Modern Plastic Surgery
Vol.3 No.3(2013), Article ID:33937,5 pages DOI:10.4236/mps.2013.33017
Management of Diabetic Foot Ulcers Using Negative Pressure with Locally Available Materials*
![]()
1Department of Surgery, Komfo Anokye Teaching Hospital, School of Medical Sciences, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana; 2Reconstructive Plastic Surgery & Burns Unit, Department of Surgery, Komfo Anokye Teaching Hospital, School of Medical Sciences, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana.
Email: #pimagben@yahoo.com
Copyright © 2013 Joseph Yorke et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received February 9th, 2013; revised March 11th, 2013; accepted March 20th, 2013
Keywords: Diabetic Ulcers; Negative Pressure Therapy; Cost; Locally Manufactured Materials
ABSTRACT
Introduction: Diabetic ulcers are one of the main causes of morbidity and hospitalisation and thereby affecting the quality of life of persons suffering from the condition. The aim of the study was to assess the level of satisfaction of persons who underwent treatment for diabetic ulcers using negative pressure produced from locally available materials. Materials and Methods: Creating negative pressure using locally available materials such as sterilized foam, tubes with diameter between 0.5 and 0.8 cm, transparent adhesive plaster and a suction machine. Results: Thirty-seven patients were enrolled in the current study; 70.3% (n = 26) were known diabetic patients on regular treatment while 29.7% (n = 11) were diagnosed when they presented for the first time with ulcers. Patients were made to grade their level of satisfaction with therapy involving these locally used materials. Out of the 37 patients, 35 (94.6%) stated their therapy was excellent while 1 (2.7%) said the therapy was good; therapy was discontinued in one patient (2.7%) who had some complication. Conclusion: Desirable outcomes were obtained when patients were treated using negative pressure wound therapy (NPWT) produced using locally manufactured materials. Patients were able to pay for the therapy since the cost was reasonably low.
1. Introduction
Diabetic ulcers are the most common cause of morbidity and hospitalisation among patients with diabetes [1-4]. Persons suffering from diabetes have a 12% - 15% lifetime risk of developing foot ulcer. Foot ulcer impacts negatively on the quality of life of persons and also costly as well (about USD 17,500 - 27,987) [5,6]. Also, there may be a need for the lower limb to be amputated [7,8] which may bring untold hardship to the individual. Management of diabetic ulcers entails a lot and demands a need for more intensive program [9,10]. The use of negative pressure wound therapy (NPWT) via the Kinetic Concepts Inc. (KCI) Vacuum Assisted Closure (VAC) Therapy system to manage diabetic foot ulcers have been reported by quiet a number of authors [11,12]. This therapy has been effective in the treatment of complex diabetic ulcers and promoted wound healing by removing fluid from open wounds through a sealed dressing and tubing which is connected to a collection container by use of sub-atmospheric pressure dressings or negative pressure available as the KCI VAC device [13-16]. Management of diabetic ulcers has been a major challenge in most institutions in Ghana over the years. Several methods had been tried including conventional wound dressing. The use of advanced methods like the KCI Wound VAC system for providing negative-pressure therapy for wounds had not been popular in Ghana because it is relatively expensive and not easily available for patients in Ghana. The KCI Wound VAC system produces good results, but because of financial considerations this system of providing negative pressure from the use of locally manufactured materials was developed as a method of providing patients with similar negative pressure therapy without the significant costs of purchasing or renting the KCI VAC system, which can be very expensive in the Ghanaian setting. We use this system whenever negative pressure therapy is indicated and the KCI VAC system is not available.
2. Materials and Methods
2.1. Study Setting
Komfo Anokye Teaching Hospital (KATH), located in Kumasi is the second-largest hospital in Ghana and the only tertiary health institution in the middle belt of the country. It is the main referral hospital for the Ashanti, Brong-Ahafo, Northern, Upper East and Upper West Regions.
2.2. Creating Negative Pressure Using Locally Available Materials
The construction of the locally-made system requires a combination of materials readily available on the surgical wards. The system is made of: 1) sterilized foam; 2) tubes with diameter between 0.5 and 0.8 cm; 3) transparent adhesive plaster; and 4) a suction machine. Adhesive transparent plaster, a connecting bag tube measuring about 0.5 - 0.8 cm in diameter, and foam are used to assemble a dressing connected to a suction machine (negative 40 - 75 mmHg) to create NPWT that is relatively cheap, accessible at short notice and produces equivalent results as to using the KCI VAC system. The foams are sterilized using Pera Safe (a sterilising agent for sanitizing theatre instruments). The system, once constructed, is maintained to a standard suction at 45 to 70 mmHg negative pressure.
