Open Journal of Medical Imaging
Vol.05 No.02(2015), Article ID:56367,6 pages
10.4236/ojmi.2015.52007
Superiority of Digital Subtraction for Analysis of Simultaneously-Acquired Dual-Radiopharmaceutical Parathyroid Scintigraphy
Matthieu Pelletier-Galarneau, Oyebola O. Sogbein, Laurent Dinh, Lionel S. Zuckier
Division of Nuclear Medicine, University of Ottawa, Ottawa, Canada
Email: mattgalarneau@gmail.com
Copyright © 2015 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 27 March 2015; accepted 11 May 2015; published 15 May 2015
ABSTRACT
With dual-radiopharmaceutical (DR) parathyroid scintigraphy, imaging with 99mTcO4-or 123I-NaI is combined with 99mTc-sestamibi scintigraphy for localization of parathyroid adenomas. The set images are then either visually compared or digitally subtracted to aid in interpretation. While both EANM and SNMMI guidelines recommend use of digital subtraction over visual interpretation alone, to date, the few formal comparisons performed have not demonstrated superiority. The purpose of this investigation is to rigorously assess the added value of digital subtraction over visual interpretation alone using simultaneously-acquired 123I-NaI and 99mTc-sestamibi images. Materials: 90 consecutive patients with DR parathyroid scintigraphy for primary hyperparathyroidism who underwent successful parathyroidectomy were included. DR planar acquisition was performed 15 minutes post injection using 10% dual energy windows. Digital subtraction was subsequently performed using commercially available software. Images were independently reviewed by 3 nuclear medicine trainees and 2 experienced nuclear medicine physicians with and without digital subtraction. Results were compared with surgical and histopathologic findings, which served as ground truth. Results: 90 patients had a total of 91 confirmed parathyroid lesions. All 5 readers had significantly greater sensitivity with digital subtraction compared with visual interpretation alone while specificity was not significantly diminished. Area under the ROC curve was significantly greater with digital subtraction in 3 of 5 readers. Agreement was greater among trainees and experienced physicians when using digital subtraction. Conclusion: Using an optimized DR planar co-imaging technique, digital subtraction significantly improved inter-observer agreement and confidence of interpretation and increased sensitivity, without diminishing specificity.
Keywords:
Parathyroid Scintigraphy, Dual-Isotope, Dual-Radiopharmaceutical, Digital Subtraction, Visual
Comparison

1. Introduction
Primary hyperparathyroidism is among the most common endocrine disorders with a prevalence reaching 0.1% to 0.4% [1] [2] . Diagnosis of primary hyperparathyroidism is based on biochemical markers, including serum parathyroid hormone (PTH) and serum calcium [3] [4] . With the introduction of minimally invasive unilateral surgical techniques, preoperative localization of these lesions has become part of the routine clinical workup [5] - [7] . Multiple imaging modalities have been used over the past decades for this purpose, but parathyroid scintigraphy is considered as the modality of choice according to many experts [8] [9] .
Several imaging protocols have been described for the scintigraphic evaluation of parathyroid tissue, utilizing different radiopharmaceuticals and acquisition techniques. As a rule, these protocols fall into two broad categories: those that exploit differences in the rate of washout of 99mTc-sestamibi between thyroid tissue and parathyroid adenomas, and those that utilize 2 disparate radiopharmaceuticals to contrast functional aspects of tissue in the thyroid bed. In this latter category of dual-radiopharmaceutical (DR) imaging (often referred to as dual-iso- tope imaging), radiopharmaceuticals such as 201Tl-thallous chloride or 99mTc-sestamibi are used to identify areas of cellularity in the thyroid bed, while 123I-NaI and 99mTc-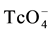 , which are substrates of the sodium iodide symporter, are used to identify thyroid tissue [10] [11] . Areas of cellular tissue which do not exhibit trapping of iodide-like substrates are suspect for parathyroid adenoma [12] [13] .
, which are substrates of the sodium iodide symporter, are used to identify thyroid tissue [10] [11] . Areas of cellular tissue which do not exhibit trapping of iodide-like substrates are suspect for parathyroid adenoma [12] [13] .
