and Craggs, M.D. (2012) Functional electrical stimulation for bladder, bowel, and sexual function. Handbook of Clinical Neurology, 109, 247-257. doi:10.1016/B978-0-444-52137-8.00015-2
- Abo, T. and Kawamura, T. (2002) Immunomodulation by the autonomic nervous system: Therapeutic approach for cancer, collagen diseases, and inflammatory bowel diseases. Therapeutic Apheresis, 5, 348-357. doi:10.1046/j.1526-0968.2002.00452.x
- Toyabe, S., Iiai, T., Fukuda, M., Kawamura, T., Suzuki, S., Uchiyama, M. and Abo, T. (1997) Identification of nicotinic acetylcholine receptors on lymphocytes in the periphery as well as thymus in mice. Immunology, 92, 201- 205. doi:10.1046/j.1365-2567.1997.00323.x
- Suzuki, S., Toyabe, S., Moroda, T., Tada, T., Tsukahara, A., Iiai, T., Minagawa, M., Maruyama, S., Hatakeyama, K., Endoh, K. and Abo, T. (1997) Circadian rhythm of leucocytes and lymphocytes subsets and its possible correlation with the function of the autonomic nervous system. Clinical & Experimental Immunology, 110, 500-508. doi:10.1046/j.1365-2249.1997.4411460.x
- Dorfer, L., Moser, M., Spindler, K., Bahr, F., Egarter-Vigl, E. and Dohr, G. (1998) 5200-year-old acupuncture in central Europe? Science, 282, 242-243. doi:10.1126/science.282.5387.239f
- Sato, T., Sato, K. and Akira Sato, A. (2010) Medication reduction in a convalescent rehabilitation ward. Japanese Journal of geriatrics, 47, 440-444. doi:10.3143/geriatrics.47.440
- Mita, Y., Akishita, M., Tanaka, K., Yamada, S., Nakai, R., Tanaka, E., Nakamura, T. and Toba, K. (2004) Improvement of inappropriate prescribing and adverse drug withdrawal events after admission to long-term care facilities. Geriatrics & Gerontology International, 4, 146-150. doi:10.1111/j.1447-0594.2004.00244.x
NOTES
*These authors contributed equally to this work.

