Open Journal of Obstetrics and Gynecology
Vol.3 No.1A(2013), Article ID:27778,5 pages DOI:10.4236/ojog.2013.31A040
Morbidly Adherent Placenta (MAP): Lessons learnt
![]()
1Department of Obstetrics & Gynecology, ESI-PGIMSR, Basaidarapur, Delhi
2Department of Radiology ESI-PGIMSR, Basaidarapur, Delhi
Email: *ajgupta80@hotmail.com, sangeetagupta58@hotmail.com
Received 25 October 2012; revised 27 November 2012; accepted 3 December 2012
Keywords: Placenta Accreta; Morbidly Adherent Placenta; Cesarean Section; Hemorrhage; Maternal Mortality
ABSTRACT
Context: Once a rare occurrence, MAP is becoming an increasing threat to maternal lives. Aims: To summarize our experience in the management of patients with morbidly adherent placenta. Introduction: MAP is a potentially life threatening hemorrhagic condition responsible for 7% - 10% maternal mortality. Settings and Design: Tertiary care center. Methods and Material: Retrospective study in which data of twelve patients with clinical diagnosis of morbidly adherent placenta was reviewed from Jan 2009 till Sept 2012. Results: The incidence of placenta accreta was found to be increasing every year. Out of twelve cases with clinical diagnosis of MAP, placenta previa was present in 10/12 patients with MAP. All patients had history of previous section. Two patients with preoperative diagnosis of MAP on USG/MRI were found to be normal intra-operative and in one patient focal accreta was diagnosed intraoperatively. Nine patients of MAP underwent caesarean hysterectomy due to excessive bleeding during placental separation and were confirmed histo-pathologically (3 accreta vera, 3 increta and 3 percreta). Internal iliac artery ligation was done in 2 patients. Two patients with placenta percreta had bladder rupture which was repaired and these two patients subsequently expired. Conclusions: The incidence of placenta accreta is increasing due to higher cesarean section (C/S) rate. Key to successful outcome is awareness, anticipation, preoperative counseling, planning and multidisciplinary approach.
1. INTRODUCTION
Placenta accreta is a significant cause of maternal morbidity and mortality. It leads to significant maternal hemorrhage at the time of delivery. Normally, the placenta adheres to decidua basalis layer, allowing for a smooth separation of the placenta from the uterus after delivery. In patients with abnormal placentation, placenta is firmly bound to the defective decidua basalis layer or even to the myometrium, the condition is called as placenta accreta.
Varying degrees of placenta accreta are:
• Placenta accreta vera (placenta adheres to myometrium);
• Placenta increta (placenta invades the myometrium);
• Placenta percreta (placenta invades through the myometrium to the uterine serosa and may include invasion into other pelvic organs.
Major risk factor for MAP is Placenta previa with a history of previous Caesarean section.
Women with a previous Cesarean section (CS) require a higher index of suspicion as there are two problems to exclude: placenta previa and placenta accreta. Placenta previa itself raises the risk for accreta due to implantation over a highly vascular, poorly contractile lower uterine segment and an existing scar in the same area, obviously compounds the risk. Women with history of previous CS and who also have either placenta previa or an anterior placenta in the present pregnancy are at increased risk of placenta accreta and should be managed accordingly. Others risk factors are previous uterine surgery, previous dilatation and curettage, previous myomectomy, asherman Syndrome (endometrial defects), submucous leiomyomata, advanced maternal age, multiparity and tobacco use.
This study was conducted with an aim to review the incidence, presentation and management of MAP in our tertiary care institution in last four years and summarize our experiences in the management of such cases with review of literature. The purpose was to learn from our experiences and utilize the lessons learnt for planning future strategies for handling such life threatening situations as and when required.
