Food and Nutrition Sciences
Vol.06 No.13(2015), Article ID:60152,8 pages
10.4236/fns.2015.613125
Validation of Total Daily Energy Expenditure Calculated with Actiheart against Doubly Labeled Water Method in Costa Rican Schoolchildren
Juan Diego Zamora-Salas, Adriana Laclé-Murray
Health Research Institute, University of Costa Rica, San José, Costa Rica
Email: juan.zamorasalas@ucr.ac.cr
Copyright © 2015 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 26 July 2015; accepted 5 October 2015; published 8 October 2015
ABSTRACT
The purpose of this study was to use the measurement of the PAEE taken from Actiheart in order to calculate the TEE in Costa Rican schoolchildren, and at the same time, to determine the effectiveness when it is compared against the TEE obtained by the DLW. A total of sixteen male schoolchildren were measured for their total daily energy expenditure (TEE) with the doubly labeled water (DLW) technique. The TEE obtained by the Actiheart monitor was calculated and validated against the DWL. The TEE was obtained adding the physical activity energy expenditure given by the Actiheart, plus the basal metabolic rate, and the energy cost of growth. The Pearson’s product? moment correlation coefficient and the paired t?test sample were measured in order to identify the association of the data and to evidence the differences between both measurements of TEE respectively. The Lin’s concordance correlation coefficient and the Bland-Altman plot evaluated the concordance of both methods. The correlation between the TEE obtained by DLW and the one calculated by Actiheart was r = 0.97, P < 0.001. The paired t-test showed no significant differences between both methods. Lin’s concordance correlation coefficient was Cb = 0.99, classified as almost perfect. The study validated the TEE calculated with Actiheart against the TEE measured by the DLW.
Keywords:
Actiheart, Doubly Labeled Water, Energy Expenditure, Isotopic Technique, Schoolchildren, Total Energy Expenditure

1. Introduction
Modern lifestyles have turned more sedentary among children [1] [2] ; this has been drawing the public’s attention [3] since there has been an increase in childhood obesity regardless of the socioeconomic and academic levels [4] [5] .
As a result of physical inactivity, there has been a decrease of the total energy expenditure (TEE) and therefore, childhood obesity has increased [1] [2] . That is why the screening of the energy expenditure (EE) in the condition of a free lifestyle is a fundamental matter for this study that deals with the etiology of obesity and of other chronic diseases [6] -[9] .
There are several screening techniques to measure the EE [9] but the doubly labeled water (DLW) isotopic technique has been set as the “gold standard” one for the measure of EE in a free lifestyle condition [9] [10] . The gold standard technique is high in cost; therefore, now there are other devices that measure EE such as: heart rate monitors (HR) [9] [11] , pedometers [12] , and accelerometer monitors (AC) [13] . These devices are small, portable, non-invasive, and lower in cost. They also provide the physical activity energy expenditure (PAEE). The readings of the total energy expenditure (TEE) obtained by these devices have been validated against the DWL readings [14] .
Nowadays, the HR monitor is considered to be the most popular method for calculation of the EE and the physical activity (PA) patterns in a free lifestyle condition [9] , nevertheless, it is also known that the calculation of the EE might be altered by the influence of factors such as stress, hydration level, and other environmental factors [15] , also because low intensity activities limit the capacity of prediction of PAEE [9] [11] .
It has been reported that AC monitors register correlations between EE and AC that range from moderate to high; on the other hand, accelerometers are not as accurate when certain physical activities, static jobs, and movements against external forces have to be measured [16] . This certainly is the limitation for the calculation of the TEE in sedentary populations. Therefore, the use of HR and AC monitors decreases the limitations and at the same time provides a more accurate reading of the TEE [9] [16] [17] . Nowadays, the Actiheart is one of the most accurate monitors for the measurement of PAEE, which is an essential component for the calculation of TEE in a free lifestyle condition, for both the adult and the pediatric population [18] - [21] .