2.3. Patient Management
The wound to be treated was debrided to remove necrotic or infected tissue before the application of negative pressure dressings. To ensure an adequate seal with the overlying adhesive film, the surrounding skin was kept as dry as possible. Foam sponges were cut larger than the wound to be treated using a scalpel blade. A layer of transparent adhesive plaster was then wrapped tightly to seal the entire wound. The adhesive was cut from the centre with a scalpel to create a proportionately long defect as per the wound size. The urine bag tube drain which been fenestrated was placed in the defect and secured with another layer of the adhesive. Additional layers of adhesive were wrapped around the tube to seal the wound completely. A suction connector was then used to establish continuity between the tube and suction machine. A negative pressure of 40 - 75 mmHg induced a characteristic collapse of the foam sponges as seen in other systems. Thirty-seven patients with various degrees of diabetic foot ulcers were treated using this locally modified negative pressure therapy. The study was carried out from January, 2007 to December, 2011.
2.4. Ethical Clearance
Ethical Clearance was obtained from the Kwame Nkrumah University of Science and Technology School of Medical Sciences/Komfo Anokye Teaching Hospital Committee on Human Research, Publication and Ethics. Kumasi.
3. Results
Out of the 37 patients, 89.6% (n = 21) were females and 10.4% (n = 16) were males; 70.3% (n = 26) were known diabetic patients on regular treatment while 29.7% (n = 11) were diagnosed when they presented for the first time with ulcers. The figure below shows a patient undergoing therapy using the negative pressure created with locally available materials (Figure 1).
Patients were made to grade their level of satisfaction with the therapy involving these locally assembled materials. Out of the thirty-seven patients, 35 (94.6%) stated their therapy was excellent while 1 (2.7%) said the therapy was good. However, one person (2.7%) developed some complication and the therapy was discontinued. The assessments were done by the patients being asked to grade their satisfaction on a scale of 1-5 as follows: 1—Bad; 2—Fair; 3—Satisfactory; 4—Good; 5—Excellent (Table 1).
4. Discussion
The locally available system was found to be particularly good for managing ulcers of various causes, and it is now a routinely used system in the study setting. The advantages of negative pressure therapy appears to include better control of wound secretions, reduction of wound oedema, promotion of granulation, improved patient comfort, and, from some clinical trial data, more rapid healing. The use of NPWT to aid acute and chronic wound healing has been reported by some authors [17-24].
Based on our hospital procurement expenses, the overall cost required to assemble a locally available system using urine bag, a foam sponge measuring 25 × 14 × 3 cm, a transparent plaster, is less than Ten Ghana Cedis (Gh¢10.00—equivalent of about US$5.00). This estimate does not take into account electricity cost and sterilization.
Persons with bleeding tendencies may develop some form of complication. We encountered one patient with haemorrhage using this method and had to discontinue the therapy. There is some concern that large wounds or persons with bleeding wounds at the time of dressing application could bleed excessively into the suction canister, which unlike commercial systems does not have a volume cut-off level. Because of this limitation, we urge caution in using this method for paediatric wounds in which drainage volumes should be monitored carefully, and for very large wounds or those likely to bleed excessively. None of our cases used was a paediatric.
