World Journal of Cardiovascular Diseases
Vol.4 No.1(2014), Article ID:42115,4 pages DOI:10.4236/wjcd.2014.41002
Intramural cardiac hydatid cyst—Incidental finding
Princess Muna AL-Hussein Cardiac Center, King Abdullah University Hospital, Faculty of Medicine, Jordan University of Science and Technology, Jordan
Email:*emad_hijazi@hotmail.com
Copyright © 2014 Emad M. Hijazi et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. In accordance of the Creative Commons Attribution License all Copyrights © 2014 are reserved for SCIRP and the owner of the intellectual property Emad M. Hijazi et al. All Copyright © 2014 are guarded by law and by SCIRP as a guardian.
Received 15 November 2013; revised 26 December 2013; accepted 8 January 2014
ABSTRACT
Hydatid cyst was commonly found in the liver followed by lungs and brain. Cardiac hydatid cysts are less common compared to hepatic ones. We report a case of intramural hydatid cyst that is incidentally found during the work-up of a hepatic hydated cyst.
KEYWORDS
Cardiac Cyst; Hydated Disease; Intramural Cardiac Cyst
1. CASE REPORT
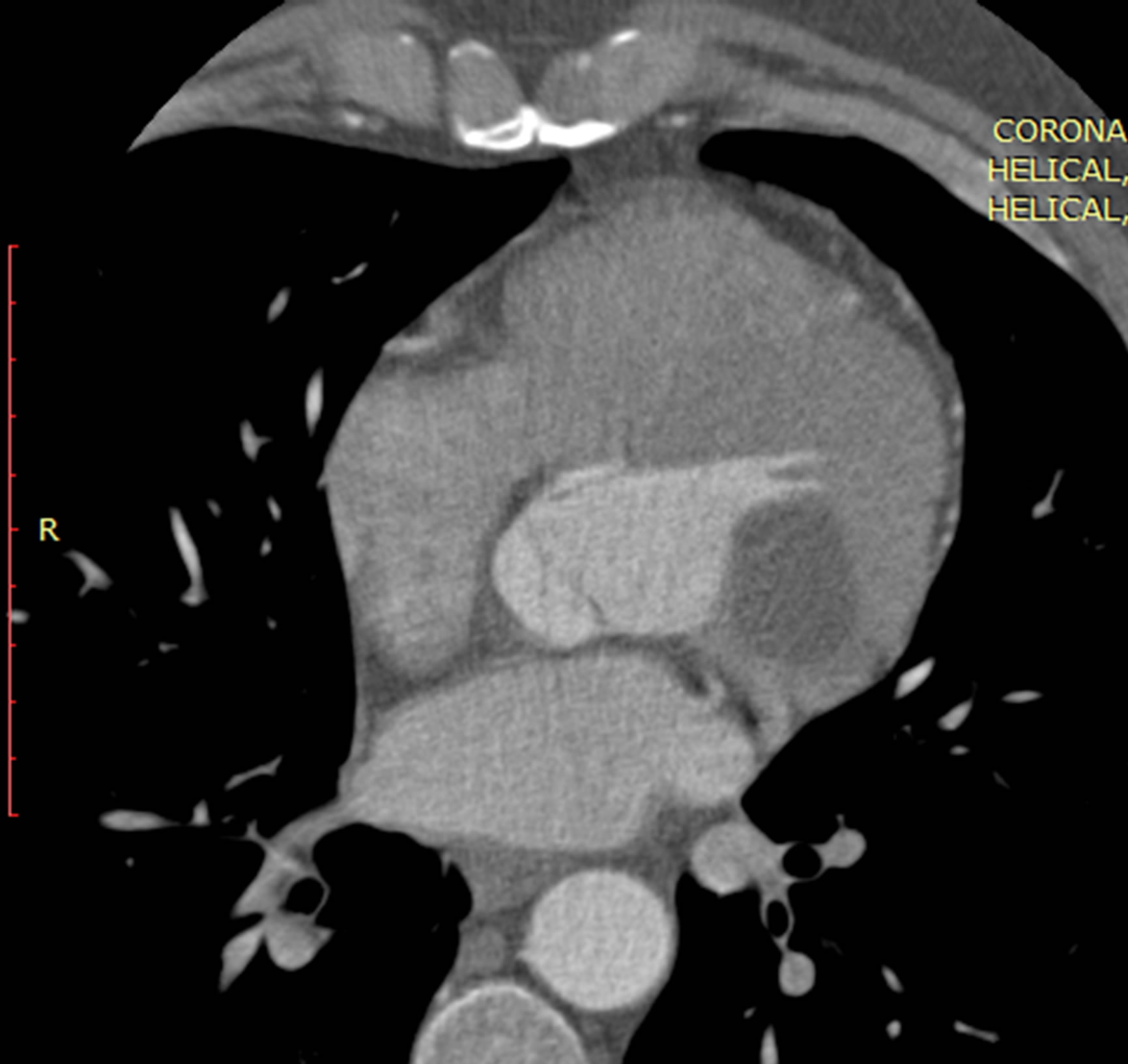
A 43-year-old male presented with history of dull aching right sided abdominal pain. His pulse rate was regular and 75 per minute and blood pressures were 130/80 mm Hg. Heart sound was normal and there was no murmur. Chest and abdominal examinations were unremarkable. Ultra Sound abdomen shows a cystic mass in the liver segment VII, so further investigations are carried out. CT brain was free. CT chest + CTA show intramural cystic lesion (Figures 1(a), (b)). Lungs were free. CT abdomen + CTA show cystic lesion in the liver (Figure 2).
ECG was normal. Transthoracic echocardiography demonstrated a mixed echogenic mass of 54 × 51 mm on the posterolateral aspect of left ventricular free wall subpericardially. Transesophgeal echocardiography confirmed the findings of a mass lesion with areas of hypoechogenicity. The serum by ELISA was also positive for echinococcosis. Based on the CT scan findings, a diagnosis of Hydatid cyst in the liver and the heart was made and surgical excision was advised. The patient was on albendazole for 2 weeks prior to the surgery for the hepatic hydatid cyst, where deroofing of the cyst was made. Then after 3 months, we did the cardiac hydatid cyst
