Open Journal of Urology
Vol.06 No.09(2016), Article ID:70660,7 pages
10.4236/oju.2016.69024
Occlusive Syndrome Revealing a Nonseminoma Germ Cell Tumor Metastatic Testicular
N. M. Diagne Gueye1, R. Kane2*, Y. Diallo3, A. R. Ndiaye4, A. R. Ndiaye1
1Department of Internal Medicine, Principal, Dakar, Senegal
2Urologic Surgery Department, Principal, Dakar, Senegal
3Urology Thies, Senegal
4Medical-Hospital Imaging Department, Principal, Dakar, Senegal

Copyright © 2016 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY 4.0).
http://creativecommons.org/licenses/by/4.0/



Received: April 5, 2016; Accepted: September 14, 2016; Published: September 19, 2016
ABSTRACT
Testicular cancer is rare. The authors report the case of a young Senegalese 21, who has consulted for an occlusive syndrome evolving for 48 hours that prompted his hospitalization. Note that the patient has consulted several times to persistent inguinal scrotal pain, a big right purse with chronic analgesic requirements and anti-inflammatory. Occlusive before this table, abdominal pelvic CT was performed and highlighted the presence of lung metastases, a large pelvic lymph node casting bridging the inter vesico-rectal space and responsible for extrinsic compression of the small intestine, lymph node inter casting aorto-cellar and latero aortic liver and multiple secondary locations. Faced with this bundle of arguments, clinical and laboratory, metastatic testicular tumor was raised and measured tumor markers. A right orchiectomy by inguinal was made with histology: A non-seminomatous germ cell tumor stage III. After orchiectomy germinal markers were still high and there was the problem of persistent occlusive syndrome despite resuscitation. A chemotherapy regimen was initiated with 4 cycles of chemotherapy according to the protocol BEP (bleomycin, etoposide, cisplatin). A significant regression of occlusive syndrome with a decline in clinical symptoms was noted. The revaluation at 3 months, 6 months and 1 year were highlighted: A normal clinical examination associated with a persistent correction rate of germline markers and lack of active lesion at thoraco-abdominopelvic CT.
Keywords:
Testicular Cancer, Non Seminomatous Germ Cell Tumor, Intestinal Obstruction

1. Introduction
Testicular cancers are rare [1] . They are the leading cause of solid tumor of young men in the West. The diagnosis is often made between 20 and 40 years [1] . Non-seminoma germ cell tumors are the most common histological form with an increasing incidence in the northern European countries. This condition is rare in the black subject. Very few studies have been reported in sub-Saharan Africa [2] [3] , where the diagnosis metastatic stage making poor prognosis. The observation described here by the authors is a perfect illustration.
2. Observation
The authors report the case of a young Senegalese 21 years who consulted urgently for an occlusive syndrome is abdominal pain, vomiting and stopping materials and gas occurred 48 hours before admission to Home emergency department of the hospital. This patient consulted several times for persistent groin pain and a big purse with chronic of painkillers and anti-inflammatories.
On arrival Clinical examination objectified had a patient whose condition was altered. Examination of the abdomen is a diffuse tenderness to palpation with a hypo gastric defense. External genitalia there was a painful swelling, inflammation of the right testicle, stony consistency and rectal presence is noted of a painful mass, dishing farm in the rectum to reduce the anterior rectal light. The remainder of the physical examination was normal.
The blood test preoperative germinal markers showed the following results: AFP greater than 1210 ng/ml (N: 0 - 12); LDH: 4304 IU/l (N: 100 - 200); free hCG: 7939 IU/l (N: less than 5).