Another limitation to the use of this locally created
 (a)
(a)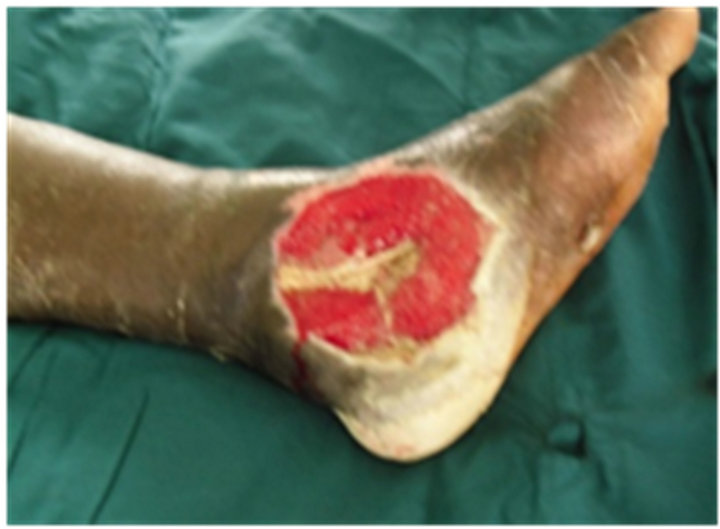 (b)
(b) (c)
(c)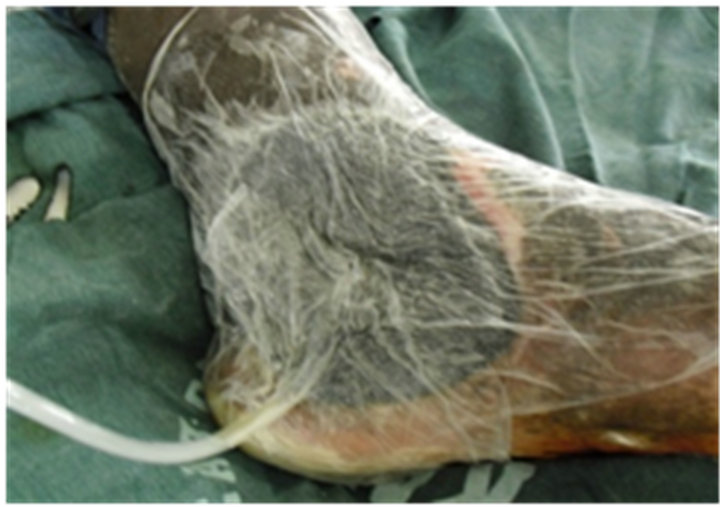 (d)
(d)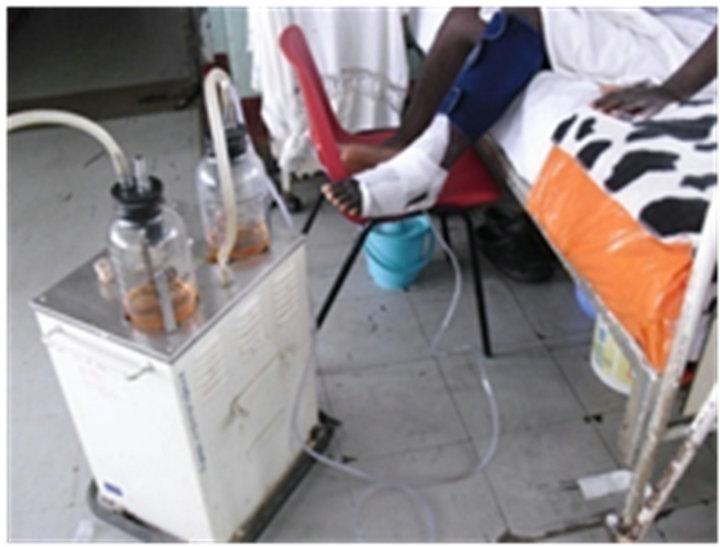 (e)
(e)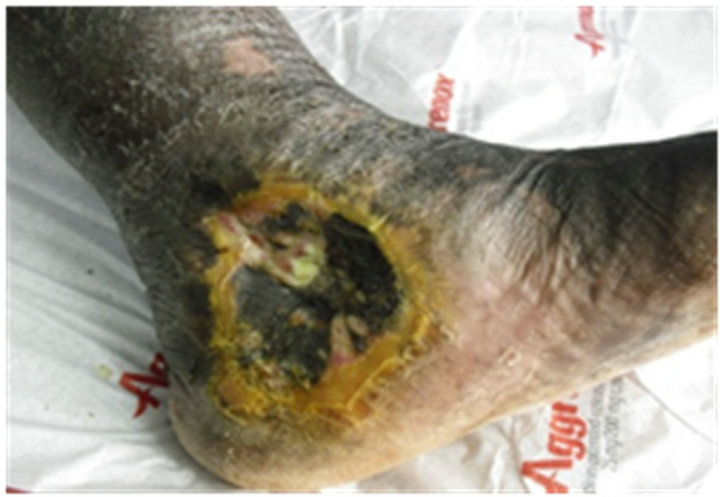 (f)
(f)
Figure 1. A patient undergoing therapy using negative pressure. (a) Presentation; (b) After debridement; (c) Local VAC system; (d) Local VAC in use; (e) Local VAC system; (f) Healing of the diabetic ulcer.

Table 1. Satisfaction grade of patients.
negative pressure is power failure. Unlike the KCI VAC systems that have rechargeable batteries, the suction machines have no batteries hence when there is power failure, the therapy cannot take place. The failure to treat patients on outpatient basis because of inadequate number of suction machines on the wards is also a limitation.