 (a)
(a) (b)
(b)
Figure 1. a axial and b reformatted coronal ECG (Electrocardiogram) gated images of heart showing well definite cystic mass lesion involving the anterolateral wall of the left ventricle in intramuscular location at the level of the left ventricular outflow without calcifications.

Figure 2. Axial post contrast images of the liver demonstrate the typical appearance of liver hydatid cyst with partially collapsed membrane.
enuculation. The operation was performed with median sternotomy and aorta-bicaval cannulation. The aorta was cross-clamped, hypothermic crystalloid cardioplegia and Isothermic. Potassium-enriched blood cardioplegic solution was used. Sponges soaked with hypertonic saline solution were distributed throughout the pericardial cavity to prevent local invasion by the parasite. The cyst was localized using needle aspiration until a greenish fluid had come out, then the incision to excise the cyst was parallel to and on the right side of the left anterior descending coronary artery to avoid damaging that vessel, we reached the cyst directly (Figures 3(a), (b)). We aspirated the entire contents of the cyst, removed its germinative membrane, and washed the cavity with 20% hypertonic saline solution. Capitonnage was performed, and the incision was closed with the use of Teflon felt. The postoperative period was uneventful.
2 weeks later, we did another CTA for the Chest. It was (Figures 4(a), (b)):
The postoperative period was uneventful. The patient came for the follow-up 1 week after discharged home, and he was doing fine, with stable vital sign, clean wound and stable sternum with no new complaints. A follow-up was done after 1, 3, 6, 12 months later and all were unremarkable.
2. DISCUSSION
Hydatid disease is a zoonotic infection caused by larval stages of dog tapeworms belonging to the genus Echinococcus and is also referred to as echinococcosis [1]. It is a common health problem in Mediterranean and especially in sheep-farming countries [2]. Cardiac Hydatid cysts are rare and occur in less than 2% of all hydatid cases [3].
