Open Journal of Anesthesiology
Vol.3 No.3(2013), Article ID:31260,2 pages DOI:10.4236/ojanes.2013.33039
Epidural Blood Patch for Treatment of Postdural Puncture Headache in a Patient with Spinal Fusion and Recent Implantation of Intrathecal Pain Pump*
![]()
Division of Anesthesiology, Scott & White Memorial Hospital Temple, College of Medicine, Texas A&M University, College Station, USA.
Email: mvulcan@swmail.sw.org
Copyright © 2013 Chistopher J. Burnett et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received November 23rd, 2012; revised April 19th, 2013; accepted May 6th, 2013
Keywords: Epidural Blood Patch; Intrathecal Pain Pump; Spinal Fusion
ABSTRACT
We present an interesting case report of a 49-year-old female who presented with symptoms of post-dural puncture headache following implantation of an intrathecal pain pump. Her history was complicated by previous multi-level spinal fusion with hardware. The patient was evaluated and felt to be a candidate for epidural blood patch, which she elected to proceed with. Under fluoroscopic guidance epidural blood patch was successfully performed. Immediately following the procedure the patient noted significant improvement in the headache and six hours following the procedure was headache free and remained so at follow up three weeks later.
1. Introduction
Epidural blood patch is well described in the literature for treatment of postdural puncture headache especially in the area of obstetrical anesthesia. However, little information exists on the safety and efficacy of epidural blood patch in patients with a history of spinal surgery and persistent dural compromise from devices such as an intrathecal pain pump. This case report demonstrates that epidural blood patch can be performed safely and efficaciously in a subset of these patients.
2. Case Report
A 49-year-old female with chronic lower back pain and a history of lumbar fusion presented for severe headache of three weeks duration. The patient had medical history significant for six lumbar vertebrae and spinal fusion at the L5-L6-S1 levels with pedicle screws, intradiscal cages and bone grafts at multiple levels. The patient had undergone intrathecal pain pump implantation in the lumbar region 7 weeks prior to presentation at our clinic. She presented with a severe headache with photophobia and nausea that started 3 weeks after the implantation. The headache was alleviated by lying flat and worsened with standing or mobilization. The patient had attempted and failed conservative management. She was seen in referral per request of surgical team for evaluation for possible epidural blood patch. She was felt to be candidate for epidural blood patch and was subsequently counseled on risks and benefits of procedure and consent forms were signed.
She was placed in prone position in fluoroscopy suite and the lumbar spine was imaged which demonstrated six lumbar vertebrae and spinal hardware bilaterally, extending from L5 through S1 (Figure 1) and an intrathecal pain pump with catheter insertion at the L5-L6 level. An 18 gauge Touhey needle was inserted at the L5-L6 level to the right of midline and advanced into what was felt to be the epidural space using loss-of-resistance technique and intermittent fluoroscopy. Injection of 2 mL of contrast demonstrated satisfactory cephalad and caudal epidural spread. A total volume of 20 mL of autologous blood was then injected through the needle. The patient was observed in clinic for a brief period post-procedure and then discharged home with complete resolution of her headache. Follow up at three weeks demonstrated continued relief from the headache.
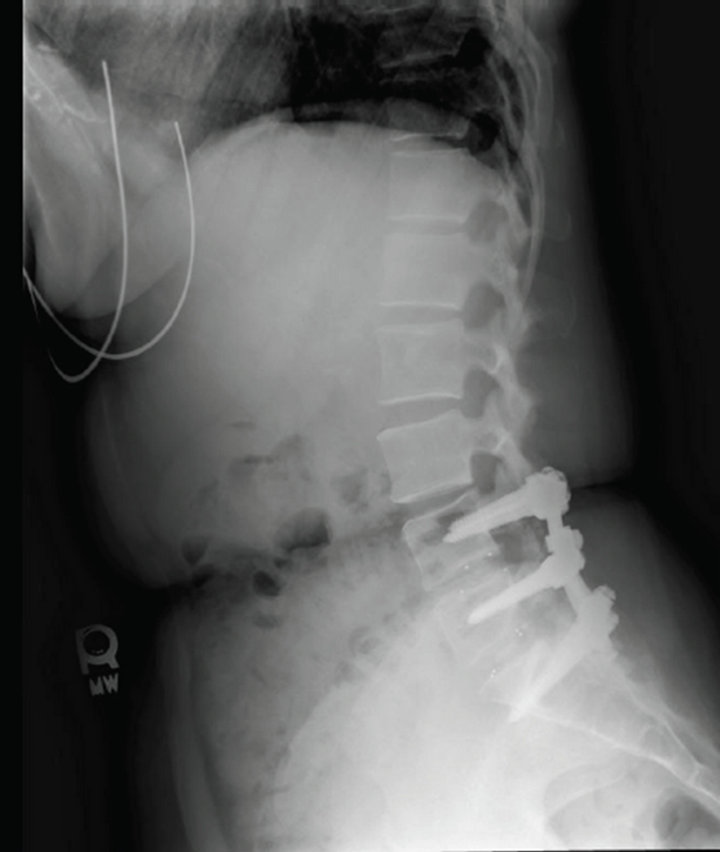

Figure 1. AP and lateral X-ray demonstrating multilevel fusion with hardware at levels L5 to S1.
3. Discussion
Epidural blood patch is a widely utilized treatment for post-dural puncture headache that has been studied and validated primarily in obstetrical anesthesia with reported success rates in the 70% - 95% range [1]. A paucity of information exists in patients with postsurgical changes that can cause a potential alteration or complete obliteration of the epidural space. Patients with history of lumbar spinal surgery could theoretically have no epidural space or significant alteration of the space, thus rendering lossof-resistance technique impossible and/or potentially dangerous. Additionally, with no epidural space, the question arises whether blood patching will be effective and by what mechanism the blood patch works in such a patient. Knight reports that up to 20% of all intrathecal pump implantations are associated with a persistent CSF leak [2] post-operatively and the potential exists for a significant number of those to be candidates for epidural blood patch. A case series by Munts involving 24 patients demonstrated an efficacy of only 54% for epidural blood patch [3] versus the previously stated 70% - 95% efficacy [1] for obstetrical anesthesia epidural blood patch. Epidural blood patch was performed successfully in this case, but further research into this modality of treatment is probably warranted so that the mechanism of action and safety profile can be further elucidated in patients with history of spinal surgeries before widespread adaptation can be advocated for.
REFERENCES
- F. van Kooten, “Efficacy of the Epidural Blood Patch for the Treatment of Post Lumbar Puncture Headache BLOPP: A Randomised, Observer-Blind, Controlled Clinical Trial,” BMC Neurology, 2005, Vol. 5, No. 12, 2005. doi:10.1186/1471-2377-5-12
- K. H. Knight, “Implantable Intrathecal Pumps for Chronic Pain: Highlights and Updates,” Croat Med Journal, Vol. 48, No. 1, 2007, pp. 22-34.
- A. G. Munts, “Postdural Puncture Headache in Complex Regional Pain Syndrome: A Retrospective Observational Study,” Pain Medicine, Vol. 10, No. 8, 2009, pp. 1469- 1475. doi:10.1111/j.1526-4637.2009.00727.x
NOTES
*We declare that there are no conflicts of interest present in any of the authors of this report.