Noise pollution is a problem since most of our suction machines are old; the noise is sometimes unbearable to some patients who might need some form of rest. Despite these limitations, our system is invaluable for some patients who would otherwise have had amputations for diabetic foot ulcers because there is no access to commercial KCI VAC systems as a result of cost considerations.
Furthermore, advanced commercial technology is not always available due the maintenance cost. Whereas the components required in this locally available system are available in most district and regional hospitals in Ghana and are easy to apply to manage inpatient wound problems tools to help in maintenance of this advanced technology, as in the case of the KCI VAC systems are not readily available commercially.
5. Conclusion
The adoption of provision of negative pressure from the use of locally produced materials as shown in this study is one of a kind making it possible for persons who would have otherwise had amputation to be able to access this kind of care which promotes quick healing of their ulcers. Desirable results were obtained when patients were treated using this negative pressure wound therapy created or produced using these locally manufactured materials. It was also cost-effective since the materials are always readily available on the ward or commercially at very reasonable low prices.
REFERENCES
- N. Singh, D. G. Armstrong and B. A. Lipsky, “Preventing Foot Ulcers in Patients with Diabetes,” Journal of the American Medical Association, Vol. 293, No. 2, 2005, pp. 217-228. doi:10.1001/jama.293.2.217
- C. A. Abbott, A. P. Garrow, A. L. Carrington, J. Morris, E. R. Van Ross and A. J. Boulton, “Foot Ulcer Risk Is Lower in South-Asian and African-Caribbean Compared with European Diabetic Patients in the UK: The NorthWest Diabetes Foot Care Study,” Diabetes Care, Vol. 28, No. 8, 2005, pp. 1869-1875. doi:10.2337/diacare.28.8.1869
- S. D. Ramsey, K. Newton, D. Blough, et al., “Incidence, Outcomes, and Cost of Foot Ulcers in Patients with Diabetes,” Diabetes Care, Vol. 22, No. 3, 1999, pp. 382-387. doi:10.2337/diacare.22.3.382
- G. Ragnarson Tennvall and J. Apelqvist, “Health-Economic Consequences of Diabetic Foot Lesions,” Clinical Infectious Diseases, Vol. 39, No. 2, 2004, pp. 132-139. doi:10.1086/383275
- A. J. Boulton, “The Diabetic Foot: A Global View,” Diabetes/Metabolism Research and Reviews, Vol. 16, No. 1, 2000, pp. 2-5. doi:10.1002/1520-7560(200009/10)16:1+<::AID-DMRR105>3.0.CO;2-N
- R. G. Frykberg, “Diabetic Foot Ulcers: Current Concepts,” Journal of Foot and Ankle Surgery, Vol. 37, No. 5, 1998, pp. 440-446. doi:10.1016/S1067-2516(98)80055-0
- R. E. Pecoraro, G. E. Reiber and E. M. Burgess, “Pathways to Diabetic Limb Amputation, Basis for Prevention,” Diabetes Care, Vol. 13, No. 5, 1990, pp. 513-521. doi:10.2337/diacare.13.5.513
- D. J. Margolis, L. Allen-Taylor, O. Hoffstad and J. A. Berlin, “Diabetic Neuropathic Foot Ulcers and Amputation,” Wound Repair and Regeneration, Vol. 13, No. 3, 2005, pp. 230-236. doi:10.1111/j.1067-1927.2005.130303.x
- A. Nather, Y. H. Ng, K. L. Wong and A. S. Joshi, “Effectiveness of Bridge VAC Dressings in the Treatment of Diabetic Foot Ulcers,” Diabetic Foot Ankle, Vol. 2, 2011, p. 5983.
- S. B. Chionh, Y. Y. Han, P. L. Chan and A. Nambiar, “Effectiveness of Vacuum-Assisted Closure (VAC) Therapy in the Healing of Chronic Diabetic Foot Ulcers,” Annals Academy of Medicine Singapore, Vol. 39, No. 5, 2012, pp. 353-358.