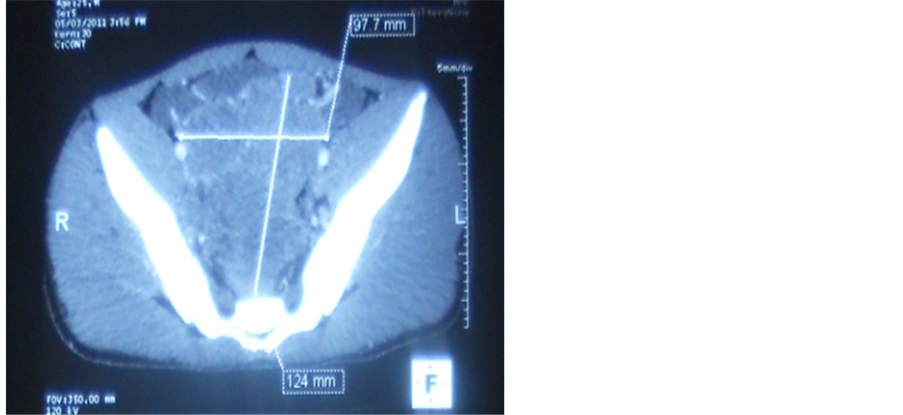
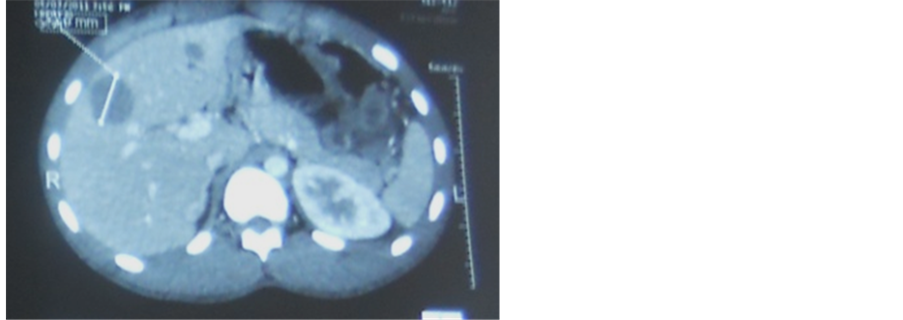
Radiography of the abdomen without preparation highlighted many water-scarce hydro levels. Testicular ultrasound highlighted an aspect of suspect heterogeneous testicle and bilateral testicular stones. A thoraco-abdominal-pelvic CT scan, there was the presence of 4 pulmonary nodules consistent with metastases, a bulky pelvic lymph node casting bridging the inter vesico-rectal area and responsible for extrinsic compression of the small intestine, lymph node inter casting aorto-caval and latero aortic and multiple hepatic secondary locations. Given this body of evidence, metastatic testicular tumor was raised (Figure 1 and Figure 2).
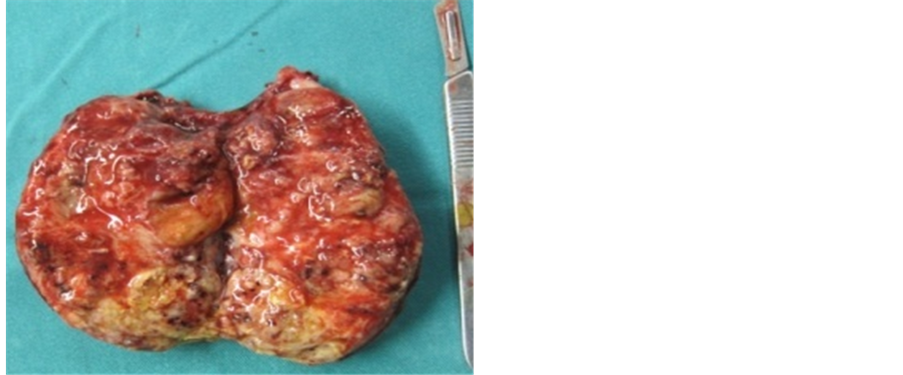
A right orchiectomy (Figure 3 and Figure 4) was performed with histology: A nonseminoma germ cell tumor composed of sac, embryonal carcinoma, teratoma and choriocarcinoma without seminoma quota. The tumor invaded the epididymis with the presence of many tumor emboli outside. This allowed a finding of nonseminoma germ cell tumor in stage III.
