Advances in Lung Cancer
Vol.2 No.3(2013), Article ID:35417,8 pages DOI:10.4236/alc.2013.23008
A pilot double-blind, randomized, placebo-controlled trial of curcumin/bioperine for lung cancer chemoprevention in patients with chronic obstructive pulmonary disease*
![]()
1Department of Medicine, Baylor College of Medicine, Houston, USA; #Corresponding Author: amirs@bcm.edu
2Medical Care Line, Michael E. DeBakey VA Medical Center, Houston, USA
3Department of Biostatistics, The University of Texas MD Anderson Cancer Center, Houston, USA
4Department of Pathology, The University of Texas MD Anderson Cancer Center, Houston, USA
5Department of Experimental Therapeutics, The University of Texas MD Anderson Cancer Center, Houston, USA
6Department of Pulmonary Medicine, The University of Texas MD Anderson Cancer Center, Houston, USA
7Division of Cancer Medicine, The University of Texas MD Anderson Cancer Center, Houston, USA
8Department of Thoracic/Head and Neck Medical Oncology, The University of Texas MD Anderson Cancer Center, Houston, USA
Copyright © 2013 Amir Sharafkhaneh et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received 27 March 2013; revised 30 April 2013; accepted 10 May 2013
Keywords: Lung Cancer; Inflammation; Nutraceutical Agents; COPD; Cytological Abnormalities
ABSTRACT
Chronic obstructive pulmonary disease is an inflammatory condition with increased risk of lung cancer. We hypothesized that curcumin/ bioperine (CB), which has anti-inflammatory effects, may reduce cytological abnormalities in the sputum of patients with COPD. We conducted a 3-month, three-to-one randomized, doubleblind, pilot trial of escalating doses of CB in patients with moderate or worse COPD who were capable of producing sputum. The primary efficacy endpoint was changed in sputum cytology. We also explored changes in fluorescence in situ hybridization (FISH). We obtained sputum samples for cytology and chromosome abnormalities at baseline and each monthly follow-up visit. We enrolled 57 participants, with 35 completing the study. The participants’ mean age (standard deviation [SD]) was 66.6 (8.2) years, and they were mainly male (91.2%), with an average of 63.8 pack-years of smoking history. Also, 42.1% of participants were active smokers and the mean (SD) FEV1 was 37% (13%). At baseline, 13 subjects had moderate or worse dysplasia (22.8%). Subjects with moderate to severe sputum dysplasia had more chromosome abnormalities in epithelial cells and neutrophils, as measured by deletion and aneuploidy in 10q22.3. The changes in sputum cytology and chromosome abnormalities did not differ between the active and placebo arms. CB was well tolerated at the bid doses of 1, 1.5, and 2 gm of curcumin and 5 mg of bioperine, with minor side effects related to the gastrointestinal tract. In this short pilot trial, CB compared to placebo did not alter cytological and chromosomal abnormalities seen in sputum of patients with COPD.
1. INTRODUCTION
Chronic obstructive pulmonary disease (COPD) is a debilitating disease that results in significant morbidity and mortality. Physiologically, COPD is characterized by expiratory airflow limitation that is partially reversible [1]. Pathologically, COPD is characterized by emphysema, small airway wall thickening, mucous metaplasia, occlusion of small airways with inflammatory mucus, and mucous gland hypertrophy and hyperplasia in large airways [2-4]. Various inflammatory cells including macrophages, neutrophils and CD8—T lymphocytes are increased in the airways of patients with COPD [2]. Associated with these inflammatory changes, COPD patients exhibit varying degrees of dysplasia upon cytologic examination of sputum or bronchial biopsy. Among smokers, there is a statistically significant increased risk of lung cancer in those patients with coexistent COPD [5]. Interestingly, cancer ensued up to 5 years after the initial abnormal sputum, with an accumulation of worsening cytopathologic findings until cancer was diagnosed. The association between inflammation and lung cancer in COPD patients has led to the hypothesis that targeting aspects of the inflammatory response will reverse premalignancy and reduce lung cancer risk in COPD patients.
Curcumin (diferuloylmethane) is a potent anti-inflammatory agent that has shown substantial anticarcinogenic properties in cellular and animal models of cancer [6,7]. Its efficacy has been attributed to its capacity to inhibit the NFkB transcription factor, which regulates inflammation, angiogenesis, and tumor cell survival, invasion, and metastasis [8]. Several clinical trials have revealed activity of curcumin in cancer patients [9]. In a dose-escalation study of 15 patients with advanced colorectal cancer refractory to standard treatment, study subjects received doses of 440 to 2200 mg/day of curcuma extracts (containing 36 - 180 mg of curcumin) daily for 4 months. Five patients had radiologically stable disease during treatment for 2 to 4 months [10]. Cruz-Correa and colleagues demonstrated a dramatic reduction in polyps (60.4%) in patients with familial adenomatous polyposis (FAP) treated with curcumin and quercetin, further demonstrating the potential of the combination [11].
Because clinical and preclinical studies have shown that curcumin has poor bioavailability, Shoba and colleagues examined the effects of piperine on the bioavailability of curcumin in rats and healthy volunteers [12]. When curcumin was given to rats at a dose of 2 g/kg with concomitant piperine at a dose of 20 mg/kg, the serum concentration of curcumin increased and its bioavailability increased by 154% compared to that of curcumin given alone. Also, the time to maximum concentration significantly increased (P < 0.002), and the rate of clearance significantly decreased (P < 0.02). In healthy volunteers, serum levels of curcumin were very low or undetectable (approximately 0.006 pg/ml) 1 hr after a 2 g dose. When piperine was added at a dose of 20 mg, significantly higher concentrations of curcumin (as much as 0.18 pg/ml) were observed 1 hr after administration for up to 0.75 hours (P < 0.01). These concentrations decreased to 0 by 3 hr after administration. No toxicity with curcumin or piperine was reported at these doses.
Given the association between airway inflammation and lung cancer risk in COPD patients, in this study we evaluated the effects of the curcumin/bioperine (an extract of piperine) combination on epithelial and FISH detected abnormalities, lung function, and exercise capacity in a 3-month dose-escalation, double-blind, randomized, pilot clinical trial in patients with COPD.