Higher-quality and lower-cost equipment is necessary to obtain the information required to calculate the TEE accurately. Accuracy is important to know how the EE deals with the prevention of overweight and obesity in the pediatric population. Consequently, one of the objectives of this study is to use the reading of PAEE provided by the Actiheart monitor in order to calculate the TEE in Costa Rican schoolchildren and at the same time to determine its effectiveness when it is compared against the TEE obtained by the DLW technique.
2. Materials and Methods
This is a cross-sectional analytical study. The participants were sixteen male schoolchildren with an average age of 7.2 ± 0.98 ranging from six to nine years old. They all belonged to a school in the metropolitan area, specifically in the city of San Jose. The project was approved by the Ethics Committee for Research of the University of Costa Rica, and an informed written consent was obtained from all the participants’ parents.
2.1. Anthropometric Data
The body height was measured to the nearest 0.1 cm, and the body weight was measured in individuals wearing light clothes to the nearest 0.1 kg using a balance beam scale. The mean of the three measurements was recorded. Once these anthropometric measurements were recorded, the BMI was calculated with the formula: BMI = weight (kg)/heigh2 (m). All the measurements were obtained after twelve hours of overnight fasting and relative resting.
2.2. Calculation of the Total Energy Expenditure
The “gold standard” isotopic technique known as Doubly Labeled Water (DLW) measured the TEE in a free lifestyle condition of the human being, it belongs to the dosage of 18O at deuterium (2H) water in which the 99.9% of the hydrogen atoms present the form of 2H. The method was developed during seven days for purposes of the study.
After twelve hours of fasting and relative resting, each student was given a DLW aliquot by mouth (0.22 g of 18O per kg body weight enriched at 10% and 0.11 g of 2H per kg of body weight enriched at 99.9%). The students were observed during the intake of the dosage in order to make sure that it was done correctly and completely. The dosage was prepared at the laboratory of the Health Research Institute of the University of Costa Rica.
Before the DLW dosage was provided, a basal urine specimen was collected from each student to determine the natural basal content of 2H and 18O in the body could. Afterwards, the first urination of the day was collected each morning for the first seven days. The exact time of collection was recorded and the samples were kept at −70˚C until their next analysis.
A continuous flow mass spectrometer HYDRA (Europa Scientific, Crewe, United Kingdom) conducted by triplicate the analysis of the content of 2H and 18O in each of the urine samples at the Energy Metabolism and Stable Isotopes Laboratory of the Institute of Nutrition and Food Technology, of the University of Chile.
2.3. Calculation of the TEE Using the Actiheart Monitor
In order to obtain the formula for the measurement of the TEE, it was necessary to use the values of the basal metabolic rate (BMR), the energy cost of growth (ECG), and the PAEE obtained by the Actiheart for three days. For purposes of the study, the formula was defined as:
TEEActiheart = BMR + PAEE + ECG; and the factors are explained as follows.
2.3.1. Basal Metabolic Rate (BMR)
Using the Schofield equation [22] , which is coincident with the one established by Henry & Rees [23] for children that reside in tropical regions.
2.3.2. Physical Activity Energy Expenditure (PAEE)
It was obtained through the Actiheart monitor (Mini Metter Company, Inc., USA), ambulatory compact device (thickness 7 mm, diameter 33 mm, weight 10 g) equipped with an omnidirectional accelerometer and a processor of ECG signal that measures the HR and the AC together providing that way the PAEE.
2.3.3. Energy Cost of Growth (ECG)
2 kcal・kg−1・day−1 was the reference used for the body growth. FAO/WHO/UNU [24] provided the reference, which is for children between 6 and 9 years old.
Right after the intake of the DLW dosage, each of the students got an Actiheart monitor placed and they were asked to use it without taking it off for three consecutive days; these days were two weekdays and one day of the weekend (i.e. Thursday, Friday and Saturday). The device was secured in the chest of each child with pediatric electrodes (3M® Red Dot 2248). The main sensor was placed in the left side of the breastbone, and the wire was placed parallel along the midclavicular line at the third intercostal space (upper position), or just below the left breast (lower position). Each parent received a supply of electrodes and they were instructed on how to take care of the monitor and how to replace the electrodes in the event they were attached incorrectly.
