Surgical Science
Vol. 3 No. 3 (2012) , Article ID: 18046 , 3 pages DOI:10.4236/ss.2012.33032
Respiratory Epithelial Adenomatoid Hamartoma of the Nasal Cavity: A Case Report
Government Medical College & Hospital, Chandigarh, India
Email: {drpunia, drharshmohan}@gmail.com, *irneet04@yahoo.co.in, adkusum@yahoo.com
Received November 23, 2011; revised January 30, 2012; accepted February 10, 2012
Keywords: Respiratory Epithelial Adenomatoid Hamartoma; Hamartoma; Nasal Cavity
ABSTRACT
Respiratory epithelial adenomatoid hamartoma (REAH) is an uncommon lesion of the upper aerodigestive tract. It usually presents as a nasal or as a sinus or nasopharyngeal mass. The potential danger associated with REAH is the risk of misdiagnosis. Recognition and awareness of this benign lesion is necessary to distinguish it from inverted papilloma and adenocarcinoma. This is important to avoid aggressive surgery. We report a case of REAH diagnosed on histopathology.
1. Introduction
Hamartoma is a rare, non-neoplastic malformation of tissue characterized by an abnormal mixture of tissues, which are indigenous to the region. Hamartomas are common in the lung, kidney, liver, spleen and intestine. Hamartomas of the sinonasal tract are uncommon and most often of the epithelial type. Respiratory epithelial adenomatoid hamartoma (REAH) is a recently described entity that usually presents as a nasal or, infrequently, as a sinus or nasopharyngeal mass [1]. Morphologically, it is composed of respiratory-lined glands surrounded by a thickened and hyalinized basement membrane often accompanied by an inflammatory background. It is a benign condition but the histopathological features can mimic inverted papilloma or well differentiated adenocarcinoma leading to misdiagnosis. Histopathological diagnosis is important as complete excision is curative for this entity. Misdiagnosis can lead to aggressive surgery.
2. Case Report
A 62 year female presented to the ENT OPD with complaints of nasal obstruction and hyposmia for the past 4 months. There was no other significant medical history. On physical examination there was a polypoidal mass occupying the right nasal cavity. CT scan revealed a mass in the upper nasal cavity and opacification of the ethmoid sinus. The patient underwent polypectomy and the tissue was sent for histopathological examination with a clinical diagnosis of inflammatory polyp.
Pathological Findings
Grossly there were variable sized multiple polypoidal tissue pieces which were grey white in appearance and all together measured 3 × 2 × 2 cm.
Microscopic examination of hematoxylin and eosin stained sections showed polyps lined by respiratory epithelium. The subepithelium showed glandular proliferation. The glands were of variable size and lined by ciliated respiratory epithelium. These were surrounded by hyalinized basement membrane. The nuclear features were bland. The lumina contained amorphous debris. The surrounding stroma showed edema and inflammation with prominence of eosinophils (Figures 1 and 2). Based on these findings a diagnosis of allergic polyp with respiratory epithelial adenomatoid hamartoma was made.
3. Discussion
Respiratory epithelial adenomatoid hamartoma (REAH) is an uncommon lesion of the upper aerodigestive tract, first described by Wenig and Heffner in 1995 [2]. In the largest series to date (31 cases), REAH was defined as an excessive proliferation of glandular respiratory epithelium and therefore considered to be a hamartoma. The authors postulated that the lesion arose from the surface epithelium in the setting of inflammatory polyps and in all likelihood were etiologically related to the inflammatory process [3]. This association was also seen in the present case.
Over 80% of patients with REAH are males, ranging in age from third to ninth decade with a median age in the sixth decade [4]. Symptoms of adenomatoid hamar-
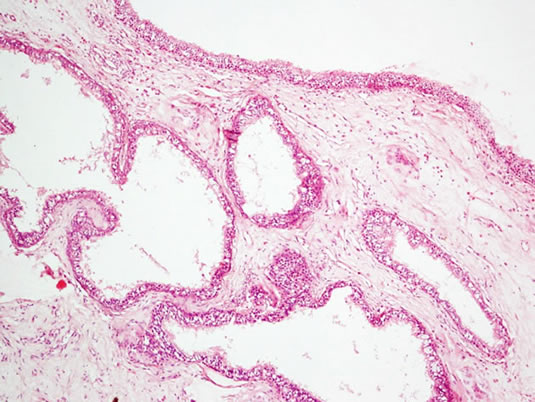
Figure 1. Photomicrograph showing glandular proliferation beneath the mucosal surface (H&E ×200).
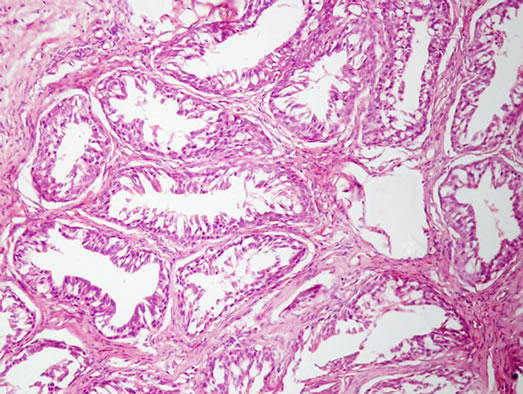
Figure 2. Photomicrograph showing back to black glands lined by respiratory epithelium within inflamed stroma (H &E ×400).
toma in the nasal cavity resemble chronic rhinosinusitis such as nasal obstruction, nasal stuffiness and epistaxis [5]. The most common identified site of occurrence is the nasal cavity, specifically the posterior septum. The lesion does not have predilection for laterality and often involves both nasal cavities. Radiographically the most common finding of REAH is an opacification of the affected sinus and some connection to the nasal septum [2].