2. MATERIALS AND METHODS
This was a pilot study with intent to evaluate cytology changes in sputum by treatment of curcumin plus bioperine (CB). The ultimate goal was to gain information for planning a large scale study using CB. A total of 40 patients were planned to be enrolled, 30 in CB and 10 in placebo groups. The protocol was approved by the Baylor College of Medicine Institutional Review Board and the Research and Development Committee of the Michael E. DeBakey Veterans Affairs Medical Center (MEDVAMC) in Houston, Texas, USA. The study was conducted between August 2006 and March 2008. The clinical investigation described herein was conducted in accordance with the guidelines in The Declaration of Helsinki. All subjects provided written informed consent.
2.1. Study Subjects
The potential subjects were recruited from our pulmonary clinics at the MEDVAMC. We enrolled subjects with COPD who were at least 40 years old and who had a smoking history of at least 10 pack-years and a history of chronic bronchitis to increase the likelihood of sputum production. Subjects with a history of COPD exacerbations within the previous 8 weeks; other chronic respiratory conditions, including asthma, symptomatic heart failure, liver failure, or renal failure; any cancer within the past 5 years; or any lung or upper airway cancer were excluded. After signing the consent form, the study subjects underwent spirometry to test for COPD, which we defined as an FEV1/FVC ratio < 70% (ref GOLD guideline). Subjects who did not meet the spirometry criteria for COPD were excluded from the study. Furthermore, subjects who were not able to produce sputum at the time of consent were excluded. We screened 75 subjects from who 59 subjects met the study criteria; 1 subsequently withdrew consent and 1 was already in another study and was excluded. Thus, 57 patients enrolled in the study and received at least one dose of the study agents/placebo. Thirty-five patients completed the study. Among the 22 patients who dropped out of the study, 12 dropped out after baseline evaluation, 5 after 1 month, and 5 after 2 months (Figure 1).
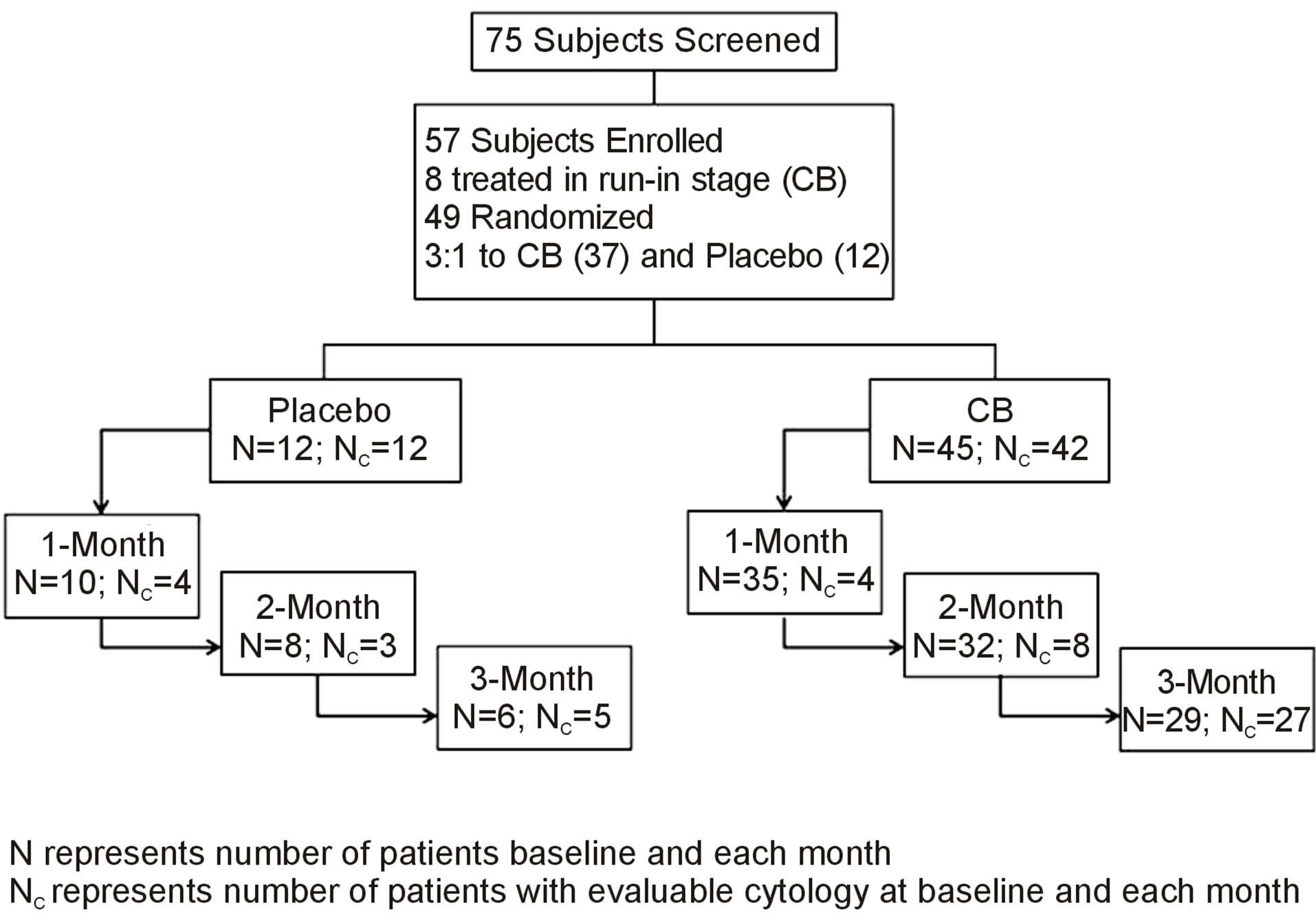
Figure 1. The consort diagram.
2.2. Study Design
The curcumin, bioperine, and placebo were obtained pre-packaged from Sabinsa Corporation (East Windsor, New Jersey, USA). The study medication/placebo was stored in the MEDVAMC research pharmacy and was dispensed by the research pharmacist. Each capsule contained 500 mg of curcumin and each tablet contained 5 mg of bioperine. We initially enrolled 8 participants in an open-label study to evaluate the safety and tolerability of curcumin plus bioperine (CB). The dosing schedule was similar (see below) to the double-blinded part of the study. Subsequently, the participants were randomized (3 to 1) to receive CB versus placebo, a design intended to maximize the number of patients who receive the active drug. Each participant received CB at 1 g curcumin/5mg bioperine b.i.d. for a month, then CB at 1.5 g/5mg b.i.d. for a month, and finally, CB at 2 g/5 mg b.i.d. for an additional month. The escalating doses design was used for the concern of safety in the COPD population. The participants were seen at the research clinic at the MEDVAMC at baseline, one, two and three months after randomization. At each visit, the participants were asked to give a sputum sample. On the first visit, following inhalation of nebulized 3% saline, the participants were instructed to cough into a container filled with Sacommano’s fixative (90% alcohol, 5% acetic acid, and 5% polyethylene glycol). For subsequent visits, the participants were given containers with the fixative to take home. The participants were instructed to cough their morning sputum into the container on the day of their visit to the research center.