3. Statistical Analysis
The factors that required descriptive statistics were: age, weight, height, BMI, ECG, BMR, the TEE measured with the DLW, and the TEE calculated with the Actiheart monitor. They were expressed as means ± standard deviation values. We used the Pearson’s correlation coefficient to evaluate the correlation between the TEEs, and the Paired sample t-test to test the differences between both means obtained. The reproducibility between the DLW and the Actiheart was assessed using the Lin’s concordance correlation coefficient [25] . Lin’s strength of agreement [25] was considered poor (<0.90), moderate (0.90 - 0.95), substantial (0.95 to 0.99), and almost perfect (>0.99). The Bland-Altman procedure plotted the differences between the DLW and the Actiheart monitor [26] .
Analyses were performed using MedCalc statistical software version 11.5.1 (Mariakerke, Belgium) and SPSS for Windows version 16.1 (IBM Corporation, New York, USA). The significance level was adopted in p < 0.05.
4. Results
Table 1 shows the age, the body characteristics, the ECG and the BMR of the schoolchildren. Results according
Table 1. Characteristic of the schoolchildren.
to the TEE, and the TEE corrected by the daily body weight are shown in Table 2.
The measurements of the TEE were not significantly different (1938 ± 235 vs. 1955 ± 265 kcal・d−1, p = 0.33) when the t-test analysis was performed. The correlation analysis between TEEs was r = 0.97, p < 0.0001, meaning that there was a strong concordance between both measurements. The Lin’s concordance correlation coefficient identified a substantial strength of agreement (Cb = 0.99).
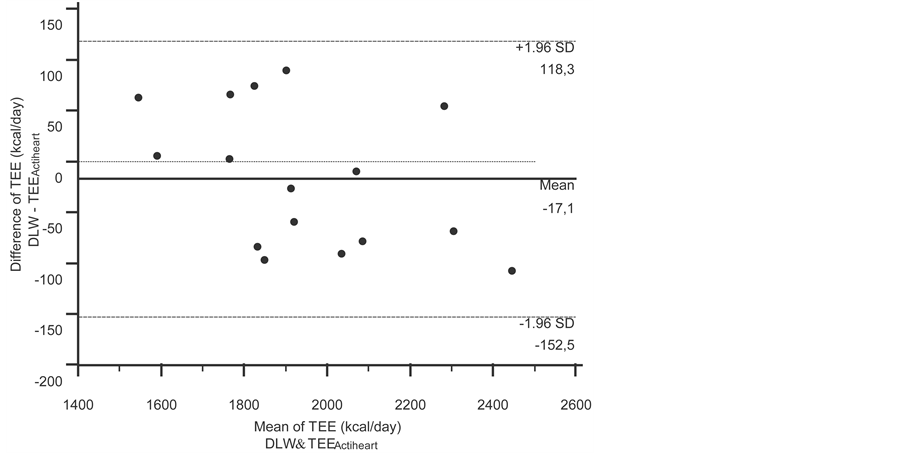
The plot of the differences between DLW and Actiheart according to the Bland-Altman procedure can be seen in Figure 1.
The TEE mean (±SD) with the DLW method was 1938 (±235) kcal・d−1; the Actiheart’s TEE mean was 1955 (±265) kcal・d−1. The bias of the Actiheart was −17.1 kcal・d−1 (95% CI = −53.92 to 19.67) showing that the Actiheart measured a higher TEE than the DLW method. The lowest limit of agreement was of −152.5 (95% CI = −216.76 to −88.23) and the highest limit of agreement was of 118.3 (95% CI = 53.98 to 182.51), showing a reliable limit of the 270.8 kcal [118.3 kcal − (−152.5 kcal)]. The percentage of error is 14% (reliable limit of 270.8 divided by the mean value of 1938 and multiplied by 100).
