Surgical Science
Vol.5 No.1(2014), Article ID:41756,4 pages DOI:10.4236/ss.2014.51002
Dartos Fascio-Myo-Cutaneous Flap for Penile Skin Loss: A Simple Flap with an Immense Potential
Plastic Surgery Unit, General Surgery Department, Zagazig University, Zagazig, Egypt
Email: aahazab2@hotmail.com
Received November 26, 2013; revised December 20, 2013; accepted December 28, 2013
ABSTRACT
Introduction: Penile skin loss poses a particular challenge for reconstruction to the plastic surgeon. These defects, depending on their size, have been reconstructed using skin grafts or regional flap. Patients & Methods: Ten patients with variable sized penile skin defects were included in this work. Scrotal fascio-myo-cutaneous (Dartos) flap was harvested and used for penile shaft resurfacing. Results: All harvested flaps were successful. None of them showed any ischemic manifestations. Discussion: Despite being a simple and robust flap, its use for resurfacing of moderate to extensive penile skin defects isn’t popular. We propose the use of Dartos flap as a good alternative for challenging moderate to extensive penile skin losses.
Keywords:Scrotal Blood Supply; Penile Skin Loss; Penile Reconstruction
1. Introduction
Genital skin loss can occur as a consequence of trauma, infections such as Fournier’s gangrene, burns and iatrogenic as in excessive circumcision or surgical excision of benign or malignant penile skin lesions [1].
Necrotizing gangrene due to polymicrobial infection in the genital area, Fournier’s gangrene, is the most common cause of extensive genital skin loss. Skin loss is iatrogenic, caused by the necessity for acute debridement of necrotic genital skin when the patient is seen initially [2].
Penile skin loss can result from traction by mechanical devices, such as farm or industrial machinery, or by suction devices, such as vacuum cleaners. Because the superficial penile tissue is loose areolar tissue, it is often torn free without damage to the underlying structures. Penile burns, although rare, are often full thickness because the penile skin is so thin [2].
Genital lymphedema is one of the benign conditions that require total excision of penile skin and Dartos muscle followed by reconstruction. This occurs when there is interference with lymphatic drainage of the genital area either as a congenital anomaly or secondary to interference with the iguinal lymph nodes (surgical trauma, radiotherapy, malignancy and venereal disorders) [3,4].
A variety of local skin flaps can be used for penile skin cover. However, many authors believe that the best cosmetic results are obtained with the use of skin grafts. In particular, full-thickness skin grafts (FTSG) guarantee superior results to their split thickness counterpart since they heal with less contracture and therefore preserve the physiological girth and length expansion during erection [4].
Functional reconstruction requires regaining satisfactory sensations, providing redundant and durable skin envelop for complete erection and sexual intercourse. Therefore, a thin skin flap may be preferable to achieving better functional and cosmetic results rather than a skin graft or a thick flap [5].
Scrotal flap used in the treatment of different kinds of penile defects has been described for reconstruction of patch defects of penis in previous reports [6]. This article describes the use of scrotal fascio-myo-cutaneous flap for management of large or circumferential penile skin loss.
2. Patients and Methods
This study was carried out in Zagazig University Hospitals during the period from May 2011 till March 2014. Ten patients with penile skin loss were selected from attendants of Plastic Surgery Clinic or Emergency Unit. Patients with scrotal skin loss and those with associated urethral injury were excluded from this work. All patients were subjected to detailed medical and sexual history and meticulous physical examination (Table 1). An informed consent about surgery, possible outcome and expected complications was obtained. This study was approved by the IRB of Zagazig University Hospitals.
3. Technique
As a single stage procedure, general or spinal anaesthesia was given and 1 gm of a broad spectrum antibiotic (ceftriaxone) was given for prophylaxis. Debridment of necrotic tissue was done followed by separation of suspensory ligament at the root of the penis to counteract wound contraction. Scrotal myo-cutaneous flap was designed to match the size of the defect (Figures 1 and 2). The flap pedicle width ranged between 2.5 and 4 cm at the neck of the scrotum while flap length varied between 8 up to 12 cm. The flap included the Dartos myo-fascial layer but not the tunica vaginalis. Donor site was closed primarily (Figures 1 and 2).
From the 2nd day on, all patients received 5 mg Stilbosterol and 5 mg Diazepam 30 minutes before sleep to reduce painful nocturnal erection for 5 days. All patients were followed up for 6 - 12 months and were advised to do laser hair ablation of their new penile skin.
4. Results
Primary healing occurred in all 10 cases. There was no wound infection, dehiscence or flap ischemia. The colour, luster, texture, sensations and shape of the scrotal flap were all good. Erection and sexual function were good and satisfactory after the operation.
Donor site morbidity was also reported to be minimal. Only one case showed wound infection and partial dehiscence (10%). It was managed conservatively by repeated dressing till healed by second intention.