After orchiectomy germinal markers were still high on day 7 post-operative AFP > 1200 IU/l HCG: 7939 IU/l LDH: 4304 IU/l. The patient received 4 cycles of chemotherapy according to BEP (Bleomycin 15 mg/m2, etoposide 100 mg/m2 cisplatin 20 mg/ m2) from D1 to D5 as J1 = J21 cycles. Regression markers was noted after 2 courses (AFP: 400 IU/l HCG 3200 IU/l LDH: 2000 IU/l) and a significant regression of occlu-
Figure 1. Pelvic lymph node casting.
Figure 2. Liver met a stases.
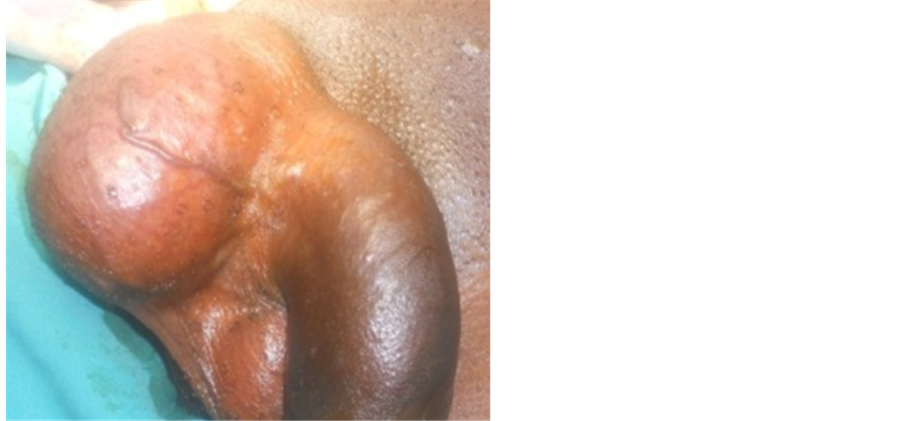
Figure 3. Chronic big purse.
Figure 4. Orchiectomy specimen.
sive syndrome with lower abdominal pain, stop vomiting a laxation made of a liquid bowel movement every two days. Normalization of markers was noted after 4 treatments. The revaluation BEP after 4 treatments were: A normal clinical examination associated with persistent correction rate of germ line markers and no active lesion in the thoraco-abdominal-pelvic scan.
3. Comments
Non-seminoma testicular germ cell tumors are rare in Africa, where some cases have been reported [2] - [4] . In terms of histological type, the predominance of germ cell tumors is admitted by all authors with a variable frequency according to the authors but around 90% [1] .
Testicular tumors are four times more common in Caucasians [1] [5] . The increased incidence and geographic distribution of these tumors can be related to different exposure to external factors or carcinogenic role of the environment in their initiation or development. [1] The peak incidence is between 20 and 40 years [1] [5] . Non-semin- oma testicular germ cell tumors are tumors of young adults, as illustrated in this observation. In the literature, it is described that the intra-abdominal position of these tumors (iliac fossa, para umbilical region) offers them a space to grow to reach high volumes before being symptomatic of where the diagnostic delay [1] [5] .
Non-seminoma germ cell tumors are characterized by high tissue variability. Indeed 55% of germ cell tumors are Nonseminomatous while 45% are constituted by seminomas [1] .
The circumstances of discovery of non-seminoma germ cell tumors vary but are often common to all testicular tumors. They can range from the palpation of a nodule indurated to the fortuitous discovery of testicular lesion on ultrasound during an infertility evaluation. In the forms with acute necrosis, there is a big aspect of clinical inflammatory hyperalgesia purse with scrotal pain; In the metastatic forms, often rapidly progressive, abdominal pain syndrome may be indicative of a retroperitoneal tumor extension performing a mass palpable on physical examination sometimes associated with dyspnea related lung secondary locations [6] - [9] . In this observation, the painful symptoms hyperalgic was in the foreground, treated with painkillers and was complicated by a retroperitoneal tumor extension responsible for an occlusive synd-rome.
The diagnosis is made by elevated tumor markers. They have diagnostic and prognostic value and are important in monitoring [10] [11] . In this patient has been a dramatic decline after two markers BEP cures and persistent normalization after 4 cycles these markers are normal 1/3 in the early stages of the tumor [11] . In metastatic forms, these markers have an independent prognostic value and are part of the classification criteria of IGCCCG Group (International Germ Cell Cancer Collaborative Group) [11] .