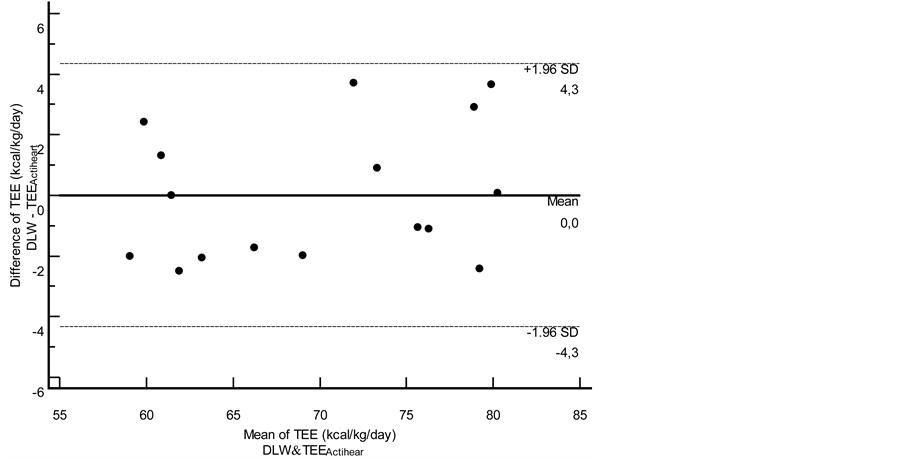
The TEE corrected by the body weight per day was analyzed to know if both results were also showing an adequate concordance. It was not possible to identify any significant difference for the means of both methods (69.8 ± 8.3 vs. 69.8 ± 7.8 kcal・kg−1・d, p = 0.98) after the t-test analysis was performed. The correlation analysis and the substantial strength of the agreement (Cb = 0.99) evidenced a strong relationship between both results (r = 0.96, p < 0.0001) (Figure 2).
The TEE mean (±SD) of the DLW method was 69.8 (±8.3) kcal・kg−1・d−1. The Actiheart’s TEE mean was 69.8 (±7.8) kcal・kg−1・d−1. The bias of the Actiheart was 0.0 kcal・kg−1・d−1 (95% CI = −1.17 to 1.18) showing that the Actiheart measured the same TEE than the DLW. The lowest limit of agreement was −4.32 (95% CI = −6.38 to −2.26), the highest limit of agreement was 4.34 (95% CI = 2.2869 to 6.4045), evidencing a reliable limit of the 8.6 kcal・kg−1・d−1 [4.34 kcal・kg−1・d−1 − (−4.32 kcal・kg−1・d−1)]. The percentage error is of 12% (reliable limit of 8.6 divided by mean value of 69.8 and multiplied by 100) (Figure 2).
5. Discussion
Up until a few years ago, there was no trustable method for measuring the EE in a free lifestyle condition in quantity terms; therefore, it was difficult to detect the differences of this variable among populations [27] .
With the introduction of the DLW method, it is now possible to obtain the EE measurements in quantity terms, and at the same time, to validate the methods that allow a more accurate and cheaper estimation of the EE short-term changes in groups of individuals [27] .
In the last years, the Actiheart monitor has measured the PAEE in an accurate way [28] and the results have been validated against the DLW technique; nevertheless, these studies have only calculated the EE provided by the PA. The EE results belong to one single portion of the daily TEE, but the most important measure to calculate in overweight and obese children is the daily TEE. Because of this, other studies have been performed, studies that allow to calculate the daily TEE in a free lifestyle condition in an accurate way using variables as the fat-free mass, the resting energy expenditure, Harris-Benedict equations [29] , and the use of non-invasive and low cost methods such as pedometers [12] [30] , HR monitors [9] and accelerometers [31] . These results have also been validated against the DLW technique.
Since the TEE estimation is the sum resulting from the addition of diverse variables, it is recommended to include the ECG [32] and the PAEE, which preferable has to be measured directly [33] with an ambulatory device,
Figure 1. Bland-Altman plot showing limits of agreement between TEEActiheart and DLW total energy expenditure measures (kcal・kg−1).
Figure 2. Bland-Altman plot showing limits of agreement between TEEActiheart and DLW total energy expenditure measures (kcal・kg−1・d−1).
Table 2. Energy expenditure of the schoolchildren using different methods (mean ± SD).
in order to obtain an accurate estimation of the TEE in the pediatric population.
