Open Journal of Psychiatry
Vol.04 No.04(2014), Article ID:50956,5 pages
10.4236/ojpsych.2014.44045
Cultural Influences on the Presentation of Depression
Ahmed Mohamed Abdel Shafi1, Reem Mohamed Abdel Shafi2
1Barts and The London School of Medicine and Dentistry, London, UK
2Fremantle Hospital, Fremantle, Australia
Email: a.m.a.shafi@smd10.qmul.ac.uk, Reem.Shafi@health.wa.gov.au
Copyright © 2014 by authors and Scientific Research Publishing Inc.
This work is licensed under the Creative Commons Attribution International License (CC BY).
http://creativecommons.org/licenses/by/4.0/



Received 23 August 2014; revised 10 September 2014; accepted 16 October 2014
ABSTRACT
Depression is predicted to become the second highest disease burden by 2020 as well as being a common mental health condition across the globe. Nevertheless, the presentation of depression varies depending on several factors with the patient’s cultural background playing a significant role. Although depression is such a universal condition, the manner of how a patient presents not only affects the clinician’s ability to make a diagnosis, but ultimately affects the wellbeing of the patient. It is therefore paramount that as clinicians we appreciate how culture not only affects the presentation of depression but also how cultural beliefs affect the patient’s acceptance of such a diagnosis.
Keywords:
Depression, Cultural Psychiatry, Affective Disorder

1. Introduction
Depression is an important diagnosis for doctors to make. Its prevalence is increasing and is a condition that some patients may not readily seek help for and suffer in silence. Due to advances in travel technology, there has been a worldwide phenomenon of cultural integration, leading to the phrase “multicultural”. However, due to the vast number of cultures there are different beliefs and opinions on many aspects. The focus of this review will be on how culture affects the way suffering patients present with depression.
2. Epidemiology of Depression
It is important to appreciate just how common depression is before delving into the subject matter. It is estimated that one in four people will suffer with a mental disorder at some time in their life time. Depression is predicted to be the second highest disease burden by 2020 as per the World Health Organisation (WHO) [1] .
Since the UK population is living longer psychiatric conditions will increase in prevalence. In 2002 depression was estimated to account for approximately around 4.5% of the total disease burden (in terms of disability) worldwide [2] .
The prevalence of several psychiatric disorders were compared and published in 2009, looking at the incidence over a 14 years period, showing that depression was the most common, illustrated in the following graph [3] [4] .
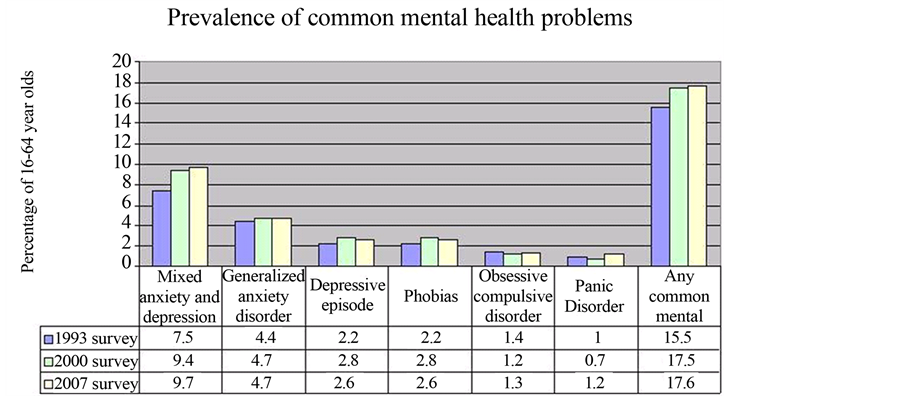
Graph shows the prevalence of common mental health problems since 1993 [3] .
Depression is a condition which may worsen over a period of time and is commonly found in patients who already suffer with a chronic condition. In a study published in 2007 by Moussavi et al., depression was found to produce the greatest decrement in the health of an individual when compared to other chronic conditions, illustrated in the following graph [5] .