DR images may be acquired sequentially, if radiopharmaceuticals with disparate energies are used, simultaneously, utilizing a dual-energy acquisition technique [10] . Diagnosis is based on comparing and contrasting the distribution of the two radiopharmaceuticals, either in a simple side-by-side comparison or by way of a more sophisticated process of image registration and graded subtraction. Both the current SNMMI Practice Guidelines [10] and EANM Parathyroid Guidelines [11] advocate use of digital subtraction over simple comparison alone. Many [14] -[17] , though not all [18] , published studies assessing the diagnostic performance of DR parathyroid imaging have also employed software-based digital subtraction. Digital subtraction, when performed using images which are not intrinsically coregistered, is subject to errors caused by potential subtle variations in patient position [19] . This pitfall has motivated some physicians to rely primarily on visual comparison and not risk introduction of software-based artifacts [18] .
Interestingly, very few studies have formally compared visual and digital subtraction in DR parathyroid imaging, and of these, no advantage of digital subtraction has been demonstrated. Liehn et al. compared visual assessment to digital subtraction and were unable to demonstrate improvement in sensitivity and inter-observer reproducibility with the use of the latter technique [20] . Chen et al. also showed no increase in sensitivity and specificity with use of computer assisted digital subtraction [21] . Both of the investigations studied the effect of digital subtraction on planar images which were sequentially acquired which, as discussed, had potential for introducing errors of misregistration. In the present study, we have evaluated the effect of digital subtraction on simultaneously-acquired 123I-NaI and 99mTc-sestamibi images, a technique which yields intrinsically coregistered data which are not subject to registration errors.
2. Materials and Methods
2.1. Study Population
The study group consisted of all patients studied with DR parathyroid scintigraphy between August 2007 and August 2012 at The Ottawa Hospital, referred with biochemical evidence of primary hyperparathyroidism and who underwent successful parathyroidectomy. Successful parathyroidectomy was defined as normalization of serum PTH level intra-operatively and 6 months following surgery with histopathologic confirmation of parathyroid adenoma, hyperplasia, or carcinoma. Patients with chronic renal failure, incomplete imaging, ectopic adenoma, or prior parathyroidectomy or thyroidectomy were excluded. The study was approved by the Ottawa Health Science Network Research Ethics Board.
2.2. Image Acquisition and Processing
Patients received 15 MBq of 123I-NaI orally. Four hours later, 740 MBq of 99mTc-sestamibi was injected intravenously. Fifteen minutes thereafter, 10 minute DR planar acquisitions over the neck and upper two thirds of the mediastinum were performed using a low energy high resolution (LEHR) collimator and 10% dual energy windows centered on 140 keV and 159 keV. Images were stored in a 128 × 128 matrix for processing. Digital subtraction employing 4 fixed normalization thresholds (25%, 50%, 75% and 100%) was performed on the intrinsically co-registered images using commercially available software (Hermes Medical Solution, Sweden).
2.3. Interpretation
Retrospective image interpretation was independently performed by 3 nuclear medicine trainees and 2 experienced nuclear medicine physicians blinded to all clinical information. For the purpose of analysis, the neck was divided into 4 regions of interest (ROI) relative to the thyroid; right upper, right lower, left upper, and left lower. For each of the 4 regions, the readers rated their confidence that an abnormal parathyroid gland was present on a five-point scale: 1) definitely absent, 2) probably absent, 3) equivocal, 4) probably present, and 5) definitely present. Two sets of images were reviewed. The first set of images consisted of side-by-side 99mTc- sestamibi and 123I-NaI images for simple visual comparison (Figure 1). The second set of images included the 99mTc-sestamibi and 123I-NaI planar images with addition of the 4 digital subtractions described above (Figure 2). Image interpretation was conducted in a single session; all images of the first set (visual comparison
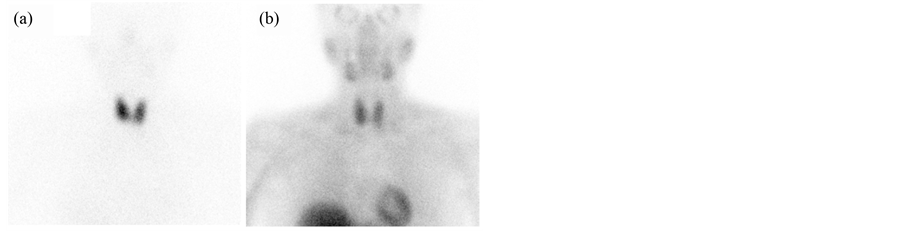
Figure 1. Simultaneously acquired anterior planar 123I-NaI (a) and 99mTc-sestamibi (b) images over the neck in a patient with primary hyperparathyroidism. There is relatively congruent 99mTc-sestamibi and 123I-NaI uptake without apparent discordant uptake to suggest location of a parathyroid adenoma. In this case, 0 out of 5 reviewers accurately localized the adenoma.