The results of this study in which the ECG and the PAEE measured by the Actiheart were included, show the high correlation and concordance in the estimation of the daily TEE and the TEE adjusted by the student’s body weight when comparing the results with those obtained by the DLW technique. It also showed that the measurements of PAEE obtained by the Actiheart that were used for the calculation of the TEE provided an accurate estimation of it.
The difference between the TEE obtained by the DLW technique and the one calculated using the measurements provided by the Actiheart is considered minimum (17 kcal・d−1) in comparison with the differences reported in other studies that range between 24 to 98 kcal・d−1 and that were obtained by estimating the TEE using other monitors. These results were also compared against the DLW [34] [35] .
Wilson et al. [21] reported a similar calculation to the one obtained in this study. In their study, the TEE was estimated by using the Actiheart monitor in male schoolchildren with similar characteristics (ages range from 7 to 9 years old, height 120 cm, weight 27.04 kg, BMI 18.20), and they obtained an estimate TEE of 1986 ± 332 kcal・d−1. The difference between their study and this study is only 31 ± 67 kcal・d−1.
Wilson et al. [21] mention that one of the limitations responsible of the inadequate estimation of the TEE in their study was the deficient adhesion of the electrodes in the students’ skin because of the elevated rate of sweating caused by the high temperatures of the tropical zone where the study was performed. Because of this, the electrodes had to be changed more frequently. Such situation limited the permanent contact of the Actiheart with the chest of the children during the monitoring process. This also happened in another study done with adults located in high temperature geographic zones [18] . This limitation was not present in this study despite of the fact that the students wore the Actiheart for three consecutive days in the summer season; there was no need for replacement.
An unknown factor about Wilson et al. [21] study was the type of electrode used to place the Actiheart, which can also be a limiting factor in the adequate adhesion to the skin in case of a high sweating rate.
For Wilson et al. [21] , other limitation that may affect the correct calculation of the TEE is the young-age students’ ability to follow instructions, especially by avoiding touching the Actiheart since it could have caused an inadequate entry of the data. This situation was not a limitation in this study either, since both parents and students were provided with the correct induction of the methodology and this prevented what Wilson et al. [21] described.
The elements that allowed an accurate estimation of the TEE in this study were: 1) to request the students’ parents not to interfere in the usual physical activity patterns of their children in order to prevent a less accurate estimation of the EE, 2) the students were to keep the monitor every second including bedtime, 3) to use the Actiheart for two days of the week according to their normal school schedule and one day of the weekend, since some of the physical activity patterns and energy expenditure could vary. It is recommended to take into account the previous conditions for future studies.
It is important to remark a different aspect of this study, and that is the particularity of using the isotopic technique of DLW to validate the estimated TEE by the Actiheart in a free lifestyle condition, which is a new feature that had never been implemented among the Costa Rican schoolchildren.
The use of the non-invasive, low cost and easy to handle equipment to estimate the TEE in an accurate way, just as has been demonstrated by the Actiheart, is utterly important since the daily study of the TEE plays an important role in the prevention or treatment of several illnesses that are related to lifestyles such as overweight and obesity in schoolchildren. The increase of these conditions start by the age of six [36] [37] , and it has also been identified in Costa Rican schoolchildren with a prevalence of the 26.2% [38] .
6. Conclusion
The study concludes that the Actiheart monitor provides highly reliable data and its use in future researches will allow an estimation of the TEE at lower cost using a larger sample of Costa Rican schoolchildren that present either overweight or obesity.
Disclosure
The authors declared no conflict of interest.
Cite this paper
Juan DiegoZamora-Salas,AdrianaLaclé-Murray, (2015) Validation of Total Daily Energy Expenditure Calculated with Actiheart against Doubly Labeled Water Method in Costa Rican Schoolchildren. Food and Nutrition Sciences,06,1193-1201. doi: 10.4236/fns.2015.613125
References
- 1. Pereira, A.P., Seabra, T.A., Silva, G.R., Katzmarzyk, T.K., Beunen, P.G. and Maia, J.A. (2010) Prevalence of Overweight, Obesity and Physical Activity Levels in Children from Azores Islands. Annals of Human Biology, 37, 682-691.