After the collection of sputum samples, spirometry tests were performed. For spirometry, we obtained at least three reproducible forced expiratory maneuvers. For the forced maneuvers, each subject was instructed to inspire to total lung capacity and then to expire with maximal effort to residual volume. Quality control measures as outlined by the American Thoracic Society were used to select appropriate maneuvers [13]. Each subject was instructed to expire forcefully for at least 6 seconds. Subsequently, the subjects underwent a 6-minute walk test according to the guidelines published by the American Thoracic Society [14].
2.3. Sputum Cytologic Analysis
The sputum samples were transferred to the cytology laboratory at The University of Texas MD Anderson Cancer Center for processing. Samples were transferred to 50-mL conical tubes and centrifuged at 1500 rpm for 10 minutes. Supernatant was removed, leaving behind 2 - 3 mL of the solution with the cell pellet. Four millimeters of 1X phosphate-buffered saline (PBS) was added to the cell pellet and centrifuged at 1500 rpm for 5 minutes. The supernatant was discarded and 4 mL of pre-warmed 3.25-mM Sputolysin (0.05 g DDT, 5 mL PBS, and 45 mL H2O) was added to the cell pellet and incubated for 5 minutes at 37˚C in the incubator. Next, the supernatant was discarded and the cell pellet was washed with 1X PBS and saved. Finally, 2 mL of 50% ethanol was added to the cell pellet, which was then divided and mounted on several super-frosted slides. One Diff Quick slide was made to check the cellularity and adequacy of the sample (at least 10 macrophages per slide were required for a slide to be deemed adequate). Once the cellularity and adequacy were determined, cytospins were made using a Shandon Cytocentrifuge (Thermo Fisher Scientific Inc., Waltham, MA). Two slides were fixed in 95% ethanol for Papanicolaou staining, and the rest of the slides were fixed in Carnoy’s fixative (3:1, methanol:acetic acid) for FISH analysis. Samples were given a score (negative, squamous metaplasia, or mild, moderate, or severe dysplasia) using standard criteria [15].
2.4. FISH Analysis
We used fluorescence in situ hybridization (FISH) to analyze abnormal gene amplifications and/or deletions in epithelial cells and neutrophils in sputum at baseline and at monthly follow-up. Two-color FISH was performed on sputum samples using in-house bacterial artificial chromosome probes for 3p22.1 and 10q22.3. For internal controls, we combined in-house 3p22.1 (green) probe with the centromeric 3 (orange) probe and the 10q22.3 (green) probe with the centromeric 10 (orange) probe (centromeric 3 and 10 probes obtained from Vysis, Inc.; Downers Grove, IL). One slide was used for centromeric 3 and 3p22.1 FISH assay and another slide was used for centromeric 10 and 10q22.3 FISH assay.
Slides were pretreated in 2X sodium saline citrate (SSC) for 2 minutes at 73˚C, digested in Protease (Vysis, Inc.) solution (50 mL of 1X PBS [pH < 2.0] at 37˚C and 25 mg of protease), washed with 1X PBS, fixed with 1% formaldehyde, and rinsed again with 1X PBS. Slides were then dehydrated in a series of 70%, 85%, and 100% ethanol. Seven microliters of probe preparation was applied to each slide, slides were covered with a small coverslip, and rubber cement was applied. Slides were kept in a Hybrid machine (Vysis, Inc.; Downers Grove, IL) using a melting temperature of 77˚C for 5 minutes and then incubated at 37˚C for 18 - 20 hrs.
The next day after hybridization, the slides were washed using 0.4X SSC/0.3% NP-40 for 2 minutes at 74˚C and then 2X SSC/0.1% NP-40 at room temperature for 1 minute. Slides were counterstained with 10 µL of DAPI (4,6-diamidino-2-phenylindole) and visualized under a fluorescent microscope equipped with triple, red and green dual band, single green, and red filters.
2.5. Manual and Automated Scoring of FISH Signals
For each sample, at least 100 epithelial cells were scored manually for deletions of centromeric 3, 3p22.1, centromeric 10, and 10q22.3 and for other chromosomal abnormalities, including aneusomy or gain of any chromosomal material compared to an internal centromeric probe. Single non-overlapping cells with good FISH signals were scored. Cells with chromosomal abnormalities were selected. At the same time and in the same fields, neutrophils were also scored for similar abnormalities.
For centromeric 3 and 3p probes, 2 orange (centromeric 3) and two green (locus specific 3p21) signals were classified as normal, cells with 2 orange signals and 1 green signal were put in the 3p deletion class, cells with 2 orange signals and 3 green signals were classified as having polysomy, and cells with more than 2 signals for green and orange were classified as aneuploid. At least 100 consecutive non-overlapping epithelial cells and 100 neutrophils were analyzed for each sample. A similar scheme of classification existed for scoring abnormalities of chromosome 10 and locus specific 10q22.3 where chromosome 10 was orange and 10q22.3 was green.
Slides for 3p22.1/centromeric 3 and 10q22.3/centromeric10 probes were scanned separately using the Bioview Duet™ automated scanner (Bioview Ltd., Nes Ziona, Israel). The automated system scans and classifies each FISH probe into normal class (2 green [G]:2 orange [O]), 3p deletions (1 G:2 O), 10q deletions (1 G:2 O), polysomy of 3p (3 G:2 O), polysomy of 10q (3 G:2 O), and abnormal class (>2 G:>2 O). After automated scanning, the operator checks the accuracy of the machine classification and reclassifies the cells visually as defined above, based on the number of orange and green signals present, if there is disagreement with the machine classification.
2.6. Statistical Analysis
The original sample size calculation of this study was based on modulation of a continuous marker in the sputum over time. With 40 patients, 30 and 10 in the active treatment and placebo groups (3:1), respectively, we would have 86% power to detect an effect size of 1.14 using two-sided t-test with a two-sided significance level of 0.05. With a 10% drop-out rate, the study will still have more than 80% power. Subsequently, the primary endpoint was revised to be the change of cytology score by one or more level in the sputum. The percentage of changes in each group from baseline to 3 months after treatment would be estimated. Fisher’s exact test will be applied to compare the percentage of changes between the CB and the placebo group.