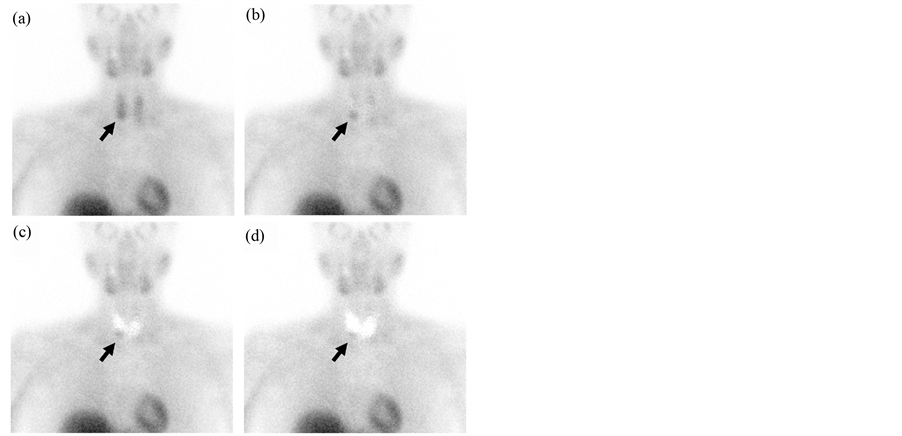
Figure 2. Digital subtraction of 123I-NaI from 99mTc-sestamibi planar images from Figure 1 using normalization thresholds of 25% (a), 50% (b), 75% (c), and 100% (d). On subtraction images, there is evidence of discordant uptake in the right lower lobe region (arrow), suggesting the presence of a parathyroid adenoma. Patient underwent successful parathyroidectomy of a parathyroid adenoma located in the lower right gland. With the addition of digital subtraction, 5 out of 5 reviewers accurately localized position of the parathyroid adenoma.
alone) were reviewed initially, followed by the second set of images (digital subtraction). The images of each set were presented in a different order. The testing paradigm was designed to assess if addition of subtraction images would improve test performance. For this reason, the subtraction images were never shown without the non-subtracted images nor were they shown prior to the non-subtracted images, so as to avoid the unlikely possibility of training the reader as to the position of the abnormalities.
2.4. Statistical Analysis
The surgical and pathological reports served at the gold standard. Receiver operating characteristic (ROC) curve and area under the curves (AUCs) were obtained using each ROI as a unit of analysis [22] . Sensitivity, specificity and accuracy were calculated by dichotomizing the readings; scores of 3 to 5 were considered positive and scores of 1 and 2 were considered negative for abnormal parathyroid gland. Reader’s confidence was computed by calculating proportions of definitely present and definitely absent (score 1 and 5) responses for each set of images. Inter-observer agreement was calculated using the Intraclass Correlation Coefficient (ICC) [23] . Statistical analyses were performed by using MedCalc for Windows, version 12.2 (MedCalc Software, Ostend, Belgium) and Matlab for Windows, version 2011b (The MathWorks Inc., Massachusetts).