http://dx.doi.org/10.3109/03014461003639223 - 2. Pirinçci, E., Durmus, B., Gündo-Gdu, C. and Açik, Y. (2010) Prevalence and Risk factors of Overweight and Obesity among Urban School Children in Elazing City (Eastern Turkey, 2007). Annals of Human Biology, 37, 44-56.
http://dx.doi.org/10.3109/03014460903218984 - 3. Katzmarzyk, P.T., Baur, L.A., Blair, S.N., Lambert, E.V., Oppert, J.M. and Riddoch, C. (2008) Expert Panel Report from the International Conference on Physical Activity and Obesity in Children, 24-27 June 2007, Toronto, Ontario: Summary Statement and Recommendations. Applied Physiology Nutrition and Metabolism, 33, 371-388.
http://dx.doi.org/10.1139/H07-176 - 4. Aballay, L.R., Eynard, A.R., Díaz, M.P., Navarro, A. and Muñoz, S.E. (2013) Overweight and Obesity: The Relationship to Metabolic Syndrome, Cardiovascular Disease, and Cancer in South America. Nutrition Reviews, 71, 168-179.
http://dx.doi.org/10.1111/j.1753-4887.2012.00533.x - 5. Ball, K., Cleland, V., Timperio, A., Salmon, J. and Crawford, D. (2009) Socioeconomic Position and Children’s Physical Activity and Sedentary Behaviors: Longitudinal Findings from the CLAN Study. Journal of Physical Activity and Health, 6, 289-298.
- 6. Audelin, M.C., Savage, P.D., Toth, M.J., Harvey-Berino, J., Schneider, D.J., Bunn, J.Y., et al. (2011) Change of Energy Expenditure from Physical Activity Is the Most Powerful Determinant of Improved Insulin Sensitivity in Overweight Patients with Coronary Artery Disease Participating in an Intensive Lifestyle Modification Program. Metabolism, 61, 672-679.
http://dx.doi.org/10.1016/j.metabol.2011.10.001 - 7. Slinde, F., Grönberg, A.M., Svantesson, U., Hulthén, L. and Larsson, S. (2011) Energy Expenditure in Chronic Obstructive Pulmonary Disease-Evaluation of Simple Measures. European Journal of Clinical Nutrition, 65, 1309-1313.
http://dx.doi.org/10.1038/ejcn.2011.117 - 8. Takken, T., Stephens, S., Balemans, A., Tremblay, M., Esliger, D., Schneiderman, J., et al. (2010) Validation of the Actiheart™ Activity Monitor for Measurement of Activity Energy Expenditure in Children and Adolescents with Chronic Disease. European Journal of Clinical Nutrition, 64, 1494-1500.
http://dx.doi.org/10.1038/ejcn.2010.196 - 9. Yu, Z., Völgyi, E., Wang, R., et al. (2012) Comparison of Heart Rate Monitoring with Indirect Calorimetry for Energy Expenditure Evaluation. Journal of Sport and Health Science, 1, 178-183.
http://dx.doi.org/10.1016/j.jshs.2012.07.004 - 10. Abrams, S.A. and Wong, W.W. (2003) Stable Isotopes in Human Nutrition. Laboratory Methods and Research Applications. CABI Publishing, London.
http://dx.doi.org/10.1079/9780851996769.0000 - 11. Bouchard, D.R. and Trudeau, F. (2008) Estimation of Energy Expenditure in a Work Environment: Comparison of Accelerometry and Oxygen Consumption/Heart Rate Regression. Ergonomics, 51, 663-670.
http://dx.doi.org/10.1080/00140130701780484 - 12. Hoyt, R.W., Buller, M.J., Santee, W.R., Yokota, M., Weyand, P.G. and Delany, J.P. (2004) Total Energy Expenditure Estimated Using Foot-Ground Contact Pedometry. Diabetes Technology & Therapeutics, 6, 71-81.
http://dx.doi.org/10.1089/152091504322783459 - 13. Plasqui, G., Joosen, A.M., Kester, A.D., Goris, A.H. and Westerterp, K.R. (2005) Measuring Free-Living Energy Expenditure and Physical Activity with Triaxial Accelerometry. Obesity Research, 13, 1363-1369.