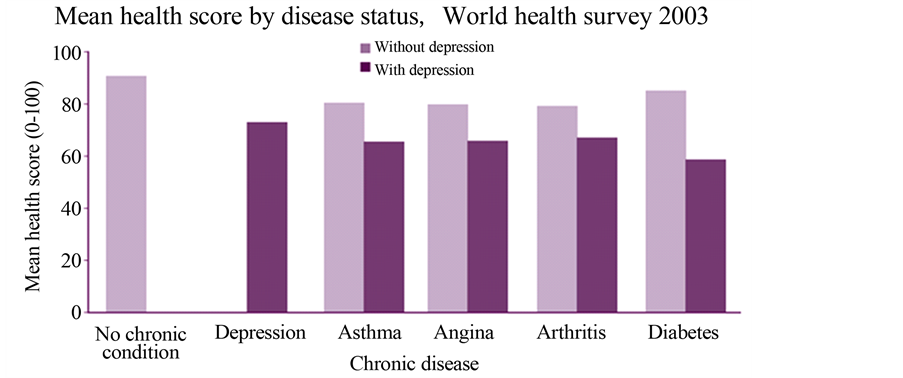
Graph illustrating the prevalence of depression in a number of chronic diseases [2] .
3. Depression: Its Symptoms and Presentations
Depression is a mood disorder with three core features; low mood (excessive sadness), anhedonia and anergia. These should be present for over two weeks. Additional symptoms include negative thoughts and pessimistic views of oneself, the future and the present (Becks triad of depression). Cognitive, biological or psychotic symptoms may also be in attendance [6] [7] .
Depression can be classified as mild, moderate, severe and severe with psychotic features. Some symptoms are more common than others as indicated in the following image [7] -[9] .
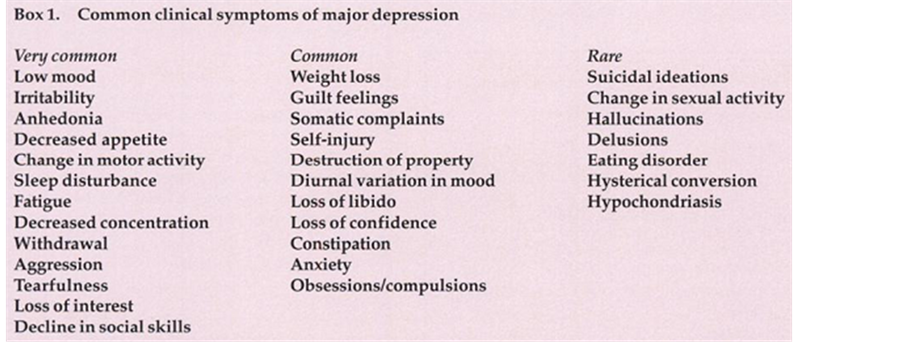
This summaries the very common, common and rare symptoms of major depression [9] .
Depression is diagnosed using the ICD-10 criteria or the DSM-IV criteria, however there are no tests that can be carried out to confirm if a patient has depression. The diagnosis is based on the presenting complaints of a patient and is the physician’s task to ask the relevant questions to make an accurate diagnosis.
Depression is not limited to a certain place or group of people and is therefore not confined by borders, racial background, age or wealth. The exact aetiology of depression remains unknown with multiple theories proposed. One of these is the monoamine theory, which hypothesises that depression may be due to a decrease in nora- drenaline, serotonin or dopamine which explains why antidepressants work as a treatment by increasing the level of these neurotransmitters [8] .
There are a number of risk factors that increase the likelihood of an individual developing depression e.g. female gender. A number of studies have shown that depression is more prevalent in women. Child-bearing women are also at risk of developing postpartum depression, with prevalence estimated to be 10% - 15% worldwide [10] . Other risk factors include (but are not limited to) suffering with a chronic condition, poverty, alcoholism, traumatic childhood experienced or bereavement, which may increase the chances of developing a stressful life.
In a study by McGirr et al., individuals that suffered with depression had a greater risk of committing suicide, with the onset of insomnia being indicative of immediate suicide risk whereas other symptoms (loss of appetite, thoughts of death and feeling worthless) where characteristic for the predisposition for suicide [11] .
4. Cultural Variations in the Presentation of Depression
Culture is defined as “the ideas, customs and social behaviour of a particular group of people or society”, suggesting that culture is a dynamic and evolving process that varies over time. However the discussion of culture in Psychiatry focuses on minorities that are considered to be distinct in some way [12] [13] .
The term culture can be influenced by your gender, age, race, religion, country of residence, country of origin and education. Globalisation has had a great effect on the integration of several cultures, with respect to cultural beliefs and ideology being accepted into other cultures. Several studies have looked into the variations in the presentation of depression, which could provide important clues as to why these variations occur.
A study by Kirmayer et al. (1993), found that the rate of diagnosis varied depending on how the patient presented. In some cultures visiting a doctor with depression is culturally unacceptable. It is therefore more common for these people to present with somatic symptoms, which is a frequently cited feature of depression. This may be viewed in some cultures to be a more appropriate reason to visit a doctor. This is referred to as “ticket behaviour” which may have less stigma associated with it, but can make it harder for the physician to diagnose depression and lead to unnecessary investigations as illustrated in the following graph [13] [14] .