Summary statistics, including frequency tabulation, means, and standard deviations, were given to describe subject characteristics, cytology readings, and FISH results. Fisher’s exact test was applied to compare the proportions of improved cytology from baseline to posttreatment between the two treatment groups. The Wilcoxon rank sum test was used to compare baseline FISH results between two cytology groups and the difference in FISH results between two treatment groups.
3. RESULTS
Table 1 shows the demographic data for the 57 subjects who were randomized in this study. The mean age was 66.6 years, and subjects had smoked substantially, with average pack-years of 63.8. Pulmonary function tests showed that the patient population suffered from severe COPD, defined as forced expiratory volume in 1 second (FEV1) ≤ 50% of predicted.
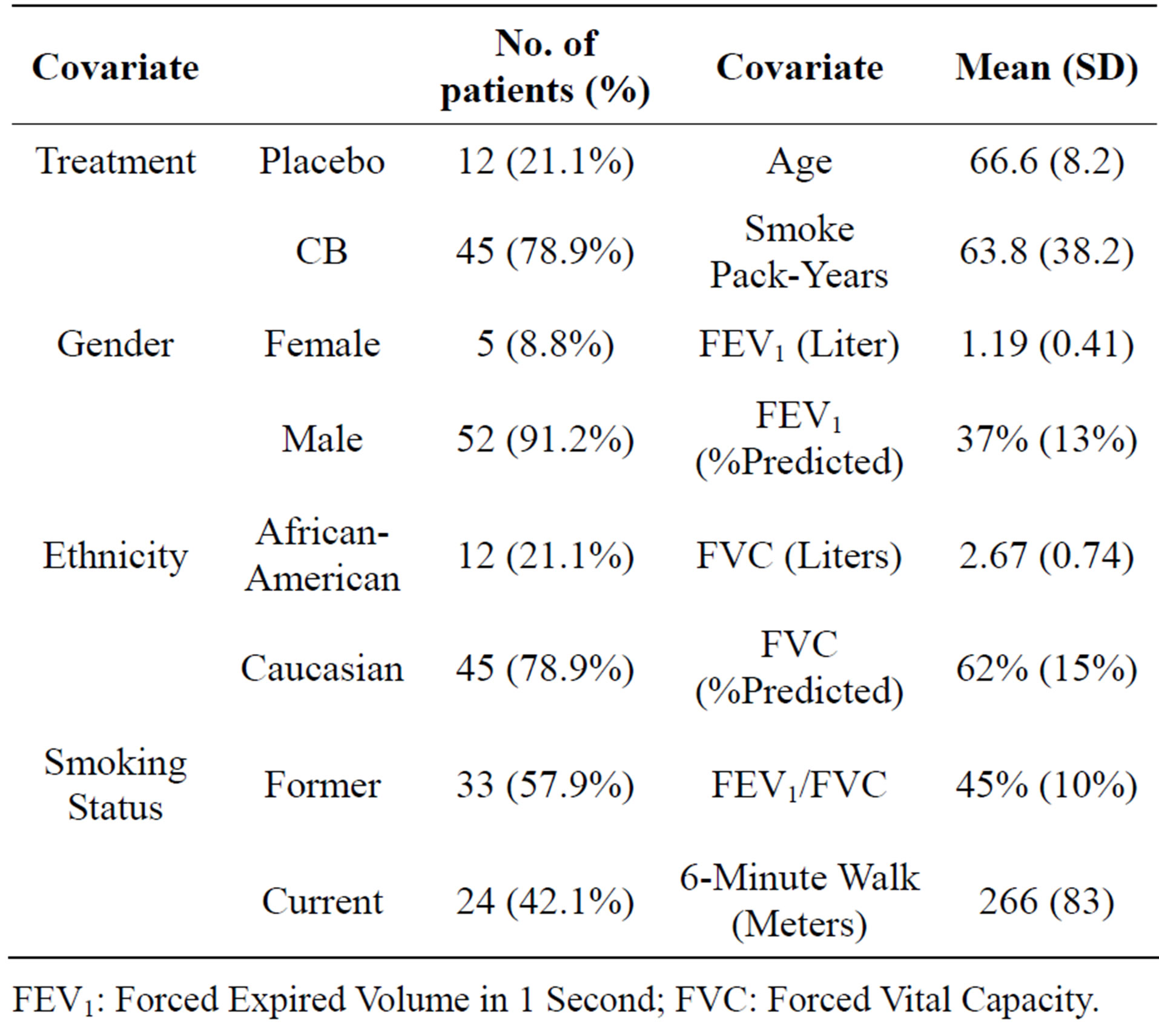
Table 1. Demographic and treatment information for 57 patients who received treatment.
FEV1: Forced Expired Volume in 1 Second; FVC: Forced Vital Capacity.
A total of 12 and 45 patients were randomized into the placebo and active treatment groups, respectively. Table 2 shows the baseline sputum cytology data for the two treatment groups. Thirteen of 57 patients at baseline showed advanced dysplasia (moderate or worse) (22.8%). Of these, four subjects (33%) in the placebo group and nine (20%) in the active arm had advanced dysplasia.