- P. A. Blume, J. Walters, W. Payne, J. Ayala and J. Lanitis, “Comparison of Negative Pressure Wound Therapy Using Vacuum-Assisted Closure with Advanced Moist Wound Therapy in the Treatment of Diabetic Foot Ulcers: A Multicenter Randomized Controlled Trial,” Diabetes Care, Vol. 31, No. 4, 2008, pp. 631-636. doi:10.2337/dc07-2196
- L. A. Lavery, A. J. Boulton, J. A. Niezgoda and P. Sheehan, “A Comparison of Diabetic Foot Ulcer Outcomes Using Negative Pressure Wound Therapy VERSUS Historical Standard of Care,” International Wound Journal, Vol. 4, No. 2, 2007, pp. 103-113. doi:10.1111/j.1742-481X.2007.00317.x
- E. Joseph, C. A. Hamori, S. Bergman, E. Roaf, N. F. Swann and G. W. Anastasi, “A Prospective, Randomized Trial of Vacuum Assisted Closure versus Standard Therapy of Chronic Non Healing Wounds,” Wounds, Vol. 12, No. 3, 2000, pp. 60-67.
- T. E. Philbeck, W. J. Schroeder and K. T. Whittington, “Vacuum-Assisted Closure Therapy for Diabetic Foot Ulcers: Clinical and Cost Analysis,” Home Health Consult, Vol. 8, 2001, pp. 26-34.
- T. Schwien, J. Gilbert and C. Lang, “Pressure Ulcer Prevalence and the Role of Negative Pressure Wound Therapy in Home Health Quality Outcomes,” Ostomy Wound Management, Vol. 51, No. 9, 2005, pp. 47-60.
- E. Moisidis, T. Heath, C. Boorer, K. Ho and A. K. Deva, “A Prospective, Blinded, Randomized, Controlled Clinical Trial of Topical Negative Pressure Use in Skin Grafting,” Plastic and Reconstructive Surgery, Vol. 114, No. 4, 2004, pp. 917-922. doi:10.1097/01.PRS.0000133168.57199.E1
- D. G. Armstrong and L. A. Lavery, “Diabetic Foot Study Consortium. Negative Pressure Wound Therapy after Partial Diabetic Foot Amputation: A Multicentre, Randomised Controlled Trial,” Lancet, Vol. 366, No. 9498, 2005, pp. 1704-1710. doi:10.1016/S0140-6736(05)67695-7
- M. T. Eginton, K. R. Brown, G. R. Seabrook, J. B. Towne and R. A. Cambria, “A Prospective Randomized Evaluation of Negative-Pressure Wound Dressings for Diabetic Foot Wounds,” Annals of Vascular Surgery, Vol. 17, No. 6, 2003, pp. 645-649. doi:10.1007/s10016-003-0065-3
- J. T. Thompson and M. W. Marks, “Negative Pressure Wound Therapy,” Clinics in Plastic Surgery, Vol. 34, No. 4, 2007, pp. 673-684. doi:10.1016/j.cps.2007.07.005
- P. E. Campbell, “Surgical Wound Case Studies with the Versatile1 Wound Vacuum System for Negative Pressure Wound Therapy,” Journal of Wound Ostomy and Continence Nursing, Vol. 33, No. 2, 2006, pp. 176-190. doi:10.1097/00152192-200603000-00014
- L. C. Argenta, M. J. Morykwas, M. W. Marks, A. J. DeFranzo, J. A. Molnar and L. R. David, “Vacuum-Assisted Closure: State of Clinic Art,” Plastic and Reconstructive Surgery, Vol. 117, No. 7, 2006, pp. 127-142. doi:10.1097/01.prs.0000222551.10793.51
- P. E. Campbell, G. S. Smith and J. M. Smith, “Retrospective Clinical Evaluation of Gauze-Based Negative Pressure Wound Therapy,” International Wound Journal, Vol. 5, No. 2, 2008, pp. 280-286. doi:10.1111/j.1742-481X.2008.00485.x
- J. D. Vuerstaek, T. Vainas, J. Wuite, P. Nelemans, M. H. Neumann and J. C. Veraart, “State-of-the-Art Treatment of Chronic Leg Ulcers: A Randomized Controlled Trial Comparing Vacuum Assisted Closure (V.A.C.) with Modern Wound Dressings,” Journal of Vascular Surgery, Vol. 44, No. 5, 2006, pp. 1029-1038. doi:10.1016/j.jvs.2006.07.030
- J. P. Stannard, J. T. Robinson, E. R. Anderson, G. McGwin Jr., D. A. Volgas and J. E. Alonso, “Negative Pressure Wound Therapy to Treat Hematomas and Surgical Incisions Following High Energy Trauma,” Journal of Trauma, Vol. 60, No. 6, 2006, pp. 1301-1306. doi:10.1097/01.ta.0000195996.73186.2e
NOTES
*Conflict of interest: None was declared by all the authors.
#Corresponding author.