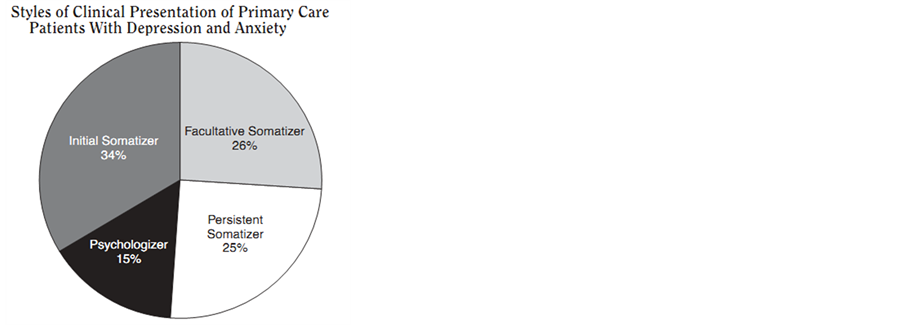
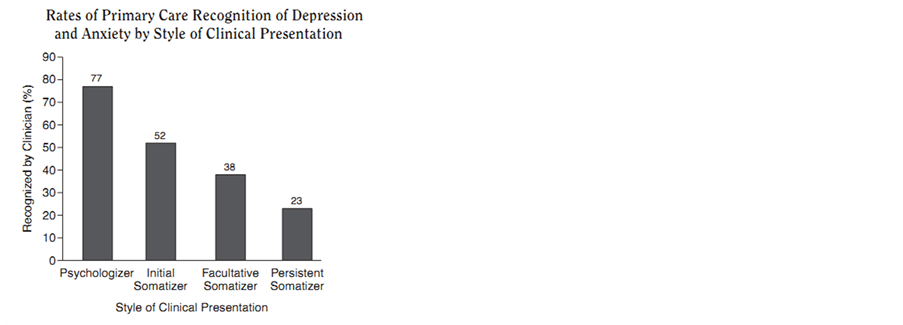
Pie chart shows the proportion of clinical presentation for patients with depression and anxiety. Bar chart shows the percentage of diagnosis of depression depending on the clinical presentation of the patient [13] .
Another study by Bhugra et al., concluded that the influence of culture and religion will lead to variation in presentation of depression, with somatic symptoms being the most common presenting compliant. This point is previously stated by Dejarlais et al., when they thought that cultural background would determine whether or not depression was expressed in psychological or physical terms [15] .
If we look at more specific studies we find different reasons for the variation in presentation. Looking at a study by Kleniman et al., we find that in the mid 1980’s only 1% of patients in a one week period who attend a psychiatric out patient’s clinic in Hunan, China were diagnosed with depression. However 30% were diagnosed as “neurasthenic”, which is commonly understood by the Chinese to mean “neurological weakness” which has become a common illness accepted by the public. Kleniman also noted that neurasthenia was a diagnosis more
accepted by Chinese patients and their psychiatrists [16] .
However a study by Yan et al., noted that patients who were commonly diagnosed with neurasthenia presented with insomnia, headache and poor concentration [17] . Neurasthenia is therefore a non-stigmatising diagnosis which is distinct from any psychiatric label such as depression which can be perceived as degrading. In a study by Lee et al., it described the popularity of the term “shenjongshuairuo” which is a translation of neurasthenia as “the indigenisation of a culture-friendly condition”, unlike depression which has several meanings in Chinese including, “restrain” or “gloomy” thereby making it socially and morally unacceptable [17] [18] . From this we can appreciate that a term in a certain language may have a different meaning and interpretation in another.
In another study, Bhugra et al., looked at Punjabi women of two generations, and found that pain was the most common symptom, which can be explained by understanding their culture. In Asian culture pain can mean suffering while at the same time disguising an underlying psychological disorder. The term depression was found to be recognised by the younger generation, whereas the older generation used terms such as “weight on my mind” or “pressure on the mind” [15] .
On interviewing an Arab patient, he told me that in Arab culture “there is no depression as such” and made a distinction between depression and illness. He also believed that if you were a “good believer” you didn’t deserve to be depressed and the solution is prayer rather than visiting a psychiatrist.