Table 3 shows changes in cytology before and after treatment in evaluable patients. The sputum samples at follow-up contained evaluable cells in only 28 and 5 participants in active and placebo groups, respectively. In the active treatment group, 12 of 28 patients had improved cytology, which included 6 patients with moderate dysplasia at baseline (one down-regulated to negative, one to squamous metaplasia, and four to mild dysplasia), 3 patients with mild dysplasia (one down-regulated to negative and two to squamous metaplasia), and 3 patients with squamous metaplasia (all down-regulated to negative). In the placebo group, 3 of 5 patients had improved cytology, which included one patient who went from
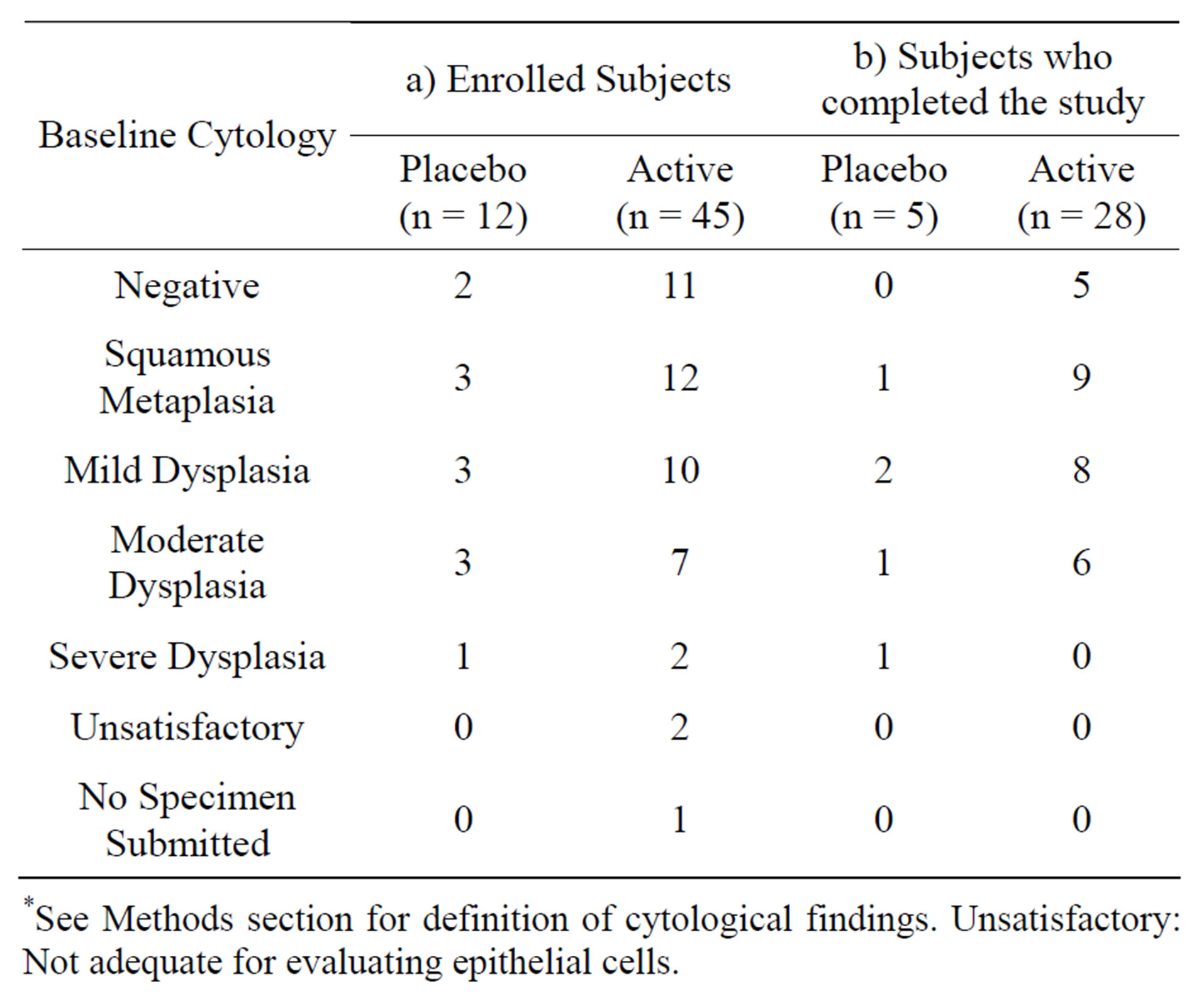
Table 2. Baseline cytology by treatment assignment for all a) Enrolled subjects & b) Subjects who completed the study AND have both baseline and 3-month cytology reading*.
*See Methods section for definition of cytological findings. Unsatisfactory: Not adequate for evaluating epithelial cells.
having severe dysplasia to moderate dysplasia, one from moderate dysplasia to negative, and one from mild dysplasia to squamous metaplasia. Overall, 43% of the curcumin/bioperine-treated patients and 60% of the placebo patients had improved cytology. The changes in cytological abnormalities did not differ between the active treatment and placebo groups (p = 0.64, Fisher’s exact test).
The main abnormalities detected by FISH analysis were at chromosomes 3p22.1 and 10q22.3 in the form of deletion and aneuploidy (Table 4). At both 3p22.1 and 10q22.3 chromosomal regions, all measurements had higher mean values of chromosomal abnormalities (gains and deletions) in samples with moderate or worse dysplasia compared with the lower severity group. In epithelial cells, the mean (SD) deletions of 10q22.3 were 4.64 (±2.91) in sputum with advanced cytological abnormalities vs. 2.14 (±1.77) in sputum with low-grade cytologycal abnormalities (p = 0.02). In neutrophils, the mean (SD) deletions of 10q were 2.64 (±4.03) in sputum with advanced cytological abnormalities versus 0.29 (±0.64) in sputum with low-grade cytological abnormalities (p = 0.02). Similarly, in epithelial cells, the mean (SD) aneuploidy of 10q22.3 was 5.09 (±3.30) in sputum with advanced cytological abnormalities versus 2.62 (±2.36) in sputum with low-grade cytological abnormalities (p = 0.04). In neutrophils, the aneuploidy of 10q22.3 was 3.55 (±4.51) in sputum with advanced cytological abnormalities versus 0.67 (±1.28) in sputum with low-grade cytological abnormalities (p = 0.05). Similar findings were seen in chromosome 3p22.1, but the differences in FISH results between the two histology groups were not statistically significant. For the FISH analysis, the treatment effect on abnormal cells did not differ significantly between the active treatment and placebo groups, although only 4 samples in the placebo group and 21 samples in the active group were analyzed (data not shown).
Table 5 shows lung function data at baseline and 3-month follow-up in the study participants. On average, lung function parameters remained unchanged in active
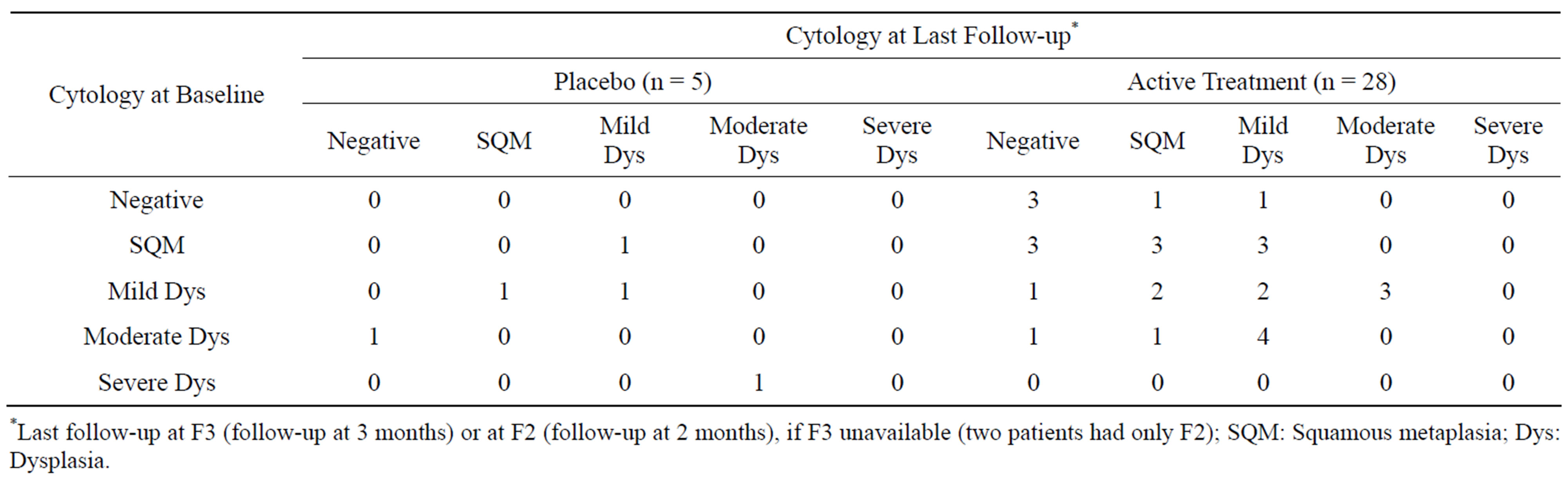
Table 3. Treatment effect on cytology.