2. SUBJECTS AND METHODS
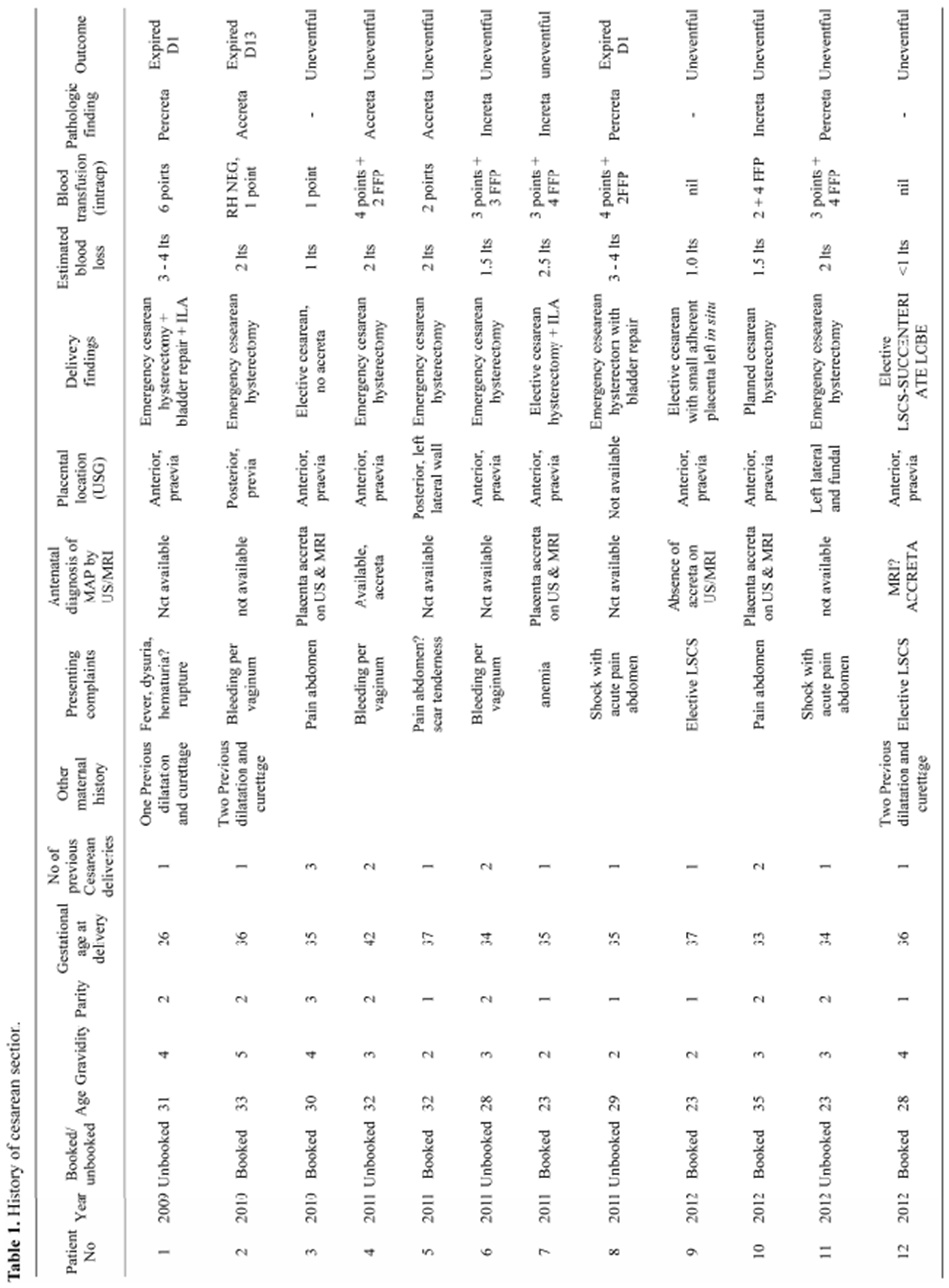
This was a retrospective study at a tertiary care centre in which data of twelve patients with clinical diagnosis of morbidly adherent placenta were reviewed from Jan 2009 till Sept 2012. The individual records of these patients were retrieved from medical record department of the hospital and analysed for age, fertility situation and disease history (Table 1). The study was approved by the departmental ethical committee.
3. RESULTS
There were 20,735 numbers of deliveries from year January 2009-September 2012. Among these we had 10 confirmed cases of morbidly adherent placenta making an incidence of 1/2073. The incidence of MAP increased from 1/5647 deliveries in 2009 to 1/969 deliveries in 2012.
All patients had history of previous cesarean section. Seven out of 10 cases had a history of 1 previous LSCS, 3 had history of 2 LSCS. Dilatation and curettage was done in 2 cases. All patients presented at the POG of 33 - 42 weeks except one patient who presented at POG of 26 weeks (Table 1).
Diagnosis of placenta accreta was made intra-operatively in 7 out of 10 patients while in 3 patients diagnosis of placenta accreta was made preoperatively by USG/ MRI. In 2 patients although MRI suspected accreta, intra operatively in one patient there was succenturiate lobe and in the other there was no MAP. Seven out of 10 cases had anterior placenta, while one had posterior-lateral and yet another had fundo-posterior placenta intraoperatively and one patient did not have the USG findings.