This view is reflected by other Arab patients as illustrated by Sulaiman et al., who looked at opinions of Arab woman and men in Dubai. There were different opinions among woman in the importance of crying when depressed. The older generation viewed it as shameful, believing that their inner feelings should be hidden and kept to themselves. If the emotional burden became unbearable they should cry when alone, as highlighted in one quote, “we are Arabs, we never cry, we endure, but these new generations, they are so soft and weak, they cry for any reason”. Whereas the young generations felt that expressing emotions through crying was more beneficial then hiding it, “a woman who cries feels better” [19] .
The view of turning to God as an adequate cure to treat depression is shared among Arab men and women. The accepted coping resources are speaking to relatives, asking God for help, reading a religious scripture, praying or asking a religious leader for guidance. These are viewed more favourably compared with seeking help from a psychiatrist. When you feel depressed, “complaining to Allah is enough”, “a psychiatrist cannot help the depressed patient if the problem which create this depression still exists” [19] .
Both genders appreciated the fact that if treatment was not sought, depression could progress to madness “jinoon”, “it may increase suicidal ideas”. This is interesting as although seeking treatment for depression from a psychiatrist was not a popular solution, there was an understanding that complications could arise without adequate treatment [19] .
Another study also analysing Arab patients noted that they used metaphors and proverbs to describe their depression, such as “a dark life” in addition to describing physical symptoms, which are accepted as a legitimate and morally acceptable reason to go to the doctor. In a study by Bazzoui et al., it states that the average Iraqi would come in with symptoms such as “oppression in the chest”, or “hunger for air” to describe their depression [20] .
5. The Issue of Stigma and Depression
Depression is considered in a number of cultures as degrading [18] . Patients may not readily seek help from a doctor instead turning to alternative means such as witch doctors or religious figures first. Stigma is therefore a barrier to treating depression and exacerbated by lack of public awareness and understanding of mental health [21] .
There have been efforts in the past to combat stigma associated with depression. For example in 1992 an initiative entitled “defeat depression” was launched by the Royal College of Psychiatrists and Royal College of General Practitioners [22] .
The role of stigma and depression is noted in Arab cultures, as a patient’s resistance to report depression is usually associated with fear of embarrassment or shaming their family. As stated in the study by Sulaiman et al., “our society looks at the person who visits the psychiatric clinic as though he is mad (majnoon) [19] [20] .
The issue of stigma can be summed up by the fact that it is a label of infamy and social disgrace in which the individual’s behaviour embarrasses family and friends. This can lead to fear of being disowned and brushed aside, leading patients to attempt concealing their true feelings as they don’t have the confidence to confide in someone to share their burden. The unfortunate consequence then is that treatment is sometimes not sought until they find themselves in very desperate situations or several areas of their lives have been affected (e.g. employment, relationships). Stigma exacerbates a condition that already negatively impacts very vulnerable individuals and their families.
6. Conclusions
It is clear from available research studies of different cultures that the understanding, meaning and implications of depression for individuals vary across cultures and continents. Since integration of cultures has occurred in many countries, it is important for a doctor to have some appreciation as to how a patient’s culture will affect their presentation, beliefs and acceptance of a diagnosis like depression.
In Western society the term depression is perhaps accepted more freely compared with other cultures. The term is readily used in everyday conversation, “I’m so depressed when we have exams”. However despite this, stigma is still a significant factor that hinders presentation and the progress of depressed patients. It is a doctor’s responsibility and duty to combat stigma by remaining open minded and facilitating clinical encounters with the aim of enabling the patient to confide in the doctor, safe in the knowledge that it is our aim to listen, treat and help without judgment.
It is therefore befitting to end with a statement by Skottowe, “The initial psychiatric interview is always important, but in no group of illnesses is it of greater importance as a first step in treatment than it is in the depressions. The gentle elucidation of all the symptoms is of the highest importance. Let the patient see that the doctor is thoroughly familiar with the kind of illness that confronts him; he knows the kind of feelings and thoughts that it brings the patient. This in itself is a most reassuring step” [23] .
Acknowledgements
We would like to thank Professor Korzsun, Dr. Bains and Dr. Darwiche for their advice and help. We would also like to thank our family and friends for their support.
References
- World Health Organisation. Mental Health, Disorders Management, Depression. http://www.who.int/mental_health/management/depression/en/
- World Health Organisation (WHO). World Heath Statistics 2007: Part 1—Ten Statistical Highlights in Global Public Health, 16.