*Last follow-up at F3 (follow-up at 3 months) or at F2 (follow-up at 2 months), if F3 unavailable (two patients had only F2); SQM: Squamous metaplasia; Dys: Dysplasia.
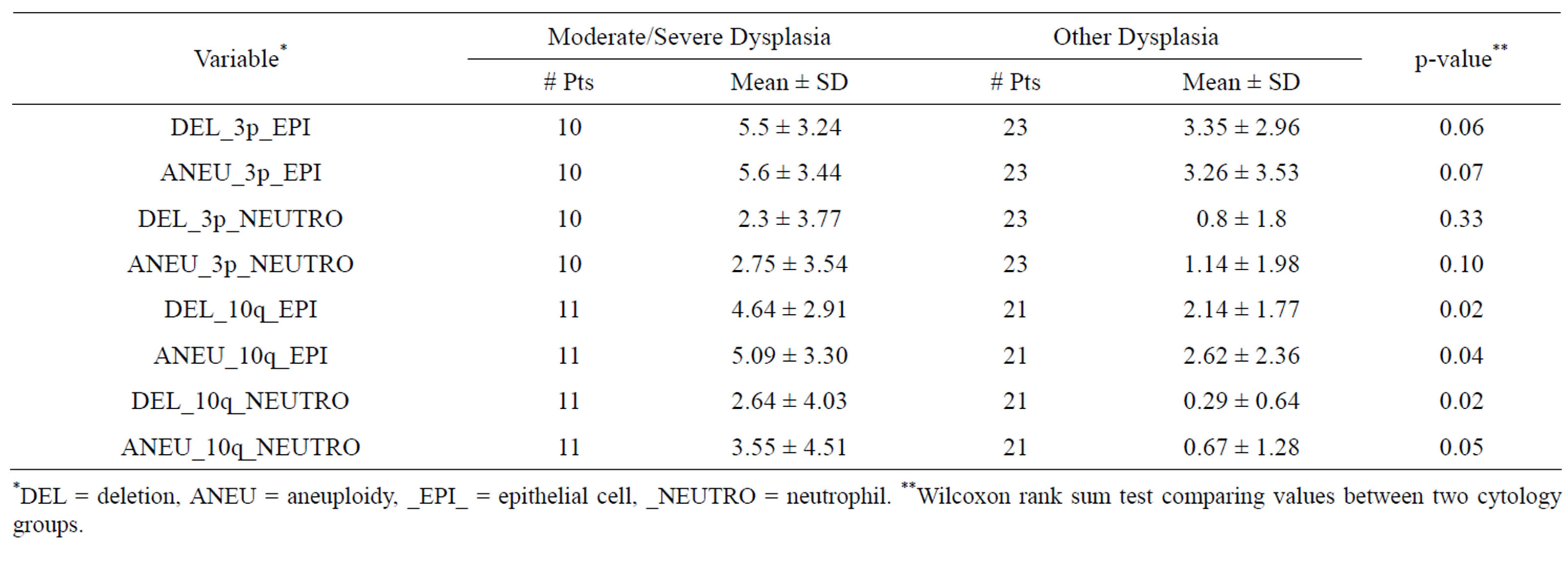
Table 4. Baseline FISH Analysis of Chromosomes 3p22.1 and 10q22.3 by Severity of Dysplasia.
*DEL = deletion, ANEU = aneuploidy, _EPI_ = epithelial cell, _NEUTRO = neutrophil. **Wilcoxon rank sum test comparing values between two cytology groups.
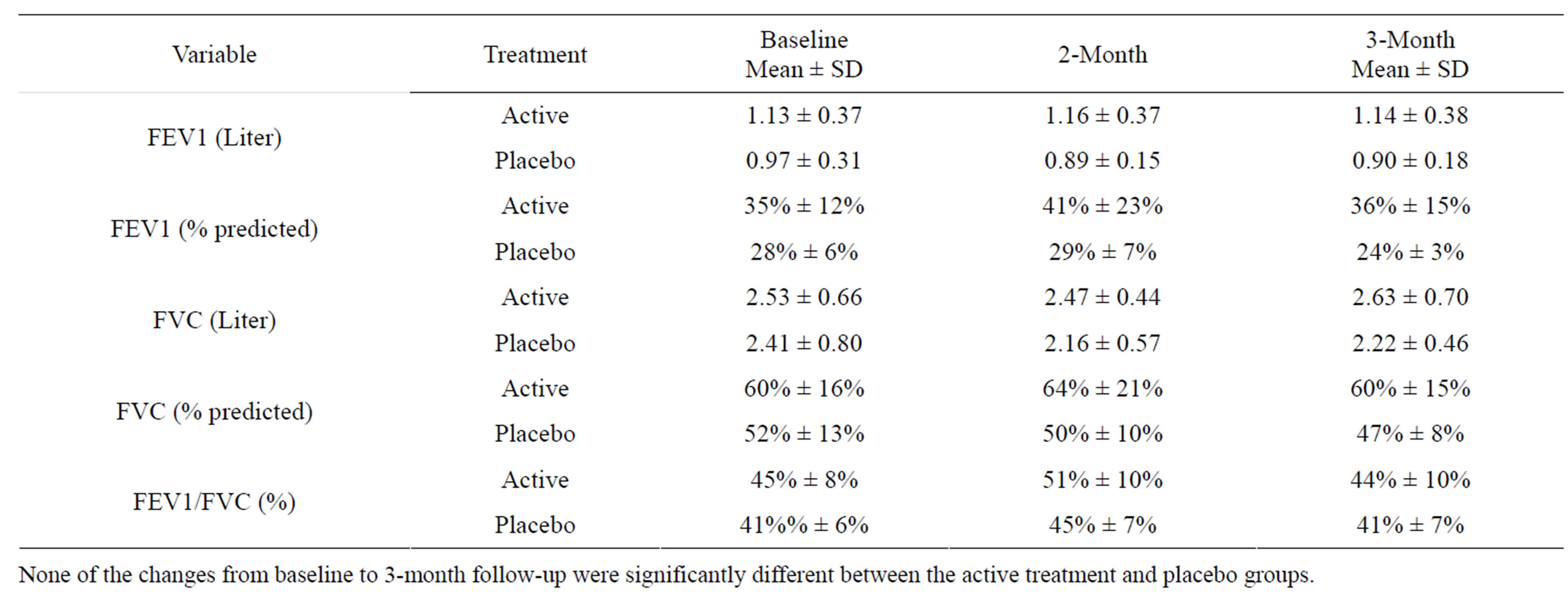
Table 5. Lung function data (Mean [SD]) by treatment group at baseline and 3-month follow-up for 32 patients (27 CB and 5 Placebo) who have both baseline and 3-month data. The 2-month data are from 17 patients (14 CB and 3 placebo).