Nine patients of MAP underwent caesarean hysterictomy due to excessive bleeding during placental separation and were confirmed histo-pathologically (3 accreta vera, 3 increta and 3 percreta). Internal iliac artery ligation was done in 2 patients. Two patients with placenta percreta had bladder rupture which was repaired and these two patients subsequently expired.
Only 2 out of 10 had elective caesarean hysterectomy while rest 7 had emergency caesarean hysterectomy and one patient of focal accreta had elective cesearean delivery.
4. DISCUSSION
Placenta accreta is the most common reason for emergency postpartum hysterectomy and mortality rate is 7% - 10% [1] Placenta previa, especially with a history of Cesarean section, is a major risk factor for placenta accrete [2]. Incidence of morbidly adherent placenta is increasing secondarily to the rise of Cesarean section. In 1970 it was 1/7000, from 1985-1994 it increased to 1/ 2510 [3] and from 1992-2002 reported incidence is 1/533 [4].
In our study incidence of MAP was found to increase every year and especially all were patients with previous cesarean section. So it is important that one should counsel patients of previous cesarean about the possibility of MAP and risk involved with it.
Clinical consequences of placenta accreta are uterine perforation, massive hemorrhage at the time of placental separation, infection, hysterectomy & associated comorbidites as ureteral injury and fistula formation (5%), mortality (7.4%), postoperative infection (28%), transfusion (90%) [1].
In patients of previous cesarean section, whether placenta is anterior or posterior or not even previa, possibility of MAP should be kept in mind. The risk of placenta accreta increases from 3.3% in patients with history of one caesarean section and placenta previa to 11% in patients with history of two caesarean section and placenta previa to 40% with history of three caesarean section and placenta previa. While without placenta previa the risk of placenta accreta is just 0.03% in patients with history of one caesarean section, 0.2% in patients with history of two cesarean section to 0.1% with history of three caesarean section [5]. Thus placenta previa compounds the risk of placenta accreta in patients with history of caesarean section.
In the first case, patient presented at 26 weeks gestation with hematuria, intra-operatively diagnosed as placenta percreta invading the bladder and handling of which led to profuse uncontrollable hemorrhage and patient could not be saved. Placenta percreta is a catastrophic event. Placenta percreta induced uterine rupture has been reported as early as 9 and 14 wks. It can lead to the destruction of adjacent organs, most often the bladder, or surgical injury of pelvic structures due to loss of tissue planes. 75% cases of percreta are associated with placenta previa. The maternal mortality reported is 20% and perinatal mortality—30% [6]. In meta-analysis of 54 reported cases of placenta percreta, the diagnosis of MAP was made prenatally by USG or MRI in 33% of the cases. There were 39 urologic complications which included laceration of the bladder (26%), urinary fistula (13%), gross hematuria (9%), ureteral transaction (6%), and small capacity bladder (4%). Partial cystectomy was necessary in 24 cases (44%). There were 3 maternal deaths (5.6%) and 14 fetal deaths (25.9%) [7].
Management should involve multidisciplinary team of a uro-gynecologist, a urologist, and/or a gyne-oncologist. Preoperative cystoscopy and placement of ureteric stents may aid in identification of the ureters. If bladder invasion identified preoperative biopsy is contraindicated. Hemorrhage can be reduced by bilateral internal iliac artery and/or uterine artery ligation/placement of catheters in both internal iliac artery. Hysterectomy should be done by posterior approach-dividing uterosacral liga-
ments and entering vagina posteriorly. Involved portion of bladder is then resected with hysterectomy specimen.
In 2011, there was another undiagnosed case of placenta accreta which was detected intra-operatively. The surgeon had placenta accreta mindedness and was wise enough to arrange adequate blood preoperative, anticipate problem and took decision for hysterectomy timely. In such a case the uterine incision for delivering the baby should be made vertically and above the placental insertion site. One should never pull placenta. Intra-operatively, bleeding is rarely a problem until an attempt is made to remove the placenta and resort to hysterectomy sooner rather than later.
In subsequent cases the awareness increased and patients were well diagnosed and managed prenatally and intraoperatively. Sensitivity of USG in diagnosing placenta accreta is 93% and Specificity-79% [8]. MRI is no more sensitive than USG for diagnosing placenta accreta. Routine ultrasound scanning at 20 weeks of gestation should include placental localisation and these patients should have follow-up imaging if the placenta covers or overlaps the cervical os at 20 weeks gestation [9]. Those that were managed in emergency presented with vaginal bleeding at 33 - 42 weeks. In order to avoid an emergency cesarean and to minimize complications of prematurity it is acceptable to schedule cesarean at 34 to 35 weeks of gestation for suspected placenta accrete [10]. Multidisciplinary team & blood bank preparation may help reduce maternal morbidity and mortality. Mean estimated blood loss during surgery is 3 to 5 liters. Blood bank preparations include arrangement of cross matched blood and component therapy. Postoperative complication include DIC, fistula formation, ureteral stricture, urinary stasis, infection, Pelvic and renal abscess formation, Renal compromise, transfusion reaction, sepsis, ARDS, multi organ failure.