A semen collection must be systematic for forensic reasons. The orchiectomy and testicular histology confirmed the diagnosis and define the local extension and prognosis. Histological analysis is a fundamental step in terms of the different tumor components and their respective proportions within the lesion. This examination also for the presence of vascular or lymphatic emboli, and the existence of a significant relapse embryonal carcinoma prognostic factor [11] . Pathological examination of the part of orchiectomy in this observation revealed a nonseminoma germ cell tumor composed of sac, embryonal carcinoma, teratoma and choriocarcinoma without seminoma quota. The tumor invaded the epididymis with the presence of many tumor emboli confi- rming the poor prognosis in this patient.
More generally, the factors of testicular tumors Risk Factor are polymorphic and classified into intrinsic and extrinsic factors. Intrinsic factors are: Genitourinary abnormalities such as cryptorchidism which is a major factor, less than 12 ml testicular atrophy, subfertility, sexual ambiguity and gonadal dysgenesis or testicular micro stones. Hormonal factors involved are: Intrauterine as maternal hyper-ostéogénie during pregnancy or extrauterine as low androgenic impregnation and the high level of FSH. There is a risk in areas such as agriculture, leather work, or mechanical, painting, mining, plastics and metals, as well as exposure to radiation emitted by radar [11] . These risk factors have not been found in this observation.
The prognosis of non-seminoma germ cell tumors is determined by the classification according to IGCCCG (International Germ Cell Cancer Collaborative Group). Despite advances in treatment modalities, improving the prognosis still depends on early diagnosis of cancer in a still little advanced stage [11] .
Our patient according to these criteria (including liver extra pulmonary metastases) was rated poor prognosis.
Therapeutically, orchiectomy by inguinal approach is routinely recommended as first line. The orchiectomy should always be performed by ligation with inguinal first vessels [12] [13] . Then, as recommended, the therapeutic management is guided by the stage according to AJCC Classification stages of testicular germ cell tumors updated in 2009.
Stage III with advanced metastases, in case this observation, the standard treatment lies in the combination Bleomycin, Etoposide and Cisplatin in 3 or 4 courses according prognosis group IGCCCG spaced 3 weeks. In terms of the management of residual masses in case of normalization of markers, all supra-centimeter mass must be surgical resection of object 4 to 6 weeks after chemotherapy. All metastatic sites are concerned in the framework of a regional surgery, multidisciplinary at the sacrifice of a neigh- boring organ. The evaluation by computed tomography thoraco abdominal pelvic of this patient has no evidence of secondary locations, or residual masses requiring surgical intervention [1] [14] .
4. Conclusion
Non-seminoma germ cell tumors are chemo sensitive. This chemo sensitivity has significantly improved the prognosis of the disease through the provision of cisplatin [15] . The prognosis is even better than the diagnosis is made early stage [1] . The poor prognosis of stages also received chemotherapy associated with salvage surgery with complete resection of residual masses. Testicular germ cell tumors are certainly rare in African blacks, but of late diagnosis [3] [4] . Despite this prognosis was improved by chemotherapy regardless of stage [11] [16] . That is why this tumor pathology deserves to be better known and sought after by practitioners in time particularly in developing countries for early diagnosis. Therapeutic advances allow the best choice for every patient with significantly reduced toxicity [17] .
Cite this paper
Diagne Gueye, N.M., Kane, R., Diallo, Y., Ndiaye, A.R. and Ndiaye, A.R. (2016) Occlusive Syndrome Re- vealing a Nonseminoma Germ Cell Tumor Metastatic Testicular. Open Journal of Uro- logy, 6, 147-153. http://dx.doi.org/10.4236/oju.2016.69024
References
- 1. Durand, X., Rigaud, J., Avances, C., Camparo, P., Culine, S., Iborra, F., Mottet, N., Sébe, P., Soulié, M., et al. (2010) Recommandations en Onco-Urologie 2010: Tumeurs germinales du testicule. Progres En Urologie, 4, 297-211.
http://dx.doi.org/10.1016/S1166-7087(10)70046-4 - 2. Niang, L., Diao, B., Gueye, S.M., Fall, P.A., Moby-Mpah, H., Jalloh, M., Ndoye, A. and Diagne, B. (2007) Cancer sur testicule non descendu intra-abdominal à propos de 5 cas. Progres En Urologie, 17, 947-949.