REAHs are typically polypoidal or exophytic, rubbery, tan-white to red brown, and range upto 4.9 cm [6]. Microscopically, they appear as glandular proliferations, which in some places are in direct continuity with the surface epithelium. The glands themselves are composed of ciliated respiratory epithelial cells with lumina often filled with mucinous or amorphous debris. It has been hypothesized that they arise from overlying schneiderian epithelium like the normal seromucinous glands of the nasopharynx and paranasal sinuses [7]. The glands are widely spaced and characteristically surrounded by thick eosinophilic basement membranes [6]. Other histologic features described include stromal edema, polypoid growth, seromucinous gland proliferation, acute and chronic inflammation including neutrophils, eosinophils, lymphocytes, plasma cells and histiocytes and vascular and fibroblastic proliferation [2].
The importance of knowing this condition lies in the fact that it may be confused with more aggressive lesions, particularly the inverted papilloma (IP) and sinonasal adenocarcinoma. This may result in an unnecessarily aggressive surgical resection. In contrast to REAH which occurs primarily on the nasal septum IP arise almost exclusively on the lateral nasal wall in the vicinity of the middle turbinate and ethmoid sinus area. IPs are composed predominately of hyperplastic islands of squamous epithelium with a few interspersed mucus cells and a prominent intraepithelial component of neutrophils. The basement membrane around the epithelial islands is thin and delicate, unlike thick and hyalinized layer as seen in REAH. Seromucinous glands are sparse to absent in IPs [6]. The other entity from which REAH should be distinguished is sinonasal adenocarcinoma. Identification of the intervening stroma between the ciliated glands of a REAH is the most reliable way to distinguish this entity from low grade sinonasal adenocarcinoma, whose cribriform growth pattern has no intervening stroma between the glands. Mitotic figures are more often identified in sinonasal adenocarcinoma and can occasionally be abundant [7-9]. These features can help in correctly diagnosing REAH which being a rare entity is usually not considered in the differential diagnosis.
Complete surgical resection is the treatment of choice for REAH. Recurrences are practically nonexistent [5].
4. Conclusion
Respiratory epithelial adenomatoid hamartoma is a recently described entity characterized by abnormal glandular formations arising from the epithelium of the nasal cavity. Diagnostic misinterpretation is a serious issue regarding this lesion. REAH can mimic inverted papilloma and adenocarcinoma which are aggressive conditions. Pathologists and clinicians must be aware of REAH in order to avoid overdiagnosis and excessive surgical procedures for the patient.
REFERENCES
- J. A. Ozolek, E. L. Barnes and J. L. Hunt, “Basal/ Myoepithelial Cells in Chronic Sinusitis, Respiratory Epithelial Adenomatoid Hamartoma, Inverted Papilloma and Intestinal Type and Non Intestinal Type Sinonasal Adenocarcinoma: An Immunohistochemical Study,” Archives of Pathology and Laboratory Medicine, Vol. 131, No. 4, 2007, pp. 530-537.
- V. A. Fitzhugh and N. Mirani, “Respiratory Epithelial Adenomatoid Hamartoma: A Review,” Head and Neck Pathology, Vol. 2, No. 3, 2008, pp. 203-208. doi:10.1007/s12105-008-0064-3
- B. M. Weing and D. K. Heffner, “Respiratory Epithelial Adenomatoid Hamartomas of the Sinonasal Tract and Nasopharynx: A Clinicopathologic Study of 31 Cases,” Annals of Otology, Rhinology, and Laryngology, Vol. 104, 1995, pp. 639-645.
- R. D. Carlo, R. Rinaldi, G. Ottaviano and G. Pastore, “Respiratory Epithelial Adenomatoid Hamartoma of the Maxillary Sinus: A Case Report,” Acta Otorhinolaryngologica Italica, Vol. 26, 2006, pp. 225-227.
- C. Delbrouck, S. F. Aguilar, G. Choufani and S. Hassid, “Respiratory Epithelial Adenomatoid Hamartoma Associated with Nasal Polyposis,” American Journal of Otolaryngology, Vol. 25, No. 4, 2004, pp. 282-284. doi:10.1016/j.amjoto.2004.02.005
- L. Barnes, “Schneiderian Papillomas and Nonsalivary Glandular Neoplasms of the Head and Neck,” Modern Pathology, Vol. 15, No. 3, 2001, pp. 279-297. doi:10.1038/modpathol.3880524
- W. F. Ingram, M. C. Noone and M. B. Gillespie, “Respiratory Epithelial Adenomatoid Hamartoma: A Case Report,” Ear, Nose & Throat Journal, Vol. 85, No. 3, 2006, pp. 190-192.
- Z. Cao, Z. Gu, J. Yang and M. Jin, “Respiratory Epithelial Hamartoma of Bilateral Olfactory Clefts Associated with Nasal Polyposis: Three Cases Report and Literature Review,” Auris Nasus Larynx, Vol. 37, No. 3, 2010, pp. 352-356. doi:10.1016/j.anl.2009.10.003
- J. G. Seol, V. A. Livolsi, B. W. O’Malley Jr., J. Y. Chen and L. A. Loevner, “Respiratory Epithelial Hamartoma of Bilateral Olfactory Recesses: A Neoplastic Mimic?” AJNR, Vol. 31, 2010, pp. 277-279. doi:10.3174/ajnr.A1755
NOTES
*Corresponding author.