In last case of placenta percreta which presented in shock the team was well prepared in emergency and managed the patient effectively (Figure 1). Counseling was done for increase hemorrhage, massive transfusion and its affects, need for hysterectomy, senior obstetrician managed the case, availability of blood and component therapy and team work helped in saving life. Now we have standard operating protocols in labour ward for management of MAP and a contingency plan for an emergency delivery patient. Awareness of the entity, anticipating problem in advance and arranging help is a key to saving life of a mother.
Interventional radiology can be life saving for the treatment of massive postpartum hemorrhage, and therefore having this facility available locally is desirable. Since in our set up this facility is not available, internal iliac artery ligation is done if need arises. Balloon catheterisation/Selective arterial embolization (SAE) requires
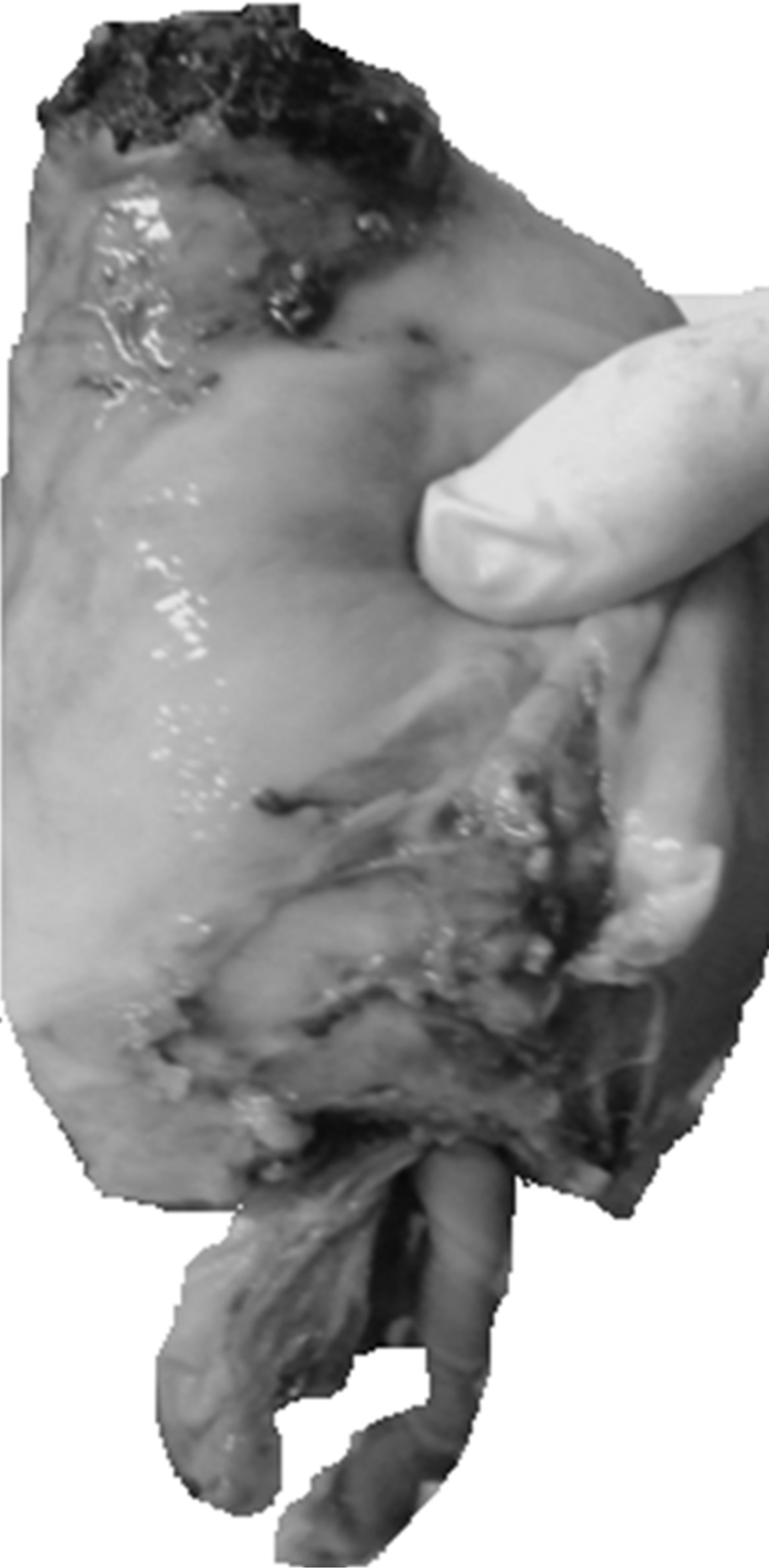
Figure 1. Placenta percreta popping out from fundus.