The overall incidence of Echinococcus infection is 0.4 per 100,000 persons. Humans are an accidental intermediary host, although most often found in the liver (60% -
 (a)
(a) (b)
(b)
Figure 3. a: The cyst during the operation shown at the tip of the forceps. b: the cyst after excision in compare to syringe 20 cc.
70%) and lung (20% - 30%), hydatid cysts can occur in any organ or tissue. The Larvae reach the right side of the heart through thoracic duct and superior venacava; from the right ventricle the embryo passes through the pulmonary capillaries into the left ventricle, from where it could reach any part of the body through the systemic circulation. Some authors have suggested transmigration of embryo through the interatrial and interventricular septum to the left side of the heart. Larvae reach the myocardium through the coronary circulation. So involvement of the heart can occur from the systemic or pulmonary circulation or as direct extension from adjacent structures [4].
Dogs and other carnivores are the primary host and sheep the intermediate host, whereas humans are the accidental intermediate host who do not complete the life-cycle of the parasite. Humans usually become affected by the ingestion of food or water contaminated by dog faeces containing the eggs [5]. The embryos called oncospheres hatch in the intestine and migrate either through the portal venous system or the lymphatic
 (a)
(a)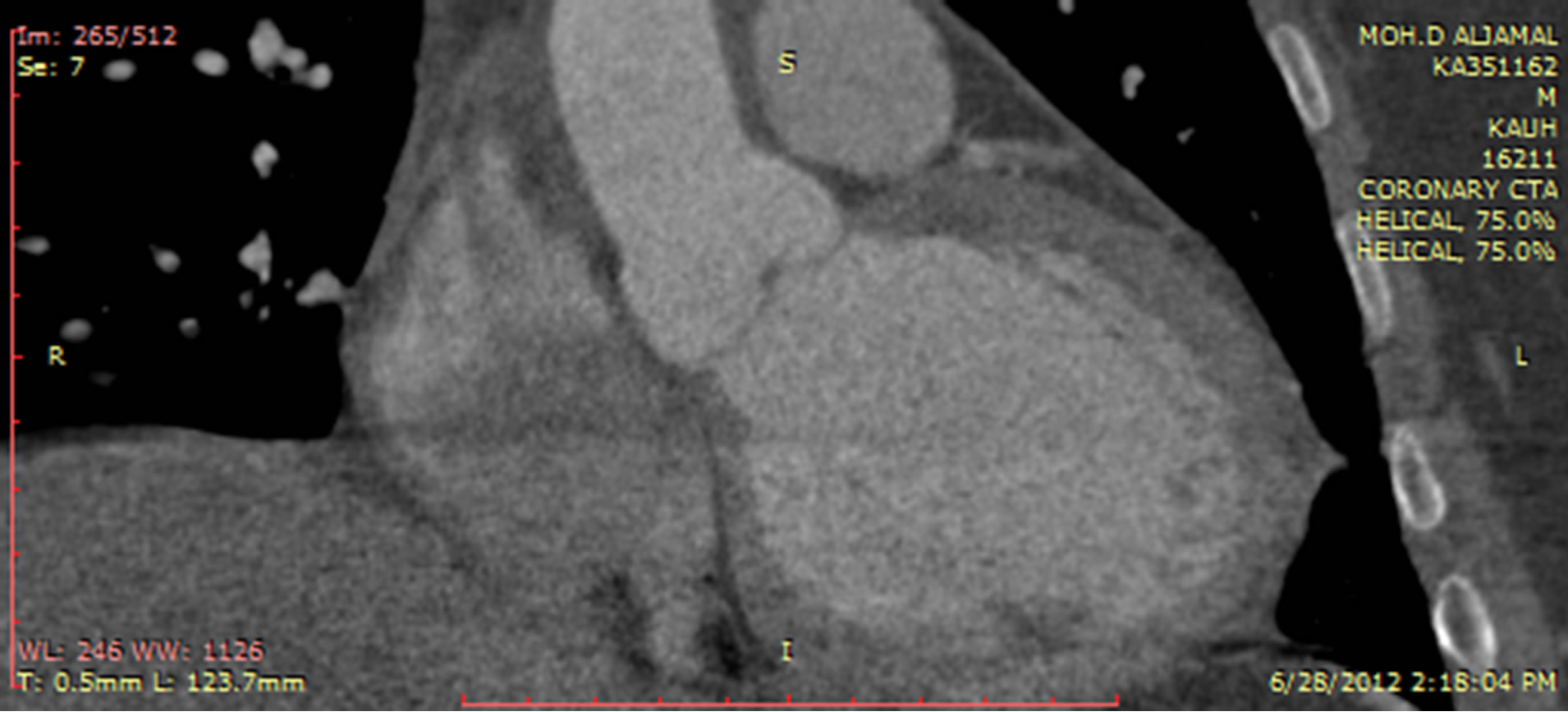 (b)
(b)
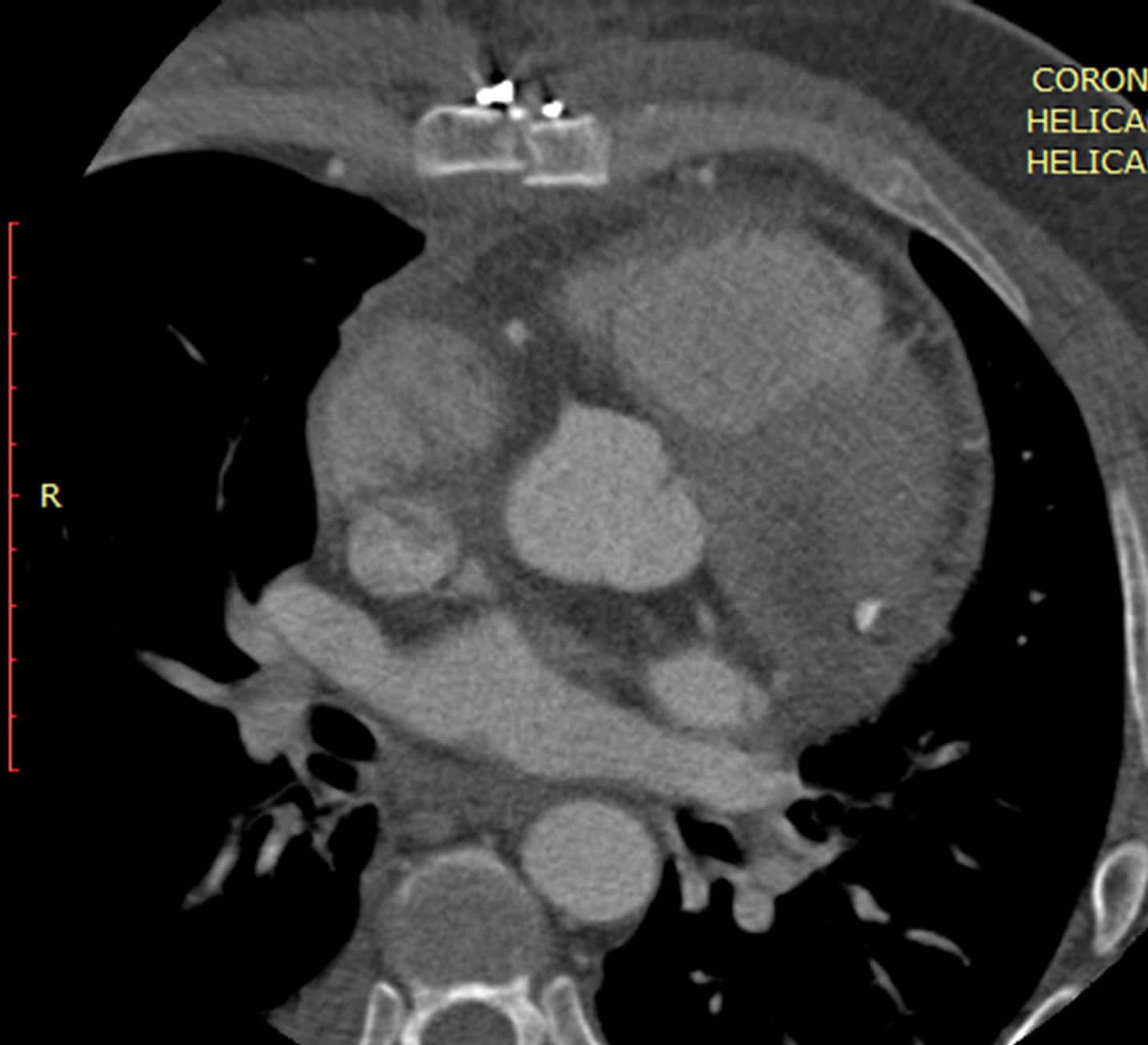
Figure 4. a axial and b coronal reformatted ECG gated images of the heart were obtained postoperatively showing post-operative changes with surgical sutures (arrow) and surgical scar at the site of previous surgery.