- Mind.org.uk, for Better Mental Health, How Can We Help You, Mental Health Statistics, How Common Are Mental Health Problems. http://www.mind.org.uk/information-support/types-of-mental-health-problems/statistics-and-facts-about-mental-health/
- McManus, S., Meltzer, H., Brugha, T.S., Bebbington, P.E. and Jenkins, R. (2009) Adult Psychiatric Morbidity in England, 2007: Results of a Household Survey.
- Moussavi, S., Chatterji, S., Verdes, E., et al. (2007) Depression, Chronic Diseases, and Decrements in Health: Results from the World Health Surveys. The Lancet, 370, 851-858. http://dx.doi.org/10.1016/S0140-6736(07)61415-9
- Martin, E. (2007) Concise Medical Dictionary. 7th Edition, Oxford University Press, Oxford, 195.
- Bourke, J., Castle, M. and Cameron, A.D. (2008) Crash Course: Psychiatry. 3rd Edition, MOSBY Elsevier, Amsterdam, xii and 99-102.
- Stringer, S., Church, L., Davison, S. and Lipsedge, M. (2009) Psychiatry P.R.N.—Principles. Reality. Next Steps. Oxford University Press, Oxford, 32-40.
- Prasher, V. (1999) Presentation and Management of Depression in People with Learning Disability. Advances in Psychiatric Treatment, 5, 447-454.
- Halbreich, U. and Karkun, S. (2006) Cross-Cultural and Social Diversity of Prevalence of Postpartum Depression and Depressive Symptoms. Journal of Affective Disorders, 9, 97-111. http://dx.doi.org/10.1016/j.jad.2005.12.051
- McGirr, A., Renaud, J., Seguin, M., Alda, M., Benkelfat, C., Lesage, A., et al. (2007) An Examination of DSM-IV De- pressive Symptoms and Risk for Suicide Completion in Major Depressive Disorder: A Psychological Autopsy Study. Journal of Affective Disorders, 97, 203-209. http://dx.doi.org/10.1016/j.jad.2006.06.016
- (2011) Oxford Dictionaries, Dictionary, Meaning of Culture. Oxford University Press, Oxford.
- Kirmayer, L.J. (2001) Cultural Variations in the Clinical Presentation of Depression and Anxiety: Implications for Diagnosis and Treatment. Journal of Clinical Psychiatry, 62, 22-30
- Kirmayer, L.J., Robbins, J.M., Dworkind, M. and Yaffe, M.J. (1993) Somatization and the Recognition of Depression and Anxiety in Primary Care. American Journal of Psychiatry, 150, 734-741
- Bhugra, D. and Mastrogianni, A. (2006) Globalisation and Mental Disorders: Overview with Relation to Depression. The British Journal of Psychiatry, 184, 10-20. http://dx.doi.org/10.1192/bjp.184.1.10
- Kleinman, A., Anderson, J.M., Finkler, K., Frankenberg, R.J. and Young, A. (1986) Social Origins of Distress and Di- sease: Depression, Neurasthenia, and Pain in Modern China. Yale University Press, New Haven.
- Parker, G., Gladstone, G. and Chee, K.T. (2001) Depression in the Planet’s Largest Ethnic Group: The Chinese. Ame- rican Journal of Psychiatry, 158, 857-864. http://dx.doi.org/10.1176/appi.ajp.158.6.857
- Lee, S. (1998) Estranged Bodies, Simulated Harmony, and Misplaced Cultures: Neurasthenia in Contemporary Chinese Society. Psychosomatic Medicine. Journal of Behavioural Medicine, 33, 197-206.
- Sulaiman, S.O.Y., Bhugra, D. and Da Silva, P. (2001) Perceptions of Depression in a Community Sample in Dubai. Transcultural Psychiatry, 38, 201-218. http://dx.doi.org/10.1177/136346150103800204
- Al-Krenawi, A. and Grham, J.R. (2000) Culturally Sensitive Social Work Practise with Arab Clients in Mental Health Settings. Health and Social Work, 25, 9-22. http://dx.doi.org/10.1093/hsw/25.1.9
- Givens, J.L., Katz, I.R., Bellamy, S., Holmes, W.C. (2007) Stigma and the Acceptability of Depression Treatments among African Americans and Whites. Society of General Internal Medicine, 22, 1292-1297. http://dx.doi.org/10.1007/s11606-007-0276-3
- Sims, A. (1993) Discussion Paper: The Scar That Is More than Skin Deep: The Stigma of Depression. British Journal of General Practise, 43, 30-31.
- Maj, M. and Sartorius, N. (2002) WPA Series Evidences and Experiences in Psychiatry: Depressive Disorders. 2nd Edition, Wiley, Hoboken, 115-116.