None of the changes from baseline to 3-month follow-up were significantly different between the active treatment and placebo groups.
treatment (n = 27) but appeared to worsen in the placebo group (n = 5). None of the changes were statistically significant or clinically meaningful. Results of the 6-minute walk test did not differ between the two arms (data not shown).
Five patients had side effects after exposure to the study agent (see Table 6" target="_self"> Table 6). All the toxicities were grade 1 or mild. Of these, four reported gastrointestinal symptoms at various doses. Four patients had mild diarrhea at doses of 1 g (1), 1.5 g (1), and 2 g (2). Two of the four patients discontinued the study. In the other two, the symptoms improved with dose reduction. One patient reported a skin rash at a low dose of CB (1 g/5mg). This patient was removed from the study after developing a similar rash with re-challenge. During the study, six moderate-to-acute COPD exacerbations were reported by the study subjects. Moderate exacerbation was defined as worsening dyspnea with increased cough and/or sputum production that lasted more than 48 hours and warranted therapy with antibiotics or systemic steroid. Two of the
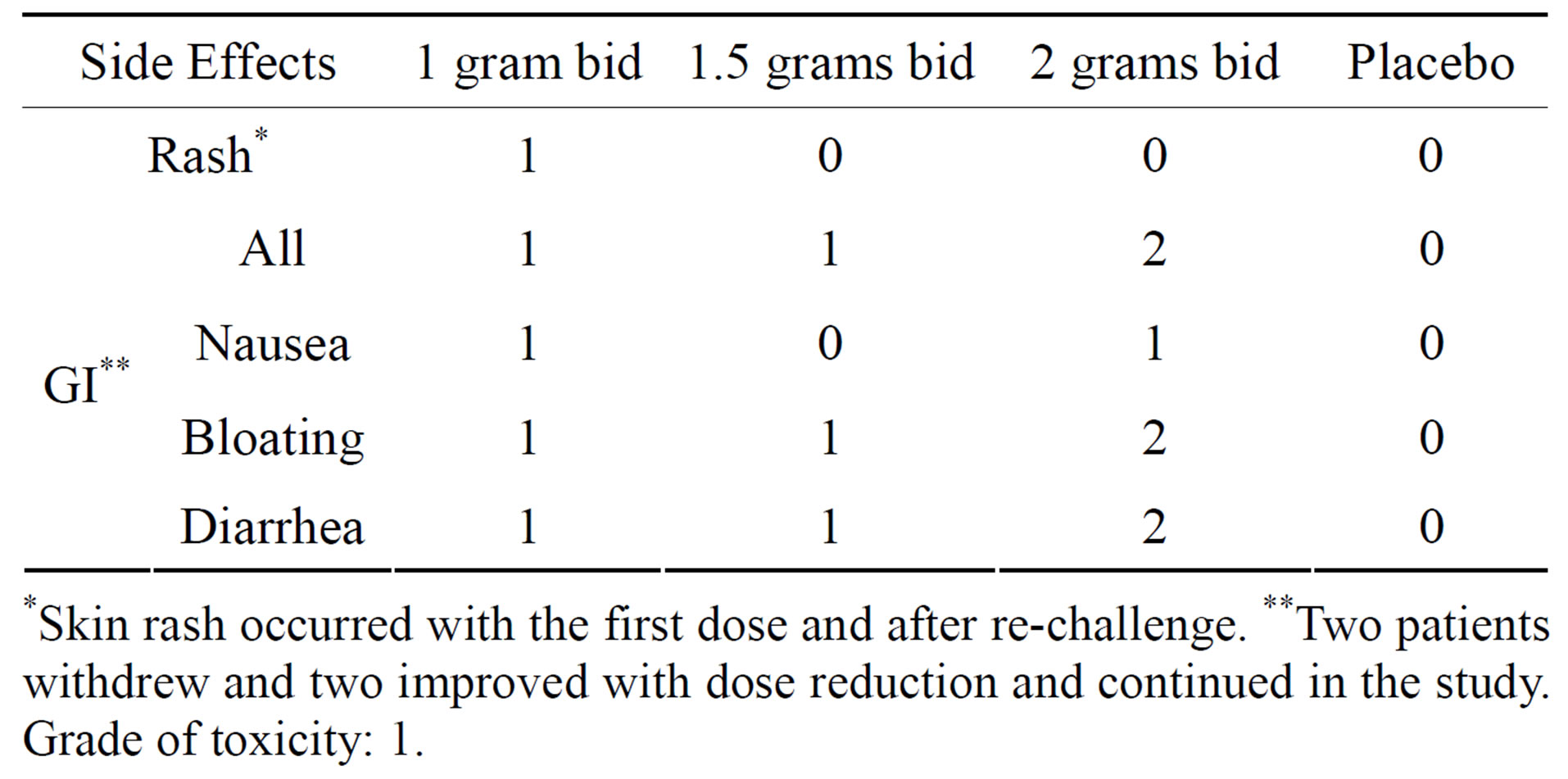
Table 6. Significant drug toxicity.