system through the thoracic duct. Those entering the portal system become lodged in the capillaries of the liver, where they either die or develop into hydatid cysts [5]. Some pass through this capillary sieve and lodge in other organs, including the lungs and the right side of the heart [5]. The parasite reaches the heart via the pulmonary artery, the coronary artery or via a patent foramen ovale [6]. In the initial stages of infection, the hydatid cyst often appears unilocular and contains a watery transudate. Histologically, the hydatid cyst consists of three layers: the pericyst is the protective outer layer formed principally by host reactive tissue; the middle layer is the laminated membrane permeable to nutrients; and the inner germinal layer gives rise to the scolices [5]. As the cyst grows, daughter cysts or brood capsules are formed from the germinal layer within the mother cyst, giving rise to the typical multiloculated ‘‘cystwithin-cyst’’ or ‘‘cartwheel’’ appearance. The daughter cysts are filled with a watery transudate of serum which contains proteins that are antigenic and capable of provoking anaphylaxis. These daughter cysts are separated from each other by the hydatid matrix. The matrix is composed of hydatid sand-containing membranes of broken daughter vesicles and scolices [5]. A dead cyst becomes calcified.
Cardiac hydatid cysts account for less than 2% of all hydatid diseases [3]. They most commonly affect the left ventricle (55% - 60%), but also the right ventricle, left atrium (8%), pulmonary artery, pericardium (7% - 8%) and the interventricular septum (5% - 9%) [5].
The clinical features of cardiac hydatid disease depend upon the site, size and stage of the cyst and the presence of haemodynamic consequences. When the interventricular septum is involved, disturbances in rhythm and haemodynamics, conduction blocks and features of right or left ventricular outflow tract obstruction can occur. Angina, valvular dysfunction and pulmonary hypertension, depending upon the location of the lesion, have also been reported. Complications such as anaphylaxis and embolisation into pulmonary and systemic sites can occur. Early diagnosis of this condition is crucial to avoid these complications. Occasionally, these cysts have been reported to cause coronary artery compression [7].
Surgical removal of the hydatid cyst remains the definitive treatment [8]. Risks at surgery from leakage of fluid include anaphylaxis and dissemination of the infected scolices. The latter complication can be minimised by the instillation of scolicidal solutions like hypertonic saline or ethanol. Hypertonic saline does not have any effect on the conduction system of the heart. Percutaneous aspiration has been effective in many cases of hepatic echinococcosis. Puncture - aspiration of cyst contentsinfusion of scolicidal agents and re-aspiration (PAIR) has been used as a percutaneous treatment in the management of cystic echinococcosis of the liver, peritoneum, spleen, kidneys and muscle, PAIR has not been used for cardiac echinococcosis [9].
The treatment of choice even for asymptomatic cardiac hydatid cysts is surgical excision, which yields complete recovery and excellent prognosis [10]. Although superficially located cysts can successfully be removed with a beating-heart (off-pump) technique, resection under cardiopulmonary bypass, since 1962, has been considered the safest method, with the least risk of spillage of cyst contents during the procedure.
Medical treatment with an anthelmintic regimen, a benzimidazole given either alone or combined with praziquantel, has been proven to give sometimes dramatic reduction in the number and size of hydatid cysts, but cannot be relied on to totally eradicate the disease [11]. Thus its role should be either prophylactic (preoperatively) or palliative when the disease cannot be extirpated because of multiple cyst infestation of an organ, or multiorgan involvement. Although it is recommended that medical treatment be started a few weeks prior to hydatid cyst surgery, delay of operation may not be advisable in cases of cardiac hydatidosis.