http://dx.doi.org/10.1038/oby.2005.165 - 14. Butte, N.F., Wong, W.W., Adolph, A.L., Puyau, M.R., Vohra, F.A. and Zakeri, I.F. (2010) Validation of Cross-Sectional Time Series and Multivariate Adaptive Regression Splines Models for the Prediction of Energy Expenditure in Children and Adolescents Using Doubly Labeled Water. Journal of Nutrition, 140, 1516-1523.
http://dx.doi.org/10.3945/jn.109.120162 - 15. Green, J.A., Halsey, L.G., Wilson, R.P. and Frappell, P.B. (2009) Estimating Energy Expenditure of Animals Using the Accelerometry Technique: Activity, Inactivity and Comparison with the Heart-Rate Technique. The Journal of Experimental Biology, 212, 471-482.
http://dx.doi.org/10.1242/jeb.026377 - 16. Zakeri, I.F., Adolph, A.L., Puyau, M.R., Vohra, F.A. and Butte, N.F. (2008) Application of Cross-Sectional Time Series Modeling for the Prediction of Energy Expenditure from Heart Rate and Accelerometry. Journal of Applied Physiology, 104, 1665-1673.
http://dx.doi.org/10.1152/japplphysiol.01163.2007 - 17. Brage, S., Brage, N., Franks, P.W., Ekelund, U., Wong, M.Y., Andersen, L.B., Froberg, K. and Wareham, N.J. (2004) Branched Equation Modeling of Simultaneous Accelerometry and Heart Rate Monitoring Improves Estimate of Directly Measured Physical Activity Energy Expenditure. Journal of Applied Physiology, 96, 343-351.
http://dx.doi.org/10.1152/japplphysiol.00703.2003 - 18. Assah, F.K., Ekelund, U., Brage, S., Wright, A., Mbanya, J.C. and Wareham, N.J. (2011) Accuracy and Validity of a Combined Heart Rate and Motion Sensor for the Measurement of Free-Living Physical Activity Energy Expenditure in Adults in Cameroon. International Journal of Epidemiology, 40, 112-120.
http://dx.doi.org/10.1093/ije/dyq098 - 19. Barreira, T.V., Kang, M., Caputo, J.L., Farley, R.S. and Renfrow, M.S. (2009) Validation of the Actiheart™ Monitor for the Measurement of Physical Activity. International Journal of Exercise Science, 2, 60-71.
- 20. Van Remoortel, H., Giavedoni, S., Raste, Y., et al. (2012) Validity of Activity Monitors in Health and Chronic Disease: A Systematic Review. International Journal Behavioral Nutrition and Physical Activity, 9, 84.
http://dx.doi.org/10.1186/1479-5868-9-84 - 21. Wilson, H., Dickinson, F., Griffiths, P., Bogin, B. and Varela-Silva, M. (2011) Logistics of Using the Actiheart™ Physical Activity Monitors in Urban Mexico among 7- to 9-Year-Old Children. American Journal of Human Biology, 23, 426-428.
http://dx.doi.org/10.1002/ajhb.21150 - 22. Schofield, W.N. (1985) Predicting BMR: New Standard and Review of Previous Work. Human Nutrition Clinical Nutrition, 39, 5-41.
- 23. Henry, C.J. and Rees, D.G. (1991) New Predictive Equations for the Estimation of Basal Metabolic Rate in Tropical Peoples. European Journal of Clinical Nutrition, 45, 177-185.
- 24. FAO/WHO/UNU (2001) Report of Expert Consultation. Human Energy Requirement, Rome, 1-96.