3. Results
90 patients met the inclusion criteria and were included in this study. The average age was 60.5 ± 12.8 years and 68.9% (62/90) of subjects were female. Average serum PTH level before imaging was 24.9 ± 22.9 pmol/L (normal 1.6 - 9.3 pmol/L). 99% (89/90) of patients had solitary parathyroid lesions and 1% (1/90) had two parathyroid adenomas, as confirmed by histopathological examination. Of these 91 lesions, 86% (78/91) were adenoma, 13% (12/91) were hyperplasia and 1% (1/91) was a parathyroid carcinoma. Mean parathyroid lesion size was 2.0 ± 0.85 cm in largest diameter based on histopathological examination. Table 1 shows the sensitivity, specificity and AUC for visual comparison and digital subtraction. All readers had significantly greater sensitivity with digital subtraction compared to visual comparison alone. Three out of 5 readers exhibited a significantly greater AUC with digital subtraction compared to visual comparison alone.
When using digital subtraction, ICC was greater among trainees (0.8399 vs. 0.7484, p = 0.0008), among expe-
Table 1. Sensitivity, specificity and receiver operating characteristic (ROC) area under the curve (AUC) of visual comparison compared to digital subtraction.
*p < 0.05.
rienced readers (0.8973 vs. 0.8492, p = 0.0062), and among all readers (0.8632 vs. 0.7648, p = 0.0001) as compared to visual interpretation alone. Finally, readers were more definitive in their interpretation of the studies with the digital subtraction of ROIs compared to visual interpretation alone (92% vs. 85%, p = 0.0365).
4. Discussion
The diagnostic performance of DR imaging was significantly improved with the use of digital subtraction. Sensitivity of all readers significantly increased with digital subtraction compared to visual interpretation alone, without significant effect on specificity. Furthermore, the AUC was significantly greater for 3 out of 5 readers. These findings held true for both experienced readers and novice trainees. There was also significant improvement of inter-observer agreement when using digital subtraction compared to visual interpretation alone for both experienced readers and trainees. Based on the Landis et al. interpretation [24] , the inter-observer agreement improved from substantial to almost perfect in trainees.
These results are discordant from previously published data [20] [21] . We hypothesize that this is related to the fact that our study used simultaneous co-imaging thereby providing intrinsically coregistered images; this was not the case in the referenced articles, where subtle misregistration could have reduced the accuracy of the subtracted images.
5. Limitations
A potential limitation inherent to the statistical methodology used in this study is that every ROI was analyzed individually and independently, which differs from routine clinical reading. Such an approach could minimize the satisfaction of search effect [25] , leading to improved sensitivity and potentially decreased specificity. However, given that the sample contained only one patient with 2 lesions, this effect should be minimal. Another potential limitation of this study is that the study population was confined to patients with confirmed parathyroid adenomas at surgery. This selection might prevent the inclusion of patients with equivocal imaging findings who did not proceed to parathyroidectomy. Nonetheless, there is no reason to believe that inclusion of these more equivocal cases would have favored the visual over the image subtraction method.
The sensitivities obtained in this study are relatively low, ranging from 73% to 80%, but comparable to studies using only DR planar imaging [26] . Because the purpose of this study was to evaluate the added value of digital subtraction, delayed planar images and SPECT-CT were purposely excluded, resulting in lower sensitivity. It is important to emphasize that, even with the use of digital subtraction, utilization of delayed images and/ or SPECT-CT images remains recommended [26] [27] .
6. Conclusion
The results of this study, performed using intrinsically co-registered and simultaneously 99mTc-sestamibi and 123I-NaI images, are the first to rigorously demonstrate an advantage of using digital subtraction over visual assessment alone for DR parathyroid scintigraphy. Use of subtraction imaging in this study resulted in improved inter-observer agreement, superior accuracy and greater confidence for both experienced readers and trainees.
References
- Clarke, B.L. (2013) Epidemiology of Primary Hyperparathyroidism. Journal of Clinical Densitometry, 16, 8-13. http://dx.doi.org/10.1016/j.jocd.2012.11.009
- Delbridge, L.W., Younes, N.A., Guinea, A.I., Reeve, T.S., Clifton-Bligh, P. and Robinson, B.G. (1998) Surgery for Primary Hyperparathyroidism 1962-1996: Indications and Outcomes. The Medical Journal of Australia, 168, 153-156.