pre-delivery consultation with the interventional radiology team. Pre-operative placement of arterial catheters in internal iliac artery is done and after delivery balloons are inflated to achieve temporary homeostasis. If successful, uterus can also be preserved in highly selected cases. The place of prophylactic catheter placement for balloon occlusion or in readiness for embolisation if bleeding ensues requires further evaluation [10]. Advantages include avoidance of hysterectomy and preservation of fertility, lower estimated blood loss, reduced blood transfusion, low frequency of complications as post procedure fever and pelvic infection. Disadvantages are illiac artery thrombosis, uterine necrosis, sepsis, multiple organ dysfunction syndrome (MODS).
Uterus preserving modalities should be considered only in highly selected cases when blood loss is minimal and there is desire for fertility preservation [11]. There is currently insufficient data to recommend conservative approach routinely. In general, the recommended management of suspected placenta accreta is planned preterm cesarean hysterectomy with the placenta left in situ because attempts at removal of the placenta are associated with significant hemorrhagic morbidity.
5. CONCLUSION
Placenta accreta mindedness helps in saving maternal lives. Counseling and monitoring of patients at high risk for MAP on basis of history and ultrasound should start early in the antenatal period. Standard operating protocols should be available for handling and management for such life threatening situations as and when required. In cases of MAP, one should resort to hysterectomy SOONER RATHER THAN LATER and intra operatively; bleeding is rarely a problem until an attempt is made to remove the placenta.
REFERENCES
- O’Brien, J.M., Barton, J.R. and Donaldson, E.S. (1996) The management of placenta percreta: Conservative and operative strategies. American Journal of Obstetrics & Gynecology, 175, 1632-1638. doi:10.1016/S0002-9378(96)70117-5
- Hung, T.H., Shau, W.Y., Hsieh, C.C., Chiu, T.H., Hsu, J.J. and Hsieh, T.T. (1999) Risk factors for placenta accreta. Obstetrics & Gynecology, 93, 545-550. doi:10.1016/S0029-7844(98)00460-8
- Miller, D.A., Chollet, J.A. and Goodwin, T.M. (1997) Clinical risk factors for placenta previa-placenta accreta. American Journal of Obstetrics & Gynecology, 177, 210- 214. doi:10.1016/S0002-9378(97)70463-0
- Wu, S., Kocherginsky, M. and Hibbard, J.U. (2005) Abnormal placentation: Twenty-year analysis. American Journal of Obstetrics & Gynecology, 192, 1458-1461. doi:10.1016/j.ajog.2004.12.074
- Silver, R.M., Landon, M.B., Rouse, D.J., Leveno, K.J., Spong, C.Y., et al. (2006) Maternal morbidity associated with multiple repeat Cesarean deliveries. Obstetrics & Gynecology, 107, 1226-1232. doi:10.1097/01.AOG.0000219750.79480.84
- Price, F.V., Resnick, E., Heller, A.K. and Christopherson, A.W. (1991) Placenta previa percreta involving the urinary bladder. A Report of two cases and review of the literature. Obstetrics & Gynecology, 78, 508-511
- Washecka, R. and Behling, A. (2002) Urologic complications of placenta percreta invading the urinary bladder: A case report and review of the literature. Hawaii Medicine Journal, 61, 66-69.
- Fimberg, H.J. and Williams, J.W. (1992) Placenta accreta: Prospective sonographic diagnosis in patients with placenta previa and prior caesarean section. Journal of Ultrasound in Medicine, 11, 333-343.
- RCOG Green-top guidelines No 27, December 2011. www.rcog.org
- The American College of Obstetricians and Gynecologist, Committee Opinion Number 529, July 2012. www.acog.org.
- Steins Bisschop, C.N., Schaap, T.P., Vogelvang, T.E. and Scholten, P.C. (2011) Invasive placentation and uterus preserving treatment modalities: A systematic review. Archives of Gynecology and Obstetrics, 284, 491-450. doi:10.1007/s00404-011-1934-6
NOTES
*Corresponding author.