*Skin rash occurred with the first dose and after re-challenge. **Two patients withdrew and two improved with dose reduction and continued in the study. Grade of toxicity: 1.
exacerbations occurred before randomization, and these patients were excluded from the study. Of the remaining exacerbations, three were in the active arm and one in the placebo group.
4. DISCUSSION
Given the refractoriness of invasive lung carcinomas to all known treatment modalities, a number of interventions have been made over the past 20 years to reverse or arrest the progression of lung premalignancy using a diverse array of anti-inflammatory drugs, retinoids, and other agents, but the outcomes of these chemoprevention studies have not been promising. Here we sought to test the hypothesis that inflammation is a driver of sputum atypia by carrying out a pilot study using a curcumin/ bioperin combination treatment in COPD patients with sputum atypia. This patient cohort was chosen based on the underlying assumption that, in the absence of acute respiratory tract infection, sputum production in COPD patients is a consequence of mucous metaplasia resulting from chronic inflammation.
The primary endpoint in this trial was reversal of cytological abnormalities in patients with moderate or worse COPD. Baseline evaluation showed that about 46% of the patients had dysplasia of any severity and 23% had moderate dysplasia or worse in sputum samples. Treatment was well tolerated, with attrition due to treatment-related toxicity in only four patients. There was substantial attrition (state overall percentages) due to other factors, including difficulty with commute (percent), family emergencies (percent), and not having time (percent). With respect to primary endpoint analysis, the changes in cytological abnormalities were not different between the treatment groups. The lack of efficacy can be related to several factors, including the small cohort sample size, the short duration of treatment, low bioavailability of drug, and using endpoints that do not measure activity of the drug. Although several exploratory cytologic molecular markers were included in this study, none of them was different in outcome from standard cytotologic grading.
These findings do not warrant additional studies of curcumin/bioperin as chemoprevention agents in COPD patients. They reinforce the need to better delineate the genetic mutations and biologic processes that drive malignant progression in the bronchial epithelium of at-risk populations. Strategies can then be devised to use agents that target those key mutations and processes in a “personalized” approach similar to those that have successfully reduced tumor burden in lung cancer patients with advanced disease.
5. ACKNOLWEDGEMENTS
This material is based upon work supported in part by the Office of Research and Development (R&D) Medical Research Service, Department of Veteran Affairs (VA). Curcumin and bioperine were generously supplied by Sabinsa Corporation.
REFERENCES
- Rabe, K.F., Hurd, S., Anzueto, A., et al. (2007) Global strategy for the diagnosis, management, and prevention of COPD—2006 update. American Journal of Respiratory and Critical Care Medicine, 176, 532-555.
- Hogg, J.C., Chu, F., Utokaparch, S., et al. (2004) The nature of small-airway obstruction in chronic obstructive pulmonary disease. The New England Journal of Medicine, 350, 2645-2653. doi:10.1056/NEJMoa032158
- Hogg, J.C., Macklem, P.T. and Thurlbeck, W.M. (1968) Site and nature of airway obstruction in chronic obstructive lung disease. The New England Journal of Medicine, 278, 1355-1360. doi:10.1056/NEJM196806202782501
- Hogg, J.C., Chu, F.S., Tan, W.C., et al. (2007) Survival after lung volume reduction in chronic obstructive pulmonary disease: Insights from small airway pathology. American Journal of Respiratory and Critical Care Medicine, 176, 454-459. doi:10.1164/rccm.200612-1772OC
- Omenn, G.S., Goodman, G.E., Thornquist, M.D., et al. (1996) Effects of a combination of beta carotene and vitamin A on lung cancer and cardiovascular disease. The New England Journal of Medicine, 334, 1150-1155. doi:10.1056/NEJM199605023341802
- Moghaddam, S.J., Barta, P., Mirabolfathinejad, S.G., et al. (2009) Curcumin inhibits COPD-like airway inflammation and lung cancer progression in mice. Carcinogenesis, 30, 1949-1956. doi:10.1093/carcin/bgp229
- Gupta, S.C., Kim, J.H., Prasad, S., et al. (2010) Regulation of survival, proliferation, invasion, angiogenesis, and metastasis of tumor cells through modulation of inflammatory pathways by nutraceuticals. Cancer Metastasis Reviews, 29, 405-435. doi:10.1007/s10555-010-9235-2
- Gupta, S.C., Kim, J.H., Kannappan, R., et al. (2011) Role of nuclear factor kappaB-mediated inflammatory pathways in cancer-related symptoms and their regulation by nutritional agents. Experimental Biology and Medicine (Maywood), 236, 658-671. doi:10.1258/ebm.2011.011028
- Goel, A. and Aggarwal, B.B. (2010) Curcumin, the golden spice from Indian saffron, is a chemosensitizer and radiosensitizer for tumors and chemoprotector and radioprotector for normal organs. Nutrition and Cancer, 62, 919-930. doi:10.1080/01635581.2010.509835
- Sharma, R.A., McLelland, H.R., Hill, K.A., et al. (2001) Pharmacodynamic and pharmacokinetic study of oral Curcuma extract in patients with colorectal cancer. Clinical Cancer Research, 7, 1894-1900.
- Cruz-Correa, M., Shoskes, D.A., Sanchez, P., et al. (2006) Combination treatment with curcumin and quercetin of adenomas in familial adenomatous polyposis. Clinical Gastroenterology and Hepatology, 4, 1035-1038. doi:10.1016/j.cgh.2006.03.020
- Shoba, G., Joy, D., Joseph, T., et al. (1998) Influence of piperine on the pharmacokinetics of curcumin in animals and human volunteers. Planta Medica, 64, 353-356. doi:10.1055/s-2006-957450
- (2005) ATS/ERS recommendations for standardized procedures for the online and offline measurement of exhaled lower respiratory nitric oxide and nasal nitric oxide, 2005. American Journal of Respiratory and Critical Care Medicine, 171, 912-930. doi:10.1164/rccm.200406-710ST
- (2002) ATS statement: Guidelines for the six-minute walk test. American Journal of Respiratory and Critical Care Medicine, 166, 111-117. doi:10.1164/ajrccm.166.1.at1102
- Katz, R.L., Zaidi, T.M., Fernandez, R.L., et al. (2008)
NOTES
*Disclosure of Potential Conflicts of Interest: No potential conflicts of interest were disclosed.
Grant Support: National Foundation for Cancer Research (NFCR) grant LF01-065-1 (W. K. Hong).