- Bilezikian, J.P., Brandi, M.L., Eastell, R., Silverberg, S.J., Udelsman, R., Marcocci, C., et al. (2014) Guidelines for the Management of Asymptomatic Primary Hyperparathyroidism: Summary Statement from the Fourth International Workshop. The Journal of Clinical Endocrinology & Metabolism, 99, 3561-3569. http://dx.doi.org/10.1210/jc.2014-1413
- Flint, R.S., Harman, C.R., Carter, J. and Snyman, G. (2002) Primary Hyperparathyroidism: Referral Patterns and Outcomes of Surgery. ANZ Journal of Surgery, 72, 200-203. http://dx.doi.org/10.1046/j.1445-2197.2002.02343.x
- Carty, S.E., Worsey, J., Virji, M.A., Brown, M.L. and Watson, C.G. (1997) Concise Parathyroidectomy: The Impact of Preoperative SPECT 99mTc Sestamibi Scanning and Intraoperative Quick Parathormone Assay. Surgery, 122, 1107- 1114. http://dx.doi.org/10.1016/S0039-6060(97)90215-4
- Worsey, M.J., Carty, S.E. and Watson, C.G. (1993) Success of Unilateral Neck Exploration for Sporadic Primary Hyperparathyroidism. Surgery, 114, 1024-1029.
- Khan, M.A.A., Rafiq, S., Lanitis, S., Mirza, F.A., Gwozdziewicz, L., Al-Mufti, R., et al. (2013) Surgical Treatment of Primary Hyperparathyroidism: Description of Techniques and Advances in the Field. Indian Journal of Surgery, 76, 308-315. http://dx.doi.org/10.1007/s12262-013-0898-0
- Lew, J.I. and Solorzano, C.C. (2009) Surgical Management of Primary Hyperparathyroidism: State of the Art. Surgical Clinics of North America, 89, 1205-1225. http://dx.doi.org/10.1016/j.suc.2009.06.014
- Giordano, A., Rubello, D. and Casara, D. (2001) New Trends in Parathyroid Scintigraphy. European Journal of Nuclear Medicine, 28, 1409-1420. http://dx.doi.org/10.1007/s002590100596
- Greenspan, B.S., Dillehay, G., Intenzo, C., Lavely, W.C., O’Doherty, M., Palestro, C.J., et al. (2012) SNM Practice Guideline for Parathyroid Scintigraphy 4.0. Journal of Nuclear Medicine Technology, 40, 111-118. http://dx.doi.org/10.2967/jnmt.112.105122
- Hindié, E., Ugur, O., Fuster, D., O’Doherty, M., Grassetto, G., Urea, P., et al. (2009) EANM Parathyroid Guidelines. European Journal of Nuclear Medicine and Molecular Imaging, 36, 1201-1216. http://dx.doi.org/10.1007/s00259-009-1131-z
- Ell, P.J., Todd-Pokropek, A. and Britton, K.E. (1975) Localization of Parathyroid Adenomas by Computer-Assisted Parathyroid Scanning. British Journal of Surgery, 62, 553-555. http://dx.doi.org/10.1002/bjs.1800620711
- Ferlin, G., Borsato, N., Camerani, M., Conte, N. and Zotti, D. (1983) New Perspectives in Localizing Enlarged Parathyroids by Technetium-Thallium Subtraction Scan. Journal of Nuclear Medicine, 24, 438-441.
- Mazzeo, S., Caramella, D., Lencioni, R., Molea, N., De Liperi, A., Marcocci, C., et al. (1996) Comparison among Sonography, Double-Tracer Subtraction Scintigraphy, and Double-Phase Scintigraphy in the Detection of Parathyroid Lesions. American Journal of Roentgenology, 166, 1465-1470. http://dx.doi.org/10.2214/ajr.166.6.8633466
- Hindié, E., Mellière, D., Jeanguillaume, C., Urea, P., de Labriolle-Vaylet, C. and Perlemuter, L. (2000) Unilateral Surgery for Primary Hyperparathyroidism on the Basis of Technetium Tc 99m Sestamibi and Iodine 123 Subtraction Scanning. Archives of Surgery, 135, 1461-1468. http://dx.doi.org/10.1001/archsurg.135.12.1461
- Hindié, E., Mellière, D., Jeanguillaume, C., Perlemuter, L., Chéhadé, F. and Galle, P. (1998) Parathyroid Imaging Using Simultaneous Double-Window Recording of Technetium-99m-Sestamibi and Iodine-123. Journal of Nuclear Medicine, 39, 1100-1105.