We didn’t find any identical case about intramural hydatid cyst in the literature review, so we did the basic principle management for hydatid cyst in the heart.
3. CONCLUSION
Due to the high risk of associated complications, cardiac hydatid cysts should be removed surgically, even in asymptomatic patients. During the operation, measures should be taken to prevent perioperative embolization of a germinative membrane. Surgical excision under cardiopulmonary bypass is the treatment of choice.
REFERENCES
- Craig, P.S., McManus, D.P., Lightowlers, M.W., Chabalgoity, J.A., Garcia, H.H., Gavidia, C.M., Gilman, R.H., Gonales, A.E., Lorca, M., Naquira, C., Nieto, A. and Schantz, P.M. (2007) Prevention and control of cystic echinococcosis. The Lancet Infectious Diseases, 7, 385- 394. http://dx.doi.org/10.1016/S1473-3099(07)70134-2
- Safioleas, M., Misiakos, E.P., Kakisis, J., Manti, C., Papachristodoulou, A., Lambrou, P., Tsinary, K.K. and Skalkeas, G. (2000) Surgical treatment of human echinococcosis. International Surgery, 85, 358-365.
- Eckert, J. and Deplazes, P. (2004) Biological, epidemiological, and clinical aspects of Echinococcosis, a zoonosis of increasing concern. Clinical Microbiology Reviews, 17, 107-135. http://dx.doi.org/10.1128/CMR.17.1.107-135.2004
- Ozer, N., Aytemir, K., Kuru, G., Atalar, E., Ozer, Y., Ovünç, K., Aksöyek, S., Gököz, A., Gürsel, G. and Kes, S. (2001) Hydatid cyst of the heart as a rare cause of embolization: report of 5 cases and review of published reports. Journal of the American Society of Echocardiography, 14, 299-302. http://dx.doi.org/10.1067/mje.2001.108474
- Polat, P., Kantarci, M., Alper, F., Suma, S., Koruyucu, M.B. and Okur, A. (2003) Hydatid disease from head to toe. Radiographics, 23, 475-494. http://dx.doi.org/10.1148/rg.232025704
- Thameur, H., Abdelmoula, S., Chenik, S., Bey, M., Ziadi, M., Mestiri, T., Mechmeche, R. and Chaouch, H. (2001) Cardiopericardial hydatid cysts. World Journal of Surgery, 25, 58-67. http://dx.doi.org/10.1007/s002680020008
- Elangovan, S., Harshavardan, K., Meenakshi, K., Swaminathan, T.S. and Murthy, P. (2004) Left ventricular hydatid cyst with myocardial infarction in a patient with severe rheumatic mitral stenosis. Indian Heart Journal, 56, 664-667.
- Kaplan, M., Demirtas, M., Cimen, S. and Ozler, A. (2001) Cardiac hydatid cysts with intracavitary expansion. The Annals of Thoracic Surgery, 71, 1587-1590. http://dx.doi.org/10.1016/S0003-4975(01)02443-2
- Gargouri, M., Ben Amor, N., Ben Chehida, F., Hammou, A., Gharbi, H.A., Ben Cheikh, M., Kchouk, H., Ayachi, K. and Golvan, J.Y. (1990) Percutaneous treatment of hydatid cysts (Echinococcus granulosis). CardioVascular and Interventional Radiology, 13, 169-173. http://dx.doi.org/10.1007/BF02575469
- Miralles, A., Bracamonte, L., Pavie, A., Bors, V., Rabago, G., Gandjbakhch, I. and Cabrol, C. (1994) Cardiac echinococcosis. Surgical treatment and results. The Journal of Thoracic and Cardiovascular Surgery, 107, 184-190.
- El-On, J. (2003) Benzimidazole treatment of cystic echinococcosis. Acta Tropica, 85, 243-252. http://dx.doi.org/10.1016/S0001-706X(02)00217-60
NOTES
*Corresponding author.