5. Discussion
The goal of the treatment, after extensive loss of penile skin, is to achieve good cosmetic appearance of the penis and restoring adequate sexual function. Multistage operations with a significant time delay can lead to secondary sexual dysfunction due to psychological phenomena so, less aggressive approach performed as a single stage surgery is preferable [7].
Implantation of the penis under the scrotal skin that
 (a)
(a) (b)
(b) (c)
(c)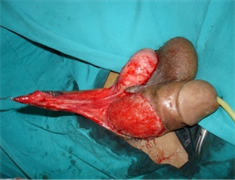 (d)
(d) (e)
(e)
Figure 1. (a) and (b) The defect and design of the flap; (c) and (d) Elevation and insetting of the flap; and (e) 2 months postoperatively.
was first described by Goodwin and Thelen, 1950 is an old, simple and reliable method for penile skin reconstruction. However, multistage surgery with the resultant delayed management and final multiple scars had limited its use [8].
Various flaps, such as lower abdominal pedicled fascia flap, paraumbilical island flap, pedicled deep inferior epigastric perforator flap and radial forearm flap, have been
 (a)
(a) (b)
(b) (c)
(c) (d)
(d) (e)
(e)
Figure 2. (a) and (b) The penile skin loss and design of the flap; (c) Immediate postoperative; (d) and (e) 3 months postoperative.
reported for reconstruction of penile defects. Nevertheless, the bulky nature of these flaps may impede vaginal penetration when they are wrapped around the penile shaft [2].
Skin grafting from non-hirsute area for the penile shaft is generally less successful and strictly depends on surgical technique and infection prophylaxis. The most important prerequisite for graft survival is well-vascularized bed, appropriate tension, as well as firm compression of dressing over it. Split-thickness skin graft is used in numerous reports successfully, but tight scarring and contracture of skin graft may restrict the filling of the corpus spongiosa. Full thickness skin graft was a more successful technique and keeps elasticity of the skin better [9- 14].
Each side of the scrotum has 4 blood vessels; anterior scrotal artery, lateral scrotal artery, lateral branch of posterior scrotal artery and septal scrotal artery. These arteries form multi-origined blood supply system to the skin of the scrotum, so, ischemic necrosis seldom occurred in scrotal flaps [15,16].
The skin of the scrotum is thin, soft and extensible. The membraneous superficial fascia has no adipose layer. Feeding arteries of the scrotal flap course in the Dartos fascia of the scrotum. This makes the scrotal flap to be referred to as an axial fascio-myo-cutaneous flap [17].
The scrotal skin is similar to the penile skin in colour. Compared with the skin graft, this flap provides better skin laxity for erection, superior skin colour match and durability for sexual intercourse [5].
In this study, ten fascio-myo-cutaneous scrotal flaps based on the anterior scrotal vessels, were harvested and successfully used for penile skin reconstruction. None of the flaps suffered ischemia in the postoperative period. All patients were satisfied about the appearance of their penis, its pliability and sexual function they resumed with a length and girth. Similar outcome was reported by Zhou et al., 2009 [18]. Although they used this flap in penile lengthening, not coverage, but they gained similar results regarding flap survival and versetility. Donor site closure was easy and was not complicated in their study. In the current study, only one patient suffered donor site wound breakdown that healed by second intention. Otherwise, in the rest of cases, donor sites were closed easily primarily and resulted in a hardly visible linear scar.
The only disadvantage of this flap, that was reported by most of patients (6 out of 10) to be worrisome, is the hair growth on the scrotal skin. We advised the patient to do laser hair removal whenever he feels annoyed.
6. Conclusions
Dartos fascio-myo-cutaneous flap technique is an effective technique for penile skin reconstruction. It has the advantages of being technically easy, using a well-vascularized axial flap to provide a homogenous long-term substitution of penile skin loss. Moreover, it is a safe technique with no associated intra-operative or significant postoperative complications.
It can be suggested as a valuable way for skin substitution of the penile shaft due to durability, sensitivity and good elasticity. It remains to be a good option, for the singleact surgery, in cases with moderate penile skin loss.