- 3. Kane, R., Ndiaye, A., Diagne, N.M. and Ogougbemy, M. (2013) Retard diagnostic et therapeutique du cancer du testicule au Senegal. Journal Africain Du Cancer, 5, 133-136.
- 4. Kane, R., Zakou, A.R., Diao, B., Ndiaye, A., Thiam, A., Sow, Y. and Diagne, B.A. (2014) Cancer du testicule: Particularités cliniques et limites thérapeutiques en milieu hospitalier urologique au Senegal. African Journal of Urology, 20, 149-153.
- 5. Miladi, M., Peyromaure, M., Remi, J., Beuzeboc, P., Debre, B. and Zerbib, M. (2003) Tumeurs germinales du testicule : étude pronostique. Progres En Urologie, 13, 92-97.
- 6. Goïta, A. Aspects épidémio-cliniques et prise en charge des tumeurs testiculaires dans le service d’urologie du C.H.U du Point-G. Th Med Bamako 2006-2007.
- 7. Houlgatte, A. and Vedrine, L. (2007) Tumeurs germinales non séminomateuses. EMC (Elsevier Masson SAS, Paris). Urologie, 18-650-A-20.
- 8. Schmoll, H.-J., Osanto, S., Kawai, K., Einhorn, L. and Fizazi, K. (2011) Advanced Seminoma and Nonseminoma: SIU/ICUD Consensus Meeting on Germ Cell Tumors (GCT), Shanghai 2009. Urology, 78, S456-S468.
http://dx.doi.org/10.1016/j.urology.2011.08.001 - 9. Winter, C. and Albers, P. (2011) Testicular Germ Cell Tumors: Pathogenesis, Diagnosis and Treatment. Nature Reviews Endocrinology, 7, 43-53.
http://dx.doi.org/10.1038/nrendo.2010.196 - 10. Nallu, A., Mannuel, H.D. and Hussain, A. (2013) Testicular Germ Cell Tumors: Biology and Clinical Update. Current Opinion in Oncology, 25, 266-272.
http://dx.doi.org/10.1097/cco.0b013e32835ff3e3 - 11. Riese, M.J. and Vaughn, D.J. (2009) Chemotherapy for Patients with Poor Prognosis Germ Cell Tumors. World Journal of Urology, 27, 471-476.
http://dx.doi.org/10.1007/s00345-009-0404-2 - 12. Krege, S. (2011) What Is New in 2011 Regarding Testicular Cancer. Urol Ausg A., 50, 187-191.
http://dx.doi.org/10.1007/s00120-011-2671-y - 13. Diamantopoulos, N. and Kortsaris, A. (2010) Testicular Germ Cell Tumors. J BUON off J Balk Union Oncol., 15, 421-434.
- 14. Lakmichi, M.A., Niang, L., Tligui, M., Traxer, O., Cussenot, O., Gattegno, B., et al. (2007) Infertility and Testicular Seminoma. Presse Médicale (Paris Fr. 1983), 36, 1753-1755.
- 15. Hartmann, M., Krege, S., Souchon, R., De Santis, M., Gillessen, S., Cathomas, R., et al. (2011) Follow-Up of Testicular Germ Cell Cancer Patients: Interdisciplinary Evidence-Based Recommendations. Urol Ausg A., 50, 830-835.
http://dx.doi.org/10.1007/s00120-011-2556-0 - 16. Droz, J.-P., Boyle, H., Culine, S., Fizazi, K., Fléchon, A. and Massard, C. (2013) Treatment of Testicular Cancer. Bull Cancer (Paris), 100, 1319-1332.
- 17. Vaughn, D.J. (2009) Chemotherapy for Clinical Stage I Nonseminomatous Germ Cell Tumours. BJU International, 104, 1381-1386. http://dx.doi.org/10.1111/j.1464-410X.2009.08863.x