- 25. Lin, L.I. (1989) A Concordance Correlation Coefficient to Evaluate Reproducibility. Biometrics, 45, 255-268.
http://dx.doi.org/10.2307/2532051 - 26. Bland, J.M. and Altman, D.G. (1986) Statistical Methods for Assessing Agreement between Two Methods of Clinical Measurement. The Lancet, 1, 307-310.
http://dx.doi.org/10.1016/S0140-6736(86)90837-8 - 27. Bratteby, L., Sandhagen, B., Fan, H. and Samuelson, G. (1997) A 7-Day Activity Diary for Assessment of Daily Energy Expenditure Validated by the Doubly Labelled Water Method in Adolescents. European Journal of Clinical Nutrition, 51, 585-591.
http://dx.doi.org/10.1038/sj.ejcn.1600449 - 28. Maddison, R., Jiang, Y., Hoorn, S.V., Mhurchu, C.N., Lawes, C.M., Rodgers, A. and Rush, E. (2009) Estimating Energy Expenditure with the RT3 Triaxial Accelerometer. Research Quarterly for Exercise and Sport, 80, 249-256.
http://dx.doi.org/10.1080/02701367.2009.10599559 - 29. Kien, C.L. and Ugrasbul, F. (2004) Prediction of Daily Energy Expenditure during a Feeding Trial Using Measurements of Resting Energy Expenditure, Fat-Free Mass, or Harris-Benedict Equations. The American Journal of Clinical Nutrition, 80, 876-880.
- 30. Tharion, W.J., Yokota, M., Buller, M.J., DeLany, J.P. and Hoyt, R.W. (2004) Total Energy Expenditure Estimated Using a Foot-Contact Pedometer. Medical Science Monitor, 10, CR504-CR509.
- 31. Bonomi, A., Plasqui, G., Goris, A. and Westerterp, K. (2009) Improving Assessment of Daily Energy Expenditure by Identifying Types of Physical Activity with a Single Accelerometer. Journal of Applied Physiology, 107, 655-661.
http://dx.doi.org/10.1152/japplphysiol.00150.2009 - 32. Wen, W., Piao, J. and Zhuo, Q. (2010) Energy Requirements of Children and Adolescents. Journal of Hygiene Research, 39, 790-794.
- 33. Yu, C.W., Sung, R.Y., So, R., Lam, K., Nelson, E.A., Li, A.M.C., Yuan, Y. and Lam, P.K.W. (2002) Energy Expenditure and Physical Activity of Obese Children: Cross-Sectional Study. Hong Kong Medical Journal, 8, 313-317.
- 34. Moore, S.A., Hallsworth, K., Bluck, L., Ford, G.A., Rochester, L. and Trenell, M.I. (2012) Measuring Energy Expenditure after Stroke Validation of a Portable Device. Stroke, 43, 1660-1662.
http://dx.doi.org/10.1161/STROKEAHA.111.646257 - 35. Spierer, D.K., Hagins, M., Rundle, A. and Pappas, E. (2011) A Comparison of Energy Expenditure Estimates from the Actiheart™ and Actical Physical Activity Monitors during Low Intensity Activities, Walking, and Jogging. European Journal of Applied Physiology, 111, 659-667.
http://dx.doi.org/10.1007/s00421-010-1672-7 - 36. Kain, J., Corvalán, C., Lera, L., Galván, M. and Uauy, R. (2009) Accelerated Growth in Early Life and Obesity in Preschool Children. Obesity, 17, 1603-1608.
http://dx.doi.org/10.1038/oby.2009.37 - 37. Ogden, C.L., Carroll, M.D., Curtin, L.R., McDowell, M.A., Tabak, C.J. and Flegal, K.N. (2006) Prevalence of Overweight and Obesity in the United States, 1999-2004. Journal of the American Medical Association, 295, 1549-1555.
http://dx.doi.org/10.1001/jama.295.13.1549 - 38. Núñez, H., Monge, R., León, H. and Roselló, M. (2003) Prevalence of Overweight and Obesity among Costa Rican Elementary School Children. Pan American Journal of Public Health, 13, 24-32.
Abbreviations
AC: Accelerometer.
BMI: Body Mass Index.
BMR: Basal Metabolic Rate.
DLW: Doubly Labeled Water.
ECG: Energy Cost of Growth.
EE: Energy Expenditure.
HR: Heart Rate.
PA: Physical Activity.
PAEE: Physical Activity Energy Expenditure.
TEE: Total Energy Expenditure.