REFERENCES
- G. Garaffa, A. Abdel Raheem and D. J. Ralph, “An Update on Penile Reconstruction,” Asian Journal of Andrology, Vol. 13, No. 3, 2011, pp. 391-394. http://dx.doi.org/10.1038/aja.2011.29
- C. J. Salgado, S. Eidelson, R. Madalon and Z. Sun, “Penile Reconstruction,” Anaplastology, Vol. 1, 2012, p. 105. http://dx.doi.org/10.4172/2161-1173.1000e105
- R. A. Nelson, G. L. Alberts and L. E. King Jr., “Penile and Scrotal Elephantiasis Caused by Indolent Chlamidia Trachomatis Infection,” Urology, Vol. 61, No. 1, 2003, p. 224. http://dx.doi.org/10.1016/S0090-4295(02)02078-2
- G. Garaffa, A. N. Christopher and D. J. Ralph, “The Management of Genital Lymphoedema,” BJU International, Vol. 102, No. 4, 2008, pp. 480-484. http://dx.doi.org/10.1111/j.1464-410X.2008.07559.x
- C. Weil-Ching, L. Han-Tusing, G. U. Betul, et al., “Salvage of Complicated Penis Replantation Using Bipedicled Scrotal Flap Following a Prolonged Ischemia Time,” Journal of Plastic, Reconstructive & Aesthetic Surgery, Vol. 63, No. 8, 2010, pp. 639-643. http://dx.doi.org/10.1016/j.bjps.2010.01.017
- Z. Q. Hu, H. Hyakusoku, J. H. Gao, R. Aoki, R. Ogawa and X. Yan, “Penis Reconstruction Using Three Different Operative Methods,” British Journal of Plastic Surgery, Vol. 58, No. 4, 2005, pp. 487-492. http://dx.doi.org/10.1016/j.bjps.2004.11.007
- K. I. Paraskevas, D. Anagnostou and C. Bouris, “An Extensive Traumatic Degloving Lesion of the Penis; a Case Report and Review of the Literature,” International Urology and Nephrology, Vol. 35, No. 4, 2003, pp. 523-527. http://dx.doi.org/10.1023/B:UROL.0000025631.34893.79
- I. Ignjatović, K. Predrag, M. Nina, et al., “Reconstruction of the Penile Skin Loss Due to Radical Circumcision with a Full Thickness Skin Graft,” Vojnosanitetski Pregled, Vol. 67, No. 7, 2010, pp. 593-595. http://dx.doi.org/10.2298/VSP1007593I
- D. Ratner, “Skin Grafting; from Here to There,” Dermatologic Clinics, Vol. 16, No. 1, 1998, pp. 75-90. http://dx.doi.org/10.1016/S0733-8635(05)70488-5
- M. C. Robson and T. J. Krizek, “Predicting Skin Graft Survival,” The Journal of Trauma, Vol. 13, No. 3, 1973, pp. 213-217. http://dx.doi.org/10.1097/00005373-197303000-00005
- A. Borsellino, A. Spagnoli, S. Vallasciani, L. Martini and F. Ferro, “Surgical Approach to Concealed Penis: Technical Refinements and Outcome,” Urology, Vol. 69, No. 6, 2007, pp. 1195-1198. http://dx.doi.org/10.1016/j.urology.2007.01.065
- C. Wilson and M. Wilson, “Plastic Repair of the Denuded Penis,” Southern Medical Journal, Vol. 52, No. 3, 1959, pp. 288-290. http://dx.doi.org/10.1097/00007611-195903000-00007
- P. C. Black, J. B. Friedrich, L. H. Engrav and H. Wessells, “Meshed Unexpanded Split-Thickness Skin Grafting for Reconstruction of Penile Skin Loss,” Journal of Urology, Vol. 172, No. 3, 2004, pp. 976-979. http://dx.doi.org/10.1097/01.ju.0000133972.65501.44
- F. Jannah, H. Thompson, P. Zmaj, J. Cummings and J. Steinhardt, “An Approach for Using Full Thickness Skin Grafts for Complex Penilesurgeries in Children,” Journal of Urology, Vol. 175, No. 5, 2006, pp. 1869-1871. http://dx.doi.org/10.1016/S0022-5347(05)00931-6
- F. Giraldo, M. G. Mora, A Solano, C. Gonzalez and V. Smith-Fernandez, “Male Perineogenital Anatomy and Clinical Application in Genital Reconstruction and Maleto-Female Sex Reassignment Surgery,” Plastic and Reconstructive Surgery, Vol. 109, No. 4, 2002, pp. 1301- 1310. http://dx.doi.org/10.1097/00006534-200204010-00014
- J. A. Grossman, A. Caldomone, R. Khouri and D. M. Kenna, “Cutaneous Blood Supply of the Penis,” Plastic and Reconstructive Surgery, Vol. 83, No. 2, 1989, pp. 213-216. http://dx.doi.org/10.1097/00006534-198902000-00001
- M. A. Mendez-Fernandez, C. Hollan, D. H. Frank and J. C. Fisher, “The Scrotal Myocutaneous Flap” Plastic and Reconstructive Surgery, Vol. 78, No. 5, 1986, pp. 676- 678. http://dx.doi.org/10.1097/00006534-198611000-00020
- Q. Zhuo, S. Li, J. Wu, Z. Wang, D. Yang and L. Tao, “Clinical Application of Scrotal Flap on Penis Lengthening,” Saudi Medical Journal, Vol. 30, No. 3, 2009, pp. 418-421.