- O’Doherty, M.J., Kettle, A.G., Wells, P., Collins, R.E. and Coakley, A.J. (1992) Parathyroid Imaging with Technetium-99m-Sestamibi: Preoperative Localization and Tissue Uptake Studies. Journal of Nuclear Medicine, 33, 313-318.
- Krausz, Y., Lebensart, P.D., Klein, M., Weininger, J., Blachar, A., Chisin, R. and Shiloni, E. (2000) Preoperative Localization of Parathyroid Adenoma in Patients with Concomitant Thyroid Nodular Disease. World Journal of Surgery, 24, 1573-1578. http://dx.doi.org/10.1007/s002680010280
- Caveny, S.A., Klingensmith III, W.C., Martin, W.E., Sage-El, A., McIntyre Jr., R.C., Raeburn, C., et al. (2012) Parathyroid Imaging: The Importance of Dual-Radiopharmaceutical Simultaneous Acquisition with 99mTc-Sestamibi and 123I. Journal of Nuclear Medicine Technology, 40, 104-110. http://dx.doi.org/10.2967/jnmt.111.098400
- Liehn, J.C., Amico, S., Delisle, M.J. and Flament, J.B. (1988) Improvement of Parathyroid Tl-Tc Scintigraphy by Using a New Image Subtraction Method. European Journal of Nuclear Medicine, 14, 184-189. http://dx.doi.org/10.1007/BF00257325
- Chen, C.C., Holder, L.E., Scovill, W.A., Tehan, A.M. and Gann, D.S. (1997) Comparison of Parathyroid Imaging with Technetium-99m-Pertechnetate/Sestamibi Subtraction, Double-Phase Technetium-99m-Sestamibi and Technetium-99m- Sestamibi SPECT. Journal of Nuclear Medicine, 38, 834-839.
- Obuchowski, N.A., Lieber, M.L. and Powell, K.A. (2000) Data Analysis for Detection and Localization of Multiple Abnormalities with Application to Mammography. Academic Radiology, 7, 516-525. http://dx.doi.org/10.1016/S1076-6332(00)80324-4
- McGraw, K.O. and Wong, S.P. (1996) Forming Inferences about Some Intraclass Correlation Coefficients. Psychological Methods, 1, 30-46. http://dx.doi.org/10.1037/1082-989X.1.1.30
- Landis, J.R. and Koch, G.G. (1977) The Measurement of Observer Agreement for Categorical Data. Biometrics, 33, 159-174. http://dx.doi.org/10.2307/2529310
- Berbaum, K.S., Franken, E.A., Dorfman, D.D., Rooholamini, S.A., Kathol, M.H., Barloon, T.J., et al. (1990) Satisfaction of Search in Diagnostic Radiology. Investigative Radiology, 25, 133-140. http://dx.doi.org/10.1097/00004424-199002000-00006
- Nichols, K.J., Tomas, M.B., Tronco, G.G., Rini, J.N., Kunjummen, B.D., Heller, K.S., et al. (2008) Preoperative Parathyroid Scintigraphic Lesion Localization: Accuracy of Various Types of Readings. Radiology, 248, 221-232. http://dx.doi.org/10.1148/radiol.2481071066
- Lavely, W.C., Goetze, S., Friedman, K.P., Leal, J.P., Zhang, Z., Garret-Mayer, E., et al. (2007) Comparison of SPECT/CT, SPECT, and Planar Imaging with Single- and Dual-Phase 99mTc-Sestamibi Parathyroid Scintigraphy. Journal of Nuclear Medicine, 48, 1084-1089. http://dx.doi.org/10.2967/jnumed.107.040428